Abstract
The study aims to transdifferentiate rat bone marrow–derived mesenchymal stem cells (BM-MSCs) more efficiently into islet-like cells and encapsulate and transplant them with vital properties like stability, proliferation, and metabolic activity enhanced for the treatment of T1DM. Trans-differentiation of BM-MCs into islet-like cells induced by high glucose concentration combined with Nicotinamide, ꞵ-Mercaptoethanol, ꞵ-Cellulin, and IGF-1. Glucose challenge assays and gene expression profiles were used to determine functionality. Microencapsulation was performed using the vibrating nozzle encapsulator droplet method with a 1% alginate concentration. Encapsulated ꞵ-cells were cultured in a fluidized-bed bioreactor with 1850 μL/min fluid flow rates and a superficial velocity of 1.15 cm/min. The procedure was followed by transplanting transdifferentiated cells into the omentum of streptozotocin (STZ)-induced diabetic Wistar rats. Changes in weight, glucose, insulin, and C-peptide levels were monitored for 2 months after transplantation. PDX1, INS, GCG, NKx2.2, NKx6.1, and GLUT2 expression levels revealed the specificity of generated β-cells with higher viability (about 20%) and glucose sensitivity about twofold more. The encapsulated β-cells decreased the glucose levels in STZ-induced rats significantly (P < 0.05) 1 week after transplantation. Also, the weight and levels of insulin and C-peptide reached the control group. In contrast to the treated, the sham group displayed a consistent decline in weight and died when loss reached > 20% at day ~ 55. The coated cells secrete significantly higher amounts of insulin in response to glucose concentration changes. Enhanced viability and functionality of β-cells can be achieved through differentiation and culturing, a promising approach toward insulin therapy alternatives.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In Type 1 Diabetes Mellitus (T1DM), insulin-producing pancreatic cells are destroyed by an autoimmune process. T1DM could be cured by replacing lost insulin-secreting cells with functional ones like those lost during the process (Yoon and Jun 2005). Attaining insulin levels comparable to those of mature β-cells has been attempted using various tissue sources and differentiation techniques. Recent studies have suggested PDX1, PAX4, Nkx2.2, and NKX6.1 as essential transcription factors for β-cell development, facilitating the direct differentiation of precursor cells into insulin-producing β-cells. Many protocols have been modified to enhance β-cell differentiation (Wang and Zhang 2021). Repetition of in vivo signals that regulate the tissue microenvironment of the endocrine pancreas is a potential approach for β-cell generation (Huang et al. 2020). However, the critical issue is stem cells’ effective and repeatable differentiation into functional insulin-secreting β-cells (Silva et al. 2022).
As proof of principle, replacement therapy using deceased donor islets has been demonstrated to restore normoglycemia and insulin independence in patients. The lack of donors, variability in their islets quality, and the requirement of lifelong systemic immunosuppression have limited the development of this treatment (Rickels and Robertson 2019). Several studies have evaluated the safety of microencapsulating pancreatic islets in alginate to avoid the need for immunosuppression (de Vos et al. 2006; Alagpulinsa et al. 2019). Maintaining normoglycemia is challenging, even with regular monitoring of blood glucose levels, and this is true even though the introduction of exogenous insulin has increased the lifespan of people with diabetes (Lysy et al. 2012). Long-term consequences in these people include blindness and kidney disease due to hypoglycemia (low blood glucose) and hyperglycemia (high blood glucose) (Amorim et al. 2019). Therefore, encapsulating pancreatic insulin-secreting β-cells in a semipermeable polymeric membrane is a promising alternative for blood glucose regulation. This would allow for the bidirectional diffusion of oxygen, nutrients, insulin, and other cell products while providing an immune-isolated environment to protect pancreatic β-cells from cytokines and T-cells (Barkai et al. 2016).
Although numerous research efforts into cell transplantation are utilizing microencapsulating technology, their clinical application has been hampered by several difficulties, such as inadequate nutrition transfer and a lack of a storage technique for maintaining encapsulated cells before transplantation (Zhang et al. 2022). Bioreactors are a potentially helpful approach to the problem of transferring physiological quantities of encapsulated cells from a lab to a clinical setting for testing and treatment. Compared to flask-based culture methods, bioreactors’ contamination risk is much lower, allowing easier clinical accessibility. Due to fewer medium changes, these devices are more cost-effective for cell-based therapeutic investigations than standard flasks (Anane et al. 2021).
In this study, we differentiated bone marrow mesenchymal stem cells (BM-MSCs) to ꞵ-cells using growth and tropic factors affection on the tissue microenvironment in culture conditions to achieve alginate microcapsules with uniform size and shape; a vibrating nozzle system was used to obtain the microcapsules. The cultivation of alginate-encapsulated mature ꞵ-cells was applied using a fluidized-bed bioreactor, and viability and insulin secretion ability was evaluated. After transplanting ꞵ-cell microcapsules, the transplant results were assessed within 2 months.
Materials and methods
Twenty-two male Wistar rats weighing 200 ± 20 g and 2–3 months of age were used in this study. Cell culture medium L-DMEM, HDMEM, and FBS were purchased from GIBCO™, USA. The FGF, Trypsin–EDTA, Nicotinamide, β-Mercaptoethanol, β-Cellulin, and IGF-1 were obtained from Sigma-Aldrich, USA.
BM-MSCs extraction
Bone marrow–derived mononuclear cells (MNCs) were isolated from sacrificed by cervical dislocation in a 6-month-old male Wistar rat. Under sterile conditions, the tibias and femurs were dissected. After cutting the metaphyseal ends of the bones, L-DMEM was passed through a needle inserted into one end of the bone to flush the marrow plugs. Rat bone marrow was diluted with normal saline at a ratio of 1:1. Gradient centrifugation using 1.073 g/mL Ficoll at 1500 rpm for 30 min was used to obtain the fraction of the MNCs. Hemocytometers were used to count the cells after they had been rinsed twice with normal saline.
Trans-differentiation process
In brief, the mesenchymal stem cells (MSCs) were seeded in polystyrene T25 culture flasks that were not coated with proteins and incubated at 37 °C in a humid 5% CO2 incubator for 48 h in a complete medium containing L-DMEM, FBS (10%), penicillin (100 IU/mL), streptomycin (100 IU/mL), gentamycin (50 IU/mL), amphotericin B (2.5 μg/mL) and FGF (10 ng/mL). After discarding non-adherent cells, adherent cells were cultured in a complete medium for 10 days, with the medium being replaced every 3 days. In T75 flasks, cells were trypsinized with Trypsin–EDTA and passaged until 70–90% confluency was achieved in the second generation of cells. MSCs were characterized into functional ꞵ-cells from bone marrow following differentiation (Koppula et al. 2009; Yamazaki et al. 2020).
The first step in the differentiation process was to pre-stimulate MSCs with L-DMEM supplemented with Nicotinamide (10 mmol/L), β-Mercaptoethanol (2.5 mmol/L), and FBS (5%) for 24 h to eliminate nestin-negative cells. A second step involved re-stimulating cells with Nicotinamide (10 mmol/L) and β-Mercaptoethanol (2 mmol/L) for ten additional hours to induce their differentiation into premature islets. To maintain the islet-like clusters of premature ꞵ-cells in long-term culture, IGF-1, and ꞵ-Cellulin at concentrations of 10 ng/mL in a serum-free culture medium were added for 3 weeks to obtain mature, insulin-secreting ꞵ-cells. We have employed control cells induced without incorporating Nicotinamide, β-Mercaptoethanol, IGF-1, or ꞵ-Cellulin (Wang et al. 2012; Alessandra et al. 2020).
qPCR performance
Total cellular RNA was extracted from mature pancreatic ꞵ-cell using TRIzol reagent (Invitrogen) according to the manufacturer’s instructions. Reverse transcription reactions were performed with total RNA ≥ 20 ng/μl using the RevertAID™ First Strand cDNA synthesis kit (Thermo Fisher Scientific), following the manufacturer’s instructions. Real-time PCR was conducted using a 2 μl sample of single-stranded cDNA and the SYBR Green PCR master mix (QIAGEN). Table 1 provides the applied sequences of the primers and annealing temperature (Kutlu et al. 2009). The relative gene expression levels were calculated, and GAPDH was used as an endogenous control to normalize gene expression in the samples.
Encapsulation process
Alginate with medium viscosity was dissolved in sterile deionized water at a ratio of 1%w/v, and 100-mM granular calcium chloride was dissolved in deionized water to prepare the cross-linking solution. With the assistance of the Trypsin–EDTA solution, the cells were detached from the culture flask. After being washed in PBS, 1 × 106 cells were suspended per 1 mL of the sterile alginate solution. Microcapsules were formed using the vibrational B-395 pro encapsulator (Buchi, UK) by optimized processing parameters. A bath of 100 mM CaCl2 was then used to incubate the newly formed microparticles for 10 min. Following gelation, a two-step wash of PBS and DMEM was performed to ensure that calcium ions were removed from the encapsulated particles.
The differentiated cells were cultured using fluidized culture involving DMEM supplemented with 15% FBS, 2 mM L-glutamine, and 0.05 mM β-Mercaptoethanol. β-Mercaptoethanol has been added to maintain and reduce environmental oxidative stress in the cell culture medium, thereby limiting the formation of toxic oxygen radicals. The bioreactor with 1850 μL/min fluid flow rates (superficial velocity of 1.15 cm/min) was incubated at 37 °C with 5% CO2 until encapsulated ꞵ-cells reached 70–80% confluency. Cell growth and viability were enhanced by changing the culture medium every other day (Nikravesh et al. 2017). The viability of micro-encapsulated β-cells was assayed using a live/dead cytotoxicity kit (Invitrogen), and the procedures were done based on the kit protocol.
GSIS assay
The functionality of ꞵ-cells was evaluated by measuring the secreted amount of insulin from encapsulated cells in response to changes in glucose. Briefly, we washed and pre-incubated samples with 1 × 106 cells/mL in Krebs–Ringer bicarbonate buffer (KRBH) before plating with 0.1% BSA for 2 h. Subsequently, samples were incubated for 1 h with 2 mM and 20 mM glucose concentrations. An enzyme-linked immunosorbent assay (ELISA) kit (BioVendor, Brno, Czech Republic) was used to determine the amount of insulin secreted in low and high-glucose solutions. Control cells were tested during the same period. A CCK-8 cell counting kit (Dojindo, Japan) was used to normalize the results to compensate for size variation.
Transplant process
Adapted versions of the standard procedure were used to create diabetic animal models. We injected 50 mg/L streptozotocin (STZ) intravenously into 14 Wistar rats through their caudal veins and assessed glucose levels a week later using Roche ACCU-CHEK glucose tests (Mannheim, Germany). Two animals did not develop diabetes, one died, and three reverted to normal. Consequently, the glucose-controlling functionality of ꞵ-cells was evaluated using five rats in the treatment group and three in the sham (untreated) group.
Based on the previously reported data, a consensus dose and route were adopted for experiment. Encapsulated ꞵ-cells (93.42 ± 7% viability and 1 × 106 cell density) were administered in the peritoneum at about 0.5 mL with saline as the medium in each rat. In the sham group, saline was the only treatment administered. Approximately 2 months after treatment, insulin, C-peptide, glucose, and weight levels were measured.
Statistical analyses
Results are presented as mean ± standard error of the mean unless otherwise stated. A one-way and two-way ANOVAs were performed to identify significant differences between pairs of groups, assuming equal variance (GraphPad Prism v9.3.1). In addition, Turkey’s multiple comparison tests and non-parametric Mann–Whitney test for comparison with the control group were performed if the analysis of variance delivered a p-value < 0.05.
Results
Gene expression
The expression level of the PDX1 gene, which is involved in the endodermal germ line and an inductor gene of embryonic pancreas development, Insulin and Glucagon as the pancreas genes, GLUT2 in glucose transporter, NKX6.1 in functional and proliferation, and NKx2.2 in regulatory and function of mature ꞵ-cell were studied in BM-MSCs transition to ꞵ-cells. Changes in relative expression by qPCR of the genes above at specific maturation stages (0, 7, 14, and 21 days of differentiation) are summarized in Fig. 1.
Median relative gene expression levels of pancreatic transcription factors such as PDX1, endocrine markers, insulin, glucagon, and β-cells specific genes like NKx2.2, NKx6.1, and GLUT2 were analyzed for control cells gene name-C and differentiated cell with microenvironmental factors gene name-T at each stage of differentiation. The transcript value is shown in each graph as mean ± SEM
On day 0, the expression levels of GCG, PDX1, and GLUT2 genes are low in undifferentiated cells (Fig. S1). The expression levels of the specific markers on day 0 (Fig. S2) and their morphology (Fig. S3) were also examined to the characteristics of the isolated cells. Figure 1 demonstrates that on the first day of differentiation, cells expressed a negligible amount of INS and PDX1 (0.03-fold) in comparison to glucagon (1.17-fold), GLUT2, NKx6.1, and NKx2.2 (0.52-fold). INS gene was expressed on day 1 like PDX1; then significantly increased on days 7 and 14 and peaked at day 21 (96.1-fold) like glucagon (42.3-fold). Other genes (PDX1, GLUT2, and NKx6.1) exhibited a slight increase from day 7 to day 14 and decreased from day 14 to the end of the differentiation protocol. Approximately one-fold expression of NKx2.2 was observed on day 1, followed by downregulation (0.08-fold) on day 7, an increase (0.35-fold) on day 14, and a subsequent decrease (0.17-fold) on day 21. Also, Fig. 1 reveals the 0.05-fold expression level of INS and PDX1, 1.23-fold glucagon, and 1.14-fold for GLUT2, NKx6.1, and NKx2.2 on the first day. INS significantly increased on days 7 and 14 and reached its peak on day 21 (182.3-fold), as to glucagon (72.4-fold). Other genes, such as those found in control cells, underwent comparable variations until the end of the experiment.
Characterization of microcapsules
The ꞵ-cells alginate microcapsules manufactured using the optimized vibrating nozzle method exhibited an average diameter of 204 μm and about 7.6% relative standard deviation (Fig. 2a). Light micrograph imaging also helps visualize encapsulated ꞵ-cell location within the alginate matrix (Fig. 2b–e). ꞵ-cells were distributed homogeneously between the core and the inner surface of alginate hydrogels. Statistically significant differences in microparticle diameter were observed from day 7 to 14 versus day 0 (* P = 0.035, **P = 0.027).
Produced spherical alginate microcapsules a Average alginate microcapsules diameters and relative standard deviations; (n = 30), *, ** P < 0.05 by Turkey`s multiple comparison tests after one-way ANOVA with P < 0.05. b Light micrographs of ꞵ-cells embedded within microcapsules cultured on days initial, c 7, d 14, and e 21 of culture
Live/dead assay
Figure 3 reveals a two-dimensional micrograph of alginate microcapsules containing fluorescently stained live/dead β-cells on various days with a cell density of 1 × 106 that were positive for calcein-AM in differentiated and control cells (93.42% and 67.78% on day 7 and 87.48% and 69.49% on day 14 respectively). Transdifferentiated cells exhibited higher viability (* p = 0.03, **, *** p = 0.02) when compared with the control cells in separated days.
Quantitative evaluation of encapsulated ꞵ-cell viability. Merged a"- f" and unmerged two-dimensional confocal micrograph showing live a-f /dead a′-f′ cells within an alginate microcapsule group overlaid (calcein-AM markers: green channel/PI marker: red channel). g The cells viability and relative standard deviations; (n = 10 capsules), (* P < 0.05 Transdifferentioated cells versus Control cells on day 0, ** P < 0.05 Transdifferentioated cells versus Control cells on day 7, *** P < 0.05 Transdifferentioated cells versus Control cells on day 14 by Turkey’s multiple comparison tests after one-way ANOVA with P < 0.05.) (Scale bars = 200 μm)
GSIS assay
Insulin secretion in response to changes in glucose concentration was assessed using the GSIS assay in in vitro conditions. Figure 4a indicates that differentiated cells secreted significantly more insulin at 2 and 20 mM glucose concentrations (P < 0.001) than control cells on the first and day 7 [(32.2 ng/mL ± 3.5 and 103.04 ng/mL ± 9.7) (SI = 1.4) and (48.4 ng/mL ± 8.7 and 174.4 ng/mL ± 12.4) (SI = 3.3)], exhibiting higher insulin sensitivity. Figure 4b depicts a minimal change in the stimulated index through day 32, suggesting the functional stabilization of cells.
Evaluation of the metabolic activity of ꞵ-cells a Normalized insulin secretion has been calculated based on insulin releases from 1000 cells; analyses are represented by mean ± SEM (n = 4), *,** P < 0.05 versus Control cells by non-parametric Mann–Whitney test for comparison with the control group after two-way ANOVA with P < 0.05. b Stimulation index of encapsulated cells on days 7, 14, 21, 28, and 32; SI value shows the ratio between high glucose and basal glucose (* P < 0.05)
Transplant evaluation
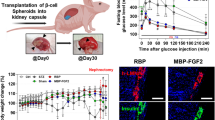
In hosts receiving transplant recipients, levels of glucose decreased significantly (P < 0.05) compared to the sham group from day 7 and remained until 60 days of post-implantation (Fig. 5a) (Table 2). Initially, the treated group lost weight for up to 15 days but then gained weight ranging up to 20% (Fig. 5b); conversely, the sham group carried on losing weight. The mean weights of the treated group were significantly higher than the sham (P < 0.01) (Table 3). The treated group remained healthy and were diarrhea-free. In the treated group, insulin (Fig. 5c) and C-peptide (Fig. 5d) levels became measurable 1 week after transplantation and reached the level of the control group at the end of this experiment.
Discussion
It has long been demonstrated that the encapsulation of living cells in polymeric carriers can facilitate cell-based therapies by providing significant benefits for autoimmune diseases such as T1DM since these approaches may mask the encapsulated cells from the immune system of the host (Ben-Akiva et al. 2018).
Nicotinamide and ꞵ-Mercaptoethanol were used to induce the pre-induction stage of differentiation in endocrine glands from bone marrow progenitor cells. As a morphogen, Nicotinamide may induce chromatin rearrangements and changes in gene transcription by inhibiting poly(ADP-ribose) synthase (Otonkoski et al. 1993; Vaca et al. 2008). Nicotinamide and ꞵ-Mercaptoethanol can regulate mature progenitor cells with the islet microenvironment at high glucose concentrations as suppressors of the Notch pathway (Kim and Choe 2011). GLUT2 is essential to maintaining ꞵ-cell homeostasis and Pdx-1 is crucial in activating the insulin gene in the nucleus. Pdx-1 is expressed by approximately 90% of ꞵ-cells and 15% of ꞵ-cells in mature islets (Moulis et al. 2022). These markers are thus helpful for assessing the function of ꞵ-cells based on their expression. The dual role of Pdx-1 in maintaining pancreatic cell function (Pavathuparambil et al. 2019; Zhang et al. 2021), as demonstrated by qPCR results, suggests that Pdx-1 serves both as an endocrine factor during embryogenesis and as a physiological regulator of pancreatic cells. NKx6.1 and NKx2.2 were the genes whose expression increased on day 14 compared to day 0 and correlated with a decrease in late differentiation, which agrees with studies that revealed its critical role in the development of pancreatic cells (Aigha and Abdelalim 2020). The obtained result in Fig. 1 showed almost the same expression pattern in control and differentiated cells. However, the level of gene expression in differentiated cells was significantly higher, indicating the increased ability of differentiated cells.
A vibrating nozzle technology was utilized to encapsulate differentiated ꞵ-cells in 1% alginate microparticles using a laminar fluid jet which naturally breaks into droplets at a specific frequency, causing the nozzle to break up nearly twice as large (Mooranian et al. 2021). The vibrating nozzle encapsulation process was simple, fast (∼5 min to encapsulate 10 mL of cell suspension in the polymer), and generated well-defined microdroplets of reasonably uniform diameter throughout the process (Costa and Mano 2017). The pH and room temperature were maintained constantly throughout the encapsulation process (Pentela et al. 2019). The experimental parameters were optimized based on preliminary studies, including polymer flow rate, vibration frequency, polymer concentration, cross-linking solution, and hardening time. Optimizing these parameters resulted in the generation of spherical microparticles with an average diameter of 204 μm ± 27 when using a 1%w/v alginate solution (Fig. 2a, b–e). Due to oxygen limitations and hypoxia, the formation of microcapsules with appropriate diameters (> 300 μm) is critical (Schweicher et al. 2014; Mooranian et al. 2021; Wang et al. 2021). This study’s manufacturing of cellular microcapsules provided a potential opportunity to apply a fluidized-bed bioreactor.
There is evidence that fluid bed bioreactors contribute significantly to the high viability of capsulated β-cells in fluid culture. Comparing our results with other studies, the bioreactor did not adversely affect β-cell viability (Coward et al. 2009; Mendonca da Silva et al. 2020). Alamar-blue spectrophotometry tests were performed at different time intervals to determine the viability and metabolic activity of β-cells encapsulated in alginate 1% w/v hydrogel (Eilenberger et al. 2018). Notably, obtained results from the GSIS assay on day 1 versus 7 showed that the value of the insulin-stimulated index exhibited an increasing trend to 3.4. Moreover, encapsulated islets continued to secrete encouraging insulin, not only functional but proliferated to form a three-dimensional tissue around the islets, suggesting that seeding islets with such cells transduced to secrete hormones improve the lifespan and function of the encapsulated islet (Aamodt and Powers 2017; Wassmer et al. 2020). By demonstrating a secretion index more significant than one, we showed that encapsulated β-cells could accommodate changes in glucose concentration during the GSIS assay. However, in contrast to the in vivo study, our long-term in vitro study revealed a significant decrease in the secretory capacity of the encapsulated β-cells after 2 weeks, followed by a slight increase by day 28 and a further reduction in insulin secretion after that; different physiological conditions in vivo may contribute to this difference.
The mature form of insulin is released from the endoplasmic reticulum after exposure to several specific endopeptidases, and its C-peptide is removed (Omar-Hmeadi and Idevall-Hagren 2021). A secretory granule containing insulin and free C-peptide accumulates in the cytoplasm of cells within the Golgi. Glucose responsiveness is the gold standard for determining ꞵ-cell function. Differentiated islets release an appropriate amount of insulin in response to different levels of glucose in the environment (Burns et al. 2004; Silva et al. 2022). Our glucose challenges and animal experiments confirmed insulin release from pancreatic ꞵ-cells, where C-peptide and mature insulin are found in equal molar proportions and with the same secretory granules (Rohli et al. 2022).
Even though the STZ-induced diabetic model could not consistently attain normoglycemia, transplanted islets provided a significant therapeutic effect. The glucose levels of diabetic rats treated significantly decreased (Fig. 5a), but normoglycemia lasted less than 3 months; this suggests that implanted islets provide therapeutic benefits despite sustained elevated glucose. However, diabetes induced by STZ treatment is a markedly less severe disease than that associated with diabetic rats (Wei et al. 2003; Furman 2015). The untreated group rapidly lost weight and died 55 days after, when > 20% weight loss occurred (Fig. 5b). To simulate the prospective therapy more accurately for T1DM children, who are often diagnosed after the beginning of the illness, we opted to administer islets to rats after the development of diabetes to achieve normoglycaemia.
Conclusion
We successfully differentiated BM-MSCs into more functional β-cells and formed uniform-sized and shaped spheroids in vitro using a construct based on alginate. This construct enables the formation of 3D spheres that may be easily harvested. Increased insulin sensitivity to changes in glucose concentration, improved microparticle shape, and high viability were all achieved. An analysis of post-transplantation outcomes showed that the reported differentiation and encapsulation approach enhanced the glucose response, survival, and function of pancreatic ꞵ-cells. ꞵ-cells retain their metabolism and viability during this step of differentiation and maturation. In addition to having a longer lifespan than non-coated cells, coated pancreatic ꞵ-cells responded more rapidly to external glucose fluctuations. A more effective differentiation method, combined with ꞵ-cell coating, proved promising immunotherapy. As well as treating T1DM, these approaches could also be used to treat other endocrine disorders.
References
Aamodt KI, Powers AC (2017) Signals in the pancreatic islet microenvironment influence beta-cell proliferation. Diabetes Obes Metab 19(Suppl 1):124–136
Aigha II, Abdelalim EM (2020) NKX6.1 transcription factor: a crucial regulator of pancreatic beta cell development, identity, and proliferation. Stem Cell Res Ther 11(1):459
Alagpulinsa DA, Cao JJL, Driscoll RK, Sirbulescu RF, Penson MFE, Sremac M, Engquist EN, Brauns TA, Markmann JF, Melton DA, Poznansky MC (2019) Alginate-microencapsulation of human stem cell-derived beta cells with CXCL12 prolongs their survival and function in immunocompetent mice without systemic immunosuppression. Am J Transplant 19(7):1930–1940
Alessandra G, Algerta M, Paola M, Carsten S, Cristina L, Paolo M, Elisa M, Gabriella T, Carla P (2020) Shaping pancreatic beta-cell differentiation and functioning: the influence of mechanotransduction. Cells 9(2)
Amorim RG, Guedes GDS, Vasconcelos SML, Santos JCF (2019) Kidney disease in diabetes mellitus: cross-linking between hyperglycemia, redox imbalance and inflammation. Arq Bras Cardiol 112(5):577–587
Anane E, Knudsen IM, Wilson GC (2021) Scale-down cultivation in mammalian cell bioreactors—the effect of bioreactor mixing time on the response of CHO cells to dissolved oxygen gradients. Biochem Eng J 166:107870
Barkai U, Rotem A, de Vos P (2016) Survival of encapsulated islets: more than a membrane story. World J Transplant 6(1):69–90
Ben-Akiva E, Est Witte S, Meyer RA, Rhodes KR, Green JJ (2018) Polymeric micro- and nanoparticles for immune modulation. Biomater Sci 7(1):14–30
Burns CJ, Persaud SJ, Jones PM (2004) Stem cell therapy for diabetes: do we need to make beta cells? J Endocrinol 183(3):437–443
Costa AM, Mano JF (2017) Solvent-free strategy yields size and shape-uniform capsules. J Am Chem Soc 139(3):1057–1060
Coward SM, Legallais C, David B, Thomas M, Foo Y, Mavri-Damelin D, Hodgson HJ, Selden C (2009) Alginate-encapsulated HepG2 cells in a fluidized bed bioreactor maintain function in human liver failure plasma. Artif Organs 33(12):1117–1126
de Vos P, Faas MM, Strand B, Calafiore R (2006) Alginate-based microcapsules for immunoisolation of pancreatic islets. Biomaterials 27(32):5603–5617
Eilenberger C, Kratz SRA, Rothbauer M, Ehmoser EK, Ertl P, Kupcu S (2018) Optimized alamarBlue assay protocol for drug dose-response determination of 3D tumor spheroids. MethodsX 5:781–787
Furman BL (2015) Streptozotocin-induced diabetic models in mice and rats. Curr Protoc Pharmacol 70:5–47
Huang H, Bader TN, Jin S (2020) Signaling molecules regulating pancreatic endocrine development from pluripotent stem cell differentiation. Int J Mol Sci 21(16)
Kim SO, Choe WK (2011) Effect of EGCG on expression of neurogenin 3 via the MAP kinase signaling pathway in AR42J cells, a rat pancreatic tumor cell line. Korean J Nut 44(3):196–202
Koppula PR, Chelluri LK, Polisetti N, Vemuganti GK (2009) Histocompatibility testing of cultivated human bone marrow stromal cells - a promising step towards pre-clinical screening for allogeneic stem cell therapy. Cell Immunol 259(1):61–65
Kutlu B, Burdick D, Baxter D, Rasschaert J, Flamez D, Eizirik DL, Welsh N, Goodman N, Hood L (2009) Detailed transcriptome atlas of the pancreatic beta cell. BMC Med Genomics 2:3
Lysy PA, Weir GC, Bonner-Weir S (2012) Concise review: pancreas regeneration: recent advances and perspectives. Stem Cells Transl Med 1(2):150–159
Mendonca da Silva J, Erro E, Awan M, Chalmers SA, Fuller B, Selden C (2020) Small-scale fluidized bed bioreactor for long-term dynamic culture of 3D cell constructs and in vitro testing. Front Bioeng Biotechnol 8:895
Mooranian A, Jones M, Ionescu CM, Walker D, Wagle SR, Kovacevic B, Chester J, Foster T, Johnston E, Kuthubutheen J, Brown D, Mikov M, Al-Salami H (2021) Artificial cell encapsulation for biomaterials and tissue bio-nanoengineering: history, achievements, limitations, and future work for potential clinical applications and transplantation. J Funct Biomater 12(4)
Moulis M, Runser SVM, Glorieux L, Dauguet N, Vanderaa C, Gatto L, Tyteca D, Henriet P, Spagnoli FM, Iber D, Pierreux CE (2022) Identification and implication of tissue-enriched ligands in epithelial-endothelial crosstalk during pancreas development. Sci Rep 12(1):12498
Nikravesh N, Cox SC, Ellis MJ, Grover LM (2017) Encapsulation and fluidization maintains the viability and glucose sensitivity of beta-cells. ACS Biomater Sci Eng 3(8):1750–1757
Omar-Hmeadi M, Idevall-Hagren O (2021) Insulin granule biogenesis and exocytosis. Cell Mol Life Sci 78(5):1957–1970
Otonkoski T, Beattie GM, Mally MI, Ricordi C, Hayek A (1993) Nicotinamide is a potent inducer of endocrine differentiation in cultured human fetal pancreatic cells. J Clin Invest 92(3):1459–1466
Pavathuparambil Abdul Manaph N, Sivanathan KN, Nitschke J, Zhou XF, Coates PT, Drogemuller CJ (2019) An overview on small molecule-induced differentiation of mesenchymal stem cells into beta cells for diabetic therapy. Stem Cell Res Ther 10(1):293
Pentela N, Rainu S, Duraipandy N, Boopathi AA, Kiran MS, Sampath S, Samanta D (2019) Microcapsules responsive to pH and temperature: synthesis, encapsulation and release study. SN Appl Sci 1(5):448
Rickels MR, Robertson RP (2019) Pancreatic islet transplantation in humans: recent progress and future directions. Endocr Rev 40(2):631–668
Rohli KE, Boyer CK, Blom SE, Stephens SB (2022) Nutrient regulation of pancreatic islet beta-cell secretory capacity and insulin production. Biomolecules 12(2)
Schweicher J, Nyitray C, Desai TA (2014) Membranes to achieve immunoprotection of transplanted islets. Front Biosci (landmark Ed) 19(1):49–76
Silva IBB, Kimura CH, Colantoni VP, Sogayar MC (2022) Stem cells differentiation into insulin-producing cells (IPCs): recent advances and current challenges. Stem Cell Res Ther 13(1):309
Vaca P, Berna G, Araujo R, Carneiro EM, Bedoya FJ, Soria B, Martin F (2008) Nicotinamide induces differentiation of embryonic stem cells into insulin-secreting cells. Exp Cell Res 314(5):969–974
Wang LH, Ernst AU, Flanders JA, Liu W, Wang X, Datta AK, Epel B, Kotecha M, Papas KK, Ma M (2021) An inverse-breathing encapsulation system for cell delivery. Sci Adv 7(20)
Wang Q, Ye L, Liu H, Liu X, Li S, Chen Z (2012) Reprogramming of bone marrow-derived mesenchymal stem cells into functional insulin-producing cells by chemical regimen. Am J Stem Cells 1(2):128–137
Wang W, Zhang C (2021) Targeting beta-cell dedifferentiation and transdifferentiation: opportunities and challenges. Endocr Connect 10(8):R213–R228
Wassmer CH, Bellofatto K, Perez L, Lavallard V, Cottet-Dumoulin D, Ljubicic S, Parnaud G, Bosco D, Berishvili E, Lebreton F (2020) Engineering of primary pancreatic islet cell spheroids for three-dimensional culture or transplantation: a methodological comparative study. Cell Transplant 29:963689720937292
Wei M, Ong L, Smith MT, Ross FB, Schmid K, Hoey AJ, Burstow D, Brown L (2003) The streptozotocin-diabetic rat as a model of the chronic complications of human diabetes. Heart Lung Circ 12(1):44–50
Yamazaki K, Kawabori M, Seki T, Houkin K (2020) Clinical trials of stem cell treatment for spinal cord injury. Int J Mol Sci 21(11)
Yoon JW, Jun HS (2005) Autoimmune destruction of pancreatic beta cells. Am J Ther 12(6):580–591
Zhang Q, Gonelle-Gispert C, Li Y, Geng Z, Gerber-Lemaire S, Wang Y, Buhler L (2022) Islet encapsulation: new developments for the treatment of type 1 diabetes. Front Immunol 13:869984
Zhang Y, Xu J, Ren Z, Meng Y, Liu W, Lu L, Zhou Z, Chen G (2021) Nicotinamide promotes pancreatic differentiation through the dual inhibition of CK1 and ROCK kinases in human embryonic stem cells. Stem Cell Res Ther 12(1):362
Author information
Authors and Affiliations
Contributions
D.Z. planned and undertook experimental work and wrote the manuscript. M.A. advised and supervised the research and read the final proofreading manuscript.
Corresponding author
Ethics declarations
Ethics approval
Ethics approval for all animal experiments was obtained from the institutional animal care and use Committee of Tehran North Branch of Islamic Azad University, Tehran.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zaeifi, D., Azarnia, M. Promoting β-cells function by the recapitulation of in vivo microenvironmental differentiation signals. Cell Tissue Res 393, 37–46 (2023). https://doi.org/10.1007/s00441-023-03773-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-023-03773-7