Abstract
Objectives
Oral tactile perception is important for better mastication, appetite, and enjoyment of food. However, previous investigations have not utilized comprehensible variables thought to have negative effect on oral perception, including aging, denture wearing, and cognitive function. The aim of this study was to elucidate the impact of cognitive function on oral perception in independently living older individuals.
Materials and methods
The study sample was comprised of 987 participants (466 males, 521 females; age 69–71 years). Oral examinations, assessments of cognitive function in preclinical level by Montreal Cognitive Assessment (MoCA)-J, and determination of oral stereognostic ability as an indicator of oral perception were performed. Related variables were selected by univariate analyses; then, multivariate logistic regression model analysis was conducted.
Results
Univariate analyses revealed that number of teeth, removable dentures usage, and cognitive function respectively had a significant relationship with stereognostic score. Next, the subjects were classified into good and poor perception groups (lowest 17.4%) according to oral stereognostic ability. Logistic regression analysis revealed that lower cognitive function was significantly associated with poor oral perception (OR = 0.934, p = 0.017) after controlling for other variables.
Conclusions
Cognitive decline even in preclinical stage was associated with reduced oral perception after controlling for gender, tooth number and denture use in independent living older people.
Clinical relevance
This study suggested that preclinical level of change in cognitive function affected oral perception. Dental practitioners and caregivers may need to pay attention to reduced oral perception among older people even if they do not have trouble in daily life.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral perception plays a key role in recognizing shapes in the mouth, and also provides information that is important for mastication and swallowing [1], and appetite and enjoyment of food. It is generally recognized that deterioration in most sensory modalities inevitably occurs with aging. For example, age-related alterations in two-point discrimination by orofacial segments, such as the lip and cheek were seen in subjects older than 80 years [2]. In addition, reduced stereognostic ability by the tongue [3] and reduced taste sensitivity [4] have been reported in geriatric individuals, while similar studies have found a negative influence of aging on oral stereognostic ability [5, 6]. In another study, females were speculated to have better perceptive ability in the lip, cheek, and chin areas [7], while another found no significant impact of gender on stereognostic ability [6], which seems to be the widely accepted view. In a study by Smith et al., edentulous individuals were shown to have reduced stereognostic ability as compared with dentate subjects [8]. In addition, masticatory performance was found to have a significant association with oral stereognostic ability in denture wearers [1, 9].
Reduced oral perception seems to be a consequence of peripheral sensory and/or central neurological disorder, and previous studies have reported a strong association between peripheral hearing impairment and cognitive disorder in geriatric populations [10, 11]. Therefore, we focused on the link between cognitive status and oral stereognostic ability in this cross-sectional study.
The aim of the present investigation was to elucidate the association between cognitive function and oral perception after controlling for possible related variables.
Materials and methods
Study population and procedures
This research was based on a cohort study of health and longevity termed the SONIC (Septuagenarians, Octogenarians, Nonagenarians Investigation with Centenarians) study, a multidisciplinary research project focused on the health and longevity of Japanese elderly individuals conducted by dentists, nutritionists, psychologists, sociologists, and geriatrics physicians. Data were collected from subjects residing in two main regions of eastern (Tokyo Prefecture) and western (Hyogo Prefecture) Japan, with two additional areas (urban and rural) included in each of the regions: Itami City (western, urban), Asago City (western, rural), Itabashi Ward (eastern, urban), and Nishitama District (eastern, rural).
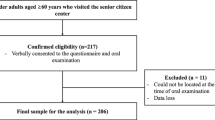
Assessments of subjects aged 69 to 71 years were performed from July 2010 to March 2011. Potential study participants were randomly chosen from a complete enumeration of the residential district and invitation letters were sent to 4267 eligible individuals. Ultimately, 987 volunteers participated in the examinations. The participants were invited to come to the examination venue in groups of 30 to 50 participants per day.
The study protocol was approved by the Institutional Review Board of Osaka University Graduate School of Dentistry (approval number H22-E9). All subjects gave written informed consent prior to participation.
Oral examinations
Oral examinations were performed by nine registered and calibrated dentists with a dental mirror and dental explorer. A penlight was used to conduct oral examinations. The periodontal pocket depth (PPD) was measured with a color-coded probe (CP-12, Hu-Friedy Mfg. Co LLC, Chicago). Usage of removable dentures (maxilla and mandible) was also noted [12].
Assessment of cognitive status
To assess cognitive function, the Montreal Cognitive Assessment Japanese version (MoCA-J) [13] was employed as a general index of cognitive status. Although the mini-mental state examination (MMSE) has been most widely used in previous studies [14], the MoCA is a brief cognitive screening tool for older adults with mild cognitive impairment, and the reliability and validity of the Japanese version (MoCA-J) have been established. Furthermore, this test has been shown to concur with the normal range of the MMSE [13].
Determination of oral stereognostic sensitivity
Oral tactile perception was examined by testing oral stereognostic ability using test pieces comprised of variously shaped forms, as previously described [15, 16], with minor modifications. Briefly, the subjects were asked to use their tongue and palate to identify the shape, and instances of correct identification were noted. The test pieces were 8 × 8 × 2 mm in size and comprised six different shapes: circle, ellipse, semicircle, square, rectangle, and triangle. The test pieces were kept out of the subject’s sight during the test, and each was asked to use their tongue and palate to identify the shape. They were instructed to respond as quickly as possible after placement in the mouth and to avoid biting the test pieces. Five of the six shape forms, excluding ellipse, were examined by each of the subjects. After each piece was removed from the mouth, pictures of all six were shown to the subject and they were asked to point to the picture corresponding to the shape of the piece. Participants were not informed of correct answers at any point during testing. The six shape forms were grouped into three pairs of similar forms, i.e., circles and ellipses, squares and rectangles, and triangles and semicircles. A correct identification was scored as two points, an incorrect identification within the same group was scored as one point, and incorrect identification of a dissimilar form was scored as zero points. Based on their stereognostic ability score, the participants were categorized into the good or poor sensitivity group, with the cutoff point between good and poor sensitivity set so that approximately 20% were included in the poor group.
Assessment of socioeconomic status and fitness status
Assessments of socioeconomic status were based on answers in the questionnaire. As socioeconomic status, we examined self-assessed financial status and educational level. All participants were divided into the following groups based on each variable: sex, self-assessed financial status (dissatisfied, moderately satisfied, satisfied), educational level (≦ 9 years, 10–12 years, ≧ 13 years). Furthermore, we examined instrumental activities of daily living (IADL) [17] and hand grip strength as fitness status.
Statistical analysis
Data analysis was conducted using SPSS version 20.0 for Windows (SPSS Inc., Chicago, IL, USA). Mann-Whitney’s U test was used to evaluate differences in oral stereognostic ability by gender and usage of removable dentures. Spearman’s correlation coefficient test was used to evaluate the association of MoCA-J score, number of teeth, hand grip strength, IADL, and mean PPD with oral stereognostic ability. Kruskal-Wallis test was used to evaluate differences in oral stereognostic ability by socioeconomic status.
For multivariate analysis, explanatory variables were examined using a logistic regression model. The contribution of each variable to the model was evaluated to assess its influence. Odds ratios (ORs) were calculated with a 95% confidence interval. Statistical significance was considered for p values less than 0.05.
Results
The median number of teeth in the subjects was 24. The basic profiles are shown in Table 1, while histograms for number of teeth, MoCA-J scores, and stereognostic ability scores are shown in Fig. 1.
Distribution of subjects with examined variables. Shown are histograms for number of teeth, cognitive (MoCA-J) score, and oral stereognostic ability score. Black arrows indicate the median value for each variable. The median number of teeth, MoCA-J score, and oral stereognostic ability score were 24, 23, and 9, respectively
First, we analyzed the relationship between oral stereognostic ability and related variables. Univariate analyses revealed that number of teeth, maxillary and mandibular denture usage, and MoCA-J score each had a significant relationship with stereognostic score (Table 1). Furthermore, self-assessed financial status (p = 0.042) and educational level (p = 0.045) also had a significantly positive relationship with stereognostic score. Next, we classified the subjects into the good (oral stereognostic score 7–10, n = 815) or poor (oral stereognostic score 0–6, n = 172, 17.4%) perception group based on their stereognostic ability to find factors related to oral stereognostic score. Multivariate logistic regression analysis showed that oral perception was significantly associated with cognitive status (OR = 0.934, p = 0.017), gender (OR = 2.469, p = 0.001), and hand grip strength (OR = 0.951, p = 0.003) after controlling for gender, number of teeth, usage of removable dentures, mean PPD, socioeconomic status, and instrumental activities of daily living (Table 2). In contrast, maxillary and mandibular denture usage, and number of teeth did not have a significant association with cognitive function in multivariate analysis.
Discussion
The present results showed that cognitive decline in a preclinical level had a significantly negative relationship with oral stereognostic ability after controlling for other variables in adults aged 69–71 years old. It was previously reported that cognitive status in older people is associated with number of teeth, periodontal status, and denture usage [18]. In our study, univariate analyses found that oral stereognostic score was significantly related to maxillary and mandibular denture usage and number of teeth. On the other hand, those did not have a significant association with oral stereognostic score in multivariate analysis. Furthermore, number of teeth had a significant correlation with MoCA-J score (data not shown). These findings indicated that those variables may be confounded by cognitive function. The relationship between oral stereognostic ability and cognitive function is apparently robust; therefore, cognitive status was likely to play a pivotal role in oral perception in older individuals.
It has been widely reported that declines in most sensory and motor modalities inevitably occur with aging, including oral stereognostic ability and masticatory function [1,2,3,4,5,6, 9, 16, 18, 19]. In addition, edentulous individuals have been shown to have a lower level of stereognostic ability as compared with dentate [8]. However, the present multivariate analysis findings indicated that dental status has no significant impact on stereognostic ability. For discrimination of the shapes of test pieces in the oral cavity, elaboration by or sensitivity of the tongue seems to be more important as compared to the palate, as previously reported [20]. Although aging, tooth loss, and denture usage have been considered as causes of decline in oral perception, cognitive decline may be the root cause.
We recognize that our study has several limitations. All subjects were considered to be cognitively eligible in spite of their elderly status, because their functional capacity was at a high level, thus they may not have a comprised a representative sample of Japanese elderly individuals. Furthermore, the methodology used to assess oral tactile perception included some factors that are difficult to align. For example, the psychophysical situation, which potentially affects stereognostic ability, is sometimes less controllable during examinations of a large sample.
Nevertheless, this is the first study to utilize a multivariate model to elucidate association between decline in cognitive function within clinically normal level and oral stereognostic ability in older subjects. We consider that our novel findings will provide useful information for both clinical practices and future research in masticatory difficulty and poor appetite. Dentists should explain to people who have cognitive dysfunction and their family, and introduce them to a medical institution.
In conclusion, we found that cognitive status, in contrast to dental status, was a major factor affecting oral tactile perception in elderly individuals.
References
Ikebe K, Amemiya M, Morii K, Matsuda K, Furuya-Yoshinaka M, Yoshinaka M, Nokubi T (2007) Association between oral stereognostic ability and masticatory performance in aged complete denture wearers. Int J Prosthodont 20:245–250
Calhoun KH, Gibson B, Hartley L, Minton J, Hokanson JA (1992) Age-related changes in oral sensation. Laryngoscope 102:109–116
Kawagishi S, Kou F, Yoshino K, Tanaka T, Masumi S (2009) Decrease in stereognostic ability of the tongue with age. J Oral Rehabil 36:872–879
Yoshinaka M, Ikebe K, Uota M, Ogawa T, Okada T, Inomata C, Takeshita H, Mihara Y, Gondo Y, Masui Y, Kamide K, Arai Y, Takahashi R, Maeda Y (2016) Age and sex differences in the taste sensitivity of young adult, young-old and old-old Japanese. Geriatr Gerontol Int 16:1281–1288
Grasso JE, Catalanatto FA (1979) The effects of age and full palatal coverage on oral stereognostic ability. J Prosthet Dent 41:215–219
Jacobs R, Bou Serhal C, van Steenberghe D (1998) Oral stereognosis: a review of the literature. Clin Oral Investig 2:3–10
Chen CC, Essick GK, Kelly DG, Young MG, Nestor JM, Masse B (1995) Gender-, side- and site-dependent variations in human perioral spatial resolution. Arch Oral Biol 40:539–548
Smith PW, McCord JF (2002) Oral stereognostic ability in edentulous and dentate individuals. Eur J Prosthodont Restor Dent 10:53–56
Garrett NR, Kapur KK, Jochen DG (1994) Oral stereognostic ability and masticatory performance in denture wearers. Int J Prosthodont 7:567–573
Lin MY, Gutierrez PR, Stone KL, Yaffe K, Ensrud KE, Fink HA, Sarkisian CA, Coleman AL, Mangione CM (2004) Study of Osteoporotic Fractures Research Group. Vision impairment and combined vision and hearing impairment predict cognitive and functional decline in older women. J Am Geriatr Soc 52:1996–2002
Panza F, Solfrizzi V, Logroscino G (2015) Age-related hearing impairment—a risk factor and frailty marker for dementia and AD. Nat Rev Neurol 11:166–175
Engelen L, Prinz JF, Bosman F (2002) The influence of density and material on oral perception of ball size with and without palatal coverage. Arch Oral Biol 47:197–201
Fujiwara Y, Suzuki H, Yasunaga M, Sugiyama M, Ijuin M, Sakuma N, Inagaki H, Iwasa H, Ura C, Yatomi N, Ishii K, Tokumaru AM, Homma A, Nasreddine Z, Shinkai S (2010) Brief screening tool for mild cognitive impairment in older Japanese: validation of the Japanese version of the Montreal Cognitive Assessment. Geriatr Gerontol Int 10:225–232
Nasreddine ZS, Phillips NA, Bédirian V, Charbonneau S, Whitehead V, Collin I, Cummings JL, Chertkow H (2005) The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc 53:695–699
Hirano K, Hirano S, Hayakawa I (2004) The role of oral sensorimotor function in masticatory ability. J Oral Rehabil 31:199–205
Ikebe K, Amemiya M, Morii K, Matsuda K, Furuya-Yoshinaka M, Nokubi T (2007) Comparison of oral stereognosis in relation to age and the use of complete dentures. J Oral Rehabil 34:345–350
Ishizaki T, Watanabe S, Suzuki T, Shibata H, Huga H (2000) Predictors for functional decline among nondisabled older Japanese living in a community during a 3-year follow-up. J Am Geriatr Soc 48:1424–1429
Wu B, Fillenbaum GG, Plassman BL, Guo L (2016) Association between oral health and cognitive status: a systematic review. J Am Geriatr Soc 64:739–751
Engelan L, van der Bilt A, Bosman F (2004) Relationship between oral sensitivity and masticatory performance. J Dent Res 83:388–392
Kaiba Y, Hirano S, Hayakawa I (2006) Palatal coverage disturbance in masticatory function. J Med Dent Sci 53:1–6
Acknowledgments
The authors thank all of the participants who were involved in this study. We also express our appreciation to Drs. Enoki K. and Tada S. for data collection.
Funding
This study was supported by Grants-in-Aid for Scientific Research (JP15H05025 and JP16H05523) from the Japan Society for the Promotion of Science.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Fukutake, M., Ogawa, T., Ikebe, K. et al. Impact of cognitive function on oral perception in independently living older people. Clin Oral Invest 23, 267–271 (2019). https://doi.org/10.1007/s00784-018-2433-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2433-y