Abstract
Background
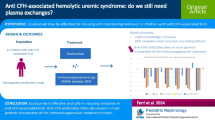
Disorders of complement regulation are the most important etiology of atypical hemolytic uremic syndrome (aHUS). Recent studies demonstrate that eculizumab is beneficial in long-term aHUS treatment. We present a series of children with aHUS resistant to/dependent on plasma exchange (PE) who were treated with eculizumab.
Methods
This was a retrospective study in which data were retrieved from the medical files of children who had received PE as treatment for aHUS. The data retrieved included age, sex, presenting symptoms, presence of diarrhea/vomiting, hospitalization duration, laboratory data on admission and follow-up, need for transfusion or dialysis, response to PE, response to eculizumab and outcome.
Results
Of the 15 children diagnosed with aHUS in 2011 and 2012 in our departments, ten were resistant to, or dependent on, plasma therapy and treated with eculizumab; these children were enrolled in the study. Three patients had relapses, and seven had a new diagnosis. Nine children had oliguria or anuria, and eight required dialysis. Hypertension was observed in six patients. Neurologic involvement developed in six patients, with the symptoms including seizures, loss of balance, vision loss and severe confusion. Five and five patients were resistant to and dependent on plasma therapy, respectively. Following the start of eculizumab treatment, all patients achieved full recovery of renal function and hematologic parameters.
Conclusions
In our ten pediatric patients with aHUS who did not respond to PE, eculizumab was a lifesaving therapy and improved their quality of life. Early eculizumab use was a rescue therapy for renal function. Our results show that eculizumab is an effective treatment for aHUS. However, more studies are needed on the long-term efficacy and safety of eculizumab in children with aHUS and to determine the optimal duration of treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atypical hemolytic uremic syndrome (aHUS) is a heterogeneous disease that is defined by the association of hemolytic anemia, thrombocytopenia and acute renal failure. Disorders of complement regulation are the most important factors in the etiology of aHUS. Patients with aHUS have a poor prognosis with high morbidity and mortality. Mortality is higher in children, but renal prognosis is worse in adults than children. In children, relapses during the first year of the disease occur in 57 % of patients. Progression to end-stage renal disease (ESRD) occurs in 20 % of children with aHUS [1]. Based on the results of their nation-wide study comparing children and adults with aHUS, Fremeaux-Bacchi et al. recently demonstrated that 23 % of all patients and 56 % of pediatric patients had aHUS before the age of 2, but that approximately 60 % of all cases occurred during adulthood [1]. These findings indicate that aHUS is not an illness that occurs only during early infancy.
Some cases of complement dysfunction appear to respond to plasma therapy, including plasma infusion and plasma exchange (PE) [2]. Until recent years, plasma therapy was the only available therapy for aHUS, but it often was not effective. It has recently been shown that eculizumab, a humanized monoclonal antibody directed against complement C5, is an effective therapy in complement-related aHUS and that it may be beneficial in the long-term treatment of aHUS [3, 4]. Eculizumab binds to C5 and prevents the cleavage of C5 to C5a and C5b and the formation of the C5b-C9 membrane attack complex. It is effective in patients with or without identified complement mutations [5]. In their recent review Wong et al. found that eculizumab therapy is effective in approximately 85 % of patients who are resistant to, or dependent on, plasma therapy [6].
Here, we report our case series of children with aHUS who were resistant to, or dependent on, plasma therapy and who were successfully treated with eculizumab.
Methods
This was a retrospective study in which data were retrieved from the medical files of children who had received plasma therapy as treatment for aHUS. The data retrieved included age, sex, presenting symptoms, presence of diarrhea and/or vomiting, hospitalization duration, laboratory data on admission and follow-up, need for transfusions, need for dialysis, response to PE, response to eculizumab and outcome.
aHUS was defined as HUS negative for Shiga toxin-producing Escherichia coli (STEC). Stool culture and serologic tests for Shiga toxin-producing organisms were performed for all patients. Glomerular filtration rate was calculated using serum creatinine and urine creatinine measured in a 24-h urine collection. Proteinuria was assessed using 24-h urine protein excretion.
Blood samples were collected prior to the start of plasma therapy to measure complement C3, complement C4, autoantibodies against complement factor H (CFH) and the activity of a disintegrin and metalloproteinase with a thrombospondin type 1 motif, member 13 (ADAMTS13). Serum samples were tested for the presence of autoantibodies against CFH using an enzyme-linked immunosorbent assay (normal range <1 AU/mL). Genetic screening of the genes encoding CFH, complement factor I (CFI), complement factor B (CFB), C3 and membrane cofactor protein (MCP) was performed for all patients by direct sequencing of the coding sequences and flanking intronic lesions. Genomic DNA was extracted from blood leukocytes.
PE was achieved by plasma filtration with anticoagulant cover using fresh frozen plasma (1.5× plasma volume) and was performed daily during the first 5 days of treatment, then continued with five sessions per week. Fresh frozen plasma infusions were given daily during the first 5 days, then continued every other day. Patients showing no clinical or laboratory improvement by the second week were defined as plasma-resistant, and patients showing inadequate clinical and laboratory improvement by the second week, or who had clinical or laboratory deterioration after tapering of plasma therapy, were defined as plasma-dependent. In pediatric aHUS patients aged <18 years, the eculizumab dosing regimen was based on patient body weight.
Results
Patient characteristics
In 2011 and 2012, 15 children were diagnosed with aHUS in our pediatric nephrology departments. Five patients responded to plasma therapy, which could be stopped after recovery of the clinical and laboratory parameters. In one of these patients, an MCP mutation was detected, and genetic screening is ongoing for other patients.
The remaining ten patients (7 girls, 3 boys) did not respond to, or were dependent on, plasma therapy and were treated with eculizumab; these patients were enrolled in this study. Three patients had a relapse and seven patients had a new diagnosis of aHUS (Table 1). The median age at aHUS onset was 4 (range 1.5–-12.5) years. Nine children (90 %) had oliguria or anuria, and eight (80 %) required dialysis. Hypertension was observed in six children (Table 1).
Neurologic involvement developed in six patients, with the symptoms including seizures, balance loss, vision loss and severe confusion. Of these six patients, two had lesions related to posterior reversible encephalopathy syndrome (PRES) on magnetic resonance imaging (MRI), and four had normal MRI findings. No patient had evidence of central nervous system (CNS) infarction.
Stool specimens were negative for STEC and Shigella dysenteriae type 1. Diarrhea developed in two patients without positive stool specimens. Gastrointestinal involvement was present with vomiting and stomach ache in three patients (Table 1). Laboratory studies at onset of aHUS showed that five patients (50 %) had low C3 levels and nine patients (90 %) had low haptoglobulin levels (Table 2). Levels of autoantibodies to CFH were negative, and ADAMTS13 activity was normal in all patients (Table 2). The results of mutation analysis were obtained for three patients; genetic screening of the other patients is ongoing (Table 2).
Plasma therapy
The initial treatment of all patients was PE and plasma infusion (Table 3). Five patients (50 %) were resistant to plasma therapy (Table 1). Recovery of clinical and laboratory parameters was achieved in the remaining five patients (50 %) with plasma therapy, but this did not stop the syndrome, and relapses occurred after discontinuation of therapy; these patients were rated as having aHUS dependent on plasma therapy (Table 4).
Eculizumab therapy
A median number of two doses of eculizumab was required to achieve clinical and laboratory improvement (range 1–5 doses). Median follow-up after initiation of eculizumab therapy was 23 (range 20–38) months. Full recovery of hematologic parameters and renal function was obtained in all patients (Tables 5, 6). No systemic complications related to eculizumab were observed.
Discussion
Atypical HUS is associated with defective regulation of the alternative complement pathway in >50 % cases. Mutations in genes encoding CFH, MCP (CD46), CFI, thrombomodulin, CFB or C3 or CFH autoantibodies have been reported to predispose to aHUS. All of these changes cause overactivation of the alternative pathway [4, 7]. CFH and thrombomodulin mutations are associated with the earliest onset of aHUS and highest mortality. Autoantibodies against CFH or MCP mutation-related aHUS mainly occur after 2 years of age. MCP mutations are associated with the best prognosis [8]. The genetic results on all of our patients were not available at the time of writing. The results from genetic screening alone cannot predict the severity and outcome of the disease [9], but they are helpful, although not necessary, for treatment planning and may affect long-term treatment options [3]. In fact, a medical history and rapid laboratory tests are sufficient for aHUS diagnosis, although Shiga toxin-related HUS and ADAMTS13 deficiency must be excluded before treatment..
Low C3 levels can be detected in one-third of all aHUS patients [1]. In our patient group, five (50 %) children presented with low C3 levels. Low levels of complement C3 may indicate complement dysregulation in aHUS, but this is not a definite indication [10].
In their recent study, Fremeaux-Bacchi et al. demonstrated neurologic involvement in 16 % of patients with aHUS [1]. Neurologic complications are a major cause of morbidity and mortality; among extrarenal complications, CNS manifestations are observed in 20–50 % of patients [11]. Neurologic symptoms range from irritability to coma and can be a consequence of cerebral microangiopathy, hypertension, cerebral edema or late referral for treatment. Complement activation, and subsequent C5a generation, is thought to play an important role in the progression of CNS disease [12]. In our study, six patients had neurologic complications, and three of these had higher blood pressure when manifesting neurologic symptoms. Plasma electrolyte concentrations were normal at the time these patients developed signs of CNS disease. Four patients were referred after 1 week for treatment. The MRI findings of CNS involvement in HUS are diverse, and PRES-related lesions can be demonstrated. Another type of lesion has also been described during the acute phase of HUS, with bilateral and symmetric thalami, brainstem and deep white matter involvement [13]. We demonstrated PRES-related lesions in only two patients, and the MRI features of these patients were not consistent with the diagnosis of PRES or aHUS involvement [12].
In contrast with typical HUS, aHUS is characterized by relapses in many cases. Plasma therapy is considered to be the first-line therapy for patients during the acute episode of aHUS and should be started within 24 h of diagnosis [14]. However, this is not always possible in clinical practice, as in our cases. Plasma therapy is also not successful in all patients, and patients can become dependent on, or resistant to, this treatment. The necessity of lifelong treatment in patients who are dependent on plasma therapy could result in reactions to plasma and may worsen school performance and social activities. The morbidity and mortality of catheter placement and PE are also important issues, and most studies suggest that plasma therapy often fails to rescue kidney function [15, 16]. More recently, combined kidney and liver transplant, a high-risk procedure, has been considered a last alternative for patients resistant to plasma therapy. Combined kidney–liver transplant should not be performed unless a patient is at high risk for life-threatening complications. Eculizumab is also a treatment option in the setting of transplant following ESRD [17, 18].
In 2014, The European Paediatric Study Group for Haemolytic Uraemic Syndrome published a new audit analysis of a clinical practice guideline for the investigation and initial therapy of aHUS. The guideline continues to recommend plasma therapy. Only two patients were treated with eculizumab in their registry, and eculizumab is not recommended in this guideline because of the lack of prospective pediatric trials [19]. Eculizumab has high potential in this area. The long-term use of eculizumab is associated with extremely high costs, and the optimal duration of therapy is unpredictable, but it is a rescue therapy for aHUS. In addition, eculizumab has a successful effect on recovery of renal function. Legendre et al. recently demonstrated that five of their seven plasmapheresis-resistant dialysis patients could come off dialysis following treatment with eculizumab [20]. In our study, full recovery of renal function was obtained in all patients. Proteinuria disappeared and complete neurologic recovery was achieved after eculizumab therapy.
The results of eculizumab use in patients with aHUS are encouraging. After exclusion of STEC-HUS and ADAMTS13 deficiency, and if eculizumab is available, this therapy can be the first-line treatment for aHUS. We do not know the circumstances under which eculizumab can be safely discontinued and which patients are at high risk of severe recurrence. At present, we can suggest that eculizumab is lifesaving and may improve quality of life. We also suggest that early use of eculizumab is a rescue therapy for renal function. However, more studies should be conducted to understand the long-term efficacy and safety of eculizumab in children who have aHUS. Large studies are needed to determine the optimal duration of treatment.
References
Fremeaux-Bacchi V, Fakhouri F, Garnier A, Bienaimé F, Dragon-Durey MA, Ngo S, Moulin B, Servais A, Provot F, Rostaing L, Burtey S, Niaudet P, Deschênes G, Lebranchu Y, Zuber J, Loirat C (2013) Genetics and outcome of atypical hemolytic uremic syndrome: a nationwide French series comparing children and adults. Clin J Am Soc Nephrol 8:554–562
Ariceta G, Besbas N, Johnson S, Karpman D, Landau D, Licht C, Loirat C, Pecoraro C, Taylor CM, Van de Kar N, VandeWalle J, Zimmerhackl LB (2009) The European Paediatric Study Group for HUS. Guideline for the investigation and initial therapy of diarrhea-negative hemolytic uremic syndrome. Pediatr Nephrol 24:687–696
Zuber J, Fakhouri F, Roumenina LT, Loirat C, Frémeaux-Bacchi V (2012) Use of eculizumab for atypical haemolytic uraemic syndrome and C3 glomerulopathies. Nat Rev Nephrol 8:643–657
Tschumi S, Gugger M, Bucher BS, Riedl M, Simonetti GD (2011) Eculizumab in atypical hemolytic uremic syndrome: long-term clinical course and histological findings. Pediatr Nephrol 26:2085–2088
Kavanagh D, Goodship TH, Richards A (2013) Atypical hemolytic uremic syndrome. Semin Nephrol 6:508–530
Wong EKS, Goodship THJ, Kavanagh D (2013) Complement therapy in atypical haemolytic uraemic syndrome (aHUS). Mol Immunol 56:199–212
Geerdink LM, Westra D, Van Wijk JAE, Dorresteijn EM, Lilien MR, Davin JC, Kömhoff M, Van Hoeck K, Van der Vlugt A, Van den Heuvel LP, Van de Kar NCA (2012) Atypical hemolytic uremic syndrome in children: complement mutations and clinical characteristics. Pediatr Nephrol 27:1283–1291
Noris M, Caprioli J, Bresin E, Mossali C, Pianetti G, Gamba S, Daina E, Fenili C, Castelletti F, Sorinosa A, Piras R, Donadelli R, Maranta R, van der Meer I, Conway EM, Zipfel PF, Goodship TH, Remuzzi G (2010) Relative role of genetic complement abnormalities in sporadic and familial aHUS and their impact on clinical phenotype. Clin J Am Soc Nephrol 5:1844–1859
Rees L (2013) Atypical HUS: time to take stock of current guidelines and outcomes measures? Pediatr Nephrol 28:675–677
Kavanagh D, Goodship TH, Richards A (2006) Atypical haemolytic uraemic syndrome. Br Med Bull 77–78:5–22
Koehl B, Boyer O, Biebuyck-Gougé N, Kossorotoff M, Frémeaux-Bacchi V, Boddaert N, Niaudet P (2010) Neurological involvement in a child with atypical hemolytic uremic syndrome. Pediatr Nephrol 25:2539–2542
Gulleroglu K, Fidan K, Hancer VS, Bayrakci U, Baskin E, Soylemezoglu O (2013) Neurologic involvement in atypical hemolytic uremic syndrome and successful treatment with eculizumab. Pediatr Nephrol 28:827–830
Nathanson S, Kwon T, Elmaleh M, Charbit M, Launay EA, Harambat J, Brun M, Ranchin B, Bandin F, Cloarec S, Bourdat-Michel G, Piètrement C, Champion G, Ulinski T, Deschênes G (2010) Acute neurological involvement in diarrhea-associated hemolytic uremic syndrome. Clin J Am Soc Nephrol 5:1218–1228
Waters AM, Licht C (2011) aHUS caused by complement dysregulation: new therapies on the horizon. Pediatr Nephrol 26:41–57
Rizvi MA, Vesely SK, George JN, Chandler L, Duvall D, Smith JW, Gilcher RO (2000) Complications of plasma exchange in 71 consecutive patients treated for clinically suspected thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Transfusion 40:896–901
Loirat C, Frémeaux-Bacchi V (2011) Atypical hemolytic uremic syndrome. Orphanet J Rare Dis 6:60
Noris M, Remuzzi G (2005) Hemolytic uremic syndrome. J Am Soc Nephrol 16:1035–1050
Saland J (2014) Liver-kidney transplantation to cure atypical HUS: still an option post-eculizumab? Pediatr Nephrol 29:329–332
Johnson S, Stojanovic J, Ariceta G, Bitzan M, Besbas N, Frieling M, Karpman D, Landau D, Langman C, Licht C, Pecoraro C, Riedl M, Siomou E, van de Kar N, Walle JV, Loirat C, Taylor CM (2014) An audit analysis of a guideline for the investigation and initial therapy of diarrhea negative (atypical) hemolytic uremic syndrome. Pediatr Nephrol 29:1967–1978
Legendre CM, Licht C, Muus P, Greenbaum LA, Babu S, Bedrosian C, Bingham C, Cohen DJ, Delmas Y, Douglas K, Eitner F, Feldkamp T, Fouque D, Furman RR, Gaber O, Herthelius M, Hourmant M, Karpman D, Lebranchu Y, Mariat C, Menne J, Moulin B, Nürnberger J, Ogawa M, Remuzzi G, Richard T, Sberro-Soussan R, Severino B, Sheerin NS, Trivelli A, Zimmerhackl LB, Goodship T, Loirat C (2013) Terminal complement inhibitor eculizumab in atypical hemolytic-uremic syndrome. N Engl J Med 368:2169–2181
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baskin, E., Gulleroglu, K., Kantar, A. et al. Success of eculizumab in the treatment of atypical hemolytic uremic syndrome. Pediatr Nephrol 30, 783–789 (2015). https://doi.org/10.1007/s00467-014-3003-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-014-3003-4