Abstract
Purpose
The purpose of this study was to investigate the clinical outcomes of femoral fracture with implants on the proximal and distal sides to verify whether actual fracture morphologies follow the fracture types of Baba classification focusing on implant designs useful for periprosthetic femoral fracture.
Methods
Prosthesis was present in 85 with periprosthetic femoral fractures. Excluding 73 patients with fracture around the femoral stem or fracture of the TKA femoral component alone, 12 patients with 14 legs with both implants were investigated. All patients were radiographically assessed for implant stability according to the Baba classification. For clinical evaluation, intra- and postoperative complications, the operation time, and intra-operative blood loss were investigated.
Results
The Baba classification fracture type showed the implant as unstable and stable types in 3 and 11 legs, respectively. The consistency rate between the Baba classification-based judgment of plain radiograms acquired at the time of injury and actual surgical findings was 100%. As a result of treatment according to the Baba classification, bone union was achieved in all patients. There were no intra- or postoperative complications.
Conclusions
Applying the Baba classification, implant stability could be sufficiently evaluated in not only periprosthetic femoral fractures following hip arthroplasty, but also interprosthetic femoral fractures, thereby verifying its usefulness in setting the treatment strategy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Periprosthetic femoral fractures around the hip or knee are complications predicted to increase in future as patients with an arthroplasty and the number of elderly patients increases [1,2,3]. When the prostheses are inserted on the ipsilateral proximal and distal sides of the femur, a fracture between them is generally termed an interprosthetic femoral fracture. This is positioned as a relatively rare fracture [4], and its definition, classification, and treatment methods are still controversial and a major challenge [4,5,6,7].
For classification of interprosthetic femoral fracture, the proximal implant (hip prosthesis)-based Vancouver classification and the distal implant (knee prosthesis)-based Rorabeck and Su classifications are used alone or in combination [2, 8, 9]. Platzer et al. [10] modified the Vancouver classification with regard to interprosthetic femoral fracture, in which the presence or absence of adjacency of the fracture region to the implant and loosening are mentioned. However, implant stability evaluated in all classifications largely depends on the experience and subjective judgment of operators [11,12,13].
We prepared the Baba classification method to objectively evaluate implant stability for the treatment of periprosthetic femoral fracture in 2015 [12, 13]. We previously reported the high sensitivity and specificity of Baba classification with regard to the actual stem stability in periprosthetic fracture and a higher interobserver agreement rate of judgments made based on plain radiograms acquired at the time of injury than that employing the Vancouver classification. The Baba classification predicts implant stability based on the relationship between the implant design and fracture site employing a completely novel concept, and the conditions are divided into 2 types: with or without the use of cement, and each type is further divided into 2 subgroups (Fig. 1). According to the Baba classification-based treatment algorithm, an intra-operative stem stability test is performed in types 1 and 2A. Revision (with ORIF) is recommended when the implant is really unstable, and ORIF is recommended for others.

(According to [13])
Baba classification focusing on implant designs useful for periprosthetic femoral fractures around total hip arthroplasty
Interprosthetic femoral fractures are generally considered fractures between the proximal and distal implants, but based on the concept of the Baba classification, the main fracture line is present in a region other than the bone-fixed regions, indicating that the implant is stable. In contrast, when the implant is unstable, the main fracture line is present in the region of the implant fixed to the bone, based on which a hypothesis is established that fracture does not exist between the implants.
The objective of this study was to investigate the clinical outcomes of femoral fracture with implants on the proximal and distal sides to verify whether actual fracture morphologies follow the fracture types of Baba classification and the validity of a Baba classification-based treatment strategy.
Subjects and methods
Prosthesis was present in 85 patients with periprosthetic femoral fractures between 2007 and 2013. Excluding 73 patients with fracture around the femoral stem or fracture of the TKA femoral component alone, 12 patients with 14 legs with both implants were investigated (Table 1). The mean age at the time of injury was 76.1 years old (58–84 years old), and there were one male (one leg) and 11 females (13 legs) patients. The primary disease was osteoarthrosis in 7 and rheumatoid arthritis in 5. Previous hip surgery was hemiarthroplasty in 8 and total hip arthroplasty in 4. Hip prosthesis was cementless in all patients, whereas cement was used for the TKA femoral component in all patients. The mean duration of follow-up was 4.8 years (2–8 years). All patients were followed up by clinical and radiographic evaluation on an outpatient basis at intervals of one to 3 months until 1 year after the operation and at intervals of 6 months thereafter.
Baba classification-based evaluation
The fracture type was evaluated following the Baba classification for interprosthetic femoral fracture (Fig. 2). The Baba classification was originally classification of periprosthetic femoral fractures around the hip, but here it was applied for TKA, and implant stability was evaluated with regard to the presence or absence of the use of cement and the location of the fracture. Accordingly, when a fracture line was present in the stem of the TKA femoral component or region fixed to the bone, the implant was classified as unstable, and when fracture occurred in other regions, the implants were regarded as stable.
Illustration of the Baba classification for femoral fracture with implants on the proximal and distal sides. Type 1A-hip, 1A-Knee. Fractures in which the main fractured region involve the porous-coated region of the prosthesis. Since the porous-coated region is the region firmly bonding the stem to bone necessary to stabilize the prosthesis, the prosthesis is likely to be unstable when this region is fractured. Type 2A-hip, 2A-Knee. Cement and prosthesis directly contacting bone are collectively regarded as ‘implant.’ Fractures in which the main fractured region involve the implant. Fixation of cement and bone may be broken, and the implant is likely to be unstable. Type1B-inter., Fractures in which the main fractured region is outside the porous-coated region. Since the prosthesis is firmly bonded to bone in the porous-coated region, the implant is stable when the fracture occurred in other regions. Type 2B-inter., Fractures distal to the implant (including fracture of the tip) of hip prosthesis. The implant is stable because cement and bone are fixed in this type, and the fracture occurs distally. Fractures in which the main fractured region is outside the cemented region. Since the cement and bone are fixed in this type, the implant is stable when the fracture occurred in other regions
Validity of Baba classification based on clinical course
All patients were radiographically assessed for implant stability according to the Baba classification, as follows. When implant stability was assessed directly during surgery, if the following two conditions were met, the implant was considered stable: (1) the implant was difficult to remove during surgery. (2) Postoperatively, the implant showed no evidence of loosening after full weight bearing. When implant stability was not assessed during surgery, the stem was considered stable if postoperatively there was no evidence of loosening after full weight bearing.
Treatment methods were surveyed by the Baba classification. For clinical evaluation, intra- and postoperative complications, the operation time and intra-operative blood loss were investigated. In addition, walking ability was assessed before injury and 1 year after surgery by categorizing into independent walking, walking with a cane, walking with 2 crutches, walking using a walker or while holding on to something in the house, and wheelchair use (unable to walk). Radiographic union was defined by evidence of bridging bone at two or more cortices on standard anterior–posterior and lateral radiographs.
Surgical technique and postoperative care
Since a lateral femoral approach facilitates a favorable visual field for anterior and medial operations of the region and the approach is safe for passing a cable, patients with femoral shaft fractures were positioned laterally on a radiolucent table. When instability of the proximal implant was predicted, the hip joint was reached through the posterior approach, the hip joint was dislocated, and the implant was removed, followed by revision and osteosynthesis. Patients with femoral supracondylar fractures were placed in a supine position for a lateral femoral approach. When applying a locking plate, the fracture region was opened via the lateral side, as necessary, periosteal dissection was minimized and reduced, and the absence of implant loosening was directly confirmed visually. The plate was slid under the femoral lateral vastus muscle layer centering in the fracture region and set to the femur under fluoroscopy.
The postoperative rehabilitation schedule of patients undergoing osteosynthesis included the initiation of partial weight bearing after 6 weeks and full weight bearing after 10 weeks. The postoperative rehabilitation schedule of patients undergoing revision with osteosynthesis included the initiation of partial weight bearing after 2 weeks and full weight bearing after 4 weeks.
Results
Baba classification-based evaluation (Table 2)
The Baba classification fracture type showed the implant as unstable (type 1A or 2A) and stable (type 1B or 2B) types in 3 and 11 legs, respectively. In all 3 legs of the implant unstable type cases, the fracture line was present in the region of the uncemented stem fixed to the bone, and there was no case of fracture in the region of the femoral component fixed to the bone. In all 11 legs of the implant stable type, the main fracture line was noted in the distal bone-fixed region over the tip of the stem in 2, femoral diaphysis in 1, slightly distal to the diaphysis in 5, and supracondylar region in 3.
Instability of the stem was confirmed by the intra-operative stem instability test in all cases of the implant unstable type. It was also confirmed that the implant was stable during surgery and the course after surgery in all implant stable-type legs. The consistency rate between the Baba classification-based judgment of plain radiograms acquired at the time of injury and actual surgical findings was 100%.
Surgical procedure and clinical outcomes
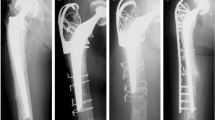
Revision with a cementless long stem was performed in both the implant unstable type cases, and internal fixation with a cable was concomitantly applied to the fracture region. A locking compression plate (LCP) was used in all 11 legs of the implant stable type. In the 2 cases in which the main fracture line was noted in the region distal to the bone-fixed region of a proximal fixation-type uncemented stem over the tip of the stem, internal fixation was applied using an inverted LCP-distal femur (LCP-DF). Broad LCP was used in the case in which the main fracture line was present in the femoral diaphysis, and LCP-DF with 9 or more holes was used in the 5 cases in which the main fracture line was present slightly distal to the diaphysis. In all of these cases, 2 or 3 cables were used, in addition to locking screws, for fixation because the stem was present in the femoral bone marrow cavity proximal to the fracture region. For femoral supracondylar fracture, LCP-DF with 5 holes was used without a cable.
The mean operation time was 113.6 (65–153) min (the ORIF; 106.3 min, the revision; 150.5 min). The mean blood loss was 333.3 (100–600) mL (the ORIF; 333 mL, the revision; 335 mL).
Regarding walking ability before injury and 1 year after surgery (Fig. 3), four patients (28.6%) recovered to the same level, and the level declined by one grade in 8 (57.1%), and 2 grades in 2 (14.3%). On the final follow-up, bone union was achieved in all patients. There were no intra- or postoperative complications.
Discussion
For classification of interprosthetic femoral fracture, the proximal implant (hip prosthesis)-based Vancouver classification and the distal implant (knee prosthesis)-based Rorabeck and Su classifications are used alone or in combination [2, 8, 9]. In addition, a unified classification system [14] applying the Vancouver classification to periprosthetic fractures of the whole body has recently been reported, incorporating interprosthetic femoral fracture as Type D of the Vancouver classification. However, the presence or absence of implant stability in this Type D is not discussed. Furthermore, which of the proximal and distal implants the fracture location is close to and the presence or absence of loosening are described in the classification reported by Pires RE et al. [15]. Loosening of implants is described in all classifications, but we consider that the evaluation of loosening is subjective and depends on the operator’s experience. It has been pointed out in many reports that a misjudgment regarding implant loosening leads to a poor outcome [11, 16, 17].
Thus, considering that evaluation of implant stability is also most important for interprosthetic femoral fracture, we applied the Baba classification as a classification capable of objectively evaluating implant stability. This is a classification method for fractures around the femoral stem based on the new concept of paying attention to the positional relationship between the implant design and fracture location, which has not been available before. When the main fracture is located in the region fixed to the bone, the implant is unstable, whereas the implant is stable when fracture occurs in a region other than the regions fixed to the bone. We think the evaluation of bone stock is subjective and dependent on the surgeon. So we did not take it into account in the classification. Based on this concept of this classification, it makes sense to consider that fractures which occur at a site distal to the region of hip prosthesis fixed to the bone over the proximal region of knee prosthesis fixed to the bone as one type of fracture, and according to the Baba classification, the prosthesis is likely to be stable in fractures within this range. In our subjects actually treated by surgery, implants were stable in 100%. In contrast, in cases in which the main fracture line was present in the bone-fixed region, the implant was unstable.
Regarding treatment methods, taking the presence or absence of implant loosening into consideration, revision (in combination with osteosynthesis) is recommended when only one implant is loosened, and total femur replacement is recommended when both the proximal prosthesis and TKA component are loosened [3, 15, 18]. However, based on the Baba classification proposed by us, fractures located ‘between the distal and proximal implants’ are not involved in the bone-fixed regions, and thus, the fracture does not contribute to loosening or instability of the implants. We consider that when the implant is unstable, the fracture line is not present ‘between the distal and proximal implants’ and that fracture occurred in the bone-fixed region, while fractures with the main fracture lines simultaneously observed in the bone-fixed regions of both implants are very rare. Total femur replacement recommended by various researchers may be one option, but it is not a realistic treatment method for this fracture.
Lehmann et al. showed that the presence of two intramedullary implants in the same femur causes a 30% increase in the risk of fracture [19]. This increase was well-described and documented in the 2003 work of Iesaka et al. [20], carried out on finished models, regarding what effects the size of the interprosthetic gap, stem stability and cortical thickness between two intramedullary and ipsilateral press-fit implants have on ‘stress risers’ (stress concentration). Based on this, for osteosynthesis of interprosthetic femoral fracture, the use of a locking plate long enough to overlap the implant as much as possible is recommended [7, 21, 22]. For screw fixation, fixation with 6–8 cortical screws and wire as necessary is recommended for proximal bone fragment in cases in which hip prosthesis occupies the medullary cavity [6]. We also used a sufficiently long locking plate as a measure against stress concentration, and selected the type of locking plate corresponding to the fracture location. When the fracture line was present immediately distal to the bone-fixed region of the hip prosthesis, a sufficient number of screws could not be inserted into the proximal bone fragment using the normal broad plate. Thus, a condylar locking plate, into which many screws can be inserted, was inverted and applied [23]. Using this method, strong fixation with many screws and wire was possible. On the other hand, we selected a short locking plate for the 3 cases of supracondylar femoral fracture, which is the most distal fracture. Normally, fixation overlapping the proximal implant using a sufficiently long locking plate should be applied, but the size of the existing locking plates did not fit. The causes include the small size of the femoral condyle in elderly Asian females [24], the position for plate setting is limited because of the presence of the TKA implant, and the strong anterior curvature of the femur [25]. Accordingly, a long locking plate does not align with the bone axis, and the forced tightening of wire to the proximal bone fragment was likely to cause an unfavorable reduction of the fracture region (Fig. 4). Although re-fracture due to the concentration of stress on the most proximal region of the plate is of concern, it puts the priority backwards unless treatment for fracture succeeds. Thus, prioritizing bone fusion by anatomical reduction, we used a short locking plate.
The limitation of this study was the small number of cases. However, this fracture is relatively rare and it is difficult to perform a large-scale study, as reported by various researchers. As shown in Table 1, all TKAs are cemented. In this series, we did not include only cemented TKA. However, as a result, no case of uncemented and hinged TKA was enrolled in the present study. We speculate that non-cemented and hinged TKA in Japan has not commonly performed, although the exact number has not been reported.
Moreover, the influence of stress concentration on a short locking plate has not been investigated. However, a sufficiently long plate is not applicable for cases with a strong anterior curvature of the femur and small condyle, raising the possibility of a short locking plate as an option.
Conclusions
Baba classification is a new classification method capable of objectively evaluating implant stability based on the relationship between the implant design and fracture location, and it is possible to prepare a treatment strategy, without the influence of the operator’s experience and subjective judgment, from which stable treatment outcomes can be expected. Applying this classification, implant stability could be sufficiently evaluated in not only periprosthetic femoral fractures following hip arthroplasty, but also interprosthetic femoral fractures, verifying its clear usefulness in setting a treatment strategy.
References
Della Rocca GJ, Leung KS, Pape HC (2011) Periprosthetic fractures: epidemiology and future projections. J Orthop Trauma 25:S66–S70
Rorabeck CH, Taylor JW (1999) Classification of periprosthetic fractures complicating total knee arthroplasty. Orthop Clin North Am 30:209–214
Solarino G, Vicenti G, Moretti L, Abate A, Spinarelli A, Moretti B (2014) Interprosthetic femoral fractures—a challenge of treatment. A systematic review of the literature interprosthetic femoral fractures. Int J Care Inj 45:362–368
Kenny P, Tice J, Quinlan W (1998) Interprosthetic fracture of the femoral shaft. J Arthroplasty 13:361–364
Weiser L, Korecki MA, Sellenschloh K, Fensky F, Püschel K, Morlock MM, Rueger JM, Lehmann W (2015) Interposition sleeve as treatment option for interprosthetic fractures of the femur: a biomechanical in vitro assessment. Int Orthop 39:1743–1747
Sah AP, Marshall A, Virkus WV, Estok DM 2nd, DellaValle CJ (2010) Interprosthetic fractures of the femur: treatment with a single-locked plate. J Arthroplasty 25:280–286
Hou Z, Moore B, Bowen TR, Irgit K, Matzko ME, Strohecker KA, Smith WR (2011) Treatment of interprosthetic fractures of the femur. J Trauma 71:1715–1719
Duncan CP, Masri BA (1995) Fractures of the femur after hip replacement. Instr Course Lect 44:293–304
Su ET, DeWal H, Cesare PE (2004) Periprosthetic femoral fractures above total knee replacement. J Am Acad Orthop Surg 12:12–20
Platzer P, Schuster R, Luxl M, Widhalm HK, Eipeldauer S, Krusch-Mandl I et al (2011) Management and outcome of interprosthetic femoral fractures. Injury 42:1219–1225
Laurer HL, Wutzler S, Possner S, Geiger EV, El Saman A, Marzi I, Frank J (2011) Outcome after operative treatment of Vancouver type B1 and C periprosthetic femoral fractures: open reduction and internal fixation versus revision arthroplasty. Arch Orthop Trauma Surg 131:983–989
Baba T, Homma Y, Momomura R, Kobayashi H, Matsumoto M, Futamura K, Mogami A, Kanda A, Morohashi I, Kaneko K (2015) New classification focusing on implant designs useful for setting therapeutic strategy for periprosthetic femoral fracture. Int Orthop 39:1–5
Baba T, Homma Y, Ochi H, Kobayashi H, Matsumoto M, Sakamoto Y, Kuwahara H, Maeda K, Kaneko K (2015) Higher reliability and validity of Baba classification with CT imaging and implant information for the periprosthetic femoral fractures. Int Orthop 39:1695–1699
Duncan CP, Haddad FS (2014) The unified classification system (UCS): improving ouyr understanding of periprosthetic fractures. Bone Jt J 96B:713–716
Pires RE, de Toledo Lourenço PR, Labronici PJ, da Rocha LR, Balbachevsky D, Cavalcante FR, de Andrade MA (2014) Interprosthetic femoral fractures: proposed new classification system and treatment algorithm. Injury 45:S2–S6
Corten K, Vanrykel F, Bellemans J, Frederix PR, Simon JP, Broos PL (2009) An algorithm for the surgical treatment of periprosthetic fractures of the femur around a well-fixed femoral component. J Bone Jt Surg Br 91:1424–1430
Naqvi GA, Baig SA, Awan N (2012) Interobserver and intraobserver reliability and validity of the Vancouver classification system of periprosthetic femoral fractures after hip arthroplasty. J Arthroplasty 27:1047–1050
Ochs B, Stöckle U, Gebhard F (2012) Interprosthetic fractures—a challenge of treatment. Eur Orthop Traumatol 4:1–7
Lehmann W, Rupprecht M, Hellmers N, Sellenschloh K, Briem D, Puschel K et al (2010) Biomechanical evaluation of peri- and interprosthetic fractures of the femur. J Trauma 68:1459–1463
Iesaka K, Kummer FJ, Di Cesare PE (2005) Stress risers between two ipsilateral intramedullary stems. J Arthroplasty 20:386–391
Soenen M, Migaud H, Bonnomet F, Girard J, Mathevon H, Ehlinger M (2011) Interprosthetic femoral fractures: analysis of 14 cases. Proposal for an additional grade in the Vancouver and SoFCOT classifications. Orthop Traumatol Surg Res 97:693–698
Ebraheim N, Carroll T, Moral MZ, Lea J, Hirschfeld A, Liu J (2014) Interprosthetic femoral fractures treated with locking plate. Int Orthop 38:2183–2189
Baba T, Homma Y, Morohashi I, Maruyama Y, Shitoto K, Kaneko K (2015) Is internal fixation using a reversed condylar locking plate useful for treating Vancouver type B1 periprosthetic femoral fractures? Eur Orthop Traumatol 6:137–143
Urabe K, Mahoney OM, Mabuchi K, Itoman M (2008) Morphologic differences of the distal femur between Caucasian and Japanese women. J Orthop Surg 16:312–315
Maratt J, Schilling PL, Holcombe S, Dougherty R, Murphy R, Wang SC, Goulet JA (2014) Variation in the femoral bow: a novel high-throughput analysis of 3922 femurs on cross-sectional imaging. J Orthop Trauma 28:6–9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Baba, T., Kaneko, K., Homma, Y. et al. The Baba classification focused on implant designs is useful in setting the therapeutic strategy for interprosthetic femoral fracture. Eur J Orthop Surg Traumatol 28, 247–254 (2018). https://doi.org/10.1007/s00590-017-2045-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-017-2045-2