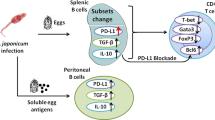
Abstract
Galectin-3 is a β-galactoside-binding protein with an inhibitory role in B cell differentiation into plasma cells in distinct lymphoid tissues. We use a model of chronic schistosomiasis, a well-characterized experimental disease hallmarked by polyclonal B cell activation, in order to investigate the role of galectin-3 in controlling IgA production through peritoneal B1 cells. Chronically infected, galectin-3-deficient mice (Lgals3 −/−) display peritoneal fluid hypercellularity, increased numbers of atypical peritoneal IgM+/IgA+ B1a and B1b lymphocytes and histological disturbances in plasma cell niches when compared with Lgals3 +/+ mice. Similar to our infection model, peritoneal B1 cells from uninfected Lgals3 −/− mice show enhanced switching to IgA after in vitro treatment with interleukin-5 plus transforming growth factor-β (IL-5 + TGF-β1). A higher number of IgA+ B1a lymphocytes was found in the peritoneal cavity of Lgals3 −/−-uninfected mice at 1 week after i.p. injection of IL-5 + TGF-β1; this correlates with the increased levels of secreted IgA detected in the peritoneal fluid of these mice after cytokine treatment. Interestingly, a higher number of degranulated mast cells is present in the peritoneal cavity of uninfected and Schistosoma mansoni-infected Lgals3 −/− mice, indicating that, at least in part, mast cells account for the enhanced differentiation of B1 into IgA-producing B cells found in the absence of galectin-3. Thus, a novel role is revealed for galectin-3 in controlling the expression of surface IgA by peritoneal B1 lymphocytes; this might have important implications for manipulating the mucosal immune response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Schistosomiasis represents a critical illness in developing countries and affects more than 207 million people. It is caused by the trematode Schistosoma mansoni, which promotes a chronic liver fibrotic disease (Utzinger et al. 2009). The pathogenesis of schistosomiasis results from the penetration of early parasite larvae (cercariae) into the skin of humans or mice hosts and by egg-laying adult worms inhabiting the mesentery. The eggs are frequently drained to the hepatic portal system and liver parenchyma evoking an acute-to-chronic progressive fibrogranulomatous reaction in host tissues (Andrade 2009; Borojevic 1992). The hallmarks of chronic phase are liver fibrosis and hepatomegaly, splenomegaly correlated with polyclonal B cell activation, extramedullary hematopoiesis and peritoneal responsiveness associated with macrophage hyperactivity (El-Cheikh et al. 1994). In addition, soluble schistosoma-antigens and increased circulating levels of cytokines continuously stimulate peritoneal B cells during schitosomiasis (Pinho et al. 2005; Weinberg et al. 1992). In particular, peritoneal B1 lymphocytes have been shown to switch from IgM to IgE during S. mansoni infection (Oliveira et al. 2005).
S. mansoni synthesizes immunogenic glycoproteins-containing polylactosamines that are recognized by endogenous glycan-binding proteins such as galectin-3 and elicits a robust humoral immune response (Nyame et al. 1999; Van de Vijver et al. 2006; van den Berg et al. 2004). Galectin-3, a 30-kDa protein characterized by having a carbohydrate recognition domain (CRD) and an N-terminal regulatory domain, is currently considered a biomarker in chronic diseases, including heart and liver fibrosis (de Boer et al. 2014; Henderson and Sethi 2009). Galectin-3 is highly expressed by liver cells located around the intrahepatic granulomas during chronic schistosomiasis. Recently, we demonstrated that S. mansoni-infected Lgals3 −/− mice exhibit abnormal plasmacytosis in the bone marrow, mesenteric lymph nodes and spleen followed by significant hyperglobulinemia (Brand et al. 2012; Oliveira et al. 2007, 2011). However, the involvement of galectin-3 in B cell physiology is far from being completely understood and only a few reports in the literature address the role of galectin-3 on B cell activation/differentiation. Kimata (2002) first reported that neutrophils could control IgE+ B cell differentiation via galectin-3 during IgE-associated atopic eczema/dermatitis syndrome. An interesting report on the role of galectin-3 in interleukin-4 (IL-4)-induced B cell commitment toward a memory phenotype was then published by Acosta-Rodríguez et al. (2004). Using Lgals3 −/− mice to study B1 cell physiology, we demonstrated that galectin-3 can act as an inhibitor of peritoneal and conventional B cell differentiation into plasma cells (Oliveira et al. 2007, 2009). Recently, by means of an autoantibody transgene model, Clark et al. (2013) revealed that the absence of galectin-3 leads to a significant increase in the number of Tg spleen B cells, thus interfering with B cell fate during autoantibody production and autoimmunity (Clark et al. 2013).
In the current study, we investigate whether galectin-3 controls B cell production of IgA during experimental chronic schistosomiasis and under treatment with cytokines that enhance IgA-class switching. Our data demonstrate that peritoneal B1 cells derived from both S. mansoni-infected or cytokine-treated Lgals3 −/− mice express higher levels of IgA on their surface in comparison with Lgals3 +/+ control mice. In addition, the lack of galectin-3 also correlates with high levels of secretory IgA in the peritoneal fluid and increased numbers of degranulated mast cells in the peritoneal cavity. These data suggest a novel role for galectin-3 in regulating peritoneal B1 cell activation and differentiation into IgA-secreting B1 lymphocytes.
Materials and methods
Mice and infection with Schistosoma mansoni
Inbred wild-type (WT) C57/bl6 (Lgals3 +/+) and galectin-3-deficient mice (Lgals3 −/−; Hsu et al. 2000) that were age- and sex-matched were obtained from the colony bred at the Federal University of Rio de Janeiro, Brazil. All procedures with mice were performed in accordance with institutional guidelines (protocol no. DAHEICB 070, Federal University of Rio de Janeiro). Mice of 4–6 weeks of age were infected by the transcutaneous penetration of 40 S. mansoni cercariae (BH strain, Oswaldo Cruz Institute/RJ, Brazil) and killed under carbon dioxide in a chamber at 90–95 days after infection, corresponding to the chronic phase of the disease (Dutra et al. 1998). Uninfected mice were used as experimental controls during in vivo assays.
Peritoneal cellularity and cytosmears
Resident peritoneal cells obtained from WT and Lgals3 −/− infected mice were harvested under sterile conditions after injection of 10 ml phosphate-buffered saline (PBS), pH 7.2, supplemented with 3 % fetal bovine serum into the abdominal cavity. Peritoneal leukocytes were counted by using a hemocytometer. Cytosmears were performed with 2.0 × 104 cells in 300 μl PBS, centrifuged at 36g for 3 min (Thermo Scientific Cytospin 4 Cytocentrifuge, Mass., USA), fixed in absolute methanol by 24 h and stained with May-Grünwald-Giemsa (El-Cheikh and Borojevic 1990). Morphological analysis was performed by using high-power microscopy (Zeiss-Axioplan, Germany). The images were acquired by bright field microscopy via a camera (Evolution MP 5.0 RTV-Color-Media Cybernetics, Canada).
Flow cytometry: DNA content and phenotypic analysis
Cell cycle analysis was performed according to Vindelov’s protocol (Vindeløv 1985). Briefly, peritoneal cells (5 × 105 cells per mouse) were resuspended in 500 μl propidium iodide solution (PBS, 0.1 % Triton X-100, 0.1 % RNAse, 50 μg/ml propidium iodide; Sigma Aldrich, USA) and incubated on ice for 5 min. For the phenotypic analysis, approximately 1 × 106 cells/ml obtained from the peritoneal wash were incubated with Fc block (Clone 2.4G2; Cell Bank of Rio de Janeiro) for 20 min before the addition of the following monoclonal antibodies: fluorescein isothiocyanate (FITC) conjugated to anti-IgM and anti-CD3; phycoerythrin (PE) conjugated to anti-IgA and anti-CD19; peridinin chlorophyll (PerCP) conjugated to anti-CD5 and anti-CD45; allophycocyanin (APC) conjugated to anti-B220 (BD Bioscience, USA). Samples were examined in a flow cytometer (FACSCalibur, BD Bioscience, USA) and analyzed by using CellQuestPro (BD Bioscence, USA). Total B cells were characterized as B220+CD19+CD45+CD3− cells. Peritoneal B cells were phenotypically identified as B1a cells (B220lowCD5lowIgMhigh cells), B1b (B220lowCD5negIgMhigh cells) and B2 cells (B220highCD5negIgMlow cells). Peritoneal B cells were also selected based on their morphometric features by using forward scatter (FSC) and side scatter (SSC) parameters.
Interleukin-5 and transforming growth factor-β1 induction in vitro and in vivo
For the in vitro analysis, peritoneal cells (5 × 105 cells/ml) obtained from non-infected WT and galectin-3−/− mice were cultured in DMEM (Dulbecco’s modified Eagle medium) supplemented with 10 % fetal bovine serum and antibiotics (penicillin and streptomycin) at 37 °C under a 5 % CO2 atmosphere. Interleukin-5 (IL-5) was obtained from a supernatant of a XR63-IL5 (Cell Bank of Rio de Janeiro) cell line transfected with IL-5 cDNA (Karasuyama and Melchers 1988). IL-5 and transforming growth factor-β1 (TGF-β1; 2 ng/ml; Sigma-Aldrich, USA) were used to induce IgA-class switching. For the in vivo analysis, a single dose of DMEM (0.5 ml) supplemented with IL-5 and TGF-β1 was injected into the peritoneal cavity of WT and Lgals3 −/− mice. The phenotype and morphological analyses of cells (in vitro) and mice (in vivo) were performed by flow cytometry and optical microscopy, respectively, after 1 week of treatment with the cytokines under both experimental conditions. Control groups were cultured or injected with medium alone. Trypan blue exclusion was used to evaluate cell viability in the culture systems. Under all experimental conditions, cell viability was more than 90 % after 1 week of culture.
Immunocytochemistry
Anti-CD138 was used to investigate the presence of plasma cells after cytokine induction. At 1 week after stimulation, peritoneal cells from non-infected WT and galectin-3−/− mice were collected by cytospin on poly-L-lysine-coated coverslips. The samples were fixed for 15 min in 4 % paraformaldehyde in PBS pH 7.4 at room temperature. A permeabilization step was not required because CD138 is preferentially detected on the cell membrane. Cells were incubated with anti-CD138 (BD Bioscience, USA) and counterstained with Harris’ hematoxylin. Images were acquired by bright field microscopy via a camera (Evolution MP 5.0 RTV-Color-Media Cybernetics, Canada).
IgA and IgM secretion
Wild-type and Lgals3 −/− mice were injected intraperitoneally with IL-5 (5 ng/ml) and TGF-β1 (10 ng/ml), whereas PBS-injected mice were used as negative controls. The serum and peritoneal lavage fluid of WT and galectin-3−/− mice were collected (7 and 14 days after stimulation) and analyzed individually by enzyme-linked immunosorbent assay (ELISA) according to the manufacturer’s instructions (Mabtech, Sweden). The optical density was measured by an ELISA microplate reader (Thermo Scientific, Mass., USA) and the absorbance values were directly proportional to the concentration of secretory IgA and IgM.
Mast cell count
Peritoneal cells were cytocentrifuged for 3 min (Thermo Scientific Cytospin 4 Cytocentrifuge) and fixed in absolute methanol for 24 h. Mast cells were identified after metachromatic staining with May-Grünwald Giemsa. Mast cells containing cytoplasmic granules were considered as non-activated cells, whereas degranulated mast cells were considered as activated cells. In total, 300 cells per sample/mouse were counted and the percentage value to mast cells was quantified.
Histological analysis of mesentery and omentum
For histological analysis of the omentum, the abdominal cavity of WT and Lgals3 −/− infected mice (5 animals per group) was exposed in order to remove the mesenteric membranes and omentum as described elsewhere (Pinho et al. 2005). Immediately after extirpation, the omentum was fixed for 24 h in 10 % buffered formalin, dehydrated and embedded in paraffin. Tissue sections (5 μm thick) were stained with hematoxilin and eosin or processed for further immunohistochemistry analysis (Oliveira et al. 2011). The tissue was analyzed by a light microscope (Zeiss-Axioplan, Jena, Germany) and images were acquired by bright field microscopy via a camera (Evolution MP 5.0 RTV-Color-Media Cybernetics, Canada).
Immunohistochemistry
Paraffin-embedded sections of the omentum from WT and Lgals3 −/− infected mice (5 animals per group) were dewaxed and hydrated. After inhibition of endogenous peroxidase, sections were incubated for 1 h with 0.01 M PBS containing 5 % bovine serum albumin, 4 % skim milk, 0.1 % Triton X-100 (Sigma Aldrich, USA), 0.05 % Tween-20 and 10 % normal goat serum. The following purified antibodies were used: anti-galectin-3 (M3/38; ATCC, USA), anti-CD138 and Blimp-1 (Santa Cruz Biotechnology, USA). Bound antibodies were detected by using a biotinylated anti-rat IgG (BA-4001, Vector Laboratories, USA) followed by incubation with avidin-peroxidase (Sigma-Aldrich, USA) and then revealed by using diaminobenzidine as the chromogen. Sections were counterstained with Harris’ hematoxylin. The images were acquired by bright field microscopy via a camera (Evolution MP 5.0 RTV-Color-Media Cybernetics, Canada). As negative controls, sections of WT and knockout mice tissues were incubated with non-immune rat serum, instead of anti-galectin-3 antibody. Positive cells were quantified by using Image J software.
Statistical analysis
The statistical analyses were performed by using Tukey’s multiple comparison test (t-test); the significance threshold was fixed at P ≤ 0.05.
Results
Galectin-3 controls cellular proliferative status and decreases peritoneal B1b and B2 cell numbers during schistosomiasis
We previously reported that galectin-3 depletion caused a reduction in peritoneal cavity cellularity and favored B cell differentiation in non-infected mice (Oliveira et al. 2009). Therefore, Lgals3 −/− mice were considered an excellent model for studying the cellular events involving B cell responses. Here, we evaluated the peritoneal micromilieu in Lgals3 −/− mice that were chronically challenged with S. mansoni. During the chronic phase of infection, a marked polyclonal B cell activation occurred with enhanced peritoneal hyperresponsiveness (El-Cheikh et al. 1994). Since peritoneal cellularity was significantly reduced in uninfected Lgals3 −/− mice but substantially increased during infection with S. mansoni (Fig. 1a), we therefore investigated whether galectin-3 could modulate the proliferative status of peritoneal cells. The DNA content of peritoneal cells was analyzed by flow cytometry and we could observe a significant accumulation of cells in both the S and G2/M phases of the cell cycle in Lgals3 −/− infected mice in comparison with Lgals3 +/+ infected mice (Fig. 1b). In Lgals3 +/+ infected mice, cytosmears of peritoneal cells revealed neutrophils, monocytes, lymphocytes, mast cells (Fig. 1c), eosinophils and macrophages (Fig. 1d) dispersed in the peritoneal fluid. In infected Lgals3 −/− mice, we could observe all the mitotic phases, including prophase (Fig. 1e), metaphase (Fig. 1f) and anaphase and telophase (karyokinesis and cytokinesis, Fig. 1g, h, respectively).
Cellularity and morphological analysis of peritoneal cells in Lgals3 +/+ and Lgals3 −/− mice during schistosomiasis. Lgals3 +/+ or Lgals3 −/− mice were infected with Schistosoma mansoni and (a) the total number or (b) the cell cycle of peritoneal cells was evaluated (black bars wild-type mice, white bars Lgals3 −/− mice). Data represent the mean of three experiments (error bars standard deviation). *P < 0.05. Morphological analysis of cytosmears of both infected Lgals3 +/+ (c, d) and Lgals3 −/− mice (e–h) by light microscopy (arrows proliferative cells, mn monocyte, mc mast cell, ly lymphocyte, eo eosinophil, mo macrophage). Prophase (e), metaphase (f) anaphase and telophase, including karyokinesis (g) and cytokinesis (h). Magnification: ×400. Bars 10 μm
In order to identify a possible alteration in the balance of B cell subsets during chronic schistosomiasis in Lgals3 −/− mice, we monitored the phenotype of the peritoneal B cells. B cell subpopulations of Lgals3 +/+ and Lgals3 −/− infected mice were quantified according to their typical phenotype: B220lowCD5+ B1a lymphocytes (Fig. 2a, gate R2), B220lowCD5neg B1b lymphocytes (Fig. 2a, gate R3) and B220highCD5neg conventional or B2 cells (Fig. 2a, gate R4). The number of B1a lymphocytes was significantly decreased, whereas both B1b and B2 lymphocytes were numerically increased in the peritoneal cavity of infected galectin-3−/− mice (Fig. 2b). Noticeably, peritoneal cellularity and especially the B lymphocyte compartment of S. mansoni-infected Lgals3 −/− mice were affected by the absence of galectin-3 when compared with Lgals3 +/+ mice. These results suggest that galectin-3 inhibits B cell proliferation/differentiation and exerts a negative effect on B1 cell accumulation in the peritoneal cavity during infection with S. mansoni.
Phenotype of peritoneal B lymphocytes. Peritoneal B subpopulations of control and S. mansoni-infected Lgals3 +/+ and Lgals3 −/− mice were identified according to B220 and CD5 expression. a B1a lymphocytes (B220+CD5+ cells, gate R2), B1b lymphocytes (B220lowCD5− cells, gate R3) and B2 lymphocytes (B220highCD5− cells, gate R3). b Bar graph representative of the absolute number of each B cell subtype. c, d Histograms represent expression of sIgM and sIgA by B1a cells. e Absolute number of B1a IgA+ cells. f, g Histograms represent expression of sIgM and sIgA by B1b cells. h Absolute number of B1b IgA+ cells. i, j Histograms represent expression of sIgM and sIgA by B2 cells. k Number of B2 IgA+ cells. Black bars represent Lgals3 +/+ mice, white bars represent Lgals3 −/− mice, gray histograms represent S. mansoni-infected Lgals3 +/+ mice, empty histograms indicate S. mansoni-infected Lgals3 −/− mice, dashed histograms represent isotype control. Data are representative of three experiments with three mice per group. *P < 0.05. Antibodies: allophycocyanin conjugated to anti-B220 (B220-APC), peridinin chlorophyll conjugated to anti-CD5 (CD5-PerCP), fluorescein isothiocyanate conjugated to anti-IgM (IgM-FITC) and phycoerythrin conjugated to anti-IgA (IgA-PE)
Galectin-3 inhibits differentiation of peritoneal B1 cells into IgA+ plasma cells during chronic schistosomiasis
Lgals3 −/− mice chronically infected by S. mansoni have previously been reported to exhibit high levels of serum immunoglobulins (Igs), suggesting a potential regulatory role for galectin-3 in Igs production (Oliveira et al. 2007). Therefore, we evaluated whether the absence of galectin-3 interferes with Ig expression on peritoneal B cell subpopulations during the chronic phase of the disease. As B1 cells in mucosa-associated tissues are an important source of IgA-producing cells (Bao et al. 1998; Roy et al. 2013), we monitored the expression of surface IgA (sIgA) and IgM (sIgM) on peritoneal B1 cells in our model of infection. We observed that peritoneal B1a lymphocytes from Lgals3 −/− infected mice expressed lower levels of sIgM (Fig. 2c) and higher levels of sIgA (Fig. 2d) in comparison with Lgals3 +/+ infected mice. Indeed, we observed a four-fold increase in the number of IgA+ B1a cells in Lgals3 −/− infected mice compared with Lgals3 +/+ infected mice (Fig. 2e). Taking into account that all cells were positive for IgM, we assumed that B1a IgA+ cells also expressed IgM on the membrane.
We also found that, in B1b lymphocytes from infected Lgals3 −/− mice, the levels of sIgM were reduced (Fig. 2f), whereas the expression of sIgA was significantly increased (Fig. 2g), in comparison with Lgals3 +/+ infected mice. Moreover, the number of peritoneal IgA+ B1b cells was increased approximately 15-fold in the absence of galectin-3 (Fig. 2h). On the other hand, the expression of sIgM and sIgA by conventional B2 lymphocytes and the number of B2 IgA+ cells did not change in the absence of galectin-3 (Fig. 2i). These results indicate that galectin-3 negatively affects the terminal differentiation of B1a and B1b lymphocytes into IgA-producing plasma cells during chronic schistosomiasis.
Galectin-3 impairs IL-5/TGF-β-induced IgA-class switching in vitro
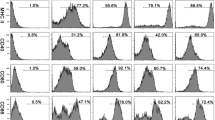
In order to verify whether B cells of uninfected Lgals3 −/− mice also display higher expression of surface IgA, we induced IgA-class switching by in vitro stimulation with IL-5 and TGF-β1, two master cytokines that promote IgA synthesis (Stavnezer and Kang 2009). Peritoneal cells from Lgals3 +/+ or Lgals3 −/− mice were stimulated in vitro with IL-5 and TGF-β1 for 1 week. Flow cytometry analysis revealed that B220neg/low IgA+ cells of galectin-3−/− mice were significantly increased after cytokine treatment when compared with cells of Lgals3 +/+ mice (Fig. 3a, gate R2, lower dot plot). Although the absolute number of total B cells (total B220+ cells) from both Lgals3 +/+ and Lgals3 −/− mice did not change after cytokine treatment (Fig. 3b), the number of B220neg/lowIgA+ cells increased approximately 4.5-fold in the presence of galectin-3 and about 9.8-fold in the absence of galectin-3 (Fig. 3c). Accordingly, the number of B220+IgAneg cells was proportionally reduced in both Lgals3 +/+ and Lgals3 −/− cells after cytokine treatment (Fig. 3d). The expression of sIgM on cultured peritoneal cells was also monitored in control and cytokine-treated groups. Lgals3 +/+ and Lgals3 −/− B cells co-expressing B220 and sIgM were predominant in control groups (Fig. 3e, f, gates R2, R3, respectively). Interestingly, the numbers of sIgMLowB220neg/Low cells were higher in peritoneal Lgals3 −/− B cells before (Fig. 3e, f) and after (Fig. 3g, h) treatment with IL-5 and TGF-β when compared with peritoneal B cells from Lgals3 +/+ mice. These data suggest that galectin-3 deletion accelerates IL-5/TGF-β-induced IgA-class switching.
IgA-class switching after interleukin-5 (IL-5) and transforming growth factor-β1 (TGF-β1) treatment in vitro. Peritoneal cells from Lgals3 +/+ or Lgals3 −/− mice were cultured in the presence or absence of IL-5 and TGF-β1 for 1 week. a B220 and IgA expression was evaluated by flow cytometry. b Absolute number of B cells (B220+ cells) was quantified. c Determination of number of B220+IgA+ cells of wild-type (Lgals3 +/+) and galectin-3−/− (Lgals3 −/−) mice. d Determination of B220+IgA− cells of Lgals3 +/+ and Lgals3 −/− mice in control (−) and cytokine-treated (+) cells. e–h IgM and B220 expression on the peritoneum of (e) control Lgals3 +/+ cells, (f) control Lgals3 −/− cells, (g) cytokine-treated Lgals3 +/+ cells and (h) cytokine-treated Lgals3 −/− cells was analyzed by flow cytometry. Gate R2 includes B220+IgMhigh cells, Gate R3 includes B220+IgMint cells and Gate R4 includes B220low/-IgMLow cells. These data are representative of three independent experiments with three mice per group. *P < 0.05, **P < 0.01
Galectin-3 impairs IL-5/TGF-β-induced IgA-class switching in peritoneal B1a lymphocytes
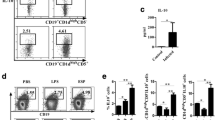
In order to study the effects of IL-5 and TGF-β on peritoneal B cell differentiation into IgA+ cells in vivo, Lgals3 +/+ and uninfected Lgals3 −/− mice were treated intraperitoneally with both cytokines. After 1 week, peritoneal cells were harvested and analyzed by flow cytometry. FSC x SSC parameters were used to distinguish small lymphocytes, large lymphocytes and granulocytes (Fig. 4a-d). Large lymphocytes were selected in R1 and B220+ cells were analyzed in the subsequent experiments. B220+IgA+ cells from Lgals3 +/+ unstimulated control mice represented 4.4 ± 0.9 % of the total peritoneal cells and increased to 10.3 ± 1.4 % after cytokine stimulation (Fig. 4a, b). On the other hand, in Lgals3 −/− unstimulated control mice, we found a percentage of B220+IgA+ cells of 3.5 ± 0.8 % of the total peritoneal cells (Fig. 4c); this increased to 26.9 ± 2.1 % after IL-5 and TGF-β treatment (Fig. 4d). Treatment with IL-5 and TGF-β resulted in a 2.86-fold increase in the absolute number of sIgA+ peritoneal B cells in Lgals3 +/+ mice and a 6.11-fold increase in Lgals3 −/− treated mice (Fig. 4e) compared with the untreated controls.
B1a lymphocytes respond promptly to IL-5 and TGF-β1 induction in vivo in the absence of galectin-3. IL-5 and TGF-β1 cytokines were injected i.p. at 1 week before phenotypic analysis. Control Lgals3 +/+ mice (a) exhibited 4.4 % of peritoneal cells positive to IgA, whereas cytokine-treated Lgals3 +/+ mice (b) increased their number of IgA+ cells to 10.3 % of peritoneal cells. Control Lgals3 −/− mice (c) showed 3.5 % of peritoneal cells positive to IgA. Cytokine-treated Lgals3 −/− mice (d) increased to 26.9 % the peritoneal cells positive to IgA. Absolute number of cells expressing B220 and IgA (e). Flow cytometry of peritoneal cells derived from Lgals3 +/+ or Lgals3 −/− mice treated with IL-5 and TGF-β1 cytokines. Approximately 50 % of B220+ IgA+ cells of Lgals3 +/+ mice (f) and 69 % of peritoneal B220+IgA+ cells of Lgals3 −/− mice (g) were CD5+. Absolute number of B1 cells from Lgals3 +/+ or Lgals3 −/− mice treated with IL-5 and TGF-β1 cytokines (h). Black bars represent Lgals3 +/+ mice, white bars represent Lgals3 −/− mice. Data are representative of three experiments with three mice per experimental group. *P < 0.05, **P < 0.01
In order to calculate the percentage of B1a and B1b cells, we monitored the expression of CD5, which is present on B1a but not on B1b cells. In Lgals3 −/− mice, approximately 69 % of peritoneal cells co-expressed sIgA and CD5 (IgA+CD5Low cells), in comparison with 50 % of peritoneal cells from Lgals3 +/+ mice (Fig. 4f, g). In Lgals3 −/−-treated mice, an approximately three-fold increase was seen in the number of peritoneal IgA+ B1a cells in comparison with Lgals3 +/+ treated mice (Fig. 4h). These results indicate that galectin-3 deletion favors the differentiation of B1a cells into IgA-producing cells after in vivo stimulation with IL-5 and TGF-β.
Galectin-3 inhibits IgA and IgM secretion in peritoneal cavity
Since B cells of Lgals3 −/− mice expressed high levels of surface IgA, we sought to measure the levels of IgM and IgA in the serum and peritoneal fluid of both Lgals3 +/+ and Lgals3 −/− mice in response to IL-5 and TGF-β stimulation. IgA serum levels did not change significantly in Lgals3 +/+ and Lgals3 −/− mice, even after cytokine stimulation (Fig. 5a). On the other hand, Lgals3 −/− mice displayed higher levels of peritoneal IgA before and after treatment with IL-5 and TGF-β in comparison with Lgals3 +/+ mice (Fig. 5b). The levels of IgM in the serum and peritoneal fluid were also increased in untreated Lgals3 −/− mice and did not change after the treatment with cytokines (Fig. 5c, d). On average, the levels of peritoneal IgA were 1.5-fold higher in untreated and cytokine-treated Lgals3 −/− mice (Fig. 5e). Untreated Lgals3 −/− mice showed a two-fold higher level of peritoneal IgM; however, no difference was detected in IgM levels between Lgals3 +/+ and Lgals3 −/− mice at 7 days after cytokine treatment (Fig. 5f). Together, these data indicate that galectin-3 negatively modulates IgA secretion by peritoneal cavity B cells upon stimulation with IL-5 and TGF-β.
IgA and IgM levels in serum and in peritoneal fluid from Lgals3 +/+ and Lgals3 −/− mice treated with IL-5 and TGF-β1. The levels of IgA were evaluated in the serum (a) and peritoneal liquid (b) of Lgals3 +/+ and Lgals3 −/− mice following treatment with IL-5 and TGF-β1 cytokines for 7 and 14 days. Additionally, the levels of IgM were quantified in the serum (c) and peritoneal fluid (d). Graphs showing the relative increase in the peritoneal levels of (e) IgM and (f) IgA. Data are illustrated as fold-change relative to Lgals3 +/+ mice. Black bars represent Lgals3 +/+ mice, white bars represent Lgals3 −/− mice. Data are representative of two experiments with five mice per experimental group. *P < 0.05, **P < 0.01
Galectin-3 negatively controls mast cell degranulation in peritoneal cavity
Mast cells have been previously demonstrated to enhance B cell expansion and to drive B cells toward differentiation into IgA-producing plasma cells (Merluzzi et al. 2010). Therefore, in order to investigate further the mechanism behind the enhanced production of sIgA found in Lgals3 −/− mice, we next quantified the number of degranulated mast cells present in the peritoneal cavity of Lgals3 −/− and Lgals3 +/+ mice. Three times more degranulated mast cells were found in the peritoneal cavity of S. mansoni-infected Lgals3 −/− mice in comparison with S. mansoni-infected Lgals3 +/+ mice (Fig. 6a, d, e). Interestingly, when cells from the peritoneal cavity from uninfected Lgals3 −/− and Lgals3 +/+ mice were stimulated in vitro (Fig. 6b, f, g) or in vivo (Fig. 6c, h, i) with IL-5 + TGF-β1, we still found increased numbers of degranulated mast cells in the absence of galectin-3. These data indicate that mast cell degranulation/activation accounts, at least in part, for the increased number of IgA-producing plasma cells found in Lgals3 −/− mice.
Mast cell degranulation in vivo and in vitro in the absence of galectin-3. Peritoneal mast cells were identified according to the cytoplasm degranulation in the chronic phase of schistosomiasis. Data are shown as the percentage of degranulated mast cells under control conditions (a) and after IL-5 and TGF-β1 treatment in vitro (b) and in vivo (c). In all situations, more activated mast cells were found in the absence of galectin-3. Black bars indicate Lgals3 +/+ mice, white bars represent Lgals3 −/− mice. These data are representative of three independent experiments with three mice per group. *P < 0.05. Cytosmears showed granulated mast cells (GM) and degranulated mast cells (DM) in the peritoneal fluid of wild-type (d) and Lgals3 −/− mice (e) infected with S. mansoni. After 1 week of cytokine treatment in vitro, non-activated and activated mast cells derived from Lgals3 +/+ (f) and Lgals3 −/− (g) mice could be identified. The same pattern was observed in cytosmears of peritoneal fluid obtained from Lgals3 +/+ (h) and Lgals3 −/− (i) mice. Magnification: ×400. Bars 10 μm
Galectin-3 restrains plasma cell response in mesentery and omentum following S. mansoni infection
Taking into account the results described so far, we decided to investigate the presence of plasma cell niches in the omentum and mesentery during chronic schistosmiasis. Plasma cells were only rarely found in the mesentery of Lgals3 +/+ infected mice (Fig. 7a) but were found frequently attached to the mesentery of Lgals3 −/− infected mice (Fig. 7b). We next evaluated the histological architecture of the omentum, a coelomic-derived tissue involved in B cell responses against abdominal antigens (Rangel-Moreno et al. 2009) and receiving activated B cells migrating from the peritoneal cavity (Carlow et al. 2009). In Lgals3 +/+ infected mice, the omentum was strongly cellularized and various types of cells could be identified, such as granulocytes, lymphocytes and plasma cells (Fig. 7c). The omentum of Lgals3 −/− infected displayed fewer cells in comparison with Lgals3 +/+ infected mice (Fig. 7d, k). In order to quantify the number of plasma cells in the omentum of Lgals3 +/+ and Lgals3 −/− infected mice, we stained tissue sections with anti-CD138 and anti-Blimp-1 antibodies. Both CD138 and Blimp-1 are plasma cell markers but the latter identifies Ig-secreting plasma cells. CD138+ plasma cells were preferentially confined to perivascular spaces in Lgals3 +/+ infected mice (Fig. 7e). On the other hand, a higher number of CD138+ plasma cells was found randomly dispersed throughout the omental parenchyma of Lgals3 −/− infected mice in comparison with Lgals3 +/+ infected mice (Fig. 7f, l). Blimp-1+ plasma cells were dominantly observed in well-defined milky spot-like structures in Lgals3 +/+ infected mice (Fig. 7g), whereas in Lgals3 −/− infected mice, we found a higher number of Blimp-1+ plasma cells in distinct histological regions of the omentum (Fig. 7h, m). Interestingly, galectin-3 was expressed in a wide range of cells types in omental tissue, predominantly at perivascular niches and inside blood vessels (Fig. 7i, insert). As expected, galectin-3-expressing cells were not detected in the omentum of Lgals3 −/− infected mice (Fig. 7j).
Photomicrographs of mesentery and omentum reveal disturbances on plasma cell niches in the absence of galectin-3 during chronic schistosomiasis. Mesentery of Lgals3 +/+ mice (a) with mast cells (arrow), monocytes/macrophages (arrowhead) and lymphocytes (asterisk) and of Lgals3 −/− mice (b) predominantly occupied by lymphocytes (asterisk) and plasma cells (arrows) as stained with May-Grünwald Giemsa (MGG). Omentum sections of Lgals3 +/+ and Lgals3 −/− mice were stained with hematoxilin and eosin (H&E; c, d, respectively) or immunostained for CD138 (e, f, respectively), Blimp-1 (g, h, respectively) and galectin-3 (i, j, respectively). As expected, omental cells did not express galectin-3 in Lgals3 −/− mice. Number of cells per area (cells/μm2; k), number of CD138-positive plasma cells (l) and number of Blimp-1-positive Ig-secreting cells (m) counted in the omentum. Black bars represent Lgals3 +/+ mice, white bars represent Lgals3 −/− mice. Data are representative of three independent experiments with three mice per experimental group. *P < 0.05
The number of cells per area in the omentum of both Lgals3 +/+ and Lgals3 −/− infected mice was quantified according to the expression of CD138 and Blimp-1. In the absence of galectin-3, the omentum exhibited a reduced number of cells per 100 μm2 (Fig. 7k). On the other hand, the number of CD138+ cells (Fig. 7l) and Blimp-1+ cells (Fig. 7m) was significantly increased in these Lgals3 −/− infected mice. Taken together, our data demonstrate that galectin-3 deletion favors the accumulation of plasma cells in the mesentery and omentum.
Discussion
The inhibitory effect of galectin-3 on B lymphocyte differentiation was originally demonstrated by Acosta-Rodriguez and colleagues using a Trypanosoma cruzi infection experimental model (Acosta-Rodríguez et al. 2004). Subsequently, we demonstrated that S. mansoni-infected Lgals3 −/− mice have hyperglobulinemia and intense plasmacytogenesis in the bone marrow, mesenteric lymph nodes and spleen (Brand et al. 2012; Oliveira et al. 2007, 2011). Here, we propose a new regulatory role for galectin-3 in IgA+ plasma cell differentiation in the peritoneal cavity during chronic schistosomiasis inflammation and during IL-5 and TGF-β1 treatment in vitro and in vivo.
The absence of galectin-3 in the peritoneal cavity is favorable to the generation of a quantitative and qualitative B1a/B1b imbalance. During schistosomiasis, nearly 65 % of peritoneal cells display a DNA content compatible with a proliferative status in the absence of galectin-3 (accumulating in the S and G2/M phases of cell cycle), whereas only 25 % of Lgals3 +/+ peritoneal cells have been detected in the proliferative phase. On the other hand, a possible cell cycle arrest (Rieder 2011) and consequently more propensity to apoptosis cannot be excluded because galectin-3 is considered an anti-apoptotic molecule in various cell types (Hoyer et al. 2004; Matarrese et al. 2000; Nangia-Makker et al. 2007). Indeed, the peritoneal hypercellularity in Lgals3 −/− mice indicates a disorder in the proliferative status of these cells during chronic schistosomiasis but not after cytokine induction.
Previously, we have shown that peritoneal B1 cells from S. mansoni-infected mice switch from an IgM class to an IgE class (Oliveira et al. 2005) and that infected Lgals3 −/− mice present high levels of serum IgE during schistosomiasis (Oliveira et al. 2007). However, we found no differences in IgE+ B cells of Lgals3 +/+ and Lgals3 −/− mice (data not shown). As peritoneal B cells are committed to an IgA repertoire (Roy et al. 2013) and as high levels of IgA are found in the serum during schistosomiasis (Gaber et al. 2010), we monitored sIgA expression by peritoneal B cells and conclude that a significant correlation exists between galectin-3 and IgA+ differentiating plasma cells in the peritoneal cavity. Kracker and colleagues demonstrated that IgA/IgM co-expression is a remarkable event in the course of immunoglobulin class switching (Kracker and Durandy 2011) and our data indicate that galectin-3 is a potent regulator of IgA expression on B1 cells during chronic schistosomiasis and cytokine induction.
The concomitant expression of IgA and IgM on peritoneal B cells has been demonstrated preferentially in B1b cells (Roy et al. 2009). Here, we found, during chronic schistosomiasis, a higher number of peritoneal B1a- and B1b-IgA+ lymphocytes coexpressing sIgM in Lgals3 −/− mice. Nevertheless, the concomitant expression of IgA and IgM is also associated with IgA deficiency, as shown by Conley and Cooper (1981) who described that 90 % of patients presenting an IgA+IgM+ phenotype have a pathological blocker on IgA+ B cell differentiation during the IgA-class switch. Selective IgA deficiency is associated with a higher prevalence of infections and a variety of concomitant autoimmune diseases, including Graves’ disease, systemic lupus erythematosus, type 1 diabetes, celiac disease, myasthenia gravis and rheumatoid arthritis (Wang et al. 2011). Galectin-3 plays a pro-inflammatory role exacerbating the effects in autoimmune disorders (Radosavljevic et al. 2012), however the involvement of galectin-3 in IgA physiology is not fully understood. The absence of galectin-3 favors IgA accumulation on the membrane of B1a and B1b lymphocytes but the exact significance of these findings remains unclear.
Our results indicate that galectin-3 negatively regulates IgA expression or that galectin-3 inhibits the proliferation of peritoneal IgA+ B1 cells when challenged by appropriate factors. Our in vitro and in vivo data suggest that, at least in part, peritoneal B1 cells of Lgals3 +/+ and Lgals3 −/− mice do not proliferate after IL-5 and TGF-β1 treatment but that they differentiate into IgA+ cells. Interestingly, in the absence of galectin-3, the number of IgA+ B1 cells is significantly increased under both experimental conditions. IL-5 and TGF-β1 are essentials for IgA-class switching (Cerutti and Rescigno 2008) and the expression/synthesis of these cytokines can be modulated by galectin-3. IL-5 gene expression is down-regulated by galectin-3 in distinct cell types (Cortegano et al. 1998), whereas Lgals3 −/− mice present TGF-β-mediated myofibroblast activation and matrix production strongly inhibited after chronic CCL4-induced liver fibrosis (Henderson et al. 2006). Accordingly, TD139 (inhibitor of galectin-3) blocks TGF-β-induced β-catenin activation and attenuates progressive lung fibrosis after experimental bleomycin induction (Mackinnon et al. 2012). Based on data from the literature, we hypothesized that, in the absence of galectin-3, increased levels of IL-5 and TGF-β1 could account, at least in part, for the higher number of IgA+ B1 cells found in Lgals3 −/− mice.
Peritoneal B1 lymphocytes express IL-5R constitutively (Hitoshi et al. 1990) and higher levels of IL-5 in Lgals3 −/− mice (Oliveira et al. 2009) and promptly synthesize IgA (Takatsu et al. 2009). On the other hand, peritoneal B1 cells switch more readily to IgA than do splenic follicular or peritoneal B2 cells after B lymphocyte stimulator/lipopolysaccharide/TGF-β in vitro (Kaminski and Stavnezer 2006) and specifically, peritoneal B1b cells switch to IgA under the influence of the synergistic effect of TGF-β and retinoic acid (Roy et al. 2013). Indeed, we have arguments to suggest that galectin-3 plays a regulatory role on IgA+ cell differentiation controlling IL-5 and TGF-β functions in the peritoneal cavity.
Lgals3 +/+ and Lgals3 −/− mice intraperitoneally treated with IL-5 and TGF-β do not modify the IgA and IgM levels in their serum, suggesting a poor systemic effect on the IgA/IgM secretion dependent on galectin-3. On the other hand, the lack of galectin-3 significantly disturbs the peritoneal levels of IgA and IgM, indicating a potent local effect of galectin-3 during IgA and IgM secretion. Our experimental data show that IL-5 and TGF-β induce IgA secretion by peritoneal cells after 1 week of injection and normal levels of IgA can be detected 14 days post-induction. In Lgals3 −/− mice, cytokine induction modifies the kinetics of IgA secretion and after 14 days of treatment, the IgA levels remain extremely high in comparison with Lgals3 +/+ mice. As the IgA+ B1a cell subpopulation is markedly increased in Lgals3 −/− mice after cytokine induction, one can conclude that peritoneal B1a cell differentiation into IgA-secreting plasma cells is regulated by galectin-3, although the mechanisms remain unclear.
In vivo and in vitro experimental conditions revealed an intense plasmacytogenesis strictly associated with mast cell degranulation. Merluzzi and colleagues (2010) have recently shown that mast cells control B cell proliferation and regulate IgA+ plasma cell differentiation in secondary lymphoid organs. In parallel, Chen and colleagues (2006) proposed that galectin-3 has an important role in mast cell biology and revealed that mast cells of Lgals3 −/− secrete lower amounts of histamines and exhibit a reduced cutaneous anaphylaxis reaction when compared with Lgals3 +/+ mice. Although our data are not conclusive concerning the role of mast cells from Lgals3 −/− mice on peritoneal B1 lymphocyte activation, we have evidence that indicates mast cell degranulation, at least in part, as a possible cellular mechanism disturbed in the absence of galectin-3 and responsible for exacerbated IgM- to IgA-class switching on peritoneal B1 lymphocytes of Lgals3 −/− mice.
During schistosomiasis, peritoneal cells react against S. mansoni antigens (Panasco et al. 2010). The peritoneal cavity is a reservoir of circulating leukocytes, including monocytes, T and B lymphocytes and granulocytes frequently detected attached in the omentum and mesentery (Carlow et al. 2009; Lenzi et al. 1996). Since B1a and B1b lymphocytes were directly associated with high plasmacytogenesis in Lgals3 −/− infected mice, intraperitoneal plasma cell niches were studied and we found that the mesentery and omentum are widely disorganized in Lgals3 −/− mice chronically infected by S. mansoni. Whether the absence of galectin-3 damages the dynamics of peritoneal cell homing is uncertain but the high number of CD138+ plasma cells and Blimp-1+ immunoglobulin-secreting plasma cells indicates that galectin-3 has a relevant participation on peritoneal cell migration during inflammatory responses. In agreement with this hypothesis, perivascular galectin-3+ cells are frequently found in this organ and we sometimes observed cells expressing galectin-3 inside blood vessels. At least in part, we have evidence that the lack of galectin-3 modifies the scenario of moving peritoneal B cell and provokes an abnormal accumulation of plasma cells inside of the peritoneal cavity during chronic schistosomiasis.
In conclusion, we propose a novel regulatory role for galectin-3 on peritoneal B cell differentiation. Our results indicate that galectin-3 regulates a specific step of peritoneal B cell differentiation into IgA-secreting plasma cells during schistosomiasis and after IL-5 and TGF-β induction. Moreover, these data indicate that increased mast cell degranulation accounts for the higher number of IgA-producing plasma cells found in Lgals3 −/− mice. Thus, we suggest that both cell types should be investigated in future studies in order to determine the exact role of galectin-3 in regulating the cellular and molecular mechanisms for the induction of the mucosal immune response.
References
Acosta-Rodríguez EV, Montes CL, Motrán CC, Zuniga EI, Liu FT, Rabinovich GA, Gruppi A (2004) Galectin-3 mediates IL-4-induced survival and differentiation of B cells: functional cross-talk and implications during Trypanosoma cruzi infection. J Immunol 172:493–502
Andrade ZA (2009) Schistosomiasis and liver fibrosis. Parasite Immunol 31:656–663
Bao S, Beagley KW, Murray AM, Caristo V, Matthaei KI, Young IG, Husband AJ (1998) Intestinal IgA plasma cells of the B1 lineage are IL-5 dependent. Immunology 94:181–188
Berg TK van den, Honing H, Franke N, Remoortere A van, Schiphorst WE, Liu FT, Deelder AM, Cummings RD, Hokke CH, Die I van (2004) LacdiNAc-glycans constitute a parasite pattern for galectin-3-mediated immune recognition. J Immunol 173:1902–1907
Boer RA de, Velde AR van der, Mueller C, Veldhuisen DJ van, Anker SD, Peacock WF, Adams KF, Maisel A (2014) Galectin-3: a modifiable risk factor in heart failure. Cardiovasc Drugs Ther 28:237–246
Borojevic R (1992) Experimental murine schistosomiasis mansoni: establishment of the chronic phase of the disease. Mem Inst Oswaldo Cruz 87 (Suppl 4):171–174
Brand C, Oliveira FL, Takiya CM, Palumbo A Jr, Hsu DK, Liu F-T, Borojevic R, Chammas R, El-Cheikh MC (2012) The involvement of the spleen during chronic phase of Schistosoma mansoni infection in galectin-3(−/−) mice. Histol Histopathol 27:1109–1120
Carlow DA, Gold MR, Ziltener HJ (2009) Lymphocytes in the peritoneum home to the omentum and are activated by resident dendritic cells. J Immunol 183:1155–1165
Cerutti A, Rescigno M (2008) The biology of intestinal immunoglobulin A responses. Immunity 28:740–750
Chen HY, Sharma BB, Yu L, Zuberi R, Weng IC, Kawakami Y, Kawakami T, Hsu DK, Liu FT (2006) Role of galectin-3 in mast cell functions: galectin-3-deficient mast cells exhibit impaired mediator release and defective JNK expression. J Immunol 177:4991–4997
Clark AG, Weston ML, Foster MH (2013) Lack of galectin-1 or galectin-3 alters B cell deletion and anergy in an autoantibody transgene model. Glycobiology 23:893–903
Conley ME, Cooper MD (1981) Immature IgA B cells in IgA-deficient patients. N Engl J Med 305:495–497
Cortegano I, Pozo V del, Cárdaba B, Andrés B de, Gallardo S, Amo A del, Arrieta I, Jurado A, Palomino P, Liu FT, Lahoz C (1998) Galectin-3 down-regulates IL-5 gene expression on different cell types. J Immunol 161:385–389
Dutra HS, El-Cheikh MC, Azevedo SP, Rossi MI, Borojevic R (1998) Murine schistosomiasis mansoni: experimental analysis of bone marrow and peripheral myelopoiesis. Parasitol Res 84:668–675
El-Cheikh MC, Borojevic R (1990) Extramedullar proliferation of eosinophil granulocytes in chronic schistosomiasis mansoni is mediated by a factor secreted by inflammatory macrophages. Infect Immun 58:816–821
El-Cheikh MC, Dutra HS, Minóprio P, Borojevic R (1994) Increase of B-lymphocyte number and activity during experimental murine schistosomiasis mansoni. Braz J Med Biol Res 27:1605–1617
Gaber HM, Maghraby AS, Ahmed MB, Ruppel A, Bahgat MM (2010) Immune responses in mice after immunization with antigens from different stages of the parasite Schistosoma mansoni. Z Naturforsch C 65:289–302
Henderson NC, Sethi T (2009) The regulation of inflammation by galectin-3. Immunol Rev 230:160–171
Henderson NC, Mackinnon AC, Farnworth SL, Poirier F, Russo FP, Iredale JP, Haslett C, Simpson KJ, Sethi T (2006) Galectin-3 regulates myofibroblast activation and hepatic fibrosis. Proc Natl Acad Sci U S A 103:5060–5065
Hitoshi Y, Yamaguchi N, Mita S, Sonoda E, Takaki S, Tominaga A, Takatsu K (1990) Distribution of IL-5 receptor-positive B cells. Expression of IL-5 receptor on Ly-1(CD5)+ B cells. J Immunol 144:4218–4225
Hoyer KK, Pang M, Gui D, Shintaku IP, Kuwabara I, Liu FT, Said JW, Baum LG, Teitell MA (2004) An anti-apoptotic role for galectin-3 in diffuse large B-cell lymphomas. Am J Pathol 164:893–902
Hsu DK, Yang RY, Pan Z, Yu L, Salomon DR, Fung-Leung WP, Liu FT (2000) Targeted disruption of the galectin-3 gene results in attenuated peritoneal inflammatory responses. Am J Pathol 156:1073–1083
Kaminski DA, Stavnezer J (2006) Enhanced IgA class switching in marginal zone and B1 B cells relative to follicular/B2 B cells. J Immunol 177:6025–6029
Karasuyama H, Melchers F (1988) Establishment of mouse cell lines which constitutively secrete large quantities of interleukin 2, 3, 4 or 5, using modified cDNA expression vectors. Eur J Immunol 18:97–104
Kimata H (2002) Enhancement of IgE production in B cells by neutrophils via galectin-3 in IgE-associated atopic eczema/dermatitis syndrome. Int Arch Allergy Immunol 128:168–170
Kracker S, Durandy A (2011) Insights into the B cell specific process of immunoglobulin class switch recombination. Immunol Lett 138:97–103
Lenzi HL, Oliveira DN, Pelajo-Machado M, Borojevic R, Lenzi JA (1996) Coelom-associated lymphomyeloid tissue (milky spots): site of lymphoid and myelomonocytic cell generation. Braz J Med Biol Res 29:19–24
Mackinnon AC, Gibbons MA, Farnworth SL, Leffler H, Nilsson UJ, Delaine T, Simpson AJ, Forbes SJ, Hirani N, Gauldie J, Sethi T (2012) Regulation of transforming growth factor-beta1-driven lung fibrosis by galectin-3. Am J Respir Crit Care Med 185:537–546
Matarrese P, Fusco O, Tinari N, Natoli C, Liu FT, Semeraro ML, Malorni W, Iacobelli S (2000) Galectin-3 overexpression protects from apoptosis by improving cell adhesion properties. Int J Cancer 85:545–554
Merluzzi S, Frossi B, Gri G, Parusso S, Tripodo C, Pucillo C (2010) Mast cells enhance proliferation of B lymphocytes and drive their differentiation toward IgA-secreting plasma cells. Blood 115:2810–2817
Nangia-Makker P, Nakahara S, Hogan V, Raz A (2007) Galectin-3 in apoptosis, a novel therapeutic target. J Bioenerg Biomembr 39:79–84
Nyame AK, Leppanen AM, DeBose-Boyd R, Cummings RD (1999) Mice infected with Schistosoma mansoni generate antibodies to LacdiNAc (GalNAc beta 1→4GlcNAc) determinants. Glycobiology 9:1029–1035
Oliveira F, Aguiar A, Borojevic R, El-Cheikh M (2005) IgE expression on the surface of B1 and B2 lymphocytes in experimental murine schistosomiasis. Braz J Med Biol Res 38:1033–1042
Oliveira FL, Frazao P, Chammas R, Hsu DK, Liu FT, Borojevic R, Takiya CM, El-Cheikh MC (2007) Kinetics of mobilization and differentiation of lymphohematopoietic cells during experimental murine schistosomiasis in galectin-3(−/−) mice. J Leukoc Biol 82:300–310
Oliveira FL, Chammas R, Ricon L, Fermino ML, Bernardes ES, Hsu DK, Liu F-T, Borojevic R, El-Cheikh MC (2009) Galectin-3 regulates peritoneal B1-cell differentiation into plasma cells. Glycobiology 19:1248–1258
Oliveira FL, Brand C, Paula AA, Arcanjo KD, Hsu DK, Liu F-T, Takiya CM, Borojevic R, Chammas R, El-Cheikh MC (2011) Lack of galectin-3 disturbs mesenteric lymph node homeostasis and B cell niches in the course of Schistosoma mansoni infection. PLos One 6:e19216
Panasco MS, Pelajo-Machado M, Lenzi HL (2010) Omental and pleural milky spots: different reactivity patterns in mice infected with Schistosoma mansoni reveals coelomic compartmentalisation. Mem Inst Oswaldo Cruz 105:440–444
Pinho MF, Hurtado SP, El-Cheikh MC, Borojevic R (2005) Haemopoietic progenitors in the adult mouse omentum: permanent production of B lymphocytes and monocytes. Cell Tissue Res 319:91–102
Radosavljevic G, Volarevic V, Jovanovic I, Milovanovic M, Pejnovic N, Arsenijevic N, Hsu DK, Lukic ML (2012) The roles of galectin-3 in autoimmunity and tumor progression. Immunol Res 52:100–110
Rangel-Moreno J, Moyron-Quiroz JE, Carragher DM, Kusser K, Hartson L, Moquin A, Randall TD (2009) Omental milky spots develop in the absence of lymphoid tissue-inducer cells and support B and T cell responses to peritoneal antigens. Immunity 30:731–743
Rieder CL (2011) Mitosis in vertebrates: the G2/M and M/A transitions and their associated checkpoints. Chromosom Res 19:291–306
Roy B, Shukla S, Łyszkiewicz M, Krey M, Viegas N, Düber S, Weiss S (2009) Somatic hypermutation in peritoneal B1b cells. Mol Immunol 46:1613–1619
Roy B, Brennecke AM, Agarwal S, Krey M, Duber S, Weiss S (2013) An intrinsic propensity of murine peritoneal B1b cells to switch to IgA in presence of TGF-beta and retinoic acid. PLoS One 8:e82121
Stavnezer J, Kang J (2009) The surprising discovery that TGF beta specifically induces the IgA class switch. J Immunol 182:5–7
Takatsu K, Kouro T, Nagai Y (2009) Interleukin 5 in the link between the innate and acquired immune response. Adv Immunol 101:191–236
Utzinger J, Raso G, Brooker S, De Savigny D, Tanner M, Ornbjerg N, Singer BH, N'goran EK (2009) Schistosomiasis and neglected tropical diseases: towards integrated and sustainable control and a word of caution. Parasitology 136:1859–1874
Van de Vijver KK, Deelder AM, Jacobs W, Van Marck EA, Hokke CH (2006) LacdiNAc- and LacNAc-containing glycans induce granulomas in an in vivo model for schistosome egg-induced hepatic granuloma formation. Glycobiology 16:237–243
Vindeløv LL (1985) Flow cytometric DNA analysis. Eur J Respir Dis 66:313–314
Wang N, Shen N, Vyse TJ, Anand V, Gunnarson I, Sturfelt G, Rantapaa-Dahlqvist S, Elvin K, Truedsson L, Andersson BA, Dahle C, Ortqvist E, Gregersen PK, Behrens TW, Hammarstrom L (2011) Selective IgA deficiency in autoimmune diseases. Mol Med 17:1383–1396
Weinberg DF, Baldo-Correa E, Lenzi HL, Borojevic R (1992) Schistosoma mansoni: peritoneal plasmacytogenesis and polypoid transformation of mesenteric milky spots in infected mice. Exp Parasitol 74:408–416
Acknowledgments
We thank Dr. Marcelo Sampaio Narciso, Professor of Histology at Universidade Federal do Rio de Janeiro (Instituto de Ciências Biomédicas), who kindly reviewed the English grammar.
Author information
Authors and Affiliations
Corresponding author
Additional information
Felipe L. Oliveira and Emerson S. Bernardes contributed equally to this work.
This work was supported by grants from the Foundation Carlos Chagas Filho of Research Support at Rio de Janeiro (Fundação de Amparo a Pesquisa no Estado do Rio de Janeiro – FAPERJ; grant no. E-26.111.411.2013).
The authors declare no financial or commercial conflicts of interest.
Rights and permissions
About this article
Cite this article
Oliveira, F.L., Bernardes, E.S., Brand, C. et al. Lack of galectin-3 up-regulates IgA expression by peritoneal B1 lymphocytes during B cell differentiation. Cell Tissue Res 363, 411–426 (2016). https://doi.org/10.1007/s00441-015-2203-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-015-2203-y