Abstract
Periprosthetic knee fractures following total knee arthroplasty are increasing proportionally to the number of primary procedures done. We performed a retrospective review of Rorabeck type II fractures treated with a retrograde nail, trying to find the relationship between failure and the number of distal locking screws used. Twenty-six patients were included. The number of distal interlocking screws (patients with one or two distal interlocking screws and patients with three screws) correlated with nonunion (p < 0.1), did not correlate with the malunion rate (p > 0.1) and correlated with the reintervention rate (p < 0.1).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Periprosthetic knee fractures following total knee arthroplasty are increasing proportionally to the number of primary procedures done, with an incidence between 1.3 and 5.5 % [1–3]. The most accepted classification for fractures above the knee has been the one proposed by Rorabeck [4]. Different treatments have been used [6], but the “gold standard” for type II fractures has become internal fixation [5].
We have performed a retrospective review of Rorabeck type II periprosthetic fractures treated at our institution with a retrograde nail, trying to find a correlation between the number of distal locking screws and the complication rate.
At the best of our knowledge, we are the first to correlate the number of distal locking screws with the complication rate in the treatment of Rorabeck type II periprosthetic fractures treated with a retrograde nail.
Materials and methods
From our admission records database at the “Hospital 12 de Octubre,” we identified all of the patients who sustained a type II Rorabeck periprosthetic knee fracture treated with a retrograde nail. From all of them, we excluded pathological fractures and patients with lack of data. At the end, twenty-six patients were included between January 1998 and April 2012. All patients had a posterior cruciate retaining TKA, and all were treated with Trigen retrograde nail (Smith and Nephew). We recorded all demographic data, the number of distal locking screws, the distance from the distal tip of the fracture to the prosthesis (to the more distal point of the condylar area), and the number of nonunions, infections and malunions. We also recorded the need for a revision surgery and the progression to an aseptic loosening.
Clinical records were reviewed by the two main authors of the article (A.T.I. and A.A.J.M).
The average age of the patients was 75 years (48–84). There were 4 males and 22 females. All of the fractures were due to low energy trauma. The minimum follow-up was 16 months (the last patient), with an average of 81 months (16–131)
For the implantation of the nail, we use the previous approach used for the primary TKA, changing the polyethylene in all patients. Postoperative status consisted in 8 weeks of partial weigh bearing, with full range of motion allowed. At this point, depending on the fracture status full weigh bearing was permitted.
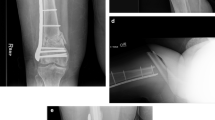
We defined consolidation as a clinical and radiological situation, where there is bone bridging in three of four cortices in two orthogonal X-rays, and there is no pain in the fracture site (Fig. 1).
We defined nonunion as a condition that has to happen after 9 months from the surgery that consists in 3 months of no radiological progression, without signs of union and with pain in the fracture site (Fig. 2). We defined malunion as a valgus angle >10°, a varus angle >0° (for the measurement of valgus and varus we chose this prosthesis malalignment, because it is a more reliable parameter, and we consider as anatomical 6° of valgus) an extension angle >5°, clinical malrotation, or fracture collapse >2 cm compared to contralateral side. We defined a positive case of infection as any infectious process affecting the operated limb treated with antibiotics (superficial and deep infections). We defined component loosening by the surgeon criteria. We defined revision surgery as any posterior surgical procedure in the operated femur.
The main outcome measurements defined as failure were nonunion, malunion and revision surgery. The predictors of failure studied were the number of distal locking screws used (one and two or three).
Statistical analysis: SPSS version 17.0 (SPSS Inc., Chicago, Illinois) was used for the statistical analysis. Due to the small sample size, we decide to accept as statistically significant a p value of 0.05.
Results
The predictor variables and the main outcome (failure due to malunion, nonunion, reintervention or infection) are resumed in Table 1.
After union, the coronal alignment averaged 5° of valgus (17° of varus to 15° of valgus) and the average sagittal alignment average was 5° of extension (0° to −15° of extension). Seven prostheses needed revision surgery during the follow-up, four cases because a periimplant fracture (two secondary to a nonunion and two proximal to the tip of the nail), two due to femoral component loosening and one due to infection.
None of the patients died within 6 months from the operation, but ten deceased during the whole follow-up.
The number of distal interlocking screws (patients with 1 or 2 distal interlocking screws, and patients with 3 screws) correlated with nonunion (p < 0.1), did not correlate with the malunion rate (p > 0.1) and correlated with the reintervention rate (p < 0.1).
The distance from fracture to the first distal locking screw (Table 1) did not correlate with an increase in complication rates (p > 0.1).
Discussion
Bong et al. [6] suggested that the retrograde-inserted nail may provide greater stability for the management of periprosthetic supracondylar femur fractures in patients with a posterior cruciate ligament-retaining femoral total knee arthroplasty component, in their study in cadaver compared to the Less Invasive Stabilization System (LISS; Synthes USA, Paoli, PA), specially in fractures with medial gap.
Han et al. [7] supported the use of retrograde intramedular nailing for periprosthetic supracondylar fractures of the femur without nonunions, malunions, infections and component loosening.
Pelfort et al. [8] demonstrate that patients treated with a retrograde nail, who united in extension, had a good clinical outcome, and none of the patients had signs of nonunion of implant loosening.
Betzwada et al. [9] compared the use of plating and retrograde nailing finding no differences in terms of complications. In their series of patients, only one patient complicated with nonunion, and no severe malunions were observed.
Horneff et al. [10] recommend the use of locking plated instead of intramedullary nails for the treatment of Rorabeck type II fractures because of the complications rate.
A systematic review from Herrera et al. [5] review the treatment of periprosthetic fractures above the knee, and they find out a nonunion rate of 9 %, a fixation failure rate of 4 %, an infection rate of 3 %, a revision surgery rate of 13 %. It is interesting that the use of retrograde nail was associated with a reduction of relative risk of 70 % for revision surgery and a 87 % for nonunion. This study included conventional plates and nonoperative treatment. Fir retrograde intramedular nailing, they found a nonunion rate of 1.5 % and a reintervention rate of 4.6 %.
At the best of our knowledge, we are the first to correlate the number of distal locking screws with the complication rate in the treatment of Rorabeck type II periprosthetic fractures treated with a retrograde nail. Our series has a high complication rate compared to other series published, but when we exclude patients with <3 distal locking screws, complication rates became really low (no nonunions, three malunions and no reinterventions).
We also have learned that it is expected some degree of hyperextension when treating theses fractures with a retrograde nail, but as we have learned from Pelfort et al. [8] this issue don´t have a clinical repercussion.
Because of these, we cannot recommend the use of retrograde nails in fractures which cannot be fixed with a minimum of three distal locking screws due to the high complication rate.
More prospective studies must be done to confirm our data.
References
Berry DJ (1999) Epidemiology: hip and knee. Orthop Clin North Am 30(2):183–190
Healy WL, Siliski JM, Incavo SJ (1993) Operative treatment of distal femoral fractures proximal to total knee replacements. J Bone Joint Surg Am 75(1):27–34
Schroder HM, Berthelsen A, Hassani G, Hansen EB, Solgaard S (2001) Cementless porous-coated total knee arthroplasty: 10-year results in a consecutive series. J Arthroplasty 16(5):559–567. doi:10.1054/arth.2001.23565
Rorabeck CH, Taylor JW (1999) Periprosthetic fractures of the femur complicating total knee arthroplasty. Orthop Clin North Am 30(2):265–277
Herrera DA, Kregor PJ, Cole PA, Levy BA, Jonsson A, Zlowodzki M (2008) Treatment of acute distal femur fractures above a total knee arthroplasty: systematic review of 415 cases (1981–2006). Acta Orthop 79(1):22–27. doi:10.1080/17453670710014716
Bong MR, Egol KA, Koval KJ, Kummer FJ, Su ET, Iesaka K, Bayer J, Di Cesare PE (2002) Comparison of the LISS and a retrograde-inserted supracondylar intramedullary nail for fixation of a periprosthetic distal femur fracture proximal to a total knee arthroplasty. J Arthroplasty 17(7):876–881
Han HS, Oh KW, Kang SB (2009) Retrograde intramedullary nailing for periprosthetic supracondylar fractures of the femur after total knee arthroplasty. Clin Orthop Surg 1(4):201–206. doi:10.4055/cios.2009.1.4.201
Pelfort X, Torres-Claramunt R, Hinarejos P, Leal J, Gil-Gonzalez S, Puig L (2013) Extension malunion of the femoral component after retrograde nailing: no sequelae at 6 years. J Orthop Trauma 27(3):158–161. doi:10.1097/BOT.0b013e3182629641
Bezwada HP, Neubauer P, Baker J, Israelite CL, Johanson NA (2004) Periprosthetic supracondylar femur fractures following total knee arthroplasty. J Arthroplasty 19(4):453–458
Horneff JG 3rd, Scolaro JA, Jafari SM, Mirza A, Parvizi J, Mehta S (2013) Intramedullary nailing versus locked plate for treating supracondylar periprosthetic femur fractures. Orthopedics 36(5):e561–e566. doi:10.3928/01477447-20130426-16
Conflict of interest
All authors do not have conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Toro-Ibarguen, A., Moreno-Beamud, JA., Porras-Moreno, MÁ. et al. The number of locking screws predicts the risk of nonunion and reintervention in periprosthetic total knee arthroplasty fractures treated with a nail. Eur J Orthop Surg Traumatol 25, 661–664 (2015). https://doi.org/10.1007/s00590-014-1541-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-014-1541-x