Abstract
We aimed to investigate the efficacy of denosumab for rheumatoid arthritis (RA). This study enrolled 70 RA patients who received denosumab 60 mg subcutaneous injection at baseline and at 6 months. Bone mineral densities (BMD) of the lumbar spine, total hip, femoral neck, and hand were measured by dual energy X-ray absorptiometry. Changes in total modified Sharp score (mTSS), erosion (EN) score, and joint space narrowing score at baseline from 12 months before and at 12 months from baseline. The mean values of BMD of the lumbar spine, total hip, femoral neck, and hand significantly increased by 7.3, 4.7, 3.9, and 5.4%, respectively, at 12 months. At 12 months from baseline, there were significant decreases in the values of mTSS (1.13 vs. 0.59; p = 0.002) and EN score (0.40 vs. 0.07; p < 0.001), compared with the values at baseline from 12 months before. The existing combined modality therapy with denosumab might be effective for osteoporosis and joint destruction in patients with RA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is an inflammatory disease that causes pain, swelling, stiffness, and loss of function in joints throughout the body. This autoimmune disease mainly results in progressive joint destruction and deformity with varying degrees of diminished quality of life, as well as limitations in daily activities and work [1,2,3,4]. Increased osteoclast activity in RA contributes to local and systemic abnormalities of bone remodeling, including bone loss and bone erosion [5]. Bone loss is thought to be mediated by osteoclast and the receptor activator of nuclear factor kappa β ligand (RANKL) pathway, which is a key driver of bone destruction in RA. RANKL has been identified as an essential cytokine for differentiation, function, formation, activation, and survival of osteoclasts [6,7,8]. The known effect of RA is increase in radiographic scores of joint destruction, including joint space narrowing and erosion [9, 10].
Denosumab is a fully human monoclonal antibody that specifically and avidly binds to human RANKL, leading to diminished survival and activation of osteoclasts to inhibit bone resorption [7, 11]. The efficacy and safety of denosumab were investigated in a randomized, double-blind, placebo-controlled, phase II clinical trial of RA patients on methotrexate in the United States. This study showed that after 12 months of administration of both 60 and 180-mg doses of subcutaneous denosumab every 6 months, the modified Sharp erosion (EN) score significantly decreased and the bone mineral density (BMD) of the lumbar spine, total hip, and femoral neck significantly increased [12]. Likewise, in Japan, a randomized, double-blind, placebo-controlled, phase II clinical trial of patients with RA on methotrexate treatment was performed [13]. After 12 months of administration of 60-mg denosumab every 6, 3, and 2 months, the EN score and BMD of the lumbar spine and total hip significantly improved in all groups. However, in actual practice, treatment of patients with RA continues for a long period. The objectives of this study were to verify the efficacy of denosumab on BMD at 12 months and joint destruction at baseline from 12 months before, and at 12 months from baseline.
Materials and methods
Study design
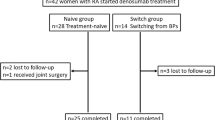
This study investigated the clinical course and background variables of RA patients who fulfilled the American College of Rheumatology (ACR) classification criteria (1987) and the ACR/European League against Rheumatism criteria [14, 15]. This study enrolled 70 patients who were treated with disease-modifying antirheumatic drugs (DMARDs) for RA for more than 2 years. The patients included postmenopausal women with a T score ≤−2.0 at the lumbar spine or total hip by dual energy X-ray absorptiometry (DXA) or a previous fragility fracture. The patients were administered denosumab 60 mg subcutaneous injection (SC) at baseline and at 6 months. All patients were instructed to take daily 0.5–0.75-mg doses of eldecalcitol, an active vitamin D3 analog. Informed consent was obtained from the patients after explaining the study protocol. This study was approved by the independent ethics committee of Kamagaya General Hospital and was undertaken following the principles of the Declaration of Helsinki.
Study assessments
The BMDs of the lumbar spine, total hip, femoral neck, and hand were measured by DXA (PROGIDY system; GE Healthcare, Madison, WI, USA) at baseline and at 3, 6, and 12 months. Vertebral fractures were evaluated by plain X-ray of the thoracic and lumbar spines at 12 months before from baseline, baseline and 12 months. Clinical assessments recorded at 12 months before from baseline, baseline, 3, 6, and 12 months included C reactive protein (CRP), erythrocyte sedimentation rate (ESR), matrix metalloproteinase-3 (MMP-3), disease activity score in 28 joints (DAS28)-CRP, DSA28-ESR, and simplified disease activity index (SDAI). The bone turnover makers of N-propeptide of type I collagen (PINP) and tartrate-resistant acid phosphatase-5b (TRACP-5b) were recorded at baseline and at 3, 6, and 12 months. The radiographs were evaluated by the van der Heijde-modified Sharp method at 12 months before from baseline, baseline, and 12 months [16].
The primary endpoint was percent change from baseline in BMD of the lumbar spine, total hip, femoral neck, and hand at 3, 6, and 12 months. The secondary endpoints were changes in van der Heijde-modified total sharp score (mTSS), EN score, and modified Sharp joint space narrowing (JSN) score at 12 months before from baseline and at 12 months from baseline. The rheumatologist who was blinded to the patient information read the digitized X-ray. Efficacy analysis included all patients who received at least one dose of denosumab and who had baseline plus at least one post-baseline evaluation. The demographic characteristics were evaluated by analysis of variance and the Bonferroni method. The percent changes at 3, 6, and 12 months from baseline in BMD and bone turnover makers were analyzed by the paired t test. Multivariate logistic regression analysis was performed to compare between patients with increase of 3% and more from baseline and patients with increase of less than 3% from baseline in BMD for determine independent predictors of increase of 3% and more from baseline in BMD at lumbar spine, total hip, femoral neck and hand. Multivariate logistic regression analysis was performed using the variables with p value <0.1 from the univariate logistic regression analysis. The changes in mTSS, JSN score, and EN score at baseline from 12 months before and at 12 months from baseline were analyzed by paired Student’s t test. At 12 months, the comparison between patients with and without structural remission was performed for baseline factors that may be related to joint destruction [age, rheumatoid factor, anti-cyclic citrullinated peptide antibody, disease duration, biological DMARDs (bDMARDs), methotrexate (MTX), corticosteroid, CRP, ESR, matrix metalloproteinase-3, DAS28-CRP, DAS28-ESR and SDAI] using the Wilcoxon rank sum test and Fisher’s exact test. Significance was established at p < 0.05.
Results
All 70 RA patients enrolled in this study were Japanese women (Table 1). The changes in the number of patients on bDMARDs, MTX, and corticosteroid, as well as the changes in the dosage of MTX and corticosteroid, were not significant. On the other hand, the value of DAS28-CRP at 12 months before from baseline was significantly higher than those at baseline and 12 months.
At 3, 6, and 12 months, the percent changes from baseline in the BMD values were 2.7 ± 4.0% (p < 0.001), 4.8 ± 5.8% (p < 0.001), and 7.3 ± 8.3% (p < 0.001), respectively, for the lumbar spine; 1.8 ± 7.0% (p = 0.056), 3.9 ± 5.9% (p < 0.001), and 4.7 ± 5.5% (p < 0.001), respectively, for the total hip; 1.8 ± 8.9% (p = 0.127), 2.7 ± 9.1% (p < 0.05), and 3.9 ± 8.3% (p < 0.001), respectively, for the femoral neck; and 2.4 ± 7.2% (p < 0.05), 4.4 ± 11.3% (p < 0.01), and 5.4 ± 10.5% (p < 0.001), respectively, for the hand (Fig. 1). The percent change from baseline in P1NP were −49.2 ± 22.7% (p < 0.001), −50.3 ± 28.8% (p < 0.001), and −42.8 ± 42.2% (p < 0.001) at 3, 6, and 12 months, respectively. The percent change from baseline in TRACP-5b were −48.5 ± 26.5% (p < 0.001), −48.8 ± 25.4% (p < 0.001), and −45.8 ± 33.4% (p < 0.001) at 3, 6, and 12 months, respectively. The incidence of new vertebral fractures on plain X-ray of the thoracic and lumbar spines was 12 patients at baseline from 12 months before and five patients at 12 months from baseline. The relative reduction rate of new vertebral fractures was 58.3%.
The predictors of efficacy in increase of BMD at the lumbar spine were baseline BMD at the lumbar spine and baseline BMD at the hand. The predictors of efficacy in increase of BMD at the total hip were changed from baseline at 3 months in PINP. The predictors of efficacy in increase of BMD at the femoral neck were zero. The predictors of efficacy in increase of BMD at the hand were baseline BMD at the hand (Table 2).
The mTSS at baseline from 12 months before significantly decreased at 12 months from baseline (1.13 vs. 0.59; p = 0.002). The EN score at baseline from 12 months before significantly decreased at 12 months from baseline (0.40 vs. 0.07; p < 0.001). The JSN score at baseline from 12 months before had a tendency to decrease at 12 months from baseline, but this was not significant (0.73 vs. 0.51; p = 0.052) (Fig. 2). The cumulative probability plots of mTSS, EN score and JSN score at baseline from 12 months before and at 12 months from baseline (Fig. 3). The structural remission (change in mTSS ≤ 0.5) rates at baseline and 12 months were 52.9 and 61.4%, respectively. At 12 months, in comparison of baseline demographic characteristics between patients with and without structural remission, there were not significant related factors (Table 3).
Change in modified total sharp score, erosion score, and joint space narrowing score at baseline from 12 months before and at 12 months from baseline. mTSS modified total sharp score, EN erosion score, JSN joint space narrowing score, baseline at baseline from 12 months before, 12 months at 12 months from baseline, vertical bar standard deviation
Change in van der Heijde-modified total sharp score represented by cumulative probability plots at baseline from 12 months before and at 12 months from baseline; a mTSS, b EN score and c JSN score. mTSS modified total sharp score, EN erosion score, JSN joint space narrowing score, baseline at baseline from 12 months before, 12 months at 12 months from baseline, circle plot baseline, triangle plot 12 months
The adverse events were itching (1.4%) and hypocalcemia (1.4%). The retention rate was 98.6% at 12 months.
Discussion
Denosumab 60 mg SC every 6 months treatment significantly increased the BMDs of the lumbar spine, total hip, femoral neck, and hand in patients with RA at 12 months. In particular, the BMD of the lumbar spine significantly increased at 3 months. In the DIRECT study on Japanese postmenopausal women and men with osteoporosis, the mean percent change in BMD from baseline to 24 months was 9.1% for the lumbar spine, 4.6% for the total hip, and 4.0% for the femoral neck [17]. In the FREEDOM trial on postmenopausal women with osteoporosis, the mean percent change in BMD from baseline to 36 months was 9.2% for the lumbar spine and 6.0% for the total hip [18]. On the other hand, in the DRIVE trial on Japanese women and men with RA treated with denosumab 60 mg SC every 6 months, mean BMD percent change from baseline to 12 months was about 4% for the lumbar spine and about 2% for the total hip [13]. Another study on a similar set of patients showed that the mean BMD percent change from baseline to 12 months was 3.0% for the lumbar spine and 1.6% for the total hip [12]. In this study, the mean percent change in BMD from baseline to 12 months was 8.3% for the lumbar spine and 4.7% for the total hip. Moreover, the BMD of the hand, which contains much cortical bone, was significantly increased at 12 months in this study. In patients with RA, loss of BMD in the hand is predictive of worse hand function; denosumab inhibition of this BMD loss may help prevent functional deterioration of the hand [19]. Although patient backgrounds were different, the results of this study were better than those of previous reports in increasing BMD at the lumbar spine and total hip, probably because our study patients were taking active vitamin D3 analog, had low RA disease activity, and high rate of bDMARDs use at baseline. Infliximab therapy for patients with RA was demonstrated to have beneficial effects on increasing BMD at the lumbar spine or total hip [20, 21]. In vitro, exposure of human osteoclast precursors to abatacept led to rapid downregulated expression of osteoclast marker genes [22]. In this study on Japanese patients with RA, denosumab treatment was shown to significantly increase the BMDs of the lumbar spine, total hip, femoral neck, and hand regardless of changes in other therapies and disease activity. Moreover, the efficacy of increase BMD at the lumbar spine depends on baseline BMD at the lumbar spine and the hand rather than disease activity of RA, although no patients with high disease activity in DAS28-ESR were present at baseline. We assume that the effect of denosumab may be more easily manifested in patients with controlled disease activity like those in this study.
One of the goals of RA treatment is structural remission. In this study, joint destruction at 12 months from the start of denosumab treatment was significantly reduced. In particular, the EN score was extremely suppressed. In one study on Japanese RA patients on DAS28-CRP 3.63 and MTX use, the change in EN score from baseline to 12 months was 0.27 [13]. MRI showed that hand erosion was lower in RA patients on denosumab 60 mg SC treatment compared with placebo [23]. In this study, differences in disease activity at before 12 months and at baseline may have led to this result. In RA patients with positive rheumatoid factor, disease activity causes joint destruction [24]. However, considering the reduction rate, we think that denosumab was involved in the suppression of bone erosion. In fact, the structural remission rate increased to 8.5%. Moreover, in mTSS and EN scores, the rates of patients with joint destruction progress at 12 months from the baseline were 10.0 and 5.7%, respectively. The DAS28-ESR of the patients with and without structural remission was 2.80 and 2.85, respectively. Denosumab had no influence on improvement of disease activity as DAS28-CRP, DAS28-ESR and SDAI in this study. These results were similar to those of previous reports [12, 13]. Our results suggest that add-on denosumab treatment might suppress progressive joint destruction in patients with RA.
In conclusion, our study demonstrated that denosumab increased the BMDs of the lumbar spine, total hip, femoral neck and hand, and suppressed joint destruction of Japanese patients with RA. The existing RA treatment combining modality therapy with denosumab might be effective for osteoporosis and joint destruction in patients with RA in whom disease activity can be controlled like those in this study, especially.
Limitations
This study had some limitations. This study had a small sample size; thus, the results would likely change if the case number was higher. Because this study did not have a control group, we could not clarify the relationship between RA and BMD in the general population. Moreover, the results of this study are undeniably the impact of RA treatment. In the future, a prospective study of the same patient backgrounds such as age and RA treatment would be necessary to conclude in regard to the effect of denosumab.
References
Kvien TK, Uhlig T (2005) Quality of life in rheumatoid arthritis. Scand J Rheumatol 34:333–341
Odegard S, Finset A, Kvien TK, Mowinckel P, Uhlig T (2005) Work disability in rheumatoid arthritis is predicted by physical and psychological health status: a 7-year study from the Oslo RA register. Scand J Rheumatol 34:441–447
Masiero S, Boniolo A, Wassermann L, Machiedo H, Volante D, Punzi L (2007) Effects of an educational-behavioral joint protection program on people with moderate to severe rheumatoid arthritis: a randomized controlled trial. Clin Rheumatol 26:2043–2050
Scott DL, Wolfe F, Huizinga TW (2010) Rheumatoid arthritis. Lancet 376:1094–1108
Schett G, Hayer S, Zwerina J, Redlich K, Smolen JS (2005) Mechanisms of Disease: the link between RANKL and arthritic bone disease. Nat Clin Pract Rheumatol 1:47–54
Lacey DL, Timms E, Tan HL, Kelley MJ, Dunstan CR et al (1998) Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell 93:165–176
Boyle WJ, Simonet WS, Lacey DL (2003) Osteoclast differentiation and activation. Nature 423:337–342
Hofbauer LC, Schoppet M (2004) Clinical implications of the osteoprotegerin/RANKL/RANK system for bone and vascular diseases. JAMA 292:490–495
van der Heijde DM (2000) Radiographic imaging: the ‘gold standard’ for assessment of disease progression in rheumatoid arthritis. Rheumatology 39:9–16
Van der Heijde D (2001) Radiographic progression in rheumatoid arthritis: dose it reflect outcome? Dose it reflect treatment? Ann Rheum Dis 60:47–50
Josse R, Khan A, Ngui D, Shapiro M (2013) Denosumab, a new pharmacotherapy option for postmenopausal osteoporosis. Curr Med Res Opin 29:205–216
Cohen SB, Dore RK, Lane NE, Ory PA, Peterfy CG, Sharp JT, van der Heijde D, Zhou L, Tsuji W, Newmark R (2008) Denosumab treatment effects on structural damage, bone mineral density, and bone turnover in rheumatoid arthritis: a twelve-month, multicenter, randomized, double-blind, placebo-controlled, phase II clinical trial. Arthritis Rheum 58:1299–1309
Takeuchi T, Tanaka Y, Ishiguro N, Yamanaka H, Yoneda T, Ohira T, Okubo N, Genant HK, van der Heijde D (2016) Effect of denosumab on Japanese patients with rheumatoid arthritis: a dose-response study of AMG 162 (Denosumab) in patients with RheumatoId arthritis on methotrexate to Validate inhibitory effect on bone Erosion (DRIVE)-a 12-month, multicentre, randomised, double-blind, placebo-controlled, phase II clinical trial. Ann Rheum Dis 75:983–990
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF et al (1988) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 16:65–67
Aletaha D, Neogi T, Silman AJ, Funovits J, Felson DT et al (2010) 2010 Rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum 62:2569–2581
van der Heijde D (2000) How to read radiographs according to the Sharp/van der Heijde method. J Rheumatol 27:261–263
Nakamura T, Matsumoto T, Sugimoto T, Hosoi T, Miki T, Gorai I, Yoshikawa H, Tanaka Y, Tanaka S, Sone T, Nakano T, Ito M, Matsui S, Yoneda T, Takami H, Watanabe K, Osakabe T, Shiraki M, Fukunaga M (2014) Clinical Trials Express: fracture risk reduction with denosumab in Japanese postmenopausal women and men with osteoporosis: denosumab fracture intervention randomized placebo controlled trial (DIRECT). J Clin Endocrinol Metab 99:2599–2607
Cummings SR, San Martin J, McClung MR, Siris ES, Eastell R, Reid IR, Delmas P, Zoog HB, Austin M, Wang A, Kutilek S, Adami S, Zanchetta J, Libanati C, Siddhanti S, Christiansen C (2009) Denosumab for prevention of fractures in postmenopausal women with osteoporosis. N Engl J Med 361:756–765
Deodhar AA, Brabyn J, Pande I, Scott DL, Woolf AD (2003) Hand bone densitometry in rheumatoid arthritis, a five year longitudinal study: an outcome measure and a prognostic marker. Ann Rheum Dis 62:767–770
Dischereit G, Tarner IH, Müller-Ladner U, Lange U (2013) Infliximab improves bone metabolism and bone mineral density in rheumatoid arthritis and ankylosing spondylitis: a prospective 2-year study. Clin Rheumatol 32:377–381
Haugeberg G, Conaghan PG, Quinn M, Emery P (2009) Bone loss in patients with active early rheumatoid arthritis: infliximab and methotrexate compared with methotrexate treatment alone. Explorative analysis from a 12-month randomised, double-blind, placebo-controlled study. Ann Rheum Dis 68:1898–1901
Bozec A, Zaiss MM, Kagwiria R, Voll R, Rauh M, Chen Z, Mueller-Schmucker S, Kroczek RA, Heinzerling L, Moser M, Mellor AL, David JP, Schett G (2014) T cell costimulation molecules CD80/86 inhibit osteoclast differentiation by inducing the IDO/tryptophan pathway. Sci Transl Med. doi:10.1126/scitranslmed.3007764
Deodhar A, Dore RK, Mandel D, Schechtman J, Shergy W, Trapp R, Ory PA, Peterfy CG, Fuerst T, Wang H, Zhou L, Tsuji W, Newmark R (2010) Denosumab-mediated increase in hand bone mineral density associated with decreased progression of bone erosion in rheumatoid arthritis patients. Arthritis Care Res 62:569–574
Welsing PM, Landewé RB, van Riel PL, Boers M, van Gestel AM, van der Linden S, Swinkels HL, van der Heijde DM (2004) The relationship between disease activity and radiologic progression in patients with rheumatoid arthritis: a longitudinal analysis. Arthritis Rheum 50:2082–2093
Author information
Authors and Affiliations
Contributions
The sponsors were not involved in the: study design; collection, analysis, and interpretation of data, writing of the paper, and/or decision to submit the results for publication.
Corresponding author
Ethics declarations
Conflict of interest
T. Mochizuki received honorariums for lectures from AbbVie, Inc., Asahi Kasei Pharma Corp., Bristol-Myers Squibb Co., Chugai Pharmaceutical Co., Daiichi Sankyo Co., Ltd., Eisai Co., Ltd., Eli Lilly Japan Co., Janssen Pharmaceutical K.K., Mitsubishi Tanabe Pharma Co., and Takeda Pharmaceutical Co., Ltd. K. Ikari received honorariums for lectures and/or unrestricted research Grants from AbbVie, Inc., Asahi Kasei Pharma Corp., Astellas Pharma Inc., Bristol-Myers Squibb Co., Chugai Pharmaceutical Co., Eisai Co., Ltd. Hisamitsu Pharmaceutical Co., Inc., Janssen Pharmaceutical K.K., Kaken Pharmaceutical Co., Ltd., Mitsubishi Tanabe Pharma Co., Santen Pharmaceutical Co., Ltd., Taisho Toyama Pharmaceutical Co., Ltd. and Takeda Pharmaceutical Co., Ltd. S. Momohara received honorariums for lectures and/or unrestricted research Grants from AbbVie, Inc., Asahi Kasei Pharma Corp., Bristol-Myers Squibb Co., Chugai Pharmaceutical Co., Daiichi Sankyo Co., Ltd., Eisai Co., Ltd., Mitsubishi Tanabe Pharma Co., Nakashima Medical Co., Ltd., Santen Pharmaceutical Co., Ltd., Taisho Toyama Pharmaceutical Co., Ltd. and Takeda Pharmaceutical Co., Ltd. The other authors declare that they have no conflicts of interest.
About this article
Cite this article
Mochizuki, T., Yano, K., Ikari, K. et al. Effects of denosumab treatment on bone mineral density and joint destruction in patients with rheumatoid arthritis. J Bone Miner Metab 36, 431–438 (2018). https://doi.org/10.1007/s00774-017-0848-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-017-0848-1