Abstract
Lymphatic filariasis (LF) is a serious vector-borne health problem, and Wuchereria bancrofti (W.b) is the major cause of LF worldwide and is focally endemic in Egypt. Identification of filarial infection using traditional morphologic and immunological criteria can be difficult and lead to misdiagnosis. The aim of the present study was molecular detection of W.b in residents in endemic areas in Egypt, sequence variance analysis, and phylogenetic analysis of W.b DNA. Collected blood samples from residents in filariasis endemic areas in five governorates were subjected to semi-nested PCR targeting repeated DNA sequence, for detection of W.b DNA. PCR products were sequenced; subsequently, a phylogenetic analysis of the obtained sequences was performed. Out of 300 blood samples, W.b DNA was identified in 48 (16%). Sequencing analysis confirmed PCR results identifying only W.b species. Sequence alignment and phylogenetic analysis indicated genetically distinct clusters of W.b among the study population. Study results demonstrated that the semi-nested PCR proved to be an effective diagnostic tool for accurate and rapid detection of W.b infections in nano-epidemics and is applicable for samples collected in the daytime as well as the night time. PCR products sequencing and phylogenitic analysis revealed three different nucleotide sequences variants. Further genetic studies of W.b in Egypt and other endemic areas are needed to distinguish related strains and the various ecological as well as drug effects exerted on them to support W.b elimination.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Lymphatic filariasis (LF) is a serious vector-borne health problem, and Wuchereria bancrofti (W.b) is the major cause (90%) of LF worldwide and is focally endemic in Egypt. The disease has been identified by World Health Organization (WHO) as a leading cause of permanent and long-term disability. In addition to medical problems, there are severe social and psychological consequences especially for those who suffer from elephantiasis or hydrocoele (Melrose 2002; Foo et al. 2011).
Following the launching of the “Global Program to Eliminate Lymphatic Filariasis” (GPELF), Egypt was among the first countries to implement a national program to eliminate LF based on WHO’s strategy of repeated rounds mass drug administration (MDA) in the form of albendazole with diethylcarbamazine (DEC). Subsequently, transmission was shown to be markedly reduced among villages that prior to MDA exhibited some of the highest rates of LF (Hotez et al. 2012; Upadhyayula et al. 2012).
Diagnostic tools play a significant role in the control of LF. The exponential growth of GPELF has highlighted the need for sensitive tools to monitor progress toward programmatic endpoints, to conduct surveillance with rapid and early detection of cases that can be often challenging. A definitive diagnosis requires detection of the parasite, parasite antigen, or parasite DNA. However, the limitations of microfilariae (Mf) detection and immunoassays have made the identification of filarial infection difficult, which can lead to misdiagnosis (Lammie et al. 2004; Weil and Ramzy 2007; Mendoza et al. 2009; Nuchprayoon 2009; Fox and King 2012). Recent advances in molecular biological technology have influenced parasitologists toward the use of polymerase chain reaction (PCR)-based assays, which not only offer the possibility of improved sensitivity and specificity but also provide new insights into the structure and function of the filarial genome, in addition to helping in the identification of drug targets (Lulitanond et al. 2004; Kanjanavas et al. 2005; Liu and Austin 2013).
The present study was a continuation of an earlier work (Abdel Shafi et al. 2016), and its aim was to determine the molecular epidemiology of W.b in blood samples collected from cohort of Egyptians residing in selected endemic areas. Presently, there is a lot of genetic and genomic data for infectious and vector borne diseases such as malaria; however, there is a scarcity of this data for W.b. Consequently, the present study aimed for sequence variance analysis and phylogenetic analysis of W.b DNA sequences and explores its interspecies and intraspecies variation to hasten the elimination programs of W.b.
Method
The study setting and most of the sampling were conducted under the authorization and guidance of the Egyptian Ministry of Health and Population (MOHP)–Malaria, Filariasis and Leishmaniasis Control Department, between October 2012 and March 2014.
The study was reviewed and approved by the Research Ethics Committee of the Faculty of Medicine, Cairo University (N-42-2013). An informed consent was obtained from each participant.
Sampling
The study was carried out on 300 blood samples collected from individuals residing in filariasis endemic areas in five governorates (Giza, Qualioubiya, Menoufiya, Dakahliya, and Sharkiya). Relevant data were obtained with each blood sample. The sample collection was performed at night in Qualioubiya and part of Giza, while the rest of sampling was done during the daytime.
Parasitological examination
For the microscopic examination of Mf, MOHP personnel prepared the thick blood films for the samples collected at night, examined them in their laboratory, and reported the results. Knott’s concentration technique was performed for the blood samples collected in the daytime as described by Garcia (2007).
DNA extraction
All the blood samples were subjected to DNA extraction using QIAamp DNA Blood Mini Kit (Qiagen, Germany). The procedure was performed according to the manufacturer’s instructions with modifications in the form of prolongation of incubation after 56°C at 50 min to 90°C for 10 min, and then the purified DNA was measured for concentration and purity.
Molecular assay
DNA samples were subjected to semi-nested PCR amplification which consisted of two PCR runs. Three primers—a forward primer WbF (5′-CACCGGTATCGAGATTAATT-3′), and reverse primers WbR (5′-TTGTTCCTCTATTTGAGACC-3′) and Wb2 (5′-TGGATGTATGTCAAAAAGCA-3′)—were used for PCR amplification targeting repetitive DNA sequences (pWb12 repetitive region) specific for W.b as described by Kanjanavas et al. (2005). In the 1ry PCR, the reaction volume was 25 μl in each tube composed of 12.5 μl of DreamTaq Green PCR Master Mix (2×), 1 μl (5 pmol) of WbF, 1 μl (5 pmol) of WbR, 0.1 μl DreamTaq Polymerase enzyme–ThermoScientific (5 U/μl), 4 μl of DNA sample, and 6.4 μl of sterile dd H2O. Using the Biometra TPersonal thermocycler, the 1ry amplification was optimized in the following conditions: initial denaturation at 95°C for 4 min, 30 cycles each consisting of denaturation at 95°C for 1 min, annealing at 50°C for 1 min, and extension at 72°C for 1.5 min, and final extension at 72°C for 10 min. The expected fragment length was 780 bp. While in the 2ry PCR, the reaction volume was 25 μl composed of 12.5 μl of DreamTaq Green PCR Master Mix (2×) 1 μl of WbF, 1 μl of Wb2, 0.1 μl DreamTaq Polymerase enzyme (5 U/μl), 1 μl of product from the 1ry PCR run, and 9.4 μl of sterile dd H2O. The conditions for the 2ry amplification were optimized on initial denaturation at 95°C for 4 min, 30 cycles each consisting of denaturation at 95°C for 30 s, annealing at 55°C for 30 s and extension at 72°C for 45 s, and final extension at 72°C for 10 min. The expected fragment length was 400 bp. For the PCR assay, every 1ry and 2ry run included a negative control, using sterile dd H2O instead of DNA extract in the reaction mix, as well as a positive control from DNA extract of a reference sample. Analysis of PCR products was performed via 1.5% agarose gel electrophoresis and was visualized under UV light transilluminator.
DNA sequencing
Secondary PCR products showing the positive W.b band of 400 bp were prepared to be set for sequencing. Amplicons were first purified using Illustra GFX PCR DNA and Gel band Purification Kit–GE Healthcare. The procedure was performed following the manufacturer instructions. The recovered purified DNA was tested for quantity and purity using a nanodrop spectrophotometer and then kept in refrigerator at 4°C. For each purified DNA sample, a WbF primer mixture and a Wb2 primer mixture were prepared in a 96-well PCR plate; each mixture contained 1 μl purified DNA, 8 μl of dd H2O, and 1 μl of WbF or Wb2 (6 pmol/μl), accordingly. The mixtures were subjected to sequencing using Sanger method at the Genome unit – National Centre of Microbiology – Instituto De Salud Carlos III. The sequencing output was proofread and edited by using Chromas LITE v2.1.1 and BioEdit Sequence Alignment Editor v7.2.5.0 programs. The nucleotide sequences obtained were checked by BLAST search in NCBI website for determining similarities with previously reported sequences. Multiple sequence alignment was done for the retrieved reference sequences from GenBank together with the study sequences by using ClustalW tool in BioEdit program.
Phylogenetic analysis
From the multiple sequence alignment, phylogenetic tree was calculated by the neighbor-joining distance matrix method and was statistically evaluated by bootstrap test using TREECON program.
Results
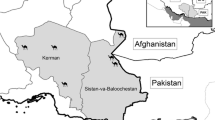
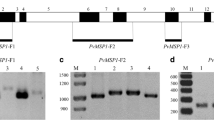
Out of 300 blood samples, W.b Mf was detected in only one sample collected at night, and it was considered a reference sample after molecular identification, sequencing, and alignment against GenBank databases. W.b DNA was detected in 48 samples (16%) including the reference sample (Fig. 1), of which 29 samples (60.4%) were collected in daytime and 19 samples at night (39.6%). Complete data were available for 46 cases out of 48 positive cases. Regarding the demographic data of the positive cases, 54.2% were females and 45.8% were males. As age data were missing for two cases, the age distribution was performed for a total of 46 cases ranging from 10 to 86 years old, with a mean age of 36.7 (Fig. 2). The 48 positive cases were residing in various governorates: 2 in Dakahlia, 9 in Giza, 23 in Menoufia, 13 in Qualioubia, and one in Sharkia (Fig. 3). Concerning the clinical data, 41 (85.4%) of the positive cases were normal endemics, 3 (6.2%) clinically suspected cases, 2 (4.2%) asymptomatic LF cases diagnosed by MOHP personnel during routine screening, and 2 (4.2%) chronic LF cases with lymphoedema. Among the 46 positive cases with complete data, 5 individuals reported having a household member diagnosed or suffering from LF, and 36 individuals gave history of MDA intake.
Detection of W. bancrofti DNA using semi-nested PCR on ethidium bromide stained agarose gel. Molecular weight marker of 100 bp (lane 1), test samples (lanes 2–11), positive control (lanes 12 and 13), negative control (lane 14), positive control of 2ry PCR (lane 15), and negative control of 2ry PCR reaction (lane 16)
DNA sequencing was performed for the amplified semi-nested PCR product of 15 samples, and these included the reference sample in addition to 14 positive samples collected from 4 governorates, Giza, Menoufiya, Dakahliya, and Qualioubiya.
Blast analyses of the obtained nucleotide sequences showed high similarity with W.b (clone pWb 2.5) repeat region, W.b repetitive DNA sequence, and W.b genome assembly (W.b Jakarta, scaffold WBA-contig 0007364), available in NCBI database (GenBank accession no: L30137.1, L19892.1, and LM008700.1, respectively). The retrieved reference sequences together with the study sequences were subjected to multiple sequence alignment. Patterns of nucleotide variation were observed among the study sequences (Fig. 4). A rooted neighbor-joining tree was constructed using Brugia timori as outgroup (Fig. 5). The phylogenetic tree also depicted the genetic variation within the study sequences. W.b sequences obtained in the present study were submitted to the GenBank and were assigned the following accession numbers: KP114615, KP114616, KP114617, KP114618, KP114619, KP114620, KP114621, KP114622, KP114623, KP114624, KP114625, KP114626, KP114627, KP114628, and KP114629.
Multiple sequence alignment of the sequenced DNA and the reference W. bancrofti sequences on NCBI-BLAST. There are 404 nucleotide position in this matrix data. The regions of similarity between the sequences are shown as dots, while the dispersed letters indicate the nucleotide variations. The gaps are represented in dashes. Black, yellow, and red boxes indicate the three observed patterns of nucleotide diversity
Discussion
Bancroftian filariasis is a worldwide major disabling disease, requires simple, accurate diagnostic tool to determine its true prevalence especially in nano-epidemic areas and areas with MDA that have low intensity of infection. Since there is scarce knowledge about W.b biology due to difficulty to access adult stage and no culture or animal model to amplify in lab though, molecular studies and phylogeny are essentials.
In the present work, WbF, WbR, and Wb2 primers targeting the W.b repetitive region were used. This region was first cloned and characterized by Siridewa et al. (1994). The cloned repeats, designated pWb12, consisted of 969 bp of moderate copy number (450–700) and were interspersed within the parasite genome. In 1996, Siridewa et al. designed a conventional PCR targeting the 490-bp fragment within the pWb12 repeat region for the specific identification of W.b in various clinical samples.
To combat low amplification of single-step PCR, Kanjanavas et al. (2005) developed a semi-nested PCR targeting pWb12 repeat region for the detection of W.b in samples of low parasitaemia as well as long-term stored blood which can detect W.b infection in low prevalence following MDA (Gordon et al. 2011; Gass et al. 2012). Lately, Ximenes et al. (2014) standardized a semi-nested PCR assay for the diagnosis of bancroftian filariasis from various clinical samples. Both studies agreed that this PCR system is species-specific, showing no cross-reactivity with other parasites or Homo sapiens DNA. This species-specific PCR assay was used in this study and revealed high molecular prevalence among studied population. Since Mf are required to transmit infection, the parasitological detection of Mf is a measure of justifiable interest to the GEPLF. However, this method posed many problems, as it misdiagnosed low-density microfilaraemic and amicrofilaramic individuals. The GPELF considers it un-preferred method by for field application (Melrose et al. 2004; Pandey et al. 2011; Rebollo and Bockarie 2013). Determination of molecular epidemiology of W.b and its early diagnosis in MDA areas impact effective treatment and infection control.
Our study found a discrepancy between Mf and W.b DNA detection. There are many factors that may explain this discrepancy. The semi-nested PCR used in the present work has detected all parasite stages of development of infection, including Mf, adult worms, and free circulating DNA derived from the parasite. It was suggested that the higher sensitivity of PCR may be attributed to the shedding of parasitic DNA from parasitic components such as cuticular cells rather than actual presence of a parasite within the portion of clinical sample used for DNA extraction (Fischer et al. 2003; Wong et al. 2014; Ximenes et al. 2014).
Accordingly, W.b DNA may be detected in patients with low or no microfilaraemia as well as from various clinical samples, in addition to whole blood, such as plasma, serum, and samples collected in noninvasive manner, like urine and sputum (Fischer et al. 2003; Kanjanavas et al. 2005; Ximenes et al. 2014).
In addition, 60% (29/48) of PCR positive samples were daytime blood samples which are not valid for Mf detection. Many studies reported similar findings (Furtado et al. 1997; Lucena et al. 1998; Ramzy 2002; Ximenes et al. 2014).
PCR-based assays may not be applicable for field studies; nonetheless, they remain important laboratory tools with growing potential for clinical applications, due to their high accuracy, and the relative ease of the interpretation of results using optimized protocols. Furthermore, PCR-based assays enable identification of sequence variations in order to distinguish between related species and strains (Fischer et al. 2003; Gordon et al. 2011; Small et al. 2014).
Due to the long interval between the performance of PCR and sequencing, and excluded samples with low nanodrop readings, DNA sequencing was performed for the amplified semi-nested PCR product of only 15 samples from 4 governorates. Small et al. (2014) highlighted that W.b falls far behind the other filarial nematodes in available genomic data, of which only one whole genome sequence has been published (Desjardins et al. 2013). Two more studies published mitochondrial genomes from Mali and India (Ramesh et al. 2012; McNulty et al. 2013). However, several studies have used selected nuclear and mitochondrial loci for DNA sequence (Schwab et al. 2005; Sakthidevi et al. 2013; Small et al. 2013; De Souza et al. 2014).
Molecular typing, genetic diversity, and phylogenetics of W.b. enable the inference of history of infection, strain typing, and the understanding of population structure and dynamics. These information help to interrupt transmission, to apply drug treatment, to predict drug resistance, and to support GPELF goals. Sequence analysis confirmed the results of semi-nested PCR and identified only W.b. In the present study, sequence alignment and phylogenetic analysis revealed new strains of W.b. clustered in three different patterns of nucleotide sequences, all of them belonging to a monophyletic group. McNulty et al. (2013) reported that regardless of the genetic marker analyzed, both Wuchereria and Brugia consistently form a monophyletic group. Despite, the small size of our data set, the three clusters found are distributed within the four governorates and are not restricted to one geographical location. W.b strain distribution varies by infection locality, after MDA intervention and can be extremely focal yet heterogeneous in small geographic area (WHO 2012).
Tracking of genetic variation of parasite strains can lead to detection of transmission pattern and determine cause of re-introduction of infection especially with MDA intervention. The obtained genetic diversity in the present study may be attributed to environmental stresses, MDA intervention, and high diversity of population dynamics compounded by higher population densities in the studied governorates. Similarly, the use of phylogenetic tree-based RAPD 2 studies in Ghana and India revealed interspecies variation among W.b (Thangadurai et al. 2006; Patra et al. 2007). Variation in symptomatic/asymptomatic patients and different disease manifestations among study populations can be explained by the presence of different parasite strains.
Such genetic diversity may influence vector-parasite co-adaptation and affect vector competence. The same W.b vector strain, Culex quinquofasciatus, showed two different susceptibility patterns of two variant W.b strains from Liberia (vector was more efficient) and Sri-Lanka (vector was less efficient) and explained the difference in disease epidemiology in East and West Africa (Jayasekera et al. 1980; Ramesh et al. 2012; Ughasi et al. 2012) and in southern and northern Ghana (de Souza et al. 2014).
GPELF relies upon ivermectin and albendazole for which there is no clear evidence of development of drug resistance in filaria (Schwab et al. 2005; Bisht et al. 2006). The pressure of using these drugs in human may lead to genetic diversity of W.b populations.
The GPELF in Egypt has resulted in a significant reduction of W.b prevalence. The new data of strain distribution provided in the present study contributes toward understanding infection dynamics in Egypt and W.b elimination strategies. The genetic diversity should be further studied to investigate the possibilities of resurgence of Egyptian endemic parasite strains or parasite importation.
Conclusion
In conclusion, study results demonstrate that the semi-nested PCR is an effective diagnostic tool for accurate, easy, early, and rapid detection of W.b infections in nano-epidemics. It is applicable for samples collected in the daytime as well as the night time and should replace conventional tests in GPEFL for identification of MDA areas, MDA surveillance, monitoring, and termination. In addition, semi-nested PCR products can be sequenced and phylogenetic tree can be constructed. The PCR products sequencing and phylogenitic analysis of the present study revealed three different nucleotide sequences variants. Although this study was analyzed a small number of W.b sequences, we cannot neglect the possibility that this genetic diversity may be influenced MDA. However, further genetic studies of W.b in Egypt and other endemic areas are required in order to distinguish related strains as well as identify the various ecological and drug related effects, which may influence the GPELF outcome.
References
Abdel Shafi IR, Shoeib EY, Attia SS, Rubio JM, El-Badry AA (2016) Wuchereria bancrofti microfilariae and quantitative circulating antigen detection in selected endemic areas in Egypt. Kasr Al Ainy Med J 22:34–40. doi:10.4103/1687-4625.182556
Bisht R, Hoti SL, Thangadurai R, Das PK (2006) Isolation of Wuchereria bancrofti microfilariae from archived stained blood slides for use in genetic studies and amplification of parasite and endosymbiont genes. Acta Trop 99:1–5. doi:10.1016/j.actatropica.2005.12.009
De Souza DK, Osei-Poku J, Blum J, Baidoo H, Brown CA, Lawson BW, Wilson MD, Bockarie MJ, Boakye DA (2014) The epidemiology of lymphatic filariasis in Ghana, explained by the possible existence of two strains of Wuchereria bancrofti. Pan Afr Med J 17:133. doi:10.11604/pamj.2014.17.133.3370
Desjardins CA, Cerqueira GC, Goldberg JM, Dunning Hotopp JC, Haas BJ, Zucker J, Ribeiro JMC, Saif S, Levin JZ, Fan L, Zeng Q, Russ C, Wortman JR, Fink DL, Birren BW, Nutman TB (2013) Genomics of Loa loa, a Wolbachia-free filarial parasite of humans. Nat Genetics 45:495–500. doi:10.1038/ng.2585
Fischer P, Boakye D, Hamburger J (2003) Polymerase chain reaction-based detection of lymphatic filariasis. Med Microbiol Immunol 192(1):3–7. doi:10.1007/s00430-002-0152-z
Foo PK, Tarozzi A, Mahajan A, Yoong J, Krishnan L, Kopf D, Blackburn BG (2011) High prevalence of Wuchereria bancrofti infection as detected by immunochromatographic card testing in five districts of Orissa, India, previously considered to be non-endemic. Trans Roy Soc Trop Med Hyg 105(2):109–114. doi:10.1016/j.trstmh.2010.10.006
Fox LM and King CL (2012) Lymphatic filariasis. In: Magill AJ, Hill DR, Solomon T, Ryan ET (ed) Hunter’s Tropical Medicine and Emerging Infectious Diseases, 9th edn. Saunders Elsevier Press, pp 816–822.
Furtado AF, Abath FGC, Regis L, Gomes YM, Lucena WA, Furtado PB, Dhalia R, Miranda JC, Nicolas L (1997) Improvement and application of a polymerase chain reaction system for detection of Wuchereria bancrofti in Culex quinquefasciatus and human blood samples. Mem Inst Oswaldo Cruz 92(1):85–86
Garcia LS (2007) Diagnostic Medical Parasitology. 5th edition, ASM Press.
Gass K, Beau de Rochars MVE, Boakye D, Bradley M, Fischer PU, Gyapong J, Itoh M, Ituaso-Conway N, Joseph H, Kyelem D, Laney SJ, Legrand AM, Liyanage TS, Melrose W, Mohammed K, Pilotte N, Ottesen EA, Plichart C, Ramaiah K, Rao RU, Talbot J, Weil GJ, Williams SA, Won KY, Lammie P (2012) A multicenter evaluation of diagnostic tools to define endpoints for programs to eliminate bancroftian filariasis. PLoS Negl Trop Dis 6(1):e1479. doi:10.1371/journal.pntd.0001479
Gordon CA, Gray DJ, Gobert GN, McManus DP (2011) DNA amplification approaches for the diagnosis of key parasitic helminth infections of humans. Mol Cell Probes 25(4):143–152. doi:10.1016/j.mcp.2011.05.002
Hotez PJ, Savioli L, Fenwick A (2012) Neglected tropical diseases of the Middle East and North Africa: review of their prevalence, distribution, and opportunities for control. PLoS Negl Trop Dis 6(2):e1475. doi:10.1371/journal.pntd.0001475
Jayasekera N, Curtis CF, Zielke E, Kuhlow F, Jansen CG, Chelliah RV (1980) The susceptibility of Liberian Culex quinquefasciatus to Wuchereria bancrofti in Sri Lanka. Tropenmed Parasitol 31(4):507–511
Kanjanavas P, Tan-ariya P, Khawsak P, Pakpitcharoen A, Phantana S, Chansiri K (2005) Detection of lymphatic Wuchereria bancrofti in carriers and long-term storage blood samples using semi-nested PCR. Mol Cell Probes 19(3):169–172. doi:10.1016/j.mcp.2004.11.003
Lammie PJ, Weil G, Noordin R, Kaliraj P, Steel C, Goodman D, Lakshmikanthan VB, Ottesen E (2004) Recombinant antigen-based antibody assays for the diagnosis and surveillance of lymphatic filariasis – a multicenter trial. Filaria J 3:9. doi:10.1186/1475-2883-3-9
Liu D and Austin FW (2013) Wuchereria. In: Liu D (ed) Molecular Detection of Human Parasitic Pathogens. CRC Press Taylor & Francis group, pp 723–729.
Lucena WA, Dahlia R, Abath FGC, Nicolas L, Regis LN, Furtado AF (1998) Diagnosis of Wuchereria bancrofti infection by the polymerase chain reaction using urine and day blood samples from amicrofilaremic patients. Trans Roy Soc Trop Med Hyg 92(3):290–293
Lulitanond V, Intapan PM, Pipitgool V, Choochote W, Maleewong W (2004) Rapid detection of Wuchereria bancrofti in mosquitoes by LightCycler polymerase chain reaction and melting curve analysis. Parasitol Res 94:337–341
McNulty SN, Mitreva M, Weil GJ, Fischer PU (2013) Inter and intra-specific diversity of parasites that cause lymphatic filariasis infection. Infect Genet Evol 14:137–146. doi:10.1016/j.meegid.2012.11.002
Melrose WD (2002) Lymphatic filariasis: new insights into an old disease. Int J Parasitol 32(8):947–960. doi:10.1016/S0020-7519(02)00062-0
Melrose WD, Durrheim DD, Burgess GW (2004) Update on immunological tests for lymphatic filariasis. Trends Parasitol 20(6):255–275. doi:10.1016/j.pt.2004.04.002
Mendoza N, Li A, Gill A, Tyring S (2009) Filariasis: diagnosis and treatment. Derm Therapy 22(6):475–490. doi:10.1111/j.1529-8019.2009.01271.x
Nuchprayoon S (2009) DNA-based diagnosis of lymphatic filariasis. SE Asian J Trop Med Pub Health 40(5):904–913
Pandey V, Madhumathi J, Karande AA, Kaliraj P (2011) Antigen detection assay with parasite specific monoclonal antibodies for diagnosis of lymphatic filariasis. Clin Chim Acta 412(19–20):1867–1873. doi:10.1016/j.cca.2011.06.029
Patra KP, Ramu T, Hoti SL, Pragasam GS, Das PK (2007) Identification of a molecular marker for genotyping human lymphatic filarial nematode parasite Wuchereria bancrofti. Exp Parasitol 116(1):59–65. doi:10.1016/j.exppara.2006.11.011
Ramesh A, Small ST, Kloos ZA, Kazura JW, Nutman TB, Serre D, Zimmerman PA (2012) The complete mitochondrial genome sequence of the filarial nematode Wuchereria bancrofti from three geographic isolates provides evidence of complex demographic history. Mol Bioch Parasitol 183(1):32–41. doi:10.1016/j.molbiopara.2012.01.004
Ramzy RMR (2002) Recent advances in molecular diagnostic techniques for human lymphatic filariasis and their use in epidemiological research. Trans Roy Soc Trop Med Hyg 96(Suppl 1):225–229
Rebollo MP, Bockarie MJ (2013) Rapid diagnostics for the endgame in lymphatic filariasis elimination. AmJTrop Med Hyg 89(1):3–4. doi:10.4269/ajtmh.13-0202
Sakthidevi M, Prabhu PR, Chowdhary S, Hoti SL, Kaliraj P (2013) Functional analysis of genetic polymorphism in Wuchereria bancrofti glutathione S-transferase antioxidant gene: impact on protein structure and enzyme catalysis. Mol Biochem Parasitol 192:10–20. doi:10.1016/j.molbiopara.2013.10.001
Schwab AE, Boakye DA, Kyelem D, Prichard RK (2005) Detection of benzimidazole resistance-associated mutations in the filarial nematode Wuchereria bancrofti and evidence for selection by albendazole and ivermectin combination treatment. AmJTrop Med Hyg 73(2):234–238
Siridewa K, Karunanayake EH, Chandrasekharan NV, Abeyewickreme W, Franzen L, Aslund L, Pettersson U (1994) Cloning and characterization of a repetitive DNA sequence specific for Wuchereria bancrofti. AmJTrop Med Hyg 51(4):495–500
Siridewa K, Karunanayake EH, Chandrasekharan NV (1996) Polymerase chain reaction-based technique for the detection of Wuchereria bancrofti in human blood samples, hydrocele fluid, and mosquito vectors. AmJTrop Med Hyg 54(1):72–76
Small ST, Ramesh A, Bun K, Reimer L, Thomsen E, Baea M, Bockarie MJ, Siba P, Kazura JW, Tisch DJ, Zimmerman PA (2013) Population genetics of the filarial worm Wuchereria bancrofti in a post-treatment region of Papua New Guinea: insights into diversity and life history. PLoS Neg Trop Dis 7(7):e2308. doi:10.1371/journal.pntd.0002308
Small ST, Tisch DJ, Zimmerman PA (2014) Molecular epidemiology, phylogeny and evolution of the filarial nematode Wuchereria bancrofti. Infect Genet Evol 28:33–43. doi:10.1016/j.meegid.2014.08.018
Thangadurai R, Hoti SL, Kumar NP, Das PK (2006) Phylogeography of human lymphatic filarial parasite, Wuchereria bancrofti in India. Acta Trop 98:297–304. doi:10.1016/j.actatropica.2006.06.004
Ughasi J, Bekhard H, Coulibaly M, Adabie-Gomez D, Gyapong J, Appawu M, Wilson MD, Boakye DA (2012) Mansonia Africana and Mansonia Uniformis are vectors in the transmission of Wuchereria bancrofti lymphatic filariasis in Ghana. Parasit Vectors 5:89. doi:10.1186/1756-3305-5-89
Upadhyayula SM, Mutheneni SR, Kadiri MR, Kumaraswamy S, Nelaturu SCB (2012) Data base management system for lymphatic filariasis a neglected tropical disease. PLoS One 7(7):e39970. doi:10.1371/journal.pone.0039970
Weil GJ, Ramzy RMR (2007) Diagnostic tools for filariasis elimination programmes. Trends Parasitol 23(2):78–82. doi:10.1016/j.pt.2006.12.001
WHO (2012) Global programme to eliminate lymphatic filariasis: progress report, 2011. Wkly Epidemiology Red 87(37):346–356
Wong SSY, Fung KSC, Chau S, Poon RWS, Wong SCY, Yuen KY (2014) Molecular diagnosis in clinical parasitology: when and why? Exp Biol Med 239(11):1443–1460. doi:10.1177/1535370214523880
Ximenes C, Brandão E, Oliveira P, Rocha A, Rego T, Medeiros R, Aguiar-Santos A, Ferraz J, Reis C, Araujo P, Carvalho L, Melo FL (2014) Detection of Wuchereria bancrofti DNA in paired serum and urine samples using polymerase chain reaction-based systems. Mem Inst Oswaldo Cruz 109(8):978–983. doi:10.1590/0074-0276140155
Contribution of each author
All the manuscript authors contributed to every activity of it: idea of paper, study design, collection of materials, methodology, writing the paper, and revising it.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Abdel-Shafi, I.R., Shoieb, E.Y., Attia, S.S. et al. Molecular identification and phylogenetic analysis of Wuchereria bancrofti from human blood samples in Egypt. Parasitol Res 116, 963–970 (2017). https://doi.org/10.1007/s00436-017-5372-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-017-5372-7