Abstract
Background
Peroral endoscopic myotomy (POEM) has been described as a novel treatment for esophageal achalasia. Owing to its technical difficulty, POEM is not widely performed. This study was aimed to prospectively assess the factor predicting technical difficulty of POEM in a single center with large volume cases.
Methods
A total of 105 cases of achalasia treated by POEM from April 2011 to September 2014 were analyzed. Difficult cases of POEM were defined as procedure time ≥90 min and occurrence of adverse events, including mucosal perforation, pneumothorax, and major bleeding. Univariate and multivariate logistic regression analyses were performed to assess the predictive factors of difficult POEM.
Results
POEM was successfully completed in all the patients, and no one was converted to laparoscopy. The number of cases with procedure time ≥90 min was 17. Mucosal perforations occurred in six (5.7 %) patients during submucosal tunnel creation, major bleeding occurred in seven (6.7 %) patients, and pneumothorax occurred in six (5.7 %) patients immediately after procedure. All the complications were managed conservatively. No other intraoperative and immediate postoperative complications, including infections and pneumoperitoneum, occurred. Multivariate analysis showed that early period (odds ratio [OR] 4.173, 95 % confidence interval [95 % CI] 1.36–6.829, P = 0.023) and triangular tip knife ([OR] 6.712, [95 % CI] 1.479–30.460, P = 0.014) were independent factors associated with technical difficulty regarding longer procedure time (procedure time ≥90 min).
Conclusion
POEM is safe for the treatment of esophageal achalasia. Triangular tip knife and early period were independent risk factors for longer procedural time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Achalasia is a rare esophageal motility disorder with aperistalsis of the esophageal body and impaired relaxation of lower esophageal sphincter (LES), with an incidence of 5 per 1,000,000 persons per year [1]. The common clinical symptoms include dysphagia, regurgitation, chest pain, and/or loss of weight [2]. Owing to its unknown cause, current treatments focus on destruction or forced relaxation of the LES. Endoscopic pneumatic dilation (PD) and surgical myotomy are the first-line treatments for this disease because of their more lasting effects [3–5]. But these two treatments are limited by complications, such as perforation and bleeding [6, 7]. Additionally, surgical myotomy is invasive and complicated by gastroesophageal reflux (GER), stricture formation, and skin scarring [7].
Recently, a novel endoscopic technique, peroral endoscopic myotomy (POEM), has been developed to treat achalasia with excellent clinical outcomes [8]. Since the first case was performed 6 years ago, the number of POEM procedures performed around the world has reached up to about 500 per year [8]. As a less invasive intervention, POEM allows for cutting the esophageal circular muscle bundle by creating a submucosal tunnel. To date, a number of studies have demonstrated that POEM could achieve a 82–100 % success rate of eliminating dysphagia symptoms [9]. However, only a few centers in the world can perform the procedure because of it being highly technique-demanding. Although several training methods or modes were designed to improve endoscopist’s skill of POEM [10–12], a practical high-level training environment has not been established yet. To improve the safety and outcomes of POEM and the training, it is very crucial to identify the risk factors associated with procedural difficulty.
Teitelbaum et al. [13] revealed that prior endoscopic treatment, longer symptom duration, and esophageal dilatation may result in increased operative difficulty during POEM, but their study was limited by small sample size (36 patients). Therefore, the aim of this study was to prospectively assess the factor predicting technical difficulty of POEM in a large volume of cases.
Materials and methods
Patients
Between April 2011 and September 2014, achalasia patients who underwent POEM were enrolled consecutively in our study. Data were prospectively collected and retrospectively reviewed. The inclusion criteria were symptomatic achalasia confirmed by contrast fluoroscopy, manometry and esophagoduodenoscopy (EGD), and patients’ age greater than 18 years. The exclusion criteria were active esophagitis, esophageal varices, pregnancy, Barrett’s esophagus, esophageal stricture, esophageal malignancy, and liver cirrhosis. Previous endoscopic dilation, a botulinum toxin injection, or laparoscopic Heller myotomy was not considered as exclusion criteria.
This study was approved by the Institutional Review Board of Nanfang Hospital, Southern Medical University. Written informed consent was obtained from all patients.
POEM procedure
Patients were fasted for 24 h before the procedure. POEM was performed under general anesthesia with endotracheal intubation and CO2 insufflation. All POEM procedures were performed by a single operator (W. G.). The steps of the procedure were as described below: firstly, a submucosal injection of 10 ml saline with 0.3 % indigo carmine and 1:100,000 epinephrine was made 6–10 cm above the gastroesophageal junction (GEJ), followed by a 2-cm longitudinal incision using a hybrid knife (ERBE, Tübingen, Germany); secondly, the submucosal layer was dissected to make a tunnel along the esophagus and across GEJ 2–3 cm into proximal stomach; thirdly, myotomy started 4 cm below the mucosal entry and extended 2–3 cm into the proximal stomach, the circular muscle bundle was dissected, and the longitudinal muscle bundle was preserved; finally, the mucosal entry site was closed with hemostatic clips from the distal to the proximal end of the mucosal defect (EZ-CLIP, HX-110QR, Olympus, Tokyo, Japan). Patients were kept fast for 24 h after POEM and on a liquid diet for an additional 24 h. Patients were asked to keep a soft diet and take proton pump inhibitors (PPI) for 2 weeks after discharge.
Variable selection and definition
Difficult cases of POEM were defined as any one of four points: procedure time more than 90 min, or occurrence of adverse events, including mucosal perforation, pneumothorax and major bleeding. Factors predicting difficult POEM were as follows: age, sex, BMI (kg/m2), symptoms duration, pre-POEM Eckardt scores [14], dysphagia scores [15], previous interventions, manometric findings, Chicago classification of achalasia [16], and esophagogram findings. Moreover, the variables of early period and late period were also included. Fifty-four cases of POEM were performed between April 2011 and May 2013 in the early period, while 51 cases were performed between June 2013 and September 2014 in the late period. Mucosal perforation was defined as having occurred when a hole was easily recognizable by endoscopy during POEM. Pneumothorax was confirmed when collapsed lung was detected on a chest X-ray taken after POEM. Major bleeding was defined as an oozing or spurting bleeding observed and requiring the use of coagulating forceps or endoclips.
Statistical analysis
Parametric data are presented as mean ± standard deviation (SD) or median (range), and categorical variables were expressed as numbers and percentages. Univariate and multivariate logistic regression analyses were performed to assess the factors of difficult POEM (procedure time ≥90 min, perforation, pneumothorax, or major bleeding). The method of selecting a variable is the forward stepwise method, and variables with P values for association ≤0.2 on univariate analysis were considered potential risk factors in multivariate analysis. Odds ratios (OR) and 95 % confidence intervals (95 % CI) were calculated to evaluate the predictors of difficult POEM. A P value less than 0.05 was considered statistically significant. Data were analyzed using commercially available statistical software package SPSS version 17.0 (SPSS Inc., Chicago, IL, USA).
Results
Baseline patient characteristics
During the study period, a total of 105 patients received the POEM procedure described above. Baseline and clinical characteristics are shown in Table 1. The mean age of the patients was 38.2 ± 10.7 years (range 18–64). The female-to-male ratio was 52:53, with a mean BMI of 20.3. The median preoperative duration of symptoms was 10 months (range 6–32). Median pre-POEM Eckardt score was 8 (range 4–12). Of the patients, 25 received prior therapy for treating achalasia, in which 22 (21.0 %) patients underwent endoscopic Botox injection and three (2.9 %) had balloon dilatations. Based on high-resolution esophageal manometry (HRM), 38 (36.2 %) were classified as type I achalasia and 67 (63.8 %) as type II achalasia patients. There were no type III achalasia patients in our cases. The mean LES pressure was 40.0 ± 13.8 mmHg (range 20.3–76.3). Esophagogram findings showed mean esophageal width at 5 min was 30.4 ± 10.0 mm. With regard to endoscopic equipments, triangular tip knife was used in 59 (56.2 %) POEM procedures and hybrid knife in 46 (43.8 %) procedures.
Clinical outcomes of POEM
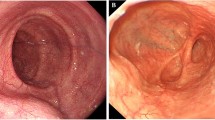
POEM was successfully completed in all the patients, and no one was converted to laparoscopy. Mucosal perforations at cardia occurred in six (5.7 %) patients during submucosal tunnel creation and were successfully managed by endoclips (Fig. 1). Major bleeding occurred in seven (6.7 %) patients and was promptly controlled by a pair of coagulating forceps (Fig. 2). Twelve patients had subcutaneous emphysema in the neck, which resolved spontaneously after the POEM. Six patients experienced a decrease in oxygen saturation during the procedure; X-ray verified the occurrence of pneumothorax in them. The patients were treated with thoracic drainage, and they recovered after chest tube placement for 1 week (Fig. 3). No other intraoperative and immediate postoperative complications such as infections or pneumoperitoneum occurred.
Predictors of technical difficulty: univariate and multivariate analyses
Tables 2 and 3 show the results of univariate and multivariate analyses of factors associated with technical difficulty of POEM . Results for variables meeting the P < 0.05 criteria are shown in bold, and the multivariate analysis results show only the variables with statistical significance.
Based on the results of univariate analysis, endoscopic equipments (triangular tip knife) and procedure period (early period) were significantly associated with longer procedure time (P = 0.011 and P = 0.005, respectively); previous interventions were associated with occurrence of perforation (P = 0.021), and procedure period (early period) was also related to occurrence of major bleeding during the procedure (P = 0.048). There is no variable associated with occurrence of pneumothorax.
Multivariate analysis showed that early period (odds ratio [OR] 4.173, 95 % confidence interval [95 % CI] 1.36–6.829, P = 0.023) and triangular tip knife ([OR] 6.712, [95 % CI] 1.479–30.460, P = 0.014) were independent factors for predicting technical difficulty regarding longer procedure time, while no factor was significantly associated with the occurrence of adverse events (mucosal perforation, pneumothorax, and major bleeding).
Discussion
POEM has been a novel alternative treatment option for esophageal achalasia. This technique enables endoscopists to complete a myotomy of esophageal circular muscle fibers across the esophagogastric junction (EGJ) and into the stomach through a submucosal tunnel. Pasricha et al. [17] initially described the feasibility of this technique in pig model in 2007, and then Inoue et al. [18] firstly reported their experience of performing this treatment method in human beings successfully. Since then, more than 3000 POEM procedures have been performed worldwide with promising clinical outcomes [8]. As POEM continues to gain popularity, many studies focus on its long-term efficacy and safety. But it is also very crucial to identify the risk factors associated with procedural difficulty.
In our present study, we applied this novel treatment in 105 patients of achalasia. In all cases, small mucosal perforation in the cardia occurred in six patients and was successfully closed using endoclips. The incidence of perforation of POEM was not common, as estimated less than 10 % [9]. The perforation rate in our study was 5.7 %, and all of them occurred in the early period. When the endoscopist becomes experienced at the technical skills of POEM in the late period no perforation occurred. Therefore, we think that mucosal perforation can be completely avoided as soon as the operator masters the skills of procedure. For the management of mucosal perforation during POEM, endoclips are widely applied and proved to be useful. While in the setting of large mucosal perforation or endoclips failed to close the defect, other treatments have been described. Li et al. [19] reported two cases of cardiac mucosal penetration managed with fibrin sealant when hemostatic clips failed to seal the defect. Saxena et al. [20] successfully used over-the-scope clips to close large esophageal mucosal flaps in two patients after inability to initially close the mucosal defect using standard clips. Ling et al. [21] also described closure of a 2-cm mucosal flap rupture at the lower esophagus using a retrievable nickel-titanium stent to reduce the risk of restenosis. Therefore, mucosal perforation in POEM can be managed easily by endoscopic method, and its incidence decreases as operator becomes more experienced.
Major bleeding and pneumothorax occur infrequently during the procedure. Just like the occurrence of mucosal perforation, both of the complications were also encountered in the early period of POEM cases. In the multivariate analysis, early period was a significant predictor for the complication of major bleeding and pneumothorax. In our patients, seven suffered major bleeding due to cutting the artery accidentally during creation of submucosal tunnel, and the submucosal oozing was controlled successfully by a pair of coagulating forceps. In case of bleeding spot not being identified, some investigators reported the use of the tip of the endoscope in natural lumen to compress the tunnel at the bleeding site for 10–20 min [22] and temporary hemostasis can be achieved. As to the complication of pneumothorax, it occurred in six patients. In contrast to our findings, Zhou and colleagues showed a high incidence of POEM-related pneumothorax complications (25.2 %, 30/119) in their study [23]. In addition to that, they also demonstrated that the rate of other postoperative complications, including subcutaneous emphysema (55.5 %, 66/119), mediastinal emphysema (29.4 %, 35/119), pleural effusion (48.7 %, 58/119), and pneumoperitoneum (39.5 %, 47/119), was much higher than our results and other reports [24]. The reason for the above discrepancy of complication rate may be related to the use of air or CO2 insufflation during POEM. In Zhou’s report, room air insufflation was used in all the procedures, while in our trial, CO2 insufflation was applied in all cases. CO2 insufflation is safe, is quick absorptive, and decreases intra-procedural pain, post-procedural pain, and recovery time [25], and it can also reduce the risk of mediastinal emphysema and air embolization. Endoscopic CO2 insufflation has been recommended as a routine tool in POEM procedure [9].
Botox injection and PBD are the primary endoscopic therapeutic options for achalasia, but these treatments are limited by short-term solutions requiring repetitive applications or are simply ineffective [26]. Submucosal fibrosis around the LES resulting from prior Botox injection and PBD is the main concern for POEM procedure, which may make creation of the submucosal tunnel technically difficult, even unsafe. Beckingham et al. [27] reported a 30 % complication of mucosal perforation during Heller myotomy for patients who had symptoms recurrence after balloon dilatation. Smith et al. [28] also indicated a twofold or higher rate of intraoperative and postoperative complications in a large series of patients undergoing Heller myotomy after prior endoscopic therapy compared to patients with no prior therapy. In our cases, 25 patients received prior endoscopic interventions (Botox injection or PBD). The incidence of perforation in these patients (16 %, 4/25) was much higher than in patients (2.5 %, 2/80) without previous treatment. However, multivariate analysis demonstrated that previous interventions were not an independent risk factor for procedural difficulty, including longer operation time and occurrence of complication. Based on several studies, it appears that no evidence suggests prior Botox injection or PBD affects the efficacy or complication risk of a subsequent POEM procedure [29, 30]. So previous endoscopic interventions were not a significant factor associated with technical difficulty of POEM.
Procedure time is a common measurement used to assess surgical learning curves [31], and Kurian et al. [32] reported a modest reduction in the procedure time with the increase in POEM experience. But Teitelbaum et al. [13] suggested that overall procedure time did not decrease with experience in a series of 36 POEM procedures. We found a decrease in length of procedure in the late period, and early period was an important factor predicting longer procedure time. Based on data from a single-center, single-operator series of 93 POEMs, Patel et al. [33] concluded that skill efficiency is achieved after 40 procedures and mastery after 60 procedures. Our results are similar to Patel’s finding. After performing 54 cases of POEM in early period, subsequent POEM procedures in late period become less technique-demanding with shorter procedural time and safer presenting with few adverse events.
Although one of the strengths of this trial was our prospectively collected large sample size, we acknowledge there are several limitations in our study. Firstly, all procedures in this series were performed by a single operator in a single center, so the results may not be generalizable. Future studies conducted in multiple centers by a number of operators are warranted to clearly define the predictor for technical difficulty of POEM.
In conclusion, POEM is effective for the treatment of achalasia, with a low complication rate. We found that triangular tip knife and early period were important risk factors for longer procedural time. Our finding may facilitate development of training strategy for POEM procedure and decreasing the occurrence of complication in clinical practice.
References
Richter JE (2010) Achalasia—an update. J Neurogastroenterol Motil 16(3):232–242
Boeckxstaens GE, Zaninotto G, Richter JE (2014) Achalasia. Lancet 383(9911):83–93
Triadafilopoulos G, Boeckxstaens GE, Gullo R, Patti MG, Pandolfino JE, Kahrilas PJ, Duranceau A, Jamieson G, Zaninotto G (2012) The Kagoshima consensus on esophageal achalasia. Dis Esophagus 25(4):337–348
Boeckxstaens GE, Annese V, des Varannes SB, Chaussade S, Costantini M, Cuttitta A, Elizalde JI, Fumagalli U, Gaudric M, Rohof WO, Smout AJ, Tack J, Zwinderman AH, Zaninotto G, Busch OR, European Achalasia Trial I (2011) Pneumatic dilation versus laparoscopic Heller’s myotomy for idiopathic achalasia. N Engl J Med 364(19):1807–1816
Richter JE, Boeckxstaens GE (2011) Management of achalasia: surgery or pneumatic dilation. Gut 60(6):869–876
Karamanolis G, Sgouros S, Karatzias G, Papadopoulou E, Vasiliadis K, Stefanidis G, Mantides A (2005) Long-term outcome of pneumatic dilation in the treatment of achalasia. Am J Gastroenterol 100(2):270–274
Kilic A, Schuchert MJ, Pennathur A, Gilbert S, Landreneau RJ, Luketich JD (2009) Long-term outcomes of laparoscopic Heller myotomy for achalasia. Surgery 146(4):826–831 discussion 831–823
Bechara R, Ikeda H, Inoue H (2015) Peroral endoscopic myotomy: an evolving treatment for achalasia. Nat Rev Gastroenterol Hepatol 12(7):410–426
Committee NPWP, Stavropoulos SN, Desilets DJ, Fuchs KH, Gostout CJ, Haber G, Inoue H, Kochman ML, Modayil R, Savides T, Scott DJ, Swanstrom LL, Vassiliou MC (2014) Per-oral endoscopic myotomy white paper summary. Gastrointest Endosc 80(1):1–15
Eleftheriadis N, Inoue H, Ikeda H, Onimaru M, Yoshida A, Hosoya T, Maselli R, Kudo SE (2012) Training in peroral endoscopic myotomy (POEM) for esophageal achalasia. Ther Clin Risk Manag 8:329–342
Bang BW, Choi YC, Kim HG, Kwon KS, Shin YW, Lee DH, Kim JM (2013) Peroral endoscopic myotomy for treating achalasia in an animal model: a feasibility study. Clin Endosc 46(1):54–58
Chiu PW, Wu JC, Teoh AY, Chan Y, Wong SK, Liu SY, Yung MY, Lam CC, Sung JJ, Chan FK, Lau JY, Ng EK (2013) Peroral endoscopic myotomy for treatment of achalasia: from bench to bedside (with video). Gastrointest Endosc 77(1):29–38
Teitelbaum EN, Soper NJ, Arafat FO, Santos BF, Kahrilas PJ, Pandolfino JE, Hungness ES (2014) Analysis of a learning curve and predictors of intraoperative difficulty for peroral esophageal myotomy (POEM). J Gastrointest Surg 18(1):92–98 (discussion 98–99)
Gockel I, Junginger T (2007) The value of scoring achalasia: a comparison of current systems and the impact on treatment–the surgeon’s viewpoint. Am Surg 73(4):327–331
Kochman ML, McClave SA, Boyce HW (2005) The refractory and the recurrent esophageal stricture: a definition. Gastrointest Endosc 62(3):474–475
Bredenoord AJ, Fox M, Kahrilas PJ, Pandolfino JE, Schwizer W, Smout AJ, International High Resolution Manometry Working G (2012) Chicago classification criteria of esophageal motility disorders defined in high resolution esophageal pressure topography. Neurogastroenterol Motil 24(Suppl 1):57–65
Pasricha PJ, Hawari R, Ahmed I, Chen J, Cotton PB, Hawes RH, Kalloo AN, Kantsevoy SV, Gostout CJ (2007) Submucosal endoscopic esophageal myotomy: a novel experimental approach for the treatment of achalasia. Endoscopy 39(9):761–764
Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, Satodate H, Odaka N, Itoh H, Kudo S (2010) Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy 42(4):265–271
Li H, Linghu E, Wang X (2012) Fibrin sealant for closure of mucosal penetration at the cardia during peroral endoscopic myotomy (POEM). Endoscopy 44(Suppl 2 UCTN):E215–E216
Saxena P, Chavez YH, Kord Valeshabad A, Kalloo AN, Khashab MA (2013) An alternative method for mucosal flap closure during peroral endoscopic myotomy using an over-the-scope clipping device. Endoscopy 45(7):579–581
Ling T, Pei Q, Pan J, Zhang X, Lv Y, Li W, Zou X (2013) Successful use of a covered, retrievable stent to seal a ruptured mucosal flap safety valve during peroral endoscopic myotomy in a child with achalasia. Endoscopy 45(Suppl 2 UCTN):E63–E64
Phalanusitthepha C, Inoue H, Ikeda H, Sato H, Sato C, Hokierti C (2014) Peroral endoscopic myotomy for esophageal achalasia. Ann Transl Med 2(3):31
Ren Z, Zhong Y, Zhou P, Xu M, Cai M, Li L, Shi Q, Yao L (2012) Perioperative management and treatment for complications during and after peroral endoscopic myotomy (POEM) for esophageal achalasia (EA) (data from 119 cases). Surg Endosc 26(11):3267–3272
Yang D, Wagh MS (2013) Peroral endoscopic myotomy for the treatment of achalasia: an analysis. Diagn Ther Endosc 2013:389596
Yasumasa K, Nakajima K, Endo S, Ito T, Matsuda H, Nishida T (2006) Carbon dioxide insufflation attenuates parietal blood flow obstruction in distended colon: potential advantages of carbon dioxide insufflated colonoscopy. Surg Endosc 20(4):587–594
Eckardt AJ, Eckardt VF (2011) Treatment and surveillance strategies in achalasia: an update. Nat Rev Gastroenterol Hepatol 8(6):311–319
Beckingham IJ, Callanan M, Louw JA, Bornman PC (1999) Laparoscopic cardiomyotomy for achalasia after failed balloon dilatation. Surg Endosc 13(5):493–496
Smith CD, Stival A, Howell DL, Swafford V (2006) Endoscopic therapy for achalasia before Heller myotomy results in worse outcomes than Heller myotomy alone. Ann Surg 243(5):579–584 (discussion 584–576)
Sharata A, Kurian AA, Dunst CM, Bhayani NH, Reavis KM, Swanstrom LL (2013) Peroral endoscopic myotomy (POEM) is safe and effective in the setting of prior endoscopic intervention. J Gastrointest Surg 17(7):1188–1192
Ling T, Guo H, Zou X (2014) Effect of peroral endoscopic myotomy in achalasia patients with failure of prior pneumatic dilation: a prospective case-control study. J Gastroenterol Hepatol 29(8):1609–1613
Ramsay CR, Grant AM, Wallace SA, Garthwaite PH, Monk AF, Russell IT (2000) Assessment of the learning curve in health technologies. A systematic review. Int J Technol Assess Health Care 16(4):1095–1108
Kurian AA, Dunst CM, Sharata A, Bhayani NH, Reavis KM, Swanstrom LL (2013) Peroral endoscopic esophageal myotomy: defining the learning curve. Gastrointest Endosc 77(5):719–725
Patel KS, Calixte R, Modayil RJ, Friedel D, Brathwaite CE, Stavropoulos SN (2015) The light at the end of the tunnel: a single-operator learning curve analysis for per oral endoscopic myotomy. Gastrointest Endosc 81(5):1181–1187
Acknowledgments
This study was supported by the grant from the National Natural Science Foundation of China (No. 81101610), Scientific Research Projects of Guangdong Province (No. 2013B021800311), and Medical Research Foundation of Guangdong Province (No. WSTJJ2011110142092192119760913465X).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Xiaowei Tang, Yutang Ren, Zhengjie Wei, Zhiliang Deng, Jieqiong Zhou, Zhenyu Chen, Bo Jiang, and Wei Gong have no conflicts of interest or financial ties to disclose.
Additional information
Xiaowei Tang and Yutang Ren have contributed equally to this article.
Rights and permissions
About this article
Cite this article
Tang, X., Ren, Y., Wei, Z. et al. Factors predicting the technical difficulty of peroral endoscopic myotomy for achalasia. Surg Endosc 30, 3774–3782 (2016). https://doi.org/10.1007/s00464-015-4673-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-015-4673-0