Abstract
Basel-Vanagaite-Smirin-Yosef syndrome (BVSYS) is an extremely rare autosomal recessive genetic disorder caused by variants in the MED25 gene. It is characterized by severe developmental delay and variable craniofacial, neurological, ocular, and cardiac anomalies. Since 2015, through whole exome sequencing, 20 patients have been described with common clinical features and biallelic variants in MED25, leading to a better definition of the phenotype associated with BVSYS. We report two young sisters, born to consanguineous parents, presenting with intellectual disability, neurological findings, and dysmorphic features typical of BVSYS, and also with bilateral perisylvian polymicrogyria. The younger sister died at the age of 1 year without autoptic examination. Whole exome sequencing detected a homozygous frameshift variant in the MED25 gene: NM_030973.3:c.1778_1779delAG, p.(Gln593Argfs). This report further delineates the most common clinical features of BVSYS and points to polymicrogyria as a distinctive neuroradiological feature of this syndrome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Basel-Vanagaite-Smirin-Yosef syndrome (MIM #616449) is an extremely rare autosomal recessive genetic disorder caused by variants in the MED25 gene on chromosome 19q13 (MIM *610197). This syndrome is characterized by severe developmental delay and variable craniofacial, neurological, ocular, and cardiac anomalies. It was first described in 2015 by Basel-Vanagaite et al. in 7 affected children from 4 unrelated families originating from an Israeli village [1] and by Figueiredo et al. in 7 affected adults from a consanguineous Brazilian family [2].
To date, only 20 patients have been described (Table 1) [1,2,3,4,5]. Almost all had severely delayed psychomotor development since infancy and were unable to speak or walk independently. Common dysmorphic facial features included high forehead, epicanthus, hypertelorism, sparse eyebrows, broad and overhanging nasal tip, short philtrum, exaggerated cupid’s bow, mandibular prognathia, sparse hair, high frontal hairline and nevus flammeus simplex of the forehead. Additional common features were 2–3 toe syndactyly, abnormal cardiac septum morphology, hypotonia, thin corpus callosum, ventriculomegaly, cerebral atrophy and seizures. In all patients, whole exome sequencing (WES) identified biallelic variants in the MED25 gene [1,2,3,4,5].
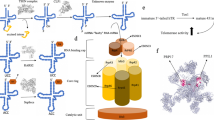
MED25 encodes a component of the Mediator complex, an evolutionarily conserved multi-protein complex that interacts with the RNAse polymerase II machinery and functions as a transcriptional co-regulator [6]. It has been proposed that distinct Mediator subunits, by relaying signals from different transcription factors in a preferential manner, may have gene- and tissue-specific roles [6]. The MED25 subunit is found only in higher eukaryotes and is highly expressed in dorsal root ganglia, cerebellum, cortex, and optic nerve, suggesting an important function in the nervous system [1].
We report two young sisters, born to consanguineous parents, presenting with typical dysmorphic features and neurological findings of BVSYS, and also with bilateral perisylvian polymicrogyria. Through WES, we identified a rare homozygous frameshift variant in MED25.
Materials and methods
WES (SureSelect Human All Exome V7) was performed on proband 1, her parents and healthy siblings through procedures and analysis pipelines we had reported previously [7]. The patients’ family provided written informed consent for genetic testing and publication of the results, including clinical details and photographs. All information was treated according to the European Regulations on personal data protection (EU 2016/679).
Results
Clinical phenotype and genetic findings
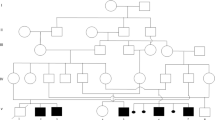
The probands are two sisters, the third and fourth child of healthy, consanguineous parents (first cousins once removed). They have an older brother and sister, both in good health. The mother has had two previous miscarriages.
Proband 1 was born at term by vaginal delivery at the 37th week, with a birth weight of 2370 g (5th–10th centile). Apgar scores were 10/10 at the 1st and 5th minute. She showed hypotonia, dysmorphic facial features, erratic eye movements, and feeding difficulties. She was hospitalized in a neonatal intensive care unit and fed by gavage for 1 month. Her psychomotor development was severely delayed: she gained head control at the age of 1 year and was able to sit unaided at 7 years. She had distinctive facial dysmorphisms: high forehead, epicanthus, strabismus, broad and overhanging nasal tip, short philtrum, downturned corners of the mouth, exaggerated cupid’s bow, micrognathia, and thick alveolar ridges (Fig. 1a, b, f–h). She also had bilateral tapered fingers, broad and hyperconvex nails (Fig. 1c.i), single transverse palmar crease in the right hand, Y-shaped bilateral 2–3 toe syndactyly (Fig. 1d, e, j), and scoliosis. Cardiac ultrasound revealed patent foramen ovale, while transfontanellar ultrasound detected bilateral ventriculomegaly and microcalcifications. Brain MRI showed bilateral perisylvian polymicrogyria, thin corpus callosum, temporal and parietal atrophy, cavum septum pellucidum and cavum vergae cysts, and dilated third and lateral ventricles (Fig. 2a–c). Since the first months of life, the patient has displayed myoclonic epilepsy, successfully controlled with antiepileptic drugs (topiramate, then oxcarbazepine in combination with lorazepam, and finally levetiracetam). Ophthalmologic examination revealed erratic eye movements, hyperpigmented fundus oculi and macular abnormalities; audiometry (BAEP) was normal. Metabolic investigations showed high levels of lactic and pyruvic acid. Skin and muscle biopsy did not reveal any significant result.
Pictures of proband 1 at the age of 4 months (a–e) and at the age of 7 years (f–j). Pictures of proband 2 at the age of 40 days (k–o). (a, b, f–h) Facial phenotype of proband 1 with high forehead, epicanthus, strabismus, broad and overhanging nasal tip, short philtrum, downturned corners of the mouth, exaggerated cupid’s bow, micrognathia, and thick alveolar ridges. (c, i) Hands of proband 1 showing tapered fingers, broad and hyperconvex nails. (d, e, j) Y-shaped 2–3 toe syndactyly in proband 1. (k, l) Facial phenotype of proband 2 with high forehead, downslanting palpebral fissures, epicanthus, broad and overhanging nasal tip, short philtrum, downturned corners of the mouth, micrognathia, and thick alveolar ridges. (m, n) Hands of proband 2 showing tapered fingers with ulnar deviation, camptodactyly of the 3rd–4th fingers, broad and hyperconvex nails. (o) Y-shaped 2–3 toe syndactyly in proband 2
Brain MRI of proband 1 performed at the age of 7 years (a–c). Brain MRI of proband 2 performed at the age of 2 weeks (d–f). a T1 midline sagittal view: Slightly thin, high-arched corpus callosum. b T2 axial FLAIR: perisylvian polymicrogyria, dilation of the lateral ventricles. c T2 coronal view: bilateral perisylvian polymicrogyria. d T1 midline sagittal view: Slightly thin corpus callosum. e T2 coronal view: perisylvian polymicrogyria. f T2 coronal view: perisylvian polymicrogyria
The patient showed a marked delay in growth, confirmed during the last examination at the age of 15 years and 3 months: her head circumference was 52 cm (10th–25th centile), her height was 140 cm (< 3rd centile), and her weight was 35 kg (< 3rd centile). She was unable to walk unaided and she had not yet developed bladder and bowel control. She exhibited vocalization without communicative purposes and could only speak a few words. Neurological evaluation revealed severe hypotonia with absent tendon reflexes and skeletal muscle atrophy, especially of the lower limbs. Indeed, electroneurography (ENoG) showed axonal motor polyneuropathy of the lower limbs. Electrophysiological analysis demonstrated a bilateral reduction of the compound muscle action potential of the common peroneal nerve, with normal motor-nerve conduction velocity.
Karyotype, 7-dehydrocholesterol, and FISH analysis for 4p- syndrome and array-CGH were normal.
On the other hand, WES revealed a homozygous frameshift variant in MED25 exon 16: NM_030973.3:c.1778_1779delAG, NP_112235.2:p.(Gln593Argfs), which was detected in a heterozygous state in her parents as well as in her healthy brother and sister (Online resource 1). This small deletion is extremely rare in gnomAD v.2.1.1, where only three heterozygotes (3/238374) and no homozygotes are reported. It has not been described in the literature, but it has been reported as a variant of uncertain significance and with unknown zygosity in two ClinVar database records (accession VCV000409952.1), associated with a suspected neuropathy [8]. This variant is predicted to cause a frameshift that alters the highly conserved and functionally important C-terminal portion of MED25 and that may also lead to transcript degradation by non-stop decay. According to the ACMG recommendations [9], we classified this variant as pathogenic.
Proband 2, the younger sister of the first patient, was born at term by cesarean section (prompted by abnormal cardiotocography results) with a weight of 3390 g (50th–75th centile). At birth, she showed hypotonia, abnormal limb and eye movements, and a cleft palate and was hospitalized in a neonatal intensive care unit for 1 month. She also presented with facial dysmorphisms: high forehead, downslanting palpebral fissures, epicanthus, broad and overhanging nasal tip, short philtrum, downturned corners of the mouth, micrognathia, and thick alveolar ridges (Fig. 1k, l). She had bilateral tapered fingers, ulnar deviation of the fingers, camptodactyly of 3rd–4th fingers, broad and hyperconvex nails, adducted thumb (Fig. 1m, n), single transverse palmar crease in the left hand, and bilateral Y-shaped 2–3 toe syndactyly (Fig. 1o). Her psychomotor development during the first year of life was severely delayed. Cardiac ultrasound revealed patent ductus arteriosus, while transfontanellar ultrasound detected bilateral ventriculomegaly. Brain MRI showed bilateral perisylvian polymicrogyria, thin corpus callosum, cavum septum pellucidum and cavum vergae cysts, and dilated third and lateral ventricles (Fig. 2d–f). Screening for metabolic and mitochondrial diseases was negative. The proband died at the age of 1 year and autoptic examination was not performed. Unfortunately, no DNA samples of this patient were available for analysis.
Discussion
In this report, we describe two sisters with severe developmental delay, hypotonia, cardiac defects, and distinctive facial and limb dysmorphisms commonly observed in BVSYS patients. WES revealed a MED25 homozygous frameshift variant in proband 1. Although we could not confirm the presence of the same variant in proband 2, we assumed bona fide that this would be the case considering the striking clinical overlap observed in the two sisters.
Biallelic changes in MED25 have been described in a total of 20 BVSYS patients [1,2,3,4,5]. With the exception of a compound heterozygote for a missense and a frameshift variant [5], all other individuals had homozygous missense changes. Variant p.(Tyr39Cys), located in the critical von Willebrand factor type A domain, was shown to impair the interaction of MED25 with the rest of the Mediator complex [1], suggesting loss of protein function as the underlying pathogenic mechanism. In support of this hypothesis, the homozygous frameshift variant identified in our patient affects the C-terminus and is expected to result in a disrupted protein product.
Brain imaging abnormalities were reported in at least 10 individuals affected by BVSYS (Table 1). As a whole, these features may be more common than previously recognized, especially if we take into account that several patients did not undergo brain imaging (e.g., the seven described by Figueiredo et al. [2]). Individually, there is a high degree of variability in the anomalies reported, although thin corpus callosum seems to be fairly recurrent. The neuroimaging findings in our probands recapitulate most of the features reported in other patients to date. Notably, both of our patients also showed bilateral perisylvian polymicrogyria. Through WES data analysis, we excluded other causal variants in genes known to be associated with this specific phenotype [10]. Considering that polymicrogyria has been reported in another patient with BVSYS recently [5], we suggest its inclusion among the brain anomalies of MED25-related disorders.
It should be mentioned that initially, in 2009, a homozygous missense variant in MED25 was associated with Charcot-Marie-Tooth disease (CMT) in a large Costa Rican family [11]. A subsequent study by the same authors ascribed the phenotype of the original family to a homozygous nonsense variant in the neighboring PNKP gene, in linkage disequilibrium with the MED25 variant [12]. Nevertheless, after the 2009 report, MED25 variants have occasionally been considered as a possible contributing factor in neuropathies [13]. The two ClinVar records for variant p.(Gln593Argfs) are probably set in this context, since they refer to a patient with a suspected CMT (SCV000550350.2) and a patient diagnosed with failure to thrive, hypotonia, and sensory ataxic neuropathy (SCV000854512.1) [8]. Strikingly, at the last examination, our first proband has manifested signs of peripheral neuropathy, which is likely progressive since a previous ENoG examination at the age of 5 years was normal. To the best of our abilities, we have excluded any involvement of PNKP or other neuropathy-related genes at both the clinical and the genetic (exome) level. Basel-Vanagaite et al. [1] also reported features suggestive of a neuropathy in patient 4 (pes cavus, contractures, hypotonia, decreased deep tendon reflexes), but the diagnosis was not confirmed by a specific neurophysiologic evaluation. Overall, further studies would be recommended to determine if neuropathy is an intrinsic and possibly progressive feature of MED25-related conditions.
In conclusion, our report further depicts the clinical phenotype of BVSYS and emphasizes the importance of a detailed neuroradiological evaluation of patients under this clinical suspicion.
Data availability
Data is available from the corresponding author upon reasonable request.
References
Basel-Vanagaite L, Smirin-Yosef P, Essakow JL, Tzur S, Lagovsky I, Maya I, Pasmanik-Chor M, Yeheskel A, Konen O, Orenstein N, Weisz Hubshman M, Drasinover V, Magal N, Peretz Amit G, Zalzstein Y, Zeharia A, Shohat M, Straussberg R, Monté D, Salmon-Divon M, Behar DM (2015) Homozygous MED25 mutation implicated in eye-intellectual disability syndrome. Hum Genet 134:577–587. https://doi.org/10.1007/s00439-015-1541-x
Figueiredo T, Melo US, Pessoa ALS, Nobrega PR, Kitajima JP, Correa I, Zatz M, Kok F, Santos S (2015) Homozygous missense mutation in MED25 segregates with syndromic intellectual disability in a large consanguineous family. J Med Genet 52:123–127. https://doi.org/10.1136/jmedgenet-2014-102793
Nair P, Lama M, El-Hayek S, Sleymane GA, Stora S, Obeid M, Al-Ali MT, Delague V, Mégarbané A (2018) COQ8A and MED25 mutations in a child with intellectual disability, microcephaly, seizures and spastic ataxia: synergistic effect of digenic variants? Mol Syndromol 9:319–323. https://doi.org/10.1159/000494465
Nair P, Sabbagh S, Bizzari S, Brunner F, Stora S, Al-Ali MT, Gencik M, El-Hayek S, Mégarbané A (2019) Report of a second Lebanese family with Basel-Vanagaite-Smirin-Yosef syndrome: possible founder mutation? Mol Syndromol 10:219–222. https://doi.org/10.1159/000501114
Haynes D, Pollack L, Prasad C, Goobie S, Colaiacovo S, Wolfinger T, Lacassie Y (2020) Further delineation of Basel-Vanagaite-Smirin-Yosef syndrome: report of three patients. Am J Med Genet Part A 182:1785–1790. https://doi.org/10.1002/ajmg.a.61603
Malik S, Roeder RG (2010) The metazoan Mediator co-activator complex as an integrative hub for transcriptional regulation. Nat Rev Genet 11:761–772. https://doi.org/10.1038/nrg2901
Errichiello E, Mustafa N, Vetro A, Notarangelo LD, de Jonge H, Rinaldi B, Vergani D, Giglio SR, Morbini P, Zuffardi O (2017) SMARCA4 inactivating mutations cause concomitant Coffin-Siris syndrome, microphthalmia and small-cell carcinoma of the ovary hypercalcaemic type. J Pathol 243:9–15. https://doi.org/10.1002/path.4926
National Center for Biotechnology Information. ClinVar; [VCV000409952.1], https://www.ncbi.nlm.nih.gov/clinvar/variation/VCV000409952.1 (accessed July 6, 2020)
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17:405–424. https://doi.org/10.1038/gim.2015.30
Stutterd CA, Leventer RJ (2014) Polymicrogyria: a common and heterogeneous malformation of cortical development. Am J Med Genet Part C 166C:227–239. https://doi.org/10.1002/ajmg.c.31399
Leal A, Huehne K, Bauer F, Sticht H, Berger P, Suter U, Morera B, del Valle G, Lupski JR, Ekici A, Pasutto F, Endele S, Barrantes R, Berghoff C, Berghoff M, Neundörfer B, Heuss D, Dorn T, Young P, Santolin L, Uhlmann T, Meisterernst M, Sereda MW, Sereda M, Stassart RM, Meyer zu Horste G, Nave KA, Reis A, Rautenstrauss B (2009) Identification of the variant Ala335Val of MED25 as responsible for CMT2B2: molecular data, functional studies of the SH3 recognition motif and correlation between wild-type MED25 and PMP22 RNA levels in CMT1A animal models. Neurogenetics 10:275–287. https://doi.org/10.1007/s10048-009-0183-3
Leal A, Bogantes-Ledezma S, Ekici AB, Uebe S, Thiel CT, Sticht H, Berghoff M, Berghoff C, Morera B, Meisterernst M, Reis A (2018) The polynucleotide kinase 3′-phosphatase gene (PNKP) is involved in Charcot-Marie-tooth disease (CMT2B2) previously related to MED25. Neurogenetics 19:215–225. https://doi.org/10.1007/s10048-018-0555-7
Gonzaga-Jauregui C, Harel T, Gambin T, Kousi M, Griffin LB, Francescatto L, Ozes B, Karaca E, Jhangiani SN, Bainbridge MN, Lawson KS, Pehlivan D, Okamoto Y, Withers M, Mancias P, Slavotinek A, Reitnauer PJ, Goksungur MT, Shy M, Crawford TO, Koenig M, Willer J, Flores BN, Pediaditrakis I, Us O, Wiszniewski W, Parman Y, Antonellis A, Muzny DM, Baylor-Hopkins Center for Mendelian Genomics, Katsanis N, Battaloglu E, Boerwinkle E, Gibbs RA, Lupski JR (2015) Exome sequence analysis suggests that genetic burden contributes to phenotypic variability and complex neuropathy. Cell Rep 12:1169–1183. https://doi.org/10.1016/j.celrep.2015.07.023
Acknowledgments
The authors wish to thank the patients’ family members for their cooperation in providing the medical data and photographs necessary for this publication, as well as the photographers Marco Bonazzi and Luca Valcavi.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Informed consent was obtained from the patients’ parents.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(pptx 186 kb)
Rights and permissions
About this article
Cite this article
Maini, I., Errichiello, E., Caraffi, S.G. et al. Improving the phenotype description of Basel-Vanagaite-Smirin-Yosef syndrome, MED25-related: polymicrogyria as a distinctive neuroradiological finding. Neurogenetics 22, 19–25 (2021). https://doi.org/10.1007/s10048-020-00625-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10048-020-00625-2