Abstract
Background
Combined liver and bile duct resection with biliary reconstruction for hepatobiliary malignancies are defined as highly complex surgical procedures. The robotic platform may overcome some major limitations of conventional laparoscopic surgery for these complex cases but its precise role is however still to be defined.
Methods
In our institution, patients requiring major hepatectomy with biliary reconstruction for malignancies were consecutively selected for minimally invasive robotic surgery from September 2020. All surgeries were undertaken using the da Vinci Xi Surgical System® (Intuitive Surgical, Sunnyvale, CA, USA). Intra-operative technique and postoperative outcome were analyzed.
Results
A total number of 10 patients (3 males and 7 females, median age 72 years) underwent robotic major hepatectomy and bile duct resection for hepatobiliary malignancies between September 2020 and March 2022. The indication for surgery was perihilar cholangiocarcinoma in 5 of 10 patients. Median operative time was 338 min and median blood loss was 110 mL. Postoperative length of stay was between 3 and 16 days (median: 9 days). There was no postoperative 90-day mortality.
Conclusions
A robotic approach for hepatobiliary malignancies requiring combined major hepatectomy and bile duct resection seems feasible and safe in experienced hands.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Combined major hepatectomy and bile duct resection with biliary reconstruction for hepatobiliary malignancies are defined as highly complex surgical procedures. These cases are often performed by an open approach as technical surgical challenges have limited a wide implementation of a conventional laparoscopic approach. Robotic surgery may overcome some major limitations of conventional laparoscopic surgery but its precise role in combined liver and bile duct resection with biliary reconstruction is however still to be defined.
Recent papers have demonstrated the feasibility of a conventional laparoscopic approach for major and technically difficult liver resections [1,2,3,4]. However, only few reports describe a pure laparoscopic approach for combined liver and bile duct resections with bilio-enteric reconstruction [5,6,7,8]. These cases usually involve patients with perihilar cholangiocarcinoma, already known to have a significant risk of perioperative morbidity when performed by an open approach [9]. The robotic platform has however allowed for better three-dimensional visualization, tremor filtering, increased dexterity and ease of suturing as compared to conventional laparoscopy. Recent multicenter studies already reported favorable results of robotic surgery compared to conventional laparoscopic surgery for pancreas and liver resections [10,11,12].
The aim of this paper is to report the feasibility and results of robotic combined major hepatectomy and bile duct resection with biliary reconstruction for advanced hepatobiliary malignancies.
Materials and methods
We started robotic hepatobiliary surgery in our center in the beginning of 2020. Initial robotic experience was gained with inguinal hernia cases, distal pancreatectomies and minor liver resections. Following our progressive experience with robotic pancreatic and liver surgery, patients requiring combined liver and bile duct resection were consecutively selected for minimally invasive robotic surgery from September 2020. Only patients with preoperatively suspected portal invasion or unclear resectability were selected for an open procedure upfront. Also, limited robotic access lead to immediate open surgery in a few patients in this time period. A conventional laparoscopic approach was never used in our center for this patient group.
The indication for surgery was discussed by a multidisciplinary team for all cases. All patients underwent preoperative evaluation with computed tomography imaging and magnetic resonance imaging with cholangiopancreatography to define biliary anatomy.
Information regarding patient demographics, indication for surgery, intra-operative details and postoperative course were prospectively collected in our database. Institutional review board approval and written consent was not needed for this analysis.
Surgical technique
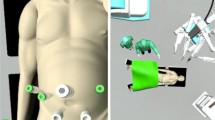
All surgeries were undertaken using the da Vinci Xi Surgical System® (Intuitive Surgical, Sunnyvale, CA, USA). Our surgical technique was described in detail in a previous publication [13]. Briefly, patients were placed in supine position with legs parted and a laparoscopic assistant standing between the legs. Three robotic trocars were placed in a straight line with a fourth trocar on the left side slightly more cranially. The robotic port on the right midclavicular line usually was a 12 mm port that could be used for robotic stapling. In obese patients or patients with a large abdomen, ports were placed above the level of the umbilicus (approximately 20 cm below the xiphoid). One or two additional 12 mm assistant trocars were generally placed in the lower abdomen in between two robotic trocars (Fig. 1). The robot was docked, coming from the patient’s right side.
Meticulous dissection of the liver hilum was generally done using the monopolar robotic hook, monopolar scissors and bipolar Maryland or bipolar forceps. Robotic ultrasound and indocyanine green were used selectively to assess individual biliary and vascular anatomy. Liver parenchymal dissection was done using the Kelly clamp crush technique with robotic Maryland and robotic vessel sealer. Total pedicular clamping was used selectively during parenchymal dissection to reduce blood loss. In general, pedicular clamping was applied when parenchymal transection was performed through non-ischemic liver. Inflow occlusion was not used when the transection line ran through ischemic liver parenchyma.
For bilio-enteric reconstruction, a Roux-en-Y loop was prepared 30 to 40 cm from Treitz ligament. In patients with non-dilated bile ducts, the hepaticojejunostomy was performed using separate sutures with vicryl 4/0 for the anterior and posterior wall. In case of dilated bile ducts, we use a running v-loc™ 4/0 suture for the posterior wall and separate vicryl 4/0 sutures for the anterior wall.
An intracorporeal robotic end-to-side entero-enterostomy was made 60 cm more distally. The anastomosis was a two layered anastomosis using two layers of a resorbable v-loc™ 3/0 running suture.
In all cases, a silicone drain was placed near the hepaticojejunostomy to detect postoperative bile leakage.
Postoperative outcome
Postoperative complications were classified using the Clavien-Dindo classification [14]. After discharge, patients were followed in our outpatient clinic at 1 month after surgery and on indication thereafter.
Statistical analysis
Descriptive statistics including percentages, medians and ranges were calculated using Microsoft Excel (Microsoft, Redmond, WA, USA).
Results
The proportion of patients that underwent minimally invasive liver surgery in our center increased from 70% in 2017 to 95% in 2021 (Fig. 2). From 2021, the majority of minimally invasive procedures was performed robotically.
Between September 2020 and March 2022, 11 patients underwent robotic combined liver and bile duct resection with biliary reconstruction for hepatobiliary malignancies. Before starting combined robotic liver and bile duct resection, we had performed already 42 technically or anatomically major robotic hepatic resections and 22 pancreatic resections. For this analysis, patients that underwent a minor hepatectomy (less than 3 segments) were excluded (N = 1). During this study period, 9 other patients underwent open surgery with combined liver and bile duct resection. In two of these cases, open surgery was performed because of unavailability of the robotic system. The other seven cases had a preoperative high suspicion of portal invasion with the need for portal reconstruction.
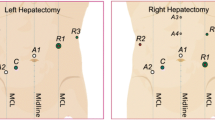
This series of patients included 3 males and 7 females between 35 and 77 years old (median age: 72 years) (Table 1). Four patients had previous open abdominal surgery. The indication for surgery was perihilar cholangiocarcinoma in 5 of 10 patients (Fig. 3). Other patients suffered from colorectal liver metastasis (N = 2), gallbladder carcinoma (N = 2) and HCC (N = 1) (Table 2). Two patients had preoperative biliary drainage and portal vein embolization was performed in one patient. In three other patients, the right portal vein was occluded by tumor resulting in hypertrophy of the left hemiliver.
Robotic major hepatectomy and bile duct resection for perihilar cholangiocarcinoma (Klatskin type IV). A hilar dissection on portal vein; B bile duct transection for frozen section; C release of segment 1 from caval vein; D left hepatectomy with segment 1; E double barrel anastomosis between right anterior and posterior bile duct; F hepaticojejunostomy
Operative characteristics
Median operative time was 338 min (range: 255 to 460 min) (Table 3). Median blood loss was 110 mL (range 40 to 350 mL). One of 4 patients operated without pedicular clamping did not tolerate inflow occlusion due to severe hypotension and subsequently had the highest blood loss in this series. There were no intra-operative complications or technical issues and no conversions.
Regarding biliary reconstruction, in 6 patients the bilio-enteric anastomosis involved only one bile duct. In 3 patients, two separate anastomoses were created for individual bile ducts. A double barrel anastomosis was made in only 1 patient.
Postoperative outcome
Postoperative length of stay ranged between 3 and 16 days (median: 9 days).
One patient was readmitted with a biloma on postoperative day 12 requiring percutaneous drainage (Clavien-Dindo grade III). On postoperative day 15, ERCP was performed with placement of a plastic stent. She was discharged with the drain in situ that was removed eventually on day 56. There was no postoperative 90-day mortality.
Discussion
In modern liver surgery, it is currently accepted that minimally invasive resections have superior outcome when compared to an open approach [12]. For complex hepatobiliary malignancies, such as perihilar cholangiocarcinoma requiring major resections and difficult reconstruction, a minimally invasive approach has however been considered impossible for a long period of time. This was related to the limitations of conventional laparoscopic surgery in terms of fine dissection and advanced suturing. However, some authors have reported acceptable feasibility and safety of a laparoscopic approach in selected patients [5, 15, 16]. Nevertheless, a supra-umbilical median incision is often used to create the hepatico-jejunal anastomosis [5]. A wide implementation of this technique has furthermore been poor [6].
The introduction of robotic surgery has allowed for better visualization, tremor filtering and increased dexterity creating the possibility of more complex minimally invasive procedures. As a result, we and others have previously reported initial experiences with robotic surgery with biliary reconstruction [13, 17]. In addition, first results were recently reported for robotic resection of extrahepatic cholangiocarcinoma in a series of 15 patients in the USA [18]. However, not all of these patients underwent combined major hepatectomy and bile duct resection. Overall, there were no intra-operative complications and short-term outcome was promising.
In this preliminary first European series, we describe 10 patients that underwent robotic resection of complex hepatobiliary malignancies requiring major hepatectomy and bile duct resection with biliary reconstruction. Of all included patients, half of them had perihilar cholangiocarcinoma type III or IV. Although it only involves 10 cases in total, this single-center series illustrates that robotic surgery is feasible with limited blood loss and minor morbidity, even in patients that previously had open surgery. Also, 9 of 10 patients had negative surgical margins, confirming the oncological safety.
In the literature, most reports come from high-volume centers in Asia. These papers also show favorable outcomes for robotic resection for perihilar cholangiocarcinoma in terms of blood loss and length of hospital stay [19, 20]. Also, oncological outcomes were not inferior. However, another paper reported worse morbidity after robotic surgery compared to an open group, possibly due to poor patient selection and insufficient robotic experience [21]. In general, robotic surgery for biliary tract cancer appeared to be non-inferior to open surgery in a recent review article [22].
We believe that sufficient robotic experience with hepatobiliary surgery is essential when offering this technique to patients with complex malignant disease. In our center, we started offering robotic surgery for these patients only after having performed a significant number of robotic pancreatic resections and robotic major hepatectomies (as well as conventional laparoscopic major hepatectomies). The complexity of dissecting the structures of the porta hepatis and biliary reconstruction can only be mastered by the sum of experiences gained with robotic pancreatic surgery and major hepatectomy.
One could argue the role of the robotic platform in these advanced cases for surgeons that are masters in conventional laparoscopic hepatobiliary surgery. One of the advantages of the robotic approach may be a higher rate of retrieved lymph nodes as previously reported after robotic gastrectomy for gastric cancer [23]. In our series, a median number of 8.5 lymph nodes was retrieved, significantly higher than the advised number of 4 lymph nodes required for adequate staging [24]. Furthermore, hilar dissection and bile duct reconstruction requiring advanced suturing can be performed more easily and precisely using the robot. Indeed, the introduction of robotic surgery in our hepatobiliary unit has increased the percentage of minimally invasive procedures to approximately 95%. This was mainly the result of including advanced cases for robotic surgery that previously would have been operated by an open approach.
To enhance a further implementation of robotic hilar dissection and biliary reconstruction, we recently developed a porcine model for training purposes (Fig. 4). With this model, arterial and portal dissection as well as biliary reconstruction can be trained in a standardized manner, helping to improve individual surgical skills.
In conclusion, this series supports the application of robotic minimally invasive surgery for complex hepatobiliary malignancies in a high-volume center with sufficient robotic case load. Standardized training may lead to a further safe implementation of this technique.
References
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263: 761-777
D’Hondt M, Tamby E, Boscart I et al (2018) Laparoscopic versus open parenchymal preserving liver resections in the posterosuperior segments: a case-matched study. Surg Endosc 32:1478–1485
Fretland AA, Dagenborg VJ, Bjørnelv GMW et al (2018) Laparoscopic versus open resection for colorectal liver metastases: the OSLO-COMET randomized controlled trial. Ann Surg 267:199–207
Schmelzle M, Krenzien F, Schöning W, Pratschke J (2020) Laparoscopic liver resection: indications, limitations, and economic aspects. Langenbecks Arch Surg 405:725–735
Ratti F, Fiorentini G, Cipriani F, Catena M, Paganelli M, Aldrighetti L (2020) Perihilar cholangiocarcinoma: are we ready to step towards minimally invasiveness? Updat Surg 72:423–433
Franken LC, van der Poel MJ, Latenstein AEJ et al (2019) Minimally invasive surgery for perihilar cholangiocarcinoma: a systematic review. J Robot Surg 13:717–727
Feng F, Cao X, Liu X et al (2019) Laparoscopic resection for Bismuth type III and IV hilar cholangiocarcinoma: how to improve the radicality without direct palpation. J Surg Oncol 120:1379–1385
Li J, Zhao L, Zhang J et al (2017) Application of the laparoscopic technique in perihilar cholangiocarcinoma surgery. Int J Surg 44:104–109
Nagino M, Ebata T, Yokoyama Y et al (2013) Evolution of surgical treatment for perihilar cholangiocarcinoma: a single-center 34-year review of 574 consecutive resections. Ann Surg 258:129–140
Lof S, Vissers FL, Klompmaker S et al (2021) Risk of conversion to open surgery during robotic and laparoscopic pancreatoduodenectomy and effect on outcomes: international propensity score-matched comparison study. Br J Surg 108:80–87
Lof S, van der Heijde N, Abuawwad M et al (2021) Robotic versus laparoscopic distal pancreatectomy: multicentre analysis. Br J Surg 108:188–195
Ciria R, Berardi G, Alconchel F et al (2020) The impact of robotics in liver surgery: a worldwide systematic review and short-term outcomes meta-analysis on 2728 cases. J Hepatobiliary Pancreat Sci. https://doi.org/10.1002/jhbp.869
D’Hondt M, Wicherts DA (2022) Robotic biliary surgery for benign and malignant bile duct obstruction: a case series. J Robot Surg. https://doi.org/10.1007/s11701-022-01392-y
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Zhang Y, Dou C, Wu W et al (2019) Total laparoscopic versus open radical resection for hilar cholangiocarcinoma. Surg Endosc. https://doi.org/10.1007/s00464-019-07211-0
Levi Sandri GB, Spoletini G, Mascianà G et al (2017) The role of minimally invasive surgery in the treatment of cholangiocarcinoma. Eur J Surg Oncol 43:1617–1621
Hawksworth J, Radkani P, Nguyen B et al (2021) Robotic hepaticojejunostomy for late anastomotic biliary stricture after liver transplantation: technical description and case series. Ann Surg. https://doi.org/10.1097/SLA.0000000000005303
Sucandy I, Shapera E, Jacob K et al (2021) Robotic resection of extrahepatic cholangiocarcinoma: institutional outcomes of bile duct cancer surgery using a minimally invasive technique. J Surg Oncol 125:161–167
Wang W, Fei Y, Liu J, Yu T, Tang J, Wei F (2021) Laparoscopic surgery and robotic surgery for hilar cholangiocarcinoma: an updated systematic review. ANZ J Surg 91:42–48
Li J, Tan X, Zhang X et al (2020) Robotic radical surgery for hilar cholangiocarcinoma: a single-centre case series. Int J Med Robot 16:e2076
Xu Y, Wang H, Ji W et al (2016) Robotic radical resection for hilar cholangiocarcinoma: perioperative and long-term outcomes of an initial series. Surg Endosc 30:3060–3070
Kone LB, Bystrom PV, Maker AV (2022) Robotic surgery for biliary tract cancer. Cancers 14:1046
Guerrini GP, Esposito G, Magistri P et al (2020) Robotic versus laparoscopic gastrectomy for gastric cancer: the largest meta-analysis. Int J Surg 82:210–228
Bagante F, Tran T, Spolverato G et al (2016) Perihilar cholangiocarcinoma: number of nodes examined and optimal lymph node prognostic scheme. J Am Coll Surg 222:750–759
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Mathieu D’Hondt and Dr. Dennis Wicherts have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
D’Hondt, M., Wicherts, D.A. Pure robotic major hepatectomy with biliary reconstruction for hepatobiliary malignancies: first European results. Surg Endosc 37, 4396–4402 (2023). https://doi.org/10.1007/s00464-023-09863-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-09863-5