Abstract
Patent foramen ovale (PFO) is a common cardiac anomaly linked with cryptogenic strokes and migraine, particularly migraine with aura. This study aims to explore the spectrum of headache disorders in PFO patients, focusing on identifying patterns beyond the well-established migraine-PFO connection. A retrospective observational study was conducted on patients diagnosed with PFO. Headache types were classified using the International Classification of Headache Disorders, 3rd edition. The study analyzed headache prevalence and patterns in PFO patients, comparing those with and without a history of stroke. Of 177 participants, 63 (35.59%) reported headaches. Tension-type headache was the most common (15.25%), followed by migraine without aura (11.30%) and migraine with aura (8.47%). Notably, migraine without aura was more prevalent than migraine with aura, contrasting previous assumptions. No significant differences were found in headache types based on stroke history. The study reveals a diverse spectrum of headache types in PFO patients, with migraine without aura being more common than migraine with aura. These findings suggest a need for broader diagnostic perspective and individualized treatment approaches in PFO patients with headaches.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patent foramen ovale (PFO), a common cardiac anomaly, has been associated with cryptogenic stroke, particularly in the younger demographic (Lamy et al. 2002). While the pathophysiological link remains a topic of investigation, longstanding evidence suggests that migraines—especially those with aura—may be more prevalent in individuals with PFO (Sztajzel et al. 2002).
Previous research has primarily concentrated on the migraine-PFO connection, potentially overlooking the incidence of other headache disorders in patients with PFO. The intricacies of this association are yet to be fully understood, raising the question if the presence of a PFO predisposes individuals to a specific pattern of headache. As there is little data regarding the occurrence of other types of headaches in persons with PFO, this study aims to explore headache in this population beyond the confines of migraine, and also to assess if there is any distinctive pattern of headache in those with PFO-related strokes.
Methodology
Study design and participants
A retrospective observational study was conducted, including consecutive patients admitted to our hospital with a diagnosis of PFO, between January 2021 and December 2023. The primary objective was to characterize headache types among persons with PFO. The secondary objective was to examine if there is a notable difference in headache patterns between those with PFO and a history of stroke and those with PFO and without such history.
Participants had to be aged between 18 and 65 years and have a confirmed diagnosis of PFO by contrast-enhanced transcranial doppler (c-TCD) and transesophageal cardiac echography (TEE). They were afterwards first divided into two groups: those with headache, and those without headache; a second comparison, taking into consideration the history of stroke was performed between the two resulting groups. For the stroke group, patients had to have had a neurologist-confirmed diagnosis of PFO-related stroke, which consisted of exclusion of cervical or cerebral artery atheromatosis by arterial ultrasound or computed-tomography arteriography, long-term cardiac rhythm monitoring (for a minimum of 24 h) confirming the absence of atrial fibrillation or atrial flutter, and cerebral magnetic resonance imaging for the exclusion of lacunar stroke. For the no-stroke group, patients had to have had no history of stroke confirmed by cerebral MRI. Patients who had incomplete medical records regarding PFO or stroke diagnosis were excluded from the study. All remaining patients were telephoned, and those who declined to participate in the telephonic interview, those who were unreachable after multiple attempts, or diagnosed with drug overuse headache after the interview, were also excluded from the study. Finally, stroke, cardiovascular risk factors, and PFO anatomical features were assessed in both headache and no-headache groups, with additional interest in headache subtypes.
Data collection
Data was collected through medical records review and telephone interviews. Patients were asked about the presence of headaches in the year prior to the inclusion in the study. To classify the headache types, we employed a standardized telephonic interview, guided by the International Classification of Headache Disorders, 3rd edition (ICHD-3) (supplementary material). This classification ensured consistency in diagnosis and comparability with other studies. Interviews were conducted by the same trained neurologist (RȘB), familiar with the ICHD-3 criteria. Demographic data, such as age and gender, were also collected, alongside cardio- and cerebrovascular risk factors such as a history of diabetes, hypertension, smoking (and smoking index, which was calculated by multiplying the number of cigarettes smoked per day by the number of years the individual has smoked). Anatomical characteristics of the PFO, such as its height, length, shunt severity (as estimated through the c-TCD on the Spencer logarithmic scale (Lao et al. 2008), and the presence of features like the Eustachian valve, septal aneurysm, and Chiari network, were documented for analysis. The heights and lengths of PFO were available for 87 and 94 patients respectively and were retained for the analysis.
Participant consent was obtained through a standardized telephonic procedure. During the call, each participant was thoroughly informed about the objectives of the study, the nature of their involvement, the confidentiality of their responses, and their right to withdraw at any time without consequence. Verbal consent was documented by the interviewer, including the date and time of the call, and was subsequently confirmed via an in-person follow-up that included signing the informed consent form. This study was conducted in strict adherence to ethical guidelines and was approved by the Board of Ethics of the University Emergency Hospital of Bucharest. Comprehensive informed consent was obtained from all participants, in line with the 1964 Helsinki Declaration and GDPR standards.
Statistical analysis
Descriptive statistics were utilized to summarize the demographic and clinical characteristics of the study population. Normality of data distribution for continuous variables was assessed using the Shapiro-Wilk test. Continuous variables with a normal distribution were presented as mean ± standard deviation, while those with a non-normal distribution were reported as median (interquartile range). Categorical variables were presented as rates (percentages). To compare differences between groups, independent t-tests, or Independent-Samples Mann-Whitney U tests were used for continuous variables, while χ2 or Fisher’s exact test was used for categorical variables. To assess the differences in demographic, clinical, and PFO characteristics across the four headache subtypes identified in our cohort, we employed both the Independent-Samples Kruskal-Wallis test and one-way ANOVA. A p-value of less than 0.05 was considered statistically significant. In cases of multiple comparisons, the Bonferroni correction was applied, and the alpha level was adjusted. The statistical analysis was performed using IBM SPSS Statistics for Windows, Version 29.0. (Armonk, NY: IBM Corp).
Results
Demographics and clinical characteristics
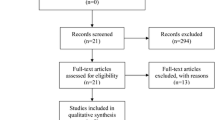
A total of 267 patients were identified, with 177 included in the final analysis; the remainder were excluded due to non-response, refusal to participate, or meeting one or more of the exclusion criteria.
The majority of participants were female (54.80%), and the mean age was 42.29 years (SD 10.76). Complete characterization of the participants can be found in Table 1.
Headache characteristics in PFO patients
Out of the total participants, 63 (35.59%) reported experiencing headaches in the previous year. While a significantly higher prevalence (p = .027) of headaches was observed in females (66.67%) compared to males (33.33%), age was similar in both groups (42.25 years, SD = 10.51 in patients with no history of headaches vs. 40.54 years, SD = 11.08 in those with headache), p = .108.
The most common type of headache among the study participants was tension-type headache, experienced by 27 patients (15.25% of all participants). This was followed by migraine without aura in 20 patients (11.30%), and migraine with aura in 15 patients (8.47%). There was also one case (0.56%) of trigeminal autonomic cephalalgia (TAC), more specifically, short-lasting, unilateral, neuralgiform headache attacks with conjunctival injection and tearing (SUNCT). No other types of headaches were identified in the studied population.
No significant gender differences were observed across the headache subtypes (p = .121). The median age varied across the 4 headache groups, with the youngest median age observed in the migraine with aura group (35.93 years, SD 8.19), while the patient diagnosed with TAC was the oldest (59 years). However, after adjusting the p-value for multiple comparisons, these age differences did not reach statistical significance (p > .005).
Headache characteristics in relation to stroke history
123 participants were classified as having PFO-related stroke. Among them, 30 (24.39%) reported experiencing headaches. In this subgroup, the most prevalent were tension-type headaches, reported by 15 patients (50.00% of those with headaches and a stroke history), followed by migraine without aura and migraine with aura, experienced by 8 (26.67%) and 7 (23.33%) patients, respectively. In contrast, among the 54 PFO patients without a stroke history, 33 (61.11%) reported headaches. In this group, tension-type headaches and migraine without aura were equally prevalent, each reported by 12 patients (each 36.36%), followed by migraine with aura in 8 patients (24.24%) (Fig. 1). Additionally, there was one case (3.03%) of TAC exclusively in the non-stroke group. Nevertheless, there were no significant differences in the types of headaches between patients with and without a history of stroke (p = .597).
Stroke, cardiovascular risk factors and PFO anatomical features in relation to overall headache and headache subtypes
A history of stroke was more common in patients without headaches (81.58%) compared to those with headaches (47.62%), showing a significant association (p < .001). Hypertension was present in 29.94% of the total cohort and was less frequent in the headache group (20.63%) compared to the no-headache group (35.09%), reaching statistical significance (p = .031). The proportion of smokers and the smoking index did not differ significantly between the headache and no-headache groups (Table 1). The frequency of cardiovascular risk factors, such as hypertension, smoking status, and smoking index, did not differ significantly between the four headache groups. (Table 2).
Regarding PFO characteristics, the median PFO height and length varied slightly among headache subtypes, with the largest PFO heights and lengths in patients with migraine with aura (3.00 [2.00–7.00] and 7.00 [2.00–9.00] respectively). However, these anatomical differences did not show a significant association with headache types (PFO height p = .563, length p = .482); furthermore, while the PFO shunt, though not significantly different, tended to be greater in patients without headaches compared to those with headaches, other PFO characteristics such as prominent Eustachian valve, septal aneurysm, and Chiari network showed no significant association with headache occurrence or type (Table 1).
Discussions
The association between PFO and migraine, particularly migraine with aura, has been a subject of considerable debate in the medical community. While numerous studies have reported a high prevalence of PFO in individuals with migraines compared to the general population (Nahas et al. 2010), this link remains under scrutiny, with some experts challenging the association (Garg et al. 2010; Rundek et al. 2008). Our research adds to this discussion by showing that, in our cohort, migraine (both with and without aura) was overall the most common headache type among patients with PFO, accounting for 19.77% of the participants. This figure is only slightly higher than the 13–16% prevalence of migraines in the general population (Collaborators 2018; Lipton et al. 2002; Rundek et al. 2008; Steiner and Stovner 2023; Stovner et al. 2022), yet, at best, it falls in the middle of the broader reported range of 9.13–61.4% for migraine prevalence in PFO patients (Calviere et al. 2013; Dao and Tobis 2011; Faggiano et al. 2012; Kimmelstiel et al. 2007; Lamy et al. 2002; Schwedt et al. 2008; Sztajzel et al. 2002; Truong et al. 2008). At the moment, there are two population-based studies (Kuper et al. 2013; Rundek et al. 2008) available, with a moderate to high quality of evidence that showed that the prevalence of PFO in patients with migraine is similar with that of patients without migraine. It is our opinion that patients with PFO may have migraines as frequent as the general population, and that more population-based studies are needed to find the true prevalence of migraine in PFO patients.
Our findings diverge from previous studies that predominantly associated PFO with migraine with aura (Carod-Artal et al. 2006; Dalla Volta et al. 2005; Ferrarini et al. 2005). In our study, migraine without aura was slightly more prevalent, representing 11.30% of our cohort, compared to 8.47% for migraine with aura. This can be due to the different classifications used for determining the type of migraines, or to the fact that previously reported association between PFO and migraine with aura is purely coincidental and suggests the need for larger studies using standardized classifications of headaches.
While the connection between this specific headache subtype and PFO has been extensively studied, the prevalence of headache other than migraine in individuals with PFO has not been adequately explored. To the best of our knowledge, there is only one study that examined the relationship between PFO and TTH and showed that the prevalence of PFO in TTH patients is similar to that of the general population (Moaref et al. 2009). In our study, we found that 15.25% of the participants experienced TTH, establishing it as the second most prevalent headache type. This prevalence rate is lower than the range reported for TTH in the general population, which in different studies varies between 19.4–26.4%(Bayraktutan et al. 2014; Collaborators 2018; Ferrante et al. 2013; Stovner et al. 2022).
Regarding TACs, existing literature suggests a prevalence of less than 0.1% in the general population (Benoliel 2012; Wei et al. 2019). In our study cohort, we identified a single case consistent with the TAC diagnosis, comprising 0.56% of the total patient population examined. While this incidence is marginally higher than reported general prevalence rates, we posit that a larger sample size would be necessary to more precisely determine the actual frequency of TAC among individuals with PFO.
An intriguing finding from our study, is the emergence of differences in headache types between groups of patients with PFO who have a history of stroke versus those without a cerebrovascular ischemic event. We noted that in patients with a history of stroke and headache, the number of those with TTH equals that of migraine patients. In contrast, within the group with headache and without a history of stroke (n = 33), the number of migraine patients exceeded that of TTH patients (20 vs. 12 patients). Furthermore, when examining the type of migraine experienced by these two groups, we observed that patients with a history of stroke more often suffered from migraine without aura, whereas those without a stroke history more commonly experienced migraine with aura. This finding is in contrast with previous studies which have indicated that migraine with aura, but not migraine without aura, is associated with an increased risk of ischemic stroke (Mahmoud et al. 2018).
Not in the least, in our investigation, we observed that PFO shunt severity was generally more pronounced in patients who did not report headaches. However, among those with headaches, individuals with migraine with aura exhibited the most severe shunt sizes as assessed through c-TCD. Conversely, the least severe shunt severity was noted in patients with TTH. These findings align with the research conducted by Ali Riza Moaref et al. (Moaref et al. 2009), which demonstrated a higher prevalence of large PFOs in patients with migraine with aura compared to those with TTH. When examining cardiovascular risk factors among PFO patients with headaches, we observed that patients without a history of headache were more frequently diagnosed with hypertension compared to those with headaches. However, it’s important to note that a majority of the patients without headaches were from the stroke group. Given that hypertension is a key risk factor for stroke (Buonacera et al. 2019), even in younger patients with PFO (Badea et al. 2023), this observation could be attributed to the disproportionate representation of stroke patients in our study compared to those in the non-stroke group, and needs further investigation through larger, case-control studies.
Limitations
This study, while providing valuable insights, has several limitations. Its retrospective and observational design limits causal inferences and may be subject to biases such as inaccurate patient recall. The sample size, though reasonable, may not be large enough to detect subtle associations, particularly in subgroup analyses, and the exclusion of non-responsive patients introduces potential selection bias. Reliance on self-reported data during telephonic interviews, despite adherence to the ICHD-3 criteria, may affect the accuracy of headache classification. As a single-center study, our findings might not be generalizable to wider populations due to regional variations in patient demographics and healthcare practices. The study did not account for all potential confounding factors, such as genetic predispositions or lifestyle choices, which could influence headache occurrence. The absence of a control group without PFO limits the ability to directly compare headache prevalence and characteristics, making it difficult to determine if the observed patterns are specific to PFO patients. These limitations highlight the need for cautious interpretation of the results and suggest that further, more comprehensive studies are needed for validation.
Conclusion
In conclusion, our study shows that migraine remains the predominant headache type in patients with PFO. Notably, contrary to earlier assertions, migraine without aura appears to be more prevalent in this demographic. Furthermore, TTH was also present in a significant proportion of our cohort, though with a prevalence that was marginally smaller compared to the general population. Our study also indicates that migraine with aura, an entity thought to be a risk factor for stroke, may not be as prevalent in the PFO-related stroke subpopulation when compared to other headache subtypes.
With minor differences, the prevalence of the various headache types in patients with PFO seems to closely mirror that in the general population. Considering this observation, along with the high frequency of both PFO and headaches as separate pathologies, their association might just be coincidental. Nevertheless, larger studies should be directed to correctly ascertain this finding.
References
Badea RS, Ribigan AC, Grecu N, Terecoasa E, Antochi FA, Mihaila B, Tiu S, C., Popescu BO (2023) Differences in clinical and biological factors between patients with PFO-related stroke and patients with PFO and no cerebral vascular events. Front Neurol 14:1104674. https://doi.org/10.3389/fneur.2023.1104674
Bayraktutan OF, Demir R, Ozel L, Ozdemir G, Ertekin A (2014) Prevalence of tension-type headache in individuals aged between 18–65 years in the Eastern Parts of Turkey. Eurasian J Med 46(2):78–83. https://doi.org/10.5152/eajm.2014.20
Benoliel R (2012) Trigeminal autonomic cephalgias. Br J Pain 6(3):106–123. https://doi.org/10.1177/2049463712456355
Buonacera A, Stancanelli B, Malatino L (2019) Stroke and hypertension: an Appraisal from Pathophysiology to Clinical Practice. Curr Vasc Pharmacol 17(1):72–84. https://doi.org/10.2174/1570161115666171116151051
Calviere L, Tall P, Massabuau P, Bonneville F, Larrue V (2013) Migraine with aura and silent brain infarcts lack of mediation of patent foramen ovale. Eur J Neurol 20(12):1560–1565. https://doi.org/10.1111/ene.12240
Carod-Artal FJ, da Silveira Ribeiro L, Braga H, Kummer W, Mesquita HM, Vargas AP (2006) Prevalence of patent foramen ovale in migraine patients with and without aura compared with stroke patients. A transcranial Doppler study. Cephalalgia 26(8):934–939. https://doi.org/10.1111/j.1468-2982.2006.01156.x
Collaborators GBDH (2018) Global, regional, and national burden of migraine and tension-type headache, 1990–2016: a systematic analysis for the global burden of Disease Study 2016. Lancet Neurol 17(11):954–976. https://doi.org/10.1016/S1474-4422(18)30322-3
Dalla Volta G, Guindani M, Zavarise P, Griffini S, Pezzini A, Padovani A (2005) Prevalence of patent foramen ovale in a large series of patients with migraine with aura, migraine without aura and cluster headache, and relationship with clinical phenotype. J Headache Pain 6(4):328–330. https://doi.org/10.1007/s10194-005-0223-9
Dao CN, Tobis JM (2011) PFO and paradoxical embolism producing events other than stroke. Catheter Cardiovasc Interv 77(6):903–909. https://doi.org/10.1002/ccd.22884
Faggiano P, Frattini S, Piovesana P, Lorusso R, Chiari E, Scolari F, Padovani A, Cas LD (2012) Low cerebrovascular event rate in subjects with patent foramen ovale and different clinical presentations: results from a prospective non randomized study on a population including patients with and without patent foramen ovale closure. Int J Cardiol 156(1):47–52. https://doi.org/10.1016/j.ijcard.2010.10.032
Ferrante T, Manzoni GC, Russo M, Camarda C, Taga A, Veronesi L, Pasquarella C, Sansebastiano G, Torelli P (2013) Prevalence of tension-type headache in adult general population: the PACE study and review of the literature. Neurol Sci 34(Suppl 1):S137–138. https://doi.org/10.1007/s10072-013-1370-4
Ferrarini G, Malferrari G, Zucco R, Gaddi O, Norina M, Pini LA (2005) High prevalence of patent foramen ovale in migraine with aura. J Headache Pain 6(2):71–76. https://doi.org/10.1007/s10194-005-0154-5
Garg P, Servoss SJ, Wu JC, Bajwa ZH, Selim MH, Dineen A, Kuntz RE, Cook EF, Mauri L (2010) Lack of association between migraine headache and patent foramen ovale: results of a case-control study. Circulation 121(12):1406–1412. https://doi.org/10.1161/CIRCULATIONAHA.109.895110
Kimmelstiel C, Gange C, Thaler D (2007) Is patent foramen ovale closure effective in reducing migraine symptoms? A controlled study. Catheter Cardiovasc Interv 69(5):740–746. https://doi.org/10.1002/ccd.21025
Kuper M, Rabe K, Holle D, Savidou I, Dommes P, Frings M, Diener HC, Katsarava Z (2013) Prevalence of cardiac right left shunts in migraine: a population-based case-control study. Neurol Sci 34(2):205–208. https://doi.org/10.1007/s10072-012-0986-0
Lamy C, Giannesini C, Zuber M, Arquizan C, Meder JF, Trystram D, Coste J, Mas JL (2002) Clinical and imaging findings in cryptogenic stroke patients with and without patent foramen ovale: the PFO-ASA Study. Atr Septal Aneurysm Stroke 33(3):706–711. https://doi.org/10.1161/hs0302.104543
Lao AY, Sharma VK, Tsivgoulis G, Frey JL, Malkoff MD, Navarro JC, Alexandrov AV (2008) Detection of right-to-left shunts: comparison between the International Consensus and Spencer Logarithmic Scale criteria. J Neuroimaging 18(4):402–406. https://doi.org/10.1111/j.1552-6569.2007.00218.x
Lipton RB, Scher AI, Kolodner K, Liberman J, Steiner TJ, Stewart WF (2002) Migraine in the United States: epidemiology and patterns of health care use. Neurology 58(6):885–894. https://doi.org/10.1212/wnl.58.6.885
Mahmoud AN, Mentias A, Elgendy AY, Qazi A, Barakat AF, Saad M, Mohsen A, Abuzaid A, Mansoor H, Mojadidi MK, Elgendy IY (2018) Migraine and the risk of cardiovascular and cerebrovascular events: a meta-analysis of 16 cohort studies including 1 152 407 subjects. BMJ Open 8(3):e020498. https://doi.org/10.1136/bmjopen-2017-020498
Moaref AR, Petramfar P, Aghasadeghi K, Zamirian M, Sharifkazemi MB, Rezaian S, Afifi S, Zare N, Rezaian GR (2009) Patent foramen ovale in patients with tension headache: is it as common as in migraineurs? An age- and sex-matched comparative study. J Headache Pain 10(6):431–434. https://doi.org/10.1007/s10194-009-0154-y
Nahas SJ, Young WB, Terry R, Kim A, Van Dell T, Guarino AJ, Silberstein SD (2010) Right-to-left shunt is common in chronic migraine. Cephalalgia 30(5):535–542. https://doi.org/10.1111/j.1468-2982.2009.02002.x
Rundek T, Elkind MS, Tullio D, Carrera MR, Jin E, Sacco Z, R. L., Homma S (2008) Patent foramen ovale and migraine: a cross-sectional study from the Northern Manhattan Study (NOMAS). Circulation 118(14):1419–1424. https://doi.org/10.1161/CIRCULATIONAHA.108.771303
Schwedt TJ, Demaerschalk BM, Dodick DW (2008) Patent foramen ovale and migraine: a quantitative systematic review. Cephalalgia 28(5):531–540. https://doi.org/10.1111/j.1468-2982.2008.01554.x
Steiner TJ, Stovner LJ (2023) Global epidemiology of migraine and its implications for public health and health policy. Nat Rev Neurol 19(2):109–117. https://doi.org/10.1038/s41582-022-00763-1
Stovner LJ, Hagen K, Linde M, Steiner TJ (2022) The global prevalence of headache: an update, with analysis of the influences of methodological factors on prevalence estimates. J Headache Pain 23(1):34. https://doi.org/10.1186/s10194-022-01402-2
Sztajzel R, Genoud D, Roth S, Mermillod B, Le Floch-Rohr J (2002) Patent foramen ovale, a possible cause of symptomatic migraine: a study of 74 patients with acute ischemic stroke. Cerebrovasc Dis 13(2):102–106. https://doi.org/10.1159/000047758
Truong T, Slavin L, Kashani R, Higgins J, Puri A, Chowdhry M, Cheung P, Tanious A, Child JS, Perloff JK, Tobis JM (2008) Prevalence of migraine headaches in patients with congenital heart disease. Am J Cardiol 101(3):396–400. https://doi.org/10.1016/j.amjcard.2007.08.047
Wei DY, Moreno-Ajona D, Renton T, Goadsby PJ (2019) Trigeminal autonomic cephalalgias presenting in a multidisciplinary tertiary orofacial pain clinic. J Headache Pain 20(1):69. https://doi.org/10.1186/s10194-019-1019-7
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by RȘB, NG and AR. The first draft of the manuscript was written by RȘB and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. This study did not receive any external funding or financial support from any public, private, or non-profit organizations. The research was conducted as an independent study by the authors, who have no financial conflicts of interest to declare. The datasets generated and analyzed for this study can be provided upon request.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Badea, R.Ș., Grecu, N., Ribigan, A.C. et al. Headache patterns in patent foramen ovale patients: beyond migraine with aura. J Neural Transm 131, 755–761 (2024). https://doi.org/10.1007/s00702-024-02760-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-024-02760-8