Abstract
The International Classification of Functioning, Disability and Health (ICF) provides a common language to understand what health means. An ICF core set, a list of ICF categories affected by a certain disease, is useful to objectify the content validity of a health status measurement. This study aims to identify the potential items of a gout specific ‘ICF core set’. A three-round Delphi exercise was conducted, using web-based questionnaires. Health professionals, specialized in gout, nominated and subsequently rated the relevance of life areas divided into ICF categories. Agreement was determined by using the UCLA/RAND criteria. Simultaneously, a systematic review of gout measure outcomes was conducted. The results of these studies were compared using the second level of the ICF categories. In the Delphi study, consensus was found for 136 relevant ICF categories. The literature study extracted 134 different ICF categories in 149 articles. Three hundred and ten were non-defined outcomes. A large number of ICF categories were deemed to be relevant for people with gout. Only 29.7 % (19/64) of the level 2 categories, deemed to be relevant by health professionals, had been assessed as relevant in at least 5 % of gout outcome studies. Conversely, 70 % (19/27) of level 2 ICF categories assessed in at least 5 % of outcome studies were deemed relevant by health professionals. These ICF codes, which are found relevant in both studies, should be considered as mandatory in further research to a validated and practical core set of ICF categories. Published gout outcomes research fails to evaluate many life areas that are thought relevant by health professionals.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gout is a metabolic disease of abnormal urate deposition, leading to arthritis and sometimes tophus formation and nephrolithiasis [1]. The acute arthritis of gout is typically intensely painful and debilitating but intermittent in early stages, sometimes becoming persistent and deforming [2]. Comprehensive assessment of patients with gout in clinical practice or in clinical trials should include the impact of the disease on the patients’ day-to-day life. To date, most clinical trials determine the efficacy of gout treatment in terms of reduction in serum urate or generic health related quality of life (such as the Short Form 36 questionnaire) [3]. Another commonly used instrument in gout trials is the Health Assessment Questionnaire Disability Index (HAQ-DI), which, while validated in a gout population [4, 5], may not target the important lower limb issues characteristic of gout. Such generic instruments may be less applicable or not specific for particular disorders such as gout. They may miss concepts of importance and may not provide a comprehensive picture of the health of the patient. The only gout-specific instrument that has been developed in gout is the Gout Impact Scale of the Gout Assessment Questionnaire [6], but this may have technical psychometric shortcomings and was not endorsed by OMERACT as a good patient reported outcome measure [7].
The World Health Organization ratified the International Classification of Functioning, Health and Disability (ICF) in 2001, providing a useful model and common language for understanding what ‘health’ means [8]. In this model, health and disability are at each end of a spectrum that is characterized by optimal versus malfunctioning. Functioning can be considered at an organ level (body functions and structures), at the level of the individual person (activity limitations) and at a social level (participation restrictions). Examples of impairment of body function and structure are renal impairment, abnormal joint range of motion or joint space narrowing. Examples of activity limitations are difficulty walking, self-care or dressing. Examples of participation restrictions are problems with family relationships, inability to work or to be able to attend to community events. Furthermore, the model recognizes the influence on health not only by the pathological process (illness or injury) but also by the environmental and personal contextual factors. Examples of environmental factors include the level of healthcare available to the individual or the provision of a building modification to allow wheelchair access. Examples of personal factors include age and gender or psychological factors such as resilience. The ICF has codified over 1400 items (categories) of human life grouped into these components (excepting personal factors). Thus, the ICF provides a very useful and practical way of organizing the range of health deficits relevant to people with any particular disease, including gout.
In this study, we sought to elicit the range of relevant life areas for patients with gout, in the opinion of health professionals, and to compare this list with the range of life areas actually assessed in outcome studies of gout. The objective was to verify that the issues thought important by health professionals were being assessed in outcome studies. In addition, this study was part of a larger project to gather data that would inform the identification of core ICF categories for gout. Such core sets of ICF categories have been identified for rheumatoid arthritis [9], low back pain [10], osteoarthritis [11], ankylosing spondylitis (AS) [12] and several other non-rheumatic diseases [13]. In the case of AS, the ICF core set has been the starting point for the development of a disease-specific measure of health status (health-related quality of life) [14].
Materials and methods
Opinion of health professionals
A web-based Delphi study was conducted amongst health professionals identified from prior surveys, OMERACT gout working group members and contacts within gout clinical researchers. The first open-ended survey requested participants to nominate life areas of relevance for people with gout, within each component of the ICF (body structures, body functions, activities and participation and environmental factors). Each nominated life area was mapped to the most precise ICF category according to published linkage rules [15]. Life areas that were not able to be linked to an ICF category were classed as non-definable general health, non-definable physical health, health condition or personal factor. Then participants were asked to rate each ICF category for the relevance to a patient with gout, using a numerical rating scale 1 through 9 (definitely not relevant through definitely relevant).
Consensus was determined by means of the UCLA/RAND disagreement index [16], whereby an index score <1 was defined as agreement. ICF categories for which there was agreement and found to be relevant (median >6) or not relevant (median <4) were not rated again. All other ICF categories (median rating 4 through 6 or for which there was disagreement) were re-rated in further surveys. The median rating and interpercentile range (IPR) for each ICF category were provided for respondents to consider when re-rating in subsequent surveys. This continued until there was no further disagreement or participants made no changes to their rating judgements.
Outcomes from published gout studies
A systematic literature review was conducted using the PubMed, Medline and Cochrane databases to identify ICF categories that were assessed in outcomes studies. Studies were selected that met the following criteria: article includes outcomes related to adult gout patients; the outcomes that have been measured only concern people with gout. Studies that included other diseases and other types of arthritis or hyperuricemia without gout were excluded. Case studies of a single individual were also excluded.
From each study, every outcome assessment was abstracted. This included baseline assessments if that assessment variable was used as a covariate in the evaluation of outcome. For questionnaires or instruments that contained multiple items, each item was abstracted. Then, each outcome item was mapped to the most precise ICF category using the same linkage rules used in the Delphi study.
Comparison of ICF categories
The extent of overlap in ICF categories between the two data sources was described using the second level of classification for each category. Categories that received a median rating >6 during the health professional survey were compared to categories in published gout outcomes research, which appear in at least 5 % of the articles. This was done for each ICF component and items not ICF classifiable separately.
Results
Delphi survey of health professionals
A total of 147 health professionals were invited to participate. On the first and second questionnaire, there was a response rate of 44 % (64 participants) and 42 % (62 participants), respectively. Of these, 79 % (49 participants) completed both surveys. The third survey was completed by 85 % (53 participants) of the participants, who completed the second survey. The respondents originated from 22 countries, divided over five continents. There were 70 rheumatologists or rheumatology residents, 3 general practitioners, 2 nurses and 1 podiatrist included.
After the first round, 905 different life areas were collected. Those could be mapped onto 309 ICF categories, which belonged to the components of body functions (93), body structures (54), activities and participation (109) and environmental factors (53). Another 26 items were not definable within the existing categories of ICF. Those were divided into nine health conditions, three personal factors, six non-definable physical health (nd-ph) items and eight non-definable general health (nd-gh) items. During the second iteration, three environmental factors and two non-definable factors were added.
In the second round, agreement was found for 120 relevant ICF categories (disagreement index <1 and median >6) divided into 35 body functions, 18 body structures, 58 activities and participation and 9 environmental factors. There were 20 additional non-definable items.
In the third round, or second scoring iteration, there was agreement for a further 16 relevant ICF categories divided in 3 body functions, 2 body structures, 5 activities and participation and 6 environmental factors. There were two additional non-definable items. As summarized, the final list of relevant ICF categories contains 136 relevant ICF categories and 22 non-ICF definable items.
Pain in body parts (b2801), pain in joints (b28016), mobility in joint functions (b710) tophi (nd-ph) and MSU deposition (nd-ph) reached the highest ratings with consensus for a median relevance rating of 8.5–9. Additionally, 32 items were judged slightly lower with ratings of a median of 7.5–8, and 121 items were judged with a median of 6.5–7. The specific results for all relevant items (median ratings 6.5–9), ordered by relevance based on their median, are displayed in supplementary Tables 1, 2, 3 and 4. These items are summarized by collapsing categories to the relevant level 2 category (Table 1). Where more than one narrower ICF category was judged as relevant within a level 2 category, the higher rated median rating is shown.
There was agreement that 25 ICF categories were not relevant (median <4) divided into 6 body functions, 15 body structures, 1 activity and participation and 3 environmental factors. There were no additional non-definable items found to be irrelevant. During the process, uncertainty (median rating between 4 and 6) remained about the relevance of 151 ICF categories and 6 non-definable items. Additionally, 16 uncertain items did not achieve consensus. Significant change in opinion (difference in median >1) in those items was not measurable anymore after 2 iterations and since there were no new items being nominated, the survey stopped.
Literature review
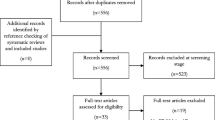
Using the pre-defined search strategy, the PubMed search contained 122 results; Medline search contained 170 results; and Cochrane search contained 19 results. After screening the titles, we excluded 149 out of 311 non-duplicate articles (23 duplicates). The reasons for exclusion were that they were about hyperuricemia rather than gout patients (n = 81); because they did not contain any outcomes; and they were just descriptions of existing knowledge about gout or literature updates (n = 32) and case reports (n = 11). One study was excluded because it only evaluated diagnostic tools. One study was excluded because it contained only pharmacological parameters.
After screening the abstracts, 12 articles were excluded. Four articles were excluded because they did not include only gout patients. Two studies were case reports. Three studies did not contain outcomes. One study was a pharmacological study. Two studies did not show any results, in which they were just study protocols. After reading the full texts, two studies were excluded. One study did not contain any outcomes. One study included patients with other diseases. One additional study that was identified after supervisor review via expert knowledge was included. In total, 149 articles were fully included for review.
In total, 1571 different outcomes were extracted. All outcomes were linked into 134 different ICF categories: body functions (445 outcomes), body structures (118 outcomes), activities and participation (197 outcomes) and environmental factors (261 outcomes). A list of all level 2 ICF categories used and the percentage of articles that used the ICF category can be found in Table 2. For level 2 categories in which more than one narrower category was used, the frequency refers to the most frequent category used in outcomes studies. The ICF codes that appear in more than 5 % of the articles are found to be relevant.
A list of the most highly rated and/or frequently published ICF second-level categories is shown in Table 3.
Discussion
A large number of ICF categories were deemed by health professionals to be relevant for people with gout. Only 29.7 % (19/64) of these have been assessed as relevant in at least 5 % of gout outcomes studies, suggesting inadequate coverage of important life areas. Conversely, 70 % (19/27) of categories assessed in at least 5 % of outcome studies were deemed relevant by health professionals. The ICF components least well assessed in published research are ‘activities and participation’ and ‘environmental factors’ (see Fig. 1). Those ICF categories which are relevant from both data sources should be considered as mandatory in further research to a validated and practical core set of ICF categories. The ICF codes that found to be relevant in only one of the two studies perhaps should be reconsidered.
Extent of overlap between reported outcomes research (at least 5 % of articles) and health professionals’ opinions (median rating at least 6) on the relevance of ICF second-level categories to people with gout, showing the number of categories in each ICF component (BS body structures, BF body functions, AP activities and participation, EF environmental factors)
Several non-definable items were rated highly by health professionals within the categories of other health conditions (e.g. diabetes mellitus), personal factors (e.g. gender), non-ICF definable physical health concepts (e.g. tophi) and non-ICF definable general health concepts (e.g. long intercritical periods). These non-definable items can be found in Table 2. Of these categories, other health conditions were recorded frequently in published outcomes literature (93 % of articles), non-ICF physical health concepts (10 % of articles), quality of life concepts (5 % of articles) and personal factors (48 % of articles).
It is very likely that patients will have different views about which ICF categories are of relevance to them, and it will be necessary to gather data directly from patients before determining a final list of the most relevant ICF categories for gout that should be assessed in outcomes research or clinical practice. A qualitative study of interview data from individuals and focus groups of people with gout is presently underway.
In the limited work already undertaken on life areas considered to be affected by gout in the opinion of gout patients, similar concerns have been identified. A study from Barcelona found that the six most frequent concerns were pain, joint stiffness, joint swelling/inflammation, dietary restrictions, not being able to work, not being able to sleep and not being able to wear shoes [17]. Another qualitative study from New Zealand found that concerns of people with gout included not only the direct effects of the disease but also the progressive nature of the condition (increasing flare frequency, dietary triggers, reduced effectiveness of acute gout medications) and lack of knowledge about gout (encompassing social stigma and stoicism) [18].
Further limitations to this study include the low response rate to the Delphi survey. Most respondents were rheumatologists with an interest in gout, and the results may be different with a much broader range of health professionals, particularly primary care physicians or nurses who treat a different spectrum of disease severity, and where the majority of gout patients received care. Further projects should involve primary care health professionals to a greater extent.
In addition, and despite the use of mapping rules, there was the possibility of inconsistently mapping the same item (whether identified from outcomes research or elicited from HP) by individual interpretation. This was mitigated to a significant extent by having a third author (WJT) independently check the mapping procedures in a sample of items from each source and resolving differences by consensus. The mapping procedure was performed by one author (MJN) for the literature review and by another author (EMK) for the Delphi survey. Furthermore, by condensing the ICF categories to the second level for the comparison, any inconsistencies from precise categorization are likely to be greatly reduced.
The large number of ICF categories elicited by health professionals partly reflects the broad question put to them, which concerned life areas of relevance for people with gout. This necessarily includes life areas of relevance to most people, whether or not they have gout and it will be sensible for the final list of important gout-specific ICF categories to consider both relevance and relationship with gout. Some items thought to be relevant by HP include comorbidities, which are more frequent in gout and contribute to impaired health status but are not intrinsic to the disease.
Ultimately, a preliminary set of core ICF categories for gout needs to be decided by a consensus meeting between patients and health professionals, having regard for the data collected in the current study and other data sources (especially data from patients). Nonetheless, the relative infrequency of outcomes in clinical gout research that pertain to patient-centred issues does suggest a need for a change in how clinical trials are designed, especially with regard the primary endpoint.
References
Neogi T (2011) Clinical practice. Gout. N Engl J Med 364:443–452
Taylor WJ, Grainger R (2012) Clinical features of gout. In: Terkeltaub R, ed. Gout and other crystal arthropathies, Firstth edn. Elsevier Saunders, Philadelphia PA
Taylor WJ (2013) Measurement of outcome in gout. Indian J Rheumatol 8:S11–S15
Alvarez_Hernandez E, Pelaez_Ballestas I, Vazquez_Mellado J et al (2008) Validation of the Health Assessment Questionnaire disability index in patients with gout. Arthritis Rheum 59:665–669
Taylor WJ, Colvine K, Gregory K, Collis J, McQueen FM, Dalbeth N (2008) The Health Assessment Questionnaire Disability Index is a valid measure of physical function in gout. Clin Exp Rheumatol 26:620–626
Colwell HH, Hunt BJ, Pasta DJ et al (2006) Gout Assessment Questionnaire: initial results of reliability, validity and responsiveness. Int J Clin Pract 60:1210–1217
Singh JA, Taylor WJ, Simon LS et al (2011) Patient-reported outcomes in chronic gout: a report from OMERACT 10. J Rheumatol 38:1452–1457
World Health Organisation (2002) Towards a common language for functioning, disability and health: ICF. World Health Organisation, Geneva
Coenen M, Cieza A, Stamm TA, Amann E, Kollerits B, Stucki G (2006) Validation of the International Classification of Functioning, Disability and Health (ICF) core set for rheumatoid arthritis from the patient perspective using focus groups. Arthritis Res Ther 8:R84
Cieza A, Stucki G, Weigl M, et al. ICF core sets for low back pain. J Rehabil Med 2004:69–74
Dreinhofer K, Stucki G, Ewert T, et al. ICF core sets for osteoarthritis. J Rehabil Med 2004:75–80
Boonen A, Braun J, van der Horst Bruinsma IE, et al. ASAS/WHO ICF core sets for ankylosing spondylitis (AS): how to classify the impact of AS on functioning and health. Ann Rheum Dis;69:102–07
Cieza A, Ewert T, Ustun TB, Chatterjee S, Kostanjsek N, Stucki G (2004) Development of ICF core sets for patients with chronic conditions. J Rehabil Med 44:9–11
Kiltz U, van der Heijde D, Boonen A et al (2015) Development of a health index in patients with ankylosing spondylitis (ASAS HI): final result of a global initiative based on the ICF guided by ASAS. Ann Rheum Dis 74:830–835
Cieza A, Geyh S, Chatterji S, Kostanjsek N, Ustun B, Stucki G (2005) ICF linking rules: an update based on lessons learned. J Rehabil Med 37:212–218
Fitch K, Bernstein SJ, Aguilar MD et al (2001) The RAND/UCLA appropriateness method user’s manual. RAND, Santa Monica, CA
Diaz_Torne C, Pou MA, Castellvi I, Corominas H, Taylor WJ (2014) Concerns of patients with gout are incompletely captured by OMERACT endorsed domains of measurement for chronic gout studies. J Clin Rheumatol 20:138–140
Lindsay K, Gow P, Vanderpyl J, Logo P, Dalbeth N (2011) The experience and impact of living with gout: a study of men with chronic gout using a qualitative grounded theory approach. J Clin Rheumatol 17:1–6
Acknowledgments
The authors gratefully acknowledge the health professionals who took part in the Delphi survey: Nicola Dalbeth, Lisa Stamp, Douglas White, Till Uhlig, Peter Gow, Michael Pillinger, Fernando Perez-Ruiz, Christian Mallen, Carlo Alberto Scire, Maureen Dubreuil, Yi-Hsing Chen, Lee S Simon, Puja Khanna, Cesar Diaz-Torne, Tuhina Neogi, Paul Doghramji, Naomi Schlesinger, John FitzGerald, Ruben Burgos-Vargas, Worawit Louthrenoo, Sjef van der Linden, Laura Durcan, Gail Kerr, Leslie Harrold, Arthur Kavanaugh, Mart A.F.J. van de Laar, Tim L Jansen, Herbert Baraf, Ric Day, Geraldo da Rocha Castelar Pinheiro, Philip Helliwell, Frédéric Lioté, Liz Davis, Tony Dowell, Annelies van Ede, Alexis Ogdie, Mike Corkill, Keith Rome, Maxim Eliseev, Alexander So, Marco A Cimmino, Jiunn-Horng Chen, Martijn Gerritsen, Anne-Kathrin Tausche, Janitzia Vazquez-Mellado, Rebecca Grainger, Merie Claridge, Lorenzo Cavagna, Ana Beatriz Vargas dos Santos, Robert Terkeltaub, Brian Mandell, Hisashi Yamanaka, Kuo-Lung Lai, Everardo Alvarez Hernandez, Eliseo Pascual, Annelies Boonen, Chingtsai Lin, N. Lawrence Edwards, Hugh de Lautour, Hsiao-Yi Lin, Zufferey Pascal, Bart Spaetgens, Helen Keen, Francisca Sivera, Maarten Boers, John Sundy, Hein Janssens, Philip Riches, Chih-Wei Tseng, Hsiao Yi Lin, Angelo Gaffo, Edward Roddy, Eugene Kissin Hang-Korng Ea, and Rieke Alten.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Sources of support
EMK and MJN were supported by scholarships awarded by Radboud University (SNUF-beurs) and the international office department of the Radboud Hospital (Radboudumc-studentenbudget).
Eveline M. Kool and Marieke J. Nijsten are joint first authors.
Rights and permissions
About this article
Cite this article
Kool, E.M., Nijsten, M.J., van Ede, A.E. et al. Discrepancies in how the impact of gout is assessed in outcomes research compared to how health professionals view the impact of gout, using the lens of the International Classification of Functioning, Health and Disability (ICF). Clin Rheumatol 35, 2259–2268 (2016). https://doi.org/10.1007/s10067-016-3325-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-016-3325-7