Abstract
This study proposes novel optimized stem geometry with low stress values in the cement using a finite element (FE) analysis combined with an optimization procedure and experimental measurements of cement stress in vitro. We first optimized an existing stem geometry using a three-dimensional FE analysis combined with a shape optimization technique. One of the most important factors in the cemented stem design is to reduce stress in the cement. Hence, in the optimization study, we minimized the largest tensile principal stress in the cement mantle under a physiological loading condition by changing the stem geometry. As the next step, the optimized stem and the existing stem were manufactured to validate the usefulness of the numerical models and the results of the optimization in vitro. In the experimental study, strain gauges were embedded in the cement mantle to measure the strain in the cement mantle adjacent to the stems. The overall trend of the experimental study was in good agreement with the results of the numerical study, and we were able to reduce the largest stress by more than 50 % in both shape optimization and strain gauge measurements. Thus, we could validate the usefulness of the numerical models and the results of the optimization using the experimental models. The optimization employed in this study is a useful approach for developing new stem designs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although improvements in the techniques for cementing and prosthetic design have reduced the incidence of complications of a cemented stem, the average 10-year crude survival rate for total hip arthroplasty (THA) was 92.5 % from 1992 to 2003. Revision was the dominant subsequent procedure, accounting for 86 % of all reoperations. Among the revisions, aseptic loosening is the primary cause, accounting for 73.9 % [1]. Although the loosening of a hip prosthesis is due to a combination of mechanical and biological factors, a body of fractographic study revealed that fatigue cracking of the cement mantle is the primary cement failure mechanism that directly contributes to such loosening. Evidence from microscopic studies has been added that in vitro tests and retrieved specimens showed similar fatigue failure pattern each other [2].
Finite element (FE) analysis has been previously employed to study the mechanical consequences of cement failure as well as interface debondings on the load transfer characteristics of the cemented stem [3, 4]. However, one of the prerequisites of FE analyses is that they have to be validated by experimental measurements independently. Stolk et al. [5] compared the results from strain gauge measurements to those of FE analyses and developed a pre-clinical test to assess the two existing stem designs against cement fracture. Other studies have also validated FE analyses by measuring cement strain values [6, 7] by stem subsidence values [8, 9] and by strain values on the cortical bone with cemented THA. Although their procedures are useful for highlighting differences in stress patterns around different stems, the methods did not include a new ideal stem design.
A shape optimization technique integrated with FE analysis is a useful method to develop an optimal prosthesis design that improves long-term clinical outcomes as well as functional performance [10, 11]. Accordingly, a common shape optimization object of a cemented stem incorporates a measure of the stress in the cement mantle surrounding the prosthesis or the stem–cement interface with the goal of minimizing the stress in these areas [12–14]. Although these optimization analyses must also be validated experimentally, no analytical study with cemented THA has been validated using experimental models. Hence, we cannot know whether a stem with an ideal geometry developed by FE analysis combined with an optimization procedure actually reduces cement stress.
The objectives of this study were to establish a procedure for developing the stem design, develop an optimum stem geometry, and to validate the usefulness of the numerical models measuring cement strain directly. This technique would be beneficial as part of a preclinical evaluation of the cemented stem in understanding the mechanical consequences of cement fracture in their cement mantle.
Materials and methods
Our study was divided into two parts. A global scheme for the study procedure is shown in Fig. 1. First, we investigated the optimum stem geometry and the cement mantle thickness numerically. In this calculation, we used an adaptive p-method FE analysis together with three-dimensional computer-aided design (CAD) software for shape optimization (Pro/ENGINEER, Pro/MECHANICA 20.0; Parametric Technology Corp., Waltham, MA, USA), which enabled us to use a parametric based CAD model for an analytical model. Second, to validate the FE analyses, strain in the cement mantle adjacent to the basic and the optimum stem was measured directly.
Numerical study
In this numerical study, we used the standardized bone model data, whose geometry corresponds to the composite femur, and is typical of cadaveric specimens [5]. As a basic model, we made a stem similar to the existing Harris Precoat stem (ZIMMER, Warsaw, IN, USA). The stem had a collar, a 38-mm head offset, a length of 140 mm from the collar to the tip of the stem, and the tip had a hemispheric profile. In the basic model, the cement was assumed to be of 2.0 mm constant thickness, and it was constructed 30 mm below the tip of the stem. The three-dimensional FE model was composed of 1,341 hexahedral and wedge-shaped p-elements (Fig. 2). Polynomial orders of the p-elements start from 3 and increase to 9 at the most. To compare the results of numerical studies with those of experimental studies, we selected the planar loading case that could be reproduced by the experimental model. We simulated the simplified heel-strike loading case, which has been used in several studies [5, 7]. The stem head load of 2.47 body weight (BW) was compressive and applied at 28° lateral to the femur long axis in the coronal plane. The greater trochanter load of 1.55 BW was tensile and applied at 40° medial to the femur long axis in the coronal plane. A body weight of 800 N was used. The distal end of the diaphysis was fully constrained. All materials were modeled as homogeneous, isotropic, and linear elastic. The elastic moduli for the cortical and cancellous bone were taken to be 12.4 GPa and 104 MPa, respectively. Although these values might be lower than those used in other studies, the values were the same as those of the composite femur and were derived from the manufacturers’ data. The cobalt-chrome stem was assigned an elastic modulus of 210 GPa, and that of the bone cement was 2.2 GPa. The Poisson ratio for all materials was 0.3. The stem–cement and cement–bone interfaces were assumed to be completely bonded.
A shape optimization problem is formulated as a minimization problem, as follows:
Minimize: \( F\left( D \right) \)
within the design space: \( d_{i}^{L} \le d_{i} \le d_{i}^{U} i = 1, 6\)
where \( D = \left\{ {d_{1} , d_{2} , \ldots d_{6} } \right\} \) is the vector of design parameters, \( d_{i}^{L} , d_{i}^{U} \) are the lower and upper limits of design parameters that are shown in Table 1, and the study object was to minimize the largest tensile principal stress F(D) in the cement mantle. Tensile principal stress was used because bone cement is a brittle material [15]. As the design parameters, we used the cross-sectional geometries of the stem, keeping other stem geometries (stem length, calcar curvature, neck angle, etc.) as constant. A suitable interpolation of each section is used to describe the entire stem geometry. An outer geometry of the cement mantle and a femoral geometry were also kept constant. Consequently, the cement mantle thickness was varied inversely with the stem size. Design parameters investigated in this study were the medial–lateral and the anterior–posterior width at three axial levels (Fig. 3 left and Table 1). A general class of the quasi-Newton method was used for the search direction. The optimization iterations were terminated at a convergence criterion, which is when errors in the norm of the stress are less than 5 %.
Left drawing shows design parameters selected in the optimization. The locations of the strain gauges are also shown as eight thick lines. A dotted line represents the outer geometry of the cement mantle. And representative strain gauge-instrumented basic stem, ready to be implanted into a composite femur is shown in right picture. Four strain gauges mounted on a thin layer of acrylic cement can be seen on the medial side of the stem. As for the medial side, four strain gauges are mounted on the lateral side
Experimental study
Ten composite femora (Model 3306; Pacific Research Labs, Vashon Islands, WA, USA) were used to compare the strains in the cement around the basic and optimum stems. It was reported that synthetic models that replicate the healthy adult’s human mechanical properties have less inter-specimen variability and are easy to handle; thus the femur model appears to be a suitable alternative to cadaveric specimens, especially for comparative analyses [5]. We manufactured a basic stem as a control model and an optimum stem calculated from the shape optimization by converting the CAD data to computer-aided manufacturing (CAM) data. These stems, which were made of cobalt-chrome, had a surface roughness (Ra = 2.0 μm) similar to the existing Harris Precoat design, although precoating was not used. To measure the strain in the cement mantle, six uniaxial strain gauges (QFLA-1-11; Tokyo Sokki Kenkyujo Co., Ltd., Tokyo, Japan) were embedded in the medial and lateral cement mantle at three levels at the stem, parallel to the stem surfaces. We also placed an additional two strain gauges near the tip of the stem, parallel to the longitudinal axis of the stem, because the largest stress was calculated near the tip of the stem in the FE analyses (Fig. 4). Instrumentation of each stem was accomplished by many steps. First, the stems were partially coated with a 0.3-mm layer of acrylic bone cement (Simplex P; Howmedica, Rutherford, NJ, USA), which was made using an oversized cast. The oversized cast was made by a combined impression using two layers of dental resins (LAB SILICONE, Matsukaze Corp., Kyoto, Japan) (TOSHICON PASTEL, Sankin Kogyo K., Tochigi, Japan) around a stem after adhering 0.3 mm thick wax (GC Sheet Wax; GC Co., Tokyo, Japan). After the 0.3-mm thick layers of the bone cement were completed, strain gauges were embedded on the cement layers (Fig. 3 right). After all strain gauges were embedded, wires were bound and placed on the anterior or posterior surfaces of the stem to avoid the areas where strain gauges were located.
Five instrumented basic stems and five instrumented optimum stems were implanted into the composite femora using a standard surgical technique performed by an experienced surgeon. Since we did not change the outer geometry of the cement mantle in the numerical study, the same rasp was used for preparing the insertion of both the basic and optimum stems. The correct stem positioning in implanted femora was verified on radiographs. The strain gauges were connected to a data acquisition unit (Remote Scanner Jr; Nippon Avionics Co., Ltd., Tokyo, Japan), and the data were transmitted to a personal computer. After preparation, femora were fixed distally at 11° of adduction. The load was applied using a cantilever system, which was similar to that used in other experimental studies [7, 8], and the cement strains were measured. A vertical force of 800 N was applied to the cantilever using a material testing machine (AUTOGRAPH AG-250kNE; Shimazu, Kyoto, Japan). This set up simulated the simplified heel-strike loading, including the hip-joint contact force and the abductor force, which was consistent with the numerical study.
Three repeated measurements were taken for each specimen, and the strains were averaged over these repetitions. Measured and predicted cement stresses were compared for the strain gauge outputs and the corresponding positions in the FE model. Measurements were compared between specimens, and outliers were detected based on the criterion of Chauvenet [16]. Outliers were detected for two strain gauges in the basic stems and for two strain gauges in the optimum stems out of the 80 total strain gauges. Moreover, two optimum reconstructions contained three strain gauges that did not function after insertion of the stems. For the remaining data, the mean stresses and the standard deviations between the specimens were determined.
Results
Numerical study
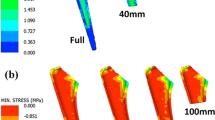
In the basic model, the largest tensile principal stress in the cement mantle was 5.48 MPa near the tip of the stem (Fig. 4). Another high stress of 2.58 MPa was observed at the proximal part of the stem.
The optimum stem geometry was calculated by decreasing the medial–lateral width at the distal and middle levels (d1, d3) together with increasing the medial–lateral and anterior–posterior width at proximal levels (d5, d6), but the anterior–posterior width at the distal and middle levels (d2, d4) were almost the same as default values (d 0 i ) (Table 1).
In the optimum model, the largest stress of 2.47 MPa was observed (Fig. 4). Hence, in the numerical study, the largest tensile principal stress in the cement mantle was reduced by almost 55 % by changing the stem geometry and the cement mantle thickness. Considering the fatigue limit of the bone cement in tensile (=6.7 MPa [2]), this reduction increases the safety factor from 1.22 to 2.71.
Experimental study
Compressive axial strains were measured on the medial side while the axial strains on the lateral side were tensile. The highest axial strains were measured in the cement mantle near the tip of the stem.
Comparisons between the results of the numerical study and those of the experimental study are shown in Fig. 5. We got axial stress values from axial strains and the elastic modulus of the bone cement. The results of the numerical studies over-predicted the magnitude of the stresses determined experimentally near the tip of the stem. Since the strain gauges were positioned at this level to measure the large strain calculated in the FE analyses, even a slight deviation in the positioning of the experimental models could contribute to large standard deviations and less experimental strains compared with the calculated strains. In the experimental study, the largest axial stress measured in the cement mantle was reduced by almost 51 % with the optimum stem.
Discussion
A new stem design and a procedure for developing a new stem design were developed, and the numerical models were validated by measuring cement strain directly. The present study was an initial attempt to validate the numerical results of the optimization of cemented prosthesis by experimental models. Based on the results of this study, a hybrid THA system was developed named “4-U” (Nakashima Medical CO., LTD., Okayama, Japan). A good mid-term clinical result was reported using the 4-U system [17].
In the numerical study, we used the standardized bone geometry, whose geometry is typical of cadaveric specimens [5], and we used an adaptive p-method FE analysis tightly integrated to a three-dimensional parameterized CAD software program for optimization, which enabled us to use an almost real geometry model in the numerical study. Several numerical studies have attempted to quantitatively assess the effect of implant shape and cement mantle thickness on cement stress. The distal cement stress was higher for larger stem cross sections that fit into the distal part of the canal more tightly, leaving less room for the cement mantle [18]. Clinical studies also reported that failure of the stem occurred when the cement mantle in Gruen zones 5 and/or 6 was too thin [19]. Hence, there is a fairly general agreement that small cross-sectional area with thick cement mantle at the distal level of the stem is preferable. These reports are in agreement with our results regarding the medial–lateral stem width and the cement mantle thickness at the middle and distal levels. According to anterior–posterior stem width, however, we do not recommend small size in this direction at the distal level, although the optimum dimension (d2) was slightly smaller than the initial value. This concept of the stem geometry was first described in our previous report [14]. Contrarily to the distal level, many numerical and experimental studies reported that by increasing the cross-sectional size of the stem, decreasing the cement thickness at the proximal level decreased the cement stress [4, 20]. These results are in agreement with those of our study regarding the medial–lateral and the anterior–posterior stem width and the cement mantle thickness at the proximal level. From what has been said, we surmise that the optimum cement mantle is not of uniform thickness. Some researchers also have the same opinion [21, 22]. Even if any argument remains regarding its optimum thickness, direct measurements of the cement mantle revealed that the thicknesses actually were not constant at each Gruen zone [23]. Our numerical study indicates that under conditions simulating a single-legged stance, the cement stress decreased by the optimum stem geometry with a non-uniform thickness of the cement mantle.
We should acknowledge some limitations of this study. First, we used only one planar loading case. We selected the loading case because it could be reproduced by the experimental model, and one of the objectives was to validate the usefulness of the numerical models and the results of the optimization using the experimental models. The second limitation is that we selected one stem design (Harris Precoat) for a basic stem. Selection of other stem designs might lead to a different optimum stem geometry and cement mantle thickness. The third limitation is related to the interface conditions. Although the use of the frictional interface would give more information, we assumed the interfaces to be bonded.
Conclusions
This study demonstrated the optimum stem geometry with smaller cement stress, a procedure for optimum stem design and a validation study of the numerical models by measuring cement strain directly. The overall trend of the experimental study is in good agreement with the numerical study. Although the standard deviation of the experimental results is large near the tip of the stem, we were able to reduce the cement stresses by more than 50 % in both the numerical and experimental studies. Thus, we could validate the usefulness of numerical models and the results of optimization using experimental models. The optimization employed in this study is a useful approach for developing new stem designs.
References
Malchau H, Garellick G, Eisler T, Karrholm J, Herberts P. Presidential guest address: the Swedish Hip Registry: increasing the sensitivity by patient outcome data. Clin Orthop Relat Res. 2005;441:19–29.
Lewis G. Fatigue testing and performance of acrylic bone-cement materials: state-of-the-art review. J Biomed Mater Res B Appl Biomater. 2003;66:457–86.
Lennon AB, Britton JR, MacNiocaill RF, Byrne DP, Kenny PJ, Prendergast PJ. Predicting revision risk for aseptic loosening of femoral components in total hip arthroplasty in individual patients–a finite element study. J Orthop Res : Off Public Orthop Res Soc. 2007;25:779–88.
Janssen D, van Aken J, Scheerlinck T, Verdonschot N. Finite element analysis of the effect of cementing concepts on implant stability and cement fatigue failure. Acta Orthop. 2009;80:319–24.
Stolk J, Verdonschot N, Cristofolini L, Toni A, Huiskes R. Finite element and experimental models of cemented hip joint reconstructions can produce similar bone and cement strains in pre-clinical tests. J Biomech. 2002;35:499–510.
Harrigan TP, Kareh JA, O’Connor DO, Burke DW, Harris WH. A finite element study of the initiation of failure of fixation in cemented femoral total hip components. J Orthop Res: Off Public Orthop Res Soc. 1992;10:134–44.
Waide V, Cristofolini L, Stolk J, Verdonschot N, Boogaard GJ, Toni A. Modelling the fibrous tissue layer in cemented hip replacements: experimental and finite element methods. J Biomech. 2004;37:13–26.
Jeffers JR, Browne M, Lennon AB, Prendergast PJ, Taylor M. Cement mantle fatigue failure in total hip replacement: experimental and computational testing. J Biomech. 2007;40:1525–33.
Waanders D, Janssen D, Berahmani S, Miller MA, Mann KA, Verdonschot N. Interface micromechanics of transverse sections from retrieved cemented hip reconstructions: an experimental and finite element comparison. J Mater Sci Mater Med. 2012;23:2023–35.
Sabatini AL, Goswami T. Hip implants VII: finite element analysis and optimization of cross-sections. Mater Des. 2008;29:1438–46.
Ruben RB, Folgado J, Fernandes PR. Three-dimensional shape optimization of hip prostheses using a multicriteria formulation. Struct Multidiscip Opt. 2007;34:261–75.
Ishida T, Nishimura I, Tanino H, Higa M, Ito H, Mitamura Y. Use of a genetic algorithm for multiobjective design optimization of the femoral stem of a cemented total hip arthroplasty. Artif Organs. 2011;35:404–10.
Katoozian H, Davy DT. Effects of loading conditions and objective function on three-dimensional shape optimization of femoral components of hip endoprostheses. Med Eng Phys. 2000;22:243–51.
Tanino H, Ito H, Higa M, Omizu N, Nishimura I, Matsuda K, et al. Three-dimensional computer-aided design based design sensitivity analysis and shape optimization of the stem using adaptive p-method. J Biomech. 2006;39:1948–53.
Stolk J, Verdonschot N, Murphy BP, Prendergast PJ, Huiskes R. Finite element simulation of anisotropic damage accumulation and creep in acrylic bone cement. Eng Fract Mech. 2004;71:513–28.
Dally JW, Riley WF. Experimental stress analysis. New York: McGraw-Hill; 1965.
Ito H, Tanino H, Yamanaka Y, Nakamura T, Matsuno T. Hybrid total hip arthroplasty using specifically-designed stems for patients with developmental dysplasia of the hip. A minimum five-year follow-up study. Int Orthop. 2011;35:1289–94.
Hertzler J, Miller MA, Mann KA. Fatigue crack growth rate does not depend on mantle thickness: an idealized cemented stem construct under torsional loading. J Orthop Res: Off Public Orthop Res Soc. 2002;20:676–82.
Kawate K, Ohmura T, Nakajima H, Takakura Y. Distal cement mantle thickness with a triangular distal centralizer inserted into the stem tip in cemented total hip arthroplasty. J Arthroplast. 2001;16:998–1003.
Cristofolini L, Erani P, Bialoblocka-Juszczyk E, Ohashi H, Iida S, Minato I, et al. Effect of undersizing on the long-term stability of the Exeter hip stem: a comparative in vitro study. Clin Biomech. 2010;25:899–908.
Berli BJ, Schafer D, Morscher EW. Ten-year survival of the MS-30 matt-surfaced cemented stem. J Bone Joint Surg Br. 2005;87:928–33.
Maloney WJ, Jasty M, Burke DW, O’Connor DO, Zalenski EB, Bragdon C, et al. Biomechanical and histologic investigation of cemented total hip arthroplasties. A study of autopsy-retrieved femurs after in vivo cycling. Clin Orthop Related Res. 1989:129–40.
Gunn E, Gundapaneni D, Goswami T. Effect of cement fill ratio in loosening of hip implants. Biomatter. 2012;2:87–93.
Conflict of interest
The authors have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Higa, M., Tanino, H., Nishimura, I. et al. Three-dimensional shape optimization of a cemented hip stem and experimental validations. J Artif Organs 18, 79–85 (2015). https://doi.org/10.1007/s10047-014-0792-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-014-0792-y