Abstract
The grafting of fat mixed with adipose-derived stem cells (ASCs) is being increasingly applied to compensate for the disadvantages of previous fat grafting methods. Devices that automatically isolate fat stem cells also have recently been developed. ASCs were isolated from the inguinal region of White rabbits using Icellator®, and the number of cells and their viability were measured. The cell count per fat graft (mL) was adjusted to the following concentrations and subcutaneously transplanted into the back: Control group, Fat + PBS; Fat + ASCs (×0.5) group, 1.6 × 105 cells/mL; and Fat + ASCs (×1) group, 3.2 × 105 cells/mL. Grafted fat weight was measured after 8 weeks, and histological, immunohistological, and specifically stained sections were prepared. Fat absorption was reduced in Fat + ASCs (×0.5) and Fat + ASCs (×1) groups. The number of blood vessels was higher in Fat + ASCs (×1) than in the control group, and blood vessel areas were higher in Fat + ASCs (×0.5) and Fat + ASCs (×1) groups than in the control group. The usefulness of the automated cell processing apparatus, Icellator®, was confirmed, and the results obtained suggest that grafted ASCs promote the vascularization and engraftment of fat grafts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Autologous free fat grafting is a useful technique for repairing various soft tissue defects because it results in low donor site morbidity and grafts that are biocompatible, versatile, natural looking, non-immunogenic, inexpensive, and readily obtainable [1, 2]. Postoperative fat absorption is a limitation to conventional free fat grafting. In addition, lipoaspirates for fat grafting, which do not contain any major blood vessels and possess few precursor cells per unit volume, are often damaged because they are collected under strong negative pressure. In order to overcome the disadvantages associated with traditional fat grafting, adipose-derived stem cell (ASC)-enriched fat grafting techniques are currently being adapted for clinical applications. ASCs are found within a heterogeneous cell population called the stromal vascular fraction and may be extracted from adipose tissue by collagenase digestion [3]. This population includes adult stem cells, endothelial progenitor cells, endothelial cells, vascular smooth muscle cells, and leukocytes [4], and supports the engraftment of grafted fat. Previous studies reported that free fat grafting with ASCs resulted in markedly smaller postoperative reductions in graft volumes than those with an ordinary fat injection, and, hence, fewer procedures are required [5].
Icellator® (Tissue Genesis LLC, Honolulu, HI, USA) was recently developed as a tool to aid in the collection of patients’ own ASCs. It automates and standardizes the extraction, washing, and collection of ASCs for clinical use and removes the need for a culturing step [4]. In recent years, various automatic ASC extraction devices have been developed with the aim of establishing a method for extracting ASCs that may then be safely administered for therapeutic purposes without the need for a cultivation process, even at facilities without a cell processing center (CPC). Stem cell extraction using automatic extraction devices is advantageous in that a CPC is not required, there is a low risk of infection as stem cells are extracted in a closed system, and a consistent cell quality level is achieved because cells are extracted in a completely automatic manner. Doi et al. performed a flow cytometric analysis and confirmed that the composition of ASCs extracted using Icellator® was similar to that of manually isolated ASCs [6]. Furthermore, clinical trials on free fat grafting using this device have been performed in Japan. The above-described pilot study obtained satisfactory outcomes and did not detect any serious side effects [6]. However, the optimal cell concentration and effects of ASCs on the histological characteristics of grafted fat after free fat grafting remain unclear.
Therefore, the purpose of this study was to investigate the utility of ASCs isolated with Icellator® for free fat grafting in a rabbit transplantation model.
Materials and methods
Icellator® and ASC isolation
Icellator® was used in this study to extract ASCs from fat tissue (Fig. 1). This system consists of two parts: one for tissue washing and digestion, and the other for cell concentration. Basically, the whole system automates the manual isolation steps modified from Zuk et al. [3]. Adipose tissue is introduced into the device, washed to remove red blood cells and debris, and then enzymatically digested. After adipose tissue digestion and the release of mononuclear cells from the adipose tissue matrix, the released cells are automatically transferred into the centrifuge processing part. Suspension cells are concentrated by centrifugation and wash cycles. These cycles are repeated until the entire volume of the input cell suspension has been processed and the desired cell population localized into the output syringe. Cells are washed one final time using lactated Ringer’s solution, and are then ready for use. The whole system may be operated aseptically with the use of clinical-grade solutions, such as saline and lactated Ringer’s, and single-use Adipase® consumable sets according to the manufacturer’s protocol. The digestion enzyme used in the present study was Adipase® (Tissue Genesis). The washed digestion solution used was a lactated Ringer’s solution called Lactec G injection (Otsuka Pharmaceutical Factory Inc., Naruto, Japan). The disposable kit, including the tissue wash, digestion containers, and cell concentration chambers, was sterile and accompanied Icellator®.
Animal model
All animal procedures were performed in accordance with the guidelines of the Kansai Medical University Animal Care and Use Committee. Animals were caged individually, and their environment was maintained at room temperature with a 12-h day/night (light/dark) cycle. Standard laboratory food for rats and water were freely provided to the animals. Nine-week-old Slc:NZW rabbits (n = 8/group) were euthanized with an intramuscular injection of Domitor (0.25 mL/kg) and Ketalar (0.25 mL/kg) into the femoral region and an intraperitoneal injection of isoflurane and Somnopentyl (pentobarbital) (2 mL/kg). Subcutaneous fat was collected from the inguinal region, minced into small pieces to liquid fat using scissors, and ASCs were then collected using Icellator® and the attached enzyme, Adipase® (Tissue Genesis), following the manufacturer’s protocol. The abdomen of each rabbit was subcutaneously injected with ASC-enriched fat (0.6 mL) using a 14-G needle. Transplants were excised and analyzed after 8 weeks, as described below.
Preparation of ASC-enriched fat grafting
The ASC-enriched fat grafting procedure is shown in Fig. 2. Fat tissue was divided into two parts: one for extraction and the other for fat grafting. The viability and concentration of ASCs obtained from Icellator® were calculated by Trypan blue staining using a hemocytometer, with dead cells staining blue and live cells remaining unstained. The number of cells and their viability were measured 5 times. Animals allocated for 0.6 mL of fat grafting without the addition of ASCs were designated as the control group, and fat was mixed with PBS (−) instead of the ASC suspension. ASC numbers were adjusted to 1.6 × 105 and 3.2 × 105/mL [Fat + ASCs (×0.5) group and Fat + ASCs (×1) group, respectively] mixed with free fat, and transplanted for ASC-enriched fat grafting. A preliminary experiment confirmed that 3.2 × 105 ASCs were extracted from 1 mL of fat. Therefore, ASC-enriched fat grafts containing 0.5- and 1-fold more ASCs than those in the control group were prepared for the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group, respectively.
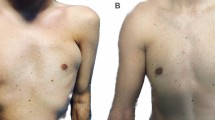
Surviving transplanted fat preparations under the skin of representative white rabbits. Regarding the group that received fat grafting without the addition of ASCs as a control group, 1.6 × 105 and 3.2 × 105 ASCs per transplanted fat volume (mL) were added to the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group, respectively. Eight weeks after surgery, transplant weights were measured using an electronic microbalance. a Gross appearance of transplanted fat. b Fat absorption was significantly less in the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group than in the control group
Weight measurements of transplanted fat tissues
Transplanted fat tissues were excised carefully, and their weights were measured using an electronic microbalance, as advocated by He et al. [7] for animal free fat grafting.
Histological examination of transplanted fat tissues
Fat grafts in each mouse were fixed in 10% formalin neutral buffer solution (pH 7.4) and demineralized with EDTA for 24 h. Four-micrometer-thick sections of the implants were mounted on glass slides and rehydrated. Sections were prepared for hematoxylin and eosin (HE) staining, Azan Mallory staining, and immunostaining as described below.
In order to establish whether ASCs promote neovascularization in fat grafts, capillary numbers and their areas in grafts were assessed using immunostaining for von Willebrand factor, an endothelial cell marker. Deparaffinized sections were used for immunostaining with von Willebrand factor. Before the primary antibody was added, antigenic sites were treated with proteinase K. Slides were immersed in 3% hydrogen peroxide solution for 10 min to inhibit endogenous peroxidase before incubating for 5 min in Tris-buffered saline T (TBST) (50 mM Tris–HCl, pH 7.6, 0.15 M NaCl + 0.05% Tween). In order to detect von Willebrand factor immunoexpression, slides were then exposed to a rabbit polyclonal anti-human von Willebrand factor antibody (DakoCytomation, Inc., Carpinteria, CA, USA), diluted 1:5000 in phosphate-buffered saline (PBS), at 4 °C overnight. After washing in TBST, EnVision™ + HRP, Rabbit (Dako North America, Inc., Carpinteria, CA, USA) was added to the slides at room temperature for 30 min. After washing in TBST, slides were exposed to the Liquid DAB + Substrate Chromogen System (DakoCytomation, Inc.) according to the manufacturer’s protocol. Sections were then counterstained with Mayer hematoxylin, cleared, and mounted with a cover slip. Histological evaluations of 10 fields per section taken from the center of surviving fat tissue were used to measure the number of capillaries (number/field) and their area (mm2/field), which is an index of neovascularization.
Statistical analysis
The Mann–Whitney U test was used for comparisons between groups, with p < 0.05 being regarded as significant. Data are presented as mean ± SD.
Results
Viability and concentration of ASCs from Icellator®
ASC viability was 88 ± 6.4%. Using Icellator®, 3.2 × 105 ± 2.2 × 105 ASCs were extracted from 1 mL of fat.
Assessment of fat tissue survival
Animals that received fat grafting without the addition of ASCs were designated the control group. The number of ASCs per grafted fat volume (mL) was adjusted to 1.6 × 105 and 3.2 × 105 cells/mL (Fat + ASCs (×0.5) group and Fat + ASCs (×1) group, respectively), mixed with free fat, and subcutaneously transplanted. None of the animals died in the 8 weeks following transplantation. Transplanted fat was extirpated at 8 weeks, as shown in Fig. 2a. Transplant weights were measured and compared with that in the control group (Fig. 2b). Transplanted fat weights in the control group, Fat + ASCs (×1) group, and Fat + ASCs (×1) group were 120.0 ± 37.5 mg, 194.8 ± 66.8 mg, and 198.3% ± 75.1 mg, respectively. Transplanted fat weights were significantly higher in the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group than in the control group, which showed that fat absorption was inhibited.
Histological evaluation of fat transplants
Cysts/vacuoles and inflammation were evaluated by HE staining. Large cysts formed in the control group, and had thin cyst walls that ruptured slightly. In the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group, most adipocytes were similar to normal adipocytes. Cyst cells were not present, while some inflammatory cells were observed between fat cells in the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group (Figs. 3). A large number of fibroblast-like cells were detected between fat cells, the number of which was greater in the Fat + ASCs (×1) group than in the Fat + ASCs (×0.5) group. Many capillary blood vessels were noted between fat cells.
A large number of collagen fibers were present between large cysts in the control group. Fewer collagen fibers were observed between fat cells in the Fat + ASCs (×0.5) group, and the nuclei of fibroblast-like cells in the interstitium stained red. Fewer collagen fibers were present between fat cells in the Fat + ASCs (×1) group (Fig. 4).
Histological evaluation of transplanted fat tissues 8 weeks after transplantation using Azan Mallory staining (bar 800 μm). Many collagen fibers were observed between large cysts in the control group. In the Fat + ASCs (×0.5) and Fat + ASCs (×1) groups, the nuclei of a large number of fibroblast-like cells present in the interstitium stained red
Evaluation of vascularization
In the control group, a few blood vessels were present in the interstitial tissue between large cysts. A large number of small new blood vessels formed between normal adipocytes in the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group (Fig. 5). The number of capillaries was significantly larger in the Fat + ASCs (×1) group than in the control group (Fig. 6a). The area of capillaries was significantly higher in the Fat + ASCs (×0.5) group and Fat + ASCs (×1) group than in the control group (Fig. 6b).
a Number of capillaries in surviving transplanted fat tissues. The number of capillaries was significantly higher in the Fat + ASCs (× 1) group than in the control group. *p < 0.05. b Area of capillaries in surviving transplanted fat tissues. Their area was significantly higher in the Fat + ASCs (×0.5) and Fat + ASCs (×1) groups than in the control group. *p < 0.05
Discussion
This study is the first to demonstrate that fresh ASC-enriched fat grafting using the Icellator® automatic cell processing apparatus results in decreased fat absorption and increases the area of new vessels in grafted fat. Fat absorption and cyst formation were significantly inhibited in the Fat + ASCs (×0.5) group (1.6 × 105 cells/mL) and Fat + ASCs (×1) group (3.2 × 105 cells/mL).
Free fat grafting is a technique for using fat obtained by liposuction in plastic and reconstructive surgery. Missana et al. [8] reported the availability of this method and observed improvements in 86% of 69 cases of breast reconstruction surgery that were performed based on liposuction and grafting. In this study, necrosis was reported as a complication in five cases (7%) among 74 procedures. Despite the advantages of this method, such as less operational scarring and invasiveness than other methods, difficulties are associated with obtaining stable postoperative results. This is due to uncertainty regarding the graft survival rate of injected free fat, which is 50% or lower [9], the impact of fat tissues that are quickly absorbed, and complications including necrosis.
A limitation to conventional free fat grafting is that the lipoaspirates to be used for fat grafting are often damaged due to their collection using a strong negative pressure and have no major vessels with few precursor cells per unit volume included [10, 11]. In order to compensate for these defects in lipoaspirated tissues, a method has been devised to mix ASCs extracted from the tissues of lipoaspirates with the same volume of other adipose tissues [12]. Previous studies reported that the maintenance of grafted tissue volumes was markedly better using free fat grafting with ASCs than an ordinary fat injection, resulting in fewer required procedures [5, 13].
A commonly used isolation technique for adipose-derived stem cells (ASCs) is dispersion by collagenase [3]. Collagenase is added to the liposuction aspirate, and after heat treatment the dispersed tissue samples are washed. After centrifugation, the residual cell fraction is used as ASCs for experiments. Isolation of ASCs by flow cytometry is not commonly conducted as specific ASCs markers are yet to be established amidst the various arguments that surround the issue. When ASCs are cultured, they develop into fibroblast-like cells. Adipase® is a collagenase product sold by Tissue Genesis. Since Icellator® automatically performs heating, washing, and centrifuging processes, many ASCs were isolated in a short amount of time.
There are two types of methods for the extraction of ASCs from adipose tissues: manual extraction and extraction using an automatic device. The manual method is simple and cost-effective for basic research; however, if used for clinical research, it cannot be conducted at any facility other than those equipped with a CPC. Over recent years, various automatic ASC extraction devices have been developed with the aim of achieving a method with the ability to extract ASCs that may then be safely administered for therapy without a cultivation process, even at a facility without a CPC. Icellator® (Tissue Genesis LLC, Honolulu, HI, USA) and Celution® (Cytori Therapeutics Inc., San Diego, CA, USA) are two typical automatic devices that are used for this purpose and have been described in clinical reports [2, 5]. Both devices extract ASCs in approximately 1–1.5 h by setting lipoaspirates and an attached disposable kit on the device. Stem cell extraction using automatic extraction devices is advantageous in that a CPC is not required, there is a low risk of infection as stem cells are extracted in a closed system, and a certain technical level of cell quality is expected every time because cells are extracted in a completely automatic manner. However, there are currently no basic animal experimental data on the grafting of free fat mixed with ASCs extracted using these devices. We previously reported that the implantation of ASCs extracted using Celution® together with free fat into nude mice resulted in the more effective inhibition of implanted fat absorption and greater vascularization of grafted fat than when free fat was implanted alone [14]. In the present study, using the White rabbit fat grafting model of He et al., we initially evaluated the effects of ASCs isolated using Icellator®. Fat absorption and cyst formation were significantly inhibited in the groups with the addition of ASCs to fat grafts.
Previous studies proposed a number of mechanisms that promote the engraftment of free fat by ASCs. Many studies confirmed that human ASCs differentiate into fat, bone, cartilage, skeletal muscle, heart muscle, blood vessels, and liver [3, 15]. In addition, these progenitor cells may have the ability to release multiple angiogenic growth factors and cytokines/chemokines including vascular endothelial growth factor (VEGF), hepatocyte growth factor (HGF), and chemokine stromal cell-derived factor-1 (SDF-1). Murohara et al. found that ASCs transplanted into an ischemic region exerted angiogenic growth-promoting effects in the local region that were not observed in the untreated group, and, in addition to the direct differentiation of ASCs into blood vessels, the angiogenic growth factors and cytokines/chemokines produced by ASCs may promote vascularization [16]. Vascularization is known to play an important role in tissue regeneration [14], and fat engraftment was shown to be promoted with vascularization in grafted fat.
Von Willebrand factor is a protein synthesized in vascular endothelial cells and megakaryocytes [17]. Von Willebrand factor is commonly used in assessing angiogenesis in the cutaneous and subcutaneous tissue [18]. While cluster of differentiation 31 (CD31) is primarily expressed on vascular endothelial cells, platelets, monocytes, and macrophages, freeze sectioning may be the only applicable method for certain antibodies. As this study used white rabbits, the selection of available antibodies was extremely limited and it did not stain well with CD31. Von Willebrand factor was selected among the various antibodies as it (a) allows immunostaining of paraffin blocks, (b) is compatible with rabbit tissue, and (c) stains to assess angiogenesis.
Several studies on ASC-mixed fat grafting have recently been reported, with Ni et al. demonstrating that the optimum fat: ASC ratio was 3:1 [19]. They used a similar rabbit model to ours, but a different ASC extraction method. They manually extracted ASCs and the number of ASCs extracted from 1 mL of fat was small (2–2.5 × 105). In the present study, fat engraftment was significantly promoted at fat: ASCs ratios of 1:1 and 2:1. When this ratio was 1:10, fibrosis was reported to occur in grafted fat [14]. It may be necessary to investigate the optimum free fat: ASC mixing ratio using a large animal species in consideration of clinical applications. The results of the present study clarified that mixing with ASCs extracted using Icellator® is useful for the engraftment of free fat.
Conclusion
Fat absorption was reduced in Fat + ASCs (×0.5) and Fat + ASCs (×1) groups. The number of blood vessels was higher in Fat + ASCs (×1) than in the control group, and blood vessel areas were higher in Fat + ASCs (×0.5) and Fat + ASCs (×1) groups than in the control group. The usefulness of the automated cell processing apparatus, Icellator®, was confirmed, and the results obtained suggest that grafted ASCs promote the vascularization and engraftment of fat grafts.
References
Leuchter I, Schweizer V, Hohlfeld J, Pasche P (2010) Treatment of velopharyngeal insufficiency by autologous fat injection. Eur Arch Otorhinolaryngol 267:977–983
Trojahn Kolle SF, Oliveri RS, Glovinski PV, Elberg JJ, Fischer-Nielsen A, Drzewiecki KT (2012) Importance of mesenchymal stem cells in autologous fat grafting: a systematic review of existing studies. J Plast Surg Hand Surg 46:59–68
Zuk PA, Zhu M, Mizuno H, Huang J, Futrell JW, Katz AJ, Benhaim P, Lorenz HP, Hedrick MH (2001) Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 7:211–228
Lin K, Matsubara Y, Masuda Y, Togashi K, Ohno T, Tamura T, Toyoshima Y, Sugimachi K, Toyoda M, Marc H, Douglas A (2008) Characterization of adipose tissue-derived cells isolated with the Celution system. Cytotherapy 10:417–426
Perez-Cano R, Vranckx JJ, Lasso JM, Calabrese C, Merck B, Milstein AM, Sassoon E, Delay E, Weiler-Mithoff EM (2012) Prospective trial of adipose-derived regenerative cell (ADRC)-enriched fat grafting for partial mastectomy defects: the RESTORE-2 trial. Eur J Surg Oncol J Eur Soc Surg Oncol Br Assoc Surg Oncol 38:382–389
Doi K, Tanaka S, Iida H, Eto H, Kato H, Aoi N, Kuno S, Hirohi T, Yoshimura K (2013) Stromal vascular fraction isolated from lipo-aspirates using an automated processing system: bench and bed analysis. J Tissue Eng Regen Med 7:864–870
He X, Zhong X, Ni Y, Liu M, Liu S, Lan X (2013) Effect of ASCs on the graft survival rates of fat particles in rabbits. J Plast Surg Hand Surg 47:3–7
Missana MC, Laurent I, Barreau L, Balleyguier C (2007) Autologous fat transfer in reconstructive breast surgery: indications, technique and results. Eur J Surg Oncol J Eur Soc Surg Oncol Br Assoc Surg Oncol 33:685–690
Bircoll M, Novack BH (1987) Autologous fat transplantation employing liposuction techniques. Ann Plast Surg 18:327–329
Matsumoto D, Sato K, Gonda K, Takaki Y, Shigeura T, Sato T, Aiba-Kojima E, Iizuka F, Inoue K, Suga H, Yoshimura K (2006) Cell-assisted lipotransfer: supportive use of human adipose-derived cells for soft tissue augmentation with lipoinjection. Tissue Eng 12:3375–3382
Eto H, Suga H, Matsumoto D, Inoue K, Aoi N, Kato H, Araki J, Yoshimura K (2009) Characterization of structure and cellular components of aspirated and excised adipose tissue. Plast Reconstr Surg 124:1087–1097
Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthetic plastic surgery 32:48–55 (discussion 56–47)
Sterodimas A, de Faria J, Nicaretta B, Boriani F (2011) Autologous fat transplantation versus adipose-derived stem cell-enriched lipografts: a study. Aesth Surg J Am Soc Aesth Plast Surg 31:682–693
Kakudo N, Tanaka Y, Morimoto N, Ogawa T, Kushida S, Hara T, Kusumoto K (2013) Adipose-derived regenerative cell (ADRC)-enriched fat grafting: optimal cell concentration and effects on grafted fat characteristics. J Trans Med 11:254
Frese L, Dijkman PE, Hoerstrup SP (2016) Adipose Tissue-Derived Stem Cells in Regenerative Medicine. Trans Med Hemoth Offizielles Organ der Deutschen Gesellschaft fur Transfusionsmedizin und Immunhamatologie 43:268–274
Murohara T, Shintani S, Kondo K (2009) Autologous adipose-derived regenerative cells for therapeutic angiogenesis. Curr Pharm Des 15:2784–2790
Randi AM, Laffan MA (2017) Von Willebrand factor and angiogenesis: basic and applied issues. J Thromb Haemost JTH 15:13–20
Kakudo N, Morimoto N, Ogawa T, Hihara M, Notodihardjo PV, Matsui M, Tabata Y, Kusumoto K (2015) Angiogenic effect of platelet-rich plasma combined with gelatin hydrogel granules injected into murine subcutis. J Tissue Eng Regen Med. doi:10.1002/term.2091
Ni Y, He X, Yuan Z, Liu M, Du H, Zhong X (2015) Effect of fat particle-to-SVF ratio on graft survival rates in rabbits. Ann Plast Surg 74:609–614
Acknowledgements
The authors thank Dr. Hara (Department of Oral Implantology, Osaka Dental University) for technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kakudo, N., Morimoto, N., Ogawa, T. et al. Adipose-derived stem cell (ASC)-enriched fat grafting: experiments using White rabbits and an automated cell processing apparatus. Med Mol Morphol 50, 170–177 (2017). https://doi.org/10.1007/s00795-017-0158-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00795-017-0158-7