Abstract
Introduction
This study aimed to evaluate, for the first time, the bone profile of adult women and men with and without normal-weight obesity (NWO) syndrome and its association with bone health-related nutrient intake, anthropometry, and body composition.
Materials and methods
This was a cross-sectional study of adults aged between 20 and 59 years with normal body weight, separated according to body fat (BF) percentage into NWO and non-NWO syndrome groups. BF > 30% and > 19% were considered high for women and men, respectively. Socioeconomic, physical activity, food consumption, anthropometric, and body composition data were evaluated. Student's t-test or Mann–Whitney test and Pearson's χ2 or Fisher's exact tests were applied for comparisons. Multiple linear regression models were developed, with bone parameters as the dependent variables and anthropometric, body composition, and food consumption data as the main independent variables.
Results
The sample consisted of 224 adults (69.2% women) with a median (interquartile range) age of 23 (21–25) years, 71% of whom had NWO syndrome. Compared with women, a higher percentage of men had a lower-than-expected spinal bone mineral density (BMD) Z-score for age (10%; p = 0.0214). Bone parameters were similar between groups. Spinal BMD was negatively associated with male sex and positively associated with body weight. The femoral BMD was negatively associated with BF percentage and positively associated with body mass index.
Conclusion
The negative association of BMD with BF percentage may suggest a higher risk of bone alterations in individuals with NWO syndrome and should be monitored over time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Due to the inability of body mass index (BMI) to differentiate between the amount and distribution of body fat (BF) and lean mass, normal-weight obesity (NWO) syndrome is characterized by normal BMI but excess BF [1]. Despite having a normal body weight, individuals with NWO syndrome are at an increased risk of developing nutrition-related chronic non-communicable diseases (NR-NCCD), such as hypertension, dyslipidemia, type 2 diabetes, and cardiovascular diseases. In addition, mechanical and bone changes may be more prevalent in these individuals [1,2,3,4,5].
The mechanisms explaining how excess BF affects and alters bone quality have not been clearly elucidated yet. Lean body mass seems to be positively associated with bone mineral density (BMD) as well as structural strength during childhood and adolescence [6]. However, excess BF correlates negatively with lean body mass and BMD [6, 7].
Several factors, such as (epi)genetics, hormones, race, physical activity levels, intercurrent diseases, prolonged use of medication, body composition, and diet, influence bone maturation at the end of the second and beginning of the third decade of life [8]. Most of these factors contribute in varying proportions to both bone maintenance and bone loss in adulthood [9]. Nutrients, such as proteins, calcium, vitamin D, and magnesium, affect the gain and maintenance of bone mass [6]. Therefore, an adequate intake of these nutrients can alleviate the long-term risk of osteoporosis, whereas a diet rich in highly processed foods, which lack protein and other essential nutrients, can be deleterious [7,8,9,10]. Thus, both body composition and the diet can determine an individual’s bone health throughout their life.
To the best of our knowledge, the bone health of adults with NWO syndrome has not been studied. The aim of our study was to evaluate the bone profile of adult women and men with NWO syndrome and their counterparts (normal BMI and BF: non-NWO), as well as its association with diet and anthropometric and body composition markers. We hypothesized that individuals with NWO syndrome have an unfavorable bone profile compared with those without the syndrome, and that the diet and anthropometric and body composition variables would be negatively associated with bone quality.
Material and methods
Study design and ethics
This was an observational, analytical, and cross-sectional study, wherein participants were recruited through the distribution of folders, social media advertisements, and emails sent to individuals in the academic (students and professors) and non-academic (employees) communities of the Federal University of Goiás, Brazil.
This study was conducted in accordance with the guidelines of the Declaration of Helsinki [11] and its amendments. All the procedures were approved by the Ethics Committee of the Federal University of Goiás (protocol number: 2.772.022). Written informed consent was obtained from all the participants.
Inclusion and exclusion criteria
Individuals from the university community at the Federal University of Goiás, aged between 20–59 years with a normal BMI (18.50–24.99 kg/m2) [12], were included in the study and separated into two groups: individuals with increased BF percentage (> 30% for women [1] and > 19% for men [13])—the NWO group—and individuals with a normal BF percentage—the non-NWO group. The cut-off points for BF percentage were chosen from previous studies analyzing individuals with NWO, considering the age group for men [1] and the value established in the first study with NWO for women [13].
We excluded individuals who had metallic implants, limb amputations, consumed drugs or vitamin/mineral supplements, were undergoing nutritional treatment, had changed their usual diet 6 months before the study (and intentionally or unintentionally experienced weight changes), women who were pregnant, breastfeeding, menopausal, or on hormone replacement therapy, individuals who self-reported acute clinical conditions, such as infection, inflammation, fever, diarrhea, or chronic diseases, such as diabetes mellitus, moderate/severe systemic arterial hypertension, cancer, and rheumatoid arthritis. Smokers and athletes were also excluded.
Sampling and data collection
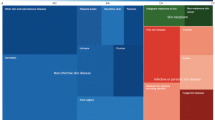
Non-probability convenience sampling [14] was adopted. The final sample set consisted of 224 individuals and data from all individuals were used in this study. Among the 224 participants, 159 (71%) were segregated into the NWO group and 65 (29%) into the non-NWO group (Fig. 1).
Flowchart of the sampling process according to the protocol STrengthening the Reporting of OBservational Studies in Epidemiology (STROBE) [18]
Data were collected at the School of Nutrition and through telephone and email communications between January and July 2019. The data collection process involved the following steps: (1) general dissemination of information about the study; (2) application of a face-to-face checklist for the inclusion and exclusion criteria, measurement of weight and height for BMI classification, application of questionnaires to obtain sociodemographic, lifestyle, and health information, collection of the first 24-h food recall (R24h), anthropometric assessment, and dual-energy X-ray absorptiometry (DXA) examination; (3) collection of the second and third R24h via phone calls [15] 15 days after the evaluations; and (4) dissemination of the results to all participants.
A standardized questionnaire was designed to collect socioeconomic and demographic data, including sex, age, and self-reported skin color (yellow, white, black, and brown). To determine the economic class, the Economic Classification Criterion of the Brazilian Association of Research Companies [16] was used. The short version of the International Physical Activity Questionnaire, validated in Brazil, was used to assess the participants' level of physical activity [17].
Anthropometry, body composition, and bone profile
Anthropometric measurements were performed by two trained researchers using standardized techniques [19]. Weight, height, BMI, and waist and hip circumferences were measured in this study. Weight was measured using a digital scale (Filizola Shop, São Paulo, Brazil) with a maximum load of 150 kg and an accuracy of 0.1 kg. Height was measured using a Seca® stadiometer (Seca Deutschland, Hamburg, Germany) with a maximum range of 220 cm and an accuracy of 0.1 cm. Circumferences were measured in duplicate using a Seca® body measure tape (Seca Deutschland, Hamburg, Germany) with a length of 200 cm and a precision of 1 mm.
Body composition and bone markers were assessed by a specialized technician, with the help of a third researcher using DPX NT Lunar® DXA equipment (General Electric Medical Systems, Madison, USA), following the recommendations of the International Society for Clinical Densitometry (ISCD) [20, 21]. By scanning the total body (except the head), the total BF percentage and appendicular lean mass (ALM) were estimated. The ALM was calculated as the sum of the lean soft tissue of the limbs minus the bones. The ALM index (ALMI) was calculated as ALM/height2 (kg/m2) [21].
To evaluate the bone markers, the BMD of the lumbar spine (L1 to L4 vertebrae; g/cm2) and right femoral neck (mg/m2) was obtained [9, 22]. To classify low BMD in premenopausal women and men aged < 50 years, the World Health Organization (WHO) and ISCD recommend the use of the Z-score with ethnic adjustments. Therefore, we applied the cut-off points for Z-score classification “below the expected range for age” when Z < −2.0 and “within the expected range for age” when Z > −2.0 [9, 21]. Z-score values were the primary outcomes of the study and were analyzed as categorical variables.
Bone health-related nutrient intake
Three R24h were used to assess the usual diet. The first R24h was applied face-to-face during the first appointment using a photographic manual and home-measuring instruments. To collect more accurate information on food consumption, we followed the multiple pass method (MPM) [23]. The other two R24h were collected on non-consecutive days via phone calls within a maximum period of 15 days, including one weekend day and following the MPM [15, 24, 25].
Information on food intake was converted into measures of mass (g)/volume (mL), and the three R24h were evaluated using the Nutrition Data System for Research software (University of Minnesota, Nutrition Coordinating Center, Minneapolis, USA). When necessary, the mean nutrient values were adjusted according to the residual method [26].
Statistical analysis
Double-entry databases were constructed to check for consistency. Data distribution was analyzed using the Shapiro–Wilk test. Data are presented as mean ± standard deviation, median (interquartile range [IQR]), or absolute and relative frequencies (%).
Differences between groups and between men and women were analyzed using Student's t-test or Mann–Whitney test for independent samples and Pearson's χ2 test or Fisher's exact test. Missing values were verified and excluded from the intergroup comparisons. To assess bone parameters related to spinal and femoral BMD, data were analyzed as continuous and categorized as Z-scores, according to the ISCD guidelines [21].
Multiple linear regression models were built to assess the associations between independent and dependent variables. For adjustments, backward or stepwise strategies were tested according to the lowest value of the Akaike Information Criterion (AIC), a relative measure of the goodness of fit of a statistical model [27]. Backward and stepwise are automated variable selection techniques used in multiple linear regression that aim to identify the most important predictor variables to include in the model. While we acknowledge that these strategies are not without limitations, they do offer several benefits over the manual selection of variables.
The dependent variables included BMD (mg/cm2) of the femoral neck and BMD (g/cm2) of the lumbar spine. Qualitative independent variables included the classification into NWO and non-NWO syndrome groups (yes/no), sex (female/male), and skin color (yellow, white, black, or brown). The quantitative independent variables included the level of physical activity, age, weight, waist and hip circumferences, BF percentage, ALM, and ALMI, as well as the intake of carbohydrates, fats, protein, calcium, magnesium, phosphorus, vitamins D, K, C, and folate, caffeine, phytic acid, and oxalic acid. To verify the existence and magnitude of multicollinearity and to decide which variables should be removed from the analysis, the variance inflation factor, which should not exceed 5, was calculated [28].
Statistical analyses were performed using R software version 4.0.4 [29], with a convenience sample, significance level of 5%, and statistical power > 80%. To assess statistical power, the pwr package version 1.3–0 of R software was used. In the comparison tests, a medium effect size (d = 0.5–0.79) was considered, according to the variation in sample number in the groups and subgroups. For all regression models, we also used a medium effect size (f2 = 0.15) [30], a sample size of 222, and the numerator and denominator of the degrees of freedom for each regression.
Results
Of the 224 individuals evaluated, most (n = 159) were classified with NWO (71%). Among these, there was a higher number of women (69.2%). The median (IQR) age of the cohort was 23 years (21–25 years, minimum: 20 years; maximum: 49 years) and did not significantly differ between the NWO and non-NWO syndrome groups. The number of individuals in each age group, divided into decades, was as follows: 20–29 years: 210 individuals, 30–39 years: 12 individuals, and 40–49 years: 2 individuals. No differences were observed in the proportion of women and men, self-reported skin color, economic classes, and level of physical activity between the two groups (Table 1).
Both women and men in the NWO syndrome group had higher weights, BMIs, and waist and hip circumferences but lower mean ALM and ALMI than those in the non-NWO syndrome group (Table 2).
The daily total energy intake of the NWO group was lower than that of the non-NWO syndrome group (1968.1 [1617.7–2599.1] versus 2255.0 [1805.0–2692.0] kcal/day; p = 0.0267) while their fat intake (% total energy) was higher (35.9 ± 5.8 versus 33.8 ± 6.0%; p = 0.0190), and slightly higher than the acceptable levels of macronutrient distribution recommended by the Institute of Medicine [31]. Carbohydrate, fiber, magnesium, and folate intakes were lower in the NWO syndrome group. Caffeine intake remained at a safe level (below 400 mg/day) [32], and no differences were observed between the two groups (Table 3).
Considering the differences in bone parameters between women and men, we compared the BMD data between the two sexes and between the two groups. Men had a higher femoral BMD than women (p < 0.0001). The prevalence of spinal Z-scores ‘below the expected range for age’ (≤ −2.0) was higher in men (10.0%; p = 0.0214) than in women. However, no differences were observed in the femoral Z-scores. In addition, although a higher percentage of men with NWO syndrome (14.3%) showed a lower spinal Z-score for age than those without NWO syndrome (4.2%), the difference was not statistically significant (p = 0.2583). The bone parameters of women did not differ between the two groups (Table 4).
Table 5 shows the multiple regression models for the associations between the independent variables and spinal and femoral BMD. Corroborating the higher percentage of men with low spine BMD Z-scores compared with women, men remained in the final model, with a negative association with spine BMD (β = − 0.12; 95% confidence interval [CI] = −0.20 to − 0.05; p = 0.0006). Body weight was positively associated with spinal BMD (β = 0.01; 95% CI = 0.006–0.01; p < 0.0001). Femoral BMD was negatively associated with BF percentage (β = − 6.52; 95% CI = − 8.37 to − 4.67; p < 0.0001) and positively associated with BMI (β = 29.0; 95% CI = 16.7–41.2; p < 0.0001). Bone parameters were not significantly associated with the evaluated nutrients (Table 5).
Discussion
This is the first study to evaluate the bone parameters of young adult women and men with and without NWO syndrome and assess the associated factors. Although we did not find differences in bone profiles between the NWO and non-NWO syndrome groups, spinal BMD was positively associated with body weight and negatively associated with male sex. The femoral BMD was positively associated with BMI and negatively associated with BF percentage, which is an important finding since BF percentage is the hallmark of NWO syndrome.
We found a high prevalence of NWO syndrome in our study (approximately 70%); however, caution should be exercised when extrapolating these data to the Brazilian population or to other populations as the sample of our study was chosen by convenience and the participants were young adults from a Brazilian public university without previously diagnosed diseases. This high prevalence may be related to the cut-off points for classifying the BF percentage. However, we chose these cut-off points considering previous studies on NWO syndrome that evaluated individuals of similar ages and with the same technique for assessing body composition [1, 13].
Regarding nutrients involved in bone health, the distribution of lipids and carbohydrates as well as the different fiber intake between individuals with and without NWO may be important factors in the study of metabolic aspects of NWO. A bidirectional Mendelian randomization study evaluated more than 200,000 European individuals and observed that lower intake of carbohydrate and higher intake of lipids are causal factors for higher BMI and waist circumference [33]. Fiber consumption is linked to certain types of carbohydrates, justifying the lower values in individuals with NWO.
We also found lower magnesium and folate consumption in the NWO group compared to non-NWO group. Magnesium intake has been positively associated to better glycemic control and negatively associated with waist circumference, weight, BMI, and BF percentage [34,35,36]. These negative associations are probably related to magnesium’s role in cell membrane stabilization, which can reduce the effects of oxidative stress and regulate inflammatory processes [36, 37]. Deficient folate intake increases the likelihood of genomic instability and may be involved in the development of NR-NCCD. In addition to evidence of a relationship between obesity and folate intake, there are reports of a negative association of folate intake with BF percentage [38]. Therefore, our results seem to be in line with such scientific evidence. However, the relationship between folate metabolism and the presence of obesity is still unclear.
The intake of other nutrients and substances considered important to bone health, such as calcium, vitamin D, caffeine, and phytic and oxalic acids, did not differ between the NWO and non-NWO syndrome groups. However, constant monitoring of the intake and status of these nutrients is important for maintaining bone health.
Although we did not observe differences in bone profiles between the two groups, we found important associations between bone markers and anthropometric and body composition variables. The multiple linear regression models showed values of R2 and adjusted R2 similar to studies that evaluated predictive variables of BMD, probably because genetic factors explain 50–85% of the BMD variance, an aspect not analyzed in our study [39, 40].
As all individuals had a normal BMI, when considering the positive association of spinal and femoral BMD with body weight and BMI, respectively, the weight variation in the total sample was restricted to the normal BMI range. However, the differences within this range were sufficient to detect a positive association with spinal BMD, corroborating the results of studies that evaluated the influence of body weight on bone quality [41,42,43]. In the Framingham Osteoporosis cohort study, 693 women and 439 men were followed from early adulthood, with periodic assessment of body weight for 40 years and BMD assessment by DXA in the 20th biennial exam. The association of bone profile with body weight was stronger in children and adolescents, but it was also observed in adults. In addition, body weight was more strongly associated with BMD in women than in men [41].
In general, the positive associations between bone parameters and body weight observed both in the literature and in our study suggest mechanical signaling induced by body weight. Osteocytes are the main sensors in mechanotransduction, a process responsible for producing biochemical reactions from mechanical stimuli such as weight or weightlessness, which can promote bone formation or resorption. Therefore, bone “deformation” promoted by weight or force causes an adaptive skeletal response, and osteocytes induce bone formation through osteoblasts [42]. The opposite occurs when tension levels caused by weight are low, which may lead to the apoptosis of osteocytes, resulting in greater activity of osteoclasts and bone resorption. However, extreme deviations in weight and body composition can impair bone strength [42, 43].
In addition to anthropometric and body composition variables, the male sex was part of the final regression model and was negatively associated with spinal BMD. This result indicates that in relation to women, the spinal BMD units decrease in men, corroborating the data from the intersex comparison, in which a higher percentage of men had a spinal BMD Z-score below the expected range for age. Similar results were described in a study involving 59 Caucasians and 44 Afro-Caribbeans aged between 20 and 37 years, which assessed the influence of ethnicity, sex, and bone turnover on BMD [44]. Men of both ethnicities had lower BMD and higher concentrations of bone resorption markers than women. The likely reason is the late maturation of the lumbar spine in men, which extends until the third decade of life [44]. Similarly, the median age of individuals in our study indicates the beginning of adulthood and can be considered a key factor in understanding the negative association between spinal BMD and the male sex.
The effects of BF and its distribution on bone health are still controversial, with some studies considering it as a protective factor for BMD while others as a deleterious factor [45,46,47,48,49,50]. Gravitational forces attributed to body weight that stimulate adaptive bone formation may be a confounding factor in the association of the bone profile with BF when excess BF is due to weight gain [47]. We found a negative association between the femoral BMD and BF percentage. These results corroborate those of a study involving American students, 150 men (17.4 ± 1.6 years old) and 150 women (17.0 ± 1.7 years old), with a BMI between 16.0 and 41.4 kg/m2, which showed that, regardless of the increase in weight and lean mass, excess adipose tissue is not beneficial to bone structure in this age group [46].
A study conducted with Chinese individuals—7137 men (47.3 ± 7.7 years old), 4585 premenopausal women (41.5 ± 5.3 years old), and 2248 post-menopausal women (52.6 ± 4.7 years old) –used DXA to assess body composition and noted that total and hip bone mineral contents were negatively associated with BF, regardless of body weight, age, and physical activity level. In addition, the odds ratios were higher for osteoporosis, osteopenia, and non-spinal fractures in men, pre- and post-menopausal women, and women with BF percentages in the upper quartiles. The sample size made it possible to stratify the sample at every 5 kg of body weight and to evaluate the associations of bone parameters with BF in different weight ranges, including analysis in individuals with normal weight [50], like in our study.
Individuals with a high BF percentage have increased pro-inflammatory cytokine concentrations, which can explain the influence of adipose tissue on bone health [51, 52]. Pro-inflammatory cytokines can stimulate osteoclast activity by regulating the receptor activator of nuclear factor-κB ligand (RANKL)/RANK/osteoprotegerin system [51]. Another important aspect is that both adipocytes and osteoblasts originate from mesenchymal stem cells [53]. Therefore, the increase in adipogenesis in the bone marrow in response to high BF can negatively impact osteoblastogenesis and/or stimulate osteoclastogenesis due to the high production of cytokines [53, 54]. However, these mechanisms have not been investigated in individuals with NWO syndrome.
While lean mass influences bone density through direct mechanical effects on muscles, adipose tissue increases estrogen production in women, which results in greater gravitational loading in those with a higher BMI [55]. However, the role of BF as a function of gravitational load in overweight individuals is not enough to establish a positive association with bone parameters since high amounts of adipose tissue can cause important metabolic changes [51,52,53,54].
Limitations of our study include the cross-sectional design and the non-probability convenience sampling, which restricts the interpretation of results. Furthermore, our discussion was somewhat limited by the lack of research assessing bone health in young individuals as a function of body composition. In addition, differences in cut-off points and techniques used to assess body composition limit discussions regarding NWO syndrome. In contrast, this is the first study to evaluate parameters associated with bone health in young women and men with NWO syndrome, and the results can be used to drive strategies to improve body composition of these individuals and in the design of other studies on bone health of individuals with excess BF.
In conclusion, young adults with NWO syndrome do not have a worse bone profile than those without this syndrome, but bone parameters were negatively associated with BF percentage, which suggests a higher risk of bone loss and fractures in individuals with NWO syndrome if their BF percentage remains high throughout life.
Indeed, knowledge of the risk factors for bone health in such individuals may help slow down the increasing worldwide prevalence of bone mass loss and fractures. Finally, our results reinforce the need for further studies on the bone health of individuals with NWO syndrome and its medium- and long-term impacts.
References
De Lorenzo A, Martinoli R, Vaia F, Di Renzo L (2006) Normal weight obese (NWO) women: an evaluation of a candidate new syndrome. Nutr Metab Cardiovasc Dis 16:513–523. https://doi.org/10.1016/j.numecd.2005.10.010
Romero-Corral A, Somers VK, Sierra-Johnson J, Korenfeld Y et al (2010) Normal weight obesity: a risk factor for cardiometabolic dysregulation and cardiovascular mortality. Eur Heart J 31:737–746. https://doi.org/10.1093/eurheartj/ehp487
Franco LP, Morais CC, Cominetti C (2016) Normal-weight obesity syndrome: diagnosis, prevalence, and clinical implications. Nutr Rev 74:558–570. https://doi.org/10.1093/nutrit/nuw019
Kang S, Kyung C, Park JS, Kim S, Lee SP et al (2014) Subclinical vascular inflammation in subjects with normal weight obesity and its association with body fat: an 18 F-FDG-PET/CT study. Cardiovasc Diabetol 13:70. https://doi.org/10.1186/1475-2840-13-70
Ho-Pham LT, Nguyen UDT, Nguyen TV (2014) Association between lean mass, fat mass, and bone mineral density: a meta-analysis. J Clin Endocrinol Metab 99:30–38. https://doi.org/10.1210/jc.2014-v99i12-30A
Weaver CM, Gordon CM, Janz KF, Kalkwarf HJ, Lappe JM et al (2016) The national osteoporosis foundation’s position statement on peak bone mass development and lifestyle factors: a systematic review and implementation recommendations. Osteoporos Int 27:1281–1386. https://doi.org/10.1007/s00198-015-3440-3
Hardcastle AC, Aucott L, Fraser WD, Reid DM, Macdonald HM (2011) Dietary patterns, bone resorption and bone mineral density in early post-menopausal Scottish women. Eur J Clin Nut 65:378–385. https://doi.org/10.1038/ejcn.2010.264
Shin S, Kim S-H, Joung H, Park MJ (2017) Milk-cereal and whole-grain dietary patterns protect against low bone mineral density among male adolescents and young adults. Eur J Clin Nut 71:1101–1107. https://doi.org/10.1038/ejcn.2017.81
WHO Scientific group on the prevention and management of osteoporosis. Prevention and management of osteoporosis: report of a WHO scientific group. World Health Organization. Tech Rep Ser 921:1–164. https://apps.who.int/iris/handle/10665/42841. Accessed 10 June 2022
Zaretsky J, Griess-Fishheimer S, Carmi A, Travinsky Shmul T, Ofer L, Sinai T, Penn S, Shahar R, Monsonego-Ornan E (2021) Ultra-processed food targets bone quality via endochondral ossification. Bone Res 9:1–13. https://doi.org/10.1038/s41413-020-00127-9
World Medical Association Declaration of Helsinki (2000): ethical principles for medical research involving human subjects. WMA http://www.wma. net/e/policy/b3. Accessed 30 June 2020
World Health Organization (2000) Obesity: preventing and managing the global epidemic Report of a WHO consultation. WHO Tech Rep Ser 894:1–253
Kosmala W, Jedrzejuk D, Dezhko R, Przewlocka-Kosmala M, Mysiak A, Bednarek-Tupikowska G (2012) Left ventricular function impairment in patients with normal-weight obesity: contribution of abdominal fat deposition, profibrotic state, reduced insulin sensitivity, and proinflammatory activation. Circ Cardiovasc Imaging 5:349–356. https://doi.org/10.1161/CIRCIMAGING.111.969956
Henry GT (1990) Practical sampling. Applied social research methods series, vol 21. Sage Publications, London, pp 17–32
Galasso R, Panico S, Celentano E, Del Pezzo M (1994) Relative validity of multiple telephone versus face-to-face 24-hour dietary recalls. Ann Epidemiol 4:332–336. https://doi.org/10.1016/1047-2797(94)90090-6
Brasil CCEB, Filiadas BE. ABEP – Associação Brasileira de Empresas de Pesquisa (2019) Available in: http://www.abep.org/criterio-brasil. Accessed 26 Mar 2022
Matsudo S, Araújo T, Matsudo V, Andrade D, Andrade E et al (2001) Questionário internacional de atividade física (Ipaq): estudo de validade e reprodutibilidade no Brasil. Rev Bras Ativ Fis Saud 6:5–18. https://doi.org/10.12820/rbafs.v.6n2p5-18
Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61:344–349. https://doi.org/10.1016/j.jclinepi.2007.11.008
Lohman TG, Roche AF, Martorell R (1988) Anthropometric standardization reference manual. Human Kinetics Books, Champaign, Illinois
Williams JE, Wells JC, Wilson CM, Haroun D, Lucas A, Fewtrell MS (2006) Evaluation of Lunar Prodigy dual-energy X-ray absorptiometry for assessing body composition in healthy persons and patients by comparison with the criterion 4-component model. Am J Clin Nutr 83:1047–1054. https://doi.org/10.1093/ajcn/83.5.1047
ISCD—The international society for clinical densitometry (2019) official positions adult 1–34. https://iscd.org/learn/official-positions/adult-positions/. Accessed 10 June 2022
Boonen S, Kaufman JM, Reginster JY, Devogelaer JP (2003) Patient assessment using standardized bone mineral density values and a national reference database: implementing uniform thresholds for the reimbursement of osteoporosis treatments in Belgium. Osteoporos Int 14:110–115. https://doi.org/10.1007/s00198-002-1321-z
Moshfegh AJ, Rhodes DG, Baer DJ, Murayi T, Clemens JC et al (2008) The US department of agriculture automated multiple-pass: method reduces bias in the collection of energy intakes. Am J Clin Nutr 88:324–332. https://doi.org/10.1093/ajcn/88.2.324
Tucker KL (2007) Assessment of usual dietary intake in population studies of gene- diet interaction. Nutr Metab Cardiovasc Dis 17:74–81. https://doi.org/10.1016/j.numecd.2006.07.010
Basiotis P, Welsh SO, Cronin FJ, Kelsay JL, Mertz W (1987) Number of days of food intake records required to estimate individual and group nutrient intakes with defined confidence. J Nutr 117:1638–1641. https://doi.org/10.1093/jn/117.9.1638
Willett WC, Howe GR, Kushi LH (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65:1220S-1228S. https://doi.org/10.1093/ajcn/65.4.1220S
Bozdongan H (1987) Model selection and Akaike’s information criterion (AIC): the general theory and its analytical extensions. Psychomet 52:345–370. https://doi.org/10.1007/BF02294361
Hair JF, Black WC, Babin BJ, Anderson RE, Tatham RL (2005) Multivariate data analysis, 6th edn. Pearson University Press, Upper Saddle River, NJ
R: A language and environment for statistical computing, R Core Team, R Foundation for Statistical Computing. 2021. Available in: https://www.R-project.org/. Accessed 26 Mar 2022
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Lawrence Erlbaum Associates, Hillsdale, NJ
Institute of Medicine (2005) Dietary reference intakes for Energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids (macronutrients). National Academy Press, Washington, DC
NDA, EFSA Scientific Panel (2015) Scientific opinion on the safety of caffeine. EFSA J 13:4102. https://doi.org/10.2903/j.efsa.2015.4102
Freuer D, Meisinger C, Linseisen J (2021) Causal relationship between dietary macronutrient composition and anthropometric measures: a bidirectional two-sample Mendelian randomization analysis. Clin Nutr 40:4120–4131. https://doi.org/10.1016/j.clnu.2021.01.047
Castellanos-Gutiérrez A, Sánchez-Pimienta TG, Carriquiry A, Costa THM, Ariza AC (2018) Higher dietary magnesium intake is associated with lower body mass index, waist circumference and serum glucose in Mexican adults. Nutr J 17:114. https://doi.org/10.1186/s12937-018-0422-2
Huang JH, Lu YF, Cheng FC, Lee JNY, Tsai LC (2012) Correlation of magnesium intake with metabolic parameters, depression and physical activity in elderly type 2 diabetes patients: a cross-sectional study. Nutr J 11:41. https://doi.org/10.1186/1475-2891-11-41
Lu L, Chen C, Yang K, Zhu J, Xun P, Shikany JM, He K (2020) Magnesium intake is inversely associated with risk of obesity in a 30-year prospective follow-up study among American young adults. Eur J Nutr 59:3745–3753. https://doi.org/10.1007/s00394-020-02206-3
Dibaba D, Xun P, He K (2014) Dietary magnesium intake is inversely associated with serum C-reactive protein levels: meta-analysis and systematic review. Eur J Clin Nutr 68:510–516. https://doi.org/10.1038/ejcn.2014.7
Piyathilake CJ, Badiga S, Alvarez RD, Partridge EE, Johanning GL (2013) A lower degree of PBMC L1 methylation is associated with excess body weight and higher HOMO-IR in the presence of lower concentrations of plasma folate. PLoS ONE 8:e54544. https://doi.org/10.1371/journal.pone.0054544
Ralston SH, Uitterlinden AG (2010) Genetics of osteoporosis. Endocr Rev 31:629–662. https://doi.org/10.1210/er.2009-0044
Reid IR (2010) Fat and bone. Arch Biochem Biophys 503:20–27. https://doi.org/10.1016/j.abb.2010.06.027
Felson DT, Zhang Y, Hannan MT, Anderson JJ (1993) Effects of weight and body mass index on bone mineral density in men and women: the Framingham study. J Bone Miner Res 8:567–573. https://doi.org/10.1002/jbmr.5650080507
Yang X, Sun LW, Liang M, Wang XN, Fan YB (2015) The response of wnt/ß-catenin signaling pathway in osteocytes under simulated microgravity. Microgravity Sci Technol 27:473–483. https://doi.org/10.1007/s12217-015-9439-8
Basso N, Heersche JN (2006) Effects of hind limb unloading and reloading on nitric oxide synthase expression and apoptosis of osteocytes and chondrocytes. Bone 39:807–814. https://doi.org/10.1016/j.bone.2006.04.014
Henry YM, Eastell R (2000) Ethnic and gender differences in bone mineral density and bone turnover in young adults: effect of bone size. Osteoporos Int 11:512–517. https://doi.org/10.1007/s001980070094
Zhu K, Briffa K, Smith A, Mountain J, Briggs AM, Lye S, Pennell C, Straker L, Walsh P (2014) Gender differences in the relationships between lean body mass, fat mass and peak bone mass in young adults. Osteopor Int 25:1563–1570. https://doi.org/10.1007/s00198-014-2665-x
Janicka A, Wren TA, Sanchez MM, Dorey F, Kim PS, Mittelman SD, Gilsanz V (2007) Fat mass is not beneficial to bone in adolescents and young adults. J Clin Endocrinol Metab 92:143–147. https://doi.org/10.1210/jc.2006-0794
Zhao L, Jiang H, Papasian CJ, Maulik D, Drees B, Hamilton J, Deng HW (2009) Correlation of obesity and osteoporosis: effect of fat mass on the determination of osteoporosis. J Bone Miner Res 23:17–29. https://doi.org/10.1359/jbmr.070813
Wang MC, Bachrach LK, Van Loan M, Hudes M, Flegal KM, Crawford PB (2005) The relative contributions of lean tissue mass and fat mass to bone density in young women. Bone 37:474–481. https://doi.org/10.1016/j.bone.2005.04.038
Douchi T, Yamamoto S, Kuwahata R, Oki T, Yamasaki H, Nagata Y (2000) Effect of non–weight-bearing body fat on bone mineral density before and after menopause. Obstet Gynecol 96:13–17. https://doi.org/10.1016/S0029-7844(00)00814-0
Hsu YH, Venners SA, Terwedow HA, Feng Y, Niu T et al (2006) Relation of body composition, fat mass, and serum lipids to osteoporotic fractures and bone mineral density in Chinese men and women. Am J Clin 83:146–154. https://doi.org/10.1093/ajcn/83.1.146
Khosla S (2001) Minireview: the OPG/RANKL/RANK system. Endocrinology 142:5050–5055. https://doi.org/10.1210/endo.142.12.8536
Cao JJ (2011) Effects of obesity on bone metabolism. J Orthop Surg Res 6:1–7. https://doi.org/10.1186/1749-799X-6-30
Kawai M, Devlin MJ, Rosen CJ (2009) Fat targets for skeletal health. Nat Rev Rheumatol 5:365–372. https://doi.org/10.1038/nrrheum.2009.102
Dirckx N, Moorer MC, Clemens TL, Riddle RC (2019) The role of osteoblasts in energy homeostasis. Nat Rev Endocrinol 15:651–665. https://doi.org/10.1038/s41574-019-0246-y
Zhu K, Hunter M, James A, Lim EM, Walsh JP (2015) Associations between body mass index, lean and fat body mass and bone mineral density in middle-aged Australians: the Busselton healthy ageing study. Bone 74:146–152. https://doi.org/10.1016/j.bone.2015.01.015
Acknowledgements
We thank Professor Alexandre S G Coelho for his assistance with statistical analyses.
Funding
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors. Acsa de Castro Santos and Anna Flavia Ferreira Passos were awarded scholarships from the Brazilian agencies ‘Fundação de Amparo à Pesquisa do Estado de Goiás’ (FAPEG) and ‘Coordenação de Aperfeiçoamento de Pessoal de Nível Superior’ (CAPES).
Author information
Authors and Affiliations
Contributions
Conceptualization, analysis, writing–original draft, and writing–review and editing [SMMCP]; methodology, investigation, analysis, writing-review [ACS and AFFP]; conceptualization, methodology, project administration, writing-original draft, writing-review and editing, and supervision [CC].
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflicts of interest.
Ethical approval
All the procedures were approved by the Ethics Committee of the Federal University of Goiás (protocol number: 2.772.022).
Consent to participant
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
de Carvalho Patriarca, S.M.M., de Castro Santos, A., Passos, A.F.F. et al. Bone mineral density and normal-weight obesity syndrome: beyond body weight and body mass index. J Bone Miner Metab 41, 512–521 (2023). https://doi.org/10.1007/s00774-023-01417-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-023-01417-y