Abstract
Background
Low-pressure pneumoperitoneum (LPP) is an attempt at improving laparoscopic surgery. However, it has the issue of poor working space for which deep neuromuscular blockade (NMB) may be a solution. There is a lack of literature comparing LPP with deep NMB to standard pressure pneumoperitoneum (SPP) with moderate NMB.
Methodology
This was a single institutional prospective non-inferiority RCT, with permuted block randomization of subjects into group A and B [Group A: LPP; 8–10 mmHg with deep NMB [ Train of Four count (TOF): 0, Post Tetanic Count (PTC): 1–2] and Group B: SPP; 12–14 mmHg with moderate NMB]. The level of NMB was monitored with neuromuscular monitor with TOF count and PTC. Cisatracurium infusion was used for continuous deep NMB in group A. Primary outcome measures were the surgeon satisfaction score and the time for completion of the procedure. Secondarily important clinical outcomes were also reported.
Results
Of the 222 patients screened, 181 participants were enrolled [F: 138 (76.2%); M: 43 (23.8%); Group A n = 90, Group B n = 91]. Statistically similar surgeon satisfaction scores (26.1 ± 3.7 vs 26.4 ± 3.4; p = 0.52) and time for completion (55.2 ± 23.4 vs 52.5 ± 24.9 min; p = 0.46) were noted respectively in groups A and B. On both intention-to-treat and per-protocol analysis it was found that group A was non-inferior to group B in terms of total surgeon satisfaction score, however, non-inferiority was not proven for time for completion of surgery. Mean pain scores and incidence of shoulder pain were statistically similar up-to 7 days of follow-up in both groups. 4 (4.4%) patients in group B and 2 (2.2%) in group A had bradycardia (p = 0.4). Four (4.4%) cases of group A were converted to group B. One case of group B converted to open surgery. Bile spills and gallbladder perforations were comparable.
Conclusion
LPP with deep NMB is non-inferior to SPP with moderate NMB in terms of surgeon satisfaction score but not in terms of time required to complete the procedure. Clinical outcomes and safety profile are similar in both groups. However, it could be marginally costlier to use LPP with deep NMB.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Since the first laparoscopic cholecystectomy in 1987 laparoscopic surgery has come a long way and is now considered gold standard for various abdominal conditions including gallstone disease [1]. Cholecystectomy is one of the most commonly performed abdominal operation. The prevalence of gallstone disease is reported to be around 10% in the western literature while it tends to be lower at or below 5% in the Asian population [2,3,4,5,6,7]. However, in the affluent cohort there seems to be an increased tendency for gallstone disease. Cholecystectomy is the gold standard in treatment of gallstone disease [8]. The reasons being its minimal invasive nature, fast recovery, lesser hospital stay, safety and cosmesis. In recent times efforts have been made to make the procedure even more comfortable and safe. The use of low-pressure pneumoperitoneum (LPP) is one such attempt.
Traditionally, an intra-abdominal pressure of 12–15 mmHg is considered satisfactory for visualization and manipulation of instruments in laparoscopic surgery. However, this “standard pressure” causes several physiological disturbances such as decreased cardiac return, increased ventilatory pressures, acid base disturbances, decreased GFR, increased postoperative pain and discomfort. LPP has been defined between 6 and 10 mmHg [9,10,11]. Studies have demonstrated that LPP is favorable for the patient in terms of the above impacts [11]. However, there is the issue of unfavorable working space for the surgeon with low-pressure pneumoperitoneum. Hence, there is evolving interest in the use of deep muscular relaxation along with LPP to increase working space. Favorable ergonomic environment was demonstrated in few studies at a low pressure of 8 mmHg when deep neuromuscular blockade (NMB) was used [12].
However, there have been few direct studies that compare LPP with deep NMB to standard-pressure pneumoperitoneum (SPP) with moderate NMB and the evidence is conflicting [13].
In the reversal of deep NMB, sugammadex is an effective option but comes with a high cost. Reversal of deep NMB by neostigmine may have residual NMB which can delay post-operative recovery, but there is a scarcity of evidence in this aspect.
Therefore, the purpose of this study is to conduct a non-inferiority randomized controlled trial that compares laparoscopic cholecystectomy using LPP with deep NMB to that using SPP with moderate NMB. The primary endpoints were ease of operation scored according to predefined surgical rating scale (surgeon satisfaction score) and the time taken for completion of procedure. The secondary endpoints were the pain score at 1 h, 6 h, 24 h and 7 days after operation, conversion rates from low pressure to standard pressure, incidence of complications, time for extubation and length of hospital stay.
Materials and methods
The single institutional prospective non inferiority randomised control trial was conducted in a tertiary care referral institute from June 2021 to May 2023. Ethical approval was obtained from the Institute Ethics Committee (IECPG-331/28.05.2021, RT-07/23.06.2021 and the trial was registered with CTRI, reg no: CTRI/2021/08/035975. This paper was written according to the CONSORT 2010 Statement guideline for reporting randomized clinical trials [14].
Participants: All patients aged between 18 and 65 years who underwent laparoscopic cholecystectomy for symptomatic gallstone disease in the unit, with BMI ≤ 35 and able to give informed written consent were included in the study. These included patients of any ASA grade fit for general anaesthesia as decided by the anaesthetist. Patients younger or older than the defined age limits, BMI higher than 35, those unfit for general anaesthesia, pregnant patients and those unable to give consent were excluded.
Permuted block randomisation with blocks of 8 was followed and the participants were randomised to group A or group B. The sequence was kept in sealed envelopes which was opened prior to every case.
Calculation of sample size: In view of the two primary outcomes measures, sample size calculation was done using means and SD of both the measures and the higher of the sample size was considered. For the surgical rating score at 5% level of significance, 80% power and a non-inferiority margin of 10% we calculated the sample size with average surgical rating score for group B being 27 and the same being 26 for group A and respective standard deviations being 2.7 and 2.3. A sample size of 97 is required for each group accordingly. Considering an exclusion rate of 10%, a sample size of 107 is considered for each group, 214 in total. For operating time at 5% level of significance, 80% power and a non-inferiority margin of 10% we calculated the sample size with average operating time for group B being 51.9 and the same being 55.7 for group A and respective standard deviations being 8.3 and 8.6. A sample size of 66 is required for each group accordingly. Considering an exclusion rate of 10%, a sample size of 73 is considered for each group. The larger sample size calculated was 107 for each group and since block randomisation with blocks of 8 will be considered the nearest approximation would be 112 in each group.
Procedure and intervention
All patients were worked up in the preoperative period according to institutional protocol. All of them underwent standard laparoscopic cholecystectomy.
According to the randomisation sequence, the patients were allotted group A or group B. Group A patients were operated under low-pressure CO2 pneumoperitoneum of 8–10 mm Hg with Deep NMB defined at a Train of Four count (TOF) of 0 and Post Tetanic Count (PTC) of 1 ≤ 2 and Group B were operated under standard pressure CO2 pneumoperitoneum of 12–14 mm Hg with Moderate NMB.
One dose of injection cefuroxime 1 g was given intravenously at the time of induction. All patients were operated under general anaesthesia with endotracheal intubation. Anaesthesia was induced with propofol and fentanyl and maintained with isoflurane in oxygen and air or nitrous oxide. Mechanical ventilation parameters were adjusted to maintain end-tidal carbon dioxide partial pressure between 35 and 40 mm of Hg. At the end of surgery, anaesthesia was reversed using standard drugs and endotracheal tube was removed when respiratory parameters were normal. Neostigmine was used for reversal of muscular blockade.
NMB: Group A was given deep NMB. Deep NMB was defined as 1 ≤ PTC ≤ 2. They required a higher dose of NMB. Neuromuscular monitoring was done to ensure deep blockade throughout the surgery. One side arm and hand were used for monitoring of NMB. NMB was monitored using neuromuscular monitor (Fig. 1). Electrodes were placed over the ulnar nerve proximal to the wrist at a distance of 3–6 cm. Electrical stimulus was applied to the ulnar nerve and contractions of the adductor pollicis muscle were measured through a sensor attached to the tip of the thumb. TOF was monitored every 1 min, and PTC every 3 min. Standard Moderate NMB was given to group B. The initial rate of cisatracurium infusion was 0.1 mg/kg/h. The infusion rate was adjusted in increments of 0.01 mg/kg/h to maintain PTC at 1–2 in the deep NMB group or TOF at 1–2 in the moderate NMB group. Core temperature was controlled at 36–37 °C. The infusion was usually stopped once the gallbladder was almost out of the gallbladder bed to allow for a good reversal. Residual Neuromuscular block was reversed through neostigmine and glycopyrrolate, avoiding need for agents such as suggamadex.
After infiltration of local anesthetic 5 mL 2% lignocaine around the umbilicus, pneumoperitoneum was created by closed technique using a Veress needle (Ethicon Endo-Surgery, LLC, Guaynabo, Puerto Rico, 00969, USA). PneumoSure high-flow insufflator (Styker Endoscopy, 5900 Optical Court, San Jose, CA, 95138, USA) with a filter was used for insufflation. CO2 was introduced at standard room temperature (19–21 °C) with 0% relative humidity. The gas flow rate was initially set at 3 L/min and increased as and when required during the surgery. The pressure was initially set at 8 mm Hg for group A and 12 mmHg for group B. A standard 4 port laparoscopic cholecystectomy was performed in all the patients. In case the surgeon felt that the working space was inadequate then in group A the pressure was increased up to 10 mmHg and any further increase in pressure beyond 10 mmHg was considered conversion to group B. In group B the pressure was set at 12 mmHg initially and if needed increased up to 14 mmHg.
The patient and the clinician assessing pain scores in the postoperative period were blinded.
The difficulty level of the operation was graded according to the Nassar scale [15, 16]. Due permission was been obtained from the author for using the same (Online Appendix). The ease in performing the operation was scored using a predefined surgical rating scale which measures surgeon satisfaction pertaining to pneumoperitoneum, in various stages of performing laparoscopic cholecystectomy, on a Likert scale of 1–5 (Fig. 2). This scale was previously used in a study from our institute. Time for completion of procedure was defined as time from successful insertion of veress needle to the desufflation and removal of all ports. Time for extubation was defined as time from closure of skin incision to removal of endotracheal tube.
Pain assessment: Pain was assessed by numeric rating scale at 1 h, 6 h, 24 h and 7 days. Incidence of shoulder pain was also recorded at 1 h, 6 h, 24 h and 7 days. Analgesia was standardized as IV paracetamol 1 g TDS. Rescue analgesia was given as bolus doses of fentanyl as and when required. Total consumption of fentanyl was recorded and compared.
Complication: Any complication like bile duct injury/bile leak, injury to adjacent organ, bleeding, surgical site infection, pulmonary complications were recorded.
Statistics: Raw data was maintained and tabulated in Microsoft excel spreadsheet. Intention to treat analysis was done primarily and per protocol analysis also reported. One sided non inferiority analysis was done for the score and time for completion of surgery. All statistical analysis was carried out using statistical software STAT16.0 12.1 (StataCorp LP, Texas, USA) by the dept of statistics in the institute. Descriptive statistics of the baseline characteristics is presented as frequency and percentage distribution for categorical variables, as mean ± SD for normally distributed continuous variables and as median ± IQR for non-normally distributed continuous variables. Quantitative data was analyzed by application of independent t-test/Mann–Whitney test. The qualitative data was analyzed by Chi-squared test/Fisher’s exact test. A p value < 0.05 was considered significant. Other appropriate tests were used as required.
Results
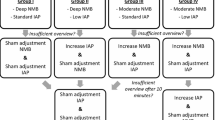
A total of 222 patients underwent laparoscopic cholecystectomy in the unit during the study period (June 2021 to May 2023) of which 41 were excluded as they did not meet inclusion criteria, were asymptomatic patients, indication other than symptomatic gallstone disease or patient did not agree to participate. A final of 181 subjects were randomized, 90 to group A and 91 to group B. Majority were women [F: 138 (76.2%); M: 43 (23.8%)]. There were significantly higher numbers of women in both groups. The demographic profile was statistically similar in both the groups as shown in Table 1. All patients in both the groups were symptomatic for gallstone disease. Imaging of all patients showed cholelithiasis. Of the 181 participants 111 (61.3%) were Nassar grade I, 47 (25.9%) Nassar grade II, 18 (9.9%) Nassar grade III and 5 (2.7%) Nassar Grade IV based on the intra operative difficulty rating scale. The flowchart of the study is shown in Fig. 3.
On intention to treat analysis the total surgeon satisfaction score (Table 2) was not statistically different among group A and B. The time required to complete the procedure was slightly higher in group A compared to group B; however, the difference was not statistically significant. On per protocol analysis also total surgeon satisfaction score and time for completion of surgery were not statistically different. We conducted a one-sided non-inferiority analysis with a predefined non-inferiority margin of 10% for the difference between the means. As shown in the Fig. 4 for both ITT and PP analysis Non inferiority was proven in terms of total surgeon satisfaction score as the mean and confidence interval of difference between means was greater than the set lower limit of non-inferiority margin (Lower Equivalence limit: − 2.6). However, in case of the time for completion of the procedure non-inferiority could not be proven as the confidence interval of the difference of means between group A and B crossed the upper limit of non-inferiority margin (Upper Equivalence Limit = 5.3).
The result remained the same even when we analyzed only Nassar grade 1 and 2 patients and also even after eliminating patients with prior abdominal surgery or BMI above 25. However, when we eliminated the subjects with a time for completion of surgical procedure ≥ 100 min, non-inferiority was upheld for time for completion of surgery. The subjects eliminated were 10 in number, 8 of them had BMI above 25, 2 patients each were Nassar grade 2, 3 and 4 and rest 4 were grade 1. 8 were group A and 2 group B. This may indicate that a greater number of patients had a prolonged surgery ≥ 100 min in group A that led to a wider confidence interval hence leading to disproving of non-inferiority. When non inferiority was analyzed for entry into peritoneal cavity separately it was found Group A was inferior to group B (Fig. S1 supplementary).
Postoperative pain and hospital stay
No significant difference was found in pain scores between the two groups at 1 h, 6 h, 24 h and 7 days of follow up (Table 3). Five (5.5%) patients in Group A and 4 (4.4%) patients in group B needed additional analgesia for pain which was provided in the form of bolus fentanyl doses on SOS basis in the postoperative period, this was statistically comparable among both groups (p = 0.72). Among these 9 patients who required additional analgesia the mean fentanyl consumption by group was 35.0 ± 25.4 for group A and 51.3 ± 15.5 for group B; p = 0.30. In terms of pain and additional requirement of analgesia Group A and Group B were comparable. Incidence of shoulder pain was higher in group B up to 24 h; however, it was not significant statistically (Table 4). Mean hospital stay also was comparable between the groups A and B (2.1 ± 0.4 and 2.1 ± 0.3 days; p = 0.4). There was no significant difference in pain scores at all follow-ups whether a drain was placed or not, though numerically, it was slightly less in patients with no drain.
Need for increase in pressure/Conversion from group A to B (low pressure to standard pressure) (Fig. 5).
Group A had 56.6% cases (51 of 90) needing increase in pressure from 8 to 10 mmHg which was significantly higher (Fisher’s exact test; p < 0.000) compared with group B which had 31.9% (29 of 91) needing increase in pressure from 12 to 14 mmHg.
4 (4.4%) patients of group A (n = 90) were converted to group B; this was, however, not statistically significant (p = 0.07). The reason for conversion in these cases were mainly inadequate space, in 2 of the cases the omentum was bulky and was encroaching the Calots triangle and blocking the view. Even after conversion to group B (with increase in pressure to 14 mmHg) the situation improved only marginally according to the surgeons. In one case the entry was very difficult as the abdomen was lax and this improved after increasing the pressure to 14 mmHg. In another case the overall working space was less and hence the surgeon decided to increase the pressure.
One patient of group B was converted to open surgery in view of difficult Calots dissection and a subtotal cholecystectomy was performed with suturing of the stump with Vicryl 2-0. The surgeon admitted that it was due to the difficult Calots dissection.
There were no mortalities, bile duct or visceral injuries in both the groups, incidence of iatrogenic gallbladder perforation and bile spill were comparable in both groups. Drain placement was decided by the surgeon and this was also comparable. One case in each group had bleed from cystic artery due to slippage of clip, both of them were reclipped and controlled on table, there was no incidence of postoperative bleeding or bile leak in any of the patients. At insufflation 4 (4.4%) patients had bradycardia in group A. This was not statistically higher when compared with group B in which 2 (2.2%) patients experienced it, p = 0.4 (Table 5).
Anesthesia related parameters
There was no statistical difference in mean, heart rate, MAP and maximum peak inspiratory pressure (Table 6). The mean time for extubation was slightly longer in group A, however, this was not statistically significant. In the post operative period there were no patients with residual paralysis in both the groups. This was assessed with clinical parameters such as the patient’s inability to smile, swallow and speak; general muscular weakness; inability to lift the head for 5 s, to lift the leg for 5 s and inability to sustain a hand grip for 5 s.
Cost analysis
The mean cisatracurium consumption in group A was 8.2 ± 3.4 mg and in Group B was 7.8 ± 3.2 mg. At 50₹ (0.6USD) per mg the cost amounted to 411.5 ± 170₹ (4.9 ± 2.1USD) per patient in group A and 390.5 ± 160₹ (4.7 ± 1.9USD) in group B. CO2 consumption was higher in group A (Group A = 112.9 ± 129.4 L vs Group B = 94.08 ± 62.84 L). At 49₹ (0.6USD) per L of CO2 the cost per patient in group A was 5532.1 ± 6343.1₹ (66.9 ± 76.8USD) and for group B it was 4609.9 ± 3079.2₹ (55.8 ± 37.3USD).
*₹- INR, 1₹ = 0.012USD = 0.11 EU49.
Higher BMI correlated with a lower surgeon satisfaction score irrespective of groups [Group A (r = − 0.22), Group B (r = − 0.3)]. The correlation was not significantly different between the groups (p = 0.34). It was found that the mean total surgeon satisfaction score was significantly lower in the subgroup with BMIs > 25 compared with those with BMIs < 25 (25 ± 3.4 vs 27.2 ± 3.3; p < 0.000). BMI was an important predictor of the total surgeon satisfaction score as determined by logistic regression. This can indicate that BMI of the patient independently influences the space during pneumoperitoneum, this may be due to the weight of the abdominal wall itself.
Surgeon satisfaction score sub analysis revealed that the score for entry into peritoneal cavity was significantly lower in Group A compared to Group B (ITT: 4.0 ± 0.8 vs. 4.4 ± 0.7, p = 0.002; PPA: 4.1 ± 0.8 vs 4.4 ± 0.7; p = 0.005). Rest of the scores were comparable statistically (Table 2). Of the total 181 cases there were 142 (78.5%) consultant cases and 39 (21.5%) trainee cases. Group A had 66 (73.3%) consultant and 24 (26.6%) trainee cases while group B had 76 (83.5%) consultant and 15 (16.4%) trainee cases. When the surgeon satisfaction scores were analyzed between consultants and trainees the total surgeon satisfaction score and time for completion of surgery were comparable among group A and B (Table S1 supplementary). It was found that numerically the scores were lower for group A among both consultants and trainee for entry in to the peritoneal cavity in both group A and group B.
Total surgeon satisfaction scores and time for completion were comparable among the 4 Nassar grades among both the groups. However, score for entry into the peritoneal cavity was significantly lower in Group A compared to Group B in both Nassar grade 1 (3.9 ± 0.7 vs 4.4 ± 0.7; p = 0.005) and Nassar Grade 2 (4.1 ± 0.8 vs 4.5 ± 0.6; p = 0.04). There was weak negative correlation of initial volume of CO2 required to achieve set pressure and the total surgeon satisfaction score (r = − 0.18, p = 0.02). This suggested that lesser the distension lesser was the working space. Overall, there was no significant variations in pulse rate, blood pressure and saturation.
Discussion
In the present study we found that LPP with deep NMB was non inferior to SPP with moderate NMB in terms of working space determined by total surgeon satisfaction score which was a subjective assessment of the working space. However, in terms of time for completion of surgery which is an objective measure the study did not prove non-inferiority. Hence when it comes to time for completion of surgery Group A is inferior to Group B.
We did not find any clinical differences in terms of post operative pain, incidence of shoulder pain or hospital stay. In terms of anesthesia, there was no significant residual paralysis post deep NMB with neostigmine reversal. On sub analysis of the surgeon satisfaction scores it was noted that entry into peritoneal cavity was significantly difficult in group A.
Our study is a clinically important comparison. Only one previous study by Barrio et al. [13] did such a comparison. They compared patients undergoing laparoscopic cholecystectomy under LPP with deep NMB with SPP. They found significantly better working conditions in standard pressure group, in contrast to our study, where working conditions were similar in both groups. There was no significant difference in the time for completion of procedure in their study while our study showed that LPP with deep NMB was inferior in terms of operating time. They, however had a small sample size of 30 in each group and 3 surgeons who were well experienced operated on patients. In our study multiple surgeons including experienced consultants and trainees operated on the patients and our sample size was also larger which could be the reason for a different result.
Studies have proven that working conditions are significantly poorer in LPP when done without deep NMB. Neogi et al. demonstrated that the scores for entry, visibility, port manipulation and dissection were significantly lower in the low-pressure group than the standard pressure group [17].
Our research pointed that BMI was an independent and significant influence on the working space. This may signify that the sheer weight of abdominal wall may also influence the working space especially in an Indian population where central obesity is more common [18]. In the obese patient the pressures are usually kept higher up to 18 mmHg for achieving good working space. Various studies have shown that deep NMB helped improving working space in obese individual [19,20,21]. Rye et al. compared deep versus moderate NMB in LPP in laparoscopic cholecystectomy and found marginally better surgical conditions with deep NMB [22]. Various studies have studied deep NMB in LPP in different laparoscopic surgeries including cholecystectomy, donor nephrectomy, colorectal surgery and metabolic surgery found that it improves surgical working conditions significantly [23,24,25,26,27].
In terms of postoperative pain studies have demonstrated LPP has better pain score and lower incidence of shoulder pain than SPP in laparoscopic cholecystectomy [28] and it has been demonstrated use of deep NMB further reduces postoperative pain and incidence of shoulder pain. In our study however, we did not find any clinically significant difference in pain outcomes in terms of postoperative pain scores or incidence of shoulder pain. We had blinded the assessors for pain and the patients were also blinded for group to avoid bias but since 56% group A patients had required increase in pressure from 8 to 10 mmHg the pressure difference between group A and B might have been small to bring about significant difference in pain. Similar to our findings in the randomized trial by Sandhu et al. [29], where they compared LPP with SPP they did not find any statistically significant difference in pain scores or incidence of shoulder pain. This was also supported by the meta-analysis [30] by Wei et al., the NISCO trial [25, 31].
The conversion to group B was lesser in our study compared with the study by Neogi et al. who did not use deep NMB, indicating that the deep NMB may have actually helped increase working space [17]. Conversion to open surgery was similar to their study and it was mainly due to surgical difficulty rather than lack of space.
The Cochrane review by Gurusamy et al. [32] demonstrated no mortality, adverse event or difference in conversion rates between low and standard pressure groups, similar to the present study. There was also no significant difference in hospital stay similar to our report. 4.4% of our patients in group A were converted to standard pressure group. Perrakis et al. [31] reported 5% conversion to higher pressure while on the contrary Joshipura et al. [33] reported 33% conversion to higher pressure, they both did not use deep NMB. This indicates starting with a lower pressure and increasing the pressure as required could allow many patients to be operated easily at a lower pressure than routine.
Previous studies have demonstrated other benefits of LPP in terms of better portal venous blood flow avoiding portal ischemia that leads to significantly raised transaminases in 14 mmHg pneumoperitoneum compared with 10 mmHg group in laparoscopic cholecystectomy [9]. However, the clinical significance beyond the immediate postoperative period and in those with essentially normal liver function is to be studied since the raised values were also not abnormal. This however could not be assessed in the present study.
It has been proven by various studies that low pressure has lesser postoperative pain and faster recovery and lesser inflammation but with reduced working space, likely because the peritoneum is stretched less. So, when deep NMB is used the working space may be good as shown by various studies including ours but theoretically this may stretch the peritoneum more [34] hence cancelling the benefits of post operative pain reduction.
Strengths and weakness
In terms of sample size our study was well powered for time for completion of surgery but may not be so for total surgeon satisfaction score as per sample size calculation. The surgeon satisfaction score is a subjective assessment of the working space, objective measures may be considered in future studies. Only 2 patients were ASA grade 3 or 4 so further studies will be required to demonstrate the effects on those individuals. Our study may not be powered enough to comment on the other clinical outcomes like post-operative pain and hospital stay, larger studies will be required for that purpose. In addition, we did not study regarding the hemodynamic aspects and the benefits that may be associated with a lower pressure in that regard. Future studies can incorporate this aspect. It might be prudent to conduct similar studies on potentially more prolonged pelvic and gastrointestinal procedures to determine if there might be any benefit.
Recommendations
In short laparoscopic procedures such as laparoscopic cholecystectomy LPP with deep NMB can be used safely but the procedure may be slightly prolonged. The clinical benefits need to be studied further. Future studies can specifically be designed to evaluate the hemodynamic parameters especially in higher ASA grades.
There is substantial inconsistency across the literature in reporting the working conditions in laparoscopic surgery [35]. The surgeon satisfaction scores reported are usually subjective and difficult to compare across studies. A standardization of reporting may be considered in future studies. The scoring used here was part of previous study from our institute and was standardized for laparoscopic cholecystectomy [28].
Considering our findings, we can suggest that a pressure of 10 mmHg with deep NMB may be considered ideal to start with, balancing surgical comfort and its impact on the patient. The pressure can be increased as and when needed, and we believe that a majority of the cases can be completed within a pressure range of 10–12 mmHg.
Conclusion
LPP with Deep NMB is non-inferior to SPP with moderate NMB in terms of surgeons’ satisfaction of working space but not in terms of time for completion of surgery for laparoscopic cholecystectomy.
LPP with Deep NMB can be used safely in laparoscopic cholecystectomy in all ASA grade patients. Clinical relevance in terms of pain outcomes and hemodynamic outcomes needs to be studied further with large sample size.
References
Basunbul LI, Alhazmi LSS, Almughamisi SA, Aljuaid NM, Rizk H, Moshref R (2022) Recent technical developments in the field of laparoscopic surgery: a literature review. Cureus 14:e22246. https://doi.org/10.7759/cureus.22246
Shabanzadeh DM (2018) Incidence of gallstone disease and complications. Curr Opin Gastroenterol 34:81–89. https://doi.org/10.1097/MOG.0000000000000418
Shaffer EA (2006) Epidemiology of gallbladder stone disease. Best Pract Res Clin Gastroenterol 20:981–996. https://doi.org/10.1016/j.bpg.2006.05.004
Barbara L, Sama C, Morselli Labate AM, Taroni F, Rusticali AG, Festi D, Sapio C, Roda E, Banterle C, Puci A (1987) A population study on the prevalence of gallstone disease: the Sirmione Study. Hepatol Baltim Md 7:913–917. https://doi.org/10.1002/hep.1840070520
Kratzer W, Mason RA, Kächele V (1999) Prevalence of gallstones in sonographic surveys worldwide. J Clin Ultrasound 27:1–7. https://doi.org/10.1002/(sici)1097-0096(199901)27:1%3c1::aid-jcu1%3e3.0.co;2-h
Saha M, Nahar K, Hosen MA, Khan M, Kumar Saha S, Chandra Shil B, Habibur Rahman M (2015) Prevalence and risk factors of asymptomatic gallstonedisease in north-east part of Bangladesh. Euroasian J Hepato-Gastroenterol 5:1–3. https://doi.org/10.5005/jp-journals-10018-1118
Moro P, Checkley W, Gilman R, Cabrera L, Lescano A, Bonilla J, Silva B (2000) Gallstone disease in Peruvian coastal natives and highland migrants. Gut 46:569–573. https://doi.org/10.1136/gut.46.4.569
McSherry CK (1989) Cholecystectomy: the gold standard. Am J Surg 158:174–178. https://doi.org/10.1016/0002-9610(89)90246-8
Eryılmaz HB, Memiş D, Sezer A, Inal MT (2012) The effects of different insufflation pressures on liver functions assessed with LiMON on patients undergoing laparoscopic cholecystectomy. Sci World J 2012:172575. https://doi.org/10.1100/2012/172575
Schietroma M, Carlei F, Mownah A, Franchi L, Mazzotta C, Sozio A, Amicucci G (2004) Changes in the blood coagulation, fibrinolysis, and cytokine profile during laparoscopic and open cholecystectomy. Surg Endosc 18:1090–1096. https://doi.org/10.1007/s00464-003-8819-0
Ibraheim OA, Samarkandi AH, Alshehry H, Faden A, Farouk EO (2006) Lactate and acid base changes during laparoscopic cholecystectomy. Middle East J Anaesthesiol 18:757–768
Staehr-Rye AK, Rasmussen LS, Rosenberg J, Juul P, Gätke MR (2013) Optimized surgical space during low-pressure laparoscopy with deep neuromuscular blockade. Dan Med J 60:A4579
Barrio J, Errando CL, García-Ramón J, Sellés R, San Miguel G, Gallego J (2017) Influence of depth of neuromuscular blockade on surgical conditions during low-pressure pneumoperitoneum laparoscopic cholecystectomy: a randomized blinded study. J Clin Anesth 42:26–30. https://doi.org/10.1016/j.jclinane.2017.08.005
Schulz KF, Altman DG, Moher D, CONSORT Group (2010) CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ 340:c332. https://doi.org/10.1136/bmj.c332
Griffiths EA, Hodson J, Vohra RS, Marriott P, CholeS Study Group, Katbeh T, Zino S, Nassar AHM, West Midlands Research Collaborative (2019) Utilisation of an operative difficulty grading scale for laparoscopic cholecystectomy. Surg Endosc 33:110–121. https://doi.org/10.1007/s00464-018-6281-2
Nassar AHM, Hodson J, Ng HJ, Vohra RS, Katbeh T, Zino S, Griffiths EA, CholeS Study Group, West Midlands Research Collaborative (2020) Predicting the difficult laparoscopic cholecystectomy: development and validation of a pre-operative risk score using an objective operative difficulty grading system. Surg Endosc 34:4549–4561. https://doi.org/10.1007/s00464-019-07244-5
Neogi P, Kumar P, Kumar S (2020) Low-pressure pneumoperitoneum in laparoscopic cholecystectomy: a randomized controlled trial. Surg Laparosc Endosc Percutaneous Tech 30:30–34. https://doi.org/10.1097/SLE.0000000000000719
Pradeepa R, Anjana RM, Joshi SR, Bhansali A, Deepa M, Joshi PP, Dhandania VK, Madhu SV, Rao PV, Geetha L, Subashini R, Unnikrishnan R, Shukla DK, Kaur T, Mohan V, Das AK (2015) Prevalence of generalized & abdominal obesity in urban & rural India—the ICMR - INDIAB Study (Phase-I) [ICMR - INDIAB-3]. Indian J Med Res 142:139–150. https://doi.org/10.4103/0971-5916.164234
Torensma B, Martini CH, Boon M, Olofsen E, In ‘t Veld B, Liem RSL, Knook MTT, Swank DJ, Dahan A (2016) Deep neuromuscular block improves surgical conditions during bariatric surgery and reduces postoperative pain: a randomized double blind controlled trial. PLoS ONE 11:e0167907. https://doi.org/10.1371/journal.pone.0167907
Fuchs-Buder T, Schmartz D, Baumann C, Hilt L, Nomine-Criqui C, Meistelman C, Brunaud L (2019) Deep neuromuscular blockade improves surgical conditions during gastric bypass surgery for morbid obesity: a randomised controlled trial. Eur J Anaesthesiol 36:486–493. https://doi.org/10.1097/EJA.0000000000000996
Aceto P, Perilli V, Modesti C, Sacco T, De Cicco R, Ceaichisciuc I, Sollazzi L (2020) Effects of deep neuromuscular block on surgical workspace conditions in laparoscopic bariatric surgery: a systematic review and meta-analysis of randomized controlled trials. Minerva Anestesiol 86:957–964. https://doi.org/10.23736/S0375-9393.20.14283-4
Staehr-Rye AK, Rasmussen LS, Rosenberg J, Juul P, Lindekaer AL, Riber C, Gätke MR (2014) Surgical space conditions during low-pressure laparoscopic cholecystectomy with deep versus moderate neuromuscular blockade: a randomized clinical study. Anesth Analg 119:1084–1092. https://doi.org/10.1213/ANE.0000000000000316
Kim JE, Min SK, Ha E, Lee D, Kim JY, Kwak HJ (2021) Effects of deep neuromuscular block with low-pressure pneumoperitoneum on respiratory mechanics and biotrauma in a steep Trendelenburg position. Sci Rep 11:1935. https://doi.org/10.1038/s41598-021-81582-0
Koo B-W, Oh A-Y, Seo K-S, Han J-W, Han H-S, Yoon Y-S (2016) Randomized clinical trial of moderate versus deep neuromuscular block for low-pressure pneumoperitoneum during laparoscopic cholecystectomy. World J Surg 40:2898–2903. https://doi.org/10.1007/s00268-016-3633-8
Blobner M, Frick CG, Stäuble RB, Feussner H, Schaller SJ, Unterbuchner C, Lingg C, Geisler M, Fink H (2015) Neuromuscular blockade improves surgical conditions (NISCO). Surg Endosc 29:627–636. https://doi.org/10.1007/s00464-014-3711-7
Madsen MV, Staehr-Rye AK, Claudius C, Gätke MR (2016) Is deep neuromuscular blockade beneficial in laparoscopic surgery? Yes, probably. Acta Anaesthesiol Scand 60:710–716. https://doi.org/10.1111/aas.12698
Yoo Y-C, Kim NY, Shin S, Choi YD, Hong JH, Kim CY, Park H, Bai S-J (2015) The intraocular pressure under deep versus moderate neuromuscular blockade during low-pressure robot assisted laparoscopic radical prostatectomy in a randomized trial. PLoS ONE. https://doi.org/10.1371/journal.pone.0135412
Bhattacharjee HK, Jalaludeen A, Bansal V, Krishna A, Kumar S, Subramanium R, Ramachandran R, Misra M (2017) Impact of standard-pressure and low-pressure pneumoperitoneum on shoulder pain following laparoscopic cholecystectomy: a randomised controlled trial. Surg Endosc 31:1287–1295. https://doi.org/10.1007/s00464-016-5108-2
Sandhu T, Yamada S, Ariyakachon V, Chakrabandhu T, Chongruksut W, Ko-iam W (2009) Low-pressure pneumoperitoneum versus standard pneumoperitoneum in laparoscopic cholecystectomy, a prospective randomized clinical trial. Surg Endosc 23:1044–1047. https://doi.org/10.1007/s00464-008-0119-2
Wei Y, Li J, Sun F, Zhang D, Li M, Zuo Y (2020) Low intra-abdominal pressure and deep neuromuscular blockade laparoscopic surgery and surgical space conditions: a meta-analysis. Medicine (Baltimore) 99:e19323. https://doi.org/10.1097/MD.0000000000019323
Perrakis E, Vezakis A, Velimezis G, Savanis G, Deverakis S, Antoniades J, Sagkana E (2003) Randomized comparison between different insufflation pressures for laparoscopic cholecystectomy. Surg Laparosc Endosc Percutaneous Tech 13:245–249. https://doi.org/10.1097/00129689-200308000-00004
Gurusamy KS, Vaughan J, Davidson BR (2014) Low-pressure versus standard pressure pneumoperitoneum in laparoscopic cholecystectomy. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD006930.pub3
Joshipura VP, Haribhakti SP, Patel NR, Naik RP, Soni HN, Patel B, Bhavsar MS, Narwaria MB, Thakker R (2009) A prospective randomized, controlled study comparing low pressure versus high pressure pneumoperitoneum during laparoscopic cholecystectomy. Surg Laparosc Endosc Percutaneous Tech 19:234–240. https://doi.org/10.1097/SLE.0b013e3181a97012
Danneels I, Mulier JP, Dillemans B, Vandebussche D (2006) Effect of muscle relaxants on the abdominal pressure-volume relation: A-126. Eur J Anaesthesiol 23:32
Boon M, Martini CH, Aarts LPHJ, Dahan A (2019) The use of surgical rating scales for the evaluation of surgical working conditions during laparoscopic surgery: a scoping review. Surg Endosc 33:19–25. https://doi.org/10.1007/s00464-018-6424-5
Acknowledgements
We acknowledge all the surgeons under the Dept of Surgical Disciplines who contributed cases to this study, the anaesthesiologists for giving the deep neuromuscular block according to protocol and being the backbone in this study, the staff including technicians who helped in the neuromuscular monitoring and adjustment of pressure during the surgery and all the residents of the department who were part of the team.
Funding
No research funding received for the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Prasanna Ramana Arumugaswamy, Sunil Chumber, Yashwant Singh Rathore, Souvik Maitra, Hemanga Kumar Bhattacharjee, Virinder Kumar Bansal, Sandeep Aggarwal, Anita Dhar, Krishna Asuri, Kamal Kataria, and Piyush Ranjan have no conflicts of interest or financial ties to disclose.
Ethical approval
A formal ethical approval was obtained before the start of the study (IECPG- 331/28.05.2021, RT-07/23.06.2021).
Trial registration
The trial was registered with CTRI, reg no: CTRI/2021/08/035975 before the start of the study.
Informed consent
An informed consent was taken from each participant.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presentation in conferences: It was presented in the KARL STORZ - EAES Award session during the 31st International EAES Congress, 20–23 June 2023 in Roma, Italy and awarded the KARL STORZ AWARD for the best oral paper presentation.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (JPEG 487 kb)
Figure S1 supplementary: Non inferiority analysis on sub groups.
Supplementary file3 (JPEG 641 kb)
Figure S2 supplementary: Intraoperative images.
Supplementary file4 (JPEG 455 kb)
Figure S3 supplementary: Pain scores up to 7 days of follow-up.
Supplementary file5 (DOCX 14 kb)
Table S1 supplementary: Comparing consultants and trainees.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arumugaswamy, P.R., Chumber, S., Rathore, Y.S. et al. Low-pressure pneumoperitoneum with deep neuromuscular blockade versus standard pressure pneumoperitoneum in patients undergoing laparoscopic cholecystectomy for gallstone disease: a non-inferiority randomized control trial. Surg Endosc 38, 449–459 (2024). https://doi.org/10.1007/s00464-023-10558-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10558-0