Abstract
Background
The operating microscope (OM) is an invaluable tool in neurosurgery but is not without its flaws. The ORBEYE™ (Olympus, Tokyo, Japan) is a 4K 3D exoscope aspiring to offer similar visual fidelity but with superior ergonomics. 2D visualisation was a major limitation of previous models which newer 3D exoscopes attempt to overcome. Here, we present our initial experience using a 4K 3D exoscope for neurosurgical procedures.
Objective
To evaluate the feasibility of the ORBEYE™ exoscope in performing neurosurgery and review of the literature.
Methods
All patients undergoing neurosurgery performed by a single surgeon, using the ORBEYE™, were assessed. Descriptive statistics and data relating to complications and operative time were recorded and analysed. An anecdotal literature review was performed for the experience of other authors using 4K 3D exoscopes in neurosurgery and compared to our subjective experience with the ORBEYE™.
Results
18 patients underwent surgery using the ORBEYE™. There were no 30-day post-operative complications observed. Our experience and that of other authors suggests that the ORBEYE™ offers comparable visualisation to the traditional OM, with superior ergonomics and an enhanced experience for assistants and observers.
Conclusion
Neurosurgery can be performed safely and effectively with the ORBEYE™, with improved ergonomics and educational benefit. There appears to be a short learning curve provided one has experience with endoscopic surgery and the use of a foot pedal.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Magnification, illumination and stereoscopic visualisation are the minimum characteristics expected of the modern operating microscope (OM) in micro-neurosurgery. Following the introduction of the binocular telescope by Carl Zeiss in 1893, it was not long before the microscope made its way into neurosurgical operating rooms. It has remained the gold standard in micro-neurosurgery, though there have been major advances in magnification, image-processing and ergonomics since Theodore Kurze performed the first neurosurgical procedure using the OM [16]. The frequent need for repositioning and fatigue associated with enforced fixation of the operators’ eyes to the OM eyepieces are among its shortcomings. In recent years, a high-definition (HD) video telescope system was proposed as an alternative to the OM [20]. However, similar to the traditional endoscope, the required hand-eye coordination for the 2-dimensional (2D) image provided is a major limitation of this system [23]. While magnification was provided in older models of the exoscope, stereoscopic vision and illumination in confined spaces are the primary advantage of the OM over other modes of magnification [16].
The ORBEYE™ (OLYMPUS, Tokyo, Japan) surgical microscope/exoscope offers 4K, three-dimensional (3D) magnified and illuminated imaging without the need for eyepieces. The operator visualises the surgical field on a 55-inch monitor using special 3-D glasses [26]. However, there is limited literature available regarding the efficacy and feasibility of the ORBEYE™ given its novelty. The benefits of the exoscope usage appear to be primarily in ease of use and comfort for the surgeon [22, 24, 29, 32], with comparatively little data regarding the outcomes of patients undergoing neurosurgery using exoscopic visualisation as compared to the OM [29]. Whether the exoscope can truly act as a substitute for an OM is uncertain, and more literature regarding patient outcomes and usability experience is therefore required to facilitate decision making for those considering the use of an exoscope in practice. Here, we describe our experience and patient outcomes using the ORBEYE™ for a variety of neurosurgical cases. We also present a review of the literature pertaining to the use of 4K 3D exoscopes in neurosurgery.
Methods
Patients
Patients were eligible for inclusion if undergoing any cranial neurosurgical procedure performed by the senior author that would ordinarily warrant the use of the OM within the study period. Patients undergoing procedures not expected to ordinarily require the use of the OM, and or those without 30-day follow-up data were excluded. Data was prospectively collected on consecutive craniotomies performed by the senior author between September 2020 and January 2021 (01/09/2020–31/12/2020) regarding operative duration, baseline patient demographics, indication and the anatomical location, size and histological variant of neoplasm, along with the surgical approach used. Patients were then followed up at 30 days post-operatively as is our standard practice. All patients meeting the eligibility criteria were included. Institutional review board approval was obtained
All patients included in this case series underwent procedures using the ORBEYE™, with a traditional OM (Leica M530 OH6) on standby. We recorded any situations where we had to convert to using the traditional OM rather than continuing with the ORBEYE™. We also extracted data relating to intraoperative and 30-day complications, and operative length for each procedure. Our primary aim was to assess whether the ORBEYE™ could be feasibly and safely used as an alternative to the OM by recording procedure duration and complications.
Descriptive statistics were collated using Stata SE v16.
Literature review
We performed an anecdotal search of the literature in the PubMed/MEDLINE and EMBASE databases for clinical experiences using 3D 4K exoscopes, searching for articles using keywords “exoscope”, “ORBEYE”, “VITOM” and “KINEVO”, and discussed the most relevant literature. We assessed studies describing their experience using exoscopes in case series of multiple patients, with particular focus on those using the ORBEYE™.
Results
The ORBEYE™ was used by the senior author in 18 consecutive craniotomies, predominantly supra-tentorial neoplasms, during a 3-month period (Table 1). Full data was available for all patients. During this time period, all craniotomies by the author were performed using ORBEYE™. The mean maximum tumour diameters were 3.89 cm (SD = 0.43). The mean operating times were 163.75 (SD = 24.38) minutes (Table 2). There were no observed 30-day peri-operative complications and the post-operative course was uneventful in all patients, who were discharged routinely. There were no 30-day readmissions related to the procedure. Although a traditional OM (Leica M530 OH6) was on standby, all cases were performed and completed without it. At no point was it necessary to change the ORBEYE™ for the OM and all cases were completed in full using only the ORBEYE™.
Discussion and literature review
Our findings suggest that the ORBEYE™ can be feasibly used in place of the OM for neurosurgery, with no requirement for switching to the OM during the procedure during any of our cases and no 30-day complications. The OM is an important neurosurgical tool which, despite its original use traceable to otolaryngology in 1921, was not adopted in neurosurgery until 1957 [35]. It has since been widely adopted in almost all areas of neurosurgery, but is not without its flaws. It has been estimated that the neurosurgeon may spend up to 40% of the operation time adjusting the microscope [35], a limitation some models attempt to overcome with the incorporation of a foot pedal and mouth piece. The ergonomics of the OM can also be problematic, requiring the surgeon to work with extended and elevated arms in a position prone to fatigue over time as a result of the distance between the eyepiece and microscope head [11]. Some models of OM may also offer the surgeon’s assistant a limited perspective, with limited visualisation also available to the other operating theatre staff, which has implications for teaching [29]. However, stereoscopic vision and illumination of confined spaces, the primary advantages of the OM, are difficult to replicate and so this has remained the gold standard of visualisation [16].
The exoscope aspires to overcome the drawbacks of the OM, offering improved ergonomics by way of a video feed of the operative field depicted on a screen visible to the surgeon. Binocular vision and excellent visual fidelity are important to the function of the OM and were suboptimal in earlier iterations of the exoscope. Newer models have incorporated 3D imaging and image quality has improved, making them more attractive as an alternative to the OM. Poor depth perception was reported as a limitation of previous 2D models [20, 21], which has been rectified with the use of dual stereoscopic sensors and full 3D visualisation in later models.
The exoscope in practice
The Olympus ORBEYE™ (Olympus, Tokyo, Japan) provides ultra-high-definition 4K in 3D, with a depth of field and field of vision that even exceeds the traditional OM6. Langer et al. reviewed multiple available exoscopes (ORBEYE™, VITOM, KINEVO, MODUS V) and suggested that the ORBEYE™ provides exceptional visual clarity that may even exceed the traditional OM based on their experience of 110 cases including tumour excision, neurovascular procedures and spinal surgery [19]. Several case series have described their experience with the ORBEYE™, across neuro-oncological [14, 22, 32, 34], neurovascular [14, 22, 24, 32, 34] and spinal surgery [14, 17, 22]. Commonly cited benefits over the OM included superior ergonomics and comfort [14, 17, 22, 24, 32, 34], wider field of vision [14, 17, 24, 32] and improved logistics and space saving [14, 17, 22, 34]. Most importantly, visualisation was generally considered equivalent or even potentially superior [14, 19, 34]. This broadly aligns with our experience. Subjectively, we found that visualisation is at least comparable to the OM but further assessment in an objective manner is required.
Two studies reported a lack of indocyanine green (ICG) support as a drawback [14, 24], though one utilised an earlier version of the ORBEYE™ without infrared capability [24] while the infrared module had not been FDA approved at the time of writing of the other [14]. The latest model of the ORBEYE™ has support for ICG [14, 22, 29] and 5-aminolevulinic acid (5-ALA) [22] which received FDA approval in October 2019.
Kwan et al. found that frequent adjustments to the ORBEYE™ were required during spinal surgery, significantly more than the OM [17]. This was not our experience with the ORBEYE™ in cranial surgery. In addition, similar to the experience of Khalessi et al. [14], we found that most adjustments could be accomplished using the foot pedal including zoom, focus and minor adjustments in position. The wide field of vision meant that the exoscope position had to be adjusted by hand infrequently. Furthermore, we found that table position adjustments are required less frequently with the ORBEYE™ compared to traditional OM, because the ORBEYE™ can be angled to allow illumination and visualisation of hidden areas such as those under bony shelves. The primary drawback reported by Murai et al. in using the ORBEYE™ was difficulty with visualisation during transsphenoidal approaches and small corticotomies [22] and similar difficulties have been reported with the VITOM 3D [5, 6]. While we have not yet tested the ORBEYE™ for pituitary surgery, our experience with small corticotomies has been positive. Difficulty with eyestrain has also been reported, and this is an issue that requires further assessment [22]. Eyestrain is a commonly reported issue in the use of 3D displays and appears to be related to the length of time spent viewing [28]. We also experienced this issue on occasion during longer procedures, which may constitute a limitation of the ORBEYE™ and require introduction of strategies to mitigate this, such as breaks during long procedures.
It was possible to angulate the ORBEYE™ to allow comfortable posturing of the operator which, like Khalessi et al. [14], we found particularly advantageous (Figs. 1 and 2). This avoids the unnatural spinal positions which the operating surgeon needs to adopt with the traditional OM [36], where there is a rigid relationship between the eyepiece and microscope head. Shimizu et al. reported a similar experience in a case series using the retrosigmoid approach in the supine position [32]. Optimal patient and microscope positioning is imperative for adequate visualisation during retrosigmoid approach, where operative corridors require an angulation of the OM that is often uncomfortable for the surgeon. They found that the flexibility and size of the ORBEYE™ allowed comfortable posture even when the operative visual axis was approximately horizontal [32]. This benefit is also apparent in spinal surgery, where significant angulation can be achieved to facilitate lateral recess and foraminal manipulations [17, 27].
Photographic illustration of the difference in surgeon posturing between a standard operating microscope (a–c) and the ORBEYE™ (d–f) during retrosigmoid cerebello-pontine angle approach in the supine position. Shown (d–f) is case 18, a microvascular decompression of the left facial nerve via retrosigmoid craniotomy in a supine patient. Classically, the retrosigmoid approach requires an awkward angulation of the OM and a consequently uncomfortable positioning for the surgeon given the orientation of the operative corridor as shown in a–c. Using the ORBEYE™, we were able to achieve visualisation that was potentially superior to the OM while maintaining normal posture (d–f) despite the angulation required with no compromise in the operative result
Photographic illustration of surgeon positioning during a midline parafalcine approach. Depicted is case 5, resection of a 3.8 cm posterior falcine meningioma accessed via the parietal interhemispheric approach, where significant microscope angulation is often required for adequate visualisation of paramedian pathology. In this case, we found that using the ORBEYE™ allowed superior visualisation with less need for adjustments and superior posture and comfort
Our neurovascular experience with the ORBEYE™ is limited to excision of a temporal arteriovenous malformation (AVM) and an MVD for hemi-facial spasm. We found the visualisation and ergonomics of surgeon and assistant’s positioning superior to our experience with the operating microscope. Other authors have also described excellent visualisation of the vasculature [14, 19, 24]. Khalessi et al. report the only other cases of AVM resection using the ORBEYE™, to our knowledge [14]. They described no issues with visualisation and found the exoscope to be particularly useful in a case of significant intraoperative bleeding where the large screen facilitated clearance of the operative field by the assistant and coordination of the staff. Nossek et al. reported their experience of five cases of STA-MCA bypass using the ORBEYE™ and had no issues with visualisation, describing it as subjectively superior to the OM [24]. Takahashi et al. also performed multiple MVDs, wherein they found the manoeuvrability of the ORBEYE™ superior to the OM as in their other cases performed via the retrosigmoid approach [34].
Other 3D 4K exoscopes are available, including the VITOM (Karl Storz, Tuttlingen, Germany) and KINEVO (Carl Zeiss AG, Oberkochen, Germany). The VITOM is the cheapest of the 3D 4K exoscopes at approximately $200,000, half the price of the ORBEYE™ ($400,000) [19]. The KINEVO costs significantly more ($1,500,000), though it consists of a hybrid design including the OM and exoscope, along with support for ICG and 5-ALA use, flow assessment and integrated neuronavigation [19]. While relatively economical, issues with the depth of field, illumination [5, 6] and ease of repositioning of the VITOM have been described [15, 33], though much literature on the VITOM relates to an older model. The VITOM was the first exoscope and originally did not have 3D or ultra-HD capability but has recently been upgraded, with multiple series demonstrating comparable outcomes of the new VITOM 3D to other 4K 3D exoscopic platforms (Table 3), though issues with visualisation appear to remain somewhat [6, 25]. A substantial proportion of literature relating to the VITOM focuses on the use of tubular retractors in tumour resection [1, 3, 7, 10, 13] and evacuation of intraparenchymal haemorrhage [2, 4, 9, 12, 18, 31]. A single series describing experience with the exoscope component of the KINEVO has been reported, with the users reporting similar limitations to visualisation [30] as the VITOM. In their prospectively randomised series, the authors experienced issues with maintaining lens focus in deep-seated areas among other issues, with the exoscope component found to be superior only in one component (upper body posture) of the ergonomic parameters evaluated. This resulted in switching from the exoscope to the OM component of the KINEVO in 50% of cases [30]. However, the KINEVO has both OM and exoscope capabilities, and so it is possible that the authors had a low threshold for switching. In our experience, these issues with focus in deep-seated areas were not present in the ORBEYE™.
Surgical outcomes
The influence of exoscope use on surgical outcomes is uncertain, though it is encouraging that there are no reports of a detrimental effect of the exoscope. It has been suggested that ergonomic benefit to exoscope usage will result in less surgeon fatigue and commensurately improved technique and outcomes, with an ergonomic study demonstrating the beneficial effects of a “heads-up” screen display over the eyepieces of the OM [36]. A systematic review found that outcomes were comparable between the exoscope and OM [29], indicating that it can be used in place of the OM where feasible.
The ORBEYE™ in surgical education
The exoscope has been proposed to improve the experience of observation by providing a more realistic view of procedures, akin to that of the operating surgeon [19,20,21]. While many OMs incorporate a video feed, this is usually not of comparable orientation or quality to that of the operating surgeon and is displayed in 2D. A systematic review found that a majority of studies described a significant benefit to the exoscope in terms of teaching, as the surgeon’s view is visible to the entire theatre [29]. Other authors have praised the educational value [14, 24, 34] and experience for assistants [17, 22, 24] of the ORBEYE™. Crucially for trainees, Nossek et al. found that using the ORBEYE™ improved participation throughout the procedure with more hands-on involvement of the co-surgeon [24].
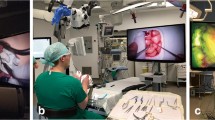
However, Takahashi et al. reported that the ORBEYE™ made the procedure more difficult for the assistant, for whom the screen was not oriented correctly to the operative field [34]. Khalessi et al. initially had similar issues, which were overcome with the addition of a second monitor [14]. Langer et al. detailed an alternative arrangement to overcome the problem with the use of a second screen and rotation of the image to match the assistant’s orientation [19], in a configuration that is especially useful for spinal surgery [17]. In our experience, an adequate operating room arrangement plan mitigated this drawback for cranial cases. By positioning the ORBEYE™ between the operating surgeon and the assistant (Fig. 3), both operators can work simultaneously with optimal orientation when the screen is placed in a line of sight directly perpendicular to the camera. We also found that the ORBEYE™ offers superior visualisation to the assistant which makes participation easier, akin to the experience of Nossek et al. [24]. Beyond the operating surgeons, we found that the ORBEYE™ also offered superior visualisation to observers which improved engagement and learning during the procedure. In contrast to our experience and that of other authors with the ORBEYE™, Burkhardt et al. found that half of the surgeons they surveyed found it more difficult to assist with the VITOM 3D as compared to the OM [6]. In their study, scrub nurses also found their positioning uncomfortable approximately 75% of the time. However, our scrub nurses did not experience this issue and additionally noted that the small physical footprint of the ORBEYE™ was beneficial, which aided set-up of the operating theatre. However, they did identify that instruments often needed to be passed in front of the assistant surgeon (Fig. 3), which can be cumbersome.
Learning curve
In our experience, one can adapt to the ORBEYE™ relatively quickly. Despite the short period of time we have been using the ORBEYE™, we did not have to switch to the OM in any of our cases. However, two important factors must be taken into account when considering the learning curve. Firstly, the senior author has experience with more than 500 endoscopic pituitary and skull base procedures and is therefore well used to operating while visualising the operative field on a screen. We feel that this made it very easy to transition from using an OM to using the ORBEYE™ for craniotomies. Secondly, the senior author always uses a foot pedal when using the OM during craniotomies. In our view, the use of a foot pedal is of paramount importance for the correct use of exoscopes. Without a foot pedal, manual adjustment of the ORBEYE™ causes shaking of the image on the screen which can be quite off putting. The use of a foot pedal almost eliminates this problem as handling of the ORBEYE™ is only necessary for significant repositioning. It also allows continuous bimanual surgery which potentially reduces surgical time. The previous version of the ORBEYE™ did not have a foot pedal, with zoom and focus having to be adjusted manually, causing significant issues [17]. Other authors have had similar experiences in this regard [14]. Kwan et al. [17] and Takahashi et al. [34] found surgeons who had performed more than five procedures with the ORBEYE™ tended to rate the experience higher than those who had performed less than five, a reflection of its quick learning curve. During the initial testing period, we performed a total of 6 procedures after which we felt we had completely adapted to the ORBEYE™ and were comfortable without an OM on standby.
Limitations
There are some limitations to our study. Firstly, our sample size was relatively small, assessing only 18 patients. Our subjective experience was limited to the perspective of a single surgeon who has 15 years’ experience in endoscopic surgery and is a regular user of the microscope foot pedal and therefore the results may not be generalisable.
Conclusion
In our experience, the ORBEYE™ offers excellent visualisation and improved ergonomics resulting in less surgeon fatigue and can be used safely in neurosurgery. In our series, we were able to use the ORBEYE™ for the entirety of all procedures and did not need to switch to the OM at any point. Other associated benefits include better visualisation and participation for assistant surgeons and enhancement of the learning experience. For neurosurgeons who are already accustomed to using a microscope foot pedal and also have experience in endoscopy, the learning curve for using the ORBEYE™ may be very short.
References
Akbari SHA, Sylvester PT, Kulwin C, Shah MV, Somasundaram A, Kamath AA, Beaumont TL, Rich KM, Chicoine MR (2019) Initial experience using intraoperative magnetic resonance imaging during a trans-sulcal tubular retractor approach for the resection of deep-seated brain tumors: a case series. Oper Neurosurg 16:292–301. https://doi.org/10.1093/ons/opy108
Alexopoulos G, Prim M, Khan M, Quadri N, Urquiaga JF, El Tecle N, Coppens J (2020) Minimally invasive evacuation of severe intraventricular hemorrhage using the brainpath endoport-assisted microsurgical system. World Neurosurg 134:e540–e548. https://doi.org/10.1016/j.wneu.2019.10.135
Bakhsheshian J, Strickland BA, Jackson C, Chaichana KL, Young R, Pradilla G, Chen JW, Bailes J, Zada G (2019) Multicenter investigation of channel-based subcortical trans-sulcal exoscopic resection of metastatic brain tumors: a retrospective case series. Oper Neurosurg 16:159–166. https://doi.org/10.1093/ons/opy079
Bauer AM, Rasmussen PA, Bain MD (2017) Initial single-center technical experiencewith the BrainPath system for acute intracerebral hemorrhage evacuation. Oper Neurosurg 13:69–76. https://doi.org/10.1227/NEU.0000000000001258
Beez T, Munoz-Bendix C, Beseoglu K, Steiger H-J, Ahmadi SA (2018) First clinical applications of a high-definition three-dimensional exoscope in pediatric neurosurgery. Cureus 10. https://doi.org/10.7759/cureus.2108
Burkhardt BW, Csokonay A, Oertel JM (2020) 3D-exoscopic visualization using the VITOM-3D in cranial and spinal neurosurgery. What are the limitations? Clin Neurol Neurosurg 198:106101–106101. https://doi.org/10.1016/j.clineuro.2020.106101
Day JD Transsulcal parafascicular surgery using brain path® for subcortical lesions. In, 2017/09//. Oxford University Press, pp 151-156. https://doi.org/10.1093/neuros/nyx324
De Divitiis O, D’Avella E, Denaro L, Somma T, Sacco M, D’Avella D (2019) Vitom 3D: preliminary experience with intradural extramedullary spinal tumors. J Neurosurg Sci. https://doi.org/10.23736/S0390-5616.19.04666-6
Eichberg DG, Di L, Shah AH, Luther EM, Jackson C, Marenco-Hillembrand L, Chaichana KL, Ivan ME, Starke RM, Komotar RJ (2020) Minimally invasive resection of intracranial lesions using tubular retractors: a large, multi-surgeon, multi-institutional series. J Neuro-Oncol 149:35–44. https://doi.org/10.1007/s11060-020-03500-0
Gassie K, Wijesekera O, Chaichana KL (2018) Minimally invasive tubular retractor-assisted biopsy and resection of subcortical intra-axial gliomas and other neoplasms. J Neurosurg Sci 62:682–689. https://doi.org/10.23736/S0390-5616.18.04466-1
Goehre F, Ludtka C, Schwan S (2020) Ergonomics of surgical microscopes for the sitting position as determined by ocular-corpus length. Surg Neurol Int 11. https://doi.org/10.25259/SNI_292_2020
Griessenauer C, Medin C, Goren O, Schirmer CM (2018) Image-guided, minimally invasive evacuation of intracerebral hematoma: a matched cohort study comparing the endoscopic and tubular exoscopic systems. Cureus 10. https://doi.org/10.7759/cureus.3569
Iyer R, Chaichana KL (2018) Minimally invasive resection of deep-seated high-grade gliomas using tubular retractors and exoscopic visualization. J Neurol Surg A Cent Eur Neurosurg 79:330–336. https://doi.org/10.1055/s-0038-1641738
Khalessi AA, Rahme R, Rennert RC, Borgas P, Steinberg JA, White TG, Santiago-Dieppa DR, Boockvar JA, Hatefi D, Pannell JS, Levy M, Langer DJ (2018) First-in-man clinical experience using a high-definition 3-dimensional exoscope system for microneurosurgery. Oper Neurosurg. https://doi.org/10.1093/ons/opy320
Krishnan KG, Schöller K, Uhl E (2017) Application of a compact high-definition exoscope for illumination and magnification in high-precision surgical procedures. World Neurosurg 97:652–660. https://doi.org/10.1016/j.wneu.2016.09.037
Kriss TC, Kriss VM (1998) History of the operating microscope: from magnifying glass to microneurosurgery. Neurosurgery 42. https://doi.org/10.1097/00006123-199804000-00116
Kwan K, Schneider JR, Du V, Falting L, Boockvar JA, Oren J, Levine M, Langer DJ (2019) Lessons learned using a high-definition 3-dimensional exoscope for spinal surgery. Oper Neurosurg 16:619–624. https://doi.org/10.1093/ons/opy196
Labib MA, Shah M, Kassam AB, Young R, Zucker L, Maioriello A, Britz G, Agbi C, Day JD, Gallia G, Kerr R, Pradilla G, Rovin R, Kulwin C, Bailes J (2017) The safety and feasibility of image-guided brainpath-mediated transsulcul hematoma evacuation: a multicenter study. Neurosurgery 80:515–524. https://doi.org/10.1227/NEU.0000000000001316
Langer DJ, White TG, Schulder M, Boockvar JA, Labib M, Lawton MT (2020) Advances in intraoperative optics: a brief review of current exoscope platforms. Oper Neurosurg 19:84–93. https://doi.org/10.1093/ons/opz276
Mamelak AN, Danielpour M, Black KL, Hagike M, Berci G (2008) A high-definition exoscope system for neurosurgery and other microsurgical disciplines: preliminary report. Surg Innov 15:38–46. https://doi.org/10.1177/1553350608315954
Mamelak AN, Nobuto T, Berci G (2010) Initial clinical experience with a high-definition exoscope system for microneurosurgery. Neurosurgery 67:476–483. https://doi.org/10.1227/01.NEU.0000372204.85227.BF
Murai Y, Sato S, Yui K, Morimoto D, Ozeki T, Yamaguchi M, Tateyama K, Nozaki T, Tahara S, Yamaguchi F, Morita A (2019) Preliminary clinical microneurosurgical experience with the 4K 3-dimensional microvideoscope (ORBEYE) system for microneurological surgery: Observation study. Oper Neurosurg 16:707–716. https://doi.org/10.1093/ons/opy277
Nishiyama K (2017) From exoscope into the next generation, vol 60. Korean Neurosurgical Society. https://doi.org/10.3340/jkns.2017.0202.003
Nossek E, Schneider JR, Kwan K, Kulason KO, Du V, Chakraborty S, Rahme R, Faltings L, Ellis J, Ortiz R, Boockvar JA, Langer DJ (2019) Technical aspects and operative nuances using a high-definition 3-dimensional exoscope for cerebral bypass surgery. Operative Neurosurgery 17:157–163. https://doi.org/10.1093/ons/opy342
Oertel JM, Burkhardt BW (2017) Vitom-3D for exoscopic neurosurgery: initial experience in cranial and spinal procedures. World Neurosurg 105:153–162. https://doi.org/10.1016/j.wneu.2017.05.109
ORBEYE 4K 3D Digital video microscope | Olympus Medical Systems. https://www.olympus-europa.com/medical/en/Products-and-Solutions/Products/Product/ORBEYE.html. Accessed 2020-12-27 2020
Oren J, Kwan K, Schneider J, Levine M, Langer D (2020) Minimally invasive navigated foraminal discectomy via contralateral approach using a 3-dimensional 4K high-definition exoscope: 2-dimensional operative video, vol 19. Oxford University Press. https://doi.org/10.1093/ons/opz392
Read JCA, Bohr I (2014) User experience while viewing stereoscopic 3D television. Ergonomics 57:1140–1153. https://doi.org/10.1080/00140139.2014.914581
Ricciardi L, Chaichana KL, Cardia A, Stifano V, Rossini Z, Olivi A, Sturiale CL (2019) The exoscope in neurosurgery: an innovative “point of view”. A systematic review of the technical, surgical, and educational aspects, vol 124. Elsevier Inc. https://doi.org/10.1016/j.wneu.2018.12.202
Roethe AL, Landgraf P, Schroder T, Misch M, Vajkoczy P, Picht T (2020) Monitor-based exoscopic 3D4k neurosurgical interventions: a two-phase prospective-randomized clinical evaluation of a novel hybrid device. Acta Neurochir 162:2949–2961. https://doi.org/10.1007/s00701-020-04361-2
Rutkowski M, Song I, Mack W, Zada G (2019) Outcomes after minimally invasive parafascicular surgery for intracerebral hemorrhage: a single-center experience. World Neurosurg 132:e520–e528. https://doi.org/10.1016/j.wneu.2019.08.087
Shimizu T, Toyota S, Nakagawa K, Murakami T, Mori K, Kishima H, Taki T (2020) Retrosigmoid approach in the supine position using ORBEYE: a consecutive series of 14 cases. Neurol Med Chir. https://doi.org/10.2176/nmc.tn.2020-0277
Shirzadi A, Mukherjee D, Drazin DG, Paff M, Perri B, Mamelak AN, Siddique K (2012) Use of the video telescope operating monitor (VITOM) as an alternative to the operating microscope in spine surgery. Spine 37:E1517–E1523. https://doi.org/10.1097/BRS.0b013e3182709cef
Takahashi S, Toda M, Nishimoto M, Ishihara E, Miwa T, Akiyama T, Horiguchi T, Sasaki H, Yoshida K (2018) Pros and cons of using ORBEYE™ for microneurosurgery. Clin Neurol Neurosurg 174:57–62. https://doi.org/10.1016/j.clineuro.2018.09.010
Uluç K, Kujoth GC, Başkaya MK (2009) Operating microscopes: past, present, and future. Neurosurg Focus 27:E4–E4. https://doi.org/10.3171/2009.6.FOCUS09120
Yu D, Green C, Kasten SJ, Sackllah ME, Armstrong TJ (2016) Effect of alternative video displays on postures, perceived effort, and performance during microsurgery skill tasks. Appl Ergon 53:281–289. https://doi.org/10.1016/j.apergo.2015.10.016
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All authors declare no competing interests.
Ethical approval
Ethical approval for this research was obtained from the local institutional review board.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurosurgery general
Rights and permissions
About this article
Cite this article
Amoo, M., Henry, J. & Javadpour, M. Beyond magnification and illumination: preliminary clinical experience with the 4K 3D ORBEYE™ exoscope and a literature review. Acta Neurochir 163, 2107–2115 (2021). https://doi.org/10.1007/s00701-021-04838-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-021-04838-8