Abstract
Background
Anterior temporal lobectomy is the most established neurosurgical procedure for temporal lobe epilepsy. Here we describe this technique.
Method
A temporal craniotomy is performed flush with the middle fossa and exposing the Sylvian fissure. The posterior extent of resection is determined as 4.5 cm in the dominant temporal lobe and 5.5 cm in the nondominant one. The first stage consists of removing the lateral neocortex and part of the fusiform gyrus, parallel to the Sylvian fissure, while keeping the temporal horn as the medial limit in the coronal plane. Then, the amygdala, uncus, fimbriae, hippocampus and collateral eminence are identified, transected and resected with the parahippocampal gyrus to complete the procedure.
Conclusion
Knowledge of the temporomesial anatomy, including neurovascular structures around the brainstem, is essential to keep this procedure safe and effective.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Temporal lobe resection for epilepsy was first performed in 1936 by Wilder Penfield, heralding the recognition of the role of this cerebral lobe in epileptogenesis and in particular of its mesial structures—with hippocampal sclerosis as the most encountered lesion. Various surgical approaches and techniques for temporal lobe epilepsy have since been proposed; the first to be introduced, and still the most established, is anterior temporal lobectomy (ATL), also known as “standard temporal lobectomy” or “2/3 temporal lobectomy.” Standard ATL as we know it today was introduced by Murray Falconer in the 1950s and 1960s [2]. It has been proven in a seminal study that ATL is superior to prolonged medical therapy in patients with drug-resistant temporal lobe epilepsy [10]. Recommendations suggest addressing these patients to referral centers for presurgical evaluation [5, 8]. Freedom from seizures is achieved in 60–80 % of these patients after ATL, in stark comparison to the <5 %/year of patients who do not undergo surgery but pursue medical treatment [1]. It must be noted that this is not an infrequent problem, since up to 30 % of temporal lobe epilepsy patients may remain refractory to medical treatment [2]. Furthermore, delaying surgical treatment may be deleterious in terms of both seizure and cognitive outcomes [4]. Although the strict definition of “drug resistance” was a matter of debate until 2010, it has since been officially considered as a failure in the treatment of two antiepileptic drugs, administered either sequentially as monotherapies or as a combined course [7].
Relevant surgical anatomy
See Fig. 1b for the temporal lobe’s lateral and inferior surface nomenclature. The lateral temporal surface lies underneath the squamous part of the temporal bone. The floor of the middle fossa is in the same plane as the superior surface of the zygomatic arch [6].
(a) Axial T2-weighted MRI depicting the right uncal apex (long white arrow), left free rim of the tentorium cerebelli (triple white arrows), right internal carotid artery (full white arrowhead), right posterior communicating artery (full black arrowhead) and P1 segment of the right posterior cerebral artery (hollow white arrowhead) seen anastomosing with the posterior communicating artery. The uncal apex faces the oculomotor nerve; the anterior segment of the uncus faces the carotid artery and its cistern, and the posterior uncal segment is vis-à-vis the cerebral peduncle, posterior cerebral artery and anterior choroidal artery. The ambient cistern separates these structures from the brainstem. (b) Coronal T2-weighted MRI in the right temporal lobe indicating the Sylvian fissure (white arrowhead), superior temporal sulcus (full white arrow), inferior temporal sulcus (double-shafted white arrow), occipitotemporal sulcus (thin white arrow) and collateral sulcus (black empty arrow); between these sulci the superior (T1), middle (T2) and inferior (T3) temporal gyri, fusiform gyrus (T4, also called the lateral occipitotemporal gyrus) and parahippocampal gyrus (T5, also called the medial occipitotemporal gyrus) can respectively be seen. Note how T3 passes over the inferior edge of the temporal lobe’s lateral surface. (c) Enlarged white window seen in (b) showing a coronal section through the body of the left hippocampus. Temporal horn of the left lateral ventricle (thick white arrow); fimbria of the hippocampus (black arrowhead); dentate gyrus (empty black arrow)—the shaft of this empty black arrow is located in the choroidal fissure; parahippocampal gyrus (asterisk); fusiform gyrus (double asterisk); relation between the collateral sulcus and its imprint in the temporal horn’s floor, called the collateral eminence (curved white arrow); P2 segment of the left posterior cerebral artery (empty white arrow) coursing in the ambient cistern; tentorium cerebelli (triple black arrow); temporal stem (dashed white line)
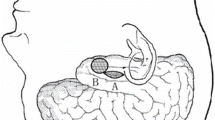
The medial temporal surface is formed anteriorly by the medial temporal pole, which is in continuation with the anterior segment of the uncus, culminating in its medially pointing apex (Fig. 1a). The hippocampal head is in direct connection with the posterior uncus and the amygdala with the anterior uncus. The fimbriae (Fig. 1c) appear at the posterior border of the uncus (Fig. 2g-h).
Intraoperative views illustrating the surgical phases and encountered anatomy (see video for more details). (a) Right temporal craniotomy; the temporal tip is in the upper left corner of the picture, and the Cushing needle, seen parallel to the superficial Sylvian vein, is lodged against it in order to measure the 5.5-cm posterior limit of resection. (b) A Merocel® sponge is placed to delineate this posterior limit. The pia mater is coagulated along this line and along a line a few millimeters below the Sylvian fissure in order to leave a protective lip of the superior temporal gyrus over the Sylvian fissure and its vessels. This coagulated tissue is then incised using scissors. (c) While keeping the plane of the middle fossa in mind, ultrasonic dissection through the lateral part of the temporal lobe is performed until the temporal horn is opened (d). (e) The plane of dissection then turns perpendicularly to follow the temporal horn; its lateral wall is opened along its length. The medial limit of the lateral temporal lobectomy is therefore the collateral eminence. (f) After the lateral temporal lobectomy, the uncus is identified (seen under the suction aspiration) and is resected using ultrasonic aspiration. (g) The head of the hippocampus lies in the posteromedial part of the uncus, and the fimbria originates at its posterior border, seen to the left of the picture. The fimbriae are seen as a white band at the tip of the dissector. The dissector is pulling at the hippocampus, i.e., the medial wall of the temporal horn, and the ultrasonic aspirator is seen transecting the hippocampal body posteriorly. (h) Same configuration as in (g). The fimbriae of the hippocampus are resected using ultrasonic aspiration. (i) While gently pulling the hippocampus away from the medial cisterns using a large dissector, subpial resection of the temporomesial structures below the fimbriae is performed, i.e., the dentate gyrus (not seen) and medial parahippocampal gyrus (seen as gray and white matter immediately to the right of the ultrasonic aspiration). (j) The inferior surface of the parahippocampal gyrus is detached at its interface with the medial fusiform gyrus, the lateral portion of the fusiform gyrus having already been resected as part of the lateral temporal lobectomy
Intraoperative view with ATL seen in Fig. 2. Right oculomotor nerve (full black arrowhead); internal carotid artery (white arrow); anterior petroclinoid fold of the tentorium cerebelli (triple black arrowheads). Note that the medial pia arachnoid is preserved intact and acts as a veil to protect medial neurovascular structures
Further posteriorly, the medial surface is formed by the medial aspect of the parahippocampal gyrus, dentate gyrus and, superior to it, fimbria (Fig. 1c). The choroidal fissure is the recess found between the fimbria and inferolateral thalamus (anteriorly the lateral geniculate body and more posteriorly the pulvinar). The inferior choroidal point is situated posterior to the hippocampal head and anterior to the lateral geniculate body. This is the point where the anterior choroidal artery enters into the temporal horn of the lateral ventricle; it is also the choroidal fissure’s anterior limit [3, 6]. Resection of mesial structures should not extend superior to this limit, as one risks entering the external pallidum [1].
The amygdala constitutes the anterior wall and superomedial roof of the tip of the temporal horn. The hippocampus (head and body) forms the medial ventricular wall; it has a whitish appearance. The collateral eminence, which corresponds to the collateral sulcus’ intraventricular imprint as it runs deep, is a bulge in the temporal horn’s floor (Fig. 1c). Tapetal, i.e., callosal fibers constitute the greater part of the roof and the lateral wall of the temporal horn. The temporal optic fibers that form Meyer’s loop course over these fibers, but do not run over the anterior portion of the temporal horn’s lateral wall. Furthermore, the loop’s anterior extension is interindividually variable.
The temporal stem is the area between the roof of the temporal horn and inferior insular limiting sulcus in direct prolongation from the limen insulae (Fig. 1c). Although ATL implies transecting the temporal stem, this structure should not be breached cranially and medially because of the risk of injuring the basal ganglia.
Description of the technique
Surgery consists of three principal steps at three different levels: (1) temporal craniotomy (superficial level); (2) removal of the lateral neocortical block (superficial/intermediate levels); (3) resection of the mesiotemporal structures (intermediate/deep levels).
-
1.
Head rotated and fixed at 90° (temporal squama in the horizontal plane, floor of the middle fossa perpendicular to this plane). Inverse question mark incision, anterior to the tragus and following the superior temporal line. Maximal anterobasal reflection of the temporal muscle. Temporal craniotomy with the superior limit slightly above the squamous suture, i.e., 0.5 cm above the Sylvian fissure. Durotomy should expose the Sylvian fissure, T1, T2 and upper T3. Anterior 2.5 cm of the temporal pole is usually covered by bone (Fig. 2a).
-
2.
A Cushing cannula is used to measure the posterior limit of the ATL (Fig. 2a), which is marked by coagulation of the pia mater (Fig. 2b). The vein of Labbé is preserved. Piercing the pia with one branch of the bipolar forceps ensures that the entire pia, including its vessels, is coagulated. Pial coagulation of T1 parallels the Sylvian fissure at 5 mm distance from it (Fig. 2b) to avoid inadvertent coagulation of undulating small interarachnoid arteries supplying structures outside the temporal lobe. The coagulated pia is cut with microscissors (Fig. 2b). Resection of the lateral neocortical block using ultrasonic aspiration follows (Fig. 2c). At the posterior border of resection, in a coronal plane, the medial limit of this surgical step consists of opening the lateral ventricle’s temporal horn (Fig. 2d). CSF outflow, even through a small opening, signals that this goal has been achieved. Having determined the depth of the temporal horn, ultrasonic aspiration of T1, parallel to the Sylvian fissure, is performed toward the pole. The basal limit of posterior resection is then extended toward the floor of the middle fossa. The pia is coagulated and cut, liberating the posteroinferior part of the tissue block. Ultrasonic aspiration is continued along the length of the temporal horn (Fig. 2e) to the level of the polar and basal arachnoid, which is cut, allowing en bloc resection of the lateral neocortical bloc.
-
3.
The following anatomical landmarks aid in orientation: the hippocampus, ependyma and choroid plexus of the temporal horn, choroidal fissure and collateral eminence (Fig. 2f). The amygdala, not readily recognizable, is the structure protruding into the ventricle anteriorly and superiorly to the choroidal point. It is resected using ultrasonic aspiration. At the junction between the amygdala and hippocampal head, resection is continued mesially, and the uncus (Fig. 2f) is thereby removed. Resection of the hippocampal head is continued from within its pial envelope. The collateral eminence is coagulated and subpially aspirated down to the tentorium. In this way, the entorhinal cortex and parts of the parahippocampal and fusiform gyri are removed as well. A 2.5–3.5-cm length of hippocampal resection is efficient in a standard ATL. The hippocampal body—left untouched so far—is coagulated and transected at the level of the posterior limit of resection (Fig. 2g). The fimbriae are aspirated along the choroidal fissure (Fig. 2h). Tissue is aspirated from both sides of the hippocampal mesentery (Fig. 2i), which contains small hippocampal arteries and veins that arise at a right angle from the larger mesiotemporal vessels. These vessels are coagulated and cut at their very distal entry point in the hippocampus to avoid coagulation of an intra-arachnoid loop of the anterior choroidal artery (Fig. 2j). Finally, the coagulated mesentery is cut and the remaining hippocampal tissue removed together with it and sent for neuropathological examination. The surgical field is irrigated, followed by standard closure.
Indications
Refractory temporal lobe epilepsy. Although a more selective approach—such as selective amygdalohippocampectomy—may be warranted in cases of a mesiotemporal origin of seizures where resection can be performed without lateral temporal cortical resection, ATL is particularly indicated for lesional or nonlesional epilepsy of diffuse temporal lobe origin.
Limitations
None.
How to avoid complications
-
Posterior border of the resection limit: 5.5 cm (nondominant lobe; Figs. 2 and 4), 4.5 cm (dominant lobe).
Fig. 4 T1-weighted MRI of a 12-year-old patient, shown in Figs. 2 and 3, with intractable epilepsy, left hemiparesia and diminished cognitive capabilities secondary to herpetic encephalitis at 11 months of age. (a–c) Preoperative MRI reveals right temporopolar and temporomesial postherpetic sequelae. Preoperative investigations (MRI, PET-CT, SPECT, video-EEG) point to a right temporal origin to the seizures. (d–f) Postoperative MRI in the same patient illustrates the extent of resection in the axial, coronal and sagittal planes. Note also the relation between the resection cavity and temporal stem
-
Preserve the vein of Labbé and prominent temporobasal veins.
-
Visualization of the temporal horn (Fig. 2d) and tentorial dura (Fig. 2d and g): important landmarks that prevent blind dissection too medially.
-
Preserve the temporomesial pia arachnoid as a protective veil over underlying neurovascular structures (Fig. 3).
-
Turn down the ultrasonic aspirator as these structures are approached.
-
In case of mesial pial bleeding, apply sponge/fibrillary hemostatics. Avoid coagulation whenever possible!
-
Neuronavigation can be useful in avoiding transgression into the basal ganglia during resection of the amygdala; nonetheless, ATL remains a standardized procedure heavily relying on the understanding of anatomical landmarks.
Specific perioperative considerations
-
Perform complete epileptological workup to ascertain a temporal origin of seizures and epileptogenic zone.
-
Perform functional MRI if there is doubt concerning hemispheric dominance.
-
Maintain antiepileptic medication pre- and postoperatively. In the absence of postoperative seizures, consider tapering after 3–12 months [9].
Specific information for the patient and family about surgery and potential risks
-
Freedom from seizures: 60–80 % (compared to <5 %/year of patients who pursue medical treatment) [1].
-
Mortality: <1 %.
-
Morbidity: <5 %; permanent morbidity: 1–2 %.
-
Visual field defects (varying degree of upper contralateral quadrantanopia; not included above): 50 % [2].
-
Neuropsychological performance can improve in 1/3 of cases, but can deteriorate in 50 % of patients; cognitive—most markedly memory—decline: More frequent with dominant lobe operations [5].
References
Chang EF, Englot DJ, Vadera S (2015) Minimally invasive surgical approaches for temporal lobe epilepsy. Epilepsy Behav 47:24–33
Clusmann H, Schramm J (2012) Surgery in adults: temporal resections. Handb Clin Neurol 108:897–913
Destrieux C, Bourry D, Velut S (2013) Surgical anatomy of the hippocampus. Neurochirurgie 59:149–158
Engel J Jr, McDermott MP, Wiebe S, Langfitt JT, Stern JM, Dewar S, Sperling MR, Gardiner I, Erba G, Fried I, Jacobs M, Vinters HV, Mintzer S, Kieburtz K, Early Randomized Surgical Epilepsy Trial Study G (2012) Early surgical therapy for drug-resistant temporal lobe epilepsy: a randomized trial. JAMA 307:922–930
Engel J Jr, Wiebe S, French J, Sperling M, Williamson P, Spencer D, Gumnit R, Zahn C, Westbrook E, Enos B, Quality Standards Subcommittee of the American Academy of N, American Epilepsy S, American Association of Neurological S (2003) Practice parameter: temporal lobe and localized neocortical resections for epilepsy: report of the quality standards subcommittee of the American Academy of Neurology, in association with the American Epilepsy Society and the American Association of Neurological Surgeons. Neurology 60:538–547
Kucukyuruk B, Richardson RM, Wen HT, Fernandez-Miranda JC, Rhoton AL Jr (2012) Microsurgical anatomy of the temporal lobe and its implications on temporal lobe epilepsy surgery. Epilepsy Res Treat 2012:769825
Kwan P, Arzimanoglou A, Berg AT, Brodie MJ, Allen Hauser W, Mathern G, Moshe SL, Perucca E, Wiebe S, French J (2010) Definition of drug resistant epilepsy: consensus proposal by the ad hoc task force of the ILAE commission on therapeutic strategies. Epilepsia 51:1069–1077
Kwan P, Sperling MR (2009) Refractory seizures: try additional antiepileptic drugs (after two have failed) or go directly to early surgery evaluation? Epilepsia 50(Suppl 8):57–62
Rathore C, Panda S, Sarma PS, Radhakrishnan K (2011) How safe is it to withdraw antiepileptic drugs following successful surgery for mesial temporal lobe epilepsy? Epilepsia 52:627–635
Wiebe S, Blume WT, Girvin JP, Eliasziw M, Effectiveness, Efficiency of Surgery for Temporal Lobe Epilepsy Study G (2001) A randomized, controlled trial of surgery for temporal-lobe epilepsy. N Engl J Med 345:311–318
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
10 key points
- Positioning: Horizontal
- Craniotomy: Strictly temporal with clear exposure of the Sylvian fissure
- Clear demarcation of the resection zone
- Lateral neocortical en bloc temporal resection
- Stop medial dissection after opening of the temporal horn to preserve mesial structures
- Identification of mesial structures as relevant anatomical landmarks
- Resection of the amygdala and uncus
- Hippocampal isolation by transection of the collateral eminence down to the arachnoid level and resection of the parahippocampal gyrus
- Resection of the fimbria
- Hippocampal resection by disconnection from its mesentery
Electronic supplementary material
Below is the link to the electronic supplementary material.
A right temporal craniotomy is performed exposing the floor of the middle fossa and Sylvian fissure, and the posterior limit of resection is determined at 5.5 cm from the temporal pole. Using ultrasonic aspiration, resection of the lateral temporal neocortical block is performed after identification of the temporal ventricular horn, followed by the resection of the uncus, fimbria, hippocampus and parahippocampal gyrus. (M4V 80277 kb)
Rights and permissions
About this article
Cite this article
Schaller, K., Cabrilo, I. Anterior temporal lobectomy. Acta Neurochir 158, 161–166 (2016). https://doi.org/10.1007/s00701-015-2640-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-015-2640-0