Abstract
Dirofilariasis is the predominant emerging zoonotic filariasis in the world. The two most frequent filarial worms that infect dogs are Dirofilaria repens and Dirofilaria immitis. This study reports filariasis among dogs brought to the Veterinary Teaching Hospital (VTH) at the University of Peradeniya and signifies the first molecular characterization of D. repens, responsible for an emerging zoonotic filarial disease in Sri Lanka. Blood samples were collected and were morphologically analyzed using Modified Knott’s Technique, followed by molecular analyses. The difference in filariasis prevalence among gender, breed, and age categories was analyzed using a chi-square test. Infection intensities were analyzed using the Mann–Whitney U test and the Kruskal Wallis test. The dogs were brought to the clinic for either vaccination and/or for a regular checkup, and most were sick having non-specific clinical signs. Among the 87 dogs tested, 27.6% were positive for Dirofilaria. Conventional PCR and bi-directional sequencing of genomic DNA of microscopically tested positive samples revealed that the species in Sri Lanka was D. repens. The infection was significantly higher in males (39.1%) than in females (14.6%; χ2 = 0.447, p = 0.011), though it is not significant between puppies (age < 1 year) and adult dogs. More crossbred dogs were infected compared to older and purebred dogs. There was no difference in intensity of infection based on their gender, age, or breed. Sequences obtained from the current study were unique and were only 63% identical to those of D. repens reported from South India. The high number of Dirofilaria infections in domestic dogs indicates a potential reservoir for emerging human dirofilariasis cases in Sri Lanka. Thus, morphological and molecular diagnosis, along with epidemiological assessment of these zoonoses, is critical for the formulation of effective public health programs and control mechanisms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Canine filariasis is a parasitic disease caused by several species of filarial nematodes. Globally, different filaria species cause canine filariasis, including Acanthocheilonema (Dipetalonema) reconditum, Dirofilaria (Nochtiella) repens, Acanthocheilonema (Dipetalonema) dranculoides, Cercopithifilaria grassi, Brugia malayi, Brugia pahangi, and Brugia ceylonensis (Ciocan et al. 2010). Among them, Dirofilaria immitis is the most ubiquitous and pathogenic canine filarial nematode responsible for heartworm disease in dogs, characterized by clinical signs such as weight loss, diminished exercise tolerance, lethargy, poor body condition, cough, dyspnea, syncope, abdominal distention/ascites, congestive heart failure (Hoch and Strickland 2008; Vieira et al. 2014), and ultimately death. Dirofilaria immitis infection in dogs is more common in Europe (Morchón et al. 2012; Khedri et al. 2014; Krämer et al. 2014; Vieira et al. 2014) and southeastern regions of Asia (Byeon et al. 2007; Boonyapakorn et al. 2008; Borthakur et al. 2015). Adult heartworms typically live in the pulmonary arteries but may invade the right ventricle, right atrium, and caudal vena cava in heavy infections. After mating, the female worms release microfilariae into the host’s bloodstream, where they can be ingested by feeding mosquitoes (Hoch and Strickland 2008).
The incidence of filarial nematodes in dogs in Sri Lanka has received much attention, mainly due to their zoonotic potential. Though Sri Lanka eliminated human lymphatic filariasis (LF) as a public health problem in 2016, the country has recorded canine filarial nematodes such as Dirofilaria repens (more than 200 cases) including Gampaha, Colombo districts (Western Province) (Dissanaike 1961; Chandrasekharan et al. 1994; Rajapakshe et al. 2005; Mallawarachchi et al. 2018, 2021), Kandy District (Central Province) (Perera 1956), Puttalam District (North-western Province) (Mallawarachchi et al. 2018), and Trincomalee District (Eastern Province) (Dasanayake et al. 2022); B. malayi, from Gampaha and Puttalam districts (Mallawarachchi et al. 2018; 2021); and B. ceylonensis in Gampha (Rajapakshe et al. 2005) based on clinical, microscopic, and PCR diagnosis. Nonetheless, according to previous studies, there has been no report of Dirofilaria immitis infecting dogs in Sri Lanka though it is prevalent in neighboring countries such as India, Malaysia, and Thailand (Dissanaike et al. 1997; Rajapakshe et al. 2005; Gunathilaka et al. 2017; Abeysinghe et al. 2018).
The most common filarial species known to parasitize dogs in Sri Lanka is Dirofilaria repens, with an infection rate of 30–60% (Dissanaike 1979; Dissanaike et al. 1997). They inhabit the subcutaneous tissues causing subcutaneous nodules in dogs. The country has a significant population of stray dogs, which pose a serious public health threat due to the potential of infected stray dogs acting as a subclinical reservoir of infection to domesticated dogs and humans. In addition to dogs, D. repens have been recorded in domesticated cats (Abdul Cader et al. 1966; Mallawarachchi et al. 2018), a civet cat (Dissanaike 1971), and monkeys (Dissanaike et al. 1997) acting as definitive hosts. Human dirofilariasis caused by D. repens is an emerging zoonosis around the world and is endemic in Sri Lanka (Abeysinghe et al. 2018) and has the highest number of cases among Asian countries (Gunathilaka et al. 2017), reporting the second highest cases in the world (Pampiglione et al. 1995). Since humans are accidental hosts, these helminths do not mature inside a human host to produce microfilariae, thus unable to continue their life cycle. Nevertheless, infection by D. repens in humans is known to cause serious clinical manifestations such as migratory swellings, mucosal lumps (oral) (Tilakaratne and Pitakotuwage 2003; Jayasinghe et al. 2015; Sinhabahu et al. 2018; Silva et al. 2021), and subcutaneous (Senanayake et al. 2013; Gunathilaka et al. 2017; Weerasekera et al. 2021) and subconjunctival nodules (Dissanaike et al. 1997; Iddawela et al. 2015; Chandrasena et al. 2019). In addition, mosquito vectors in Sri Lanka transmitting dirofilariasis (i.e., Armigeres subalbatus, Mansonia uniformis, Mansonia annulifera, and Aedes aegypti) are highly prevalent in all areas of the country, increasing the risk of dirofilariasis to humans.
Most dog filarial studies conducted in Sri Lanka have used clinical diagnosis and/or microscopy (Perera 1956; Dissanaike 1961; Rajapakshe et al. 2005), which are less sensitive and specific than molecular analyses. Although conventional PCR has been employed to identify the presence of filariasis in dogs in Sri Lanka (Mallawarachchi et al. 2018) using pan-filarial primers (Mallawarachchi et al. 2018), it is crucial to investigate further using bi-directional sequencing and phylogenetic analyses to confirm the molecular identification and to determine how different the Sri Lankan variants are compared to those found in other geographical regions.
Since zoonotic filarial diseases have been recorded in many parts of the country, this study was conducted to determine the extent of the diseases in dogs. Thus, accurate diagnosis underpins the accurate understanding of the potential public health risk as well as the development and implementation of control/prevention programs. Hence, the current study examined and characterized filaria infection of domesticated dogs brought to the Veterinary Teaching Hospital (VTH), University of Peradeniya, Sri Lanka.
Methods
Sample collection
A cross-sectional study was conducted to collect blood samples from dogs brought from different parts of the country for sudden illnesses (itchy skin, vomiting, diarrhea etc.), vaccination, and sterilization to the (VTH) at the University of Peradeniya, Sri Lanka. Blood sample was collected from dogs by an experienced veterinary surgeon from October 2020 to February 2021. Approximately 1.5 ml of blood was collected from the ear vein located on the medial side of the ear pinna into tubes containing EDTA. Samples were brought into the Parasitology Laboratory at the Department of Zoology, University of Peradeniya, within 1 h from time of collection and were kept at 4 °C until process. Information such as dog breed, gender, age, clinical signs, time of blood collection, and demographic location was obtained from both the registered directory at VTH and/or the medical records of dogs that were sampled was recorded on a data collection tag.
Morphological analysis
Modified Knott’s technique
Blood samples of domestic dogs were examined using the modified Knott’s technique (Gadahi et al. 2008; Traversa et al. 2010). In Knott’s method, 1 ml of blood was mixed with 9 ml of 2% formaldehyde and then was thoroughly shaken for few minutes for red blood cells to hemolyze. Subsequently, samples were centrifugated at 3000 rpm for 5 min. Then, the supernatant was discarded; thick smears were made using a plastic pipette and left to dry for a day. Finally, the slides were fixed in methanol and stained in Giemsa. Air-dried slides were examined for microfilariae under a light microscope (ZEISS Primo Star™). All microfilariae present in the sediment were individually counted and identified based on key morphometric (i.e., length and width) and morphological (i.e., head and tail) characteristics (Liotta et al. 2013; Ciocan et al. 2010). The length and width of microfilariae were measured using an inverted microscope (ZEISS Primo Star™, Germany) with Zen lite 2012 software.
Molecular analysis
DNA extraction and polymerase chain reaction
Seven blood samples that had the highest intensity of microfilariae were selected and subjected to molecular analyses to obtain a higher DNA yield. Genomic DNA was extracted from the selected samples using the Blood and Tissue DNA extraction kit (Promega, USA) following the manufacturer’s instructions. A region of the 5.8S-ITS2-28S gene (484 bp) was amplified by conventional PCR from genomic DNA using the primers (DIDR-F1 5′-AGT GCG AAT TGC AGA CGC ATT GAG-3′ and DIDR-R1 5′-AGC GGG TAA TCA CGA CTG AGT TGA-3′) as described previously (Rishniw et al. 2006). Each PCR reaction was carried out in a 30-μl volume containing 15 μl of Go Taq® Green Master Mix (Promega, USA), 8 μl of Nuclease Free Water, and 1 μl of each primer pair (10 μM) based on the following cycling conditions: the initial denaturing step at 94 °C for 2 min, followed by 35 cycles including denaturation at 94 °C for 30 s, annealing at 60 °C for 30 s, extension at 72 °C for 30 s, and the final extension at 72 °C for 7 min and a soak at 4 °C (Rishniw et al. 2006). Negative (no-DNA) controls were included in each PCR run. Following PCR, aliquots (5 µl) of individual amplicons were examined on 1.5% w/v agarose gels, stained with ethidium bromide, and then photographed.
Sequencing and phylogenetic analysis
All PCR products (n = 7) were purified and subjected to bi-directional automated sequencing at the Department of Molecular and Biotechnology, Faculty of Science, University of Peradeniya.
Each 5.8S-ITS2-28S sequence determined was compared with reference sequences available for Dirofilaria spp. in NCBI database (05 April 2022), and sequence identities (in %) were calculated by pairwise comparison. Subsequently, all 5.8S-ITS2-28S sequences were aligned with reference sequences of D. repens and of D. immitis (as outgroup) (Rishniw et al. 2006; Ravindran et al. 2014; Borthakur et al. 2015; Sabūnas et al. 2019; Satjawongvanit et al. 2019; Brunet et al. 2020; Cimpan et al. 2022) over a consensus length of 261 bp. The phylogenetic analysis of sequence data was conducted using the Neighbor-Joining (NJ) method (Saitou and Nei 1987) using MEGA11 software (Tamura et al. 2021). The distance was estimated employing the general time-reversible model of evolution, and nodes were tested for robustness with 10,000 bootstrap replicates (Felsenstein 1985). The tree obtained was appraised for the nodal support values.
The nucleotide sequences originating from the ITS region were used to establish the phylogenetic relationship, with Dirofilaria repens sequences from several geographical regions as Kadakkarapally: India, Kuthiathode: India (Ravindran et al. 2014), Assam: India (Borthakur et al. 2015), Lithuania (Sabūnas et al. 2019), Romania (Cimpan et al. 2022), France (Brunet et al. 2020), and USA (Rishniw et al. 2006) (GenBank accession: JQ039743.1, JQ039744.1, JX524743.1, MH469230.1, MZ677061.1, MK942385.1 and AY693808.1 respectively) and D. immitis (MK250784.1) as outgroup (Satjawongvanit et al. 2019).
Statistical analyses
Infection between gender (i.e., male and female), age groups (i.e., (< 1 year (year), 1–3 year, 3–5 year, and > 5 year) (Bamorovat et al. 2017), and breed groups (pure breed and cross breed) were compared using a chi-square test (chi-square test, p < 0.05). The microfilariae concentration was compared between gender (male vs female) and breed groups (pure-breed vs crossbreed) using Mann Whitney U test, whereas the infection intensities among age groups (i.e., < 1 year, 1–2 year, 3–5 year, > 5 year) were compared using the Kruskal–Wallis test (as the data were not normally distributed). Statistical analyses were conducted using Minitab 19.
Results
Eighty-seven domesticated dogs were tested, out of which 24 (27.6%) were positive for microfilariae of Dirofilaria by microscopy. The microfilariae were identified and differentiated by the absence of the sheath, obtuse cephalic end, sharp and filiform tail, often ending in an umbrella-handle shape (Genchi et al. 2007). However, the larvae were not differentiated into genera or species based on morphology and morphometry (Fig. 1). Of the 87 dogs examined, 46 (52.9%) and 41 (47.1%) were males and females, respectively. There was a significant difference between dirofilariasis infection in males (39.1%) and females (14.6%; χ2 = 0.447, p = 0.011). However, there was no difference in prevalence of infection in age categories and between crossbreed and pure breed (39.4%; χ2 = 3.711, p = 0.054) (Table 1). The dogs did not show filariasis-specific clinical signs but were having non-specific signs or no signs at all. They were brought to the clinic for either vaccination and/or for a regular check-up, and most were sick having non-specific clinical signs.
Intensity of infection
There was no significant difference in intensity of infection in microfilariae in males (451 ± 570 mf/ml) and females (190 ± 376 mf/ml; Mann Whitney U test, p = 0.3173), age, and breed. There was a high microfilaria intensity in age category < 1 year (563 ± 648 mf/ml) followed by age category 3–5 years (454 ± 527 mf/ml), > 5 year (328 ± 581 mf/ml), and 1–3 years (61.3 ± 82.9 mf/ml) (Table 2).
Distribution of positive cases
Of 24 Dirofilaria samples, 19 were from the Central Province, three from the North Western Province, and each one from the Sabaragamuwa Province and Western Province.
PCR, sequencing, and phylogenetic analyses
Amplicons (5.8S-ITS2-28S) of the expected size (484 bp) were produced from all 7 samples that were subjected to molecular analyses confirming the single infection by D. repens. No mixed infections were observed. Selective bi-directional sequencing of 7 amplicons defined 5.8S-ITS2-28S sequences (416–420 bp; GenBank accession nos. ON332065 to ON332071) (Figs. 2 and 3).
Pairwise comparisons (over an alignment length of 422 positions) (Fig. 4) of the seven distinct sequence types defined in the current study revealed sequence variation of 0.7 to 2.9% (Table 3). Upon pairwise comparison, variation of 97.1% was detected between the sequence 5 (GenBank accession no. ON332069) and sequence 6 (accession nos. ON332070) from Udaperadeniya and Thundeniya, respectively. Highest similarity of 99.3% was detected between the sequence 3 (GenBank accession no. ON332067) and sequence 6 (GenBank accession no. ON332070) from unknown location and Thundeniya, respectively (Table 3).
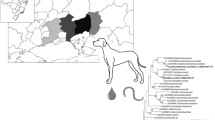
To unambiguously assign the seven distinct sequence types defined herein (accession nos. ON332065 to ON332071), a phylogenetic analysis was undertaken using these and 8 reference sequences, including those of D. immitis as the outgroup (see Fig. 3). All 15 sequences were aligned over 261 bp positions and subjected to analyses using the NJ method. The sequences with accession nos. ON332065, ON332066, ON332067, ON332068, ON332069, ON332070, and ON332071 clustered, with strong statistical support, with those representing D. repens sequences derived from other geographical regions (Fig. 3).
Discussion
Accurate diagnosis of filarial species in dogs is of paramount importance to identify the zoonotic potential of these helminths to the communities even after the human lymphatic filariasis is eliminated from Sri Lanka. This study used traditional and molecular approaches to identify filarial nematodes in domesticated dogs in and around the Kandy District of Sri Lanka. The dogs were brought to the VTH clinic for either vaccination and/or for a regular check-up, and most were sick having non-specific clinical signs. The clinical manifestations of filariasis in dogs depend on the size of the dog and the number of worms present in this infection. A high number of worms are needed for symptoms to be visible. If a dog suffers from a low infection count, symptoms may not appear. All positive cases were Dirofilaria species. As D. immitis has not been recorded in Sri Lanka so far, our species could be D. repens. According to the observed overall prevalence, it does not fall within the 30–60% range (Dissanaike et al. 1997). This could be because the dogs sampled are domesticated and so less susceptible to infection than stray dogs. However, the prevalence in this study is consistent with the range reported (7–24%) in Kerala, India (Sabu et al. 2005).
For morphological analysis, modified Knotts’ technique (MKT) has been utilized as it is the best method to identify microfilaria in blood. It is very easy, quick, and cheap, and it preserves microfilaria morphology and size while increasing the sensitivity (Gadahi et al. 2008), where Courtney and Zeng (2001) were able to discover high percentage of positive samples for D. immitis (80.9%) by the Knott’s technique. Though some filarial parasites such as B. malayi (Mallawarachchi et al. 2018) and B. ceylonensis (Rajapakshe et al. 2005) have been found in dogs in Sri Lanka, only D. repens was found in this work.
When considering gender, male dogs had a higher prevalence than female dogs, which is consistent with previous findings (Alsarraf et al. 2021). It might be because many owners prefer male dogs as guardians, and they spend most of their time outside the house. Though it is not significant, dogs in the older age categories show a higher prevalence than those in the younger age groups. Likewise, crossbreed shows a higher prevalence compared to purebred. But a higher sample size would give a clear picture as both are close to significant (χ2 = 3.820, p = 0.051) and (χ2 = 3.711, p = 0.054). In this study, the highest prevalence was found in 3–5-year-old canines (44.4%), with the lowest prevalence seen in animals under 1 year old (17.9%).
The phylogenetic tree grouped all seven sequences described in this work into a monophyletic clade, close to the D. repens sequence (JQ039743.1 and JQ JQ039744.1), with 63% of bootstrap. The sequences obtained in the present work show greater similarity between each other than with JQ039743.1 and JQ JQ039744.1, noting the importance of conducting future studies on the evolutionary phylogeny of dog filarids, and studies on the distribution of infection in domestic and wild dogs in Kandy districts and all other districts in Sri Lanka.
Most of the positive samples were from domesticated dogs in the Central Province. According to the available literature, a significant number of human cases have been reported from the Kandy district (Ratnatunga and Wijesundera 1999; Tilakaratne and Pitakotuwage 2003; Iddawela et al. 2015; Jayasinghe et al. 2015), yet there is only one publication (Perera 1956) on filariasis in dogs from Kandy district, indicating a significant lack of studies. As per the Annual Health Bulletin 2015, Sri Lanka, 2017, it was found that the estimated human to total dog population ratio was 6.7:1, and the human to domestic dog population ratio was 9.6:1.
Conclusion
The findings imply that effective microfilaria infection control in companion animals, particularly dogs, is critical for reducing microfilaria infections and to avoid acting as reservoirs for emerging zoonotic dirofilariasis. Future studies on dogs, humans, and mosquito species will be needed, and it is critical to collaborate with clinicians and veterinarians in order to limit the number of instances.
Data availability
Data available on request due to privacy/ethical restrictions.
References
Abdul Cader MHM, Tharumarajah K, Rajendran K (1966) Filarial infection in domestic cats in Ceylon. Bull Indian Soc Malar & Other Commun Dis 3:155–158
Abeysinghe AHMGB, Jiffry RAM, Perera WMM (2018) Human subcutaneous dirofilariasis: an increasing phenomenon in Sri Lanka. Sri Lanka J Surg 36:35. https://doi.org/10.4038/sljs.v36i1.8480
Alsarraf M, Levytska V, Mierzejewska EJ, Poliukhovych V, Rodo A, Alsarraf M, Kavalevich D, Dwużnik-Szarek D, Behnke JM, Bajer A (2021) Emerging risk of Dirofilaria spp . infection in Northeastern Europe : high prevalence of Dirofilaria repens in sledge dog kennels from the Baltic countries. Sci Rep 1–8. https://doi.org/10.1038/s41598-020-80208-1
Annual Health Bulletin (2015) Sri Lanka. (2017). Medical Statistics Unit, Ministry of Health, Nutrition and Indigenous Medicine. Nutrition and Indigenous Medicine 30:1–208
Bamorovat M, Sharifi I, Harandi FM, Nasibi S, Sadeghi B, Khedri J, Mohammadi MA (2017) Parasitological, serological and molecular study of Dirofilaria immitis in domestic dogs, southeastern Iran. Iran J Parasitol 12:260–266
Boonyapakorn C, Srikitjakarn L, Morakote N, Hoerchner F (2008) The epidemiology of Dirofilaria immitis infection in outpatient dogs at Chiang Mai University small animal hospital, Thailand. Southeast Asian J Trop Med Public Heal 39:33–38
Borthakur SK, Deka DK, Islam S et al (2015) Prevalence and molecular epidemiological data on Dirofilaria immitis in dogs from Northeastern States of India. Sci World J 2015:1–7. https://doi.org/10.1155/2015/265385
Brunet K, Catroux M, Yera H et al (2020) Photo Quiz : Migrating Worm Naturally Exited through the Palate. J Clin Microbiol 58:1
Byeon KH, Kim BJ, Kim SM et al (2007) A serological survey of Dirofilaria immitis infection in pet dogs of Busan, Korea, and effects of chemoprophylaxis. Korean J Parasitol 45:27–32. https://doi.org/10.3347/kjp.2007.45.1.27
Chandrasekharan NV, Karunanayake HE, Franzen L et al (1994) Dirofilaria repens: cloning and characterization of a repeated DNA sequence for the diagnosis of Dirofilariasis in dogs, Canis familiaris. Exp Parasitol 78:279–286
Chandrasena TGAN, Premaratna R, Mallawaarachchi CH et al (2019) The diversity of human Dirofilariasis in Western Sri Lanka. Biomed Res Int 2019:1–7. https://doi.org/10.1155/2019/9209240
Cimpan AA, Baneth G, Nachum-Biala Y et al (2022) Dirofilaria repens predominates in shelter dogs from South Romania. Comp Immunol Microbiol Infect Dis 84:101793. https://doi.org/10.1016/j.cimid.2022.101793
Ciocan R, Dărăbuş G, Igna V (2010) Morphometric study of microfilariae of Dirofilaria spp. on dogs. Bull Univ Agric Sci Vet Med Cluj-Napoca - Vet Med 67:45–49. https://doi.org/10.15835/buasvmcn-vm:67:2:5920
Courtney CH, Zeng QY (2001) Relationship between microfilaria count and sensitivity of the direct smear for diagnosis of canine dirofilariosis. Vet Parasitol 94:199–204. https://doi.org/10.1016/S0304-4017(00)00377-0
Dasanayake R, Balendran T, Atapattu D, Iddawela D (2022) A study on canine dirofilariasis in selected areas of Sri Lanka. BMC Res Notes 15:1–6. https://doi.org/10.1186/s13104-022-06024-0
De Silva GPUP, Udugampola DS, Ekanayake EMIB et al (2021) An underrated differential diagnosis for subcutaneous lumps : 26 cases of subcutaneous Dirofilariasis. Sri Lanka J Surg 39:31–33. https://doi.org/10.4038/sljs.v39i2.8827
Dissanaike AS (1961) On some helminths of dogs in Colombo and their bearing on human infections, with a description of a new trematode Heterophyopsis yehi sp.nov. (Heterophyidae). Ceylon J Med Sci 10:1–12
Dissanaike AS (1971) Human infections with Dirofilaria, a filarial parasite of animals in Ceylon, with a brief review of recent cases. Ceylon Med J 17:91–99
Dissanaike AS (1979) Zoonotic aspects of filarial infections in man. Bull World Health Organ 57:349–357
Dissanaike AS, Abeyewickreme W, Wijesundera MD et al (1997) Human dirofilariasis caused by Dirofilaria (Nochtiella) repens in Sri Lanka. Parassitologia 39:375–382
Felsenstein J (1985) Confidence limits on phylogenies: an apptoach using the Bootstrap. Evolution (N Y) 39:783–791
Gadahi JA, Arijo AG, Abubakar M et al (2008) Prevalence of blood parasites in stray and pet dogs in hyderabad area: comparative sensitivity of different diagnostic techniqes for the detection of microfilaria. Vet World 1:229–232
Genchi C, Venco L, Genchi M (2007) Guideline for the laboratory diagnosis of canine and feline Dirofilaria infections. Mappe Parassitologiche 8:137–144
Gunathilaka N, Siriwardana S, Wijesooriya L, et al (2017) Subcutaneous dirofilariasis caused by Dirofilaria (Nochtiella) repens in Sri Lanka: a potential risk of transmitting human dirofilariasis . SAGE Open Med Case Rep 5:1–4. https://doi.org/10.1177/2050313x17701373
Hoch H, Strickland K (2008) Canine and Feline Dirofilariasis: life cycle, pathophysiology, and diagnosis. Compendium 30:133
Iddawela D, Ehambaram K, Wickramasinghe S (2015) Human ocular dirofilariasis due to Dirofilaria repens in Sri Lanka. Asian Pac J Trop Med 8:1022–1026. https://doi.org/10.1016/j.apjtm.2015.11.010
Jayasinghe RD, Gunawardane SR, Sitheeque MAM, Wickramasinghe S (2015) A case report on oral subcutaneous Dirofilariasis. Case Rep Infect Dis 2015:1–4. https://doi.org/10.1155/2015/648278
Khedri J, Radfar MH, Borji H et al (2014) Canine heartworm in southeastern of Iran with review of disease distribution. Iran J Parasitol 9:560–567
Krämer F, Schaper R, Schunack B et al (2014) Serological detection of Anaplasma phagocytophilum, Borrelia burgdorferi sensu lato and Ehrlichia canis antibodies and Dirofilaria immitis antigen in a countrywide survey in dogs in Poland. Parasitol Res 113:3229–3239. https://doi.org/10.1007/s00436-014-3985-7
Liotta JL, Sandhu GK, Rishniw M, Bowman DD (2013) Differentiation of the microfilariae of Dirofilaria immitis and Dirofilaria repens in stained blood films. J Parasitol 99:421–425. https://doi.org/10.1645/12-10.1
Mallawarachchi CH, Chandrasena NTGA, Wickramasinghe S et al (2018) A preliminary survey of filarial parasites in dogs and cats in Sri Lanka. PLoS ONE 13:1–11. https://doi.org/10.1371/journal.pone.0206633
Mallawarachchi CH, Chandrasena TGAN, Withanage GP et al (2021) Molecular characterization of a reemergent Brugia malayi parasite in Sri Lanka, Suggestive of a Novel Strain. Biomed Res Int 2021:1–7
Morchón R, Carretón E, González-Miguel J, Mellado-Hernández I (2012) Heartworm disease (Dirofilaria immitis) and their vectors in Europe - new distribution trends. Front Physiol 3:1–11. https://doi.org/10.3389/fphys.2012.00196
Pampiglione S, Canestri TG, Rivasi F (1995) Human dirofilariasis due to Dirofilaria (Nochtiella) repens: a review of world literature. Parassitologia 37:149–193
Perera SJE (1956) Preliminary survey of the incidence of filariasis in dogs in Kandy District. Ceylon Vet J 4:22–24
Rajapakshe RPAS, Perera WSR, Ihalamulla RL et al (2005) Study of dirofilariasis in a selected area in the Western Province. Ceylon Med J 50:58–61. https://doi.org/10.4038/cmj.v50i2.1570
Ratnatunga N, de Wijesundera M, S, (1999) Histopathological diagnosis of subcutaneous Driofilaria repens infection in humans. Southeast Asian J Trop Med Public Heal 30:375–378
Ravindran R, Varghese S, Nair SN, et al (2014) Canine filarial infections in a human Brugia malayi endemic area of India. Biomed Res Int 2014:1–9. https://doi.org/10.1155/2014/630160
Rishniw M, Barr SC, Simpson KW et al (2006) Discrimination between six species of canine microfilariae by a single polymerase chain reaction. Vet Parasitol 135:303–314. https://doi.org/10.1016/j.vetpar.2005.10.013
Sabu L, Devada K, Subramanian H (2005) Dirofilariosis in dogs & humans in Kerala. Indian J Med Res 121:691–693
Sabūnas V, Radzijevskaja J, Sakalauskas P et al (2019) Dirofilaria repens in dogs and humans in Lithuania. Parasit Vectors 12:1–10. https://doi.org/10.1186/s13071-019-3406-y
Saitou N, Nei M (1987) The neighbor-joining method: a new method for reconstructing phylogenetic trees. Mol Biol Evol 4:406–425. https://doi.org/10.1093/oxfordjournals.molbev.a040454
Satjawongvanit H, Phumee A, Tiawsirisup S, et al (2019) Molecular analysis of canine filaria and its Wolbachia endosymbionts in domestic dogs collected from two animal university hospitals in Bangkok metropolitan region, Thailand. Pathogens 8:1–13. https://doi.org/10.3390/pathogens8030114
Senanayake MP, Infaq MLM, Adikaram SGS, Udagama PV (2013) Ocular and subcutaneous dirofilariasis in a Sri Lankan infant: an environmental hazard caused by dogs and mosquitoes. Paediatr Int Child Health 33:111–112. https://doi.org/10.1179/2046905512Y.0000000024
Sinhabahu VP, Hettiarachchi J, Gamage M, Beneragama DH (2018) A child with an unusual lump in the cheek. Sri Lanka J Child Heal 47:89–90. https://doi.org/10.4038/sljch.v47i1.8440
Tamura K, Stecher G, Kumar S (2021) MEGA11: Molecular Evolutionary Genetics Analysis Version 11. Mol Biol Evol 38:3022–3027. https://doi.org/10.1093/molbev/msab120
Tilakaratne WM, Pitakotuwage TN (2003) Intra-oral Dirofilaria repens infection: report of seven cases. J Oral Pathol Med 32:502–505. https://doi.org/10.1034/j.1600-0714.2003.00183.x
Traversa D, Aste G, Milillo P et al (2010) Autochthonous foci of canine and feline infections by Dirofilaria immitis and Dirofilaria repens in central Italy. Vet Parasitol 169:128–132. https://doi.org/10.1016/j.vetpar.2009.12.034
Vieira AL, Vieira MJ, Oliveira JM, et al (2014) Prevalence of canine heartworm (Dirofilaria immitis) disease in dogs of central Portugal. Parasite 21:1–7. https://doi.org/10.1051/parasite/2014003
Weerasekera CJ, Hapuachchige C, Wijeratne YMTY et al (2021) Omental dirofilariasis caused by Dirofilaria repens; visceralisation in a patient with diabetes mellitus. J Ceylon Coll Physicians 52:105. https://doi.org/10.4038/jccp.v52i2.7936
Acknowledgements
We thank Ms. A.H.M.W.S. Abeyrathne, at the Department of Veterinary Clinical Sciences, the University of Peradeniya, for assisting in collecting patient history.
Funding
This work was funded by the National Science Foundation (Grant No. RG/2019/BT/01) and National Research Council (Grant No. 20–083).
Author information
Authors and Affiliations
Contributions
Study conception and design by Rupika S. Rajakaruna and Nayana Wijayawardhane. Sample processing, data analysis, and writing of the manuscript by Sandani S. Thilakarathne. Supervision of laboratory work and data analysis by Piyumali K. Perera. Sample and patient history collection and laboratory assistance by Chandima Mallawa. All the authors critically edited and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical statement
Ethical clearance for the study was obtained from the Ethical Clearance Committee of the Postgraduate Institute of Science, University of Peradeniya, Sri Lanka. No: CES_PGIS_2022_06.
Consent to participate
N/A.
Consent for publication
All the authors read and approved the final version of the manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Handling Editor: Una Ryan
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Thilakarathne, S.S., Wijayawardhane, N., Perera, P.K. et al. Filariasis in dogs brought to the Veterinary Teaching Hospital, University of Peradeniya, Sri Lanka. Parasitol Res 122, 461–469 (2023). https://doi.org/10.1007/s00436-022-07742-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-022-07742-x