Abstract
Purpose
Unilateral sacroiliitis (US) is an uncommon disease with varied etiology. The differentiation between infective and inflammatory causes for US based on MRI alone is often difficult. We studied the efficacy of MRI findings in comparison with tissue studies in the diagnosis of US.
Methods
A retrospective analysis of patients who presented with US and evaluated with MRI, biopsy for histopathology and tissue cultures was performed. Patients with bilateral sacroiliitis, traumatic and postpartum sacroiliitis were excluded. Based on defined MRI criteria, the patients were divided into two groups—infective (group A) and inflammation (group B).
Results
In total, 33 patients (mean age—33.4 ± 17.2 years) with MRI features of US had presented with unilateral gluteal pain (100%) and positive Patrick’s test (91.9%). Based on the MRI features of severe subchondral marrow edema, widening of joint space, intra-articular abscess and periarticular muscle abscess, infective sacroiliitis (A) was diagnosed in 20/33 (60.6% cases). A total of 13/33 (39.3%) patients had features of inflammation (B), based on the following MRI criteria—subchondral sclerosis with minimal edema, erosions, maintained joint space without abscess/destruction. Tissue evidence of infection was positive in 13/20 (65%) patients in group A while it was negative in all group B patients.
Conclusion
MRI had high sensitivity (71%) and 100% specificity in diagnosing inflammatory sacroiliitis while it had low specificity, but 100% sensitivity for diagnosing infective sacroiliitis. Hence, patients diagnosed as inflammatory sacroiliitis in MRI are unlikely to benefit from further tissue studies while percutaneous biopsy is recommended in patients diagnosed in MRI as infective sacroiliitis.
Graphical abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Unilateral sacroiliitis is an uncommon, but highly painful condition and can be caused by multiple aetiologies ranging from degenerative disorders, trauma, infection and inflammatory diseases. Infection due to pyogenic organisms and tuberculosis, and inflammatory diseases like seronegative arthropathies account for most cases of unilateral sacroiliitis [1,2,3,4,5,6,7,8]. While the clinical presentation of unilateral sacroiliitis is typical, the diagnosis of the causative factor is often difficult. Identifying the causative factor is highly essential considering the variable treatment regimens for these conditions. Blood markers including white cell count, erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are elevated, but are non-specific for both infective and inflammatory causes. While radiographs are hardly diagnostic, magnetic resonance imaging (MRI) is considered as the gold standard imaging test to confirm the diagnosis of unilateral sacroiliitis. Several studies have shown independently about the diagnostic MRI features of inflammatory arthropathy and infective sacroiliitis, which include the presence of marrow edema, periarticular collection, muscle edema, sub-articular erosions and thick capsulitis [3, 6,7,8,9,10,11,12]. But, these findings are not specific, and importantly none of the studies have correlated these MRI findings with diagnostic tissue tests such as tissue culture, histopathological examination and GeneXpert PCR studies. Further, MRI diagnosis of infective sacroiliitis is also unreliable in the delineation between pyogenic and tubercular etiologies, which is essential considering the widely varied treatment regimens [3, 7,8,9]. Thus, it is paramount to assess the diagnostic value of MRI features of unilateral sacroiliitis in accordance with tissue studies. Hence, we studied the efficacy of MRI findings in comparison with tissue culture studies and histopathology as the gold standard tests, in the diagnosis of unilateral sacroiliitis.
Materials and methods
The study was approved by the institutional review board of the institute. We performed a retrospective analysis of case records of patients who presented with unilateral sacroiliitis between 2008 and 2016 and were evaluated with 1.5-T MRI. All patients had underwent clinical examination to confirm unilateral sacroiliitis, and the MRI evaluation included sagittal, coronal and axial T1, T2, STIR and contrast-enhanced fat-suppressed T1W images of both the sacroiliac joints. All patients had undergone blood investigations including erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), white cell counts and HLA B-27. Patients presenting with MRI evidence of bilateral sacroiliitis, degenerative sacroiliitis, traumatic sacroiliac dysfunction and those with positive HLA B27 were excluded from the study. The remaining patients whose MRI diagnosis was either infection or inflammation were planned for a biopsy.
Biopsy technique
Under general anesthesia, the patient was positioned prone on a radiolucent table over two horizontal bolsters, one placed under the chest and another beneath the anterior superior iliac spine. A small padded cushion of about 4 cm height was placed underneath the contralateral anterior iliac spine. This lifts the contralateral pelvis and brings the affected ipsilateral sacroiliac joint in line with the image intensifier, positioned at zero degrees of medio-lateral inclination. Under image guidance, the Jamshedi needle was used to acquire tissue from the sacroiliac joint. Multiple passes are usually made to acquire tissue from the joint cartilage and bone, from both iliac and sacral sides. The tissue acquired was sent for histopathological examination, culture for pyogenic organism, BACTEC culture for tubercular bacilli and GeneXpert test for detecting tubercular DNA.
The MRI images were reported by two musculoskeletal radiologists in consensus. Based on the MRI findings, the patients were divided into two groups—infective (group A) and inflammation (group B). In group A, MRI findings which were considered specific for infection included severe subchondral marrow edema, bone erosions (mild to moderate), widening of joint space, periarticular/intra-articular abscess (hyperintense on T2W images with rim enhancement on fat-suppressed contrast-enhanced T1W images) and periarticular muscle edema/abscess (hyperintensity on T2W images or fat-suppressed contrast-enhanced T1W images) (Fig. 1). Additionally, the presence of extensive edema in the periarticular zone and surrounding muscles, severe bone erosions (permeative bony destruction), cavitation and sequestrum formation was considered diagnostic of tubercular infection (Fig. 2). In group B, the presence of minimal to moderate subchondral edema and mild to severe subchondral sclerosis with tiny erosions, maintained joint space, without abscess or permeative/lytic bone destruction, were considered diagnostic of inflammation (Fig. 3). The predictive value of these MRI findings in diagnosing the appropriate cause for sacroiliitis was evaluated based on the tissue studies.
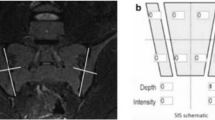
MRI images of a 33-year-old female patient diagnosed as left pyogenic sacroiliitis (Escherichia coli). Coronal T2W image (a) and coronal STIR image (b), showing the presence of joint space widening with intra-articular abscess (arrow head) and periarticular abscess (bold arrow) in the left sacroiliac joint. Coronal STIR image (b) shows the presence of marrow edema in the left ilium and sacral bone and abscess in the left psoas muscle (thin arrow)
MRI images of a 35-year-old female patient diagnosed as left tuberculous sacroiliitis. Axial T2W image (a), showing bone marrow edema (white arrow heads) and periarticular abscess (white bold arrow) involving the left sacroiliac joint; (b) axial T1W fat-suppressed contrast-enhanced images showing extensive bone marrow edema, abscess in iliacus (black arrow), rim enhancing periarticular and intra-articular abscess (white bold arrows) with joint space widening; (c) axial CT scan showing sequestrum within the left sacroiliac joint (thin arrow), erosions and cavitation
Results
During the study period, 51 patients have been evaluated for unilateral sacroiliitis, out of which 18 were excluded (bilateral sacroiliitis in seven, degenerative sacroiliitis in four, HLA B27 positivity in six and one patient was not willing for biopsy). The remaining 33 patients (M:F–12:21, mean age—33.4 ± 17.2 years) with unilateral sacroiliitis formed the study group. All patients had unilateral gluteal pain (100%) with positive Patrick’s test in 91.9% (n = 30), fever in 43.2% (n = 14) and constitutional symptoms in 10.8% (n = 4). MRI showed features of infective sacroiliitis (group A) in 20/33 (60.6%). Among these 20 patients, four had additional features of tuberculosis in MRI (based on extensive edema, permeative bony destruction, cavitation, sequestrum formation). Group B included 13/33 (39.3%) patients with MRI features of inflammation (group B).
Tissue culture and/or histopathological evidence of infection was positive in 13/33 (39%) patients, and all of them were in group A, while it was negative in all group B patients. Among the 13 patients in group A, the causative organism was isolated in 11 cases which included Staphylococcus aureus (n = 4), coagulase negative Staphylococcus (n = 1), Escherichia coli (n = 2) and Mycobacterium tuberculosis (n = 4). Thus, MRI had 100% sensitivity and 59% specificity in diagnosing infective sacroiliitis while it was 100% specific for diagnosing inflammatory sacroiliitis. In 16 patients diagnosed as pyogenic in MRI, four patients (25%) had tissue culture or histopathological evidence of tuberculosis. GeneXpert test was positive in 7/20 (35%) patients in Group A.
Discussion
Our study showed that in patients with unilateral sacroiliitis, MRI can be highly specific in confirming an inflammatory etiology while it was highly sensitive for diagnosing an infectious cause (Table 1). Gold standard tests including tissue culture and histopathology remained negative in patients diagnosed as inflammatory sacroiliitis in MRI, thus indicating the high specificity of MRI. However, in patients diagnosed to have infective etiology in MRI, the findings were indistinctive in differentiating tubercular and pyogenic infections, where further tissue tests would be helpful.
Unilateral sacroiliitis is a relatively uncommon problem with diverse etiologies like infection, inflammatory diseases, neoplastic infiltration, trauma and degenerative disorders [1,2,3,4,5,6,7,8]. Among these, infection and inflammatory diseases account for most cases. The common association of unilateral sacroiliitis with spondyloarthropathies (psoriatic arthritis, reactive arthritis, early stage of ankylosing spondylitis) poses a challenge in the differential diagnosis with other causes of unilateral sacroiliitis [1, 6].
Infectious sacroiliitis, of pyogenic or tubercular etiology, is a common cause of unilateral low back pain in developing countries [3, 7, 8]. Tuberculous sacroiliitis accounts for 10% of cases of skeletal tuberculosis [7]. While the clinical presentation of unilateral sacroiliitis is typical, the diagnosis of the causative factor is often difficult, especially in the early stages of disease when laboratory tests are variable and inconsistent for both infective and inflammatory pathologies. The need for sensitive and specific imaging tools in diagnosing the specific etiology of sacroiliitis (especially in the early stage) is highly critical, considering the widely varied treatment regimens.
MRI is considered the gold standard in diagnosing unilateral sacroiliitis as it has a high sensitivity to identify lesions in the early stage, has good interobserver reliability, ensures early and appropriate therapeutic management, aids in assessment of therapeutic efficacy and avoids risk of radiation exposure [13,14,15]. Several studies have shown independently about the diagnostic MRI features of inflammatory arthropathy and infective sacroiliitis. These include the presence of bone marrow edema, synovitis/capsulitis, periarticular collection, joint space enhancement, muscle edema, sub-articular erosions, but often these findings are not specific to reliably distinguish between infective and inflammatory etiologies [6, 11, 12, 14].
Unlike MRI features of tuberculous spondylitis, which have been well established, the MRI features of tuberculous sacroiliitis have not been clearly defined [3, 16]. Hence, MRI diagnosis of infective sacroiliitis can be unreliable in the delineation between infectious and inflammatory etiologies and further differentiation between pyogenic and tubercular causes and this was observed to be true in our study. This is highly essential considering the contrasting treatment regimens and the considerable morbidity consequent to a delay in diagnosis/misdiagnosis.
Since patients with infective sacroiliitis present without any striking symptoms of infection such as fever and sepsis, the need for tissue analysis becomes mandatory. Percutaneous biopsy is safe, is simple, helps in confirming the exact etiology of sacroiliitis and facilitates early accurate diagnosis and institution of appropriate treatment [17,18,19,20]. Now that MRI is assuming an increasingly important role in the early diagnosis of unilateral sacroiliitis, it would be useful to examine the accuracy of MRI findings in comparison with tissue culture studies and histopathology as the gold standard tests, in the diagnosis of unilateral sacroiliitis. To our knowledge, no study has examined the efficacy of MRI findings in the differential diagnosis of infectious and inflammatory sacroiliitis in comparison with tissue studies. The results of the study would suggest the treating surgeon as to when to rely on MRI findings and when to proceed with further tissue studies.
Kang et al. [21] have shown that the presence of large bone erosion, thick capsulitis, extracapsular fluid collection and periarticular muscle edema on MRI suggest infectious sacroiliitis, whereas iliac-dominant bone marrow edema and joint space enhancement favor the diagnosis of unilateral sacroiliitis in spondyloarthritis. Sacroiliitis in spondyloarthritis showed iliac dominance in the distribution of bone marrow edema, whereas infectious sacroiliitis more commonly showed either sacral dominance or an even distribution [21]. On the contrary, our results showed that bone marrow edema did not show a characteristic pattern of distribution attributable to infectious or inflammatory etiology.
The MRI findings of infective (group A) and inflammatory (group B) sacroiliitis presented in our study are comparable with those described in the previous studies [3, 6, 11, 12, 21]. A finding that was exclusively seen in patients of group A was the presence of intra-articular and/or periarticular abscess (hyperintense on T2W images with rim enhancement on fat-suppressed contrast-enhanced T1W images) in 15/20 patients (75%) and periarticular muscle edema/intramuscular abscess (hyperintensity on T2W images or fat-suppressed contrast-enhanced T1W images) in 18/20 (90%). These findings were absent in all cases of group B. Similar findings were reported by Sturzenbecher et al. [11]. Inflammation of the sacroiliac joints due to infection crosses anatomic borders, whereas in spondyloarthritis, the inflammation is limited to the bone and sacroiliac joint space [22]. This is reflected by the presence of periarticular muscle edema and extracapsular fluid collections in infective pathologies of sacroiliac joint. Periarticular muscle edema/intramuscular abscess and peri-/intra-articular abscess are two MRI findings that are specific for infective sacroiliitis. Among the 15 patients with intra-articular/periarticular abscess on MRI, tissue culture and/or histopathological evidence of infection was positive in 11 (73%) patients. In total, 13 (72%) out of the 18 patients with periarticular muscle edema/intramuscular abscess had positive tissue culture and/or histopathological evidence of infection.
There are a few limitations in the study. Unilateral sacroiliitis being a rare clinical disorder, the number of patients is small, but it is one of the largest data yet published. Secondly, we have considered tissue studies as gold standard investigations to assess the utility of MRI, but there could be false negative results in a few patients since vertebral infections are paucibacillary. Hence, such patients marked as inflammatory in MRI and without positive tissue tests may in fact be of infective origin. However, this is a potential lacuna of all studies that employ tissue tests for infection as gold standard investigations.
Conclusion
Thus, MRI has high sensitivity (71%) and 100% specificity in diagnosing inflammatory sacroiliitis while it has low specificity, but 100% sensitivity for diagnosing infective sacroiliitis. Hence, patients diagnosed as inflammatory sacroiliitis in MRI are unlikely to benefit from further tissue studies and appropriate rheumatological treatment can be initiated. MRI had less specificity to differentiate pyogenic from tubercular infections. Hence, percutaneous biopsy and tissue analysis are recommended in patients diagnosed in MRI as infective sacroiliitis for confirmation and further accurate categorization.
References
Muche B, Bollow M, Francois RJ, Sieper J, Hamm B, Braun J (2003) Anatomic structures involved in early and late-stage sacroiliitis in spondylarthritis: a detailed analysis by contrast-enhanced magnetic resonance imaging. Arthritis Rheum 48:1374–1384
Hermet M, Minichiello E, Flipo RM et al (2012) Infectious sacroiliitis: a retrospective, multicenter study of 39 adults. BMC Infect Dis 12:305
Ramlakan RJ, Govender S (2007) Sacroiliac joint tuberculosis. Int Orthop 31:121–124
Floman Y, Milgrom C, Gomori JM, Kenan S, Ezra Y, Liebergall M (1994) Acute postpartum inflammatory sacroiliitis. A report of four cases. J Bone Joint Surg Br 76(6):887–890
Jacobson JA, Girish G, Jiang Y, Sabb B (2008) Radiographic evaluation of arthritis: degenerative joint diseases. Radiology 248:737–747
Canella C, Schau B, Ribeiro E, Sbaffi B, Marchiori E (2013) MRI in seronegative spondyloarthritis: imaging features and differential diagnosis in the spine and sacroiliac joints. AJR 200:149–157
Tuli SM, Jaypee Brothers Publication; New Delhi (2010) Tuberculosis of the skeletal system (bones, joints, spine and bursal sheaths), pp 3–15
Osman AA, Govender S (1995) Septic sacroiliitis. Clin Orthop 313:214–219
Attarian DE (2001) Septic sacroiliitis: the overlooked diagnosis. J South Orthop Assoc 10(1):57–60
Goldberg J, Kovarsky J (1983) Tuberculous sacroiliitis. South Med J 76(9):1175–1176
Stürzenbecher A, Braun J, Paris S, Biedermann T, Hamm B, Bollow M (2000) MR imaging of septic sacroiliitis. Skelet Radiol 29:439–446
Klein MA, Winalski CS, Wax MR et al (1991) MR imaging of septic sacroiliitis. J Comput Assist Tomogr 15:126–132
Bakker PA, van den Berg R, Lenczner G (2017) Can we use structural lesions seen on MRI of the sacroiliac joints reliably for the classification of patients according to the ASAS axial spondyloarthritis criteria? Data from the DESIR cohort. Ann Rheum Dis 76(2):392–398
Rudwaleit M, van der Heijde D, Khan MA et al (2004) How to diagnose axial spondyloarthritis early. Ann Rheum Dis 63:535–543
Bakker PA, van den Berg R, Hooge M (2018) Impact of replacing radiographic sacroiliitis by magnetic resonance imaging structural lesions on the classification of patients with axial spondyloarthritis. Rheumatology (Oxf). https://doi.org/10.1093/rheumatology/kex532
Kim NH, Lee HM, Suh JS (1994) Magnetic resonance imaging for the diagnosis of tuberculous spondylitis. Spine 19(21):2451–2455
Gong Y, Zheng N, Chen SB et al (2012) Ten years’ experience with needle biopsy in the early diagnosis of sacroiliitis. Arthritis Rheum 64(5):1399–1406
Marzo-Ortega H, O’Connor P, Emery P et al (2007) Sacroiliac joint biopsies in early scaroiliitis. Rheumatology (Oxf) 46(7):1210–1211
Knipp D, Simeone FJ, Nelson SB et al (2018) Percutaneous CT-guided sacroiliac joint sampling for infection: aspiration, biopsy, and technique. Skelet Radiol 47(4):473–482
Pouchot J, Vinceneux P, Barge J et al (1988) Tuberculosis of the sacroiliac joint: clinical features, outcome and evaluation of closed needle biopsy in 11 consecutive cases. Am J Med 84:622–628
Kang Y, Hong SH, Kim JY et al (2015) Unilateral sacroiliitis: Differential diagnosis between infectious sacroiliitis and spondyloarthritis based on MRI findings. AJR Am J Roentgenol 205(5):1048–1055
Aydingoz U, Yildiz AE, Ozdemir ZM et al (2012) A critical overview of the imaging arm of the ASAS criteria for diagnosing axial spondyloarthritis: what the radiologist should know. Diagn Interv Radiol (Ank) 18:555–565
Funding
The study was funded by the Ganga Orthopaedic Research and Education Foundation (GOREF).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kanna, R.M., Bosco, A., Shetty, A.P. et al. Unilateral sacroiliitis: differentiating infective and inflammatory etiology by magnetic resonance imaging and tissue studies. Eur Spine J 28, 762–767 (2019). https://doi.org/10.1007/s00586-018-5800-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-018-5800-0