Abstract
Introduction/objectives
The clinicians initially prefer to define patients with the systemic autoinflammatory disease (SAID)’s based on recommended clinical classification criteria; then, they confirm the diagnosis with genetic testing. We aimed to compare the initial phenotypic diagnoses of the patients who were followed up with the preliminary diagnosis of a monogenic SAID, and the genotypic results obtained from the next-generation sequence (NGS) panel.
Method
Seventy-one patients with the preliminary diagnosis of cryopyrin-associated periodic fever syndrome (CAPS), mevalonate kinase deficiency (MKD), or tumor necrosis factor-alpha receptor-associated periodic fever syndrome (TRAPS) were included in the study. The demographic data, clinical findings, laboratory results, and treatments were recorded. All patients were examined by NGS panel analysis including 16 genes. The genetic results were compared with the initial Federici score to determine whether they were compatible with each other.
Results
Thirty patients were initially classified as MKD, 22 as CAPS, and 19 as TRAPS. The frequency of clinical manifestations was urticarial rash 57.7%, diarrhea 49.2%, abdominal pain 47.8%, arthralgia 45%, oral aphthae 43.6%, myalgia 32.3%, tonsillitis 28.1%, and conjunctivitis 25.3%, respectively. After NGS gene panel screening, 13 patients were diagnosed with CAPS, 8 with MKD, 7 with familial Mediterranean fever, 5 with TRAPS, and 2 with NLRP12-associated periodic syndrome. The remaining 36 patients were genetically identified as undefined SAID since they were not classified as one of the defined SAIDs after the result of the NGS panel.
Conclusions
We have demonstrated that clinical diagnostic criteria may not always be sufficient to establish the correct diagnosis. There is still low accordance between clinical diagnoses and molecular analyses. In the case of a patient with a preliminary diagnosis of a monogenic SAID with the negative result of target gene analysis, other autoinflammatory diseases should also be kept in mind in the differential diagnosis.
Key Points • Monogenic autoinflammatory diseases can present with different clinical manifestations. • The clinical diagnostic criteria may not always be sufficient to reach the correct diagnosis in autoinflammatory diseases. • In the case of a patient with a preliminary diagnosis of a monogenic SAID with the negative result of target gene analysis, other autoinflammatory diseases should be kept in mind in the differential diagnosis. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Systemic autoinflammatory diseases (SAIDs) are a broad spectrum of hereditary disorders characterized by unprovoked inflammatory episodes without the high-titer autoantibodies or antigen-specific T cells seen in classic autoimmune diseases. SAIDs typically present during childhood with recurrent episodes of fever, rash, abdominal pain, or disease-specific patterns of sterile organ inflammation and with a sign of inflammation in the blood [1]. Recent advances in basic sciences and human genetics have provided clinicians new insights to diagnose and differentiate these diseases. We know that most of these diseases are associated with mutations in specific genes such as in MEFV (NM_000243.2) gene in familial Mediterranean fever (FMF), MVK (NM_000431.2) gene in mevalonate kinase deficiency (MKD), TNFRSF1A (NM_001065.3) gene in tumor necrosis factor-alpha receptor-associated periodic fever syndrome (TRAPS), and NLRP3 (NM_004895.4) gene in cryopyrin-associated periodic fever syndrome (CAPS). Although all SAIDs usually present with fever, each disease has its own typical clinical findings. Thus, clinicians have created classification criteria for these diseases based on differences in clinical findings [2,3,4]. Clinicians are prone to identify suspected SAID cases based on the proposed classification criteria for autoinflammatory periodic fevers and then confirm their diagnosis by genetic testing. This approach has markedly improved the timeliness and accuracy of diagnosis, whereas at least 40% of patients with clinical signs and symptoms of the systemic inflammatory disease still do not meet any of the clinically defined diseases and have no known pathogenic mutation in well-known genes [5]. Furthermore, the genotype-phenotype correlation in these diseases has not been clarified definitely yet. Rowczenio et al. presented a lack of correlation between genotype and phenotype in patients with SAIDs, even if they were members of the same family [6]. De Piere et al. evaluated the genetic profile of 93 patients with SAIDs. Of these 93 patients, 12 patients were suspected of having a specific SAID [7]. However, after the target gene analysis, only three patients reached a definitive diagnosis. Recently, Ozyılmaz et al. evaluated the genotype-phenotype association in 211 patients with MKD, TRAPS, and CAPS [8]. Among these 211 patients, 147 patients underwent to Sanger sequence analysis of selected exons of MVK, TNFRSF1A, and NLRP3 genes while targeted NGS gene panel, covering all exons of MVK, TNFRSF1A, and NLRP3 genes, was performed on the remaining 64 patients. They concluded that the diagnostic utility rate was higher in the NGS group than the Sanger sequencing group (19% vs. 15.1%). Although the NGS gene panel provides accurate diagnosis more frequently, undoubtedly, further studies are required to demonstrate the genotype-phenotype correlation clearly.
The study aimed to compare the phenotypic diagnoses of patients who fulfilled the clinical classification criteria for MKD, TRAPS, or CAPS with their genotypic results obtained from the NGS gene panel.
Materials and methods
This is a prospectively designed study conducted at the University of Health Sciences, Umraniye Training and Research Hospital, Department Of Pediatric Rheumatology. The study group consists of patients who were admitted to the outpatient clinic after June 2016 with a preliminary diagnosis of SAID. Infections, malignancies, and other causes that may be the cause of fever were excluded in all these patients. All the participants were Caucasian and Turkish origin. The patients were followed up by the two pediatric rheumatologists (BS and FD) for a minimum of 6 months. A standard questionnaire for the differential diagnosis of SAIDs was filled out by the pediatric rheumatologist with direct conversation and medical records for each patient. The patients without fever and/or increased acute phase reactants in attack periods were excluded from the study. The patients who were found compatible clinical manifestations with the diagnosis of FMF or periodic fever, aphthous stomatitis, pharyngitis, and cervical adenitis (PFAPA) syndrome according to the Tel-Hashomer [9] or modified Marshall’s clinical diagnostic criteria [10] were also excluded from the study. The clinical diagnosis of CAPS, MKD, or TRAPS was made based on “The Eurofever clinical diagnostic/classification criteria-Federici score” [2]. According to the Federici score, cutoff values for clinical diagnosis are as follows: 52 for CAPS, 42 for MKD, and 43 for TRAPS. Finally, from the patients with the preliminary diagnoses of SAID, a total of 71 patients were fulfilled the Eurofever clinical diagnostic/classification criteria for MKD, TRAPS, or CAPS. The demographic data including age, gender, presence of consanguinity, family history of rheumatic conditions, clinical findings, and treatments were recorded. Laboratory results of the patients during the attack were also recorded. The cutoff values were defined as 0.5 mg/dL for C-reactive protein (CRP) and 7 mg/dL for serum amyloid A (SAA) by our laboratory. We determined fold changes of CRP and SAA levels compared to these cutoffs.
Following preliminary phenotypic diagnoses, all patients were examined by NGS panel analysis including 16 genes (MEFV, MVK, NLRP3, NLRP12, TNFRSF1A, TNFRSF11A, LPIN2, PSTPIP1, IL1RN, CECR1, ELANE, CARD14, IL10RA, IL10RB, NOD2, and PSMB8). The genetic diagnosis was made according to the genetic diagnosis guideline reported by Shinar et al. [11], and the new Eurofever/PRINTO classification criteria (2019) [4] for hereditary recurrent fevers including genetic and clinical variables, or with the level of evidence reported in the literature for other SAIDs [5, 12]. The patients were evaluated separately to achieve a higher rate of genetic diagnosis both with the new Eurofever/PRINTO classification criteria (2019) and the genetic diagnosis guideline by Shinar et al. Genetically undefined patients according to the specified classification criteria were also clinically classified according to the new Eurofever/PRINTO classification criteria (2019) (without genetic results) [4]. The genetic diagnosis of patients that concluded based on the NGS gene panel results and specified genetic guidelines was compared with the initial Federici score to determine whether they were compatible with each other.
Patients were classified as responsive to treatment in the absence of clinical symptoms with normalization of inflammatory markers. Partial response was defined as general amelioration of the clinical and laboratory findings without a complete normalization of the clinical manifestations and/or systemic inflammation [13].
The study was approved by the Ethics Committee of University of Health Sciences, Umraniye Training and Research Hospital. Written consents of the patients and parents were obtained according to the Declaration of Helsinki (1964).
Genetic analysis
Genomic DNA was extracted from peripheral blood samples as recommended by the manufacturer (Qiagen). The concentration and quality control (260/280 nm and 260/230 nm values) of the DNA samples were determined by fluorometrically (Qubit-v3.0) and UV-spectrophotometry. The library preparation for NGS was performed using Fever&Auto-Inflammatory Diseases Kit by Sophia-Genetics, a custom panel using a capture-based method. The gene panel consisted of 16 genes associated with periodic fever syndromes [MEFV (NM_000243.2), MVK (NM_000431.2), NLRP3 (NM_004895.4), NLRP12 (NM_144687), TNFRSF1A (NM_001065.3), TNFRSF11A (NM_003839), LPIN2 (NM_014646), PSTPIP1 (NM_003978), IL1RN (NM_000577), CECR1 (NM_017424), ELANE (NM_001972), CARD14 (NM_001257970), IL10RA (NM_001558), IL10RB (NM_000628), NOD2 (NM_022162), and PSMB8 (NM_004159)]. NextSeq-500-(Illumina) was used as the sequencing platform. Sequence analysis covers coding regions of each gene, including all coding exons, ± 10 base pairs of adjacent intronic sequences, and each nucleotide is read at a depth of at least 50×. Any variants that fall outside these regions and exonic variants with a variant fraction of less than 10% were considered as false positives and not analyzed. Variant fractions close to 50% were interpreted as heterozygous, while 100% variant fractions close to 100% were interpreted as homozygous. Deviations from these expected values were considered suspect as potential errors due to incorrect base calls or alignment and were verified by Sanger sequencing. With this analysis, copy number variations (CNV) were not examined. The DNA sequences were aligned to the NCBI Build 37 (hg19) version of the human genome. Variant calling and data analysis were performed by the Sophia-DDM-V5.2 bioinformatics analysis program. The interpretation of the variants was performed according to the 2015 ACMG standards and guidelines [14, 15]. To collect evidence reported in the ACMG guideline, we use a multi-step process. First, we exclude common polymorphic variants with a minor allele frequency of more than 1%. Since there are not enough genome and exome databases for the Turkish population, 1000 genome projects, dbSNP, ExAC, and GnomAD data were used as a control population. In the second step, synonymous variants were filtered out. Then, the effects of the variants on protein function were investigated by using prediction programs such as SIFT, Polyphen, Mutation Taster, and GERP. Variants, those with a possible pathogenic effect, were re-evaluated by using databases including ClinVAR, HGMD, and PubMed as well as with the inheritance pattern, clinical findings, and allele frequencies by literature review, based on the patient. In light of acquired evidence, variants were classified into five categories (benign, likely benign, variant of unknown significance (VUS), pathogenic, likely pathogenic) according to the 2015 ACMG standards and guidelines [14, 15]. Segregation analysis for potentially pathogenic mutations was performed by Sanger sequencing. Primer sequences and reaction conditions are available on request. Likely benign and benign variants were not reported in the results section.
Statistical analysis
Statistical package for the social sciences (SPSS) (version 23.0, SPSS-Inc., Chicago, IL, USA) was used for statistical analysis. The normality of the distribution of the variables was assessed by visual (histogram, probability plots) and analytic methods (Kolmogorov-Smirnov/Shapiro-Wilk’s test). Descriptive analyses were presented as percentages, medians, minimum (min), and maximum (max) values.
Results
Demographic and clinical features
A total of 71 patients were included in the study. Among them, 39 (54.9%) patients were male and 32 (45.1%) were female. The median (min-max) age of the patients was 8 (2–18) years. The median (min-max) age of symptom onset and diagnosis was 19 (1–135) months and 72 (13–210) months, respectively. All patients were followed up with a median of 12 (6–84) months. The consanguinity rate between parents was 28.1% (n = 20). Fourteen patients (19.7%) had a family history of SAIDs and 22 (30.9%) had a family history of autoimmune diseases in their first-degree relatives. The median (min-max) number of attacks per year was 12 (3–24) with a median duration of 5 (1–20) days.
All patients suffered from fever and 17 (23.9%) patients reported that their attacks were regular. Among 71 patients, 41 (57.7%) had urticarial rash, 35 (49.2%) had diarrhea, 34 (47.8%) had abdominal pain, 32 (45%) had arthralgia, 31 (43.6%) had oral aphthae, 23 (32.3%) had myalgia, 20 (28.1%) had tonsillitis, 18 (25.3%) had conjunctivitis, 8 (11.2%) had arthritis, and 6 (8.4%) had periorbital edema. Two patients (2.8%) had biopsy proved amyloidosis. The clinical characteristics of the patients according to phenotypic diagnosis subgroups are summarized in Table 1. The median (min-max) fold changes of C-reactive protein (CRP) (n < 0.5 mg/dL) and serum amyloid A (SAA) (n < 7 mg/dL) during attacks were 15 (3.3–90) mg/dL and 60 (4–300) mg/dL, respectively.
Among 71 patients, 30 (42.2%) patients were unresponsive to an adequate dose of colchicine, 25 (35.2%) patients had partial response while 16 (22.5%) were completely responsive to colchicine treatment. Twenty-four (33.8%) patients were using biologic agents. All patients receiving biologic agents were treated with canakinumab. Among them, 16 patients responded to canakinumab completely while eight patients had a partial response.
Genetic characteristics and final diagnosis
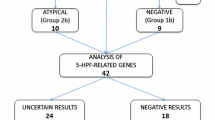
According to the Eurofever clinical diagnostic/classification criteria (Federici score), 30 (42.3%) patients were initially classified as MKD, 22 (31%) as CAPS, and 19 (26.7%) as TRAPS (Fig. 1). The median (min-max) Federici score of the patients at the initial diagnosis was 58 (43–80) for MKD, 75 (55–100) for CAPS, and 54 (48–87) for TRAPS. Based on the NGS gene panel results and specified genetic guidelines, 13 patients were genotypically diagnosed with CAPS, 8 with MKD, 7 with FMF, 5 with TRAPS, and 2 with NLRP12-associated periodic syndrome (NAPS12). Of the patients genotypically diagnosed with CAPS, 11 had heterozygous VUS, one had a compound heterozygous VUS, and another had a heterozygous likely pathogenic variant. Also, five patients diagnosed with TRAPS had heterozygous VUS. Of the patients genotypically diagnosed with MKD, three had the heterozygous pathogenic variant, two had the homozygous pathogenic variant, one had a homozygous likely pathogenic variant, one had a compound heterozygous pathogenic variant, and another one had a homozygous VUS. Among those diagnosed with FMF, three had the heterozygous pathogenic variant, two had the homozygous pathogenic variant, one had a likely pathogenic compound heterozygous variant, and another had a likely pathogenic heterozygous variant. Totally, while 23 patients were genetically diagnosed according to the new Eurofever/PRINTO criteria (2019), 33 patients were met genetic diagnostic criteria for a SAID based on the genetic diagnosis guideline by Shinar et al. [4, 11]. The diagnosis of two patients with NAPS12 was made with the level of evidence reported in the literature [12]. The remaining 36 patients were identified as undefined SAID since they were not classified as one of the defined SAID after the result of the NGS panel and reported guidelines [4, 5, 11]. One of these undefined patients was diagnosed with infantile-onset inflammatory bowel disease (IBD) during follow-up. The diagnosis of infantile-onset IBD was confirmed by colonoscopy and biopsy. The final genetic diagnosis of nine of the 35 genetically diagnosed patients (seven with FMF and two with NAPS12) was incompatible with their initial clinical diagnosis. The initial clinical diagnosis of only 26 (36.6%) patients was found consistent with the data of the NGS gene panel and genetic diagnosis (Table 2).
The patients could not be classified according to the reported genetic classification criteria (n = 36) were re-evaluated according to the new Eurofever/PRINTO clinical classification criteria (2019) [4]. The final clinical classification of 28 of these patients was consistent with their initial clinical diagnosis, while seven of these 36 patients were not classified as one of the SAID according to the new Eurofever/PRINTO classification criteria (2019) and defined as unclassified SAID. The other patient was diagnosed with infantile IBD (Table 2). The 28 patients without any confirmed genetic diagnosis were followed up and treated according to their last clinical diagnosis.
When we compared undefined SAID patients with the others, we could not find any differences in terms of demographic, clinical and laboratory findings, presence of family history and consanguinity, or treatment response.
Discussion
In the presented study, we compared the initial clinical diagnoses of patients with the genetic diagnoses, and the clinical diagnosis was confirmed with genetic results in only 26 (36.6%) patients. To our best knowledge, our study is the first to evaluate the concordance of the clinical classification criteria and genetic analysis.
Periodic fever syndromes occupy a significant place in clinical practice, especially in countries located in the Mediterranean region [16, 17]. The patients with SAIDs may express a variety of clinical findings ranging from recurrent self-limited fever and polyserositis attacks to persistent inflammatory courses including chronic arthritis, neurologic involvement, and amyloidosis. With the improvement of molecular analyses, 38 related SAID genes had been defined (https://infevers.umai-montpellier.fr/web/). However, we are still unable to point out any pathogenic mutation in at least 40% of patients with SAIDs [5, 18]. Screening of either a limited number of candidate genes or specific exons may be the cause of negative genetic results. Furthermore, screening a restricted number of genes or exons by Sanger sequencing may result in a waste of time and funding. Recently, Rusmini et al. alleged that using an NGS panel might improve the genetic diagnosis and reduce the diagnostic delay. They screened 50 patients with SAIDs with NGS including MEFV, MVK, TNFRSF1A, NLRP3, NLRP12, NOD2, PSTPIP1, IL1RN, LPIN2, and PSMB8 genes. However, they finally confirmed that it was remarkably difficult to set up a genotype-phenotype correlation without validated clinical criteria [18]. For this purpose, an international group of experts has developed a novel set of clinical classification criteria for SAIDs including FMF, MKD, TRAPS, and CAPS [2]. Subsequently, they combined clinical manifestations with genotype and proposed the new Eurofever/PRINTO classification criteria for hereditary recurrent fevers (2019) [4]. At present, we compared the accordance between the Federici score and the final genetic diagnoses of patients which were made base on the NGS panel results and current genetic diagnostic guidelines [4, 11]. We found that only one-third of patients (n = 26, 36.6%) fulfilled both the Federici score and the diagnostic criteria of current genetic diagnostic guidelines. In recent studies, patients with autoinflammatory disease clinical features who could not be classified in a monogenic SAID were defined as unclassified SAID patients [19]. We believe that further molecular analyses such as whole-exome sequencing (WES) may help clinicians to understand phenotype-genotype correlation or define a new type of SAIDs. Most recently, Kosukcu et al. [20] performed WES to 11 unclassified SAID and identified a definite or probable disease-associated variant in almost one-third of them.
Ter-Haar et al. [21] evaluated the clinical characteristics and genetic analyses of 187 patients with undefined SAIDs. Among them, 133 patients were negative for all clinical criteria while the remaining 72 patients met at least one clinical criterion. Of 187 patients, one hundred fifty-nine patients were evaluated with either complete gene screening or screening most relevant exons or mutations. Genetic variants were determined in only 15 patients. They also stated that some patients expressed distinct phenotypes. For instance, patients with pericarditis experienced their first attacks older while patients with intellectual impairment were younger at disease onset. Furthermore, they found a correlation between the presence of genetic variants and positive family history. Furthermore, De Pieri et al. showed that the response rate to corticosteroids was lower among patients with unclassified SAIDs having uncertain genetic results [7]. However, we could not find any differences in terms of demographic, clinical and laboratory findings, family history, or treatment response among undefined SAID patients comparing the others.
Colchicine is an ancient drug that acts via inhibiting cellular microtubules and it is still the mainstay treatment for FMF. However, the effectiveness of colchicine in other SAIDs is still a matter of debate. Some studies reported an inadequate response to colchicine in patients with SAIDs. Conversely, some researchers suggested that empiric colchicine and glucocorticoids controlled flares in the majority of patients with SAIDs [22]. Ter-Haar et al. [21] observed a complete response in 14.2% and partial response in 44.8% of 49 patients with unclassified SAIDs receiving colchicine. Correspondingly, Vitale et al. demonstrated a complete response in 12.5% and partial response in 58.3% of patients with TRAPS receiving colchicine [23]. In the present study, 35.2% of our patients had a partial response while 22.5% were completely responsive to colchicine. Previous studies showed that colchicine not only reduces the attack frequency in patients with FMF but also prevents secondary amyloidosis [24]. Amyloidosis is the most dreadful complication of chronic inflammation, which may develop in SAIDs other than FMF. In the present study, two patients were complicated with amyloidosis. Although biologic drugs emerge as an alternative approach while dealing with secondary amyloidosis, we prefer colchicine treatment before biologic drugs and continue colchicine treatment in these patients to prevent amyloidosis.
Herein, we evaluated 71 patients who were initially classified as MKD (n = 30), CAPS (n = 22), or TRAPS (n = 19) according to the Federici score. However, after the NGS gene panel screening, we confirmed the clinical diagnosis in only 26 patients. Patients may display overlap symptoms compatible with different SAIDs that make the assessment of genotype-phenotype association difficult. Furthermore, the presence of common variants or polymorphism complicates to decide the correct diagnosis. A group of experts evaluated genotype-phenotype correlation in 751 patients with SAIDs and a total of 149 variants were described [13]. However, the mentioned study was limited by its design of including only patients with a verified diagnosis of a SAID. In our study, seven patients were diagnosed with FMF after the NGS gene panel. Among them, three patients fulfilled the Federici score for MKD, and four met the Federici score for TRAPS. Four of the patients diagnosed with FMF had heterozygous pathogenic or likely pathogenic variants. Although FMF is an autosomal recessive inherited disease, it has been reported in the literature that the clinical features may emerge in children with heterozygous variants. In a study conducted in our center, M694V heterozygous carriage was found in 36.3% of 634 patients who had attack symptoms and were diagnosed with FMF [25]. Likewise, in this study, since three patients with heterozygous pathogenic variants and one had a heterozygous likely pathogenic variant with clinic findings of the systemic autoinflammatory disease, they were genetically diagnosed with FMF according to the genetic diagnosis guideline by Shinar et al. Furthermore, our two patients who were initially classified as having MKD finally diagnosed with NAPS12. Jeru et al. showed that the p.Arg352Cys missence mutation in the NLRP12 gene, also found in these two patients, was associated with a gain of function of caspase 1 processing [12]. NAPS12 is a rare autoinflammatory disease characterized by recurrent fever, rash, and musculoskeletal symptoms resembling familial cold autoinflammatory syndrome (FCAS). A Chinese study showed that the clinical manifestations between Chinese and Western patients may be different despite similar genotype [26]. The frequency of rash was higher in Chinese patients while oral ulcers were more common in Western patients [12]. The authors speculated that ethnic and environmental factors may influence the expression of the phenotype. Two of our patients with NAPS12 were initially diagnosed with MKD due to the presence of oral ulcers, abdominal pain attacks, diarrhea, and arthralgia.
Our study is limited by its small sample and lack of screening somatic mosaicism while it is strengthened by its method of evaluating the concordance of clinical classification criteria and genetic analyses. Furthermore, the NGS panel did not include all genes related to SAIDs.
In conclusion, we have demonstrated that clinical diagnostic criteria may not always be sufficient to establish the correct diagnosis. In the case of a patient with a preliminary diagnosis of a monogenic SAID with the negative result of target gene analysis, other autoinflammatory diseases should also be kept in mind in the differential diagnosis. Unfortunately, there is still low accordance between clinical diagnoses and molecular analyses. Therefore, we believed that these undefined patients will be diagnosed with the discovery of new SAIDs in the future, and new classification criteria will be determined.
References
Stoffels M, Kastner DL (2016) Old dogs, new tricks: monogenic autoinflammatory disease unleashed. Annu Rev Genomics Hum Genet 17:245–272
Federici S, Sormani MP, Ozen S et al (2015) Paediatric Rheumatology International Trials Organisation (PRINTO) and Eurofever Project. Evidence-based provisional clinical classification criteria for autoinflammatory periodic fevers. Ann Rheum Dis 74:799–805
Federici S, Vanoni F, Ben-Chetrit E, Cantarini L, Frenkel J, Goldbach-Mansky R, Gul A, Hoffman H, Koné-Paut I, Kuemmerle-Deschner J, Lachmann HJ, Martini A, Obici L, Ozen S, Simon A, Hofer M, Ruperto N, Gattorno M, Eurofever and the Pediatric Rheumatology International Trials Organization (PRINTO) (2019) An international Delphi survey for the definition of new classification criteria for familial Mediterranean fever, mevalonate kinase deficiency, TNF receptor-associated periodic fever syndromes, and cryopyrin-associated periodic syndrome. J Rheumatol 46:429–436
Gattorno M, Hofer M, Federici S, Vanoni F, Bovis F, Aksentijevich I, Anton J, Arostegui JI, Barron K, Ben-Cherit E, Brogan PA, Cantarini L, Ceccherini I, de Benedetti F, Dedeoglu F, Demirkaya E, Frenkel J, Goldbach-Mansky R, Gul A, Hentgen V, Hoffman H, Kallinich T, Kone-Paut I, Kuemmerle-Deschner J, Lachmann HJ, Laxer RM, Livneh A, Obici L, Ozen S, Rowczenio D, Russo R, Shinar Y, Simon A, Toplak N, Touitou I, Uziel Y, van Gijn M, Foell D, Garassino C, Kastner D, Martini A, Sormani MP, Ruperto N, Eurofever Registry and the Paediatric Rheumatology International Trials Organisation (PRINTO) (2019) Classification criteria for autoinflammatory recurrent fevers. Ann Rheum Dis 78:1025–1032
Russo RA, Brogan PA (2014) Monogenic autoinflammatory diseases. Rheumatology(Oxford) 53:1927–1939
Rowczenio DM, Trojer H, Russell T, Baginska A, Lane T, Stewart NM, Gillmore JD, Hawkins PN, Woo P, Mikoluc B, Lachmann HJ (2013) Clinical characteristics in subjects with NLRP3 V198M diagnosed at a single UK center and a review of the literature. Arthritis Res Ther 15:R30
De Pieri C, Vuch J, De Martino E et al (2015) Genetic profiling of autoinflammatory disorders in patients with periodic fever: a prospective study. Pediatr Rheumatol Online J 13:11
Ozyilmaz B, Kirbiyik O, Koc A, Ozdemir TR, Kaya Ozer O, Kutbay YB, Erdogan KM, Saka Guvenc M, Ozturk C (2019) Molecular genetic evaluation of NLRP3, MVK and TNFRSF1A associated periodic fever syndromes. Int J Immunogenet 46:232–240
Livneh A, Langevitz P, Zemer D, Zaks N, Kees S, Lidar T, Migdal A, Padeh S, Pras M (1997) Criteria for the diagnosis of familial Mediterranean fever. Arthritis Rheum 40:1879–1885
Thomas KT, Feder HM Jr, Lawton AR, Edwards KM (1999) Periodic fever syndrome in children. J Pediatr 135:15–21
Shinar Y, Obici L, Aksentijevich I, Bennetts B, Austrup F, Ceccherini I, Costa JM, de Leener A, Gattorno M, Kania U, Kone-Paut I, Lezer S, Livneh A, Moix I, Nishikomori R, Ozen S, Phylactou L, Risom L, Rowczenio D, Sarkisian T, van Gijn M, Witsch-Baumgartner M, Morris M, Hoffman HM, Touitou I, European Molecular Genetics Quality Network (2012) Guidelines for the genetic diagnosis of hereditary recurrent fevers. Ann Rheum Dis 71:1599–1605
Jéru I, Le Borgne G, Cochet E et al (2011) Identification and functional consequences of a recurrent NLRP12 missense mutation in periodic fever syndromes. Arthritis Rheum 63:1459–1464
Papa R, Doglio M, Lachmann HJ et al (2017) A web-based collection of genotype-phenotype associations in hereditary recurrent fevers from the Eurofever registry. Orphanet J Rare Dis 12:167
Richards S, Aziz N, Bale S et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17:405–424
Van Gijn ME, Ceccherini I, Shinar Y et al (2018) New workflow for classification of genetic variants’ pathogenicity applied to hereditary recurrent fevers by the International Study Group for Systemic Autoinflammatory Diseases (INSAID). J Med Genet 55:530–537
Karadag SG, Sonmez HE, Tanatar A et al (2020) Profile of new referrals to a single pediatric rheumatology center in Turkey. Rheumatol Int 40:313–321
Hashkes PJ (2003) Profile of a pediatric rheumatology practice in Israel. Clin Exp Rheumatol 21:123–128
Rusmini M, Federici S, Caroli F, Grossi A, Baldi M, Obici L, Insalaco A, Tommasini A, Caorsi R, Gallo E, Olivieri AN, Marzano AV, Coviello D, Ravazzolo R, Martini A, Gattorno M, Ceccherini I (2016) Next-generation sequencing and its initial applications for molecular diagnosis of systemic auto-inflammatory diseases. Ann Rheum Dis 75:1550–1557
Demir F, Doğan ÖA, Demirkol YK, Tekkuş KE, Canbek S, Karadağ ŞG, Sönmez HE, Ayaz NA, Doğanay HL, Sözeri B (2020) Genetic panel screening in patients with clinically unclassified systemic autoinflammatory diseases. Clin Rheumatol. https://doi.org/10.1007/s10067-020-05108-1
Kosukcu C, Taskiran EZ, Batu ED, Sag E, Bilginer Y, Alikasifoglu M, Ozen S (2020) Whole exome sequencing in unclassified autoinflammatory diseases: more monogenic diseases in the pipeline? Rheumatology (Oxford). https://doi.org/10.1093/rheumatology/keaa165
Ter Haar NM, Eijkelboom C, Cantarini L et al (2019) Clinical characteristics and genetic analyses of 187 patients with undefined autoinflammatory diseases. Ann Rheum Dis 78:1405–1411
Chandrakasan S, Chiwane S, Adams M, Fathalla BM (2014) Clinical and genetic profile of children with periodic fever syndromes from a single medical center in South East Michigan. J ClinImmunol 34:104–113
Vitale A, Sota J, Obici L, et al (2020) Role of colchicine treatment in tumor necrosis factor receptor associated periodic syndrome (TRAPS): real-life data from the AIDA Network. Mediators Inflamm. 27;2020:1936960
Livneh A, Zemer D, Langevitz P, Shemer J, Sohar E, Pras M (1993) Colchicine in the treatment of AA and AL amyloidosis. Semin Arthritis Rheum 23:206–214
Demir F, Bolac GL, Merter T et al (2020) The musculoskeletal system manifestations in children with familial Mediterranean fever. North Clin Istanb. https://doi.org/10.14744/nci.2020.96636
Wang W, Zhou Y, Zhong LQ, Li Z, Jian S, Tang XY, Song HM (2019) The clinical phenotype and genotype of NLRP12- autoinflammatory disease: a Chinese case series with literature review. World J Pediatr. 16:514–519. https://doi.org/10.1007/s12519-019-00294-8
Acknowledgment
We are grateful to all participating children and their families.
Author information
Authors and Affiliations
Contributions
B.S. and F.D. developed the concept and designed the study; B.S., F.D., H.E.S., S.G.K., and N.A.A. performed research and acquired data; B.S., F.D., Ö.A.K., Y.K.D., and H.L.D. analyzed and interpreted data; B.S. and F.D. wrote and reviewed the manuscript. All authors reviewed and revised the final version of the manuscript and they take full responsibility for the integrity of the study.
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sözeri, B., Demir, F., Sönmez, H.E. et al. Comparison of the clinical diagnostic criteria and the results of the next-generation sequence gene panel in patients with monogenic systemic autoinflammatory diseases. Clin Rheumatol 40, 2327–2337 (2021). https://doi.org/10.1007/s10067-020-05492-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05492-8




