Abstract
Background
We conducted this study to report our novel robotic thyroidectomy using gas-insufflation one-step single-port transaxillary (GOSTA) approach and compare it with a conventional transaxillary (CTA) approach using a retraction method for intraoperative and postoperative outcomes.
Methods
We retrospectively analyzed 354 patients who underwent robotic thyroidectomy between January 2019 and April 2023. Of these patients, 143 underwent the procedure through the GOSTA approach, which involves a small incision of 3 cm along the axillary folds with both arms down and a gas-insufflation, from skin flap creation to the completion of thyroidectomy as a one-step single-port procedure without the need for a retractor. The remaining 211 patients underwent the CTA approach. We analyzed the GOSTA approach and compared the surgical outcomes of the GOSTA (n = 100) and CTA (n = 167) approaches in patients with differentiated thyroid cancer who underwent thyroid lobectomy.
Results
Out of the 143 patients who underwent the GOSTA approach, 12 underwent total thyroidectomy and 9 underwent lateral neck lymph node dissection with total thyroidectomy. GOSTA-thyroid lobectomy was performed on 122 patients; of these, 100 were diagnosed with differentiated thyroid carcinoma. A comparative study with the CTA approach was only conducted in patients who underwent thyroid lobectomy. No significant differences were found in operative time, hospital stay, or complications between the two groups.
Conclusions
Despite proceeding in one-step with a single smaller incision, from skin flap creation to the completion of thyroidectomy, the GOSTA approach is as feasible and safe as the CTA approach. Additionally, the GOSTA approach allows for thyroidectomy without using a retractor and reduces the workload for the surgeon and assistants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Traditionally, thyroidectomy was performed as an open surgery without hesitation for many years. However, the operation scar on the neck cannot be ignored, and the need for cosmetic surgery has increased with the advancement of surgical instruments. To conceal the scar, surgeons have started inventing many ways to access the thyroid gland through alternate sites other than the cervical incision [1, 2]. There are now various remote approaches for thyroidectomy; transaxillary approach [3,4,5], transoral approach [6,7,8,9,10,11], retroauricular approach [12,13,14] and bilateral axillo-breast approach [15,16,17,18]. Initially, endoscopic surgery made them possible [19,20,21,22], and the advent of robotic surgery made these procedures even more feasible [23,24,25,26,27].
In 2016, our institution began performing thyroidectomies using the da Vinci S surgical robot through a trans-axillary approach [28]. Since then, the procedures have evolved with the introduction of the da Vinci Xi and SP models [29]. To overcome the limitations of the conventional approach, a novel strategy that involves a change in position was developed. This change, along with the introduction of da Vinci SP technology, has enabled us to modify and improve our surgical procedures into a one-step process. We have named this new surgical approach "gas-insufflation one-step single-port transaxillary (GOSTA) approach ".
In this study, we introduced this novel approach and compared the pre-existing conventional transaxillary (CTA) approach with this GOSTA approach.
Methods
Patients
A total of 354 patients underwent robotic-assisted thyroidectomy at the single tertiary institution, Korea University Ansan Hospital, by a single surgeon named YWC. The CTA thyroidectomy was performed on 211 patients from January 2019 to December 2021, whereas the GOSTA was performed on 143 patients from January 2022 to April 2023, consecutively. In the CTA approach group, there was one total thyroidectomy with selective neck dissection (SND), 12 total thyroidectomies alone, and 198 thyroid lobectomy cases. In the GOSTA approach group, there were nine total thyroidectomies with SND, 12 total thyroidectomies alone, and 122 thyroid lobectomy cases. The diagnosis after thyroidectomy includes not only malignant disease such as papillary thyroid carcinoma but also benign disease such as Graves’ disease and thyroid nodules. The detailed distribution of patients’ diagnoses is described in Fig. 1.
This retrospective study was approved by the Institutional Review Board of Korea University Medical Center, Ansan (approval number: 2023AS0124). A waiver of informed consent was requested and approved.
Operative procedure
Position and incision
In the GOSTA approach, the patients were draped in a supine position with both arms down. In the CTA approach, the patients were prepared with the ipsilateral arm fixed in a raised and flexed position using a bar above their head [28, 29].
In both methods, the incision was made along the skin crease at the axillary fold. The GOSTA approach required a 3 cm sized incision, while the CTA approach required a minimum of a 6 cm sized incision. A wound retractor was used for skin protection in both methods. For the CTA thyroidectomy, the wound retractor used was the same one used for open surgery, and Chung's retractor was inserted superiorly to lift the skin flap. In the GOSTA approach, a wound retractor designed for single-port surgery with multiple ports was inserted, and gas-insufflation was performed at 8 mmHg, replacing the need for mechanical retractors (Fig. 2).
Pictures of the patient’s position in the CTA and GOSTA approaches. a patient position with the arm raised for the CTA approach, b patient position with both arms down for the GOSTA approach, c, e axillary incision with a retractor for the CTA approach, d, f axillary incision without a retractor for the GOSTA approach, g manual creation of skin flap with an additional areolar incision for the CTA approach, h skin flap creation using the da Vinci SP surgical system via gas-insufflation for the GOSTA approach. CTA conventional transaxillary, GOSTA gas-insufflation one-step single-port transaxillary
Robot docking
In the GOSTA approach, the robot was docked after creating a flap of one-finger depth for the wound retractor, and the skin flap was created using the robot, making the surgery a one-step process. The SP endoscope was placed in the 12 o'clock direction while using the Maryland bipolar forceps for arm number 1, the monopolar cautery for arm number 2, and the Cadiere forceps for arm number 3, regardless of the surgical side. The remote center of the da Vinci SP trocar was placed externally; only the endoscope and devices were inserted through the axillary incision. Lastly, we used a cut J-P drain tip with continuous suction connected to prevent sight disturbance caused by smoke produced during the surgery.
In the CTA approach, the skin flap was created by the surgeon at the bedside with an assistant lifting the flapped skin and sternocleidomastoid muscle (SCM) using Chung’s retractor step-by-step. The CTA approach usually required an additional peri-areolar port, and the robot was docked after the procedures, from creating the skin flap to lifting the sternothyroid muscle up with the retractor (Fig. 2).
Skin flap creation and thyroidectomy
In the GOSTA approach, the dissection was performed along the anterior surface of the pectoralis major muscle, recognizing and preserving the supraclavicular nerve. The dissection was then continued between the sternal and clavicular heads of the SCM muscle. The omohyoid muscle and the ansa cervicalis nerve can also be detected and preserved. Behind these structures lies the thyroid gland, and anterior wall dissection from strap muscles was continued. The external branch of the superior recurrent laryngeal nerve (EBSLN) was detected and preserved during superior pole dissection. The superior thyroidal artery and vein were firmly coagulated with a monopolar cautery or bipolar forceps. On the lateral side of the thyroid gland, the recurrent laryngeal nerve (RLN) and parathyroid glands (PTGs) were preserved. Central lymph node dissection was performed along the carotid artery sheath, from the lateral side to the sternal notch [30, 31] (Fig. 3). Detailed procedures of GOSTA-thyroid lobectomy can be watched in Video 1.
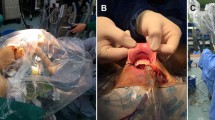
Pictures of the procedures for GOSTA-TL. a preservation of supraclavicular nerves during skin flap creation, b approach between the two heads of the SCM, c Preservation of the omohyoid muscle, d anterior dissection of the thyroid, e upper pole dissection of the thyroid while preserving EBSLN, f lateral dissection of the thyroid while preserving RLN, g dissection of level VI lymph nodes, h post-thyroidectomy. GOSTA-TL gas-insufflation one-step single-port transaxillary approach for thyroid lobectomy, SCM sternocleidomastoid muscle, EBSLN external branch of the superior laryngeal nerve, RLN recurrent laryngeal nerve
Comparison study
Of the patients above, we extracted only those who underwent thyroid lobectomy and were diagnosed with differentiated thyroid carcinoma for the comparison study of both approaches. Data were analyzed using SPSS Statistics (version 25.0.0.0; IBM Corp., Armonk, NY, USA). Continuous variables are presented as means with standard deviations, while categorical variables are presented as percentages. A Student t test was used to compare continuous variables. A Chi-squared or Fisher exact test was used to compare categorical variables. Differences were considered statistically significant at p values < 0.05.
Results
Clinicopathological characteristics
There were a total of 167 patients who underwent the CTA approach and a total of 100 patients who underwent the GOSTA approach. The mean age at the time of the operation in the CTA group and the GOSTA group was 49.3 and 48.5, respectively, with no significant difference. The proportion of female patients and body mass index were also comparable. There were patients who had follicular carcinoma in only the GOSTA approach group. The mean tumor sizes were 1.0 cm and 1.2 cm, respectively (p = 0.055), and the number of harvested and metastatic lymph nodes also had no significant differences. Although the proportion of T1b was slightly higher in the GOSTA group, there was no distinctive difference in the N classification distribution between the two groups (Table 1).
Analysis of perioperative details
There were no significant differences in the total operation time between the CTA group and the GOSTA group, which were 97.1 min and 101.6 min, respectively. The number of sacrificed parathyroid glands (PTG) was 0.34 and 0.22, respectively (p = 0.053). There were seven postoperative complications in the CTA group, four of which were transient RLN palsy and three of which were hematomas that needed surgical evacuation. During surgery, it was revealed that the bleeding focus in all four cases was small subcutaneous vessels near the incision site. In the GOSTA group, only two patients experienced postoperative complications. One patient had transient RLN palsy, and the other patient had a hematoma that also required surgical evacuation. The bleeding focus in the GOSTA group was also identified as small subcutaneous vessels near the incision site. There were no cases of permanent RLN palsy or chylous drainage in either group (Table 2).
Discussion
With advances in robotic surgical systems, recent robotic thyroidectomy has not only reduced scarring of the neck but has also improved visibility and devices, making surgery more precise and stable [32, 33]. Various surgical approaches have been utilized for robotic thyroidectomy, each with advantages and disadvantages [34,35,36,37,38,39]. Our institution has chosen the transaxillary approach as the mainstream method. Many studies have already proven the feasibility, safety, and effectiveness of the transaxillary approach for robotic thyroidectomy [40,41,42,43,44]. However, we have experienced some procedure difficulties with the CTA approach, so we have tried to modify the procedure using the da Vinci SP surgical system.
In the CTA approach, the patient's ipsilateral arm had to be raised during the surgery. This was primarily done to reduce the distance between the incision and operation sites. Since CTA thyroidectomy did not involve gas-insufflation, mechanical retractors had to be used during the surgery to lift the skin. The length of the existing retractors was limiting, so elevating the ipsilateral arm became the solution. However, this position caused the elevation of the major pectoralis muscle, narrowing the operation field and acting as an obstacle. The surgeon had to proceed beyond the elevated muscle during flap creation. The folded skin between the neck and shoulder also posed a hurdle, as it could be easily injured during flap creation and served as an upper limit for the range of movement. Throughout the flap creation process, the retractors must be continuously repositioned step-by-step as the dissection progresses [45]. These demanding and strenuous steps required for flap creation before docking the robot were another limitation of the CTA.
To address these problems, we changed the patient’s position in the GOSTA approach. The patients were prepared in a supine position with both arms in the down position. This position flattened the pectoralis major muscle, but it increased the distance from the thyroid gland to the incision. Therefore, we docked the robot from the beginning to create a skin flap. With the assistance of the da Vinci SP system, we could obtain a clear and stable visual field, preserve the supraclavicular nerve, and have delicate coagulation of subcutaneous vessels during skin flap creation. The approach to SCM and the thyroid could be made easier than the CTA approach by flattening the pectoralis major muscle (Fig. 4a, b). Furthermore, this position made the bilateral approach possible without changing the surgical drape or the elevated arm in the patients who needed total thyroidectomy [46].
Illustrations demonstrating the patient's posture for the CTA approach and GOSTA approach. a elevation of the major pectoralis muscle caused by the raised arm in the CTA approach, b flattening of the pectoralis major muscle in the GOSTA approach, c restriction of instrument movement due to folded skin in the CTA approach, d elimination of folded skin in the GOSTA approach. CTA conventional transaxillary, GOSTA gas-insufflation one-step single-port transaxillary
As the position was changed to a supine position with both arms down, the folded skin between the neck and shoulder caused by the raised arm in the CTA approach disappeared, allowing a widened range of movement for surgical instruments. This made it possible to visualize the upper pole of the thyroid gland more, identifying and preserving the external branch of the superior laryngeal nerve (Fig. 4c, d). Therefore, the surgery was possible with only a single-port in the axilla without an additional peri-areolar port to pull the thyroid caudally in the CTA approach.
We chose the gas-insufflation procedure instead of using a retractor because the surgeon could not manage the retractor directly during skin flap creation with the robot. We needed only a 3 cm axillary incision for this surgery since the robotic thyroidectomy has been performed without a retractor, and it was possible even with a 2.5 cm long axillary incision in the case of patients whose skin stretches well. We used a shortened J-P drain with continuous suction drainage to address the surgical smoke generated during dissection. The surgery with the GOSTA approach could proceed with a one-step procedure until the thyroidectomy was completed because the procedure for re-docking the robot during surgery had been eliminated. An additional advantage of replacing the retractors with gas-insufflation was the elimination of excessive traction on the platysma and SCM muscles.
SND was feasible with the single incision in the GOSTA approach [47,48,49]. There were no posture changes other than turning the head to the contralateral side of the surgery during SND. In most cases, SND was performed after thyroidectomy, and additional space for SND was created using the robot. A total of nine patients underwent SND in the GOSTA group, and their clinical data are described in Table 3. With the GOSTA approach, we could access and identify anatomical structures of level II more effectively than with open surgery due to the low angle of entry of the robot. The clavicle made it challenging to dissect level IV lymph nodes, but we were able to solve it by moving the SP trocar anteriorly and increasing the robot’s angle of entry. Although no analysis of SND was conducted, the number of harvested lymph nodes and total operation time, including the time for total thyroidectomy, were acceptable compared to those of open surgery and other robotic SND [12, 49,50,51,52,53,54,55]. The anatomic structures and clinical picture of extracted lymph node specimens are shown in Fig. 5. Detailed procedures of GOSTA-SND can be watched in Video 2.
Pictures of the procedures for GOSTA-SND. a post-dissection of level IIA lymph nodes, b post-dissection of level III and IV lymph nodes, c Specimens after the surgery. GOSTA-SND gas-insufflation one-step single-port transaxillary approach for selective neck dissection, IJV internal jugular vein, SCM sternocleidomastoid muscle, EJV external jugular vein
The retrospective nature of the study, its reliance on a single surgeon’s experience, and the lack of long-term follow-up data, including survival rate and quality of life, are the limitations of this study. Further evaluation, including multi-center prospective studies, should be conducted to confirm the efficacy of the GOSTA approach. Additionally, conducting subgroup analysis based on tumor size or location is also necessary to comprehensively examine the GOSTA approach.
In conclusion, the GOSTA approach can be performed feasibly and safely, demonstrating non-inferiority to the CTA gasless thyroidectomy.
References
Mohamed SE, Noureldine SI, Kandil E (2014) Alternate incision-site thyroidectomy. Curr Opin Oncol 26:22–30. https://doi.org/10.1097/CCO.0000000000000031
de Vries LH, Aykan D, Lodewijk L, Damen JAA, Borel Rinkes IHM, Vriens MR (2021) Outcomes of minimally invasive thyroid surgery: a systematic review and meta-analysis. Front Endocrinol (Lausanne) 12:719397. https://doi.org/10.3389/fendo.2021.719397
Eckhardt S, Maurer E, Fendrich V, Bartsch DK (2015) Transaxillary robot-assisted thyroidectomy: first experiences with a new operation technique. Chirurg 86:976–982. https://doi.org/10.1007/s00104-015-0008-x
Vidal O, Delgado-Oliver E, Pino V, Vilaca J (2018) Transaxillary endoscopic thyroidectomy: another approach to offer our patients. Cir Esp (Engl Ed) 96:586. https://doi.org/10.1016/j.ciresp.2018.06.008
Jantharapattana K, Maethasith J (2017) Transaxillary gasless endoscopic thyroidectomy versus conventional open thyroidectomy: a randomized study. Eur Arch Otorhinolaryngol 274:495–500. https://doi.org/10.1007/s00405-016-4242-8
Anuwong A, Ketwong K, Jitpratoom P, Sasanakietkul T, Duh QY (2018) Safety and outcomes of the transoral endoscopic thyroidectomy vestibular approach. JAMA Surg 153:21–27. https://doi.org/10.1001/jamasurg.2017.3366
Kasouli A, Spartalis E, Giannakodimos A, Tsourouflis G, Dimitroulis D, Nikiteas NI (2023) Comparison of cosmetic outcomes between remote-access and conventional thyroidectomy: a review of the current literature. World J Otorhinolaryngol Head Neck Surg 9:1–8. https://doi.org/10.1002/wjo2.65
Sun H, Wang X, Zheng G, Wu G, Zeng Q, Zheng H (2022) Comparison Between transoral endoscopic thyroidectomy vestibular approach (TOETVA) and conventional open thyroidectomy for patients undergoing total thyroidectomy and central neck dissection: a propensity score-matching analysis. Front Oncol 12:856021. https://doi.org/10.3389/fonc.2022.856021
Wilhelm T, Harlaar J, Kerver A, Kleinrensink GJ, Benhidjeb T (2010) Transoral endoscopic thyroidectomy. Part 1: rationale and anatomical studies. Chirurg 81:50–55. https://doi.org/10.1007/s00104-009-1823-8
Russell JO, Noureldine SI, Al Khadem MG et al (2017) Transoral robotic thyroidectomy: a preclinical feasibility study using the da Vinci Xi platform. J Robot Surg 11:341–346. https://doi.org/10.1007/s11701-016-0661-1
Anuwong A (2016) Transoral endoscopic thyroidectomy vestibular approach: a series of the first 60 human cases. World J Surg 40:491–497. https://doi.org/10.1007/s00268-015-3320-1
Byeon HK, Holsinger FC, Tufano RP et al (2014) Robotic total thyroidectomy with modified radical neck dissection via unilateral retroauricular approach. Ann Surg Oncol 21:3872–3875. https://doi.org/10.1245/s10434-014-3896-y
Chung EJ, Park MW, Cho JG et al (2015) A prospective 1-year comparative study of endoscopic thyroidectomy via a retroauricular approach versus conventional open thyroidectomy at a single institution. Ann Surg Oncol 22:3014–3021. https://doi.org/10.1245/s10434-014-4361-7
Byeon HK, Holsinger FC, Tufano RP et al (2016) Endoscopic retroauricular thyroidectomy: preliminary results. Surg Endosc 30:355–365. https://doi.org/10.1007/s00464-015-4202-1
Liu SY, Kim JS (2017) Bilateral axillo-breast approach robotic thyroidectomy: review of evidences. Gland Surg 6:250–257. https://doi.org/10.21037/gs.2017.04.05
Woo JW, Kim SK, Park I, Choe JH, Kim JH, Kim JS (2017) A novel robotic surgical technique for thyroid surgery: bilateral axillary approach (BAA). Surg Endosc 31:667–672. https://doi.org/10.1007/s00464-016-5018-3
Yu HW, Bae IE, Yi JW et al (2019) The application of subcapsular saline injection during bilateral axillo-breast approach robotic thyroidectomy: a preliminary report. Surg Today 49:420–426. https://doi.org/10.1007/s00595-018-1748-2
Lee KE, Choi JY, Youn YK (2011) Bilateral axillo-breast approach robotic thyroidectomy. Surg Laparosc Endosc Percutan Tech 21:230–236. https://doi.org/10.1097/SLE.0b013e31822d0455
Jongekkasit I, Jitpratoom P, Sasanakietkul T, Anuwong A (2019) Transoral endoscopic thyroidectomy for thyroid cancer. Endocrinol Metab Clin 48:165–180. https://doi.org/10.1016/j.ecl.2018.11.009
Miccoli P, Bellantone R, Mourad M, Walz M, Raffaelli M, Berti P (2002) Minimally invasive video-assisted thyroidectomy: multiinstitutional experience. World J Surg 26:972–975. https://doi.org/10.1007/s00268-002-6627-7
Miccoli P, Minuto MN, Barellini L et al (2004) Minimally invasive video-assisted thyroidectomy—techniques and results over 4 years of experience (1999–2002). Ann Ital Chir 75:47–51
Kang SW, Jeong JJ, Yun JS et al (2009) Gasless endoscopic thyroidectomy using trans-axillary approach; surgical outcome of 581 patients. Endocr J 56:361–369. https://doi.org/10.1507/endocrj.k08e-306
Mitchem JB, Gillanders WE (2013) Endoscopic and robotic thyroidectomy for cancer. Surg Oncol Clin 22(1–13):v. https://doi.org/10.1016/j.soc.2012.08.009
Lee KE, Rao J, Youn YK (2009) Endoscopic thyroidectomy with the da Vinci robot system using the bilateral axillary breast approach (BABA) technique: our initial experience. Surg Laparosc Endosc Percutan Tech 19:e71–e75. https://doi.org/10.1097/SLE.0b013e3181a4ccae
Perrier ND, Randolph GW, Inabnet WB, Marple BF, VanHeerden J, Kuppersmith RB (2010) Robotic thyroidectomy: a framework for new technology assessment and safe implementation. Thyroid 20:1327–1332. https://doi.org/10.1089/thy.2010.1666
Kang SW, Jeong JJ, Nam KH, Chang HS, Chung WY, Park CS (2009) Robot-assisted endoscopic thyroidectomy for thyroid malignancies using a gasless transaxillary approach. J Am Coll Surg 209:e1-7. https://doi.org/10.1016/j.jamcollsurg.2009.05.003
Richmon JD, Kim HY (2017) Transoral robotic thyroidectomy (TORT): procedures and outcomes. Gland Surg 6:285–289. https://doi.org/10.21037/gs.2017.05.05
Chang YW, Lee HY, Ji WB et al (2020) Detailed comparison of robotic and endoscopic transaxillary thyroidectomy. Asian J Surg 43:234–239. https://doi.org/10.1016/j.asjsur.2019.02.012
Yu DY, Chang YW, Lee HY et al (2021) Detailed comparison of the da Vinci Xi and S surgical systems for transaxillary thyroidectomy. Medicine (Baltimore) 100:24370. https://doi.org/10.1097/MD.0000000000024370
Chang YW, Kim HS, Kim HY, Lee JB, Bae JW, Son GS (2016) Should central lymph node dissection be considered for all papillary thyroid microcarcinoma? Asian J Surg 39:197–201. https://doi.org/10.1016/j.asjsur.2015.02.006
Chang YW, Lee HY, Kim HS, Kim HY, Lee JB, Son GS (2018) Extent of central lymph node dissection for papillary thyroid carcinoma in the isthmus. Ann Surg Treat Res 94:229–234. https://doi.org/10.4174/astr.2018.94.5.229
Kandil E, Attia AS, Hadedeya D, Shihabi A, Elnahla A (2020) Robotic thyroidectomy: past, future, and current perspectives. Otolaryngol Clin 53:1031–1039. https://doi.org/10.1016/j.otc.2020.09.001
Haidar Ismail N, Tavalla P, Uppal P et al (2022) The advantages of robotic over open thyroidectomy in thyroid diseases: a systematic review. Cureus 14:26320. https://doi.org/10.7759/cureus.26320
Akritidou E, Douridas G, Spartalis E, Tsourouflis G, Dimitroulis D, Nikiteas NI (2022) Complications of trans-oral endoscopic thyroidectomy vestibular approach: a systematic review. In Vivo 36:1–12. https://doi.org/10.21873/invivo.12671
Lee DW, Bang HS, Jeong JH, Kwak SG, Choi YY, Tae K (2021) Cosmetic outcomes after transoral robotic thyroidectomy: comparison with transaxillary, postauricular, and conventional approaches. Oral Oncol 114:105139 https://doi.org/10.1016/j.oraloncology.2020.105139
Yuan Y, Sun C, Yin T et al (2022) Comparison of endoscopic thyroidectomy by complete areola approach and conventional open surgery in the treatment of differentiated thyroid carcinoma: a retrospective study and meta-analysis. Front Surg 9:1000011. https://doi.org/10.3389/fsurg.2022.1000011
Chen GZ, Zhang X, Shi WL, Zhuang ZR, Chen X, Han H (2012) Systematic comparison of cervical and extra-cervical surgical approaches for endoscopic thyroidectomy. Surg Today 42:835–841. https://doi.org/10.1007/s00595-011-0100-x
Chai YJ, Kim HY, Kim HK et al (2018) Comparative analysis of 2 robotic thyroidectomy procedures: transoral versus bilateral axillo-breast approach. Head Neck 40:886–892. https://doi.org/10.1002/hed.25034
Dionigi G, Tufano RP, Russell J, Kim HY, Piantanida E, Anuwong A (2017) Transoral thyroidectomy: advantages and limitations. J Endocrinol Invest 40:1259–1263. https://doi.org/10.1007/s40618-017-0676-0
Fregoli L, Rossi L, Papini P, Materazzi G (2020) Robotic transaxillary thyroidectomy: state of the art. Gland Surg 9:S61–S64. https://doi.org/10.21037/gs.2019.10.11
Piccoli M, Mullineris B, Santi D, Gozzo D (2017) Advances in robotic transaxillary thyroidectomy in Europe. Curr Surg Rep 5:17. https://doi.org/10.1007/s40137-017-0180-7
Jasaitis K, Midlenko A, Bekenova A, Ignatavicius P, Gulbinas A, Dauksa A (2021) Transaxillary gasless endoscopic thyroidectomy versus conventional open thyroidectomy: systematic review and meta-analysis. Wideochir Inne Tech Maloinwazyjne 16:482–490. https://doi.org/10.5114/wiitm.2021.105722
Duncan TD, Rashid Q, Speights F, Ejeh I (2009) Transaxillary endoscopic thyroidectomy: an alternative to traditional open thyroidectomy. J Natl Med Assoc 101:783–787. https://doi.org/10.1016/s0027-9684(15)31006-3
Alzahrani HA, Mohsin K, Ali DB, Murad F, Kandil E (2017) Gasless trans-axillary robotic thyroidectomy: the technique and evidence. Gland Surg 6:236–242. https://doi.org/10.21037/gs.2017.06.04
Xu S, Yang Z, Guo Q et al (2022) Surgical steps of gasless transaxillary endoscopic thyroidectomy: from A to Z. J Oncol 2022:2037400. https://doi.org/10.1155/2022/2037400
Miyano G, Lobe TE, Wright SK (2008) Bilateral transaxillary endoscopic total thyroidectomy. J Pediatr Surg 43:299–303. https://doi.org/10.1016/j.jpedsurg.2007.10.018
Kang SW, Lee SH, Ryu HR et al (2010) Initial experience with robot-assisted modified radical neck dissection for the management of thyroid carcinoma with lateral neck node metastasis. Surgery 148:1214–1221. https://doi.org/10.1016/j.surg.2010.09.016
Shin YS, Hong HJ, Koh YW et al (2012) Gasless transaxillary robot-assisted neck dissection: a preclinical feasibility study in four cadavers. Yonsei Med J 53:193–197. https://doi.org/10.3349/ymj.2012.53.1.193
Ho J, Kim D, Lee JE et al (2023) Single-port transaxillary robotic modified radical neck dissection (STAR-RND): initial experiences. Laryngoscope 133:709–714. https://doi.org/10.1002/lary.30437
Friedman M, Lim JW, Dickey W et al (1999) Quantification of lymph nodes in selective neck dissection. Laryngoscope 109:368–370. https://doi.org/10.1097/00005537-199903000-00005
Choi JY, Kang KH (2017) Robotic modified radical neck dissection with bilateral axillo-breast approach. Gland Surg 6:243–249. https://doi.org/10.21037/gs.2017.06.09
Kim MJ, Lee J, Lee SG et al (2017) Transaxillary robotic modified radical neck dissection: a 5-year assessment of operative and oncologic outcomes. Surg Endosc 31:1599–1606. https://doi.org/10.1007/s00464-016-5146-9
Zhang Z, Sun B, Ouyang H, Cong R, Xia F, Li X (2021) Endoscopic lateral neck dissection: a new frontier in endoscopic thyroid surgery. Front Endocrinol (Lausanne) 12:796984. https://doi.org/10.3389/fendo.2021.796984
Yu HW, Chai YJ, Kim SJ, Choi JY, Lee KE (2018) Robotic-assisted modified radical neck dissection using a bilateral axillo-breast approach (robotic BABA MRND) for papillary thyroid carcinoma with lateral lymph node metastasis. Surg Endosc 32:2322–2327. https://doi.org/10.1007/s00464-017-5927-9
Chang YW, Kim HS, Jung SP et al (2017) Significance of micrometastases in the calculation of the lymph node ratio for papillary thyroid cancer. Ann Surg Treat Res 92:117–122. https://doi.org/10.4174/astr.2017.92.3.117
Funding
This study was funded by Korea University (KR) (K2208451).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Young Woo Chang was supported by a Korea University Grant (K2208451). Da Young Yu, Dohoe Ku, Seung Yeon Ko, Hye Yoon Lee, and Gil Soo Son have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 93,722 KB)
Supplementary file2 (MP4 56,422 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, D.Y., Chang, Y.W., Ku, D. et al. Robotic thyroidectomy using gas-insufflation one-step single-port transaxillary (GOSTA) approach. Surg Endosc 37, 8861–8870 (2023). https://doi.org/10.1007/s00464-023-10435-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10435-w