Abstract
Acanthamoeba causes diseases such as Acanthamoeba keratitis (AK) which leads to permanent blindness and granulomatous Acanthamoeba encephalitis (GAE) where there is formation of granulomas in the brain. Current treatments such as chlorhexidine, diamidines, and azoles either exhibit undesirable side effects or require immediate and prolonged treatment for the drug to be effective or prevent relapse. Previously, antifungal drugs amphotericin B, nystatin, and fluconazole-conjugated silver with nanoparticles have shown significantly increased activity against Acanthamoeba castellanii. In this study, two functionally diverse tetrazoles were synthesized, namely 5-(3-4-dimethoxyphenyl)-1H-tetrazole and 1-(3-methoxyphenyl)-5-phenoxy-1H-tetrazole, denoted by T1 and T2 respectively. These compounds were evaluated for anti-Acanthamoeba effects at different concentrations ranging from 5 to 50 μM. Furthermore, these compounds were conjugated with silver nanoparticles (AgNPs) to enhance their efficacy. Particle size analysis showed that T1-AgNPs and T2-AgNPs had an average size of 52 and 70 nm respectively. After the successful synthesis and characterization of tetrazoles and tetrazole-conjugated AgNPs, they were subjected to anti-Acanthamoeba studies. Amoebicidal assay showed that at concentration 10 μM and above, T2 showed promising antiamoebic activities between the two compounds while encystation and excystation assays reveal that both T1 and T2 have inhibited differentiation activity against Acanthamoeba castellanii. Conjugation of T1 and T2 to AgNP also increased efficacy of tetrazoles as anti-Acanthamoeba agents. This may be due to the increased bioavailability as AgNP allows better delivery of treatment compounds to A. castellanii. Human cell cytotoxicity assay revealed that tetrazoles and AgNPs are significantly less toxic towards human cells compared with chlorhexidine which is known to cause undesirable side effects. Cytopathogenicity assay also revealed that T2 conjugated with AgNPs significantly reduced cytopathogenicity of A. castellanii compared with T2 alone, suggesting that T2-conjugated AgNP is an effective and safe anti-Acanthamoeba agent. The use of a synthetic azole compound conjugated with AgNPs can be an alternative strategy for drug development against A. castellanii. However, mechanistic and in vivo studies are needed to explore further translational values.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acanthamoeba, an opportunistic pathogen, is commonly found in soil and water (Köhsler et al. 2016). A blinding infection of the eye known as Acanthamoeba keratitis (AK) is caused by the invasion of Acanthamoeba in the eye where it causes chronic ulceration of the cornea which often leads to permanent sight damage. AK usually occurs in contact lens wearing individuals where the malpractice of contact lenses is the main cause, such as wearing contact lenses while swimming activities (Siddiqui and Khan 2012). Another human disease caused by Acanthamoeba is granulomatous amoebic encephalitis (GAE), where the pathogen invades the central nervous system (CNS) and causes the formation of granulomas (Siddiqui and Khan 2012). GAE is known to be an opportunistic infection as it occurs mainly in immunocompromised individuals (Slater et al. 1994). This disease is rare but highly fatal as statistics show 95% of recorded patients die even when they are given different antimicrobial treatments (Kulsoom et al. 2014). Besides these two infections, Acanthamoeba also causes the lung, kidney, and skin to be compromised by the pathogen, where trophozoites and cysts usually surround the walls of blood vessels. Acanthamoeba may feed on skin tissue and cause severe skin lesions in immunocompromised patients as well (Schuster and Visvesvara 2004).
Acanthamoeba can exist as a free-living unicellular microorganism in nature or as a parasite inside a host. Acanthamoeba is known to feed on bacteria in their environments and support the growth of several other pathogens, such as Mycobacterium, Chlamydia, and certain viruses (Khan 2006). The pathogen undergoes asexual reproduction by dividing through binary fission (Band and Mohrlok 1973). There are two phases in the life cycle of Acanthamoeba: growth phase trophozoites and cellular differentiation to form cysts. The two types of cellular differentiation are known as encystment and excystment (Weisman 1976). Excystment leads to Acanthamoeba trophozoites from cysts which is the active form and is described as having protruding spine-like structure known as acanthopodia which are important for movement, engulfing bacteria, and surface adhesion. Encystment, on the other hand, leads to Acanthamoeba cysts from trophozoites, which are the resistant form of the pathogen, when it is subjected to a harsh environment such as starvation, dryness, and extreme temperatures (Khunkitti et al. 1998). Cysts are described as double walled with a wrinkled ectocyst (outer layer) and an endocyst (inner layer) which varies in shape. At the site of contact between the ectocyst and endocyst, pores covered by small lids (operculum) are present (Siddiqui and Khan 2012). These cyst walls are made up of polysaccharides of glucose and galactose; hence, polysaccharides biosynthesis pathway is considered as an important target for the development of treatments against Acanthamoeba cysts (Garajová et al. 2019; Anwar et al. 2019).
The current recommended treatment for AK is biguanide such as chlorhexidine together with a diamidine and added antibiotics if the bacterial infection was involved (Lorenzo-Morales et al. 2015). Chlorhexidine releases a cation that interacts with the cell membrane, hence increasing cell permeability and ultimately leading to cell death through leakage of ions and cytoplasmic disruption (Sharma et al. 2013). Although chlorhexidine is effective against A. castellanii, immediate and aggressive treatment with the biguanide is needed to make the treatment effective (Lamb et al. 2015). Chlorhexidine also exhibits undesirable effects when treated against AK such as mature cataracts and iris atrophy (Aqeel et al. 2016). Other anti-protozoa drug currently used are azoles such as metronidazole, which is notably effective against amoebic infections in the human gastrointestinal tracts caused by Entamoeba histolyca (Cano et al. 2014). However, the issue of metronidazole-resistant protozoa has also been brought into light and the drug is known to cause undesirable side effects such as headaches and dry mouth and is potentially toxic (Bendensky et al. 2002). There are reports of using a mixture of metronidazole, chlorhexidine, and neomycin sulfate that led to rapid resolution of inflammation in AK (Xuguang et al. 2003). Other than metronidazole, voriconazole is also found to be effective in treatment of AK; however, prolonged treatment with the drug was required to prevent relapse (Tu et al. 2010). Next, ketoconazole was found to be effective against a brain abscess caused by Acanthamoeba when treated together with a mixture of antibiotics (Nampoothiri et al. 2018). However, ketoconazole has previously shown high hepatotoxicity and endocrine dysregulation, which lead to the ban of the azole in the Australian and European markets as well as strict regulations in America (Gupta and Lyons 2015). Previously, several triazole antifungal agents were tested against Acanthamoeba castellanii and Acanthamoeba polyphaga by inhibiting the sterol 14-demethylase (CYP51) (Lamb et al. 2015). It was found that Acanthamoeba is more related to algae and plants than mammalian ancestries; therefore, existing antifungal azoles were not very effective anti-Acanthamoeba agents due to the low sequence identity of Acanthamoeba and fungal CYP51 as shown by NCBI-BLASTP (Lamb et al. 2015).
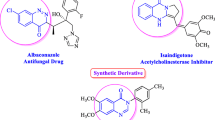
Besides known azole drugs, synthetic azoles are also of widespread interest for drug development against numerous microbes. Tetrazoles are five-membered aromatic ring compounds with four nitrogen and one carbon atom. This planar structure makes the compound electron rich and allows the compound to form weak bonds with enzymes or biological receptors (Lingling et al. 2013). This characteristic also allows tetrazoles to interact and stabilize functional molecules that were formed through combination of multiple small molecules, showing many potentials in the pharmaceutical industry (Dai et al. 2015). Besides, tetrazoyl fragments have been described as the non-toxic and non-metabolized analogues of carboxylic and cis-amide groups (Dai et al. 2015). Certain derivatives of tetrazoles have also shown strong antifungal activities through inhibition of ergosterol synthesis such as tetrazole derivatives which contain hydrazone and thiazoline portion shows high efficacy in inhibiting certain Candida, Aspergillus, and Fusarium species (Łukowska-Chojnacka et al. 2016). Several types of synthetic chromone-tetrazoles have also shown to be effective against Entamoeba histolytica, the causative agent of amoebic diarrhea and dysentery (Cano et al. 2014). Among membrane-acting agents, alkylphosphocholines such as miltefosine have been found to be effective against AK and GAE (Tavassoli et al. 2018; Barisani-Asenbauer et al. 2012; Webster et al. 2012). Furthermore, synthetic analogues of alkylphosphocholines have also been reported to exhibit potent antiamoebic effects against Acanthamoeba spp. (Timko et al. 2015; Garajová et al. 2014).
Nanoparticles may be the solution to multidrug-resistant pathogens as they have shown to increase the efficacy of compounds against various microbes (Egger et al. 2009). Researchers are interested in silver nanoparticles because silver was used as an antimicrobial agent against bacteria (Bello-Vieda et al. 2018). Besides that, conjugation of natural products, plant extracts, and contact lens solutions to silver nanoparticles have been shown to increase the in vitro effectivity of their payloads against Acanthamoeba spp. (Anwar et al. 2020; Padzik et al. 2018; Padzik et al. 2019). The mechanism of silver nanoparticles against microbes is still not fully grasped, but several mechanisms have been proposed. It is said that silver nanoparticles alter cell wall and cell membrane which in turn increases cell permeability (Bello-Vieda et al. 2018). Previously, antifungal drugs amphotericin B, nystatin, and fluconazole conjugated silver nanoparticles showed significantly increased activity against Acanthamoeba castellanii (Anwar et al. 2018). Developing a novel tetrazole silver nanoparticle with increased efficacy compared with the respective tetrazole alone against the human pathogen Acanthamoeba is the overall aim of this current study. In this study, we tested the antiamoebic properties of two novel synthetic tetrazoles against A. castellanii belonging to the T4 genotype and the effects of silver nanoparticles conjugation on the efficacy of these compounds.
Materials and methods
Chemicals
Different aromatic nitriles were purchased from different chemical suppliers including Alfa-Aesar, Merck, Sigma-Aldrich, and TCI. Silver nitrate (AgNO3) and sodium borohydride (NaBH4) was obtained from Merck, RPMI-1640 was obtained from Gibco, and absolute DMSO was obtained from Thermo Scientific.
Acanthamoeba castellanii cultures
A clinical isolate obtained in 1984 from a keratitis patient from India, A. castellanii of T4 genotype (ATCC 50492) was purchased from American Tissue Culture Collection (ATCC). The Amoeba cells were cultured in 10 ml of PYG medium consisting of 0.75% yeast extract, 0.75% protease peptone, and 1.5% glucose in T-75 cm2 culture flasks (Aqeel et al. 2016).
Henrietta Lacks cell cultures
HeLa cells (CCL-2) were obtained from American Tissue Culture Collection (ATCC). The cells were cultured in RPMI-1640 supplemented with 1% (2 mM) l-glutamine, 1% penicillin-streptomycin, 10% fetal bovine serum, and 1% minimal essential media nonessential amino acid (MEM NEAA). The cells were incubated in a CO2 incubator at 37 °C and 95% humidity. Two milliliters (0.25%) of trypsin was used to detach the cells which enabled the inoculation of cells into 96-well plates.
Synthesis and characterization of T1 and T2
The tetrazoles tested in this study are 5-(3-4-dimethoxyphenyl)-1H-tetrazole and 1-(3-methoxyphenyl)-5-phenoxy-1H-tetrazole, represented by T1 and T2 respectively (Fig. 1).
T1 and T2 were synthesized by click reaction of aromatic nitriles with sodium azide in the presence of ammonium chloride to afford T1 and T2 as given in Scheme 1 (Fatima et al. 2018).
Synthesis of Tetrazoles T1 and T2 (Fatima et al. 2018)
Characterization of T1 and T2
5-(3′,4′-Dimethoxyphenyl)-1H-tetrazole (T1)
Yield: 88%; m.p. 207–208 °C; 1H-NMR: (300 MHz, DMSO-d6): δH 16.62 (s, NH), 7.63 (s, 1H, H-2′), 7.62 (d, 1H, J6′,5′ = 8.4 Hz, H-6′), 7.18 (d, 1H, J5′,6′ = 8.4 Hz, H-5′), 3.84 (s, 3H, 3′-OCH3), 3.83 (s, 3H, 4′-OCH3); 13C-NMR (100 MHz, DMSO-d6): δc 151.1 (C-3′), 149.1 (C-4′), 120.1 (C-6′), 112.1 (C-2′), 110.0 (C-5′), 55.7 (4′-OCH3), 55.6 (3′-OCH3); IR (KBr, cm−1): 3477 (N–H), 1609 (C=N), 1144 (C–O); EI-MS: m/z (rel. abund. %), 206 [M]+ (1), 191 (4), 182 (100), 152 (50), 136 (90); HREI-MS: m/z calcd for C9H10N4O2 [M]+ 206.0804; found 206.0791.
Methyl2-[(1-phenyl-1H-1,2,3,4-tetraazol-5-yl)oxy]phenyl ether (T2)
Yield: 84%; m.p. 249–251 °C; 1H-NMR: (300 MHz, DMSO-d6): δH 7.84 (d, 2H, J2′,3′ = J6′,5′ 7.5 Hz, H-2′,6′), 7.68 (m, 3H, H-3′,4′,5′), 7.42 (dd, 1H, J4″,5″ = 9, Hz J4″,3″ = 8.4 Hz, H-4″), 7.13 (m, 1H, H-5″), 7.07 (d, 1H, J6″,5″ = 7.8 Hz, H-6″), 6.93 (d, 1H, J3″,4″ = 8.1 Hz, H-3″), EI-MS: m/z (rel. abund. %), 268 (M+, 4), 238 (36), 225 (4), 117 (100); HREI-MS: m/z calcd for C14H12O2N4 [M]+ 268.0960; found 268.0941.
Synthesis of tetrazole-conjugated AgNPs
Tetrazoles were weighed and dissolved in absolute DMSO to prepare 10-mM stocks. The 10-mM stocks of the tetrazoles were diluted with sterile water to prepare 0.5-mM and 0.1-mM stocks which was used to plate concentrations 5 μM, 10 μM, 25 μM, and 50 μM in each assay. Synthesis of tetrazole-conjugated AgNPs was done by adding 2 ml of 0.1 mM tetrazole to 2 ml of 0.1 mM silver nitrate(aq) solution and mixed on a magnetic stirrer. Sodium borohydride (4 mM, 20 μl) was added to reduce the silver ions to enable conjugation of tetrazole to AgNP (Anwar et al. 2018). The successful formation was indicated by the color change of the mixture from colorless to yellow. Further analysis such as UV-Vis spectrophotometry and FT-IR spectroscopy was done to confirm the formation and stabilization of tetrazole-conjugated AgNPs.
Amoebicidal assays
The antiamoebic properties of tetrazoles alone and tetrazole-conjugated AgNPs were tested in duplicates for this assay, as described by Sissons et al. (2006). In 24-well plates, 5 × 105 A. castellanii trophozoites were treated with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in RPMI-1640. Chlorhexidine served as the positive controls and RPMI-1640 alone as the negative control. Appropriate amounts of DMSO and water were also plated as solvent controls. After a 24-h incubation period at 30 °C, a trypan blue exclusion assay was carried out to calculate the estimated average well count for each duplicate.
Encystation assays
In 24-well plates, 5 × 105 A. castellanii trophozoites were treated with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone. All treatment was done in encystation medium comprised of 5 mM MgCl2 and 10% glucose. Chlorhexidine served as the positive controls and PBS containing an encystation medium served as the negative control. Appropriate amounts of DMSO and water were also plated as solvent controls. After a 96-h incubation period at 30 °C, 0.1% SDS was added to dissolve trophozoites to enable the counting of cysts using a hemocytometer.
Excystation assay
Preparation of cysts was done few weeks prior to this experiment by plating healthy A. castellanii trophozoites on non-nutrient agar plates for at least 14 days before it was scraped and collected. 1 × 105 cysts were treated with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in PYG. Chlorhexidine served as the positive controls and PYG alone as the negative control. Appropriate amounts of DMSO and water were also plated as solvent controls. After a 96-h incubation period at 30 °C, a trypan blue exclusion assay was carried out to calculate the estimated average well count (trophozoites only) for each duplicate.
Host cell cytotoxicity assays
In 96-well plates, HeLa cells were treated with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in RPMI-1640. Chlorhexidine served as the positive treatment and RPMI-1640 alone as the negative treatment. The positive control and negative control were achieved in quadruplicates by treating HeLa cells with 1% Triton X-100 (100% cell death) and incubating in RPMI-1640 alone respectively. After the 24-h incubation period, the supernatant of each well was transferred to microcentrifuge tubes. Lactate dehydrogenase enzyme (LDH) assay was carried out using a cytotoxicity detection kit to measure absorbance reading at 490 nm. % cytotoxicity was calculated as (sample absorbance-negative control absorbance)/(positive control absorbance-negative control absorbance) × 100 (Aqeel et al. 2015).
Host cell cytopathogenicity assays
In 24-well plates, 5 × 105 A. castellanii trophozoites were treated with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in RPMI-1640. Chlorhexidine served as the positive treatment and RPMI-1640 alone as the negative treatment. After a 2-h incubation period, the treated trophozoites were centrifuged at 3000 rpm for 10 min and resuspended in 200 μl RPMI-1640 to retrieve viable trophozoites. The treated trophozoites were used to treat HeLa cells in 96-well plates at 37 °C for 24 h. The positive control and negative control were achieved in quadruplicates by treating HeLa cells with 1% Triton X-100 (100% cell death) and incubating in RPMI-1640 alone respectively. After the 24-h incubation period, the supernatant of each well was transferred to microcentrifuge tubes. Lactate dehydrogenase enzyme (LDH) assay was carried out using a cytotoxicity detection kit to measure absorbance reading at 490 nm. % cytopathogenicity was calculated as (sample absorbance-negative control absorbance)/(positive control absorbance-negative control absorbance) × 100 (Aqeel et al. 2015).
Statistical analysis
The results were shown as mean ± standard error of the three experiments performed in duplicates for each compound. The significance of the differences between the averages of negative and sample well counts were determined by using a two-sample t test with a two-tailed distribution, done on Microsoft Excel.
Results
Analyzing the conjugation of tetrazoles with silver nanoparticles with UV-Vis spectrophotometry, dynamic light-scattering, and Fourier-transform infrared spectroscopy
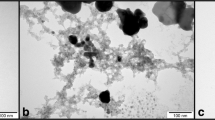
To ensure the conjugation of T1 and T2 to silver nanoparticles, the synthesized compounds were analyzed using UV-Vis spectrophotometry. From Fig. 2, the maximum absorption for T1-AgNP and T2-AgNP was observed at 417 nm and 398 nm respectively. Both maximum absorptions were within the range of the peak shown by AgNP which was expected to have a surface plasmon resonance (SPR) band at the range of 350 nm to 450 nm (Anwar et al. 2018). This shows that both tetrazoles have been successfully conjugated to the AgNP. DLS confirmed that the average size of nanoconjugates to be 52 and 70 nm. Figure 2b shows the T1-conjugated nanoparticles while Fig. 2c shows T2-conjugated nanoparticles as compared with compounds alone. Both FT-IR spectra show that the stabilization of nanoparticles was achieved by nitrogen of the tetrazole rings.
Increased antiamoebic activity was observed in tetrazole-conjugated AgNPs compared with tetrazoles alone
To determine the antiamoebic activity of tetrazoles alone and conjugated with AgNPs against A. castellanii, amoebicidal assays were carried out for each drug in duplicates for three times. Figure 3a shows the antiamoebic effect of T1 and T2 for all concentrations as compared with the negative control (5 × 105 trophozoites in RPMI-1640 alone). T1 did not exhibit significant amoebicidal activity while T2 showed significant and dose-dependent antiamoebic activity from 10 to 50 μM (*P < 0.05). The antiamoebic effect increased significantly when concentration was increased from 10 to 25 μM. IC50 of T2 was estimated to be within 10 μM to 25 μM. Figure 3b shows that both tetrazole-conjugated AgNP had higher antiamoebic activity compared with respective tetrazoles alone. However, only 10 μM T2-AgNP showed statistical significance when compared with negative control (5 × 105 trophozoites in RPMI-1640 alone), solvent control (AgNPs alone), and T2 alone (**P < 0.01). Figure 3b shows that the T2-AgNPs showed a 50% reduction in the viability of A. castellanii at 10 μM which corresponds to the IC50. This indicates that the conjugation of T2 to AgNP significantly increased the antiamoebic properties of T2 at 10 μM.
a Antiamoebic activity of T1 and T2 alone. b Antiamoebic activity of T1 and T2 conjugated with a silver nanoparticle. The assay was carried out by incubating each compound at concentrations 5 μM, 10 μM, 25 μM, and 50 μM with 5 × 105 trophozoites in RPMI-1640 at 30 °C for 24 h. Trypan blue exclusion assay was used to estimate the number of viable cells in each well and the average well count was calculated for each duplicate
Encystation of A. castellanii was inhibited with tetrazoles and nanoparticles
To determine the ability of the tetrazoles and AgNP-conjugated tetrazoles to prevent A. castellanii from converting from trophozoites to its dormant and more resistant form, cysts, encystation assay was carried out in duplicates for three times. Figure 4a shows that overall inhibition of encystation was higher for T2 compared with T1. Inhibition of encystation in T1 showed statistical difference for 10 μM (**P < 0.01), 25 μM (*P < 0.05), and 50 μM (***P < 0.001). Inhibition of encystation of T2 showed higher significance for all concentrations (***P < 0.001). From Fig. 4b, it can be observed that both T1-AgNP and T2-AgNP exhibited higher inhibition activity compared with respective tetrazoles. However, only T1-AgNP showed statistical significance as compared with the negative control (5 × 105 trophozoites in encystation medium), solvent control (AgNPs alone), and T1 alone (**P < 0.01). This indicates that the conjugation of T1 to AgNP significantly increased the inhibition of encystation at 5 μM.
a The effects of T1 and T2 on the encystation of A. castellanii. b The effects of T1-AgNP and T2-AgNP on the encystation of A. castellanii compared with T1 and T2 alone as well as AgNPs alone. The assay was carried out by incubating each compound with 5 × 105 trophozoites in PBS at 30 °C for 96 h. A total of 0.1% SDS was used to dissolve remaining trophozoites and the cysts were counted to calculate average well count for each duplicate. Statistical significance of the inhibition effects was determined using two-sample t test with two-tailed distribution, done on Microsoft Excel
Excystation of A. castellanii was inhibited with tetrazoles and nanoparticles
To determine the ability of tetrazoles alone and conjugated to AgNP to prevent A. castellanii cyst from reverting back to trophozoites, excystation assay was carried out in duplicates for three times. Figure 5a shows that both T1 and T2 have shown significant inhibition activities compared with the negative control (cyst alone) (**P < 0.01). However, activities of T1 at 25 μM and 50 μM, as well as T2 at 50 μM, showed statistical significance when compared with solvent control (0.025% DMSO (*P < 0.05)). At 25 μM, T1 shows higher effectiveness compared with T2. However, the effectiveness of T1 plateaued when concentration was increased to 50 μM. IC50 of T1 is estimated to be between 5 μM and 10 μM. From Fig. 5b, both tetrazole-conjugated AgNPs are shown to be slightly more effective compared with respective tetrazoles alone at concentration 5 μM. However, only 5 μM T2-AgNP showed statistical significance when compared with the negative control (1 × 105 cysts), solvent control (AgNPs alone), and T2 alone (*P < 0.05). This indicates that the conjugation of T2 to AgNPs significantly increases the inhibition of excystation at 5 μM.
a The effectiveness of T1 and T2 on inhibiting the excystation of A. castellanii. b The effectiveness of T1-AgNP and T2-AgNP on inhibiting the excystation of A. castellanii compared with T1 and T2 alone. The assay was carried out by incubating each compound with 5 × 105 cysts in PYG at 30 °C for 96 h. The viable trophozoites were counted with trypan blue exclusion assay and the average well count was calculated for each duplicate
Tetrazole-conjugated AgNPs and tetrazoles alone exhibited low human cell cytotoxicity
To evaluate the cell-damaging effects of tetrazole-conjugated AgNPs and tetrazoles alone on human HeLa cells, cytotoxicity assay was carried out in duplicates. From Fig. 6, T1-conjugated AgNPs exhibited the highest % cytotoxicity (18.6% and 14.8%) among all samples. However, all samples, including T1-conjugated AgNPs, showed lower % cytotoxicity compared with chlorhexidine (39% cytotoxicity) at 10 μM. Solvents used to prepare tetrazoles and NPs showed lower % cytotoxicity compared with Triton X and chlorhexidine as well.
Tetrazole-conjugated AgNPs and tetrazoles alone exhibited low host cell cytotoxicity. The assay was carried out by treating HeLa cells with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in RPMI-1640 followed by incubation for 24 h at 37 °C in a 5% CO2 incubator. After the 24-h incubation period, the supernatant of each well was transferred to microcentrifuge tubes and lactate dehydrogenase enzyme (LDH) assay was carried out to determine % cytotoxicity
Tetrazole-conjugated AgNPs significantly decreased cytopathogenicity of A. castellanii
To evaluate the A. castellanii-mediated cytotoxicity against HeLa cells after being treated with tetrazole-conjugated AgNPs and tetrazoles alone, cytopathogenicity assay was carried out in duplicates. Figure 7 shows that both T1 and T2 alone significantly decreased % cytopathogenicity of A. castellanii (*P < 0.05) compared with untreated A. castellanii (89%) only. T2-conjugated AgNPs exhibited significantly lower % cytopathogenicity compared with T2 alone (*P < 0.05).
T2-conjugated AgNPs significantly decreased % cytopathogenicity of A. castellanii. This assay was carried out by treating 5 × 105 A. castellanii trophozoites with 5 μM, 10 μM, 25 μM, and 50 μM of T1 and T2 respectively as well as 5 μM and 10 μM of tetrazole-conjugated AgNPs and AgNPs alone in RPMI-1640. After a 2-h incubation period, the treated trophozoites were used to treat HeLa cells in 96-well plates at 37 °C for 24 h. After the 24-h incubation period, the supernatant of each well was transferred to microcentrifuge tubes and lactate dehydrogenase enzyme (LDH) assay was carried out to determine % cytopathogenicity
Discussion
The major problems in GAE treatment are the formation of cysts and difficulty of drug delivery through the blood-brain barrier (BBB) due to the tight junctions; therefore, it is important to research for a formulation that can better penetrate the BBB (Anwar et al. 2018). Currently, one of the biggest challenges in research is delivering a drug to the site of treatment and release the drug at a specific rate to ensure maximum potency; thus, researchers are interested in developing efficient drug delivery systems (Kim et al. 2009). Drugs are usually low in potency due to low solubility which leads to aggregation, as well as short half-lives which causes the drug to degrade before reaching the target site (Parveen et al. 2012). Nanoparticles have much to offer in drug delivery as they allow the transport of drugs to specific target sites, sustained release of drugs, and are highly stable (Parveen et al. 2012). Metal nanoparticles such as AgNP were described to increase bioavailability and efficacy by reducing the size and shape of conjugated compounds and functioning as a drug carrier (Zazo et al. 2016).
Azoles are usually used as antifungal agents with a mode of actions such as ergosterol and CYP51 inhibition (Chopra and Khuller 1983; Hitchcock et al. 1990). Azoles were used in treating Acanthamoeba as ergosterol was found to be present on the membrane of the pathogen (Cabello-Vílchez et al. 2014). A study was also done by Lamb et al. (2015), where several antifungal agents such as fluconazole, itraconazole, and voriconazole were used to inhibit CYP51 of Acanthamoeba. However, treatment was not effective as Acanthamoeba and fungal CYP51 have low sequence identity as shown by NCBI-BLAST (Lamb et al. 2015). Existing treatments are also not effective against all strains of Acanthamoeba; therefore, it is crucial to perform mechanistically and in vivo studies to better understand the receptors and molecules that play a role in the pathogenesis of Acanthamoeba (Lorenzo-Morales et al. 2015).
As UV-Vis results (Fig. 2) show, T1 and T2 were successfully conjugated to AgNPs as both T1-AgNP and T2-AgNP showed SPR band at 417 nm and 398 nm which is within the expected SPR band range of 350 nm to 450 nm, indicating the formation of bonds between ligand (tetrazole) and AgNPs (Anwar et al. 2018). This study is focused on the development of anti-A. castellanii agent using two new synthetic tetrazoles and tetrazole-conjugated AgNPs. Antiamoebic assays showed (Figs. 3, 4, and 5) that at concentration 10 μM and above, T2 showed promising antiamoebic activities compared with T1 while encystation and excystation assays reveal that both T1 and T2 inhibited differentiation activity of Acanthamoeba castellanii. The use of T1 and T2 can allow the prevention of encystation of trophozoites, which makes the pathogen more susceptible to the antiamoebic effects of the tetrazoles or other drugs (Dart et al. 2009). Conjugation of T1 and T2 to AgNP also successfully increased the antiamoebic activities. This may be due to the increased bioavailability as AgNP allows better delivery of treatment compounds to A. castellanii by altering the shape, size, and surface properties of nanoparticles (Anwar et al. 2018). Host cell cytotoxicity and cytopathogenicity assays were also carried out to evaluate the host cell cytotoxicity as there is a lack of high-efficacy treatment with little adverse effects in treating AK and GAE. Cell cytotoxicity assay (Fig. 6) revealed that tetrazoles and AgNPs are significantly less toxic towards host cells compared with chlorhexidine which is known to cause undesirable side effects. Cytopathogenicity assay also revealed that T2-conjugated AgNPs reduced cytopathogenicity of A. castellanii compared with T2 alone (Fig. 7), suggesting that T2 is an effective anti-Acanthamoeba agent.
Conclusion
In conclusion, the study suggests that T1- and T2-conjugated AgNPs are effective anti-Acanthamoeba agents with minimal adverse effects compared with chlorhexidine. This may be due to the increased bioavailability as AgNP allows better delivery of treatment compounds to A. castellanii. Metal nanoparticles can potentially accumulate in the liver; therefore, the degradation process of nanoparticles should be addressed. It is crucial to further study the mechanism of pathogenesis of Acanthamoeba to better understand the crucial receptors that play a role in the process. This would ultimately lead to a more targeted and effective treatment for Acanthamoeba infections. However, animal studies should be performed to validate these results.
Change history
24 January 2022
This article has been retracted. Please see the Retraction Notice for more detail: https://doi.org/10.1007/s00436-022-07440-8
References
Anwar A, Siddiqui R, Hussain MA, Ahmed D, Shah MR, Khan NA (2018) Silver nanoparticle conjugation affects antiacanthamoebic activities of amphotericin B, nystatin, and fluconazole. Parasitol Res 117(1):265–271
Anwar A, Khan NA, Siddiqui R (2019) Galactose as novel target against Acanthamoeba cysts. PLoS Negl Trop Dis 13(7):e0007385
Anwar A, Ting ELS, Anwar A, Ul Ain N, Faizi S, Shah MR, Khan NA, Siddiqui R (2020) Antiamoebic activity of plant-based natural products and their conjugated silver nanoparticles against Acanthamoeba castellanii (ATCC 50492). AMB Express 10(1):24
Aqeel Y, Siddiqui R, Anwar A, Shah MR, Khoja S, Khan NA (2015) Photochemotherapeutic strategy against Acanthamoeba infections. Antimicrob Agents Chemother 59(6):3031–3041
Aqeel Y, Siddiqui R, Anwar A, Shah MR, Khan NA (2016) Gold nanoparticle conjugation enhances the antiacanthamoebic effects of chlorhexidine. Antimicrob Agents Chemother 60(3):1283–1288
Band RN, Mohrlok S (1973) The cell cycle and induced amitosis in Acanthamoeba. J Protozool 20(5):654–657
Barisani-Asenbauer T, Walochnik J, Mejdoubi L, Binder S (2012) Successful management of recurrent Acanthamoeba keratitis using topical and systemic miltefosine. Acta Ophthalmol 90:0–0
Bello-Vieda N, Pastrana H, Garavito M, Ávila A, Celis A, Muñoz-Castro A, Restrepo S, Hurtado J (2018) Antibacterial activities of azole complexes combined with silver nanoparticles. Molecules 23(2):361
Bendensky A, Menéndez D, Ostrosky-Wegman P (2002) Is metronidazole carcinogenic? Mutat Res/Rev Mutat Res 511(2):133–144
Cabello-Vílchez AM, Martín-Navarro CM, López-Arencibia A, Reyes-Batlle M, Sifaoui I, Valladares B, Piñero JE, Lorenzo-Morales J (2014) Voriconazole as a first-line treatment against potentially pathogenic Acanthamoeba strains from Peru. Parasitol Res 113(2):755–759
Cano PA, Islas-Jácome A, González-Marrero J, Yépez-Mulia L, Calzada F, Gámez-Montaño R (2014) Synthesis of 3-tetrazolylmethyl-4H-chromen-4-ones via Ugi-azide and biological evaluation against Entamoeba histolytica, Giardia lamblia and Trichomona vaginalis. Bioorg Med Chem 22(4):1370–1376
Chopra A, Khuller GK (1983) Lipids of pathogenic fungi. Prog Lipid Res 22(3):189–220
Dai LL, Zhang HZ, Nagarajan S, Rasheed S, Zhou CH (2015) Synthesis of tetrazole compounds as a novel type of potential antimicrobial agents and their synergistic effects with clinical drugs and interactions with calf thymus DNA. MedChemComm 6(1):147–154
Dart JK, Saw VP, Kilvington S (2009) Acanthamoeba keratitis: diagnosis and treatment update 2009. Am J Ophthalmol 148(4):487–499
Egger S, Lehmann RP, Height MJ, Loessner MJ, Schuppler M (2009) Antimicrobial properties of a novel silver-silica nanocomposite material. Appl Environ Microbiol 75(9):2973–2976
Fatima I, Zafar H, Khan KM, Saad SM, Javaid S, Perveen S, Choudhary MI (2018) Synthesis, molecular docking and xanthine oxidase inhibitory activity of 5-aryl-1H-tetrazoles. Bioorg Chem 79:201–211
Garajová M, Mrva M, Timko L, Lukáč M, Ondriska F (2014) Cytomorphological changes and susceptibility of clinical isolates of Acanthamoeba spp. to heterocyclic alkylphosphocholines. Exp Parasitol 145:S102–S110
Garajová M, Mrva M, Vaškovicová N, Martinka M, Melicherová J, Valigurová A (2019) Cellulose fibrils formation and organisation of cytoskeleton during encystment are essential for Acanthamoeba cyst wall architecture. Sci Rep 9(1):4466
Gupta AK, Lyons DC (2015) The rise and fall of oral ketoconazole. J Cutan Med Surg 19(4):352–357
Hitchcock CA, Dickinson K, Brown SB, Evans EGV, Adams DJ (1990) Interaction of azole antifungal antibiotics with cytochrome P-450-dependent 14α-sterol demethylase purified from Candida albicans. Biochem J 266(2):475–480
Khan NA (2006) Acanthamoeba: biology and increasing importance in human health. FEMS Microbiol Rev 30(4):564–595
Khunkitti W, Lloyd DFJR, Furr JR, Russell AD (1998) Acanthamoeba castellanii: growth, encystment, excystment and biocide susceptibility. J Inf Secur 36(1):43–48
Kim S, Kwon K, Kwon IC, Park K (2009) Nanotechnology in drug delivery: past, present, and future. In: Nanotechnology in drug delivery. Springer, New York, pp 581–596
Köhsler M, Mrva M, Walochnik J (2016) Acanthamoeba. In: Molecular parasitology. Protozoan parasites and their molecules. Springer-Verlag, Wien, pp 285–324
Kulsoom H, Baig AM, Siddiqui R, Khan NA (2014) Combined drug therapy in the management of granulomatous amoebic encephalitis due to Acanthamoeba spp., and Balamuthia mandrillaris. Exp Parasitol 145:S115–S120
Lamb DC, Warrilow AG, Rolley NJ, Parker JE, Nes WD, Smith SN, Kelly DE, Kelly SL (2015) Azole antifungal agents to treat the human pathogens Acanthamoeba castellanii and Acanthamoeba polyphaga through inhibition of sterol 14α-demethylase (CYP51). Antimicrob Agents Chemother 59(8):4707–4713
Lingling D, Shengfeng C, Damu GL, Chenghe Z (2013) Recent advances in the synthesis and application of tetrazoles. Chinese J Org Chem 33(2):224–244
Lorenzo-Morales J, Khan NA, Walochnik J (2015) An update on Acanthamoeba keratitis: diagnosis, pathogenesis and treatment. Parasite 22:10
Łukowska-Chojnacka E, Mierzejewska J, Milner-Krawczyk M, Bondaryk M, Staniszewska M (2016) Synthesis of novel tetrazole derivatives and evaluation of their antifungal activity. Bioorg Med Chem 24(22):6058–6065
Nampoothiri RV, Malhotra P, Jain A, Batra N, Gupta K, Saj F, Khurana S, Mahalingam H, Lal A, Mukherjee K, Radotra B, Varma S (2018) An unusual cause of central nervous system infection during acute myeloid leukemia induction chemotherapy: Acanthamoeba brain abscess. Indian J Hematol Blood Transfus 34(1):153–155
Padzik M, Hendiger EB, Chomicz L, Grodzik M, Szmidt M, Grobelny J, Lorenzo-Morales J (2018) Tannic acid-modified silver nanoparticles as a novel therapeutic agent against Acanthamoeba. Parasitol Res 117(11):3519–3525
Padzik M, Hendiger EB, Żochowska A, Szczepaniak J, Baltaza W, Pietruczuk-Padzik A, Olędzka G, Chomicz L (2019) Evaluation of in vitro effect of selected contact lens solutions conjugated with nanoparticles in terms of preventive approach to public health risk generated by Acanthamoeba strains. Ann Agric Environ Med 26(1):198–202
Parveen S, Misra R, Sahoo SK (2012) Nanoparticles: a boon to drug delivery, therapeutics, diagnostics and imaging. Nanomed: Nanotechnol Biol Med 8(2):147–166
Schuster FL, Visvesvara GS (2004) Free-living amoebae as opportunistic and non-opportunistic pathogens of humans and animals. Int J Parasitol 34(9):1001–1027
Sharma R, Jhanji V, Satpathy G, Sharma N, Khokhar S, Agarwal T (2013) Coinfection with Acanthamoeba and Pseudomonas in contact lens–associated keratitis. Optom Vis Sci 90(2):e53–e55
Siddiqui R, Khan NA (2012) Biology and pathogenesis of Acanthamoeba. Parasit Vectors 5(1):6
Sissons J, Alsam S, Stins M, Rivas AO, Morales JL, Faull J, Khan NA (2006) Use of in vitro assays to determine effects of human serum on biological characteristics of Acanthamoeba castellanii. J Clin Microbiol 44(7):2595–2600
Slater CA, Sickel JZ, Visvesvara GS, Pabico RC, Gaspari AA (1994) Successful treatment of disseminated Acanthamoeba infection in an immunocompromised patient. N Engl J Med 331(2):85–87
Tavassoli S, Buckle M, Tole D, Chiodini P, Darcy K (2018) The use of miltefosine in the management of refractory Acanthamoeba keratitis. Contact Lens Anterior Eye 41(4):400–402
Timko L, Fischer-Fodor E, Garajová M, Mrva M, Chereches G, Ondriska F, Bukovský M, Lukáč M, Karlovská J, Kubincová J, Devínsky F (2015) Synthesis of structural analogues of hexadecylphosphocholine and their antineoplastic, antimicrobial and amoebicidal activity. Eur J Med Chem 93:263–273
Tu EY, Joslin CE, Shoff ME (2010) Successful treatment of chronic stromal Acanthamoeba keratitis with oral voriconazole monotherapy. Cornea 29(9):1066
Webster D, Umar I, Kolyvas G, Bilbao J, Guiot MC, Duplisea K, Qvarnstrom Y, Visvesvara GS (2012) Treatment of granulomatous amoebic encephalitis with voriconazole and miltefosine in an immunocompetent soldier. Am J Trop Medi Hyg 87(4):715–718
Weisman RA (1976) Differentiation in Acanthamoeba castellanii. Annu Rev Microbiol 30(1):189–219
Xuguang S, Lin C, Yan Z, Zhiqun W, Ran L, Shiyun L, Xiuying J (2003) Acanthamoeba keratitis as a complication of orthokeratology. Am J Ophthalmol 136(6):1159–1161
Zazo H, Colino CI, Lanao JM (2016) Current applications of nanoparticles in infectious diseases. J Control Release 224:86–102
Funding
This work is supported by the Sunway University, Malaysia (GRTIN-RRO-98-2020), and the Pakistan Academy of Sciences for providing financial support Project No. (5-9/PAS/440).
Author information
Authors and Affiliations
Contributions
The study was conducted by team effort of all authors. The manuscript was submitted with the consent of all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Not required.
Additional information
Section Editor: Julia Walochnik
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article has been retracted. Please see the retraction notice for more detail: https://doi.org/10.1007/s00436-022-07440-8
About this article
Cite this article
Anwar, A., Yi, Y.P., Fatima, I. et al. RETRACTED ARTICLE: Antiamoebic activity of synthetic tetrazoles against Acanthamoeba castellanii belonging to T4 genotype and effects of conjugation with silver nanoparticles. Parasitol Res 119, 1943–1954 (2020). https://doi.org/10.1007/s00436-020-06694-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-020-06694-4