Abstract
Introduction
A disintegrin and metalloproteinase 17 (Adam17), also known as TNFα-converting enzyme (Tace), is a membrane-anchored protein involved in shedding of TNF, IL-6 receptor, ligands of epidermal growth factor receptor (EGFR), and Notch receptor. This study aimed to examine the role of Adam17 in adult articular cartilage and osteoarthritis (OA) pathophysiology.
Materials and methods
Adam17 expression was examined in mouse knee joints during OA development. We analyzed OA development in tamoxifen-inducible chondrocyte-specific Adam17 knockout mice of a resection of the medial meniscus and medial collateral ligament (medial) model, destabilization of the medial meniscus (DMM) model, and aging model. We analyzed downstream pathways by in vitro experiments, and further performed intra-articular administration of an Adam17 inhibitor TAPI-0 for surgically induced mouse OA.
Results
Adam17 expression in mouse articular cartilage was increased by OA progression. In all models, Adam17 knockout mice showed ameliorated progression of articular cartilage degradation. Adam17 knockout decreased matrix metallopeptidase 13 (Mmp13) expression in both in vivo and in vitro experiments, whereas Adam17 activation by phorbol-12-myristate-13-acetate (PMA) increased Mmp13 and decreased aggrecan in mouse primary chondrocytes. Adam17 activation enhanced release of soluble TNF and transforming growth factor alpha, a representative EGF ligand, from mouse primary chondrocytes, while it did not change release of soluble IL-6 receptor or nuclear translocation of Notch1 intercellular domain. Intra-articular administration of the Adam17 inhibitor ameliorated OA progression.
Conclusions
This study demonstrates regulation of OA development by Adam17, involvement of EGFR and TNF pathways, and the possibility of Adam17 as a therapeutic target for OA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis (OA) is the most common joint disease caused by degeneration of articular cartilage. The pathogenesis of OA includes various factors such as aging, genetics, lifestyle, obesity, joint instability, and trauma [1]. Various kinds of signaling pathways that evoke degradation of articular cartilage have been revealed by molecular biology studies of murine OA models. Proinflammatory cytokines, such as tumor necrosis factor (TNF), interleukin (IL)-6, and IL-1β, are produced by synovial cells and chondrocytes, which exert catabolic effects on articular cartilage. Nuclear factor-kappa B (NF-κB) is one of the major signaling pathways responsible for immune reactions and inflammation. NF-κB is activated by these proinflammatory cytokines and excessive mechanical loading [2]. Hyperactivation of NF-κB causes cartilage degradation by inducing catabolic enzymes including matrix metallopeptidase 13 (Mmp13), a representative protease of type 2 collagen (Col2a1) [2,3,4].
In addition to these inflammation-related pathways, Notch signaling regulates articular chondrocytes. Notch is a transmembrane cell surface receptor that plays an essential role in cell fate determination during embryogenesis and postnatal development [5]. Notch signaling is initiated when Notch ligands on a cell surface bind to Notch receptors (Notch1–4) on adjacent cells. Upon ligand binding, the Notch receptor is cleaved by proteinases, such as a disintegrin and metalloproteinases (Adams), and subsequently by a γ-secretase complex. After these successive cleavages, the Notch intracellular domain (ICD) translocates into the nucleus and binds to the transcriptional effector Rbpj to form a transcriptional activator that induces target genes including the Hes (hairy and enhancer-of-split)/Hey (hairy/enhancer-of-split related with YRPW motif) family. We previously reported involvement of the Notch-Hes1 axis in OA pathogenesis [6, 7]. ICDs of Notch1 and Notch2 are detected in cell surface of chondrocytes in normal articular cartilage, but they are located in the nucleus in OA cartilage [6]. The Notch ICD induces Mmp13 in cultured chondrocytes and tamoxifen-inducible chondrocyte-specific knockout of Rbpj suppresses OA development [6].
Epidermal growth factor (EGF) signaling is one of candidate pathways responsible for OA pathogenesis. Many molecules have been identified as EGF ligands such as EGF, transforming growth factor alpha (TGFα), amphiregulin, heparin-binding EGF, betacellulin, epiregulin, epigen, and neuregulins 1–4 [8]. These ligands bind to EGF receptor (EGFR), a transmembrane tyrosine kinase, and other EGFR family members including erb-b2 receptor tyrosine kinase 2–4. EGFR family members are expressed in almost all cell types except hematopoietic cells and play roles in normal development and the physiology of various organs and tissues [8]. In articular cartilage and OA development, in vivo studies have shown contradictory results obtained by chondrocyte-specific deletion of Egfr [9, 10]. In vitro data have also indicated dual actions of EGFR signaling in articular cartilage. EGFR signaling promotes chondrocyte proliferation and lubrication of the articular surface, but it suppresses Sox9 expression and induces Mmp13 [8, 9]. Thus, EGFR signaling has various effects on articular cartilage.
These OA-related molecules and pathways suggest that Adam17, also known as TNFα-converting enzyme (Tace), is associated with OA pathogenesis. Adam family members are membrane-anchored proteins associated with various biological processes such as cell–cell and cell–matrix interactions. Adam17 is a protease that sheds the membrane-bound precursor of TNF. TNF is then released as a soluble factor. Similarly, IL-6 receptor (IL-6R) is released as soluble IL-6R by Adam17-mediated shedding [11]. When IL-6 binds to soluble IL-6R, it stimulates downstream pathways through subsequent binding to Gp130, an IL-6 signal transducer. Both TNF and IL-6 are responsible for the pathogenesis of rheumatoid arthritis (RA) and antibody drugs against them have been used as biological treatments for RA. Adam17 has been found in synovial tissues from RA patients and contributes to TNF production [12]. Some studies have shown that Adam17 inhibitors suppress RA [13]. In addition to RA, Adam17 is involved in inflammatory conditions of the airway, lungs, bowel, and blood vessels through other various substrates [14]. Adam17 is also a candidate proteinase for cleavage of Notch receptor [5], as well as Adam10. Furthermore, Adam17 is involved in EGFR signaling. All EGFR ligands are synthesized as membrane-bound precursors and released from the cell surface after cleavage by proteases including Adam17 [11]. Considering these interactions between Adam17 and OA-related signaling and molecules, Adam17 may positively regulate OA pathogenesis. However, Adam17 has not been investigated using murine models and there is no recent study that has focused on Adam17 in OA pathophysiology. In this study, we aimed to determine the roles of Adam17 in OA development using chondrocyte-specific KO mice. We further examined downstream signaling pathways that caused the phenotype of Adam17 KO joints.
Materials and methods
RNA isolation and quantitative reverse transcription-polymerase chain reaction (qRT-PCR)
Articular cartilage, synovium, meniscus, tendon, and bone were collected from 8-week-old WT male mice using a surgical microscope. RNA isolation and cDNA preparation were performed as previously described [15]. Briefly, total RNA was purified with an RNeasy Mini Kit (Qiagen, Hilden, Germany). One microgram of total RNA was reverse transcribed using ReverTraAce qPCR RT Master Mix with gDNA Remover (Toyobo, Osaka, Japan). Each polymerase chain reaction (PCR) contained 1 × THUNDERBIRD SYBR qPCR Mix (Toyobo), 0.3 mM specific primers, and 20 ng cDNA. The copy number was normalized to rodent total RNA (Thermo Fisher Scientific, Waltham, MA) with rodent glyceraldehyde-3-phosphate dehydrogenase used as an internal control. All reactions were run in triplicate. Primer sequences are shown in Supplementary Table 1.
Animals
All experimental protocols were approved by the Animal Care and Use Committee of The University of Tokyo. All animal care and experiments were carried out in accordance with the ARRIVE guidelines. We complied with all relevant ethical regulations. In each experiment, we compared the genotypes of littermates maintained in a C57BL/6 J background. Adam17-flox mice were generated as described previously [16]. Tamoxifen-inducible Col2a1-CreERT2 mice were generously provided by Professor Di Chen (Rush University, Chicago, IL) [17]. Col2a1-CreERT2;Adam17fl/fl male mice were used for OA experiments after tamoxifen injections, and Adam17fl/fl mice were used as controls. Mice were housed in plastic cages with free access to drinking water and a pellet-based diet. Primer sequences for genotyping are shown in Supplementary Table 2.
OA experiment
We used two models to surgically induce OA as follows. We destabilized the medial meniscus (DMM) for the DMM model [18] and resected the medial collateral ligament and medial meniscus for the medial model [19]. Tamoxifen (Sigma-Aldrich, St. Louis, MO; 100 μg/g body weight) was intraperitoneally injected into Col2a1-CreERT2;Adam17fl/fl and Adam17fl/fl male mice daily for 5 days at 7 and 11 weeks of age for medial and DMM models, respectively. For sham surgery, only the skin incision was performed. All surgical procedures were performed under general anesthesia using a surgical microscope. Medial and DMM model mice were analyzed at 8 and 12 weeks after surgery, respectively. For aging experiments, tamoxifen induction was performed for 5 days at 8 weeks, 6 months, and 12 months of age. The mice were bred under physiological conditions and sacrificed at 18 months. All mice were maintained under the same conditions (five mice per cage). The severity of OA was quantified by the Osteoarthritis Research Society International system [20], which was assessed by two observers who were blinded to the experimental groups. The medial compartment was assessed in the surgical models, and both compartments were assessed in the aging model.
Histological analyses
Tissue samples were fixed in 4% paraformaldehyde/phosphate-buffered saline (PBS) at 4 °C overnight. The samples were then decalcified in 10% ethylenediaminetetraacetic acid (pH 7.4) at 4 °C for 2 weeks, embedded in paraffin, and used to prepare 4-μm-thick sagittal sections. Safranin O staining was performed in accordance with standard protocols. For immunohistochemistry, sections were incubated with antibodies against Mmp13 (1:250, #18165-1-AP; Proteintech, Rosemont, IL), type 2 collagen (1:500, MAB8887; Merck Millipore, Burlington, MA), and aggrecan (Acan, 1:500, 13880-1-AP; Proteintech). Histological analyses were performed at least three times using two-to-three mice per genotype to confirm the results. The percentages of positive cells (Mmp13) and areas (Col2 and Acan) were measured by Aperio ImageScope (Leica biosystems, Nusloch, Germany). TUNEL staining was performed using an in situ Cell Death Detection Kit (Roche Applied Science, Penzberg, Germany). For quantification, safranin O and TUNEL staining images of sequential sections were merged and the percentages of positively stained cells in the safranin O-positive area were quantified using the BZ-X710 Analyzer software program (Keyence, Osaka, Japan).
Cell cultures
Primary articular chondrocytes were isolated from 5-day-old C57BL/6 J mice in accordance with a standard protocol [21] and then cultured in Dulbecco’s modified Eagle’s medium (DMEM)/F-12 with 10% FBS. The medium was changed every 2 or 3 days. To enhance Adam17 activity, cells were treated with phorbol-12-myristate-13-acetate (PMA) (Wako, Osaka, Japan), a strong stimulator of Adam17 [22]. Recombinant human (rh) TNF (PeproTech, NJ) and rhTGFα (Research and Diagnostic Systems Inc, Minneapolis, MN) were used at 10 and 200 ng/mL, respectively.
Enzyme-linked immunosorbent assays (ELISAs)
The concentrations of TNF, IL-6R, and TGFα in culture supernatants of primary chondrocytes were determined by a Mouse TNF ELISA Kit (Research and Diagnostic Systems Inc., Minneapolis, MN), Mouse TGFA ELISA Kit (LifeSpan Biosciences, WA), and Mouse IL-6R ELISA Kit (Research and Diagnostic Systems Inc; Minneapolis, MN), respectively, in accordance with the manufacturer’s protocols.
Western blotting
Cells were lysed in M-PER and NE-PER (Thermo Fisher Scientific) containing a COMPLETE protease inhibitor mixture (Roche Applied Science, Penzberg, Germany). Total protein was quantified using a BCA Protein Assay Kit (Pierce, Rockford, IL). Equal amounts of protein were subjected to sodium dodecyl sulfate-polyacrylamide gel electrophoresis using 7.5%–15% Tris–glycine gradient gels and then blotted onto polyvinylidene fluoride membranes (Bio-Rad Laboratories, Hercules, CA). After blocking with 5% dry skim milk, the membranes were incubated with primary antibodies against Egfr (1:1000, 4267S; Cell Signaling Technology, Danvers, MA), phosphorylated Egfr on Tyr1068 (p-Egfr, 1:1,000, 3777S; Cell Signaling Technology), Notch1 (1:1000, 20687-1-AP; Proteintech, Chicago, IL), GAPDH (1:10,000, HRP-60004; Proteintech), or Lamin B1 (1:10,000, ab16048; Abcam; Burlingame, CA) in Can Get Signal solution (Toyobo). The membranes were then incubated with a horseradish peroxidase-conjugated secondary antibody (Promega). Immunoreactive bands were visualized with ECL plus (GE Healthcare, Chicago, IL) in accordance with the manufacturer’s instructions. To quantify the bands, densitometric analysis was performed using an iBright CL 1000 (Thermo Fisher Scientific) with normalization to GAPDH.
Glycosaminoglycan release assay
The glycosaminoglycan release assay was performed as described previously [23]. Femoral heads were collected from 3-week-old WT mice. For Adam17 knockout, 100 µg/g body weight tamoxifen was injected intraperitoneally into 2-week-old Col2a1-CreERT2;Adam17fl/fl and Adam17fl/fl mice, and then, femoral heads were collected after 1 week. They were cultured for 3 days in DMEM with PMA or the vehicle control. The amount of glycosaminoglycans released into the medium was measured by a colorimetric assay using dimethyl methylene blue.
Intra-articular administration
We performed the medial model surgery on right knee joints of 8-week-old WT male mice, and performed intra-articular injection of TAPI-0 (PEPTIDE INSTITUTE, INC, Osaka, Japan), an Adam17 inhibitor. For intra-articular injections, various concentrations (50 nM, 500 nM, and 5 µM) of TAPI-0 were dissolved in saline. Ten microliters of TAPI-0 or saline as vehicle was injected into the intra-articular spaces of the mouse knee joints three times per a week from 1 to 8 weeks after surgery. Mice were analyzed at 8 weeks after surgery.
Statistical analyses
Graph Pad Prism v.8 (Graph Pad Software, San Diego, CA) was employed for statistical analyses. Data are expressed as the mean ± standard deviation (SD). Statistical significance was evaluated using the two-tailed unpaired Student’s t test for comparisons between two groups. For multiple comparisons, one-way ANOVA followed by Tukey’s or Dunnett’s post hoc test was used. P < 0.05 was considered to be significant.
Results
Expression of Adam17 in articular cartilage
We initially examined mRNA levels of Adam17 in various tissues around adult mouse knee joints. Adam17 was expressed in cartilage, synovium, subchondral bone, meniscus, and tendons at similar levels (Fig. 1a). We then analyzed Adam17 expression during OA development induced by the medial model surgery in mice. mRNA levels of Adam17 in articular cartilage were increased in accordance with OA progression, while that in the synovium was increased at 2 weeks after surgery and decreased thereafter (Fig. 1b). These data imply involvement of Adam17 in cartilage degradation during OA development.
Expression of Adam17 in the mouse articular joint. a mRNA level of Adam17 in knee joint tissues of 8-week-old mice. n = 3. b mRNA levels of Adam17 in articular cartilage and synovium in a time course during osteoarthritis (OA) development induced by medial surgery, resection of the medial meniscus, and medial collateral ligament. Five mice were sacrificed at 8 weeks of age without surgery (0 w), 20 mice were operated at 8 weeks of age, and five mice each were sacrificed at 2, 4, 6, and 8 weeks after surgery. Representative safranin O staining at each time point is shown in the upper panel. Scare bars, 100 µm. All data are expressed as the mean ± S.D. with dot plots. P values determined by the one-way ANOVA followed by Tukey’s or Dunnett’s post hoc test are shown. Graph Pad Prism v.8 was used for all statistical analyses
Decelerated development of OA in chondrocyte-specific Adam17 KO mice
To identify the role of Adam17 in articular cartilage, we performed in vivo loss-of-function analyses using Adam17-flox mice and Col2a1-CreERT2 mice. We first analyzed development of OA in Col2a1-CreERT2;Adam17fl/fl and Adam17fl/fl mice after DMM surgery (Fig. 2a). mRNA level of Adam17 in articular cartilage of Col2a1-CreERT2;Adam17fl/fl mice was approximately decreased by 60% compared with that of Adam17fl/fl mice (Supplementary Fig. 1). Development of OA was significantly suppressed in Adam17 knockout mice (Fig. 2a). Suppression of OA development in the knockout mice was confirmed in medial and aging models (Fig. 2a). In contrast, sham-operated mice showed no obvious change in articular cartilage (Supplementary Fig. 2). Because articular cartilage was markedly degenerated in medial model mice, we further performed histological examinations. Chondrocyte apoptosis determined by TUNEL staining was significantly suppressed in DMM and medial models of Col2a1-CreERT2;Adam17fl/fl mice (Supplementary Fig. 3). We next examined expression of marker proteins in articular cartilage of both mice. Expression of Mmp13 was significantly downregulated by Adam17 knockout (Fig. 2b, c). Type 2 collagen was not changed obviously, while Acan, a cartilage matrix protein mainly produced by chondrocytes in middle and deep layers, was significantly increased by Adam17 knockout (Fig. 2b, c).
Development of OA in chondrocyte-specific Adam17 knockout mice. a Development of OA in Adam17fl/fl (Cntl) and Col2a1-CreERT2;Adam17fl/fl (KO) mice by destabilization of the medial meniscus (DMM model), resection of the medial meniscus and medial collateral ligament (medial model), and aging. Left, middle, and right panels indicate time courses of the protocols, representative safranin O staining, and quantification of OA development by Osteoarthritis Research Society International (OARSI) scoring, respectively. The inset boxes in safranin O staining indicate higher magnification images. Scale bars, 100 µm. Immunohistochemistry of Mmp13, type 2 collagen (Col2), and Acan in Cntl and KO cartilage of the DMM model (b) or the medial model (c). Scale bars, 50 µm. Right panels indicate the rates of positive areas in the cartilage area (n = 5), determined by the BZ-X710 Analyzer software. All data are expressed as the mean ± SD with dot plots. P values determined by the two-tailed unpaired Student’s t test are shown. Graph Pad Prism v.8 was used for all statistical analyses
Alteration of marker gene expression by gain- and loss-of-function of Adam17
We next examined the effects of Adam17 on expression of cartilage marker genes. We first obtained primary chondrocytes from Col2a1-CreERT2;Adam17fl/fl and Adam17fl/fl neonates and then analyzed the mRNA levels of marker genes. Although the mRNA level of Adam17 in knockout chondrocytes was about half of that in the control chondrocytes, the Mmp13 expression level in the Col2a1-CreERT2;Adam17fl/fl group was significantly lower than that in the Adam17fl/fl group (Fig. 3a). Expression of Col2a1 and Acan was not different obviously in both groups. When WT primary chondrocytes were treated with PMA, a stimulator of Adam17-mediated shedding, Mmp13 expression was increased and Acan expression was decreased (Fig. 3b). A decrease in Col2a1 expression induced by PMA treatment was not significant (Fig. 3b). We further applied PMA to organ culture of mouse femoral heads. The PMA treatment significantly enhanced glycosaminoglycan release into the medium from femoral heads obtained from 3-week-old Cntl mice (Fig. 3c). The enhancement of glycosaminoglycan release by PMA treatment was lower in Adam17 knockout femoral heads (Fig. 3c). Alterations of Mmp13 and Acan expression induced by PMA treatment were also restored by Adam17 knockout (Fig. 3d). The mRNA level of Adam17 was not changed by PMA treatment, which indicated that the activation of Adam17 by PMA was not dependent on its expression level (Fig. 3d).
Alteration of marker gene expression by gain- and loss-of-function of Adam17. a mRNA levels of Mmp13, Col2a1, Acan, and Adam17 in Cntl and KO primary chondrocytes. b mRNA levels of Mmp13, Col2a1, and Acan in WT primary chondrocytes treated with 50 nM PMA or vehicle for 1 day. c Amount of glycosaminoglycans released into the culture medium from Cntl and KO femoral heads treated with 50 nM PMA or vehicle for 3 days. d mRNA levels of Mmp13, Col2a1, Acan, and Adam17 in Cntl and KO femoral heads treated with 50 nM PMA or vehicle for 3 days. All data are expressed as the mean ± SD with dot plots (n = 3). P values determined by the two-tailed unpaired Student’s t test (a, b) or one-way ANOVA followed by Tukey’s or Dunnett’s post hoc test (c, d) are shown. Graph Pad Prism v.8 was used for all statistical analyses
Increases of TNF and TGFα by Adam17-mediated shedding
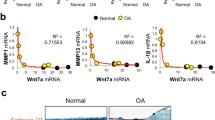
We next investigated downstream molecules of Adam17 in articular chondrocytes. Among EGFR ligands, TGFα was the most highly expressed in chondrocytes (Fig. 4a). When we examined release of Adam17 substrate proteins from primary chondrocytes into the culture medium under PMA stimulation, TNF and TGFα levels were increased significantly (Fig. 4b). The protein level of soluble IL-6R was lower than those of TNF and TGFα, and not increased by PMA treatment (Fig. 4b). Translocation of the Notch1 ICD was examined by western blotting. The Notch1 ICD was detected in the cytosol of primary chondrocytes treated with the vehicle, but it was not increased in the nucleus by PMA treatment (Fig. 4c). Phosphorylation of Egfr by PMA treatment was confirmed by western blotting (Fig. 4d). We examined the RNA levels of these substrates in the articular cartilage and synovium during mouse OA development, which were the same samples used in Fig. 1b. Expression of Egf, Tgfa, Tnf, and Notch1 in the articular cartilage was increased at 8 weeks, while that of Il6r was unchanged (Supplementary Fig. 4a). Expression of Egfr, Tgfa, and Tnf in the synovium was increased at 2 weeks after surgery and then decreased thereafter (Supplementary Fig. 4b). Notch1 and Il6r expression was not changed in the synovium (Supplementary Fig. 4b). We further treated primary chondrocytes with rhTNF or rhTGFα. Similar to PMA, rhTNF and rhTGFα treatments increased Mmp13 expression and decreased Col2a1 and Acan expression (Fig. 4e).
Downstream pathways of Adam17 in chondrocytes. a mRNA levels of EGFR ligands in the articular cartilage of 8-week-old mice. b Protein levels of Tnf, Tgfa, and Il6r in the culture supernatant of mouse primary chondrocytes after 24 h of treatment with PMA or vehicle. c Western blotting of Notch1 in cytosolic and nuclear extracts of mouse primary chondrocytes treated with 50 nM PMA or vehicle. Gapdh and Lamin B1 were used as controls for cytosolic and nuclear proteins, respectively. Right panels show relative protein levels of Notch1. d Western blotting of phosphorylated Egfr (p-Egfr), Egfr, and Gapdh in cell lysates of primary chondrocytes treated with 50 nM PMA or vehicle. Right panels show relative protein levels of p-Egfr and Egfr. e mRNA levels of Mmp13, Col2a1, and Acan in mouse primary chondrocytes treated with 10 ng/ml rhTNF, 200 ng/ml rhTGFα, or respective vehicles. All data are expressed as the mean ± SD with dot plots (n = 3–4). P values determined by the two-tailed unpaired Student’s t test are shown. Graph Pad Prism v.8 was used for all statistical analyses
Intra-articular administration of an Adam17 inhibitor ameliorates development of OA
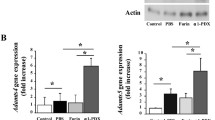
We finally examined the possibility of Adam17 as a therapeutic target of OA. We employed TAPI-0 as an Adam17 inhibitor. TAPI-0 blocks the shedding activity of Adam17 and inhibits the release of TNF and IL-6R from cells [24, 25]. We confirmed the inhibitory effects of TAPI-0 against Adam17 by ex vivo experiments. The increase in glycosaminoglycan release and alterations of Mmp13, Col2a1, and Acan expression were significantly attenuated by TAPI-0 treatment (Supplementary Fig. 5). We next prepared OA model mice by medial surgery and performed intra-articular injection of TAPI-0 (Fig. 5a). The OARSI score of the 500 nM TAPI-0 group was the lowest among all groups (Fig. 5a). Chondrocyte apoptosis and Mmp13 expression were significantly suppressed by TAPI-0 treatment (Supplementary Fig. 6). Expression of type 2 collagen and Acan was not changed obviously (Fig. 5b).
Effects of intra-articular administration of the Adam17 inhibitor. a Development of surgically induced OA in WT mice that received intra-articular injection of TAPI-0. Upper panels show time courses of the protocols and quantification of OA development by OARSI scoring. Lower panels show representative safranin O staining of each experimental group. Scale bar, 100 µm. b Immunohistochemistry of Mmp13, Col2, and Acan in articular cartilage of 500 nM TAPI-0 and vehicle groups. Scale bars, 50 µm. Right panels show the rates of positive areas in the articular area (n = 5), determined by the BZ-X710 Analyzer software. P values determined by Tukey’s or Dunnett’s post hoc test (a) or the two-tailed unpaired Student’s t test (b) are shown. Graph Pad Prism v.8 was used for all statistical analyses
Discussion
In this study, we found an increase of Adam17 expression in articular cartilage during mouse OA development. Chondrocyte-specific Adam17 knockout mice had suppressed degradation of articular cartilage in two kinds of surgical OA models and the aging model. Mmp13 expression was suppressed in Adam17 knockout cartilage. In organ culture of mouse femoral heads, Adam17 stimulation by PMA treatment increased Mmp13 expression and decreased Col2a1 and Acan expression. Among the major substrates of Adam17, TNF and TGFα, the most abundantly expressed EGFR ligands, were increased in the culture medium of mouse primary chondrocytes by PMA treatment. Moreover, release of soluble IL-6R was not enhanced and intranuclear translocation of the Notch1 ICD was not changed by PMA treatment. Phosphorylation of Egfr was enhanced by PMA treatment. Intra-articular administration of the Adam17 inhibitor suppressed development of surgically induced OA. We have summarized the present findings as a schematic diagram (Fig. 6).
Similar to the evidence in RA pathophysiology, the present data indicate the contribution of Adam17 to OA progression. Considering that many Adam17 substrates are involved in synovitis and cartilage degeneration, it is reasonable that in vivo loss-of-function of Adam17 leads to suppression of OA development induced by joint instability or aging. Moreover, we could not clearly reveal the Adam17 downstream pathways responsible for cartilage degeneration in murine OA models, because shedding of Adam17 substrates could not be directly evaluated by histological examination. Considering that in vitro experiments are somewhat dependent on context, IL-6R may be partially involved in OA progression mediated by Adam17, although release of Il6r into the medium was not increased by PMA treatment (Fig. 4b). As another limitation, we obtained the gain-of-function data of Adam17 by only using PMA. PMA activates shedding activity of Adam17 through protein kinase C [26]. Although the results of the PMA experiments were consistent, these data may have included some effects that were not specific to Adam17. Furthermore, various Adam17 substrates other than the four molecules may be associated with OA development as downstream of Adam17. Despite these limitations, we did not observe harmful effects in joints by chondrocyte-specific Adam17 knockout. Thus, Adam17 may be a potent target to modify OA development.
Despite the present data, the roles of EGFR signaling are still controversial. Chondrocyte-specific deletion of Egfr using Col2a1-Cre and Egfr-flox mice reduces the number of chondrocytes in the superficial zone of articular cartilage and enhances OA progression by surgical induction [9]. Zhang et al. showed enhancement of OA development in heterozygous mice for Wa5, a dominant negative allele of Egfr, and by oral administration of gefitinib, an EGFR inhibitor [27]. Mmp13 expression and apoptosis are enhanced in both models [27]. Jia et al. also showed that Col2a1-Cre;EgfrWa5/flox mice displayed abnormal articular cartilage development and consequently enhanced cartilage degeneration [9]. However, chondrocyte-specific deletion of Egfr in tamoxifen-inducible Col2a1-CreERT2 and Egfr-flox adult mice suppresses OA development by surgical induction [10]. This previous study employed similar methods to the present study, namely chondrocyte-specific knockout of target genes in adulthood using Col2a1-CreERT2 and OA induction by the DMM model [10]. Similar to the present data, positive cell rates for Acan and Mmp13 were increased and decreased by Egfr knockout, respectively [10]. These data indicate that the EGFR signaling pathway has various roles in articular cartilage, which may be dependent on the context.
In the present study, TGFα was the most highly expressed among the EGFR ligands in mouse primary chondrocytes and released into the medium by PMA treatment (Fig. 4a, b). TGFα increased Mmp13 expression, and suppresses expression of Col2a1 and Acan in chondrocytes [10, 28], which is similar to the present data of PMA treatment. TGFα protein was increased in rat experimental OA models, and TGFA mRNA level in articular cartilage was increased in half of human OA patients [28]. Tgfa null mice have decelerated OA development accompanied by decreased expression of Mmp13 in articular cartilage [29]. A recent genome-wide association study of OA identified a susceptibility nucleotide polymorphism in an intron of the TGFA gene [30]. Although we did not examine the roles of Adam17 and EGFR using human samples in the present study, Adam17 may be involved in human OA pathogenesis upstream of TGFα. In the previous studies, Col2a1-Cre;Adam17-flox, Col2a1-Cre;Egfr-flox, and Tgfa knockout mice displayed similar phenotypes in skeletal formation, i.e., shorter long bones with an elongated hypertrophic chondrocyte zone [31,32,33]. The Adam17-TGFα-EGFR axis might play roles in both the endochondral ossification process during skeletal development and OA progression.
Previous studies have indicated that Adam17 and Adam10 are involved in cleavage of the Notch receptor [34]. In vitro experiments have shown cleavage of Notch1 at the S2 site by Adam17 [35]. However, the phenotype of Adam17 KO mice does not support this association. Notch1-deficient embryos die before embryonic day (E) 11.5 day [36], and Rbpj-deficient embryos, in which canonical Notch signaling is completely inhibited, show a more severe phenotype [37]. Despite the lethality of these mice in mid-gestation, Adam17 knockout mice can survive until E17.5 to the first day after birth [38]. In contrast, Adam10-deficient embryos die at E9.5 and expression of Notch target genes is suppressed [39]. These previous data of knockout mice indicate that Adam10, but not Adam17, is associated with Notch cleavage in vivo, which is consistent with the findings of the present study.
In conclusion, Adam17 in articular chondrocytes regulates OA development. TNF and EGFR signaling pathways are potent candidates for downstream mediators of Adam17. Intra-articular administration of an Adam17 inhibitor suppresses development of experimental OA. The present data may contribute to further understanding of OA pathophysiology and the development of novel therapeutics.
Data availability
All data generated or analyzed during this study are included in this published article.
References
Palazzo C, Nguyen C, Lefevre-Colau MM, Rannou F, Poiraudeau S (2016) Risk factors and burden of osteoarthritis. Ann Phys Rehabil Med 59:134–138
Chang SH, Mori D, Kobayashi H, Mori Y, Nakamoto H, Okada K, Taniguchi Y, Sugita S, Yano F, Chung UI, Kim-Kaneyama JR, Yanagita M, Economides A, Canalis E, Chen D, Tanaka S, Saito T (2019) Excessive mechanical loading promotes osteoarthritis through the gremlin-1-NF-kappaB pathway. Nat Commun 10:1442
Saito T, Fukai A, Mabuchi A, Ikeda T, Yano F, Ohba S, Nishida N, Akune T, Yoshimura N, Nakagawa T, Nakamura K, Tokunaga K, Chung UI, Kawaguchi H (2010) Transcriptional regulation of endochondral ossification by HIF-2alpha during skeletal growth and osteoarthritis development. Nat Med 16:678–686
Kobayashi H, Chang SH, Mori D, Itoh S, Hirata M, Hosaka Y, Taniguchi Y, Okada K, Mori Y, Yano F, Chung UI, Akiyama H, Kawaguchi H, Tanaka S, Saito T (2016) Biphasic regulation of chondrocytes by Rela through induction of anti-apoptotic and catabolic target genes. Nat Commun 7:13336
Kopan R, Ilagan MX (2009) The canonical Notch signaling pathway: unfolding the activation mechanism. Cell 137:216–233
Hosaka Y, Saito T, Sugita S, Hikata T, Kobayashi H, Fukai A, Taniguchi Y, Hirata M, Akiyama H, Chung UI, Kawaguchi H (2013) Notch signaling in chondrocytes modulates endochondral ossification and osteoarthritis development. Proc Natl Acad Sci USA 110:1875–1880
Sugita S, Hosaka Y, Okada K, Mori D, Yano F et al (2015) Transcription factor Hes1 modulates osteoarthritis development in cooperation with calcium/calmodulin-dependent protein kinase 2. Proc Natl Acad Sci USA 112:3080–3085
Qin L, Beier F (2019) EGFR signaling: friend or foe for cartilage? JBMR Plus 3:e10177
Jia H, Ma X, Tong W, Doyran B, Sun Z, Wang L, Zhang X, Zhou Y, Badar F, Chandra A, Lu XL, Xia Y, Han L, Enomoto-Iwamoto M, Qin L (2016) EGFR signaling is critical for maintaining the superficial layer of articular cartilage and preventing osteoarthritis initiation. Proc Natl Acad Sci USA 113:14360–14365
Sun H, Wu Y, Pan Z, Yu D, Chen P, Zhang X, Wu H, Zhang X, An C, Chen Y, Qin T, Lei X, Yuan C, Zhang S, Zou W, Ouyang H (2018) Gefitinib for epidermal growth factor receptor activated osteoarthritis subpopulation treatment. EBioMedicine 32:223–233
Lisi S, D’Amore M, Sisto M (2014) ADAM17 at the interface between inflammation and autoimmunity. Immunol Lett 162:159–169
Ohta S, Harigai M, Tanaka M, Kawaguchi Y, Sugiura T, Takagi K, Fukasawa C, Hara M, Kamatani N (2001) Tumor necrosis factor-alpha (TNF-alpha) converting enzyme contributes to production of TNF-alpha in synovial tissues from patients with rheumatoid arthritis. J Rheumatol 28:1756–1763
Murumkar PR, Ghuge RB, Chauhan M, Barot RR, Sorathiya S, Choudhary KM, Joshi KD, Yadav MR (2020) Recent developments and strategies for the discovery of TACE inhibitors. Expert Opin Drug Discov 15:779–801
Moss ML, Minond D (2017) Recent advances in ADAM17 research: a promising target for cancer and inflammation. Mediators Inflamm 2017:9673537
Nakamoto H, Katanosaka Y, Chijimatsu R, Mori D, Xuan F, Yano F, Omata Y, Maenohara Y, Murahashi Y, Kawaguchi K, Yamagami R, Inui H, Taketomi S, Taniguchi Y, Kanagawa M, Naruse K, Tanaka S, Saito T (2021) Involvement of transient receptor potential Vanilloid channel 2 in the induction of lubricin and suppression of ectopic endochondral ossification in mouse articular cartilage. Arthritis Rheumatol 73:1441–1450
Horiuchi K, Kimura T, Miyamoto T, Takaishi H, Okada Y, Toyama Y, Blobel CP (2007) Cutting edge: TNF-alpha-converting enzyme (TACE/ADAM17) inactivation in mouse myeloid cells prevents lethality from endotoxin shock. J Immunol 179:2686–2689
Zhu M, Tang D, Wu Q, Hao S, Chen M, Xie C, Rosier RN, O’Keefe RJ, Zuscik M, Chen D (2009) Activation of β-catenin signaling in articular chondrocytes leads to osteoarthritis-like phenotype in adult β-catenin conditional activation mice. J Bone Miner Res 24:12–21
Glasson SS, Blanchet TJ, Morris EA (2007) The surgical destabilization of the medial meniscus (DMM) model of osteoarthritis in the 129/SvEv mouse. Osteoarthritis Cartilage 15:1061–1069
Kamekura S, Hoshi K, Shimoaka T, Chung U, Chikuda H, Yamada T, Uchida M, Ogata N, Seichi A, Nakamura K, Kawaguchi H (2005) Osteoarthritis development in novel experimental mouse models induced by knee joint instability. Osteoarthritis Cartilage 13:632–641
Glasson SS, Chambers MG, Van Den Berg WB, Little CB (2010) The OARSI histopathology initiative - recommendations for histological assessments of osteoarthritis in the mouse. Osteoarthritis Cartilage 18:S17-23
Gosset M, Berenbaum F, Thirion S, Jacques C (2008) Primary culture and phenotyping of murine chondrocytes. Nat Protoc 3:1253–1260
Shao MX, Ueki IF, Nadel JA (2003) Tumor necrosis factor alpha-converting enzyme mediates MUC5AC mucin expression in cultured human airway epithelial cells. Proc Natl Acad Sci USA 100:11618–11623
Stanton H, Golub SB, Rogerson FM, Last K, Little CB, Fosang AJ (2011) Investigating ADAMTS-mediated aggrecanolysis in mouse cartilage. Nat Protoc 6:388–404
Mohler KM, Sleath PR, Fitzner JN, Cerretti DP, Alderson M et al (1994) Protection against a lethal dose of endotoxin by an inhibitor of tumour necrosis factor processing. Nature 370:218–220
Mullberg J, Durie FH, Otten-Evans C, Alderson MR, Rose-John S, Cosman D, Black RA, Mohler KM (1995) A metalloprotease inhibitor blocks shedding of the IL-6 receptor and the p60 TNF receptor. J Immunol 155:5198–5205
Doedens JR, Black RA (2000) Stimulation-induced down-regulation of tumor necrosis factor-alpha converting enzyme. J Biol Chem 275:14598–14607
Zhang X, Zhu J, Liu F, Li Y, Chandra A, Levin LS, Beier F, Enomoto-Iwamoto M, Qin L (2014) Reduced EGFR signaling enhances cartilage destruction in a mouse osteoarthritis model. Bone Res 2:14015
Appleton CT, Usmani SE, Bernier SM, Aigner T, Beier F (2007) Transforming growth factor alpha suppression of articular chondrocyte phenotype and Sox9 expression in a rat model of osteoarthritis. Arthritis Rheum 56:3693–3705
Usmani SE, Ulici V, Pest MA, Hill TL, Welch ID, Beier F (2016) Context-specific protection of TGFalpha null mice from osteoarthritis. Sci Rep 6:30434
Zengini E, Hatzikotoulas K, Tachmazidou I, Steinberg J, Hartwig FP et al (2018) Genome-wide analyses using UK Biobank data provide insights into the genetic architecture of osteoarthritis. Nat Genet 50:549–558
Saito K, Horiuchi K, Kimura T, Mizuno S, Yoda M, Morioka H, Akiyama H, Threadgill D, Okada Y, Toyama Y, Sato K (2013) Conditional inactivation of TNFalpha-converting enzyme in chondrocytes results in an elongated growth plate and shorter long bones. PLoS ONE 8:e54853
Hall KC, Hill D, Otero M, Plumb DA, Froemel D, Dragomir CL, Maretzky T, Boskey A, Crawford HC, Selleri L, Goldring MB, Blobel CP (2013) ADAM17 controls endochondral ossification by regulating terminal differentiation of chondrocytes. Mol Cell Biol 33:3077–3090
Usmani SE, Pest MA, Kim G, Ohora SN, Qin L, Beier F (2012) Transforming growth factor alpha controls the transition from hypertrophic cartilage to bone during endochondral bone growth. Bone 51:131–141
Bozkulak EC, Weinmaster G (2009) Selective use of ADAM10 and ADAM17 in activation of Notch1 signaling. Mol Cell Biol 29:5679–5695
Brou C, Logeat F, Gupta N, Bessia C, LeBail O, Doedens JR, Cumano A, Roux P, Black RA, Israël A (2000) A novel proteolytic cleavage involved in Notch signaling: the role of the disintegrin-metalloprotease TACE. Mol Cell 5:207–216
Swiatek PJ, Lindsell CE, del Amo FF, Weinmaster G, Gridley T (1994) Notch1 is essential for postimplantation development in mice. Genes Dev 8:707–719
Oka C, Nakano T, Wakeham A, de la Pompa JL, Mori C, Sakai T, Okazaki S, Kawaichi M, Shiota K, Mak TW, Honjo T (1995) Disruption of the mouse RBP-J kappa gene results in early embryonic death. Development 121:3291–3301
Peschon JJ, Torrance DS, Stocking KL, Glaccum MB, Otten C, Willis CR, Charrier K, Morrissey PJ, Ware CB, Mohler KM (1998) TNF receptor-deficient mice reveal divergent roles for p55 and p75 in several models of inflammation. J Immunol 160:943–952
Hartmann D, de Strooper B, Serneels L, Craessaerts K, Herreman A, Annaert W, Umans L, Lübke T, Lena Illert A, von Figura K, Saftig P (2002) The disintegrin/metalloprotease ADAM 10 is essential for Notch signalling but not for alpha-secretase activity in fibroblasts. Hum Mol Genet 11:2615–2624
Acknowledgements
We thank Dr. Di Chen for generously providing Col2a1-CreERT2 mice. We thank J. Sugita, K. Kaneko, and R. Homma for technical assistance. We also thank Mitchell Arico from Edanz Group (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
This work was supported by JSPS KAKENHI Grant Numbers 20H03799, 19H05654, 19H05565, 19K09641, 18KK0254, 17H04310, and 26462285.
Author information
Authors and Affiliations
Contributions
All authors have read and approved the final manuscript. TK, KH, and TS conceived and designed the study. TK, RC, DM, and KN performed the experiment. TK, RC, FY, HI, TM, ST, and TS analyzed and interpreted the data. TK and TS wrote the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Kaneko, T., Horiuchi, K., Chijimatsu, R. et al. Regulation of osteoarthritis development by ADAM17/Tace in articular cartilage. J Bone Miner Metab 40, 196–207 (2022). https://doi.org/10.1007/s00774-021-01278-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-021-01278-3