Abstract
Accurate identification of the cricothyroid membrane (CTM) has paramount importance in the event of a ‘cannot intubate, cannot oxygenate’ scenario. We sought to determine the ability of anesthesiologists to correctly identify the CTM in obese and non-obese children. Anesthesiologists were asked to mark the entry point of the cricothyroidotomy device with an ultraviolet invisible pen on obese and non-obese (BMI < 95th percentile for age and sex) children aged 7–12 years. A correct estimation was defined as a mark made between the upper and lower borders of the CTM and within the 3-mm midline. Twenty anesthesiologists palpated 30 obese and 50 non-obese children. The CTM was accurately identified with digital palpation in a total 55% of children, and there were no differences inaccurate identification rates of the CTM between obese and non-obese children [57 vs. 54%, respectively; median difference 3%; 95% confidence interval (− 20 to 25%); p = 0.82]. Accuracy was not correlated with any demographic or morphometric features of the children. Percutaneous identification of the CTM in children aged 7–12 years was poor and not significantly different for obese and non-obese children. Pre-procedural ultrasonography may help to identify the landmarks for cricothyroidotomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Emergency cricothyroidotomy is a life-saving rescue maneuver in the ‘cannot intubate, cannot oxygenate’ (CICO) scenario recommended by the Difficult Airway Society guidelines for both adults and children [1, 2]. Thus, it is important that all anesthesiologists should be able to identify the cricothyroid membrane (CTM) accurately in emergency situations. Unfortunately, the success rates of identifying the (CTM) by palpation in adults do not seem to be satisfactory in previous studies [3]. The smaller and less prominent anatomy and soft cartilage tissue may make the condition even more difficult in children.
The objective of the present study was to determine the accuracy of CTM identification in children aged 7–12 years using palpation as compared with ultrasonography. We also hypothesized that obesity would decrease identification success.
Methods
The study was conducted after approval was granted from the ethics committee of Necmettin Erbakan University, Konya, Turkey (protocol no: 2017/937). After obtaining informed consent from the parents and participants and patient assent, we enrolled a total of 83 children aged between 7 and 12 years with ASA I or II who were undergoing day-case surgery. Those with a history of global developmental delay, known neck deformities, previous neck surgery, and children who refused to participate in this study were excluded. The patients’ demographic characteristics such as age, weight, height, body mass index (BMI), and neck circumference were recorded. A child was defined as ‘obese’ if their BMI-for-age percentile was greater than or equal to the 95th percentile [4].
Each anesthesiologist as a participant was asked to identify the CTM of four patients using traditional digital palpation. The data collected via the measurements of the participants included: years of experience since residency, history of performing surgical airways, and participation in training sessions related to front-of-neck access (FONA) within 12 months of the study.
Each patient lay in the supine position on an operating table with the neck maximally extended. The participants were asked to identify the CTM using digital palpation, and to mark the entry point of the cricothyroidotomy airway device with an ultraviolet invisible pen. Then, a single operator (BB) trained in neck ultrasonography, scanned the landmarks using ultrasound (Mindray M5®, China) with a linear high-frequency transducer (8–12 MHz) as described by Kristensen et al. [5], while the patient’s neck was kept in the same position (Fig. 1). Superior and inferior borders, and the mid-central point of the CTM was marked using an ethanol-erasable pen. Correct estimation was defined as a mark between the estimated borders of the CTM, and within 3 mm of the midline.
The longitudinal technique described for the identification of the cricothyroid membrane (CTM). Left column: the ultrasound transducer placed transversely over the neck cephalad to the suprasternal notch; a tracheal ring is seen as a horseshoe-shaped dark structure (light blue) with a posterior white line that represents the tissue–air boundary. Middle column: the transducer is slid laterally towards the patient’s right side until a half image of the trachea is left on the screen (light blue). Right column: the left edge of the transducer is rotated into the sagittal plane to obtain black hypoechoic round structures (string of pearls); then, the transducer is moved cephalad, and the anterior part of the cricoid cartilage is seen as a slightly larger and elongated structure. The light blue and red markings represent the anterior part of the tracheal rings and cricoid cartilage, respectively. The CTM (yellow) is located immediately cephalad to the cricoid cartilage, caudal to the thyroid cartilage (blue); the acoustic shadow (green), which was created by sliding a needle underneath the transducer, indicates its midlevel
The primary outcome was the accuracy of digital palpation to identify the entry point of the cricothyroidotomy device compared with ultrasonographic control. Secondary outcomes were: (1) the absolute distance of digital palpation from the target ultrasound point; (2) palpation time measured from the first palpation of the skin overlying the neck to marking the entry point of an airway device used for cricothyroidotomy; (3) demographic characteristics of patients leading to misidentification of CTM, as well as the years of experience of the anesthesiologists; (4) ease of palpation as described previously by Nicholls et al. [6].
Statistical analysis
Obesity was controlled during the study with an enrolment ratio of 1/3. The total sample size of 73 was projected on the basis of correct identification of the CTM in 39% of obese and 71% of non-obese children (α = 0.05, β = 0.8) [7]. Eighty-three patients were enrolled in the study to allow for drop-out.
Categorical data were analyzed using the Chi-square test and are presented as frequencies and percentages. Continuous data were analyzed using the t or Mann–Whitney U tests and are presented as mean (standard deviation) and median (interquartile range) where appropriate. Univariate associations were explored using logistic regression analyses. A p value < 0.05 was defined as statistically significant.
Results
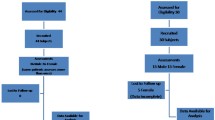
A total of 83 subjects were recruited for the study. Three patients were excluded from the study due to difficulty in capturing proper images. The data of 80 patients were analyzed. Thirty of the 80 patients were obese and 50 were non-obese.
The demographic data of the patients are presented in Table 1. Overall, the CTM was identified correctly in 44 of 80 (55%; 95% CI 44–66%) patients. From these 44 patients, 17 were obese (57%; 95% CI 39–74%); 27 were non-obese (54%; 95% CI 40–68%) (Table 2). The anesthesiologists subjectively found CTM palpation more difficult in obese patients than in non-obese children. Overall, the neck landmarks of 47% (95% CI 30–64%) obese children were graded as difficult–impossible compared with 12% (95% CI 2–14%) in non-obese children (p < 0.0001) (Table 3).
Logistic regression analysis revealed no correlation for the accuracy of CTM assessment with the following parameters: BMI, neck circumference, CTM length, time to palpate the landmarks, and anesthesiologists’ years of experience (Table 4).
Polar plots in Fig. 2 show the overall markings of the CTM in obese and non-obese children.
None of the participants had performed a cricothyroidotomy on a patient or participated in any previous academic training sessions related to FONA techniques within the previous 12 months.
Discussion
Our results suggest that the accuracy rate of palpation to estimate the location of the CTM was 55% when compared with ultrasound findings in children aged 7–12 years. The results also show that the inaccuracy of palpation was related to neither demographic reasons nor the participants’ years of experience.
The localization of the CTM by physicians in adults has been the subject of various studies, but little attention has been paid to its localization in children. This may be attributed to the fact that the majority of difficult airways can be predicted in children, and the need for a FONA rescue technique is rare [8, 9]. Nevertheless, in the event of CICO, anesthesiologists should attempt emergency cricothyroidotomy in order to establish rapid oxygenation. Accurate identification of the CTM is a key to success with fewer complications; however, the accuracy of digital palpation in the assessment of the CTM has been reported to vary between 0 and 71% with a highest rate in non-obese man [7, 10,11,12]. The overall success rate in our study (55%) was higher than the overall success rates of previous studies performed in adult populations. Despite such a high success rate, this rate can still be considered suboptimal when considering that the consequences of misidentification could be fatal.
Previous studies have shown that misidentification of the CTM is more common in female populations than in male populations [10, 12, 13]. Possible reasons for this include the acute external angulation of laryngeal cartilages in males and the similarity of palpation of the thyrohyoid space in females [14, 15]. On the other hand, this inter-sex difference in laryngeal cartilages becomes apparent after the post-puberty period. Our findings are consistent with this anatomic difference between the adult and pediatric larynx, being female was not associated with inaccuracy of digital palpation.
Obese patients may present difficulties in mask ventilation and tracheal intubation due to such patients’ having short and thick necks, and the same group of patients also pose technical threats to percutaneous transtracheal ventilation because increased pretracheal soft tissue depth may hinder identification of anatomic landmarks of the CTM in adults [11, 12, 16]. The data obtained from children also suggest that difficult mask airway and/or difficult intubation are more common in obese pediatric patients than the non-obese [17], whereas in the current study, the accuracy of landmark identification was found not to be different between obese and non-obese children. The lack of difference might be related to the hyperextended position or relatively thin pretracheal tissue of obese children, compared with obese adults.
Our study has a number of limitations. The ultrasound assessment of the CTM was performed by a single physician who is experienced in the field. This could lead to bias against digital palpation performed by participants with no prior experience. Our study was not designed to compare the times of digital palpation and ultrasonographic visualization of the CTM. The comparison of time for ultrasonography vs. conventional digital palpation merits further research. We used the definition of correct identification as a marking within 3 mm of the midline. This definition was arbitrary and was based on well-established dimensions of the CTM in 8-year-old children [18]. Another limitation is that our results cannot be applicable to infants, toddlers, and other segments of the pediatric population because the children in our study were aged 7–12 years.
In conclusion, our findings suggest that ultrasound can be used for accurate identification of the CTM in children. The accuracy of the traditional palpation method in the identification of the CTM was 55%, which would clearly be considered as unsatisfactory in a real emergency situation. Marking of the CTM before induction may be valuable, especially in children with predicted difficult airways. Therefore, physicians involved in the management of pediatric patients with possible airway trauma or deformity should undergo continuous periodic training and regular practice in order to identify the upper airway anatomy with ultrasound.
Funding
This study was funded by departmental sources.
References
Frerk C, Mitchell VS, McNarry AF, Mendonca C, Bhagrath R, Patel A, O’Sullivan EP, Woodall NM, Ahmad I, Difficult Airway Society intubation guidelines working g. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. Br J Anaesth. 2015;115(6):827–48.
Apfelbaum JL, Hagberg CA, Caplan RA, Blitt CD, Connis RT, Nickinovich DG, Hagberg CA, Caplan RA, Benumof JL, Berry FA, Blitt CD, Bode RH, Cheney FW, Connis RT, Guidry OF, Nickinovich DG, Ovassapian A, American Society of Anesthesiologists Task Force on Management of the Difficult A. Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 2013;118(2):251–70.
Law JA. Deficiencies in locating the cricothyroid membrane by palpation: we can’t and the surgeons can’t, so what now for the emergency surgical airway? Can J Anaesth. 2016;63(7):791–6.
Defining Childhood Obesity. October 20, 2016. https://www.cdc.gov/obesity/childhood/defining.html. Accessed 10 Aug 2017
Kristensen MS. Ultrasonography in the management of the airway. Acta Anaesthesiol Scand. 2011;55(10):1155–73.
Nicholls SE, Sweeney TW, Ferre RM, Strout TD. Bedside sonography by emergency physicians for the rapid identification of landmarks relevant to cricothyrotomy. Am J Emerg Med. 2008;26(8):852–6.
You-Ten KE, Desai D, Postonogova T, Siddiqui N. Accuracy of conventional digital palpation and ultrasound of the cricothyroid membrane in obese women in labour. Anaesthesia. 2015;70(11):1230–4.
Klucka J, Stourac P, Stoudek R, Toukalkova M, Harazim H, Kosinova M. Controversies in pediatric perioperative airways. Biomed Res Int. 2015;2015:368761.
Prunty SL, Aranda-Palacios A, Heard AM, Chapman G, Ramgolam A, Hegarty M, Vijayasekaran S, von Ungern-Sternberg BS. The ‘Can’t intubate can’t oxygenate’ scenario in pediatric anesthesia: a comparison of the Melker cricothyroidotomy kit with a scalpel bougie technique. Paediatr Anaesth. 2015;25(4):400–4.
Elliott DS, Baker PA, Scott MR, Birch CW, Thompson JM. Accuracy of surface landmark identification for cannula cricothyroidotomy. Anaesthesia. 2010;65(9):889–94.
Aslani A, Ng SC, Hurley M, McCarthy KF, McNicholas M, McCaul CL. Accuracy of identification of the cricothyroid membrane in female subjects using palpation: an observational study. Anesth Analg. 2012;114(5):987–92.
Lamb A, Zhang J, Hung O, Flemming B, Mullen T, Bissell MB, Arseneau I. Accuracy of identifying the cricothyroid membrane by anesthesia trainees and staff in a Canadian institution. Can J Anaesth. 2015;62(5):495–503.
Campbell M, Shanahan H, Ash S, Royds J, Husarova V, McCaul C. The accuracy of locating the cricothyroid membrane by palpation—an intergender study. BMC Anesthesiol. 2014;14:108.
Ajmani ML. A metrical study of the laryngeal skeleton in adult Nigerians. J Anat. 1990;171:187–91.
Randestad A, Lindholm CE, Fabian P. Dimensions of the cricoid cartilage and the trachea. Laryngoscope. 2000;110(11):1957–61.
Ezri T, Gewurtz G, Sessler DI, Medalion B, Szmuk P, Hagberg C, Susmallian S. Prediction of difficult laryngoscopy in obese patients by ultrasound quantification of anterior neck soft tissue. Anaesthesia. 2003;58(11):1111–4.
Nafiu OO, Reynolds PI, Bamgbade OA, Tremper KK, Welch K, Kasa-Vubu JZ. Childhood body mass index and perioperative complications. Paediatr Anaesth. 2007;17(5):426–30.
Fox S. Can’t intubate can’t ventilate. July 25, 2017; http://pedemmorsels.com/cant-intubate-cant-ventilate/. Accessed 16 Dec 2017
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All study documents and procedures were approved by the review board at Necmettin Erbakan University, Konya, Turkey (protocol no: 2017/937; chairperson Dr. Acıkgozoglu) on May 26 2017, and conducted in accordance with the Declaration of Helsinki.
Conflict of interest
The authors declare no conflict of interest.
About this article
Cite this article
Basaran, B., Egilmez, A.I., Alatas, N. et al. Accuracy of identifying the cricothyroid membrane in children using palpation. J Anesth 32, 768–773 (2018). https://doi.org/10.1007/s00540-018-2538-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-018-2538-0