Abstract
The naturally occurring dipeptide carnosine (β-alanyl-l-histidine) inhibits the growth of tumor cells. As its component l-histidine mimics the effect, we investigated whether cleavage of carnosine is required for its antineoplastic effect. Using ten glioblastoma cell lines and cell cultures derived from 21 patients suffering from this malignant brain tumor, we determined cell viability under the influence of carnosine and l-histidine. Moreover, we determined expression of carnosinases, the intracellular release of l-histidine from carnosine, and whether inhibition of carnosine cleavage attenuates carnosine’s antineoplastic effect. We observed a significantly higher response of the cells to l-histidine than to carnosine with regard to cell viability in all cultures. In addition, we detected protein and mRNA expression of carnosinases and a low but significant release of l-histidine in cells incubated in the presence of 50 mM carnosine (p < 0.05), which did not correlate with carnosine’s effect on viability. Furthermore, the carnosinase 2 inhibitor bestatin did not attenuate carnosine’s effect on viability. Interestingly, we measured a ~ 40-fold higher intracellular abundance of l-histidine in the presence of 25 mM extracellular l-histidine compared to the amount of l-histidine in the presence of 50 mM carnosine, both resulting in a comparable decrease in viability. In addition, we also examined the expression of pyruvate dehydrogenase kinase 4 mRNA, which was comparably influenced by l-histidine and carnosine, but did not correlate with effects on viability. In conclusion, we demonstrate that the antineoplastic effect of carnosine is independent of its cleavage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 1900, Gulewitsch and Amiradzibi investigated the chemical components of Liebig’s meat extract (Gulewitsch and Amiradzibi 1900), discovering the first peptide, carnosine (β-alanyl-l-histidine). Carnosine is one of several imidazole-containing dipeptides such as homocarnosine (γ-aminobutyryl-l-histidine) and anserine (β-alanyl-N-π-methyl-l-histidine), which are present in high concentrations in the central nervous system and the skeletal muscle of vertebrates (Boldyrev et al. 2013). In the human body, carnosine levels are controlled by three enzymes. The formation of imidazole-containing dipeptides is catalyzed by the ATP-requiring Carnosine Synthase 1 [EC 6.3.2.11, also known as ATP-Grasp Domain-Containing Protein 1 (ATPGD1)]. The enzyme is encoded by the CARNS1 gene, which is in humans primarily expressed in skeletal muscle, heart muscle, and olfactory neurons (Drozak et al. 2013). The degradation of carnosine can be carried out by two metalloproteases. The extracellular occurring carnosine dipeptidase 1 (CN1; EC 3.4.13.20; also known as serum carnosinase and encoded by the CNDP1 gene) is supposed to be mainly produced in brain (Jackson et al. 1991), although it may also be synthesized in the liver (Peters et al. 2011). It hydrolyses carnosine with high specificity, but is also able to cleave anserine (β-alanyl-3-methyl-l-histidine), l-alanyl-l-histidine, l-glycyl-l-histidine, and homocarnosine (deamino-3-aminomethyl-alanyl-l-histidine) (reviewed in Bellia et al. 2014). The second enzyme (CN2; EC 3.4.13.18; also known as cytosolic non-specific dipeptidase or formerly known as tissue carnosinase; encoded by the CNDP2 gene), is expressed intracellularly and occurs ubiquitously in human tissue (Teufel et al. 2003). Although CN2 was shown to have optimum activity at pH 9.5 with regard to cleavage of carnosine (Lenney et al. 1985), the dipeptide can be hydrolyzed intracellularly, but at a much lower rate compared to other histidine containing dipeptides, as demonstrated by experiments with HEK293T cells (Okumura and Takao 2017). Since the discovery of carnosine, several physiological functions have been ascribed to it, such as Ca2+ regulation, pH-buffering, metal ion chelating, scavenging of reactive oxygen species, and protection against advanced glycation end products and lipid peroxidation (for a comprehensive review see Boldyrev et al. 2013). Furthermore, we and others reported the antineoplastic effect of carnosine on cancer cells from different origin such as glioblastoma (Renner et al. 2008), colon (Horii et al. 2012; Iovine et al. 2014), gastric (Shen et al. 2014), and cervix carcinoma (Ditte et al. 2014).
In Europe, glioblastoma is the most common and in the United States the second most common primary tumor of the central nervous system (Ostrom et al. 2016; Sant et al. 2012). Under the currently recommended therapy consisting of surgical removal of the tumor, radiotherapy, and adjuvant chemotherapy with temozolomide, median survival of patients is only 14.6 months (Stupp et al. 2005). Therefore, new therapeutic options are urgently needed. Although carnosine has been intensively discussed as a potential anti-tumor drug (Gaunitz et al. 2015; Gaunitz and Hipkiss 2012; Hipkiss and Gaunitz 2014), up to now, the molecular mechanisms of carnosine’s antineoplastic effects are not completely understood. In addition, it is not known whether the intact molecule or one of its moieties (β-alanine/l-histidine) is responsible for tumor growth inhibition. Previously, we reported that l-histidine is able to mimic the antineoplastic effect of carnosine in glioblastoma cell lines (Letzien et al. 2014). In these experiments, l-histidine also induced expression of pyruvate dehydrogenase kinase 4 (PDK4) in a comparable manner to carnosine. l-histidine released from the dipeptide may then become a substrate for further reactions such as decarboxylation or deamination leading to histamine or urocanate formation, respectively. In fact, both compounds are known to be able to induce gene expression (Romero et al. 2016; Kaneko et al. 2008). Therefore, we hypothesized that cleavage of the dipeptide may be required to deploy its effect.
Materials and methods
Reagents
Unless stated, otherwise, all chemicals were purchased from Sigma-Aldrich (Taufkirchen, Germany). Carnosine was kindly provided by Flamma (Flamma s.p.a. Chignolo d’Isola, Italy).
Cell lines and primary cell cultures
The glioblastoma cell lines G55T2, 1321N1, and U373 were obtained from Sigma-Aldrich (Taufkirchen, Germany), the cell lines U87, T98G, and LN229 from the American-Type Culture Collection (ATCC; Manassas, USA); MZ54 and MZ18 were originally obtained from Donat Kögel (Frankfurt, Germany) and the lines LN405 and U343 were obtained from the “Deutsche Sammlung von Mikroorganismen und Zellkulturen” (DMSZ; Braunschweig, Germany). Primary cell cultures were established from tissue samples obtained during standard surgery performed at the Neurosurgery Department of the University Hospital Leipzig during 2011 and 2015 (see Table 1 for age and gender of patients). All patients provided written informed consent according to the German laws as confirmed by the local committee. All glioblastoma samples were diagnosed and have been approved by the Neuropathology Department of the Leipzig University Hospital. Primary cultures from glioblastoma tissue were established as described before (Renner et al. 2008). Briefly, tissue specimens from the tumor were cut into approximately 1 mm3 large pieces and then separately placed into 25 mm2 culture flasks (TPP, Trasadingen, Switzerland) until tumor cells grew out. When more than 90% confluence was reached, specimens were removed and primary cell cultures were transferred into 75 mm2 culture flasks (TPP) for further cultivation. Cell cultures were maintained in high glucose DMEM (Dulbecco’s Modified Eagle Medium with 4.5 g glucose/mL) supplemented with 2 mM GlutamaxTM, 1% penicillin/streptomycin (all from Gibco Life Technologies, now Thermo Fisher Scientific, Darmstadt, Germany) and 10% Fetal Bovine Serum (FBS; Biochrom GmbH, Berlin, Germany), further referred to as “culture medium”, and kept in incubators (37 °C, 5% CO2/95% air).
Cell based assays
For cell viability assays, cells were counted and seeded into sterile 96-well plates (µClear, Greiner Bio-One, Frickenhausen, Germany) at a density of 5000 cells/well in 200 µL culture medium (for passage number of primary cultured cells refer to Table 1). After 24 h of cultivation (37 °C, 5% CO2/95% air), the medium was removed and replaced with fresh medium (100 µL/well) containing carnosine (10, 25, 50, 75 mM) or l-histidine (10, 25, 50 mM) for the determination of viability after 48 h of incubation. For testing the effect of the CN2 inhibitor bestatin (also known as Ubenimex) on viability of cells from the glioblastoma lines G55T2 and LN405, the cells received 0 mM or 50 mM carnosine and different concentrations of bestatin (0 µM, 10 µM, 50 µM, or 100 µM). In these cells viability was determined after 24, 48, and 72 h of incubation. Cells used for the determination of viability after 48 and 72 h received fresh medium with the corresponding compounds after 24 h and 48 h to account for a possible instability of bestatin in the medium. After incubation, the CellTiter-Glo Luminescent Cell Viability Assay (CTG, Promega, Mannheim, Germany) was employed to determine viable cells by measuring ATP in cell lysates and the CellTiter-Blue Cell Viability Assay (CTB, Promega) was used to quantify the metabolic capacity in living cells. All assays were carried out according to manufacturer’s protocols. Luminescence and fluorescence were measured using a SpectraMax M5 multilabel reader (Molecular Devices, Biberach, Germany).
Real-time quantitative polymerase chain reaction
Real-time quantitative polymerase chain reaction (qRT-PCR) experiments were carried out as described (Letzien et al. 2014). Briefly, 106 cells were seeded in 10 mL of medium into 10-cm cell culture dishes (TPP, Trasadingen, Switzerland) with 10 mL culture medium. After 24 h of incubation, cells received fresh medium without test compounds or containing 25 mM l-histidine or 50 mM carnosine. RNA was isolated after 24 h of incubation using the miRNeasy mini kit (Qiagen, Hilden, Germany) according to manufacturer’s instructions. The RNA was stored at − 80 °C until further use. 500 ng of RNA was used for reverse transcription employing the ImProm-II™ Reverse Transcription System (Promega, Mannheim, Germany) according to manufacturer’s instructions using random primer sets. DNA amplification was performed on a Rotor-Gene 3000 system (Qiagen) employing SYBR Green (Maxima SYBR Green/ROX qPCR Master Mix, Thermo Scientific). Copy numbers of individual mRNAs were determined using linearized plasmid DNA (described in Letzien et al. 2014) containing the corresponding target sequence. The relative expression of pyruvate dehydrogenase kinase 4 (PDK4), serum carnosinase (CNDP1) and cytosolic non-specific dipeptidase (CNDP2) was obtained by normalization to the copy number of the mRNA encoding the TATA box-binding protein (TBP) which was used as reference gene. Data analysis was performed using the RotorGene 6 software and all amplification reactions were controlled for the appropriate products by melting curve analysis. The following primer sequences were used: For CNDP1: CNDP1 forward primer: 5ʹ GAA GAA TAC CGG AAT AGC AG 3ʹ and CNDP1 reverse primer: 5ʹ CGG CCA GGT ATG ACT GTT 3ʹ; for CNDP2: CNDP2 forward primer: 5ʹ AGA AGC CCT GCA TCA CCT AC 3′ and CNDP2 reverse primer: 5ʹ CCA CCA AAG AGC CCA TC 3ʹ; for PDK4: PDK4 forward primer: 5′ CTG TGA TGG ATA ATT CCC 3′ and PDK4 reverse primer: 5′ GCC TTT AAG TAG ATG ATA GCA 3′. For the reference gene TBP: TBP forward primer: 5′ TTG ACC TAA AGA CCA TTG CAC 3′ and TBP reverse primer: 5′ GCT CTG ACT TTA GCA CCT GTT 3′; (all from Biomers, Ulm, Germany).
Western blot
For isolation of protein, 106 glioblastoma cells were seeded into 10-cm cell culture dishes (TPP, Trasadingen, Switzerland) with 10 mL medium. After 24 h cells received fresh media and were subjected to additional 24 h of incubation. Then, cells were washed twice with ice-cold washing buffer (137 mM NaCl, 5.4 mM HCl, 0.41 mM MgSO4, 0.49 mM MgCl2, 0.126 mM CaCl2, 0.33 mM Na2HPO4, 0.44 mM KH2PO4, 2 mM HEPES, pH 7.4) and finally collected in 1 mL washing buffer. After a brief centrifugation (5 min, 500×g, 4 °C), and cells were resuspended in 150 µl of ice-cold radioimmunoprecipitation assay buffer (RIPA buffer: 50 mM Tris, 150 mM NaCl, 0.25% sodium deoxy cholate, 0.1% SDS, 1% Nonidet P40) supplemented with PhosStOP™ and an in-house protease inhibitor cocktail (0.025 g/L aprotinin, 0.025 g/L leupeptin, 0.01 g/L pepstatin A, 1 mM dithiothreitol, 2.5 mM phenylmethylsulfonylfluoride, and 2.5 mM benzamidine). After 10 min of incubation on ice, cells were lysed by sonification (Bioruptor, Diagenode, Seraing, Belgium; settings: power: high, interval: 0.5, time: 7 min). The resulting cell fraction was centrifuged (5 min at 4 °C and 5500×g) and the resulting supernatant was transferred into a new 1.5 mL reaction vial and stored at − 80 °C until further use. Protein concentration was determined using the Pierce 660 nm-assay reagent according to manufacturer’s instructions. Electrophoresis was performed using a vertical electrophoresis unit (Mini-Protean-Cell, Bio-Rad, Munich, Germany) and separation was carried out in 12% polyacrylamide gels. Before loading onto the gel, 30 µg protein was mixed with 4 µL sample buffer (0.5 mM Tris, 40% glycerol, 275 mM sodium dodecyl sulfate, 0.125% bromophenol blue, 20% 2-mercaptoethanol, pH 6.8) and volume was adjusted to 16 µL with double distilled water, followed by denaturation (5 min, 95 °C). Separated proteins were transferred overnight at 4 °C onto a low fluorescence polyvinylidene fluoride membrane (ab133411 Abcam, Cambridge, United Kingdom) using a wet blot system (Mini Trans-Blot Cell, Bio-Rad) with BSN-buffer (48 mM Tris, 39 mM glycine, 20% methanol). After transfer, membranes were blocked for 1 h at room temperature under constant shaking in Tris-buffered saline with Tween20 (TBST: 20 mM Tris, 134 mM NaCl, 0.1% Tween 20, pH 7.6) supplemented with 2% (w/v) bovine serum albumin. Then, the solution was exchanged, adding primary antibodies diluted in TBST (mouse anti CNDP2 clone AT15E5 [Abnova; MAB11202] 1:1000; rabbit anti ACTB [abcam; ab8227] 1:5000) followed by incubation of 1 h at room temperature under constant shaking. The primary antibodies were removed by three washes with TBST and a mixture of two secondary antibodies (anti-rabbit-IRDye680 [LI-COR; 925-68071] 1:8000; anti-mouse-IRDye800 [LI-COR; 925-32210] 1:8000) diluted in TBST was added to the membrane. After 1 h incubation at room temperature and constant shaking, secondary antibodies were removed by three washes with TBST. The membrane was dried overnight between two Whatman filter papers. Membranes were scanned using an Odyssey Imaging System (LI-COR, Bad Homburg, Germany) and band intensities were determined by the Image Studio 5 software (LI-COR).
Determination of intracellular l-histidine
To quantify intracellular amounts of histidine, a modified method of Csámpai et al. (2004) was used. Cells from ten glioblastoma lines and from five primary cultures were seeded at a density of 300,000 cells per well into a 6-well-plate in 2 mL of culture medium. After 24 h of cultivation, the culture medium was removed and replaced with fresh medium containing 50 mM carnosine or 25 mM l-histidine or no compound (control). Then, cells were incubated for additional 24 h before they were washed thrice with 1 mL ice-cold washing buffer followed by extraction using 400 µL ice-cold methanol. After 10 min of gentle shaking on ice, extracts were collected in 1.5 mL Eppendorf-vials, wells were rinsed twice with 400 µL high-quality water (Milli-Q) and 800 µL obtained were combined with the first 400 µL. Samples were evaporated to dryness by lyophilization (Martin Christ Gefriertrocknungsanlagen, Osterode, Germany). For derivatization, the freeze-dried extracts were dissolved in 100 µL high-quality water (Milli-Q) and 0.5% (w/v) ortho-phthalaldehyde (dissolved in 100 µL methanol) was added. Derivatization was carried out at 37 °C for 45 min, followed by the addition of 800 µL 0.1% formic acid (in HPLC grade water). The obtained solution (200 µL) was transferred into 250 µL conic glass inserts of 2 mL ND10 vials, followed by high-performance liquid chromatography coupled to mass spectrometry (HPLC-MS) with 100 µL of sample.
HPLC-MS set up and data analysis
The system used for detection was an Agilent HPLC 1100 (Agilent, Waldbronn, Germany) consisting of a variable wavelength detector (VWD), a well plate auto sampler and a binary pump, coupled with a Bruker Esquire 3000 plus electrospray ionization mass spectrometer run by Esquire Control 5.3 (Bruker, Bremen, Germany). The employed column was a Phenomenex Gemini 5 µ C18 110 Å, 150 mm × 2 mm with a 2 mm guard column of the same material (Phenomenex Ltd., Aschaffenburg, Germany). The eluent system consisted of two solvents, with eluent A: 0.1% formic acid in acetonitrile and eluent B: 0.1% formic acid in HPLC grade water. Mobile phase flow rate was 0.5 mL/min with the following gradient for separation: 0–10 min 90% B, 90–0% B within 15 min, 25–35 min 0% B, 0–90% B within 5 min and 40–47 min 90% B for column equilibration. The mass spectrometer operated in positive mode (target mass: m/z 300; scan range: m/z 70–400), the dry gas temperature was set to 360°C (with a flow rate of 11 L/min; nebulizer: 70 psi). Data were analyzed using OpenChrom version 2.0.103.v20150204-1700 (Wenig and Odermatt 2010). Histidine was identified by an authentic standard. The selective ion chromatogram of m/z = 272 was used for quantification by peak integration.
Data presentation and statistical analysis
If not stated otherwise, data are presented as mean ± standard deviation (SD). For pairwise comparisons, Welch’s t test (unpaired two-sample test with unequal variances) was performed using the algorithm implemented in Excel (Microsoft, Redmond, USA; Version: 14.0.7212.5000 32-Bit). For multivariate statistical analysis, a Kruskal–Wallis–ANOVA was performed, followed by a Welch’s t test for pairwise comparisons. To consider the false discovery rate of multiple comparisons, p values were adjusted according to Benjamini and Hochberg (1995), and a value < 0.05 was presumed to be significant. Correlation analysis (Pearson correlation coefficient) and Kruskal–Wallis–ANOVA were carried out by OriginPro 2017G (OriginLab Corporation, Northampton, USA; Version: 2017G 64-bit SR1).
Results
Cell viability in cultured primary glioblastoma cells and cell lines derived from glioblastoma cultivated in medium with different concentrations of carnosine and l-histidine
First, we analyzed the viability of ten cell lines and 21 primary cell cultures derived from glioblastoma after 48 h of incubation in the presence of various concentrations of carnosine (0, 10, 25, 50, and 75 mM) and l-histidine (0, 10, 25, and 50 mM). As can be seen in Fig. 1, viability of glioblastoma cells was significantly reduced by a concentration of 50 (p = 1.45 × 10−9) and 75 (p = 5.19 × 10−22) mM carnosine as determined by the CTB and at a concentration of 25 (p = 2.8 × 10−2), 50 (p = 7.44 × 10−8) and 75 (p = 3.63 × 10−14) mM carnosine as determined by the CTG assay (for the individual responses of all cultures see supplemental Fig. 1–e). With regard to l-histidine, even the lowest concentration employed (10 mM) was able to significantly reduce the relative amount of ATP (p = 2.13 × 10−2) and dehydrogenase activity (p = 6.77 × 10−4) in the tested glioblastoma cells. In the presence of 25 mM (CTB: p = 3.94 × 10−2; CTG: p = 5.53 × 10−3) and 50 mM (CTB: p = 1.49 × 10−3; CTG: p = 2.54 × 10−3) of l-histidine, cells from lines revealed a significantly stronger loss of viability than primary cultured cells. Overall, comparing equal concentrations, l-histidine was 1.37 ± 0.14-fold (median) more effective than carnosine in decreasing cell viability.
Viability of primary glioblastoma cell cultures and glioblastoma cell lines under the influence of carnosine and l-histidine. Primary glioblastoma cell cultures (21) and glioblastoma cell lines (10) were exposed for 48 h to different concentrations of carnosine (0, 10, 25, 50 or 75 mM) or l-histidine (0, 10, 25, or 50 mM). Viability was determined by assessing metabolic activity (CTB; a) and by measuring the amount of ATP in cell lysates (CTG; b). Each dot within the boxplot represents the mean obtained from six independent measurements of an individual culture which was normalized to the untreated control (set to 100%). Dark gray dots represent cell lines treated with carnosine or histidine, and light gray dots represent primary cell cultures treated with carnosine or histidine. Statistical significance compared to untreated control and between equal concentrations of carnosine and l-histidine was determined by Welch’s t test with: *p < 0.05; **p < 0.005; ***p < 0.0005. The individual results of each cell culture are presented in Supplemental Fig. 1a–e
Expression of serum carnosinase and cytosolic non-specific dipeptidase in human glioblastoma cells
As the experiments presented in the previous section suggest that carnosine may need first to be cleaved to l-histidine and β-alanine to deploy its effect, we asked whether the glioblastoma cells express the mRNA of the required enzymes at all. Therefore, we analyzed CNDP1 and CNDP2 expression in 31 glioblastoma cell cultures by qRT-PCR. As can be seen in Fig. 2, CNDP2 was expressed in all analyzed samples with a relative expression ranging from 0.59 to 30.24 copy numbers per TBP copy (note that TBP mRNA has ~ 100 copies per ng RNA). In contrast to that, CNDP1 was only weakly expressed or not detectable with a relative expression ranging from 0 to 0.14 copy numbers per TBP copy. Next, we asked whether the presence of CNDP2 mRNA in glioblastoma cells also results in a corresponding protein expression. In the western blot presented in Fig. 3, it can be seen that CN2 protein was detectable in all investigated samples, suggesting the possibility that carnosine could indeed be cleaved intracellularly. Noteworthy, by quantifying CN2 band intensity, we could not find a correlation between protein and mRNA expression (Pearson correlation; r = − 5.68 × 10−4; p = 0.999).
Expression of CNDP1 and CNDP2 mRNA in primary glioblastoma cell cultures and glioblastoma cell lines. Total RNA from 21 primary glioblastoma cell cultures and ten glioblastoma cell lines was extracted, reverse transcribed and analyzed by qRT-PCR. CNDP1 and CNDP2 mRNA copy numbers were determined using standards and relative expression was calculated by the normalization to the TBP mRNA copy number of each sample. Data are represented as mean and standard deviation of three measurements. An x-axis break has been used because of the high differences between the absolute expression of CNDP1 and CNDP2 mRNA
Expression of CN2 protein in glioblastoma cell lines. Protein from ten glioblastoma cell lines was isolated and subjected to SDS-PAGE. Western blotting was performed using antibodies against CN2 (53 kDa) and β-actin (42 kDa). Upper panel: western blot image as analyzed by an Odyssey Imaging System. Lower panel: quantitative analysis of bands from the upper panel determined by Image Studio 5
Cell viability under the influence of carnosine and bestatin
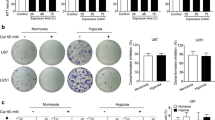
Next, we asked, whether the CN2 inhibitor bestatin attenuates the effect of carnosine on cell viability. In Fig. 4, viability in the presence of 50 mM carnosine and different concentrations of bestatin are presented, relative to viability of cells with only the indicated concentrations of bestatin but without carnosine (set as 100% for each concentration of bestatin). As illustrated, bestatin does not attenuate the effect of carnosine in both cell lines, independent of the employed concentrations of bestatin and the time of measurement. Only at concentrations of 50 µM and 100 µM bestatin and in the case of LN405 with regard to ATP in cell lysates after 72 h of incubation, the effect of carnosine on viability was statistically not significant (p = 0.31 and 0.33, respectively). However, this was most likely caused by an already strong effect of bestatin on viability after 72 h exposure even in the absence of carnosine which resulted in a high standard deviation (50 µM: 42 ± 17% viability without and 27 ± 13% with carnosine, 100 µM: 26 ± 16% viability without, and 13 ± 7% with carnosine). At this point, it has to be noted that we observed a negative effect on viability with increased concentrations of bestatin and exposure time, even in the absence of carnosine (see supplemental Fig. 2). More important, comparing viability in the presence of carnosine and different concentrations of bestatin and incubation time does not indicate an influence of the CN2 inhibitor on carnosine’s effect on viability.
Viability of G55T2 and LN405 glioblastoma cells under the influence of carnosine and the dipeptidase-inhibitor bestatin. Viability of cells from the lines G55T2 and LN405 in the presence of 50 mM carnosine and different concentrations of bestatin (0, 10, 50, or 100 µM) was compared to the viability of cells with the inhibitor bestatin but without carnosine, setting the viability without carnosine for each concentration of bestatin to 100 percent. After 24, 48, and 72 h of incubation, viability was determined by determining metabolic activity [dehydrogenase (DH) activity] and by measuring the amount of ATP in cell lysates (ATP in cell lysates). Data are represented as mean and standard deviation of six independent measurements. Statistical significance was determined by Welch’s t test with: *p < 0.05; **p < 0.005; ***p < 0.0005
Comparison of intracellular l-histidine in primary cultured glioblastoma cells and cell lines derived from glioblastoma exposed to extracellular carnosine
The experiments presented in the previous section indicated that a release of l-histidine may not be required for the antineoplastic effect of carnosine. However, as viability was obviously negatively affected by the inhibitor bestatin itself, these experiments do not unequivocally demonstrate that the antineoplastic effect of carnosine is independent of the release of l-histidine in the absence of the inhibitor. Therefore, we investigated whether the release of l-histidine and the effect of carnosine on viability show any correlation. As can be seen in Fig. 5a, except for P0297 and G55T2, treatment with 50 mM carnosine resulted in a significant 1.22 to 2.5-fold increase of the intracellular abundance of histidine (with p values reaching from 3.12 × 10−4 to 7.12 × 10−3). This indicates that the dipeptide is cleaved to a certain amount inside the cells. However, there was no correlation between the expression of CN2 (Fig. 3) and the relative release of l-histidine. This is seen, for example, in the low expression of CN2 in MZ18 compared to its higher expression in LN229, which is not reflected by a corresponding difference in l-histidine release. More important, we did not see any significant correlation between the decrease of viability under the influence of 50 mM carnosine and the relative release of l-histidine (supplemental Fig. 3). This also indicates that the antineoplastic effect is independent of the cleavage of the dipeptide. Analyzing the intracellular abundance of l-histidine in the presence of 25 mM extracellular l-histidine (a concentration resulting in a similar decrease of viability as observed in the presence of 50 mM carnosine, Fig. 1), we detected a ~ 40-fold higher abundance of intracellular l-histidine compared to incubation in the presence of 50 mM carnosine (Fig. 5). This observation also confirms the notion that cleavage of carnosine is not required for its antineoplastic effect.
Intracellular abundance of histidine in glioblastoma cells incubated in the presence of 50 mM carnosine and 25 mM histidine. a Cells from ten lines (dark gray) and five primary glioblastoma cell cultures (light gray) were exposed for 24 h to 50 mM carnosine. Then, amino acids were extracted and analyzed by HPLC-MS. Changes of the relative intracellular abundances of l-histidine are shown as mean percent and standard deviation (using error propagation) compared to untreated control cells from six independent experiments. Statistical significance was determined by Welch’s t test with: *p < 0.05; **p < 0.005; ***p < 0.0005. b Relative intracellular abundance of l-histidine in cells from 10 cell lines incubated in the presence of 50 mM carnosine or 25 mM l-histidine. Each dot represents the mean obtained from six independent measurements of an individual culture
Expression of PDK4 mRNA under the influence of carnosine and l-histidine and correlation between viability and influence on expression
Finally, we investigated whether the effect of l-histidine (25 mM) and carnosine (50 mM) on viability correlates with their influence on PDK4 expression. As can be seen in Fig. 6a, carnosine significantly induced the expression of PDK4 mRNA in eight samples, whereas a significantly reduced expression was found in four samples. Under the influence of l-histidine, PDK4 mRNA expression was significantly induced in 21 samples. Comparing the effect of the two compounds on PDK4 expression (Fig. 6b), 18 cell cultures responded in the same way (both carnosine and l-histidine induced or reduced PDK4 mRNA expression when treatment of at least one compound was significantly different compared to the untreated control), whereas six cell cultures responded in an opposite way. Furthermore, there was a significant correlation between the influence of carnosine and l-histidine on PDK4 mRNA expression (Pearson correlation; r = 0.419; p = 0.019). Comparing the effect on PDK4 expression with the effect on viability, no correlation was found neither for l-histidine (Fig. 6c) nor for carnosine (Fig. 6d).
Expression of PDK4 mRNA after exposure to carnosine or l-histidine. 21 primary glioblastoma cell cultures and ten glioblastoma cell lines were incubated in the presence of 50 mM carnosine, 25 mM l-histidine, or vehicle control for 24 h. Then, total RNA was extracted, reverse transcribed and analyzed by qRT-PCR. PDK4 mRNA copy numbers were determined using standards and relative expression was calculated by the normalization to the TBP mRNA copy number of each sample. a Fold enhancement of PDK4 expression compared to untreated control cells. Data are represented as mean and standard deviation of three measurements compared to the untreated control (set to 1). Statistical significance was determined by Welch’s t test with: *p < 0.05; **p < 0.005; ***p < 0.0005. b Comparison of PDK4 mRNA expression under the influence of carnosine and l-histidine. The data presented in a are here depicted with fold increase of relative PDK4 mRNA expression under the influence carnosine on the x-axis, and with fold increase under the influence of l-histidine on the y-axis. c Comparison between viability and PDK4 mRNA expression under the influence of 25 mM l-histidine. d Comparison between viability and PDK4 mRNA expression under the influence of 50 mM carnosine
Discussion
The antineoplastic effect of carnosine, which was first described by Nagai and Suda (1986), has been confirmed in vitro (Ditte et al. 2014; Iovine et al. 2014; Renner et al. 2008; Shen et al. 2014) and in vivo (Horii et al. 2012; Renner et al. 2010) by several research groups. Hence, its potential as an anti-tumor agent has been discussed in a number of review articles (Gaunitz et al. 2015; Gaunitz and Hipkiss 2012; Hipkiss and Gaunitz 2014). As we previously demonstrated that l-histidine is able to mimic the antineoplastic effect of the dipeptide (Letzien et al. 2014), we wondered whether carnosine has to be cleaved to inhibit tumor cell growth. Comparing the viability of 21 primary cell cultures and ten cell lines originated from glioblastoma, we observed that with regard to the effector concentrations required to induce similar losses of viability, l-histidine was more effective at lower concentrations than carnosine. We also observed increased concentrations of intracellular l-histidine when cells were exposed to carnosine. As we identified the presence of CN2, we assume that this intracellular l-histidine is produced by cleavage of carnosine catalyzed by the enzyme. Comparing CN2 expression with the amount of intracellular l-histidine, we found no correlation. However, at this point, it has to be taken into account that because of different cell sizes, it is almost impossible to precisely compare the exact changes of intracellular concentrations of l-histidine between different cells. However, cleavage appears to be weak as the intracellular concentration of l-histidine in the presence of 25 mM l-histidine in the medium is ~ 40-times higher than the amount of l-histidine in cells incubated in the presence of 50 mM carnosine. At this point, it also has to be noted that Teufel et al. (2003) claimed that the intracellular pH is far from the optimal pH required for effective cleavage of carnosine by CNDP2. A very low release of l-histidine from carnosine has also been demonstrated by Son et al. (2008), investigating the intracellular concentration of amino acids of Caco-2 cells cultivated in the presence of 50 mM carnosine for 6 and 27 h. In these experiments, the intracellular amount of l-histidine in the presence of carnosine was more than 50 times lower than that observed in the presence of 50 mM l-ala-l-his.
Obviously, carnosine does not need to be cleaved into its single amino acids to deploy its antineoplastic effect, but the question remains, whether l-histidine bound to the β-alanine moiety in carnosine is sufficient to induce the antineoplastic effect of carnosine and whether β-alanine may be substituted by another moiety. This question has to be elaborated by further experiments, as it bears the interesting aspect that it could lead to the development of anti-cancer drugs which may have an advantage over carnosine. It also has to be asked whether l-histidine could be used as a supplement instead of carnosine. As demonstrated by cell injury assays with cultivated rat hepatocytes, this appears to be no good choice (Rauen et al. 2007). In these experiments, highly increased lactate dehydrogenase (LDH) release, as an indicator of cellular necrosis, was seen in the presence of 198 mM (92 ± 1%), 76 mM (91 ± 1%), and 50 mM l-histidine (74 ± 18%), whereas a concentration of 198 mM carnosine resulted in only 39 ± 3% LDH release compared to 20 ± 5% LDH release in untreated control cells. This also points to the possibility that other mechanisms are responsible for the increased toxicity of l-histidine than those responsible for the specific antineoplastic effect of carnosine. At this point, it should also be noted that we recently demonstrated that in co-cultures of tumor cells with non-tumor cells, carnosine selectively eliminated the tumor cells (Oppermann et al. 2018). In these experiments, in which the cells were incubated up to several weeks, lower concentrations of carnosine have been employed than those that were used in the experiments presented in the present study. This has to be noted, as we are aware that it may be difficult to achieve the compound concentrations employed in the present investigation in vivo. On the other hand, it is also difficult to estimate, which intracellular concentrations may be achievable when carnosine is delivered orally, as we do not know whether carnosine can efficiently be protected from degradation by CN1 (see below). We also do not know whether it can be transported to the target cells, whether it may be resynthesized from the single amino acids, and whether it may accumulate in cells which could take it up. Anyway, the most frequently discussed obstacle using carnosine as an orally given drug is its rapid degradation by serum carnosinase in humans (Lenney et al. 1982). Despite the observation that the dipeptide is effective as a drug in different diseases (Baraniuk et al. 2013; Boldyrev et al. 2008; Chengappa et al. 2012; Chez et al. 2002) and despite the fact that it may be protected by deposition in liver (Gardner et al. 1991) or erythrocytes (Chaleckis et al. 2016), the high activity of CN1 in human serum will certainly strongly affect the effective concentration achievable in a patient’s tumor tissue when given orally. In addition, it has to be asked whether cleavage of carnosine by CN1 may increase serum concentrations of l-histidine to hepatotoxic concentrations. Therefore, it would be interesting to analyze whether other l-histidine- or imidazole-containing compounds which are not degradable by CN1 and are not toxic to other cells, may be useful alternatives. However, it has to be taken into account that these compounds need to be able to be taken up by tumor cells, can pass the blood–brain barrier in case of brain tumors, and are selective in preventing cancer cell proliferation. For the purpose of further drug development, it is also of major importance to understand the molecular mechanisms responsible for the antineoplastic effect.
Aside from a plethora of reports on carnosine’s influence on signaling molecules in different models (for review, see Gaunitz et al. 2015), the currently best described effect of carnosine on transcription in glioblastoma cells is its influence on transcription of PDK4 (Letzien et al. 2014). Therefore, we also investigated whether we could see any correlation between carnosine and l-histidine regarding their effect on PDK4 mRNA expression (Fig. 6). As we could demonstrate that carnosine and l-histidine influence PDK4 mRNA expression in 18 out of 31 cell cultures in the same way, this may indicate that at least in some cultures l-histidine and carnosine share similarities with regard to their influence on transcription. Although this only moderate correlation may be tempered by a limited sample size, it is at least obvious that there is no correlation between carnosine’s and l-histidine’s effect on viability and expression of PDK4 mRNA. Therefore, we conclude that changes of PDK4 expression may not be responsible for carnosine’s antineoplastic effect.
In summary, we demonstrate that the cleavage of carnosine and the release of l-histidine is not required for the antineoplastic effect of the dipeptide, which can be deduced from three observations: (1) The CN2 inhibitor bestatin does not attenuate the effect of carnosine on tumor cell viability. (2) Intracellular cleavage of carnosine is observable, but has a low efficiency. (3) Roughly 40-times higher amounts of intracellular free l-histidine in the presence of 25 mM extracellular l-histidine have the same effect on tumor cell viability as concentrations of free l-histidine observed in the presence of 50 mM extracellular carnosine.
References
Baraniuk JN, El-Amin S, Corey R, Rayhan R, Timbol C (2013) Carnosine treatment for gulf war illness: a randomized controlled trial. GJHS 5:69. https://doi.org/10.5539/gjhs.v5n3p69
Bellia F, Vecchio G, Rizzarelli E (2014) Carnosinases, their substrates and diseases. Molecules 19:2299–2329. https://doi.org/10.3390/molecules19022299
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Ser B (Methodological) 57:289–300
Boldyrev A, Fedorova T, Stepanova M, Dobrotvorskaya I, Kozlova E, Boldanova N, Bagyeva G, Ivanova-Smolenskaya I, Illarioshkin S (2008) Carnosine [corrected] increases efficiency of DOPA therapy of Parkinson’s disease: a pilot study. Rejuvenation Res 11:821–827. https://doi.org/10.1089/rej.2008.0716
Boldyrev AA, Aldini G, Derave W (2013) Physiology and pathophysiology of carnosine. Physiol Rev 93:1803–1845. https://doi.org/10.1152/physrev.00039.2012
Chaleckis R, Murakami I, Takada J, Kondoh H, Yanagida M (2016) Individual variability in human blood metabolites identifies age-related differences. Proc Natl Acad Sci USA 113:4252–4259. https://doi.org/10.1073/pnas.1603023113
Chengappa KR, Turkin SR, DeSanti S, Bowie CR, Brar JS, Schlicht PJ, Murphy SL, Hetrick ML, Bilder R, Fleet D (2012) A preliminary, randomized, double-blind, placebo-controlled trial of l-carnosine to improve cognition in schizophrenia. Schizophr Res 142:145–152. https://doi.org/10.1016/j.schres.2012.10.001
Chez MG, Buchanan CP, Aimonovitch MC, Becker M, Schaefer K, Black C, Komen J (2002) Double-blind, placebo-controlled study of l-carnosine supplementation in children with autistic spectrum disorders. J Child Neurol 17:833–837
Csámpai A, Kutlán D, Tóth F, Molnár-Perl I (2004) O-Phthaldialdehyde derivatization of histidine: stoichiometry, stability and reaction mechanism. J Chromatogr A 1031:67–78
Ditte Z, Ditte P, Labudova M, Simko V, Iuliano F, Zatovicova M, Csaderova L, Pastorekova S, Pastorek J (2014) Carnosine inhibits carbonic anhydrase IX-mediated extracellular acidosis and suppresses growth of HeLa tumor xenografts. BMC Cancer 14:358. https://doi.org/10.1186/1471-2407-14-358
Drozak J, Chrobok L, Poleszak O, Jagielski AK, Derlacz R (2013) Molecular identification of carnosine N-methyltransferase as chicken histamine N-methyltransferase-like protein (hnmt-like). PLoS One 8:e64805. https://doi.org/10.1371/journal.pone.0064805
Gardner MLG, Illingworth KM, Kelleher J, Wood D (1991) Intestinal-absorption of the intact peptide carnosine in man, and comparison with intestinal permeability to lactulose. J Physiol 439:411–422
Gaunitz F, Oppermann H, Hipkiss AR (2015) Carnosine and cancer. In: Preedy VR (ed) Imidazole dipeptides. The Royal Society of Chemistry, Cambridge, pp 372–392
Gaunitz F, Hipkiss AR (2012) Carnosine and cancer: a perspective. Amino Acids 43:135–142. https://doi.org/10.1007/s00726-012-1271-5
Gulewitsch W, Amiradzibi S (1900) Ueber das Carnosin, eine neue organische Base des Fleischextraktes. Ber Dtsch Chem Ges 33:1902–1903
Hipkiss AR, Gaunitz F (2014) Inhibition of tumour cell growth by carnosine: some possible mechanisms. Amino Acids 46:327–337
Horii Y, Shen J, Fujisaki Y, Yoshida K, Nagai K (2012) Effects of l-carnosine on splenic sympathetic nerve activity and tumor proliferation. Neurosci Lett 510:1–5. https://doi.org/10.1016/j.neulet.2011.12.058
Iovine B, Oliviero G, Garofalo M, Orefice M, Nocella F, Borbone N, Piccialli V, Centore R, Mazzone M, Piccialli G, Bevilacqua MA (2014) The anti-proliferative effect of l-carnosine correlates with a decreased expression of hypoxia inducible factor 1 alpha in human colon cancer cells. PLoS One 9:e96755. https://doi.org/10.1371/journal.pone.0096755
Jackson MC, Kucera CM, Lenney JF (1991) Purification and properties of human serum carnosinase. Clin Chim Acta 196:193–205
Kaneko K, Smetana-Just U, Matsui M, Young AR, John S, Norval M, Walker SL (2008) cis-Urocanic acid initiates gene transcription in primary human keratinocytes. J Immunol 181:217–224. https://doi.org/10.4049/jimmunol.181.1.217
Lenney JF, George RP, Weiss AM, Kucera CM, Chan PWH, Rinzler GS (1982) Human-serum carnosinase—characterization, distinction from cellular carnosinase, and activation by cadmium. Clin Chim Acta 123:221–231
Lenney JF, Peppers SC, Kucera-Orallo CM, George RP (1985) Characterization of human tissue carnosinase. Biochem J 228:653–660
Letzien U, Oppermann H, Meixensberger J, Gaunitz F (2014) The antineoplastic effect of carnosine is accompanied by induction of PDK4 and can be mimicked by l-histidine. Amino Acids. https://doi.org/10.1007/s00726-014-1664-8
Nagai K, Suda T (1986) Antineoplastic effects of carnosine and beta-alanine—physiological considerations of its antineoplastic effects. J Physiol Soc Jpn 48:741–747
Okumura N, Takao T (2017) The zinc form of carnosine dipeptidase 2 (CN2) has dipeptidase activity but its substrate specificity is different from that of the manganese form. Biochem Biophys Res Commun 494:484–490. https://doi.org/10.1016/j.bbrc.2017.10.100
Oppermann H, Dietterle J, Purcz K, Morawski M, Eisenlöffel C, Müller W, Meixensberger J, Gaunitz F (2018) Carnosine selectively inhibits migration of IDH-wildtype glioblastoma cells in a co-culture model with fibroblasts. Cancer Cell Int 18:111. https://doi.org/10.1186/s12935-018-0611-2
Ostrom QT, Gittleman H, Xu J, Kromer C, Wolinsky Y, Kruchko C, Barnholtz-Sloan JS (2016) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2009–2013. Neuro-Oncology 18:v1–v75. https://doi.org/10.1093/neuonc/now207
Peters V, Jansen EEW, Jakobs C, Riedl E, Janssen B, Yard BA, Wedel J, Hoffmann GF, Zschocke J, Gotthardt D, Fischer C, Köppel H (2011) Anserine inhibits carnosine degradation but in human serum carnosinase (CN1) is not correlated with histidine dipeptide concentration. Clin Chim Acta 412:263–267. https://doi.org/10.1016/j.cca.2010.10.016
Rauen U, Klempt S, de Groot H (2007) Histidine-induced injury to cultured liver cells, effects of histidine derivatives and of iron chelators. Cell Mol Life Sci 64:192–205. https://doi.org/10.1007/s00018-006-6456-1
Renner C, Seyffarth A, de Arriba S, Meixensberger J, Gebhardt R, Gaunitz F (2008) Carnosine inhibits growth of cells isolated from human glioblastoma multiforme. Int J Pept Res Ther 14:127–135. https://doi.org/10.1007/s10989-007-9121-0
Renner C, Zemitzsch N, Fuchs B, Geiger KD, Hermes M, Hengstler J, Gebhardt R, Meixensberger J, Gaunitz F (2010) Carnosine retards tumor growth in vivo in an NIH3T3-HER2/neu mouse model. Mol Cancer 9:2. https://doi.org/10.1186/1476-4598-9-2
Romero SA, Hocker AD, Mangum JE, Luttrell MJ, Turnbull DW, Struck AJ, Ely MR, Sieck DC, Dreyer HC, Halliwill JR (2016) Evidence of a broad histamine footprint on the human exercise transcriptome. J Physiol (Lond) 594:5009–5023. https://doi.org/10.1113/JP272177
Sant M, Minicozzi P, Lagorio S, Børge Johannesen T, Marcos-Gragera R, Francisci S (2012) Survival of European patients with central nervous system tumors. Int J Cancer 131:173–185. https://doi.org/10.1002/ijc.26335
Shen Y, Yang J, Li J, Shi X, Ouyang L, Tian Y, Lu J (2014) Carnosine inhibits the proliferation of human gastric cancer SGC-7901 cells through both of the mitochondrial respiration and glycolysis pathways. PLoS ONE 9:e104632. https://doi.org/10.1371/journal.pone.0104632
Son DO, Satsu H, Kiso Y, Totsuka M, Shimizu M (2008) Inhibitory effect of carnosine on interleukin-8 production in intestinal epithelial cells through translational regulation. Cytokine 42:265–276
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJB, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO, van Den Weyngaert D, Kaendler S, Krauseneck P, Vinolas N, Villa S, Wurm RE, Maillot MHB, Spagnolli F, Kantor G, Malhaire JP, Renard L, de Witte O, Scandolaro L, Vecht CJ, Maingon P, Lutterbach J, Kobierska A, Bolla M, Souchon R, Mitine C, Tzuk-Shina T, Kuten A, Haferkamp G, de Greve J, Priou F, Menten J, Rutten I, Clavere P, Malmstrom A, Jancar B, Newlands E, Pigott K, Twijnstra A, Chinot O, Reni M, Boiardi A, Fabbro M, Campone M, Bozzino J, Frenay M, Gijtenbeek J, Delattre JY, de Paula U, Hanzen C, Pavanato G, Schraub S, Pfeffer R, Soffietti R, Kortmann RD, Taphoorn M, Torrecilla JL, Grisold W, Huget P, Forsyth P, Fulton D, Kirby S, Wong R, Fenton D, Cairncross G, Whitlock P, Burdette-Radoux S, Gertler S, Saunders S, Laing K, Siddiqui J, Martin LA, Gulavita S, Perry J, Mason W, Thiessen B, Pai H, Alam ZY, Eisenstat D, Mingrone W, Hofer S, Pesce G, Dietrich PY, Thum P, Baumert B, Ryan G (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996
Teufel M, Saudek V, Ledig JP, Bernhardt A, Boularand S, Carreau A, Cairns NJ, Carter C, Cowley DJ, Duverger D, Ganzhorn AJ, Guenet C, Heintzelmann B, Laucher V, Sauvage C, Smirnova T (2003) Sequence identification and characterization of human carnosinase and a closely related non-specific dipeptidase. J Biol Chem 278:6521–6531
Wenig P, Odermatt J (2010) OpenChrom: a cross-platform open source software for the mass spectrometric analysis of chromatographic data. BMC Bioinform 11:405. https://doi.org/10.1186/1471-2105-11-405
Acknowledgements
We would like to thank Flamma [Flamma s.p.a. Chignolo d’Isola, Italy (https://www.flammagroup.com)] for the generous supply with very high-quality carnosine for all of our experiments. In addition, we would like to thank Dr. Hans-Heinrich Foerster from the Genolytic GmbH (Leipzig, Germany) for genotyping and confirmation of cell identity and last not least Mrs. Susan Billig for technical assistance.
Author information
Authors and Affiliations
Contributions
KP performed most of the experiments with contributions of HO and RB-S. CB established the HPLC-MS method with contributions of HO and performed the HPLC-MS measurements. JM did the surgery and revised the manuscript. HO and FG designed the study and wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no potential conflict of interest.
Informed consent
All patients provided written informed consent according to German law as confirmed by the local committee (#144-2008) in accordance with the 1964 Helsinki declaration and its later amendments.
Additional information
Handling Editor: W. Derave.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
726_2019_2713_MOESM1_ESM.jpg
Supplementary material 1 (JPG 3325 kb) Supplemental Figure 1a to e: Viability of 21 primary glioblastoma cell cultures and 10 glioblastoma cell lines under the influence of carnosine and L-histidine. Glioblastoma cell cultures and cell lines were exposed for 48 hours to different concentrations of carnosine (0, 10, 25, 50 or 75 mM) or L-histidine (0, 10, 25 or 50 mM). Viability was determined by assessing metabolic activity (CTB) and by measuring the amount of ATP in cell lysates (CTG) (all in sixtuplicate). The summary of the experiments is presented in the Box blot in Fig. 1 of the main text
726_2019_2713_MOESM6_ESM.jpg
Supplementary material 2 (JPG 3098 kb) Supplemental Figure 2. Cell viability under the influence of bestatin in the absence and presence of carnosine. Cells from the lines G55T2 and LN405 in the presence and absence of 50 mM carnosine were exposed to different concentrations of bestatin (0, 10, 50 or 100 µM) and the viability of cells was determined setting the viability without the inhibitor for each condition to 100 percent. Viability was determined after 24, 48 and 72 hours by measuring metabolic activity (dehydrogenase (DH) activity) and by determining the amount of ATP in cell lysates (ATP in cell lysates). Data is represented as mean and standard deviation of six independent measurements. Statistical significance was determined by Welch’s t-test with: *: p<0.05; **: p<0.005; ***: p<0.0005
726_2019_2713_MOESM7_ESM.jpg
Supplementary material 3 (JPG 1975 kb) Supplemental Figure 3. Comparison of viability in the presence of 50 mM carnosine and the relative change of the intracellular abundance of L-histidine after exposure to the dipeptide. Viability of cells exposed for 48 hours to 50 mM carnosine was compared to the amount of L-histidine determined 24 hours after exposure to 50 mM of the dipeptide relative to untreated control cells (set as 100 percent). Note: For readability, error bars were omitted from the graph
Rights and permissions
About this article
Cite this article
Oppermann, H., Purcz, K., Birkemeyer, C. et al. Carnosine’s inhibitory effect on glioblastoma cell growth is independent of its cleavage. Amino Acids 51, 761–772 (2019). https://doi.org/10.1007/s00726-019-02713-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-019-02713-6