Abstract
Background
When evaluating patients’ profile, surgeons usually note the lack of the chin projection and may suggest chin augmentation, but they rarely discuss reduction of an over-projecting chin. This is unfortunate, since there are quite many individuals who have macrogenia and would aesthetically benefit from corrective surgery, but the chin reduction is seldom offered. The reason for this is the lack of experience, lack of the technical equipment necessary, or sometimes lack of knowledge. The present study conveys 25 years of experience with the reduction genioplasty.
Methods
From 1994 to 2019, 47 patients (39 females, 6 males, and 2 male to female transsexuals) underwent 49 chin reduction procedures. All patients were operated and followed up by the author. The transoral approach was used in 23 patients, and in 24 patients the procedure was done through the straight 4- to 6-cm-long submental incision. The air-driven pneumatic chisel was employed for reduction of the mandibular bone (MicroAire, Charlottesville, VA, USA). Forty-eight operations were carried out under dissociative and local anaesthesia on an outpatient basis, and one procedure was done under general endotracheal anaesthesia.
Results
Both mandibular bone and the soft tissues of the chin were reduced, or modulated according to the needs of each patient. Operations were technically easier when executed by the submental approach because of better exposure of the mandibular rim and the higher precision in the remodelling of the soft tissues. Thirty-six patients (77%) could be followed up for a mean of 2.5 years (range 9 months to 12 years). Twenty-eight of evaluated patients (78%) described the outcome as very good or good. Four patients described the result as acceptable and another 4 as bad. In the majority of cases the evaluation by the surgeon correlated well with the opinion of patients, but in five cases surgeon estimated result with the higher score than the patient. Overall good results were illustrated by the photographs of the clinical examples. Complications were few and manageable. Transient neuropathies were common and more frequent with the transoral approach. Five patients required minor intervention for skin indentations at the jaw line developed during the healing phase.
Conclusions
Skilful chin reduction surgery is safe and the aesthetic improvement could be quite spectacular, which is also rewarding for the patients. Complications in this patient series were few and manageable. More surgeons should include chin reduction in their repertoire.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
God has given you one face, and you make yourself another.
William Shakespeare
Introduction
Similar to the nose, chin shape has great variability, but unlike the nose, chin diversity often goes unnoticed. This is probably because the chin does not carry the emotional importance of the nose. Until recently, surgeons evaluating a patient’s profile usually noted the chin projection but rarely delved deeper. Occasionally chin augmentation was offered, and this procedure has become quite popular [1]. The American Society of Plastic Surgeons (ASPS) reported in 2012 that “chin implants” were fastest growing procedure in the USA, with a 71% increase vs. year 2010, totalling 20,680 procedures [2].
Chin plays an important role in our perception of the proper facial proportions. The main determinants of chin harmony are its projection and vertical length. Chin might be excessively large and the condition is called macrogenia. Enlargement could be in the horizontal or vertical plane, or as a combination of both. Both mandibular bone shape and the overlying soft tissues are components defining chin appearance.
Quick assessment of the chin position in the facial profile could be made by drawing Riedel’s line, also called facial harmony line [3, 4]. This line connects the most prominent points of the upper and lower lip with the chin point above the pogonion (Fig. 1) and helps to determine the optimal projection of the chin. If the chin point is 3 mm or more anterior to the perpendicular plane, it suggests macrogenia in anterio-posterior direction. The exaggerated opposite position or posterior tilt indicates microgenia.
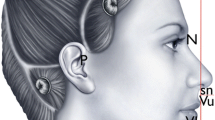
Assessment of the vertical dimension of the chin is made by the analysis of the both frontal and lateral views. The face is divided into three segments separated by the horizontal lines at the level of eyebrows and subnasale (Fig. 2). In the ideally harmonious face, the height of the all segments is approximately equal.
The lower segment is further subdivided by the line passing through the stomion. The distance from the stomion to the chin point should be twice the length of the distance between the stomion and subnasale [4]. These proportions are sometimes disrupted by the excessively long chin, which might require shortening of its vertical length.
In Asia the square-shaped or wide moon-shaped face is considered not attractive. Particularly the young Asian females desire more narrow and oval, or almond-shaped face. The mandibular contouring surgery including ramus, body, and the symphysis became in the countries like South Korea, Taiwan, or Japan one of the more frequently performed aesthetic procedures [5, 6].
Reduction genioplasty is not a routine procedure in the Western world. In Sweden patients with true prognathism and associated macrogenia are treated at the departments of oral surgery within the National Health Service. They are usually offered mandibular setback surgery and orthodontic correction of the dental occlusion. However, many individuals with macrogenia and normal occlusion would aesthetically benefit from the corrective surgery, but in contrast to augmentation, chin reduction is seldom offered. The reason for this is a lack of experience and necessary technical equipment, and sometimes knowledge. Patients repeatedly told me how difficult it was to find someone experienced with this procedure, and 20 of them travelled the long way to our clinic. When the technique was presented at the meetings in Europe, there were a very few colleagues who ever did such operation.
The aim of this study is to share my 25 years of experience with the chin reduction procedure, and to compare intraoral and submental approaches proposing indications and selection criteria for each of them. Concomitant ancillary procedures and the details of post-operative care will be described.
Material and method
A total of 47 patients (39 females, 6 males, and 2 male to female transsexuals) underwent 49 chin reduction procedures from 1994 to 2019. Six patients were initially operated elsewhere, two of them twice. Thirty-two patients were of European origin (Caucasians) and 15 patients had Middle-Eastern roots. The mean patient age was 25.4 years (range 18 to 61 years, median 26 years). One 61-year-old woman had chin reduction as a part of the face-lift procedure.
During the initial consultation every patient was provided with thorough informative material and was informed about available surgical alternatives. Each operation was designed individually after an analysis of chin morphology, including the soft tissue components, osseous component, and weighing in patient’s desires. The following anatomic features of the chin region were assessed: mandibular shape, chin protrusion in the sagittal plane, vertical length of the chin, the mentalis muscle, the soft tissue chin pad, the labiomental fold, and tilt or lack of tilt of the lower lip. The relationship between the chin and nose and the thickness of the soft tissue in the chin pad were evaluated [7,8,9,10,11].
Standardized photographs were taken of both the frontal and lateral views during the initial consultation and later hung in the operating room during the procedure. Pre-operative radiographs of the frontal and lateral views were obtained if they were warranted by the complexity of the case, which unfortunately not always was possible. Operation planning was aided by the AlterImage picture simulation program (Seattle Software Design, Seattle, WA, USA). Work-up included a dental examination to rule out the presence of caries, paradontosis, gingivitis, or other oral cavity pathology, which all were contraindications for surgery. Dental occlusion was normal or acceptable in all cases.
All patients were operated on and followed up by the author. Each patient was interviewed either during the visit or by the phone, using a standardized questionnaire containing the following topics: general satisfaction with the outcome, smoothness of the chin contour, disturbances in sensation, chewing function, or lip movements, and the quality of the scar. General satisfaction was graded on a modified Likert scale (1—poor; 2—acceptable; 3—good; 4—very good).
Twenty-seven patients lived within 200-km distance, 14 patients lived in the more remote regions of the country, and five patients lived abroad. Thirty one patients could be followed up at the clinic after 1 year or longer after operation. Five patients were followed up by the telephone interview and they returned the questionnaire by mail. One patient died and 10 did not respond, or were not available.
Surgical technique
Forty-eight operations were carried out under dissociative and local anaesthesia [12] on an outpatient basis and one procedure was done under general endotracheal anaesthesia. The mental region was anaesthetized using mental nerve and accessory mental nerve blocks and infiltrative anaesthesia with 20 to 30 ml of 1% Xylocaine with 5 μg of adrenaline/ml (AstraZeneca, London, UK). Headlight and protective facial shields were used during surgery.
Following algorithm is proposed for selecting intraoral or submental incision in the patients seeking correction of macrogenia. The transoral approach (23 procedures) was chosen for patients requiring minor or moderate chin reduction, usually younger women, but also other patients where the absence of the visible scar was most desirable and there was no indication for the auxiliary manoeuvres on the neck. Submental incision (24 procedures) was used when there was an indication for the additional surgery on the neck, like liposuction, reduction of the skin excess, and plathysma muscle plication, when the scar from the previous trauma was present and in the secondary surgery, or for the patients with the more severe mandibular hypertrophy.
At the transoral operation an incision was made in the labial sulcus from canine to canine tooth, leaving a 3- to 4-mm cuff of gingiva for later approximation [13]. Adequate soft tissue dissection, and sometimes resection, trimming, or repositioning of the soft tissue pad and/or mentalis muscles, was followed by periosteal elevation, usually from the level of first bicuspid to first bicuspid. Parts of the mentalis muscles were frequently trimmed and resected along with the fibro-fatty chin pad. Remaining mentalis muscles were reattached with the non-resorbable sutures to the pogonion [14], and PDS sutures rearranged the diminished chin pad. This prevents development of the chin ptosis. Filaments of the mental nerve are sometimes seen at the lateral extensions of the incision, and they must be handled with the gentle care.
At the submental approach the operating field was reached through the straight 4- to 6-cm long incision. Mental nerves are farther away from the dissected space and probability of the neurologic disturbance is much smaller as compared with the transoral operation, bleeding is less intensive, the visibility is better, and the precision of assessment of the degree of bone and soft tissue reduction is higher.
The resection volume was determined as described above in the “Material and method” section. By reducing and/or altering one half of the chin first, the degree of obtained reduction could be assessed and measured with the calliper at the created step in the midline of the mandible. The widest possible skin ellipse that would not leave dog ears was excised and liposuction on the neck and/or platysma tightening carried out if indicated. Two patients with very important macrogenia underwent chin reduction in two stages, first by the transoral approach and later by the submental approach.
The air-driven pneumatic reciprocating chisel (MicroAire, Charlottesville, VA, USA) was employed for reduction of the mandibular bone, removing bone chip by chip, the method called “bone shaving” [8] (Fig. 3). The operative field was flushed with cloxacillin solution (Ekvacillin, AstraZeneca). Vicryl rapide, or PDS (Ethicon, Hamburg-Norderstedt, Germany) sutures were used for the soft tissue and mucosal closure due to adequate duration strength. Densely placed sutures created a “watertight” closure, preventing contamination of the spongious bone surface with microorganisms from the oral cavity.
Pneumatic air-driven chisel at work. (Left) When a submental incision is used, the widest possible skin and subcutis ellipse that will not leave dog ears is excised and bone chips are removed. Bone chips with a smooth surface, resected skin and the fibro-fatty chin pad with the adjacent parts of the mentalis muscles
A compressive dressing was made by applying Microfoam (3 M, St. Paul, MN, USA) for 3 days and an elastic chin support garment for 1 to 4 weeks. Patients were post-operatively placed on a 7-day course of oral flucloxacillin (Heracillin, AstraZeneca) 750 mg twice daily. Patients operated on using intraoral access were given instructions concerning scrupulous oral hygiene and the avoidance of potentially contaminated food, such as shrimps or oysters.
Additional procedures performed in connection with the chin reduction were rhinoplasty (12), submental liposuction with platysma tightening (10), malar implants (2), and face-lift (1). Another 16 patients underwent rhinoplasty as a separate surgery, either before or after chin reduction.
Results
Both mandibular bone and the soft tissues were reduced in 24 patients (Table 1). Ten patients underwent bone reduction only in the sagittal plane. Six patients underwent feminization of the chin by resection of the mandibular tubercles to change their square mandibular appearance and obtain a more slender, oval, and feminine face. Only minor vertical and horizontal reduction was necessary (Fig. 4) [6].
In another six patients, only the vertical height of the chin was reduced. This required height decrease of the frontal part of the mandibular body [15]. Chin reduction in the horizontal plane in the majority of cases involved both bone and the fibro-fatty chin pad, but in some patients only the mandibular bone has to be diminished. Operations were technically easier using the submental approach compared with the transoral route. The reason for this was described above in the section “Surgical technique”.
Thirty-six patients could be followed up for a mean of 2.5 years (range 9 months to 12 years), resulting in a follow-up rate of 77%. Because validated standardized instruments with which we can assess chin aesthetics do not exist, the judgement of outcomes is subjective [10, 16]. Overall good results were achieved, which was illustrated by the photographs of the clinical examples (Figs. 5, 6, 7, 8, and 9). Twenty-eight evaluated patients (78%) described the outcome as very good (20) or good (8). Four patients described the result as acceptable and another four as bad. The surgeon’s judgement in the majority of cases correlated well with the opinion of patients, but in 5 patients surgeon evaluated result with the higher score than the patient. This was interpreted that those patients have had too high expectations.
The same patient as in Fig. 6. (Left) Before the corrective surgery. (Right) 6 months after reduction of the bone and soft tissues through the external approach
A 20-year-old woman of Moroccan origin requested profileplasty (left). Treatment was planned in two stages. First transoral chin reduction and rhinoplasty were done, and 6 months later skin excision under the chin, complementary mandibular bone reduction, submental liposuction, and platysma tightening were executed. (Right) 1 year after the last procedure. Restoration of facial harmony is confirmed and objectivized with the help of superimposed Ridel’s line
Only 9 patients were available for X-ray examination before and at the time of follow-up, at least 1 year after reduction of mandibular bone. The rest lived far away, or did not responded, or declined the request.
Obtained radiographs revealed the smooth bone contour and absence of exostoses or calcified bony fragments in the surrounding soft tissues.
Two patients with asymmetric chin expressed at the follow-up their concern about minimal persistent asymmetry, possibly because of some bone regrowth. Few millimetres of cortical bone were taken down with the chisel through an external incision 14 months and 9 years respectively after the primary operation. Obtained bone-chips were sent for histologic investigation, which in the first patient revealed ordinary bone structure and recreation of the thin neo-periosteum. Adjacent connective tissue had normal appearance, without signs of inflammation (Fig. 10). Osseous metaplasia, but no dysplasia, was noted in the bone from the second patient. Covering soft tissue was sclerotic and contained hyaline deposits.
Complications were few and manageable. Transient neuropathies, i.e. disturbances in chin or lip sensation, were common, particularly with the intraoral route and/or after the trimming of the soft tissues. Sensation gradually returned to normal during the course of a few weeks, sometimes months. One patient had an infection in the oral vestibulum due to inappropriate food intake. The infection subsided after 1 week of treatment with parenteral antibiotics and gurgling antiseptic solution. The final outcome in this case was unaffected and excellent. The occluding tape was used for too long time in another patient, who developed staphylococcal infection of the skin and required topical antibiotic treatment.
Skin indentations at the jaw line, or above the soft tissue chin pad, sometimes appeared during the healing phase, but they usually subsided after 6 months. Five patients complained of permanent indentations, which were managed in one case with soft tissue filler and in the others by scar release and undermining. The dog ears were excised in four patients.
Discussion
The available literature on chin reduction in patients with the normal occlusion was scarce at the time when this study was started and it still is. Sliding horizontal osteotomy [5, 17, 18] was not an alternative for my patients because of the complexity of the procedure, necessity of hiring an anaesthetist who will provide general endotracheal anaesthesia, and consequently its high cost. There is also the potential for known complications: injury of the mental nerve and step deformity [10, 19]. Of course the tube is in the way at the transoral procedure and mobility of the patient’s head is limited, and for these reasons, the dissociative anaesthesia with midazolam, pethidine, and ketamine was a good choice for chin reduction surgery by the employed technique. The patients could be discharged 2–3 h after the operation.
Chin reduction by the intraoral route has the huge advantage of leaving invisible scar. Young females dominated this patient cohort. Thirty patients were women under the age of 30. They could not accept to have visible scar on their face and demanded transoral operation.
However, Zide [19] reported that the submental approach for chin reduction gives more consistent results because of the better exposure of the mandibular rim and the higher precision in remodelling soft tissues. Also the platysma muscle and submental fat can be accessed through the same incision. The platysma can be sutured under some tension to the lower border of the mentalis muscle. Fat can be removed either mechanically with the large clamp or by liposuction.
Zide published extensively on chin anatomy and surgery, and he and others use the burring technique for reduction of the mandible [11, 20]. I witnessed and tried the burring procedure at another clinic, but since 1994 I have employed the pneumatic chisel for this purpose, as it works faster than a burr and creates a smoother surface. An alternative method is to use a reciprocating saw, which has become popular [5, 6, 15].
The drawback of this report is that systematic cephalometric and radiologic analysis could not be produced. This would be the possible task for a larger university centre, but realistically, publicly funded health care institutions do not offer aesthetic chin surgery. Another difficulty was change in the radiology techniques. Patients were scattered within the country and abroad and standard for radiologic examination varies from hospital to hospital. Many radiologists turned exclusively to the more lucrative MR techniques and refuse to produce the plain X-rays.
Chin has the central position on the face and, together with the nose, has the decisive impact on our perception of the human profile. A combined procedure called profileplasty is frequently required to create overall balance in the profile (Figs.4 and 9). Not surprisingly, 28 of the 47 patients in this cohort also underwent rhinoplasty. Even the most outstanding result in rhinoplasty will not make the patient face beautiful, if the chin hypoplasia or macrogenia are overlooked and/or not corrected. Most rhinoplasty experts I personally know have no, or very limited, experience in correction of macrogenia.
A natural, oblique, and slender chin contour is one of the components of the female facial beauty [16]. Males usually appreciate more square chin shape and more projection than females, and as pointed out by Guyuron [8], they have two-point light reflection (Fig.4left), whereas in women the chin has a single point light reflection (Fig. 8right above). A weak chin may for some imply a weakness of character, whereas a too prominent chin is perceived as a masculine feature, with some underlying aggressiveness, or it might be a feature of a hormonal disorder like acromegaly. Male patients can seek feminization of their chin contour for different reasons. Some are in the process of gender change, some are gay, or transsexual and some just have an idée fixe (Fig. 4).
A prominent chin may be particularly annoying for young women. One tall patient reported having inquiries of whether she had previously been a male, and she was quite devastated by such questions. In such instances, chin reduction surgery not only has an aesthetic effect, but also causes psychological healing and significantly enhances post-surgical quality of life [21].
Conclusion
This study shows that skilful chin reduction surgery is safe, the aesthetic improvement can be quite spectacular, and it is very rewarding for the patients. It is unfortunate that chin reduction is not well known among plastic surgeons practising in the Western world.
References
Niechajev I (2012) Facial reconstruction using porous high-density polyethylene (Medpor): long-term results. Aesthet Plast Surg 36:917–927
American Society of Plastic Surgeons (2012) Chin surgery skyrockets among women and men in all age groups http://www.plasticsurgery.org/ News-and-Resources/Chin-Surgery/ April 17
Lee EI (2013) Aesthetic alterations of the chin. Semin Plast Surg 27(3):155–160
Guyuron B, Weinfeld AB (2012) Genioplasty in E-book aesthetic plastic surgery. Video atlas Saunders pp 179-197
Ho C-T, Huang C-S, Jo J-L (2012) Improvement of chin profile after mandibular setback and reduction genioplasty for mandibular prognathism and long chin. Aesthet Plast Surg 36:1198–1206
Park MC, Kang M, Lim H, Lee IJ, Shin SJ (2011) Mandibular tubercle resection : a means of maximizing the benefits of reduction mandibuloplasty. Plast Reconstr Surg 127:2076–2082
Feldman JJ (2003) Chin surgery III: revelations (discussion). Plast Reconstr Surg 111:1551–1552
Guyuron B (2008) Genioplasty. Plast Reconstr Surg 121(Apr 4 Suppl): 1-7. https://doi.org/10.1097/01.prs.0000305931.98111.c3
Rosen HM (1991) Aesthetic guidelines in genioplasty: the role of the labiomenthal fold. Plast Reconstr Surg 88:760–767
Zide BM, Pfeifer TM, Longaker MT (1999) Chin surgery I. Augmentation- the allures and the alerts. Plast Reconstr Surg 10(104):1843–1853
Zide BM, Boutros S (2003) Chin surgery III: revelations. Plast Reconstr Surg 111:1542–1549
Niechajev I, Haraldsson PO (1996) Two methods of dissociative anaesthesia for rhinoplasty in outpatient setting. Aesthet Plast Surg 20:159–163
McKinney P, Rosen PB (1982) Reduction mentoplasty. Plast Reconstr Surg 70:147–152
Zide BM (2000) The mentalis muscle: an essential component of chin and lower lip position. Plast Reconstr Surg 105:1213–1215
Warren SM, Spector JA, Zide BM (2007) Chin surgery V: treatment of the long nonprojecting chin. Plast Reconstr Surg 120:760–768
Gonzales-Ulloa M (1962) Quantitative principles in cosmetic surgery of the face (profileplasty). Plast Reconstr Surg 29:186–198
Rosen HM (1995) Aesthetic guidelines in genioplasty: the role of facial dysproportions. Plast Reconstr Surg 95:463–469
Trauner R, Obwegeser H (1957) The surgical correction of mandibular prognatism and retrognathia with consideration of genioplasty. Oral Surg 10:677-18. 689
Zide BM, Warren SM, Spector JA (2007) Chin surgery IV: the large chin—key parameters for successful chin reduction. Plast Reconstr Surg 120:530–537
Zide BM, Longaker MT (1999) Chin surgery: I I. Submental ostectomy and soft- tissue excision. Plast Reconstr Surg 104:1854–1860
Rustemeyer J, Lehman A (2013) Reduction genioplasty enhances quality of life in female patients with prognathism and maxillary hypoplasia undergoing bimaxillary osteotomy. J Oral Maxillofac Surg 42:1083–1092
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Patient consent
Informed consent was obtained from all individual participants in this study.
Conflict of interest
The author declares that he has no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Niechajev, I. Reduction genioplasty for mandibular prognathism and long chin. Oral Maxillofac Surg 24, 333–341 (2020). https://doi.org/10.1007/s10006-020-00853-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-020-00853-8