Abstract
Heat stress is one of the most common complaints of health care employees who wear isolation gowns to protect themselves from biological agents, particularly during the warmer seasons. This study was conducted in a climatic chamber to determine the influence of airflow within isolated hospital gowns on physiological-perceptual heat strain indices. The experiment was conducted in three trials: regular clothes (CON), an impenetrable gown without air blowing (GO), and a gown with air blowing (GO + FAN) at temperature conditions of 27 °C and 25% relative humidity (RH). During the trial, physiological-perceptual response data were recorded for a half-hour on a treadmill at a speed of km/hr and a slope of 0% activity at 5-min intervals. The ASHRAE Likert scale was used to assess thermal comfort (TC), thermal sensation (TS), and skin wetness sensation (WS). As the results show, there was a significant difference in mean scores for TC and WS in both sexes when working in the CON, GO, and GO + FAN groups (P < 0.001). In women, the mean scores for TS, TC, and WS reduced considerably (P < 0.001) in the GO and GO + FAN in the amount of 10 and 12 CFM (20 \({m}^{3}\)/h), but in males, there was a statistically significant difference between mean scores (P < 0.001) in the GO + FAN at 12 CFM (20 \({m}^{3}\)/h) and 14 CFM (24 \({m}^{3}\)/h). Also, the greatest difference between the average heart rate, chest temperature, and temperature inside the clothes in women and men in the trials GO and GO + FAN was observed in the air flow 12 CFM and 14 CFM, respectively (P < 0.001). The usage of an air blower in isolated hospital clothes has been shown to influence physiological-perceptual parameters in men and women substantially. The existence of airflow in these gowns can improve safety, performance, and thermal comfort while also decreasing the risk of heat-related disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Human performance in work systems is influenced by a diverse array of factor (Jalil et al. 2007). One of these factors is environmental heat, which causes physiological responses in the body, such as an increased heart rate, core body temperature, and sweat rate (Habibi et al. 2015; Kjellstrom et al. 2009). Thermal strain stability during dehydration can result in heat-related illnesses. Heat-related symptoms include muscular cramps, weakness, heat exhaustion, and heat stroke (Habibi et al. 2019). Also, there are different important thermoregulatory parameters both in men and women, including anthropometric specifications, physiologic factors, sex hormones, and social behavioral specification. Due to a lot of differences between men and women regarding thermal comfort and physiological responses, it is necessary to evaluate the effect of thermal stress among women and men (Dehghan et al. 2013; Dehghan et al. 2015). The occurrence of heat stress is determined by environmental factors such as air temperature, relative humidity (RH), radiant heat, and airflow rate, as well as occupational factors such as physical activity, the type of clothing and personal protective equipment (PPE), and personal characteristics such as age, body mass index (BMI), and heat adaptation (Dehghan et al. 2015). In recent years, due to the epidemic of COVID-19 and the necessity to the protection of health care workers, the usage of protective gowns has expanded significantly (Omidi et al. 2020). Apart from protection individuals from environmental risks, PPE limited sweat rate from the skin surface, and this restriction of heat exchange results in prolonged heat stress. Heat stress causes a number of physical diseases, decreased job performance, decreased safety levels, and even medical errors (Fischer et al. 2015; Honda and Iwata 2016), all of which jeopardies an individual’s productivity, health, and safety (Khodakarami and Nasrollahi 2012). Tyler et al. demonstrated that wearing isolated gowns for extended periods of time is harmful and can increase health professionals’ exposure to heat and that their work time should be reduced to avoid heat stress (Quinn et al. 2017). According to Potter’s research, protective gowns exert heat strain on health care personnel, necessitating the usage of customized cooling systems to provide maximum safe working duration (Potter et al. 2015). Additionally, Davey et al. stated that heat stress impairs the performance, safety, and well-being of healthcare workers wearing PPE and that effective treatments are required (Davey et al. 2021). To minimize heat strain when wearing PPE in hospital environments, the most typical approach is to establish a work/rest plan and enhance rest time; however, this is not always practical in clinical settings like hospitals, particularly during COVID-19 pandemics where we suffer a medical personnel deficit (Bongers et al. 2021). Additionally, while employing PPE, particularly vapor-resistant protective equipment, there are two solutions: one is to maintain an ambient temperature of 20 °C, which is limited due to the diverse weather conditions and the restriction in cooling equipment (Foster et al. 2020). The second approach is to wear personal protective equipment with individual cooling equipment. Individual cooling equipment, such as cooling vests, is available today. Air-cooled vests, water-cold vests, and phase-change cooling vests include phase-change materials (PCMs) (Golbabaei et al. 2020). Each type of these equipments has a number of advantages and disadvantages. The use of air-cooled vests, cold water vests, and PCM cooling vest in hospital protective equipment is limited due to special requirements (Vahedian-Azimi et al. 2016). Numerous studies have also demonstrated that the use of electric fans to cool the entire body or a specific area of the body has resulted in an increase in thermal comfort for workers exposed to hot work environments (Gao 2014; Habibi et al. 2021). Given that the accumulation of water vapor in the space between the body’s skin and the protective equipment is the primary factor limiting heat loss through sweat, it would be advantageous to reduce the accumulation of water vapor or, in other words, the relative humadity (RH) inside the clothes and help in heat dissipation by evaporating sweat (Udayraj, Li et al. 2018). Thus, this study aimed to determine the effect of airflow within isolated medical gowns on physiological and perceptual responses of heat stress under laboratory conditions.
Materials and methods
Participants
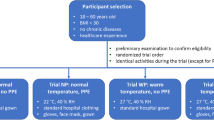
Five males (age 22.2 ± 1.78 years, height 1.78 ± 0.89 m, weight 70.95 ± 6.9 kg) and six women (age 22.5 ± 0.54 years, height 1.65 ± 0.03 m, weight 55.75 ± 8.96 kg) participated in this experimental investigation. The sample size was determined using comparable research (Ashley et al. 2008; Kakitsuba 2004). The participant was selected by inclusion criteria included age range of 20 to 40 years, normal BMI (18.5–25 kg m−2), no history of cardiovascular, pulmonary, musculoskeletal, epilepsy, seizures, or diabetes, and no use of antihypertensive medications, no history of high blood pressure medications and those that impact the heart rate, as well as abstinence from coffee and alcohol for 12 h before to the test (Habibi et al. 2012; Habibi et al. 2015). Individuals signed a written agreement to participate in the study after being informed of the study’s aims and methodology. Exclusion criteria included significant heat exhaustion, their heart rate reached 95% of the age-predicted maximum heart rate (220-age), or an elevated body temperature of more than 38 °C during the trial (Ouahrani et al. 2017).
Instruments for data collecting
The following instruments and equipment were used in this study: a blower fan (Air Blower Device BC-2.8), a hose with a diameter of 2 inches (5 CM), an airflow control valve, an 80-L (0.08\({m}^{3}\)) plastic bag, a gas meter (Shinagawa type W-NK), and a stopwatch to generate the desired airflow. Additionally, to measure physiological and perceptual parameters of related to heat stress, such as heart rate, a Finger pulse oximeter (model OXY300) with an accuracy of 0.1 °C was used; to measure skin temperature in the back and chest, a Sina RT-923 thermometer with an accuracy of 0.1 °C was used; to measure forearm and forehead skin temperature (using a device for measuring the skin temperature model Sina RT-923 with the accuracy of 0.01 °C) (Yazdanirad and Dehghan 2016); and to measure air temperature and RH inside and outside the clothing, a humidity temperature meter (TES-1364; TES Electrical Co., Taiwan) (accuracy, ± 0.5 ℃; ± 3% RH at 25 ℃) were measured, To measure the temperature and humidity inside the clothes, the instrument was placed in the space between the chest region and the clothes. (Habibi et al. 2022; Su and Chen 2015). The ASHRAE Likert scale was used to assess the TC, TS, and SS (Haddad et al. 2012; Zaki et al. 2017). The TS is defined into seven scales ranging from 0 (cold) to − 7 (very hot). TC is quantified on a four-point scale ranging from 0 (comfort) to + 4 (discomfort) (Hou et al. 2019), whereas WS is quantified on a seven-point scale ranging from − 3 (totally “dry”) to + 3 (extremely moist) (Wang et al. 2019).
Preparation of the airflow rate
To determine the range of airflow in the GO, the amount of sweat rate was determined. At this stage, four subjects (2 females and 2 males) with GO were placed in a climate chamber with temperature conditions of 25 °C and RH of 30% and moved at a speed of 2 km/h. In order to achieve thermal comfort while wearing the GO, the temperature inside the GO was considered equal to 35%, and the relative humidity was 50%. Therefore, in order to achieve these conditions, the air-blowing rate was calculated to evaporate 150 to 250 g of water in 1 h. Additionally, using a psychrometric chart and computing the ratio of humidity to a specific volume, the volume of airflow in the GO was determined to be 7.3, 10.3, and 12.9 cubic feet per minute (CFM). Flow rates were considered at 8, 10, 12, and 14 CFM (Fig. 1). Due to the fact that the minimum of the air flow in was 50 CFM(85 \({m}^{3}\)/h), which was significantly greater than the needed current air flow rates, a circuit consisting of a flow regulator valve blower, hose, plastic bag, and gas meter was employed to control the fan flow rate (Fig. 2). The fan flow rate regulated by adjusting the adjustable valve. Air was blown into the bag by a blower and timed. After the bag was filled, the fan was turned off and the suction pump(air outlet) was turned on, and the volume of air inside the bag was measured using a gas meter (calibrated by a soap bubble calibrator). The amount of air flow rate was measured based on the fan’s working duration. In order to minimize the amount of errors in each flow rate, three-time measurements were repeated and its average was calculated.
Test protocol
The experiment was conducted in three trials in CON (air permeability 150 cm3/cm2/s and thermal insulation 0.7 clo), GO and GO + FAN in a climatic chamber (the dimensions of the chamber are 3 by four and a height of 2.7 m) and a temperature of 27 °C, RH of 25% and air current speed of 0.2 ± 0.1. Each participant rested outside the room for 20 min prior to entering the test, during which time the heart rate, skin temperature (chest, back, forearm, and forehead), WS, TC, and TS were measured, as well as the temperature and RH inside and outside the GO was measured. During the trial, the subject walked for half an hour on the treadmill at a speed of 2 km/h and a slope of 0% (Dehghan and Sartang 2015) (according to the physical activity level of nurses’ job, which mainly includes light-intensity physical activity tasks (Chappel et al. 2017). During this time all physiological-perceptual data were recorded at 5-min intervals. Additionally, at the conclusion of each trial, the participant is kept outside the restroom for 20 min to allow all physiological and perceptual indications to return to normal. After establishing that all parameters returned to normal, the subject entered the next step of the experiment (Fig. 3).
Statistical analysis
In this study, descriptive statistics [means (SD)] were employed to examine the data in order to determine the average data and the amount of data dispersion depending on the study’s objectives. We performed a two-way repeated measures ANOVA to compare the measured parameters in groups with CON, GO, and GO + FAN. Data analysis was done in GraphPad Prism version 9 (Graphpad Software Inc.) (Habibi et al. 2022). P-values < 0.05 were considered statistically significant.
Results
None of the subjects displayed symptoms consistent with heatstroke or any other heat-related illness throughout the testing. Considering that the main approach in this study is to identify the most effective and at the same time the most economical (in terms of economy and energy) air flow that can improve physiological and perceptual indicators. Therefore, in the preliminary studies of the flow rate of air entering the gown in men, we came to the conclusion that the minimum flow rates considered in this research, 8 and 10 cfm, were not enough for men to improve physiological and perceptual indicators. While in women, the minimum flow rates have been somewhat effective; therefore, in this research, the minimum flow rates considered (8.10.12) for women and 12 and 14 cfm for men were evaluated.
Table 1 summarizes the enviromental and physiological parameters assessed.
Skin temperature
The statistical analysis revealed a significant difference (P < 0.05) in the mean values of the chest and back skin temperature in men and women when they walked in CON and GO (27 °C, 25%). Additionally, the mean back and chest skin temperatures were substantially different between the sexes in the trial of GO and GO + FAN (P < 0.05). The mean chest skin temperature in women was observed at an airflow of 12 CFM (20 \({m}^{3}\)/h) and at an airflow of 14 CFM (24 \({m}^{3}\)/h) in men (P < 0.001) (Fig. 4), and the mean back skin temperature in men at an airflow of 14 CFM (24 \({m}^{3}\)/h) had the greatest difference between GO and GO + FAN (P < 0.001) (Fig. 4). Figure 4C and I illustrates increases in skin temperature in the forehead area in both sexes and in CON, GO, and GO + FAN. Statistical analysis revealed no statistically significant difference in mean forehead skin temperature between subjects (P > 0.05). Figure 4J and D also depicts variations in forearm skin temperature in both sexes and in CON, GO, and GO + FAN. Statistical analysis revealed no statistically significant variation in the mean skin temperature of the forearm in different trials (P > 0.05).
Temperature and humidity
The inside temperature in CON, GO, and GO + FAN was found to be 29.5, 32.1, and 30.2 °C in men and 29.7, 31.6, and 30.2 °C in women, respectively. A statistical test revealed a significant difference in the mean of inside temperature in different trials in both sexes (P < 0.001). Thus, the greatest inside temperature difference was observed between the GO and GO + FAN in women at an airflow of 12 CFM (20 \({m}^{3}\)/h) and in males at an airflow of 14 CFM (24 \({m}^{3}\)/h) (P < 0.001) (Fig. 5).
According to the data in Table 1, the average RH in the space between the skin and clothing was 50%, 93%, and 47% for men and 39%, 87%, and 44% for women in CON, GO, and GO + FAN (14 CFM) (24 \({m}^{3}\)/h). Additionally, Fig. 5 depicts the temporal fluctuations in RH in various trials. In both sexes, a statistical test revealed a significant difference in mean RH when wearing CON, GO, and GO + FAN (P < 0.001). In women, the decrease in RH in GO + FAN at an airflow of 12 CFM (20 \({m}^{3}\)/h) compared to the GO was equivalent to 43%, while in men, the drop in RH at an airflow of 14 CFM (24 \({m}^{3}\)/h) was equal to 46% (Fig. 5).
Heart rate
According to the results in Table 1, the mean heart rate for males was 93, 103, and 99 beats per minute (BPM) in CON, GO, and GO + FAN (14 CFM) (24 \({m}^{3}\)/h), respectively, and for women was 106, 115, and 107 BPM (12 CFM). The impact was quantified on a minute basis. There was a statistically significant difference in mean heart rate values when working in CON, GO, and GO + FAN (P < 0.05). The temporal fluctuation of heart rate in various conditions is depicted in Fig. 6. The biggest drop in heart rate was seen between GO and GO + FAN in women at 12 CFM (20 \({m}^{3}\)/h) airflow (P < 0.001) and in males at 14 CFM (24 \({m}^{3}\)/h) airflow (P = 0.002). According to these adjustments, a 12 CFM (20 \({m}^{3}\)/h) airflow lowered heart rate by eight bpm in women and by four bpm in males.
Heat strain perceptual responses
The mean and standard deviation of the ratings for TS, WS, and TC are shown in Table 2.
Thermal sensation (TS)
The mean TS scores in the modes of CON, GO, and GO + FAN (14 CFM) (24 \({m}^{3}\)/h) were 3.5, 5.4, and 3.7 in males and 4.9, 4, 5.9, and 4.0 in women, respectively, based on the data in Table 2. There was a statistically significant difference in mean ratings for the TS when working in CON, GO, and GO + FAN (P < 0.05). In women, there was no significant difference in mean TS between GO and GO + FAN at air flows of 8 CFM (14 \({m}^{3}\)/h) and 10 CFM (17 \({m}^{3}\)/h) (p > 0.05), but the TS was significantly reduced at 12 CFM (20 \({m}^{3}\)/h) airflow (P < 0.001); and in men, a significant difference was observed in the mean TS in both air flows 12 CFM (20 \({m}^{3}\)/h) and 14 CFM (24 \({m}^{3}\)/h) in GO and GO + FAN (P < 0.001). The time fluctuation of the TS score in various modes is depicted in Fig. 7. Compared to the GO, the GO + FAN lowered men’s TS score by 1.7 in 14 CFM (24 \({m}^{3}\)/h) and women’s TS score by 1.9 in 12 CFM (20 \({m}^{3}\)/h) (P < 0.001).
Skin wetness sensation (SS)
According to Table 2, the mean score for SS in CON, GO, and GO + FAN (14 CFM) (24 \({m}^{3}\)/h) was 0.1, 1.5, and 0.1 for males, and 0.4, 2, 0.3 (12 CFM) (20 \({m}^{3}\)/h) for women. There was a significant difference in mean SS scores during activity when participants wore CON, GO, and GO + FAN (P < 0.001). The time fluctuation of the SS score in various conditions is depicted in Fig. 7. In women, the SS did not differ substantially between GO and GO + FAN at an airflow of 8 CFM (14 \({m}^{3}\)/h) (P > 0.05) but considerably decreased with air flows of 10 (17 \({m}^{3}\)/h) and 12 CFM (20 \({m}^{3}\)/h) (P < 0.001). Airflow of 14 CFM (24 \({m}^{3}\)/h) decreased the score by 1.4 in males, and airflow of 12 CFM (20 \({m}^{3}\)/h) decreased the SS by 1.6 in women (P < 0.001).
Thermal comfort (TC)
According to the results in Table 2, the mean score for TC in CON, GO, and GO + FAN (14 CFM) (24 \({m}^{3}\)/h) was 1.6, 2.9, and 1.6 for males and 2, 1.3, and 2.1 (12 CFM) (20 \({m}^{3}\)/h) for women. There was a significant difference in mean TC scores when working in CON, GO, and GO + FAN (P < 0.001). The time fluctuation of the TC score in various situations is depicted in Fig. 7. In women, TC was not substantially different between GO and GO + FAN with airflow of 8 CFM (14 \({m}^{3}\)/h) (P > 0.05) but dropped significantly at 10 (17 \({m}^{3}\)/h) and 12 CFM (20 \({m}^{3}\)/h) (P < 0.001). In males, the airflow of 14 CFM (24 \({m}^{3}\)/h) lowered the TC by 1.3 points; in women, the airflow of 12 CFM (20 \({m}^{3}\)/hr) decreased the TC by 1 point (P = 0.001).
Discussion
This study aimed to determine, under controlled laboratory climate conditions, the influence of airflow into isolated medical gowns on physiological-perceptual indices of heat strain. The current study’s findings indicated that there was a substantial difference in the mean values of the chest and back temperature in men and women while they exercised in CON (P < 0.05) (Fig. 4). The lowest chest temperature was found at an airflow of 12 CFM (20 \({m}^{3}\)/h) for women and 14 CFM(24 \({m}^{3}\)/h) for men, and the greatest temperature difference was seen while utilizing the GO and GO + FAN (P < 0.001) (Fig. 4). The study conducted by Song et al. examined the effects of hybrid cooling equipment (PCMs and blower airflow in the back and lower back) on physiological-perceptual parameters. The results indicated that the presence of cooling airflow could result in local cooling and a decrease in skin temperature in the chest, arm, and scapula and can contribute significantly to cooling the body when the PCMs is completely melted or when less PCM is used (Song et al. 2016). The mean back and chest temperatures in both sexes were substantially different (P = 0.05) in the case of the GO and GO + FAN in the current study, which is consistent with the study’s findings (Fig. 4). The mean heart rate in men in the three trials, CON, GO, and GO + FAN, lower than the heart rate of women in the three mentioned trials. Women are less tolerant of heat stress than males, while men have lower heart rates in response to the same degree of heat stress (Prabhavathi et al. 2014; M. Zhao et al. 2015). The mean heart rate in men in the three trials, CON, GO, and GO + FAN, lower than the heart rate of women in the three mentioned trials. In both sexes, there was a significant difference in mean heart rate during trials with various garments and air currents (P < 0.05). The biggest drop in heart rate between GO and GO + FAN was recorded in women at 12 CFM (20 \({m}^{3}\)/h) (P = 0.001) and males at 14 CFM (24 \({m}^{3}\)/h) (P = 0.002) (Fig. 6). Sweat rate and average skin temperature in response to heat differ between men and women. Women usually have more fat reserves than males, which acts as an isolator and increases heat storage and a lower aerobic capacity, which raises the task’s relative effort (Habibi et al. 2012, 2015). In women, increased airflow rate resulted in a substantial drop in mean skin temperature compared to the control group, indicating a more rapid beginning of physiological reponses to the cooling process than in males. Zhao et al. completed their study on the usage of fan-cooled gowns (12 L per second) and their influence on physiological and perceptual parameters in females during treadmill activity at 32 °C and 50% RH. The results indicated that there was no significant difference in mean skin temperature or heart rate between those who wore fan-cooled clothes and those who wore control gear. The skin temperature in the trunk area was significantly different from the control (without the use of a fan) (0.7 °C). Additionally, a significant change in air temperature and RH inside the garment was detected when wearing fan-cooled clothes vs. the control (P < 0.05). When employing fan-cooled clothes, the average temperature within the gown was around 0.8 °C lower than in control, and the skin wetedness sensation was the lowest (M. Zhao et al. 2015). The current study’s statistical data indicated that in women, the mean chest temperature at a 12 CFM (20 \({m}^{3}\)/h) blow produced the greatest temperature differential between the GO and GO + FAN (P < 0.001) (Fig. 4). In women, the air temperature inside the gown was 29.7, 31.6, and 30.2 °C for CON, GO, and GO + FAN, respectively (Table 1), with the greatest temperature difference occurring in 12 CFM (20 \({m}^{3}\)/h) airflow for GO and GO + FAN (P < 0.001) (Fig. 5). The greatest drop in average RH in the area between the skin and clothes in women was equivalent to 43% compared to the gown at an airflow of 12 CFM (20 \({m}^{3}\)/h).
The study by Johnson et al. used an air cooling vest (airflow pressure PSI 90) designed to keep gas extraction employees cool in hot-humid circumstances (35 °C and 50% RH) and hot-dry conditions (40 °C and 30% RH). The results indicated that when compared to the control, the air-cooled vest dramatically lowered the heat storage rate (by 56%) (Johnson 2013). These air-cooled vests can assist the body in evaporating through the displacement process and lowering the average heart rate and skin temperature, which is compatible with the current study's findings. Barwood et al. demonstrated that an air-cooled vest kept at 45 °C and 10% RH might minimize thermal strain in persons who had acclimated to heat without causing discomfort (Barwood et al. 2009). The accumulation of water vapor in the area between the body’s skin and the protective cover is the primary factor limiting body heat excretion via sweat evaporation; using airflow at different intensities, the accumulation of water vapor, or the RH inside the gown, could be decreased and aid in heat dissipation by evaporating sweat. When a larger blower current is employed, increased cooling by conduction and evaporation can result in a fall in temperature inside the gown and a change in the RH inside the gown, resulting in a further decrease in skin temperature owing to evaporation through sweat. Additionally, increasing the airflow velocity boosted thermal comfort, despite the fact that less air flow was employed compared to earlier research (Hadid et al. 2008; M. Zhao et al. 2015). Increased airflow resulted in a further drop in the average skin temperature in women’s and men’s chest and back areas. This is due to the effective circulation of hot air between the skin and gown layers and the discharge of heat from the body. This phenomenon is most likely caused by the quick passage of hot air via the fan in various layers between the skin and clothes and evaporation via sweat, which can effectively release body heat and the circulatory process. It has a significant influence on the release of body heat under hot weather conditions and aids in heat dissipation via sweat (Guo et al. 2019; Li et al. 2018). On the other hand, hospital employees execute a variety of duties due to the nature of their employment, including heavy tasks such as moving and transporting patients, working long shifts, and executing precise tasks. Thus, keeping workers cool and offering thermal comfort while wearing isolated clothing owing to the working environment in various areas may help maintain a high level of safety and productivity. In comparison to the scenario without blower fans, the design and installation of blower fans inside isolated clothing can offer cooling, thermal comfort, ergonomic factors (Y. J. Zhao et al. 2017), and physiological parameters (Butts et al. 2017). Among the study’s drawbacks is that it was conducted on a young, healthy group. Additional subjects with varying mean ages, a history of diseases such as diabetes, smoking, and other characteristics affecting thermal strain should be recruited in future research to determine the influence of blowing flow on the response. Different physiological and perceptual responses to heat should also be investigated (Song et al. 2016). The influence of heat acclimation in both populations and menstrual cycles on body temperature during heat exposure was not explored in this study but should be in future research. Future research should also evaluate male and female populations’ exposure to very hot temperatures. While simply blowing airflow was employed to cool in this work, combining blowing airflow with additional cooling equipment, such as PCM materials with a sufficient melting point for cooling, can increase the effectiveness of cooling (W. Song et al. 2016). In future investigations, the effect of blowing current on persons with varying vocations and various coatings will be examined in both real-world and controlled laboratory conditions (Guo et al. 2019).
Conclusion
Although the results of this study indicated that air blowing can qualitatively alleviate the level of strains in people. The main result of this study indicates that with a flow rate of 14 CFM (24 \({m}^{3}\)/h) for men and 12 CFM (20 \({m}^{3}\)/h) for women, can be reached an acceptable level of heat stress reduction and increase thermal comfort in hospital employees who are dressed in isolated gowns under moderate temperature circumstances. The usage of an air blower in isolated hospital clothes has been shown to have a substantial influence on physiological-perceptual parameters in men and women. Convective heat transfer has been found to be an effective method of lowering thermal strain and perceived comfort. The existence of airflow in these gowns can improve safety, performance, and thermal comfort while also decreasing the risk of heat-related disorders. This study may be viewed as a pilot for future research and in regions with greater temperatures and warmer seasons to increase research and the effectiveness of air-blowing within garments.
Data availability
The data supporting this study are available from the corresponding author upon reasonable request.
References
Ashley CD, Luecke CL, Schwartz SS, Islam MZ, Bernard TE (2008) Heat strain at the critical WBGT and the effects of gender, clothing and metabolic rate. Int J Ind Ergon 38(7–8):640–644
Barwood MJ, Newton PS, Tipton MJ (2009) Ventilated vest and tolerance for intermittent exercise in hot, dry conditions with military clothing. Aviat Space Environ Med 80(4):353–359
Bongers CC, De Korte JQ, Catoire M, Greefhorst J, Hopman MT, Kingma B, Eijsvogels TM (2021) Infographic Cooling strategies to attenuate PPE-induced heat strain during the COVID-19 pandemic. Br J Sports Med 55(1):69–70
Butts CL, Torretta ML, Smith CR, Petway AJ, McDermott BP (2017) Effects of a phase change cooling garment during exercise in the heat. Eur J Sport Sci 17(8):1065–1073. https://doi.org/10.1080/17461391.2017.1347205
Chappel SE, Verswijveren SJ, Aisbett B, Considine J, Ridgers ND (2017) Nurses’ occupational physical activity levels: a systematic review. Int J Nurs Stud 73:52–62
Davey SL, Lee BJ, Robbins T, Randeva H, Thake CD (2021) Heat stress and PPE during COVID-19: impact on healthcare workers’ performance, safety and well-being in NHS settings. J Hosp Infect 108:185–188
Dehghan H, Habibi E, Habibi P, Maracy MR (2013) Validation of a questionnaire for heat strain evaluation in women workers. Int J Prev Med 4(6):631
Dehghan H, Mortzavi SB, Jafari MJ, Maracy MR (2015) Development and validation of a questionnaire for preliminary assessment of heat stress at workplace. J Res Health Sci 15(3):175–181
Dehghan H, Sartang AG (2015) Validation of perceptual strain index to evaluate the thermal strain in experimental hot conditions. Int J Prev Med 6
Fischer WA II, Weber DJ, Wohl DA (2015) Personal protective equipment: protecting health care providers in an Ebola outbreak. Clin Ther 37(11):2402–2410
Foster J, Hodder SG, Goodwin J, Havenith G (2020) Occupational heat stress and practical cooling solutions for healthcare and industry workers during the COVID-19 pandemic. An Work Exp Health 64(9):915–922
Gao C (2014) Phase-change materials (PCMs) for warming or cooling in protective clothing protective clothing (pp. 227–249): Elsevier
Golbabaei F, Heydari A, Moradi G, Dehghan H, Moradi A, Habibi P (2020) The effect of cooling vests on physiological and perceptual responses: a systematic review. Int J Occup Saf Ergon(just-accepted) :1–36
Guo Y, Chan AP, Wong FK, Li Y, Sun S, Han X (2019) Developing a hybrid cooling vest for combating heat stress in the construction industry. Text Res J 89(3):254–269
Habibi P, Dehghan H, Rezaei S, Maghsoudi K (2012) Physiological and perceptual heat strain responses in Iranian veiled women under laboratory thermal conditions. Iran J Health Saf Environ 1(4):172–176
Habibi P, Moradi G, Moradi A, Heydari A (2021) The impacts of climate change on occupational heat strain in outdoor workers: a systematic review. Urban Climate 36:100770
Habibi P, Momeni R, Dehghan H (2015) Relationship of environmental, physiological, and perceptual heat stress indices in Iranian Men. Int J Prev Med 6
Habibi P, Heydari A, Moradi G, Dehghan H, Golbabaei F (2019) Effect of cooling vests on physiological and perceptual responses: a systematic review protocol: research square
Habibi P, Ostad SN, Monazzam MR, Foroushani AR, Ghazi-Khansari M, Aliebrahimi S, . . . Golbabaei F (2022) Thermal stress and TiO2 nanoparticle–induced oxidative DNA damage and apoptosis in mouse hippocampus. Environ Sci Pollut Res :1–12
Haddad S, King S, Osmond P, Heidari S (2012) Questionnaire design to determine children’s thermal sensation, preference and acceptability in the classroom. Paper presented at the Proceedings-28th international PLEA conference on sustainable architecture+ urban design: opportunities, limits and needs-towards an environmentally responsible architecture
Hadid A, Yanovich R, Erlich T, Khomenok G, Moran D (2008) Effect of a personal ambient ventilation system on physiological strain during heat stress wearing a ballistic vest. Eur J Appl Physiol 104(2):311–319
Honda H, Iwata K (2016) Personal protective equipment and improving compliance among healthcare workers in high-risk settings. Curr Opin Infect Dis 29(4):400–406
Hou J, Yang Z, Xu P, Huang G (2019) Design and performance evaluation of novel personal cooling garment. Appl Therm Eng 154:131–139
Jalil M, Sani M, Dor Z, Yahya M, Mohideen Batcha M, Hasnan K (2007) Heat stress investigation on laundry workers. Paper presented at the International Conference on Ergonomics
Johnson JK (2013) Evaluation of four portable cooling vests for workers wearing gas extraction coveralls in hot environments: University of South Florida
Kakitsuba N (2004) Dynamic changes in sweat rates and evaporation rates through clothing during hot exposure. J Therm Biol 29(7–8):739–742
Khodakarami J, Nasrollahi N (2012) Thermal comfort in hospitals–a literature review. Renew Sustain Energy Rev 16(6):4071–4077
Kjellstrom T, Holmer I, Lemke B (2009) Workplace heat stress, health and productivity - an increasing challenge for low and middle-income countries during climate change. Glob Health Action 2:46–51. https://doi.org/10.3402/gha.v2i0.2047
Li Z, Ke Y, Wang F, Yang B (2018) Personal cooling strategies to improve thermal comfort in warm indoor environments: comparison of a conventional desk fan and air ventilation clothing. Energy Buildings 174:439–451
Omidi L, Moradi G, Mostofi Sarkari N (2020) Risk of COVID-19 infection in workplace settings and the use of personal protective equipment. Work :377–378
Ouahrani D, Itani M, Ghaddar N, Ghali K, Khater B (2017) Experimental study on using PCMs of different melting temperatures in one cooling vest to reduce its weight and improve comfort. Energy Buildings 155:533–545. https://doi.org/10.1016/j.enbuild.2017.09.057
Potter AW, Gonzalez JA, Xu X (2015) Ebola response: modeling the risk of heat stress from personal protective clothing. PLoS One 10(11):e0143461
Prabhavathi K, Selvi KT, Poornima K, Sarvanan A (2014) Role of biological sex in normal cardiac function and in its disease outcome–a review. J Clin Diagn Res 8(8):BE01
Quinn T, Kim J-H, Strauch A, Wu T, Powell J, Roberge R, Coca A (2017) Physiological evaluation of cooling devices in conjunction with personal protective ensembles recommended for use in West Africa. Disaster Med Public Health Prep 11(5):573–579
Song W, Wang F, Wei F (2016) Hybrid cooling clothing to improve thermal comfort of office workers in a hot indoor environment. Build Environ 100:92–101
Su J-J, Chen Y-J (2015) Monitoring of sulfur dioxide emission resulting from biogas utilization on commercial pig farms in Taiwan. Environ Monit Assess 187(1):1–8
Udayraj Li, Z. Q., Ke, Y., Wang, F. M., & Yang, B. (2018) Personal cooling strategies to improve thermal comfort in warm indoor environments: comparison of a conventional desk fan and air ventilation clothing. Energy Buildings 174:439–451. https://doi.org/10.1016/j.enbuild.2018.06.065
Vahedian-Azimi A, Hajiesmaeili M, Amirsavadkouhi A, Jamaati H, Izadi M, Madani SJ, Miller AC (2016) Effect of the Cardio First Angel™ device on CPR indices: a randomized controlled clinical trial. Critical Care 20(1):1–8
Wang F, Song W, Ke Y, Xu P, Chow CSW, Noor N (2019) Performance enhancement of hybrid personal cooling clothing in a hot environment: PCM cooling energy management with additional insulation. Ergonomics
Yazdanirad S, Dehghan H (2016) Designing of the cooling vest from paraffin compounds and evaluation of its impact under laboratory hot conditions. Int J Prev Med 7
Zaki SA, Damiati SA, Rijal HB, Hagishima A, AbdRazak A (2017) Adaptive thermal comfort in university classrooms in Malaysia and Japan. Build Environ 122:294–306
Zhao M, Gao C, Li J, Wang F (2015) Effects of two cooling garments on post-exercise thermal comfort of female subjects in the heat. Fibers and Polymers 16(6):1403–1409
Zhao YJ, Yi W, Chan APC, Wong FKW, Yam MCH (2017) Evaluating the physiological and perceptual responses of wearing a newly designed cooling vest for construction workers. Ann Work Expo Health 61(7):883–901. https://doi.org/10.1093/annweh/wxx055
Funding
This research was supported by the Research Committee of Isfahan University of Medical Sciences and Health Services (No: 1400123).
Author information
Authors and Affiliations
Contributions
N.S. and HA.D conceived of the presented idea. P.H. helped in the coordination of the study and material preparation. N.S. performed the statistical analysis and interpretation and drafted the manuscript. HA.D. discussed the results and encouraged investigating a specific aspect of this work. P.H. helps in data collection and designing the analysis. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This research was approved by the Medical Ethics Committee of Isfahan University of Medical Sciences (IR.MUI.RESEARCH.REC.1400.191).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Soleimani, N., Habibi, P. & Dehghan, H. Effect of air blowing inside isolated hospital clothing on perceptual and physiological heat strain in laboratory conditions. Int J Biometeorol 67, 1141–1152 (2023). https://doi.org/10.1007/s00484-023-02484-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-023-02484-6