Abstract
The current study investigated the correlation between stroke mortality and temperature. Monthly and seasonal variations in stroke mortality were plotted and daily stroke-related deaths were calculated. The lag times were calculated using the time series analysis. The correlation between stroke incidence and the diurnal temperature range (DTR) was analyzed using case-crossover analysis. Global stroke mortality was described in five latitudes. In the eastern region of Inner Mongolia, the stroke mortality was 174.18/105, about twice of that of the midwestern regions (87.07/105), and temperature was negatively correlated with stroke mortality. Mortality peaked in the winter and troughed in the summer (χ2 = 13.634, P < 0.001). The days in which stroke-related deaths were greater than ten occurred between late October and early April. The effect of temperature on stroke incidence occurred during a lag time of 1 (P = 0.024) or 2 months (P = 0.039). A DTR over 13 °C was positively correlated (r = 0.95, P = 0.004) with stroke with a lag time of 1 day. The effect of temperature on stroke was shown to be the same for various populations. As the latitude increases, stroke mortality also increases with latitudes > 40°; the highest mortality was 188.05/105 at the highest latitude. Only in relatively cold regions as the temperature decreases does stroke mortality increase for various populations. Differences in the time lag as well as in the DTR lag and DTR critical point vary for both the temperature and region.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stroke is one of the leading causes of death and disability worldwide (Kim and Johnston 2011). A few epidemiological studies have described a correlation between stroke incidence and environment, with a primary focus on variations in temperature (Bi et al. 2012; Pasqualetti et al. 1990; Dawson et al. 2010). Stroke mortality has been reported to vary with temperature (Alperovitch et al. 2009; Barnett 2007; Yang et al. 2003). In some countries, the incidence of strokes or stroke mortality has been shown to have a seasonal pattern, with a peak during winter months (Capon et al. 1992; Lanska and Hoffmann 1999; Wang et al. 2013; Yang et al. 2003), although a few studies have also shown peaks during the spring and autumn months (Alter et al. 1970; Chyatte et al. 1994). The resulting conclusion has been that the majority of strokes occur in colder temperatures (Wang et al. 2013), which has been confirmed in numerous studies from the last century. Diurnal temperature range (DTR) is a meteorological indicator associated with global climate change and urbanization (Easterling et al. 1997). A number of studies regarding the correlation between temperature and stroke have also addressed the correlation between DTR and stroke. A greater than average annual DTR has been associated with an increased stroke risk in Japan (Matsumoto et al. 2010) and in the USA (Lichtman et al. 2016). In addition to temperature, the correlation between stroke incidence and other climatic parameters such as humidity, sunshine, and precipitation is still controversial (Capon et al. 1992; Goggins et al. 2012).
Stroke is the second most common cause of death among both urban and rural residents in China. The mortality from stroke was 116.63 per 100,000 individuals per year in cities and 111.74 per 100,000 individuals in rural populations. A study showed a marked geographical variation in incidence, mortality, and prevalence of stroke. Harbin, a northeast city in China, had the highest incidence of stroke, 441–486 per 100,000 individuals per year, whereas Shanghai and Chengdu, two southern cities, had incidences of 81 and 136 per 100,000 individuals per year, respectively (Liu et al. 2007). Inner Mongolia located in northern of China is one of the five autonomous regions in China. Inner Mongolia has the longest longitude, from 97° E to 126° E, and the second largest latitude, from 37° N to 53° N, in China. Inner Mongolia encompasses 1.183 million square kilometers of land area, accounting for one eighth of China, and is equivalent to the area of Britain, France, and Italy combined. The topography of Inner Mongolia is long and narrow, stretching approximately 2400 km from west to east (Tian et al. 2014). The length is twice the length of the Rhine, from the Alps to Beihai. The difference in the total amount of solar radiation between the North and South regions is 1085 MJ M−2 • A−1, which leads to changes in temperature with obvious differences between the East and Midwest regions (Chen et al. 2009). The unique geographical and climatic conditions found throughout Inner Mongolia make it an ideal area for our research. This study extensively investigates and characterizes the correlation between stroke and temperature using data from Inner Mongolia, and latitude research. The results of this study provide theoretical support for a more in-depth study regarding the correlation between stroke and temperature as well as insights into preventive measures that could be undertaken to reduce the incidence of stroke.
Methods
Data source
The collected data included the total population, total number of deaths, and the number of deaths due to stroke in Inner Mongolia from 2008 to 2012. These data were obtained from the Death Registry System (DRS), which is maintained by the Chinese Ministry of Health and executed by the Inner Mongolia Autonomous Region Centers for Disease Control and Prevention (CDC). The Chinese Ministry of Health set up five Death Registry monitoring points, while the CDC set up three Death Registry monitoring points in 102 cities and counties throughout Inner Mongolia. A total of eight monitoring points were set up to cover a population of 2.4 million individuals, which accounted for about 10% of the total population of Inner Mongolia. Five of eight monitoring points were from the DRS established by the Chinese Ministry of Health. Another three monitoring points were established by the Inner Mongolia CDC. The sampling was performed using a multistage cluster probability sampling strategy with stratification according to the classification of eastern, central, and western of China, the local gross domestic product (GDP), proportion of rural dwellers, and the total population of local areas (Xin et al. 2014a). The eight monitoring points were divided into the eastern and midwestern regions, which were classified by the administrators (officials) according to unique historical background, genetic characteristics, and geographical environment for eastern of Inner Mongolian. The eastern three monitoring points are Yakeshi City, Kailu County, and Bairin Youqi, while the midwestern five monitoring points are Sonid Youqi, Muslims District, Tumd Youqi, Ejin Horo Qi, and Linhe District. Geographic and population size of eastern region were about 39,000 km2 and 0.9 million individuals, respectively, and in midwestern region, the values were about 33,000 km2 and 1.5 million individuals, respectively. The term “stroke” in the present study denotes cerebrovascular disease (codes I60–I69) according to the Tenth Revision of the International Classification of Diseases (ICD-10) including I60, subarachnoid hemorrhage (SAH); I61, intracerebral hemorrhage (ICH); and I63, cerebral infarction (CI). Hospitals that are qualified to diagnose stroke were divided into four levels: provincial, municipal, county, and township. Diagnostic methods included pathological, clinical, surgical, and postmortem. A clinical diagnosis included an imaging diagnosis, pathological anatomy, surgical diagnosis, and a pathophysiology diagnosis (Xin et al. 2014b). Imaging diagnostic techniques included cranial computed tomography and magnetic resonance imaging in all cases. All data were checked for eligibility and validity prior to analysis. The data collected in the DRS included information on gender, age, ethnicity, marital status, educational situation, and region. Age was divided into < 50 years and ≥ 50 years. Ethnicity was divided into Mongolian, Han, and other nationalities. Marital status was divided into married and unmarried. Unmarried included unmarried, widowed, and divorced. Educational situation was divided into low and high education. Low education included illiterate and primary school; high education included middle school, college, and university. Regions were divided into rural and urban.
Four meteorological parameters were collected from the Inner Mongolia Statistical Yearbook yearly and included the average ambient temperature (AT; °C), average hours of sunshine (AS; h), average relative humidity (AH; %), and average monthly precipitation (AP; mm). Means for each parameter were based on 3-year data (2009, 2010, 2011) from the 2010, 2011, and 2012 yearbooks (Inner Mongolian Autonomous Regional Bureau of Statistics 2010, 2011, 2012). Inner Mongolia has four distinct seasons, i.e., spring (March, April, May), summer (June, July, August), fall (September, October, November), and winter (December, January, and February).
Global data describing stroke death number and population denominators from 192 countries in 2002 were obtained from the World Health Organization website (WHO 2002). We divided the globe into five temperature zones based on the following latitude ranges: 0–10, 10–23.5, 23.5–40, 40–50, and > 50° in the northern and southern hemispheres and allotted a zone to each country. The nine countries spanning the equator and those spanning the four zones of Chile (latitude18–57°) were not used.
Statistical analysis
Pearson’s correlation coefficients were used to assess the correlations between the meteorological data and stroke mortality in Inner Mongolia. Variations in the seasonal stroke mortality for the four seasons every 12 months were plotted graphically. Monthly variations were plotted as histograms separately from seasonal linear graphs. The annual percentage change (APC) was used to examine the annual change trends of stroke mortality. In addition, daily aggregation analysis and the percentage of stroke-related deaths in relation to the sociodemographic characteristics of the population in Inner Mongolia’s eastern region were examined.
A time series analysis was used to measure the temporal correlation between temperature and stroke using an average monthly temperature and monthly mortality in 2009–2011. The pairwise Granger causality (PGC) test was used to analyze whether there was a causal correlation between the two time series variables (temperature and stroke-related death). Lagged effects of temperature on stroke were also studied using the Granger causality tests of time series analysis. The premise of the Granger causality test is that the time series are stationary. Before the Granger test, the time series was verified as stationary. In our study, the augmented Dickey–Fuller (ADF) unit root test was used to examine series stability. The co-integration test was used to examine the long-term trend of two time series with the same order using a regression model to establish the regression equation.
We measured the daily number of stroke deaths in Inner Mongolia’s eastern region. We collected the highest and lowest daily temperature in order to calculate the DTR (Easterling et al. 1997) over a period of 24 h in the weather website (Tianqi) in 2011–2012. We used a case-crossover analysis to assess the correlation between DTR and the number of daily deaths from stroke. We considered the possibility of a time lag in stroke when a great change in the DTR was observed. The cases we selected were the number of stroke deaths in 1 day before death (B1), 2 days ago (B2), 3 days ago (B3), B4, B5, B6, B7, and B14; the corresponding control groups were the number of stroke deaths in day after death (A1), 2 days after (A2), 3 days after (A3), A4, A5, A6, A7, and A14, respectively.
The data were managed and analyzed using Microsoft Excel and SPSS 16.0 statistical software. The APC was calculated, Pearson’s correlation analysis, and the data were plotted. EViews 6.0 was used for the time series analysis. A significance level of P ≤ 0.05 was considered statistically significant throughout this study.
Results
Average stroke mortality was calculated to be 123.56/105/year from 2008 to 2012 at eight monitoring points in which the SAH mortality was 3.27/105 individuals (2.27%) in all stroke-related deaths, ICH mortality was 77.61/105 individuals (53.94%), and CI mortality was 59.33/105 individuals (41.24%). The total stroke data was used in the following analysis.
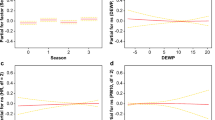
The stroke mortality in the eastern region was 174.18/105 individuals (95% confidence interval [CI], 170.47–177.90), which was twice as that in the midwestern regions, which was 87.07/105 individuals (95% CI, 84.84–89.30). An increase was observed in mortality for the eastern region (P < 0.001), with an APC of 5.8% during a 5-year period (P < 0.05), while it was not observed for the midwestern region (P = 0.154). The average temperature in the eastern region during the winter months was 7 °C lower than in the midwestern region (t = − 3.46, P < 0.001). The correlations between the meteorological parameters and stroke mortality in both regions of Inner Mongolia are shown in Table 1. AT was negatively correlated with stroke mortality for both bivariate and partial correlation analyses for the eastern region from 2008 to 2012. AT, AP, AH, and AS were all shown to have no correlations with stroke mortality for the midwestern region in both bivariate and partial correlation analyses (Supplemental material Fig. 1). The temperature in eastern region declined year by year from 2008 to 2012, fluctuating around 2.2 °C; the temperature in midwestern region was relatively stable, fluctuating around 0.8 °C (Fig. 1).
The time series included three steps. The ADF test showed that the two variables of stroke-related deaths (P = 0.012) and temperature (P = 0.0011) were fitted to the zero-order integration, indicating that the two variables were stable. PGC tests indicated that temperature was correlated with stroke-related deaths and that a 1- (P = 0.024) or 2-month (P = 0.039) lag in temperature could affect stroke-related deaths. The co-integration test showed that R2 = 0.34 after the exclusion of a one-order autocorrelation. The regression equation is y^ = 5.40–0.04Х (Supplemental material Tables 1, 2, and 3).
Seasonal and monthly stroke mortalities for the eastern and midwestern regions of Inner Mongolia are shown in Fig. 2. The mortality was 45.99/105 individuals in the spring, 35.65/105 individuals in the summer, 42.12/105 individuals in autumn, and 50.42/105 individuals in the winter in the eastern region. Mortality was observed to peak in the winter and trough in the summer (chi-square, 13.634; P < 0.001). In the midwestern region, the stroke mortality was 23.37/105 individuals in the spring, 23.30/105 individuals in the summer, 18.24/105 individuals in autumn, and 22.16/105 individuals in the winter. Mortality was shown to peak in the spring and trough in autumn (chi-square 53.93; P < 0.001).
In a graphic analysis of the seasonal data, a stroke mortality trend began in March and ended in February. A description of the monthly trend started at the beginning of January. In the eastern region, a decrease in stroke mortality was observed from January to August, whereas an increase in mortality was observed from August to December, with a trough in August. A general decline in stroke mortality was observed for the midwestern region from January to December.
A daily aggregation analysis indicates that the days in which there were ten or more stroke-related deaths occurred during late October to the following early April in the three banners in the eastern region from 2008 to 2012 (data not shown).
The percentage of stroke-related deaths by season in relation to the sociodemographic characteristics of the population in Inner Mongolia’s eastern region in 2008–2012 is shown in Table 2. The highest percentage of stroke-related deaths occurred in the winter months and the lowest percentage occurred in the summer months, regardless of the sociodemographic characteristics of the population. The seasonal pattern of the effect of temperature on stroke was not significantly different among various populations (P < 0.05).
The exposure–response correlation between DTR and the OR of stroke-related death at 1 day before death lagged day was determined using the case-crossover analysis and is shown in Fig. 3. DTR was positively correlated (r = 0.95, P = 0.004) with stroke-related death when the DTR was greater than 13 °C. No association was observed when the DTR was less than 13 °C.
The global stroke mortality within the five temperature zones is shown in Fig. 4. The stroke mortality in the southern hemisphere has a relatively smaller impact on global mortality as compared with that of the northern hemisphere, as evidenced by the almost overlapping mortality curve for the northern hemisphere with the global mortality curve. The stroke mortality curve was relatively smooth within the latitude range of 0–40° in the northern hemisphere, representing 48.41–55.62/105 individuals. The same latitude in the southern hemisphere showed a similar mortality curve despite the seemingly linear upward trend in mortality. Stroke mortality has an obvious linear upward trend at latitudes > 40°. The maximum mortality included a total of 188.05/105 individuals at the highest northern latitude (> 50°) and 89.43/105 individuals in the southern latitude range of 40–50°; this range was used due to a lack of countries located in the southern hemisphere with a latitude > 50° (Supplemental material Fig. 2).
The effect of temperature on stroke was not correlated to the characteristics of a specific population, including gender, age, ethnicity, marital status, educational status, and the region in eastern of Inner Mongolian.
Discussion
The results of our study using data from Inner Mongolia indicate that temperature is the key climatic variable for stroke occurrence and that as temperatures decrease, stroke-related deaths increase (Kyobutungi et al. 2005; Díaz et al. 2005; Donaldson 1997; Phung et al. 2016; Wang et al. 2016; Yang et al. 2016).
In this study, the temperature during the winter months in the eastern region is 7 °C lower than that observed for the midwestern region. Thus, the lower temperature in the eastern region significantly correlates with an increase in stroke mortality by twice the extent of that for the midwestern region, in which no correlation was found between temperature and stroke. Furthermore, temperature was negatively correlated with stroke mortality in the eastern region. This difference has also been reported for Sheffield and Norfolk, which are located at the north and east of England, respectively (Myint et al. 2007; Talbot 1973). These results suggest that lower temperatures have a greater effect on stroke-related mortality, whereas higher temperatures do not.
Using data from the five temperature zones, we found a negative effect of temperature on stroke mortality at latitudes > 40°, i.e., the higher the latitude, the higher the stroke mortality. In other words, the lower the temperature, the higher the stroke mortality in temperate or boreal regions. Lower temperatures in the temperate and boreal regions were associated with a stroke mortality that was twice as high as what was observed for the tropical and subtropical regions (126/105 individuals vs. 58/105 individuals). Stroke mortality in the tropical and subtropical regions of the southern hemisphere was found to be similar to that of the northern hemisphere. In the southern hemisphere, an upward trend was observed in only two countries within the temperate and boreal regions. Thus, the impact of temperature on stroke in both hemispheres was found to be consistent. The global data used in our analysis were derived from stroke deaths from the population worldwide (rather than regional or sampling). We found minimal sampling error and considered the calculated results to be reliable. Thus, stroke was ultimately associated with low temperatures worldwide. Analysis of the five temperature zones worldwide also demonstrated that the mortality peaked in the coldest regions. Temperatures in the tropical and subtropical regions did not affect stroke mortality. This result suggested that stroke mortality peaked at the coldest temperatures.
Our analysis of stroke mortality by season revealed that stroke mortality peaks in the winter in Inner Mongolia. Our daily aggregation analysis showed that the days in which stroke-related deaths were greater than ten occurred during a period in which the coldest temperatures were being experienced.
Thus, the above findings suggested that cold temperatures were a factor for stroke mortality, and further strengthened the hypothesis that the negative correlation between temperature and stroke is conditional, i.e., temperature affects stroke mortality only in cold regions. Moreover, the effect of temperature on stroke was not correlated to the characteristics of a specific population, including gender, age, ethnicity, marital status, educational status, and the region.
In our current study, the time series analysis also confirmed that lower temperatures were a reason for stroke-related deaths, even after a 1- or 2-month lag period. Many studies have reported a several-day-long lag between temperature variation and stroke occurrence (Díaz et al. 2005; Morabito et al. 2011), while only one study reported a lag of 1 month between temperature variation and stroke occurrence (Analitis et al. 2008). This lag time reached 2 months in our study. The lag interval for stroke is generally related to effects on blood viscosity or coagulation (Hong et al. 2003). In more prolonged periods of cold weather, the lag time also resulted in an increase in cholesterol (Bull et al. 1979). Nevertheless, high arterial pressure and an increased cholesterol level over a period of months or years are also well known to result in an increase in atheroma. Therefore, increased arterial pressure is likely to contribute to the slower effects of cold weather–related cerebral thrombosis (Keatinge et al. 1984; Kannel et al. 1971). This can explain the lag time of 1–2 months in mortality detected in this study.
We also found that temperature fluctuations impacted stroke mortality. It was a reflection of lower temperature in the colder regions. The influence of DTR on stroke mortality also had a time lag. A larger DTR in B1 was correlated with an increase in stroke-related deaths. Our result was consistent with what was reported from Hong Kong (Tam et al. 2009). Different lag times of 3–4 days were reported for Shanghai in China (Chen et al. 2007) and within hours in Boston (Mostofsky et al. 2014). DTR was correlated with the risk of stroke-related death and the critical point of DTR differed, depending on the local climate characteristics. The risk of stroke-related death increases with an increase in the DTR when the DTR was greater than 13 °C. Thus, 13 °C was a critical point in our study of climate conditions, with the DTR ranging from 2 to 21 °C and the greatest difference in temperature for a year ranging from − 37 to 28.5 °C. The critical point was 5 °C in Germany (Kyobutungi et al. 2005) with the greatest difference in temperature for a year ranging from − 10 to 30 °C. Thus, different temperatures in various regions have a different lag time with different critical points.
Connor et al. noted that one possible reason for the inconsistent findings might be the omission of other meteorological factors, such as humidity and solar activity (Connor 2002). Thus, our current study included AH, AS, and AP; however, no correlation was found between these factors and stroke mortality. In the last decade, investigations regarding the impact of AH, AS, and AP on stroke showed that these meteorological parameters are not primary contributing factors.
In summary, temperature affected stroke in cold regions in cold months or seasons. With the increase of temperature, the influence of temperature on stroke weakened or disappeared based on the results obtained in Inner Mongolian and at five latitudes. The effect characteristics of temperature on stroke death had no crowd specificity. The lag time between the observed temperature and the stroke death was as long as 2 months. The DTR was below 13 °C with a 1-day lag.
References
Alperovitch A, Lacombe JO, Dartigues J, Ritchie K, Ducimetiere P, Tzourio C (2009) Relationship between blood pressure and outdoor temperature in a large sample of elderly individuals: the three-city study. Arch Intern Med 169(1):75
Alter M, Christoferson L, Resch J, Myers G, Ford J (1970) Cerebrovascular disease: frequency and population selectivity in an upper midwestern community. Stroke 1(6):454–465
Analitis A, Katsouyanni K, Biggeri A, Baccini M, Forsberg B, Bisanti L, Kirchmayer U, Ballester F, Cadum E, Goodman PG, Hojs A, Sunyer J, Tiittanen P, Michelozzi P (2008) Effects of cold weather on mortality: results from 15 European cities within the PHEWE project. Am J Epidemiol 168(12):1397–1408
Barnett AG (2007) Temperature and cardiovascular deaths in the US elderly: changes over time. Epidemiology 18(3):369–372
Bi SZ, Chen JH, Yuan FS (2012) Study of the relationship between air temperature and stroke in Changzhi area. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 24(9):556
Bull GM, Brozovic M, Chakrabarti R, Meade TW, Morton J, North WR et al (1979) Relationship of air temperature to various chemical, haematological, and haemostatic variables. J Clin Pathol 32(1):16–20
Capon A, Demeurisse G, Zheng L (1992) Seasonal variation of cerebral hemorrhage in 236 consecutive cases in Brussels. Stroke 23(1):24–27
Chen G, Zhang Y, Song G, Jiang L, Zhao N, Chen B, Kan H (2007) Is diurnal temperature range a risk factor for acute stroke death? Int J Cardiol 116(3):408–409
Chen XQ, Peng JD, Hui-Min LI (2009) Seasonal and regional differences of air temperature changes in Inner Mongolia. Geogr Res 28(1):27–35
Chyatte D, Chen TL, Bronstein K, Brass LM (1994) Seasonal fluctuation in the incidence of intracranial aneurysm rupture and its relationship to changing climatic conditions. J Neurosurg 81(4):525–530
Connor MD (2002) Does the weather influence stroke incidence? Stroke 33(7):1751–1758
Dawson J, Quinn T, Walters MR (2010) Under the weather with stroke; more data emerge. Int J Stroke 4(1):19–20
Díaz J, García R, López C, Linares C, Tobías A, Prieto L (2005) Mortality impact of extreme winter temperatures. Int J Biometeorol 49(3):179–183
Donaldson G (1997) Cold exposure and winter mortality from ischaemic heart disease, cerebrovascular disease, respiratory disease, and all causes in warm and cold regions of Europe. The Eurowinter group. Lancet 349(9062):1341–1346
Easterling DR, Horton B, Jones PD, Peterson TC, Karl TR, Parker DE, et al (1997). Maximum and minimum temperature trends for theglobe.Science, 277(5324):364-367
Goggins WB, Woo J, Ho S, Chan EY, Chau PH (2012) Weather, season, and daily stroke admissions in Hong Kong. Int J Biometeorol 56(5):865-872
Hong YC, Rha JH, Lee JT, Ha EH, Kwon HJ, Kim H (2003) Ischemic stroke associated with decrease in temperature. Epidemiology 14(4):473–478
Inner Mongolian Autonomous Regional Bureau of Statistics (2010) Inner Mongolia Statistical Yearbook 2009. Inner Mongolian, China
Inner Mongolian Autonomous Regional Bureau of Statistics (2011) Inner Mongolia Statistical Yearbook 2010. Inner Mongolian, China
Inner Mongolian Autonomous Regional Bureau of Statistics (2012) Inner Mongolia Statistical Yearbook 2011. Inner Mongolian, China
Kannel WB, Gordon T, Schwartz MJ (1971) Systolic versus diastolic blood pressure and risk of coronary heart disease. The Framingham study. Am J Cardiol 27(4):335–346
Keatinge WR, Coleshaw SRK, Cotter F, Mattock MB, Murphy M, Chelliah R (1984) Increase in platelet and red cell counts, blood viscosity, and arterial pressure during mild surface cooling: factors in mortality from coronary and cerebral thrombosis in winter. Br Med J 289(6456):1405–1408
Kim AS, Johnston SC (2011) Global variation in the relative burden of stroke and ischemic heart disease. Circulation 124(3):314–323
Kyobutungi C, Grau A, Stieglbauer G, Becher H (2005) Absolute temperature, temperature changes and stroke risk: a case-crossover study. Eur J Epidemiol 20(8):693–698
Lanska DJ, Hoffmann RG (1999) Seasonal variation in stroke mortality rates. Neurology 52(5):984–990
Lichtman JH, Leifheit-Limson EC, Jones SB, Wang Y, Goldstein LB (2016) Average temperature, diurnal temperature variation, and stroke hospitalizations. J Stroke Cerebrovasc Dis 25:1489–1494
Liu M, Wu B, Wang W-Z, Lee L-M, Zhang S-H, Kong L-Z (2007) Stroke in China: epidemiology, prevention, and management strategies. Lancet Neurol 6:456–464
Matsumoto M, Ishikawa S, Kajii E (2010) Cumulative effects of weather on stroke incidence: a multi-community cohort study in Japan. J Epidemiol 20(2):136–142
Morabito M, Crisci A, Vallorani R, Modesti PA, Gensini GF, Orlandini S (2011) Innovative approaches helpful to enhance knowledge on weather-related stroke events over a wide geographical area and a large population. Stroke 42(3):593–600
Mostofsky E, Wilker EH, Schwartz J, Zanobetti A, Gold DR, Wellenius GA, Mittleman MA (2014) Short-term changes in ambient temperature and risk of ischemic stroke. Cerebrovasc Dis Extra 4(1):9–18
Myint PK, Vowler SL, Woodhouse PR, Redmayne O, Fulcher RA (2007) Winter excess in hospital admissions, in-patient mortality and length of acute hospital stay in stroke: a hospital database study over six seasonal years in Norfolk, UK. Neuroepidemiology 28(2):79–85
Pasqualetti P, Natali G, Casale R, Colantonio D (1990) Epidemiological chronorisk of stroke. Acta Neurol Scand 81(1):71–74
Phung D, Guo Y, Thai P, Rutherford S, Wang X, Nguyen M, Do CM, Nguyen NH, Alam N, Chu C (2016) The effects of high temperature on cardiovascular admissions in the most populous tropical city in Vietnam. Environ Pollut 208(2015):33–39
Talbot S (1973) Epidemiological features of subarachnoid and cerebral haemorrhages. Postgrad Med J 49(571):300–304
Tam WWS, Tzewai W, Chair SY, Wong AHS (2009) Diurnal temperature range and daily cardiovascular mortalities among the elderly in Hong Kong. Arch Environ Occup Health 64(3):202–206
Tian X, Zhang Y, Gu S, Fan Y, Sun Q, Zhang B et al (2014) New coxsackievirus b4 genotype circulating in Inner Mongolia autonomous region, China. Plos One 9(3):e90379
Wang K, Li H, Liu W, You C (2013) Seasonal variation in spontaneous intracerebral hemorrhage frequency in Chengdu, China, is independent of conventional risk factors. J Clin Neurosci 20(4):565–569
Wang X, Cao Y, Hong D, Zheng D, Richtering S, Sandset EC et al (2016) Ambient temperature and stroke occurrence: a systematic review and meta-analysis. Int J Environ Res Public Health 13(7)
WHO (2002). http://www.who.int/cardiovascular-diseases/resources/atlas/en/. Accessed 2002
Xin KP, Du ML, Li ZJ, Li Y, Li W, Su X et al (2014a) Mortality of urinary tract cancer in Inner Mongolia 2008–2012. Asian Pac J Cancer Prev 15(6):2831–2834
Xin KP, Du ML, Liu ZY, Wang WR, Qian YG, Liu L et al (2014b) Colorectal cancer mortality in Inner Mongolia between 2008 and 2012. World J Gastroenterol 20(25):8209–8214
Yang W, Levi CR, Attia JR, D’Este CA, Spratt N, Fisher J (2003) Seasonal variation in stroke in the hunter region, Australia. Stroke 34(5):1144–1150
Yang J, Peng Y, Zhou M, Ou CQ, Li M, Jing L et al (2016) The burden of stroke mortality attributable to cold and hot ambient temperatures: epidemiological evidence from China. Environ Int 92-93:232–238
Funding
The study was supported by the Inner Mongolia Medical University Students Innovation and Entrepreneurship Program Training Project Autonomous Region. (No. 201810132010) and the Natural Science Foundation of Inner Mongolia in China (No. 2013MS1124).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
This manuscript has been thoroughly edited by a native English speaker from an editing company. Editing certificate will be provided upon request.
Electronic supplementary material
ESM 1
(DOCX 229 kb)
Rights and permissions
About this article
Cite this article
Guo, W., Du, M., Sun, D. et al. The effect characteristics of temperature on stroke mortality in Inner Mongolia and globally. Int J Biometeorol 63, 159–166 (2019). https://doi.org/10.1007/s00484-018-1647-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-018-1647-7