Abstract
Intravenous administration of bone marrow-derived mesenchymal stem cells (BM-MSCs) has been shown to promote nerve cell regeneration following traumatic brain injury (TBI). As the anti-oxidant defense systems in neuronal tissue including superoxide dismutase 2 (SOD2) are crucial to defend cell against oxidative stress. We proposed a new stratege to increase the therapeutic effect of MSCs by preventing cells death from oxidative stress. We overexpressed SOD2 in BM-MSCs, transplanted these MSCs into TBI model mice, assessed the protective effect of SOD2 against oxidation-induced apoptosis in BM-MSCs both in vitro and in vivo, evaluated brain functional recovery by the rotarod behavioral test, and tested the oxidation status of TBI mice brain after BM-MSCs transplantation by monitoring the superoxide dismutase, glutathione and malonaldehyde level. We found over-expression of SOD2 protected BM-MSCs from H2O2-induced cell apoptosis. Injection of SOD2 over-expressed BM-MSCs attenuated neuro-inflammation in the ipsilateral cortex of TBI mice, and protected TBI mice against loss of blood–brain barrier integrity. Furthermore, the rotarod behavioral test showed functional recovery of TBI mice after MSC treatment. Our experiments indicated that SOD2-over-expressed BM-MSCs have an improved therapeutic effect on brain injury treatment in TBI mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Traumatic brain injury (TBI) is distinguished by a disruption of the normal brain function due to an injury following a trauma, which has the potential to induce severe physical, congnitive, and emotional impairment (Hasan et al. 2017),, leading to either death or hopitalization. More important, TBI causes primary damage to the brain followed by a secondary injury. The second injury is demonstrated in various pathophysiological mechanisms, including cytotoxicity, cerebral edema, gene activation, inflammation, and oxidative injury (Hasan et al. 2017). These mechanisms develop oxidative stress, an imbalance between oxidant and anti-oxidant agents that can cause neural dysfunction and death (Uttara et al. 2009), and this imbalance is directly related to the pathogenesis of TBI. Anti-oxidant defense enzymes such as superoxide dismutase (SOD) decrease after TBI (Rodriguez-Rodriguez et al. 2014). SOD2, one of the SOD family, is a mitochondrial anti-oxidant enzyme which scavenges superoxide radicals. Reduction of SOD2 activity was shown to increase neuronal death induced by transient cerebral ischemia (Tseng et al. 2017; Zhang et al. 2017). Over-expression of SOD2 provides direct neuroprotection, glioprotection and protection of the blood–brain barrier (BBB) (Cornelius et al. 2013). Thus, the development of anti-oxidant strategies is of immediate interest in brain injury treatment.
Mesenchymal stem cells (MSCs) are being widely used in clinical trials (Lazarus et al. 1995; Salehi et al. 2017). They are adherence cells and pluripotent for mesenchymal lineages including osteocytes, adipocytes, and chondrocytes (Dominici et al. 2006). The ability of MSCs for tissue repair and regeneration is also based on their secretion of beneficial cytokines and growth factors (Moghadasali et al. 2013; Nargesi et al. 2017; Sevivas et al. 2016). Administration of MSCs has been proposed as an innovative approach and has been proved to have therapeutic effects in clinical trials for the therapies of many diseases, which are non-treatable by current traditional therapies, including heart disease, neuron degenerative diseases, hematologic malignancies, and autoimmune diseases (Peired et al. 2016; Wang et al. 2016; Yi et al. 2016; Zhang et al. 2016). Injection of MSCs has been used for TBI treatment in animal models and proved to have potential therapeutic effect, but the efficancy of MSC therapy still needs to be improved.
As the anti-oxidant defense systems in neuronal tissue including SOD2 are critical for preventing cell death from oxidative stress, by preventing MSC death from oxidative stress, we propose a new strategy that, by increasing the survival rate of MSCs, will improve the therapeutic efficacy of MSC-mediated treatment. Thus, we over-expressed SOD2 in MSCs to investigate the therapeutic effect on TBI treatment in mice. We found over-expression of SOD2 protected BM-MSCs against H2O2-induced cell apoptosis both in vitro and in vivo, attenuated neuro-inflammation in the ipsilateral cortex of TBI mice, and also protected TBI mice against loss of BBB integrity. Furthermore, the rotarod behavioral test showed functional recovery of TBI mice after MSC treatment. Our experiments indicated that SOD2-over-expressed BM-MSCs have an improved therapeutic effect on brain injury treatment in TBI mice.
Materials and methods
Animals
This study was carried out in strict accordance with the recommendation in the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health and Weifang Yidu Central Hospital. Balb/c mice were purchased from SLAC laboratory animal (Shanghai, China). Mice were caged in a fully ventilated room and maintained in a 12:12-h light:dark cycle. They had free access to a standard chow diet and water. No animals died during the period of the experiments.
Preparation and characterization of mouse mesenchymal stem cells
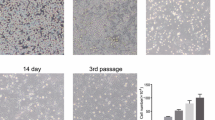
Mouse mesenchymal stem cells were prepared as described previously (Rooney et al. 2008). Briefly, bone marrow (BM) was collected by flushing the dissected femurs with complete MesenCult™ MSC Basal Medium (Mouse) (Stem cell technologies, Vancouver, Canada) supplemented with penicillin (100 U/mL) and streptomycin (100 mg/mL) (Gibco, Grand Island, NY, USA). The BM cell suspension was carefully pipetted and followed by centrifugation at 320g for 5 min. After two times washing, cells were cultured in 10-cm culture dishes with a density of 1.0 × 106/ml at 37 °C with 5% CO2. When the cultured cells reached 90% confluency, adherent cells were trypsinized and passaged. Cells underwent 4–5 passages before use in the subsequent experiments. MSC surface maker characterization was tested by mouse mesenchymal stem cell marker antibody staining. Antibodies for positive MSC markers (CD29, CD44, CD105) and negative marker (CD34, CD45) were purchased from BD Biosciences (San Jose, CA, USA). BD FACSCalibur flow cytometer (BD Biosciences, Franklin Lakes, NJ, USA) was used to analyze antibody staining.
Adenovirus production and transduction
Empty adenovirus vector and vector encoding SOD2 were purchased from Shanghai Liangtai Biotechnology (Shanghai, China). To produce adenovirus, the linearized construct DNA was transfected into 293 cells using Lipofectamine 2000™ following the manufacturer’s instructions. After 24 h, the cells were fed fresh medium, and incubation was continued for an additional 5 days. Virus was released from the cells by freezing and thawing for three consecutive cycles. After the third freeze–thaw cycle, the cells were briefly centrifuged to pellet the debris and the lysate kept in clean and sterile centrifuge tubes and stored at −20 °C for future use. For adenovirus transduction, the MSCs were plated in 6-well plates, and the next day the adenovirus was added with an MOI of 10 in 2 mL of medium. The plate was centrifuged at 220g for 90 min at 37 °C. Then, the cells were incubated in a 5% CO2 incubator for an additional 4 h. Next, the medium was removed and fresh complete growth medium was added. The cells were incubated for another 24 h and were then ready for analysis.
RT-PCR
Total RNA was extracted with the use of the RNeasy Mini Kit (Qiagen, CA, USA) from the MSCs after adenovirus transduction. Reverse transcription was performed using a reverse transcription kit (Applied Biosystem, Waltham, MA, https://en.wikipedia.org/wiki/Waltham,_Massachusetts USA). Real-time quantitative PCR reactions were set up in triplicate with SYBR® Green Master Mix (Biorad, CA, USA) and run on a LightCycler 480 (Roche, Penzberg, Upper Bavaria, Germany). The following primers were used in the current study: SOD2: (Fwd: TTAACGCGCAGATCATGCA, Rev.: GGTGGCGTTGAGATTGTTCA); GAPDH: (Fwd: AACGACCCCTTCATTGAC, Rev.: TCCACGACATACTCAGCAC).
MSCs apoptosis analysis
MSCs with mock, empty adenovirus or SOD2 adenovirus transduction were treated with H2O2 for 24 h. Then, the cells were subjected to Annexin V/PI staining using Alexa Fluor® 488 Annexin V/Dead Cell Apoptosis Kit (Thermo Fisher Scientific, USA) following the manufacturer’s instruction. A BD FACSCalibur flow cytometer (BD Biosciences) was used to analyze antibody staining.
Assessment of Evans blue extravasation
The assay of Evans blue (EB) leakage was used to evaluate BBB disruption following the experimental stroke. Briefly, 2% EB (4 mL/kg) was injected via the tail vein at 6 h after reperfusion. At 2 h after EB injection, mice were perfused under anesthesia. Tissue samples were collected from the cortex and striatum, which were then homogenized by 50% trichloracetic acid and centrifuged. The absorbance of supernatants was measured at 620 nm with infinite M200 PRO (TECAN, Austria).
Western blot
MSCs were collected and transferred to an Eppendorf tube, washed twice with phosphate-buffered solution (PBS) buffer and then lysised in RIPA lysis buffer containing 1% protease inhibitor cocktail (Santa Cruz, Dallas, TX, USA). A total of 25 μg of proteins were loaded onto a 12% SDS-PAGE gel, followed by standard western blot procedure. Mouse anti-SOD2, mouse anti-GAPDH (Abcam, Cambridge, MA, USA), and HRP-conjugated secondary antibodies were used. For the mice experiments, ipsilateral cortexes were isolated from the experimental mice and then lysis for western blot. Rabbit anti-ZO-1 and rabbit anti-occludin were purchased from Abcam.
TBI mouse model
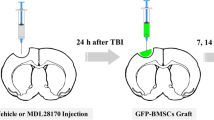
The controlled cortical impact model (CCI) of traumatic brain injury (TBI) was induced in male adult Balb/c mice (6–8 weeks). Briefly, mice were anesthetized by 4% isoflurane in oxygen and then placed in a stereotaxic device. After drilling a hole (3.5 mm × 3.5 mm) in the right skull, a pneumatic piston impactor tip (3 mm diameter) was used to induce injury in the brain at the center of the cranitomy. The tip penetration depth was 1.0 mm and the velocity was 4.5 m/s. A warming pad was used to keep body temperature around 37 °C during the surgery. The skull bone was discarded during CCI, and the skin was sealed by size 6–0 suture. We used burprenorphine as the painkiller under restricted regulatory monitoring. MSCs were administrated 6 h after TBI surgery (see study flowchart in supplementary Fig. S1). We perfused the animals with 40–50 mL PBS before dissecting the brain 1 week after MSC transplantation except for the animals for the behavioral test.
Transplantation of MSCs
MSCs with mock transduction and MSCs transduced with empty adenovirus or SOD2 adenovirus were suspended in PBS (1 × 106 cells in 100 μL PBS) and then injected into mice using a Hamilton syringe with a 31-gauge needle set intravenously through the tail vein. PBS only was used as the vehicle control group.
Rotarod behavior test
The functional recovery of mice was evaluated by a standard rotarod behavior. The latency to fall from a rotating rod is calculated by incorporated infrared sensors in a Rotamex 5 (Columbus Instruments, Columbus, OH, USA). The experiment was conducted 3 weeks (21 days) after transplantation. The animals were left to acclimate in a dark room for 1 h before the experiment. During the experiment, mice were carefully placed on the rotating rod, and the latency time on the rod was tested. The rod motor was initially set at 5 rpm with an acceleration rate of 0.3 rpm/s for a maximum trial period of 180 s, and performance was measured as latency to fall in seconds.
Malondialdehyde (MDA) assay
Harvested tissues were washed in iced cold PBS. After excising 0.4–0.5 g from each tissue, each sample was homogenized in 20 mM PBS [tissue to buffer ratio, 1:10 w/v]. 10 μL of 0.5 M butylated hydroxytoluene per ml of homogenate had been added to prevent additional sample oxidation. The homogenate was centrifuged at 4000g at 4 °C for 10 min. Next, 200 μL of supernatant from each homogenate was used to analyze the MDA level in tissue samples. Measurement of MDA is based on the reaction of a chromogenic reagent, N-methyl-2-phenylindole [R1] with MDA at 24 °C. One molecule of MDA interacts with 2 molecules of R1 to yield a stable chromophore with maximal absorbance at 586 nm, and is stable for up to 1 h at room temperature. The net absorbance at 586 nm yields a linear function of MDA ranging from 0 to 20 μM.
Glutathione assay
Concentrations of oxidized glutathione (GS-SG) in samples were analyzed using a Glutathione Assay Kit from Cayman Chemical (Ann Arbor, USA). The kit uses an enzymatic recycling method using glutathione reductase to quantify glutathione (GSH). The GSH produced from the interaction of the sulfhydryl group of GSH with 5, 5′-dithiobis-2-nitrobenzoic acid was oxidized to the disulfide dimer GS-SG and reduced to GSH by glutathione reductase. The net absorbance at 405 nm yields a linear function of GS-SG ranging from 0 to 20 μM, and these values were extrapolated based on the standard curve provided with the assay kit.
Superoxide dismutase (SOD) assay
The SOD concentration was analyzed using a Superoxide Dismutase Assay Kit from Cayman Chemical. The superoxide radical agents formed by the interaction of xanthine oxidase with hypoxanthine were detected by tetrazolium. One unit of SOD detected is equivalent to the amount of enzyme needed to exhibit 50% dismutase of superoxide radical. The net absorbance at 450 nm yields a linear function of SOD ranging from 0 to 30 U/mL. The detection of SOD is 0.1 U/ml, and these values were extrapolated based on the standard curve provided with the assay kit.
Elisa
ELISA kits including TNFα, IL10 and IFN-γ for cytokine profiling were all obtained from R&D Systems (MN, USA). Dissected TBI brain tissues were weighed and placed in 1% SDS solution overnight with proteinase inhibitor cocktail (Roche, USA). After brief sonication, samples were centrifuged at 5100g for 5 min at 4 °C. The supernatant was retrieved for ELISA analysis according to the manufacturer’s protocol.
Statistical analysis
Statistical evaluation was performed using one-way ANOVA analysis, followed by a Tukey’s post hoc test. Data are presented as mean ± SD. The significance value was set at P < 0.05.
Results
Expression of SOD2 in BM-MSCs by adenovirus vector transfection
The phenotype of bone marrow-derived MSCs in this study was confirmed by the staining of MSC-specific cell surface markers. As shown in Fig. 1a, the BM-MSCs are positive for CD29, CD44 and CD105, which are specific MSC surface markers. In addition, these cells are negative for CD34 and CD45, which are non-MSC markers. These results indicated that these BM-MSCs are typical MSCs for the subsequent experiments. To over-express SOD2 in BM-MSCs, we transduced cells with adenovirus encoding SOD2. Then, 24 h after transduction, the expression of SOD2 was analyzed on both the mRNA and protein level. We detected a significantly increased SOD2 mRNA level (Fig. 1b) as well as protein level (Fig. 1c, d) in SOD2 adenovirus-transduced BM-MSCs when compared to mock or empty adenovirus-transduced BM-MSCs.
Successful over-expression of SOD2 in BM-MSCs by adenovirus vector transfection. a Flow cytometric analysis reveals that BM-MSCs were positive for CD29, CD44 and CD105, but negative for CD34 and CD45. b Relative SOD2 mRNA levels were examined by RT-PCR and normalized to control. GAPDH was employed as an internal control. c, d SOD2 protein expressions were analyzed by western blotting. GAPDH was employed as a loading control. Data are mean ± SD. **P < 0.01 compared to control
Over-expression of SOD2 protects BM-MSCs from H2O2-induced cell apoptosis
The antioxidant defense systems in neuronal tissue including SOD2 are critical in preventing cell death from oxidative stress. We therefore assessed the protective effect of SOD2 against oxidation-induced apoptosis in BM-MSCs after exposure to H2O2. Consistent with previous reports, H2O2 treatment induced apoptosis in the BM-MSCs, as we detected significantly increased apoptotic cells after H2O2 treatment (32.57 ± 3.79%; Fig. 2a, b). In contrast, the SOD2-over-expressing BM-MSCs were resistant to H2O2 –induced apoptosis (12.65 ± 1.48%), suggesting the protective role of SOD2 to prevent oxidative stress.
Over-expression of SOD2 protects against H2O2-induced cell apoptosis in BM-MSCs. a Cells were treated by 0.2 mM H2O2 for 24 h, then subjected to Annexin V/PI staining. b Percentage of apoptotic cells in the experimental groups. Data are mean ± SD. **P < 0.01 compared to control, ##P < 0.01 compared to the H2O2-treated group
Transplantation of SOD2 over-expressing BM-MSCs promoted functional recovery in TBI mice
Brain injury caused an increase in oxidative stress, which contributed to brain damage. As over-expression of SOD2 in BM-MSCs can prevent BM-MSCs from oxidative stress, we further tested whether these SOD2-over-expressed BM-MSCs have a protective effect in vivo. Our pilot study suggests that MSCs could successfully migrate to the site of a brain injury (supplementary Fig. S2). TBI mice were transplanted with SOD2-over-expressed BM-MSCs. The rotarod behavioral test was conducted to evaluate the functional recovery of TBI mice at 21 days after initial BM-MSCs transplantation. The results show that transplantation of BM-MSCs and SOD2 over-expressed BM-MSCs significantly (62.6 ± 7.1 s, P < 0.05 for normal BM-MSCs; 85.7 ± 8.6 s, P < 0.01 for SOD2 BM-MSCs) improved the TBI mice function over the PBS-treated group (38.6 ± 4.4 s; Fig. 3).
.Examination of functional recovery by rotarod behavioral test in TBI mice 3 weeks after transplantation. Over-expression of SOD2 in BM-MSCs significantly enhanced latency time in TBI mice. n = 8 in each experimental group. Data are mean ± SD. *P < 0.05, **P < 0.01 compared to sham group, #P < 0.05, ##P < 0.01 compared to the vehicle group
Transplantation of SOD2-over-expressed BM-MSCs protected the BBB in TBI mice
In TBI mice, the BBB integrity was impaired. Our previous result has shown that transplantation of BM-MSCs promoted functional recovery in TBI mice. Thus, we continued to test the effect of BM-MSCs transplantation on BBB integrity in TBI mice using EB leakage assay. As shown in Fig. 4a, the BBB was significantly impaired in TBI mice. Once these mice were treated with BM-MSCs or SOD2-over-expressed BM-MSCs, the impairment was significantly improved (P < 0.05 for normal BM-MSCs and P < 0.01 for SOD2 BM-MSCs). Correlated to this, we also detected significantly increased expression of tight junction proteins ZO-1 and occluding (Fig. 4b and c), indicating the enhanced tight junction integrity in TBI mice after BM-MSCs transplantation.
Over-expression of SOD2 in BM-MSCs protects against loss of blood-brain barrier integrity in TBI mice 1 week after transplantation. a The contents of Evans blue leaking into the contralateral and ipsilateral brains were quantified in each experimental group. b, c Expressions of tight junction proteins (ZO-1 and occludin) in the ipsilateral cortex of experimental animals were analyzed by western blotting. GAPDH was used as a loading control. n = 8 in each experimental group. Data are mean ± SD. **P < 0.01 compared to sham group, #P < 0.05, ##P < 0.01 compared to vehicle group
Transplantation of SOD2 over-expressed BM-MSCs attenuated neuro-inflammation in the ipsilateral cortex of TBI mice
As over-expression of SOD2 in BM-MSCs prevented oxidative stress, we tested the oxidation status of TBI mice brain after the BM-MSCs transplantation by monitoring the SOD, GSH and MDA level. SOD and GSH were endogenous antioxidant and MDA was the oxidative stress marker. In the current study, TBI mice had significant decreased activity of SOD (Fig. 5a), which was consistent with previous reports. Transplantation of normal BM-MSCs did not affect SOD activity. After transplantation of SOD2-over-expressed BM-MSCs, we did detect significantly increased SOD activity, which were definitely from the over-expressed SOD2. The transplantation of BM-MSCs did not affect endogenous GSH level (Fig. 5b). In contrast, we detected a decreased MDA level (P < 0.05) in SOD2-over-expressed BM-MSCs transplanted TBI mice (Fig. 5c), indicating decreased oxidative stress in the brain of these mice.
Status of oxidative stress in each experimental group, characterized by SOD activity (a), GSH level (b) and MDA level (c) in the ipsilateral cortex of TBI mice 1 week after transplantation. n = 8 in each experimental group. Data are mean ± SD. *P < 0.05, **P < 0.01 compared to sham group, #P < 0.05 compared to vehicle group
Oxidative stress was associated with pro-inflammatory cytokines and MSCs havebeen reported to have immunomodulatory functions by producing cytokines. Thus, we also monitored the cytokine production in brain of TBI mice after transplantation. As shown in Fig. 6, there were significantly increased pro-inflammatory cytokines TNF-α (8.42 ± 0.91 pg/mg tissue; Fig. 6a) and IFN-γ (8.77 ± 0.89 pg/mg tissue; Fig. 6b) in TBI mice when compared to sham mice (2.31 ± 0.25 and 1.43 ± 0.16 pg/mg tissue, respectively). Once the mice were transplanted with SOD2-over-expressed BM-MSC, the TNF-α (4.06 ± 0.47 pg/mg tissue; Fig. 6a) and IFN-γ (3.19 ± 0.13 pg/mg tissue; Fig. 6b) levels were significantly decreased. In contrast, the level of anti-inflammatory cytokine IL-10 was significantly increased after transplantation of SOD2 BM-MSCs (7.29 ± 0.76 pg/mg tissue; Fig. 6c) compared to the vehicle group (3.08 ± 0.32 pg/mg tissue). All these results indicated that over-expression of SOD2 in BM-MSCs attenuated oxidative stress and neuro-inflammation in TBI mice after transplantation.
Over-expression of SOD2 in BM-MSCs attenuates neuro-inflammation in the ipsilateral cortex of TBI mice 1 week after transplantation, characterized by TNF-α level (a), IFN-γ level (b) and IL-10 level (c). n = 8 in each experimental group. Data are mean ± SD. *P < 0.05, **P < 0.01 compared to sham group, #P < 0.05, ##P < 0.01 compared to vehicle group
Discussion
Even mild TBIs can cause prolonged symptoms and long-term serious sequelae. Headaches whave beenere reported at weeks after the injury, and the risk of depression remains high for decades afterwards (Daneshvar et al. 2011). Evenso, TBI survivors are encountered with chronic post-injury sympotoms including learning and memory impairments (Barman et al. 2016). TBI could also increase the possibility of suffering from Alzhermer’s disease or dementia when patients get old (Thompson et al. 2006). Thus, it is urgent for investigators to find new strategies for TBI treatment.
Intravenous administration of BM-MSCs has been shown to reduce BBB compromise and improve neurocognition following TBI (Zhao et al. 2016). Here, we successfully over-expressed SOD2 in BM-MSCs, confirmed the protective effect of SOD2 against oxidation-induced apoptosis in BM-MSCs after exposure to H2O2. We also showed that SOD2-over-expressed BM-MSCs have a protective effect in vivo, evidenced by the rotarod behavioral test, and thus transplantation of SOD2-over-expressed BM-MSCs promoted functional recovery in TBI mice. These therapeutic effects were probably achieved through the improvement of BBB integrity by BM-MSCs, evidenced by increased expression of tight junction proteins ZO-1 and occluding, as well as decreased oxidative stress and neuro-inflammation in the brain of TBI mice after transplantation.
Oxidative stress and inflammation caused by TBI, subsequently induced a second brain injury. Following the initial injury caused by the trauma, a severe on-site inflammation occurs, aggravating the damage and increasing the site of the injury to the neighboring neurons. The primary injury causes ischemia, reducing the oxygen and glucose supply to the cells. SODs are endogenous anti-oxidants, their level related to the SOD2 level, so it is not surprising that SOD activity is significantly increased after SOD2-over-expressed BM-MSCs transplantation, while GSH level is unaffected.
TBI leads to impairment of BBB integrity (Yuan et al. 2016), and subsequently induces brain damage. We used EB to check the BBB integrity, and the leakage of the contralateral sham group was supposed to be zero without TBI; however, the surgery might cause some leakage, which was considered as the baseline.
The potency of MSCs for tissue repair and regeneration is based on their ability of pluoripotency, and secretion of beneficial molecules (Moghadasali et al. 2013; Nargesi et al. 2017; Sevivas et al. 2016). Over-expression of cytokines and growth factors targeting certain diseases is suggested to be a method for disease-target therapy. IV-MSC treatment attenuates loss of neural stem cells and promotes hippocampal neurogenesis in the TBI mice model (Zhao et al. 2016). MSCs over-expressed SOD2 have more potential to treat TBI through improvement of survival against oxidative stress-induced cell apoptosis in TBI mice brain. Study has shown that SOD2 overexpression in hippocampal astrocytes would improve the survival of CA1 neurons after transient forebrain ischemia (Xu et al. 2010). The mitochondrial respiratory chain is the major site of ROS production (Drose and Brandt 2012). SOD2 directly reduces mitochondrial ROS which protects mitochondria and likely reduces oxidative stress for the rest of the cell. Other factors secreted by MSCs also have a role in neurocognitive recovery following TBI. Wnt3a has a demonstrated role in the therapeutic potential of MSCs and has been identified as a potentidal standalone therapy or as part of a combination therapeutic strategy for TBI treatment (Zhao et al. 2016).
The mechanism of MSCs therapy is also widely investigated for regenerative therapy (Ikebe and Suzuki 2014; Mahmood et al. 2004; Meseguer-Olmo et al. 2017). Previous studies have shown that MSCs modulate the immunological activity of certain cell populations (Abdi et al. 2008; Hynes et al. 2016). They can effectively inhibit proliferation of CD4 and CD8 T cells. They also promote a shift for T cells from a pro-inflammatory state to an anti-inflammatory state. Moreover, MSCs can affect the production of CD4+ CD25+ regulatory T cells. B-cell proliferation can also be inhibited by MSCs which can affect pro-inflammatory cytokines secretion. In our experiment, TNF-α and IFN-γ levels were significantly decreased, while the level of anti-inflammatory cytokine IL-10 was significantly increased after transplantation of SOD2-over-expressed BM-MSCs, probably through the decreased level by preventing oxidative stress in the trauma site, though it cannot be excluded for the immunomodulatory functions of MSCs. Furthermore, overexpression of SOD2 should enhance the survival of MSCs in the trauma site, which would indirectly attenuate the overall inflammatory activities in this area, which was seen in our results. We believe that MSCs may not build the damaged tissue after TBI, rather exert microenvironment modulatory effects by inducing the surrounding cells to protect against the damage or mediate some reaction through the immune system. However, it is unclear for the exact mechanisms underlying the change of the cytokine levels. Nevertheless, because of the immunomodulatory characters of MSCs, these cells have been widely used in many clinical trials targeting autoimmune diseases such as graft-versus-host disease (Gavioli et al. 2005).
Overall, MSCs would be a potential way for cell therapy, especially in brain injury. There are about 10 million people suffering TBI worldwide each year (Hyder et al. 2007), making it an urgent task to develop new strategies for TBI treatment. Our experiment demonstrated that transplantation of SOD2-over-expressed MSC could give a new insight into treatment of TBI with great potential as a novel therapeutic strategy.
References
Abdi R, Fiorina P, Adra CN, Atkinson M, Sayegh MH (2008) Immunomodulation by mesenchymal stem cells: a potential therapeutic strategy for type 1 diabetes. Diabetes 57:1759–1767
Barman A, Chatterjee A, Bhide R (2016) Cognitive impairment and rehabilitation strategies after traumatic brain injury. Indian J Psychol Med 38:172–181
Cornelius C, Crupi R, Calabrese V, Graziano A, Milone P, Pennisi G, Radak Z, Calabrese EJ, Cuzzocrea S (2013) Traumatic brain injury: oxidative stress and neuroprotection. Antioxid Redox Signal 19:836–853
Daneshvar DH, Riley DO, Nowinski CJ, McKee AC, Stern RA, Cantu RC (2011) Long-term consequences: effects on normal development profile after concussion. Phys Med Rehabil Clin N Am 22(683–700):ix
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Prockop D, Horwitz E (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8:315–317
Drose S, Brandt U (2012) Molecular mechanisms of superoxide production by the mitochondrial respiratory chain. Adv Exp Med Biol 748:145–169
Gavioli M, Luppi G, Losi L, Bertolini F, Santantonio M, Falchi AM, D'Amico R, Conte PF, Natalini G (2005) Incidence and clinical impact of sterilized disease and minimal residual disease after preoperative radiochemotherapy for rectal cancer. Dis Colon Rectum 48:1851–1857
Hasan A, Deeb G, Rahal R, Atwi K, Mondello S, Marei HE, Gali A, Sleiman E (2017) Mesenchymal stem cells in the treatment of traumatic brain injury. Front Neurol 8:28
Hyder AA, Wunderlich CA, Puvanachandra P, Gururaj G, Kobusingye OC (2007) The impact of traumatic brain injuries: a global perspective. NeuroRehabilitation 22:341–353
Hynes K, Bright R, Proudman S, Haynes D, Gronthos S, Bartold M (2016) Immunomodulatory properties of mesenchymal stem cell in experimental arthritis in rat and mouse models: a systematic review. Semin Arthritis Rheum 46:1–19
Ikebe C, Suzuki K (2014) Mesenchymal stem cells for regenerative therapy: optimization of cell preparation protocols. Biomed Res Int 2014:951512
Lazarus HM, Winton EF, Williams SF, Grinblatt D, Campion M, Cooper BW, Gunn H, Manfreda S, Isaacs RE (1995) Phase I multicenter trial of interleukin 6 therapy after autologous bone marrow transplantation in advanced breast cancer. Bone Marrow Transplant 15:935–942
Mahmood A, Lu D, Chopp M (2004) Intravenous administration of marrow stromal cells (MSCs) increases the expression of growth factors in rat brain after traumatic brain injury. J Neurotrauma 21:33–39
Meseguer-Olmo L, Montellano AJ, Martinez T, Martinez CM, Revilla-Nuin B, Roldan M, Mora CF, Lopez-Lucas MD, Fuente T (2017) Intraarticular and intravenous administration of 99MTc-HMPAO-labeled human mesenchymal stem cells (99MTC-AH-MSCS): in vivo imaging and biodistribution. Nucl Med Biol 46:36–42
Moghadasali R, Mutsaers HA, Azarnia M, Aghdami N, Baharvand H, Torensma R, Wilmer MJ, Masereeuw R (2013) Mesenchymal stem cell-conditioned medium accelerates regeneration of human renal proximal tubule epithelial cells after gentamicin toxicity. Exp Toxicol Pathol 65:595–600
Nargesi AA, Lerman LO, Eirin A (2017) Mesenchymal stem cell-derived extracellular vesicles for renal repair. Curr Gene Ther 17:29–42
Peired AJ, Sisti A, Romagnani P (2016) Mesenchymal stem cell-based therapy for kidney disease: a review of clinical evidence. Stem Cells Int 2016:4798639
Rodriguez-Rodriguez A, Egea-Guerrero JJ, Murillo-Cabezas F, Carrillo-Vico A (2014) Oxidative stress in traumatic brain injury. Curr Med Chem 21:1201–1211
Rooney GE, Moran C, McMahon SS, Ritter T, Maenz M, Flugel A, Dockery P, O'Brien T, Howard L, Windebank AJ, Barry FP (2008) Gene-modified mesenchymal stem cells express functionally active nerve growth factor on an engineered poly lactic glycolic acid (PLGA) substrate. Tissue Eng Part A 14:681–690
Salehi H, Amirpour N, Razavi S, Esfandiari E, Zavar R (2017) Overview of retinal differentiation potential of mesenchymal stem cells: a promising approach for retinal cell therapy. Ann Anat 210:52–63
Sevivas N, Teixeira FG, Portugal R, Araujo L, Carrico LF, Ferreira N, Vieira da Silva M, Espregueira-Mendes J, Anjo S, Manadas B, Sousa N, Salgado AJ (2017) Mesenchymal Stem Cell Secretome: A Potential Tool for the Prevention of Muscle Degenerative Changes Associated With Chronic Rotator Cuff Tears. Am J Sports Med 45:179–188
Thompson HJ, McCormick WC, Kagan SH (2006) Traumatic brain injury in older adults: epidemiology, outcomes, and future implications. J Am Geriatr Soc 54:1590–1595
Tseng WL, Chou SJ, Chiang HC, Wang ML, Chien CS, Chen KH, Leu HB, Wang CY, Chang YL, Liu YY, Jong YJ, Lin SZ, Chiou SH, Lin SJ, Yu WC (2017) Imbalanced production of reactive oxygen species and mitochondrial antioxidant SOD2 in Fabry disease-specific human induced Pluripotent stem cell-differentiated vascular endothelial cells. Cell Transplant 26:513–527
Uttara B, Singh AV, Zamboni P, Mahajan RT (2009) Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. Curr Neuropharmacol 7:65–74
Wang S, Xu P, Li X, Su X, Chen Y, Wan L, Fan L, Yin K, Liu Y, Zhao RC (2016) Mesenchymal stem cells and cell therapy for bone repair. Curr Mol Pharmacol 9:289–299
Xu L, Emery JF, Ouyang YB, Voloboueva LA, Giffard RG (2010) Astrocyte targeted overexpression of Hsp72 or SOD2 reduces neuronal vulnerability to forebrain ischemia. Glia 58:1042–1049
Yi HG, Yahng SA, Kim I, Lee JH, Min CK, Kim JH, Kim CS, Song SU (2016) Allogeneic clonal mesenchymal stem cell therapy for refractory graft-versus-host disease to standard treatment: a phase I study. Korean J Physiol Pharmacol 20:63–67
Yuan J, Wang A, He Y, Si Z, Xu S, Zhang S, Wang K, Wang D, Liu Y (2016) Cordycepin attenuates traumatic brain injury-induced impairments of blood-brain barrier integrity in rats. Brain Res Bull 127:171–176
Zhang X, Huang F, Chen Y, Qian X, Zheng SG (2016) Progress and prospect of mesenchymal stem cell-based therapy in atherosclerosis. Am J Transl Res 8:4017–4024
Zhang Z, Lang J, Cao Z, Li R, Wang X, Wang W (2017) Radiation-induced SOD2 overexpression sensitizes colorectal cancer to radiation while protecting normal tissue. Oncotarget 8:7791–7800
Zhao Y, Gibb SL, Zhao J, Moore AN, Hylin MJ, Menge T, Xue H, Baimukanova G, Potter D, Johnson EM, Holcomb JB, Cox CS Jr, Dash PK, Pati S (2016) Wnt3a, a protein secreted by Mesenchymal stem cells is Neuroprotective and promotes Neurocognitive recovery following traumatic brain injury. Stem Cells 34:1263–1272
Funding
This work was supported by Medical and Healthy Technology Development Program of Shandong Province (2015WS0069).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure of potential conflicts of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 361 kb)
Rights and permissions
About this article
Cite this article
Shi, X., Bai, Y., Zhang, G. et al. Effects of over-expression of SOD2 in bone marrow-derived mesenchymal stem cells on traumatic brain injury. Cell Tissue Res 372, 67–75 (2018). https://doi.org/10.1007/s00441-017-2716-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-017-2716-7