Abstract
Purpose
To determine the timing of symptomatic venous thromboemboli (VTE) in patients sustaining a pelvic and/or acetabular fracture. Secondly, to evaluate for any factors that may influence this timing.
Methods
A retrospective cohort of 47 patients with acetabular and/or pelvic ring injuries who developed VTEs at a single academic level I trauma center were identified from 2012 to 2018. The chronology of VTE diagnosis in relation to date of injury, initial surgery, final surgery, and date of discharge was evaluated. Patients who developed VTEs were then evaluated based on known risk factors for VTE to determine if any of these affected timing.
Results
Symptomatic VTEs were diagnosed in 3.8% of patients with pelvic and/or acetabular fractures. In patients who developed a thromboembolism, diagnosis occurred on average 21.5 (± 19.2), 20.7 (± 19.9), 9.8 (± 23.4), and 4.3 (± 27.6) days after injury, index procedure, final procedure, and date of discharge. 25% of patients developed VTE more than 4 weeks after their initial injury. No known risk factors effected the timing of VTE.
Conclusion
The 2015 OTA expert panel recommends 4 weeks of anticoagulation for orthopedic trauma patients at high risk of VTE, which may be too short a duration. In our cohort, 25% of VTEs occurred greater than 4 weeks after injury. Additional research is needed to clarify the exact duration of anticoagulation after pelvic and acetabular fractures; however, surgeons may want to consider anticoagulating patients for greater than 4 weeks.
Level of evidence
Level III—retrospective cohort.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Venous thromboemboli (VTE) are a commonly encountered postoperative surgical complication that cause significant morbidity and mortality. In trauma, pulmonary emboli (PE) are the most common cause of death more than seven days after initial injury [1]. Risk factors that have been identified as increasing the risk of postoperative deep vein thrombosis (DVT) in trauma patients include age ≥ 40, extremity injury, BMI > 30, head injury, ventilator days ≥ 3, venous injury, spinal cord injury, pelvic fracture, and major surgery [2,3,4,5,6,7,8,9,10,11]. Patients with orthopedic injuries are at increased risk of DVT, particularly those with pelvic and acetabular fractures, with reports of rates from 0.21 to 41% for DVT and 0–21.7% for PE [3, 11].
Literature evaluating VTEs in pelvic and acetabular fractures has shown mixed results on whether there is a significant difference in the rate between pelvic and acetabular fractures [12,13,14]. However, they have demonstrated an increased incidence of DVT in patients with associated acetabular fracture patterns compared to elementary patterns and posterior acetabular fractures requiring a Kocher–Langenbeck approach. In pelvic ring injuries, vertical shear fractures were associated with increased development of DVT compared to lateral compression and anterior–posterior compression injuries [13,14,15].
Although many studies exist which examine risk factors for the development of VTE’s in orthopedic injury, there is a paucity of information regarding the timeline in which VTE. The recent study, PREVENTion of Clots in Orthopedic Trauma (PREVENT CLOT), evaluates symptomatic VTEs and 90-day all-cause mortality in 12,211 patients with operatively treated extremity fractures or any pelvic or acetabular fracture receiving aspirin versus enoxaparin. This study found symptomatic DVTs occurred at a median of 16 days (interquartile range 7–35) and symptomatic PEs at a median of 7 days (interquartile range 3–22) [16]. However, to the best of the authors knowledge, no papers specifically evaluate the timing of VTEs in relation to pelvic and/or acetabular fractures.
Information on the chronology of VTEs could help to guide recommendations for timing of post injury anticoagulation. Current recommendations support beginning anticoagulation within 24 h of admission or hemodynamic stability which has been found to decrease the risk of VTE [17,18,19]. However, there is no consensus on length of anticoagulation following pelvic and acetabular fractures, and sparce information guiding length of treatment [11]. A 2009 Cochrane review of prolonged thromboprophylaxis for 4 weeks with LMWH in patients undergoing major abdominal or pelvic surgery as compared with inhospital prophylaxis only showed a significant reduction in the risk of VTE without concomitant increase in bleeding complications [20]. The OTA expert panel in 2015 recommended prolonged prophylaxis (approximately 4 weeks) for patients at high risk for VTE (elderly patients with a proximal femur and multiple trauma patients) [19]. The ACCP recommends at least 10–14 days and up to 35 days of anticoagulation for hip fractures and recommends prophylaxis, without a specific duration provided, for patients with major pelvic or lower extremity trauma [21, 22]. A more thorough understanding of the timing of VTEs would help guide duration of post injury and post-surgery thromboprophylaxis.
This study has two aims. First, to identify the timeline in which symptomatic VTEs occur in patients with pelvic and acetabular fractures in relation to their injury, index procedure, final procedure, and discharge. Allowing the clinician to have a heightened sense of suspicion for when VTEs are most likely to occur and to help guide duration of thromboprophylaxis. Second, to identify what factors may alter the timing of the development of VTE.
Methods
Institutional review board approval was obtained to study the selected patient population. Patients sustaining a pelvic or acetabular fracture from 2012–2018 were reviewed for development of a symptomatic VTE. Diagnosis date of a symptomatic VTE was based on one of the following: presence of positive computed tomography scan with pulmonary embolism protocol (CT PE), positive lower extremity doppler ultrasound, or chart documentation of VTE and initiation of treatment dose anticoagulation. Inclusion criteria were patients with acetabular or pelvic ring fractures based on the following CPT codes: pelvic fractures 27193, 27194, 27197, 27198, 27215, 27216, 27217, and 27218; acetabulum fractures 27220, 27222, 27226, 27227, and 27228, who developed a VTE. Exclusion criteria included patients who had developed a VTE prior to the trauma producing a pelvic or acetabular fracture, those patients developing a VTE more than 90 days after injury, or those patients where a date of VTE diagnosis could not be ascertained.
During the study timeframe the institutional protocol for VTE prophylaxis was 30 days of enoxaparin 30 mg twice daily. Aspirin 325 mg daily was used as an alternative for patients without insurance or who were unable to afford enoxaparin.
Demographic data, injury, and fracture characteristics were collected for each patient including age, sex, BMI, mechanism of injury, fracture laterality, presence or absence of additional lower extremity fractures, open versus closed injury, smoking status, type of anticoagulation received, whether the patient received a red blood cell transfusion, whether or not the patient required ICU care and/or mechanical ventilation and fracture type and classification.
Chronology data were then obtained from patients’ who developed a VTE. Variables evaluated included: date of injury, date of initial surgery, date of final surgery, and date of hospital discharge. These dates were then evaluated in relation to the date of VTE diagnosis and each other to find the length of stay, time from injury to VTE, time from initial surgery to VTE, time from final surgery to VTE, time from discharge until VTE, time from injury until initial and final surgeries, and days from initial surgery until final surgery. Number of days in the ICU and number of days on a ventilator were also evaluated.
Measures of central tendency and spread were calculated for the following chronologic variables: length of stay, time from injury to VTE, time from initial surgery to VTE, time from final surgery to VTE, time from discharge until VTE, time from injury until initial and final surgeries, and days from initial surgery until final surgery, number of days in the ICU, and number of days on a ventilator.
Chronologic variables were then further evaluated based on sex, smoking status, presence or absence of red blood cell transfusion, BMI (healthy, overweight, and obese), age (≥ 40 versus < 40), type of anticoagulant, presence of additional lower extremity fractures, fracture (pelvic, acetabulum, and combined), operative versus nonoperative management, and whether patients required mechanical ventilation and/or a stay in the ICU for possible significance with timing of VTE. T-tests were used to determine statistical significance for single variable analyses and ANOVA tests were used for multiple variable analyses.
Results
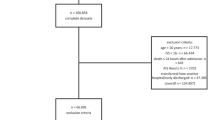
There were 1224 patients identified with pelvic and/or acetabular fractures treated at our institution from 2012–2018. Fifty-three patients were diagnosed with a symptomatic VTE (Fig. 1). Of these 2 VTE’s occurred greater than 90 days after initial injury and for 4 patients an exact date of VTE diagnosis was unavailable and thus the patients were excluded.
The overall rate of VTE was 3.8% (47 patients). The average time from injury to VTE diagnosis was 21.5 days (± 19.2), time from initial surgery to VTE diagnosis was 20.7 days (± 19.9), time from final surgery to VTE diagnosis 9.8 (± 23.4), and time from discharge to VTE diagnosis 4.3 (± 27.6) (Table 1, Figs. 2 and 3). The median time of diagnosis was 17, 16, 7, and 5 days for time from injury, initial surgery, final surgery, and discharge, respectively.
Cumulative number of VTEs after date of injury with days post injury in the x axis. 4-week mark indicated which represents that current 2015 OTA expert panel recommendation for anticoagulation, note that this timepoint occurs while the number of VTEs is still increasing in a linear fashion. Two plateau points are seen on the graph at 5 weeks and 8 weeks, respectively
None of the variables evaluated—sex, smoking status, presence or absence of red blood cell transfusion, BMI, age (≥ 40 versus < 40), type of anticoagulant, presence of additional lower extremity fractures, fracture (pelvic, acetabulum, or combined), operative management, requiring mechanical ventilation or a stay in the ICU—had any statistically significant effect on the timing of VTE development (Table 2).
Discussion
Multiple studies exist evaluating risk factors for the development of VTE following pelvic and acetabular trauma. The goals of this study were therefore not to evaluate which factors increased the incidence of VTEs, but rather to evaluate the timing of VTE development in patients with pelvic and acetabular fractures, and to see which, if any, factors known to increase VTE incidence would affect the timing of the development of VTEs.
In the studied patient population, we found that VTEs, when symptomatic, occurred an average of 21.5 (± 19.2), 20.7 (± 19.9), 9.8 (± 23.4), 4.3 (± 27.6) days after injury, initial surgery, final surgery, and hospital discharge, respectively. The smaller average, but large spread, of patients developing VTEs in relation to their final surgery was influenced by 12 patients who developed a VTE after their initial surgery but before their final surgery. This included 2 patients who had other late complications requiring return to the OR greater than 1 month after sustaining their injury and thus had values of −50 and −40 days, respectively. The same effect is seen in relation to patient discharge with 15 patients developing a VTE prior to hospital discharge including one who developed it on the 5th day of an 80-day long hospital admission. Interestingly there was not a significant difference in the timing of VTEs in patients managed operatively (22.4 ± 19.8) versus nonoperative (16.6 ± 16.6, p = 0.468). Therefore, we feel that using the time from injury gives the surgeon the most accurate understanding of when to expect this complication. This is further substantiated by a similar median time to the development of VTE from injury of 17 days.
Using the time from injury for evaluation, 75% (35/47) of the VTEs occurred within the first 4 weeks after injury. Based on 2015 OTA expert panel recommendations these VTEs would all have fallen in the time frame of recommended chemoprophylaxis for patients at high risk of VTE. Conversely 25% of VTEs occurred more than 4 weeks after the initial injury, which based on the OTA expert panel recommendations, would have occurred after cessation of chemoprophylaxis. Extending prophylaxis to 5 or 8 weeks after initial injury would decrease the uncovered rate from 25 to 17% and 6%, respectively. However, extending VTE prophylaxis is not entirely benign as there is a risk of increased bleeding events for patients receiving anticoagulation. A recent meta-analysis of medical patients on extended DVT prophylaxis found that the number needed to harm to cause one major or fatal bleeding event was 333 [23]. Additionally, patient compliance with anticoagulation is not perfect, and medications that require injection show decreased compliance compared to oral medications; for example in the PREVENT CLOT study outpatient compliance with aspirin was 94.4% while enoxaparin was only 86.6% [16]. It is also important to note that VTEs still occur despite adherence to anticoagulation regimens, often representing a failure of prophylaxis rather than a failure to provide prophylaxis.
As stated previously, the goal of this study was to evaluate factors that affected the chronologic occurrence of VTEs, not the incidence, therefore only patients who developed symptomatic VTEs were evaluated. Eleven factors previously reported to increase VTE incidence were evaluated for an effect on the timing of VTEs. None of the eleven factors were found to significantly increase or decrease the time at which VTEs occurred.
A recent meta-analysis found the rate of VTE to be from 0.21 to 41% for DVT and 0 to 21.7% for PE; our VTE rate falls within this range at 3.8%; however, this represents a broad range [11]. Our rate of 3.8% is also similar to the rate of symptomatic DVT of 2.1% (254/12,211) and PE of 1.5% (180/12,211) seen in the PREVENT CLOT study which included all operative extremity fractures or any pelvic or acetabular fracture [16]. As far as we know this is the first study to look at timing of VTE’s in pelvic and acetabular fractures. There are other studies which evaluate the timing of multiple complications following spinal surgery, rotator cuff repair, total joint arthroplasty, ankle fracture surgery, and hip fracture surgery. These studies range with an average time for postoperative DVT occurrence of 7–17 days post-op and PE occurrence of 3–14 days post-op for spinal surgery, arthroplasty, ankle fracture surgery, and hip fracture surgery [24,25,26,27,28]. And an average VTE diagnosis at 11.5 ± 7.4 days for rotator cuff repair [29]. Our average time of VTE diagnosis is greater than reported in these studies with a mean of 20.7 (± 19.9) days from first surgery and a median of 16 days. This could represent a true difference or may represent delayed diagnosis secondary to patient presentation or clinical suspicion. Additionally, one of the studies used median time instead of mean showing a median post-op DVT and PE diagnosis at 8–10.5 and 5 days, respectively, depending on the particular spinal procedure performed. These numbers, however, are still lower than the median time of VTE diagnosis post initial surgery found in our patients [24]. Conversely, in the prevent clot study symptomatic DVTs occurred at a median of 16 days (interquartile range 7–35) which is similar to our median time to the development of VTE from injury of 17 days [16].
There are multiple limitations to our study. First, although we have a complication rate similar to that found in the literature, we have a relatively small absolute sample size of 47 patients with VTEs. This number further decreased for each studied category as only 40 patients were managed operatively, and 36 patients required multiple surgeries. Additionally, due to the small sample size, DVTs and PEs were evaluated together as VTEs, rather than separately, to increase the statistical power. Further research on the timing of VTEs in pelvic and acetabular fractures with a larger sample size is required to bolster or refute the findings of this paper, and help guide recommended length of anticoagulation. Second, our studied patient population was a single tertiary care center. Patients who had symptomatic VTEs after discharge may have presented to other care centers which would influence the results of our data. Third, an assumption was made that date of recorded VTE diagnosis represented date of symptom onset which may not hold true in all circumstances, particularly if a patient was to delay in presenting for care. This would result in true values being shorter than what was found in our study.
Conclusion
There is currently no consensus on length of anticoagulation in patients sustaining pelvic and/or acetabular fractures. The 2015 OTA expert panel recommends anticoagulation for 4 weeks; 25% of VTEs occurred greater than 4 weeks after injury. Additional research is needed to clarify exact duration of anticoagulation after pelvic and acetabular fractures; however, surgeons may want to consider anticoagulating patients for greater than 4 weeks in the setting of a pelvic and/or acetabular fracture. A duration of 5 weeks would encompass 83% of VTEs and 8 weeks would encompass 94% of VTE occurrences.
References
Webb LX, Rush PT, Fuller SB, Meredith JW (1992) Greenfield filter prophylaxis of pulmonary embolism in patients undergoing surgery for acetabular fracture. J Orthop Trauma 6(2):139–145
Buerger P, Peoples J, Lemmon G, McCarthy MC (1993) Risk of pulmonary emboli in patients with pelvic fractures. Am Surg 59(8):505–508
Geerts WH, Code KI, Jay RM, Chen E, Szalai JP (1994) A prospective study of venous thromboembolism after major trauma. N Engl J Med 331(24):1601–1606
Haut ER, Chang DC, Pierce CA et al (2009) Predictors of posttraumatic deep vein thrombosis (DVT): hospital practice versus patient factors—an analysis of the National Trauma Data Bank (NTDB). J Trauma Acute Care Surg 66(4):994–1001
Knudson MM, Collins JA, Goodman SB, McCRORY DW (1992) Thromboembolism following multiple trauma. J Trauma 32(1):2–11
Knudson MM, Lewis FR, Clinton A, Atkinson K, Megerman J (1994) Prevention of venous thromboembolism in trauma patients. J Trauma 37(3):480–487
Kudsk KA, Fabian TC, Baum S, Gold RE, Mangiante E, Voeller G (1989) Silent deep vein thrombosis in immobilized multiple trauma patients. Am J Surg 158(6):515–519
Napolitano LM, Garlapati VS, Heard SO et al (1995) Asymptomatic deep venous thrombosis in the trauma patient: is an aggressive screening protocol justified? J Trauma Acute Care Surg 39(4):651–659
Rogers FB, Shackford SR, Ricci MA, Huber BM, Atkins T (1997) Prophylactic vena cava filter insertion in selected high-risk orthopaedic trauma patients. J Orthop Trauma 11(4):267–272
Velmahos GC, Kern J, Chan LS, Oder D, Murray JA, Shekelle P (2000) Prevention of venous thromboembolism after injury: an evidence-based report—part II: analysis of risk factors and evaluation of the role of vena caval filters. J Trauma Acute Care Surg 49(1):140–144
Mahmoud SS, Esser M, Jain A (2022) Thromboembolic events in pelvic and acetabulum fractures: a systematic review of the current literature on incidence, screening, and thromboprophylaxis. Int Orthop 46:1707–1720
Niikura T, Lee SY, Oe K et al (2012) Incidence of venous thromboembolism in pelvic and acetabular fractures in the Japanese population. J Orthop Sci 17(3):233–238
Kim J-W, Oh C-W, Oh J-K et al (2014) The incidence and the risk factors of venous thromboembolism in Korean patients with pelvic or acetabular fractures. J Orthop Sci 19(3):471–477
Wang P, Kandemir U, Zhang B et al (2019) Incidence and risk factors of deep vein thrombosis in patients with pelvic and acetabular fractures. Clin Appl Thromb Hemost 25:1076029619845066
Sen RK, Kumar A, Tripathy SK, Aggarwal S, Khandelwal N (2011) Risk factors of venous thromboembolism in Indian patients with pelvic-acetabular trauma. J Orthop Surg 19(1):18–24
Consortium METR (2023) Aspirin or Low-Molecular-Weight Heparin for Thromboprophylaxis after a Fracture. N Engl J Med 388(3):203–213
Steele N, Dodenhoff R, Ward A, Morse M (2005) Thromboprophylaxis in pelvic and acetabular trauma surgery: the role of early treatment with low-molecular-weight heparin. J Bone Joint Surg 87(2):209–212
Monzon DG, Iserson KV, Cid A, Vazquez JA (2012) Oral thromboprophylaxis in pelvic trauma: a standardized protocol. J Emerg Med 43(4):612–617
Sagi HC, Ahn J, Ciesla D et al (2015) Venous thromboembolism prophylaxis in orthopaedic trauma patients: a survey of OTA member practice patterns and OTA expert panel recommendations. J Orthop Trauma 29(10):e355–e362
Rasmussen MS, Jørgensen LN, Wille-Jørgensen P (2009) Prolonged thromboprophylaxis with low molecular weight heparin for abdominal or pelvic surgery. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD004318.pub2
Falck-Ytter Y, Francis CW, Johanson NA et al (2012) Prevention of VTE in orthopedic surgery patients: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 141(2):e278S-e325S
Geerts WH, Bergqvist D, Pineo GF et al (2008) Prevention of venous thromboembolism: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 133(6):381S-453S
Bajaj NS, Vaduganathan M, Qamar A et al (2019) Extended prophylaxis for venous thromboembolism after hospitalization for medical illness: a trial sequential and cumulative meta-analysis. PLoS Med 16(4):e1002797
Bohl DD, Webb ML, Lukasiewicz AM et al (2015) Timing of complications after spinal fusion surgery. Spine 40(19):1527–1535
De la Garza RR, Goodwin CR, Passias PG et al (2017) Timing of complications occurring within 30 days after adult spinal deformity surgery. Spine Deformity 5(2):145–150
Bohl D, Samuel A, Webb M et al (2018) Timing of adverse events following geriatric hip fracture surgery: a study of 19,873 patients in the American College of Surgeons National Surgical Quality Improvement Program. Am J Orthop 47(9):10. https://doi.org/10.12788/ajo.2018.0080
DePasse JM, Durand W, Eltorai AE, Palumbo MA, Daniels AH (2018) Timing of complications following posterior cervical fusion. J Orthop 15(2):522–526
Malik AT, Quatman CE, Phieffer LS, Ly TV, Khan SN (2019) Timing of complications following surgery for geriatric hip fractures. J Clin Orthop Trauma 10(5):904–911
Sager B, Ahn J, Tran J, Khazzam M (2019) Timing and risk factors for venous thromboembolism after rotator cuff repair in the 30-day perioperative period. Arthroscopy 35(11):3011–3018
Funding
No funding was provided for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Statement
This submitted manuscript and associated research was performed in compliance with ethical standards of medical research in the United States of America Medical. This research was conducted with ethical approval from the University of Mississippi Medical center IRB using IRB 20130121.
Informed consent
This research was a retrospective chart review which did not require informed consent. Patient identifiers were removed from the data set..
Conflict of interest
The authors have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dynako, J., McCandless, M., Covington, R. et al. Timing of venous thromboemboli in patients with acetabular and pelvic ring fractures. Eur J Orthop Surg Traumatol (2023). https://doi.org/10.1007/s00590-023-03643-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00590-023-03643-6