Abstract
Background
An encysted spermatic cord hydrocele (ESCH) causes an inguinal swelling resembling an inguinal hernia (IH). An ESCH should be considered as a differential diagnosis of IH. Although laparoscopic operations have been performed to treat ESCHs in pediatric patients, such operations have not been reported in adults. This study was performed to evaluate the outcomes of laparoscopic hydrocelectomy for treatment of ESCHs in adults.
Methods
The medical charts of 49 patients who underwent laparoscopic transabdominal hydrocelectomy for ESCHs from January 2015 to December 2020 at a single institution were retrospectively reviewed. The patients were divided into those with and without an IH. Laparoscopic hydrocelectomy was performed, and the internal inguinal ring was closed with iliopubic tract repair (IPTR) or transabdominal preperitoneal (TAPP) hernioplasty depending on the presence of an IH. The patients’ age, ESCH location, postoperative complications, recurrence, and operating time were examined.
Results
The patients’ mean age was 46.7 (20–77) years. All patients underwent laparoscopic hydrocelectomy without open conversion. ESCHs were more common on the right side (35/49, 71.4%) than on the left (14/49, 28.6%). The presenting symptom in all patients was inguinal swelling. The ESCH was located inside the inguinal canal in 47 patients and protruded to the abdominal cavity from the inguinal canal in 2 patients. After laparoscopic hydrocelectomy, 32 patients without an IH underwent IPTR and 17 patients with an IH underwent TAPP hernioplasty. The mean operating time was shorter in the IPTR than TAPP hernioplasty group. The postoperative complications and hospital stay were not different between the two groups. There were no recurrences in either group.
Conclusions
Laparoscopic hydrocelectomy with IPTR or TAPP hernioplasty is safe and feasible for treatment of ESCHs in adults.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
An encysted spermatic cord hydrocele (ESCH) is one of the various causes of inguinal swelling in men. An ESCH in the inguinal canal is caused by central fluid accumulation with obliteration of the distal and proximal of processus vaginalis [1]. An ESCH is often misdiagnosed as an incarcerated inguinal hernia (IH) on physical examination; however, it is easily diagnosed with ultrasonography, which shows an ESCH as a round, hypoechoic lesion in pediatrics and adults [2, 3]. The types of hydroceles that occur in men are scrotal hydroceles, communicating hydroceles, and ESCHs. Many reports have described the treatment of scrotal hydroceles and communicating hydroceles, but few have focused on the treatment of ESCHs.
Complete excision is the recommended treatment for symptomatic ESCHs. Laparoscopic operations have recently become widely used for inguinal disease. Laparoscopic hydrocelectomy for ESCHs in pediatric male patients has been reported [2]. Open hydrocelectomy has been described in several case reports of ESCHs in adults [3,4,5]; to the best of our knowledge, however, there has been no report of a consecutive series of laparoscopic hydrocelectomies with statistics on the efficacy, safety, and natural history of ESCH treatment in adults. The recommended treatment in pediatric patients is hydrocelectomy and high ligation [6], but in adult patients, high ligation alone as a method to cover the internal ring can increase the risk of recurrence. Most of the case reports to date have described hydrocelectomy by the open approach, and recurrence has not been reported because of the lack of follow-up [7]. In one case, however, hernioplasty was performed to treat the funicular type [8]. In addition, hydrocelectomy and mesh implantation are required if an ESCH is accompanied by an IH.
After laparoscopic hydrocelectomy, we performed transabdominal preperitoneal (TAPP) hernioplasty for ESCHs with an IH and iliopubic tract repair (IPTR) for ESCHs without an IH as a method of covering the internal ring. The present study was performed to evaluate the safety (complications and operating time) and efficacy (recurrence rates) of laparoscopic hydrocelectomy with IPTR or TAPP hernioplasty in treating ESCHs in adults.
Materials and methods
This was a retrospective observational cohort study. From January 2015 to December 2020, 2177 patients with an inguinal bulge underwent laparoscopic repair at Damsoyu Hospital (Fig. 1). Of these patients, 2128 patients who had an IH without an ESCH were excluded. Finally, 49 patients were included in this study. All patients were diagnosed with an ESCH by ultrasonography (Fig. 2). They were then divided into those with and without an IH (Fig. 3). Laparoscopic hydrocelectomy was performed, and the internal inguinal ring was closed by IPTR or TAPP hernioplasty depending on the presence of an IH. We considered that conventional TAPP hernioplasty was overtreatment for ESCH without IH. Therefore, the patients were divided into an ESCH with IH group and an ESCH without IH group. Postoperative pain after 1 month was evaluated using a numeric rating scale (0–10 points) [9]. This study was approved by the institutional review board of our hospital.
Types of encysted spermatic cord hydroceles. a Encysted spermatic cord hydrocele in the inguinal canal (white arrow). b Encysted spermatic cord hydrocele (white arrow) protruding into the abdominal cavity from the inguinal canal. c Encysted spermatic cord hydrocele with an inguinal hernia. d Internal ring after hydrocelectomy. IH indirect hernia, IR internal ring, IEV inferior epigastric vessel, VD vas deferens, GV gonadal vessel
Laparoscopic hydrocelectomy with IPTR or TAPP hernioplasty
All procedures were performed with the patients under general anesthesia in the supine position. The laparoscopic system comprised a 5.0-mm camera and instruments. A transumbilical incision was made, and a trocar was inserted to create carbon dioxide pneumoperitoneum that was maintained at 8–10 mmHg. Two other instruments were inserted through separate 5.0-mm stab incisions in the lateral abdomen. Intracorporeal hydrocelectomy was then performed (Fig. 4). When the ESCH was pulled into the abdominal cavity with a grasper, a distinct dissection plane between the hydrocele and the peritoneum could be identified. As the ESCH was continuously pulled into the abdominal cavity, the peritoneum attached to the hydrocele was pushed away in the opposite direction from which the ESCH was being pulled. Through this process, the vas deferens and spermatic vessel become located far enough away from the hydrocele that they were not at risk of injury. As the dissection progressed, the ESCH was gradually drawn into the abdominal cavity. The resected ESCH was extracted through the right lateral port site. After hydrocelectomy, the internal ring was covered by IPTR or TAPP hernioplasty (Fig. 4). The peritoneum was repaired using absorbable multifilament suture (2–0 Vicryl; Ethicon Inc., Somerville, NJ, USA).
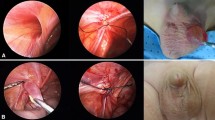
Laparoscopic hydrocelectomy for treatment of encysted spermatic cord hydrocele by iliopubic tract repair or transabdominal preperitoneal hernioplasty. a Encysted spermatic cord hydrocele without an inguinal hernia. b Hydrocelectomy. c First stitch of iliopubic tract repair (suture of iliopubic tract and transversus abdominis fascia). d High ligation after iliopubic tract repair. e Encysted spermatic cord hydrocele with an inguinal hernia. f Hydrocelectomy. g Preperitoneal space dissection. d Mesh implantation. IPT iliopubic tract, TAF transversus abdominis fascia
Statistical analysis
All statistical analyses were performed using R software version 3.6.1 (R Development Core Team, Vienna, Austria; http://www.R-project.org). Continuous variables are presented as mean and range, whereas categorical variables are presented as frequency and percentage. The Wilcoxon rank-sum test was used to test for normality of continuous variables. Fisher’s exact test or the χ2 test was used for categorical variables. A p value threshold of 0.05 was chosen, and any univariate p value of ≤ 0.05 was considered statistically significant.
Protocols and follow-up
Patients were permitted to ingest liquids postoperatively after 2 h of observation. The protocol for our institution stipulates that patients can be discharged once their condition remains stable and they are comfortable performing walking and eating. Routine outpatient follow-up included physical examinations 1 week, 1 month, and 1 year postoperatively and a telephone interview every year. Telephone interviews were performed to obtain information on patients’ postoperative statuses, such as pain and complications.
Results
The patients’ characteristics are shown in Table 1. All patients presented with inguinal swelling. In the laparoscopic view, two types of ESCHs were observed: the hour-glass type buried in the canal (47 cases) and the protruding intra-abdominal type (2 cases). The main symptom was discomfort in 44 patients and pain in 5 patients. The surgical outcomes are shown in Table 2. After laparoscopic hydrocelectomy, 32 patients without an IH underwent IPTR, and 17 patients with an IH underwent TAPP hernioplasty. The mean operating time was shorter in the IPTR group than in the TAPP hernioplasty group. Postoperative complications, the hospital stay, and the pain score were not different between the two groups. The mean follow-up period was 56.4 ± 23.7 (16–83) months in the IPTR group and 41.9 ± 25.1 (13–83) months in the TAPP hernioplasty group. There were no recurrences in either group during follow-up period.
Discussion
Laparoscopy is being increasingly used to treat disorders in the inguinal canal; however, there is little information on surgical treatment of ESCHs in adult patients. This article reports a series of 49 patients with ESCHs treated with laparoscopic hydrocelectomy. The prevalence of ESCHs in adult patients has not been accurately reported, but the prevalence of ESCHs in pediatric patients with an inguinal bulge has been reported as 1.9% [2]. In this study, the prevalence of ESCHs in men with an inguinal bulge was 2.6%.
Clinically, an ESCH presents as a pain or discomfort with an inguinal swelling that is usually nonreducible and is difficult to differentiate from an IH by clinical examination. The swelling does not spontaneously reduce, thus mimicking an incarcerated IH. A few case reports have described hemorrhagic or inflammatory ESCHs with acute severe painful swelling. In the present series, the ESCHs invariably contained serous fluid, and the patients did not complain of acute pain.
In this study, 5 (10.2%) patients reported chronic pain and the remaining 44 (89.8%) patients reported discomfort. Although there has been no report of an ESCH undergoing a malignant change, treatment is needed to resolve the pain and discomfort. Open surgery with a skin crease incision was used in many previous case reports of hydrocelectomy [3,4,5]. Our experience performing laparoscopic hydrocelectomy in pediatric male patients [2] suggests that it is reasonable to try this procedure for adult patients with ESCHs.
Hydrocelectomy is not difficult with complete removal of the ESCH while preserving the spermatic vessels and vas deferens. After hydrocelectomy, the open internal ring needs to be resolved. For patients with an ESCH accompanied by an IH, TAPP hernioplasty may be the best treatment choice. However, treatment of an ESCH without an IH using TAPP hernioplasty may be overtreatment. Therefore, in this study, TAPP hernioplasty was performed for ESCHs with an IH, and IPTR was performed for ESCHs without an IH. The Nyhus groin hernia classification system is used worldwide [10]. Nyhus [11] classified primary indirect IHs as type II and IIIB. A type II IH comprises only a dilated internal ring, while a type IIIB IH comprises a dilated internal ring with encroachment on the transversalis fascia of Hesselbach’s triangle. It has been proposed that IPTR alone is sufficient for treating a type II IH, whereas an implanted mesh is required for a type IIIB IH [12]. For patients with an ESCH without an IH, when the Nyhus classification is applied to the internal ring after hydrocelectomy, the internal ring is classified as type II. Mesh implantation may constitute overtreatment for an ESCH without an IH. Many reports have described laparoscopic IPTR [13,14,15,16]. We believe that surgeons must maintain the beneficial aspects of the old operation while transitioning to the new operation.
This study has some limitations. Only laparoscopic operations were performed; thus, no comparison with open surgery could be made. Although the number of patients (n = 49) included in our study may seem small compared with the number of patients included in studies on other diseases, this study is considered valuable in that the prevalence of ESCHs is low and there are few reports on this condition.
Conclusion
Although, ESCHs do not occur in adults as often as in pediatric patients, they require treatment because of pain and discomfort. Laparoscopic hydrocelectomy with IPTR or TAPP hernioplasty is a safe and feasible method for treating ESCHs in adults.
References
Chang YT, Lee JY, Wang JY, Chiou CS, Chang CC (2010) Hydrocele of the spermatic cord in infants and children: its particular characteristics. Urology 76(1):82–86. https://doi.org/10.1016/j.urology.2010.02.062
Choi BS, Byun GY, Hwang SB, Koo BH, Lee SR (2017) A comparison between totally laparoscopic hydrocelectomy and scrotal incision hydrocelectomy with laparoscopic high ligation for pediatric cord hydrocele. Surg Endosc 31(12):5159–5165. https://doi.org/10.1007/s00464-017-5582-1
Busigó JP, Eftekhari F (2007) Encysted spermatic cord hydroceles: a report of three cases in adults and a review of the literature. Acta Radiol 48(10):1138–1142. https://doi.org/10.1080/02841850701553163
Wani I, Rather M, Naikoo G, Gul I, Bhat Z, Baba A (2009) Encysted hydrocele of cord in an adult misdiagnosed as irreducible hernia: a case report. Oman Med J 24(3):218–219. https://doi.org/10.5001/omj.2009.43
Ogbetere FE (2021) Encysted hydrocele of the cord in a nineteen-year-old male mimicking irreducible inguinal hernia: a case report. Asian J Case Rep Surg 10(4):20–24. https://www.journalajcrs.com/index.php/AJCRS/article/view/30290
Wilson JM, Aaronson DS, Schrader R, Baskin LS (2008) Hydrocele in the pediatric patient: inguinal or scrotal approach? J Urol 180(4):1724–1727. https://doi.org/10.1016/j.juro.2008.03.111
Esen B, Sarıdemir S, Guleryuz Bolsu G, Doğanözü AC (2020) Encysted spermatic cord hydrocele in adults: a case report and review of the literature. Acta Oncol Tur 53(3):543–546. https://doi.org/10.1080/02841850701553163
Garg KM (2016) Spermatic cord hydrocele in adults: experience of three cases. IOSR J Dent Med Sci 15(11):78–79. https://doi.org/10.9790/0853-1511027879
Schiavenato M, Craig KD (2010) Pain assessment as a social transaction:beyond the ‘“gold standard.”’ Clin J Pain 26(8):667–676. https://doi.org/10.1097/AJP.0b013e3181e72507
Turnage RH, Richardson KA, Li BD, McDonald JC (2021) Abdominal wall, umbilicus, peritoneum, mesenteries, omentum, and retroperitoneum. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL (eds) Sabiston textbook of surgery, 21st edn. Elsevier, Amsterdam, p 1111
Nyhus LM (1993) Iliopubic tract repair of inguinal and femoral hernia. The posterior (preperitoneal) approach. Surg Clin North Am 73(3):487–499. https://doi.org/10.1016/s0039-6109(16)46032-9
Nyhus LM (2003) The posterior (preperitoneal) approach and iliopubic tract repair of inguinal and femoral hernias—an update. Hernia 7(2):63–67. https://doi.org/10.1007/s10029-002-0113-x
Lee SR (2018) Benefits of laparoscopic posterior wall suture repair in treating adolescent indirect inguinal hernias. Hernia 22(4):653–659. https://doi.org/10.1007/s10029-018-1745-9
Lee SR, Park PJ (2021) Adding iliopubic tract repair to high ligation reduces recurrence risk in pediatric laparoscopic transabdominal inguinal hernia repair. Surg Endosc 35(1):216–222. https://doi.org/10.1007/s00464-020-07382-1
Lee SR, Park PJ (2018) Novel transabdominal preperitoneal hernioplasty technique for recurrent inguinal hernia: overlapping of whole posterior wall with newly added mesh and pre-existing mesh by closing hernia defect. J Laparoendosc Adv Surg Tech A 28(12):1503–1509. https://doi.org/10.1089/lap.2018.0325
Lee SR, Park JY (2021) Comparison of laparoscopic transabdominal preperitoneal hernioplasty and laparoscopic iliopubic tract repair for Nyhus type II hernia in women. Surg Endosc 35(12):7260–7266. https://doi.org/10.1007/s00464-021-08739-w
Acknowledgements
The author thanks Hyejin Park for performing the primary English grammar correction of this manuscript, and Beom Seok Oh and Young Hyun Lee from the research center of Damsoyu Hospital for assisting with the statistical analysis and organizing the data in this manuscript. The author also thanks Edanz (https://www.edanz.com/ac) for editing a draft of this manuscript.
Funding
The author declares no source of funding. This research did not receive any specific grant from funding agencies in the public, commercial, or not for profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Sung Ryul Lee has no conflicts of interest or financial ties to disclose.
Ethical approval
This study was approved by the Institutional Review Board of Damsoyu Hospital (DSY-2021-004).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lee, S.R. Laparoscopic hydrocelectomy with transabdominal preperitoneal hernioplasty or iliopubic tract repair for treatment of encysted spermatic cord hydrocele. Surg Endosc 36, 5540–5545 (2022). https://doi.org/10.1007/s00464-022-09285-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09285-9