Abstract
Several lines of evidence suggest that Acanthamoeba interact with bacteria, which may aid in pathogenic bacterial transmission to susceptible hosts, and these interactions may have influenced evolution of bacterial pathogenicity. In this study, we tested if Gram-negative Pseudomonas aeruginosa and Gram-positive Corynebacterium spp. can associate/invade and survive inside Acanthamoeba castellanii trophozoites and cysts, as well as non-phagocytic human brain microvascular endothelial cells. The results revealed that both Corynebacterium spp. and P. aeruginosa were able to associate as well as invade and/or taken up by the phagocytic A. castellanii trophozoite. In contrast, P. aeruginosa exhibited higher association as well as invasion of non-phagocytic HBMEC compared with Corynebacterium spp. Notably, P. aeruginosa remained viable during the encystment process and exhibited higher levels of recovery from mature cysts (74.54 bacteria per amoebae) compared with Corynebacterium spp. (2.69 bacteria per amoeba) (P < 0.05). As Acanthamoeba cysts can be airborne, these findings suggest that Acanthamoeba is a potential vector in the transmission of P. aeruginosa to susceptible hosts. When bacterial-ridden amoebae were exposed to favourable (nutrient-rich) conditions, A. castellanii emerged as vegetative trophozoites and remained viable, and likewise viable P. aeruginosa were also observed but rarely any Corynebacterium spp. were observed. Correspondingly, P. aeruginosa but not Corynebacterium spp. exhibited higher cytotoxicity to non-phagocytic HBMEC, producing more than 75 % cell death in 24 h, compared to 20 % cell death observed with Corynebacterium spp. Additionally, it was observed that the bacterial conditioned medium had no negative effect on A. castellanii growth. Further characterization of amoebal and bacterial interactions will assist in identifying the role of Acanthamoeba in the transmission and evolution of pathogenic bacteria.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acanthamoeba, a unicellular protist pathogen, is widely dispersed in the environment. (Siddiqui and Khan 2012; Marciano-Cabral and Cabral 2003; Visvesvara et al. 2007). Being free-living, Acanthamoeba can withstand harsh environments. Acanthamoeba exists in two distinct forms: an active trophozoite form during which it reproduces and a dormant cyst form where it remains inactive with little metabolic activity, nonetheless remaining viable for years. Notably, Acanthamoeba harbours diverse microbial organisms including viruses, bacteria, yeast and protists, some of which are potential pathogens (Khan 2006). The precise nature of this symbiosis is unclear, but it is proposed that these interactions enable pathogenic microbes to endure hostile conditions, and this association may aid in their transmission to susceptible hosts in order to establish infection. For this reason, Acanthamoeba-bacteria interactions have gained substantial attention from the scientific and medical community, leading to speculations of employing novel anti-amoebic approaches in eradicating “superbugs” from the clinical setting. For example, Acanthamoeba has been found to co-occur with Mycobacterium spp. and other superbugs within the hospital environment (Ovrutsky et al. 2013; Siddiqui et al. 2013).
Pseudomonas aeruginosa is an opportunistic Gram-negative bacterium. It can result in lung infections in cystic fibrosis patients and may infect any part of the human body in immunosuppressed and hospitalized patients with cancer, transplantation and burns (Giamarellou 2000; Lyczak et al. 2000). P. aeruginosa can be found in a number of habitats, including soil, water, plant and animal surfaces, and decaying organic matter; however, the precise ecological niche of P. aeruginosa is not well understood (Ferguson et al. 2001). Corynebacterium spp. are Gram-positive bacteria and are widely distributed in nature mostly being innocuous (Collins et al. 2004). However, some are known to cause human disease. Corynebacterium diphtheriae, for example, is the pathogen responsible for diphtheria. Being co-inhabitants of soil, it is likely that both P. aeruginosa and Corynebacterium spp. interact with Acanthamoeba in the environment. In this regard, amoeba has been suggested as the “training ground” during evolution of bacterial pathogenicity (Molmeret et al. 2005). Thus, it is important to understand interactions of pathogenic bacteria with Acanthamoeba. Here, we studied P. aeruginosa and Corynebacterium spp. interactions with the environmental phagocyte, Acanthamoeba, while non-phagocytic brain microvascular endothelial cells (BMEC) were used as a control. The human BMEC used in this study are primary in nature as well as non-phagocytic offering a useful model for comparative study. Additionally, it was determined whether these bacteria can survive intracellular of Acanthamoeba castellanii cysts, a property that can allow bacterial viability in the environment in the face of harsh conditions and allow their transmission to the susceptible hosts.
Materials and methods
Cultures of A. castellanii
All chemicals were purchased from Sigma Laboratories (Poole, Dorset, England), unless otherwise stated. A clinical isolate of A. castellanii belonging to the T4 genotype, isolated from a keratitis patient (American Type Culture Collection, ATCC 50492), was used in the present study. Amoebae were grown without shaking in 15 mL of PYG medium [0.75 % (w/v) proteose peptone, 0.75 % (w/v) yeast extract and 1.5 % (w/v) glucose] in T-75 tissue culture flasks at 30 °C as previously described (Sissons et al. 2005). To obtain vegetative trophozoites, the media were refreshed 17–20 h prior to experimentation, which resulted in more than 95 % amoebae in the trophozoite forms.
Bacterial cultures and growth conditions
P. aeruginosa and Corynebacterium spp. were used in this study. P. aeruginosa is a clinical isolate from the Aga Khan University hospital, and Corynebacterium spp. are an environmental isolate as described previously (Siddiqui et al. 2013). All bacteria were grown aerobically in Luria-Bertani (LB) broth at 37 °C.
Human brain microvascular endothelial cell cultures
The primary human brain microvascular endothelial cells (HBMEC) were isolated from seizure patient who had undergone cerebral cortex resection as previously described (Stins et al. 1997). The HBMECs were grown in T-75 tissue culture flasks in RPMI-1640 containing 10 % heat-inactivated fetal bovine serum, 10 % Nu-serum, 2 mM glutamine, 1 mM Na-pyruvate, 100 U/mL penicillin, 100 μg/mL streptomycin, non-essential amino acids and vitamins as previously described (Alsam et al. 2003; Stins et al. 1997).
Cytotoxicity assays
For cytotoxicity assays, 5 × 105 HBMEC per well per 0.5 mL were cultured in 24-well plates and incubated at 37 °C in a 5 % CO2 incubator. Under these conditions, HBMEC formed complete monolayers within 48 h. P. aeruginosa and Corynebacterium spp. were grown in LB for overnight, and the optical density was adjusted to 0.22 absorbance at wavelength of 595 nm [equivalent to approximately 108 colony-forming units (c.f.u.)/mL]. Next, 10 μL containing 106 c.f.u. were transferred to 490 μL RPMI 1640 and inoculated in each well of a 24-well plate containing HBMEC monolayers. After 60 min of incubation, the monolayers were washed with PBS and incubated with gentamicin (100 μg/mL in RPMI-1640) for 60 min to kill extracellular bacteria. The wells were then washed twice with RPMI-1640, and plates were incubated at 37 °C in a 5 % CO2 incubator and monitored for monolayer disruptions over the period of 24 h. Next, the supernatants were collected and centrifuged at 13,000 × g for 5 min to remove cellular debris. Cytotoxic effects were determined by estimating the release of cytosolic lactate dehydrogenase in the medium (Cytotoxicity Detection kit; Roche Applied Sciences). The percent cytotoxicity was calculated as follows: % cytotoxicity = (sample value−control value) / (total LDH release−control value) × 100. Control values were obtained by incubating HBMEC monolayers with 500 μL RPMI-1640 alone, and total LDH was released from HBMEC by completely lysing them in 500 μL 1 % Triton X-100. The LDH release from Triton X-100-treated HBMEC was considered 100 % cell death, and bacterial-mediated cell death is expressed as the relative change.
Association assays
Assays were performed to determine if the bacterial strains associate with A. castellanii and HBMEC. For A. castellanii, amoebae were maintained in the trophozoite stage in tissue culture flasks in PYG medium. Upon confluency, the unbound amoebae were aspirated, and growing trophozoites were rinsed with phosphate buffer saline (PBS) pH 7.4. Next, 10 mL of PBS was added to the flask, and trophozoites were chilled on ice for 20 min and pelleted by centrifugation at 1,000 g for 5 min. The cell pellet was resuspended in 1 mL of PBS, and the number of amoebae was counted using a hemocytometer (106 cells). For bacteria, the optical density of cultures was adjusted to 0.22 at 595 nm [equivalent to approximately 108 colony-forming units (c.f.u.)/mL]. Bacteria (107 c.f.u) were incubated with A. castellanii (106 cells) at 30 °C for 1 h for association assays as previously described (Yousuf et al. 2013). Briefly, following 1 h of incubation, co-cultures of amoebae plus bacteria were centrifuged at 2,000 g for 2 min to limit non-associated bacterial pelleting. The supernatants were collected and plated on nutrient agar plats to determine the presence of non-associated bacteria. In contrast, the pellet was resuspended in 0.5 mL of PBS and vortexed by a brief pulse. This process was repeated three times. At the final wash, the discarded supernatant was also plated onto nutrient agar plates to determine bacterial presence. Notably, the first two washes revealed bacterial presence; however, the final wash did not reveal any bacterial presence. The amoebae were counted using a hemocytometer and then lysed by adding 0.5 % SDS for 10 min (this concentration lysed amoebae trophozoites but did not affect the viability of amoeba cysts or the bacteria tested in this study). The lysates containing bacteria were serially diluted and plated on nutrient agar plates and colonies enumerated the next day. The bacterial colony-forming units associated with A. castellanii were calculated as follows: recovered bacterial c.f.u. / number of A. castellanii = bacterial c.f.u./A. castellanii ratio.
To study bacterial interactions with human cells, HBMEC were grown to confluent monolayers in 24-well plates. Next, bacteria were incubated with HBMECs (107 c.f.u. per well in 0.5 mL) as described above and plates incubated at 37 °C in a 5 % CO2 incubator. After 60 min of incubation, the monolayers were washed with PBS, and HBMEC were lysed by adding 500 μL of distilled water for 30 min together with gentle scraping of the well. The lysates were serially diluted and plated on nutrient agar plates and the colonies enumerated the next day.
Invasion assays
Assays were performed to determine if the bacterial strains are taken up by A. castellanii and HBMEC. Briefly, amoebae were incubated with bacterial strains as described for association assays. After washing with PBS thrice, the extracellular bacteria were killed by adding gentamicin (100 μg/mL in PBS for 90 min at 37 °C in a 5 % CO2 incubator). Finally, amoebae and bacteria were enumerated as described above. The bacterial colony-forming units invading A. castellanii were calculated as follows: recovered bacterial c.f.u. / number of A. castellanii = bacterial c.f.u./A. castellanii ratio. For HBMEC, bacteria were incubated with HBMEC. After 60 min of incubation, the monolayers were washed with PBS and incubated with gentamicin (100 μg/mL in RPMI-1640) for 60 min to kill extracellular bacteria. The wells were then washed twice with RPMI-1640, and HBMEC lysed and bacterial c.f.u. were determined as described above.
Intracellular cysts survival assays
Intracellular cyst survival assays were performed to evaluate the ability of bacterial strains to survive inside A. castellanii cysts as described previously (Yousuf et al. 2013). In brief, following invasion assays, the mixtures were transferred onto non-nutrient agar plates [prepared using 3 % (w/v) purified agar]. The plates were incubated at 30 °C for up to 10 days. This allowed complete encystment of A. castellanii trophozoites into the cyst form, as observed visually under a phase-contrast microscope. Cysts were then gently scraped off the agar surface using a cell scraper by adding 5 mL of dH2O and collected by centrifugation at 2,000 g for 10 min and resuspended in 0.5 mL of PBS and counted using a hemocytometer. The cysts were treated with SDS (0.5 % final concentration), and the bacterial colony-forming units were determined by plating on nutrient agar plates. The bacterial colony-forming units surviving intracellular of A. castellanii cysts were calculated as follows: recovered bacterial c.f.u. / number of A. castellanii = bacterial c.f.u./A. castellanii ratio.
Intracellular HBMEC survival assays
Assays were performed to determine if the bacterial strains survive intracellular of HBMEC. Briefly, following invasion assays, the monolayers were washed twice with RPMI-1640, and HBMEC were incubated in 0.5 mL of RPMI-1640 for 24 h at 37 °C in a 5 % CO2 incubator. Next, HBMEC were lysed by adding 500 of distilled water for 30 min together with gentle scraping of the well. The lysates were serially diluted and plated on nutrient agar plates, and the colonies enumerated the next day and bacterial c.f.u. were determined as described above.
Effect of favourable (nutrient-rich) and unfavourable conditions (nutrient-deprivation) on excystation of A. castellanii and bacterial growth
Following invasion assays, A. castellanii plus intracellular bacterial mixtures were transferred onto non-nutrient agar plates (prepared using 3 % (w/v) purified agar). The plates were incubated at room temperature for up to 10 days. This allowed complete encystment of A. castellanii trophozoites into the cyst form; this was confirmed visually under a phase-contrast microscope. Cysts were then gently scraped off the agar surface using a cell scraper by adding 5 mL of dH2O and collected by centrifugation at 2,000 g for 10 min and resuspended in 0.5 mL of PBS and counted using a hemocytometer. The scraped cysts were inoculated in different conditions: including PYG medium, LB medium, PBS and dH2O and incubated at 30 °C for 72 h and observed under a phase-contrast microscope for effects on growth of both A. castellanii and bacteria.
Effect of P. aeruginosa and Corynebacterium spp. conditioned medium on the viability of A. castellanii
Assays were performed to evaluate the effect of bacterial conditioned medium on A. castellanii trophozoites. Bacterial conditioned media (CM) was prepared by inoculating P. aeruginosa and Corynebacterium spp. in RPMI-1640 medium overnight. The cell-free supernatant (i.e., CM) was collected by centrifugation at 13,000 × g for 5 min and incubated with A. castellanii trophozoites (106 cells) at 30 °C for 2 h and 24 h. Following this, the mixtures were transferred onto plates containing PYG medium and growth were observed visually under a phase-contrast microscope at 24 h. For controls, A. castellanii (106 cells) were incubated with RPMI-1640 medium alone for 2 and 24 h and then incubated in PYG.
Results
Bacterial association with A. castellanii and HBMEC
To determine whether P. aeruginosa and Corynebacterium spp. associate with A. castellanii and HBMEC, association assays were performed. The findings revealed that both P. aeruginosa and Corynebacterium spp. exhibited association with A. castellanii (9.27 bacteria per amoeba ratio for P. aeruginosa and 45.3 bacteria per amoeba ratio for Corynebacterium spp. respectively (Fig. 1a), albeit Corynebacterium spp. exhibited higher association compared with P. aeruginosa (P < 0.05, using two-sample t test; two-tailed distribution). Here, the term association represents bacteria both inside amoebae and those that were attached on the surface of A. castellanii. In contrast, P. aeruginosa exhibited higher association with non-phagocytic HBMEC compared with Corynebacterium spp. (P < 0.05, using two-sample t test; two-tailed distribution) (Fig. 1b).
P. aeruginosa and Corynebacterium were incubated with Acanthamoeba and HBMEC for 1 h. The unbound bacteria were removed by washing and associated bacteria enumerated as described in “Materials and Methods”. a represents ratio of bacteria per amoeba, while b represents the number of bacteria associated with HBMEC (percent of the original inoculum). The results are the mean of three independent experiments performed in duplicate. Error bars represent standard error
Bacterial invasion/uptake by A. castellanii and HBMEC
Next, to determine whether P. aeruginosa and Corynebacterium spp. invade/taken up by A. castellanii and HBMEC, invasion assays were performed and the intracellular bacteria were determined. The results showed that P. aeruginosa exhibited invasion/uptake by A. castellanii (3.55 bacteria/amoeba ratio) (Fig. 2a). Similarly, Corynebacterium spp. exhibited invasion/uptake by A. castellanii at levels similar to P. aeruginosa (3.39 bacteria/amoeba ratio) (Fig. 2a). Of note, the PBS post-gentamicin wash, plated onto nutrient agar plates, did not yield any bacterial c.f.u, confirming that the antibiotic treatment was effective. In contrast, P. aeruginosa exhibited higher invasion of HBMEC compared with Corynebacterium spp. (P < 0.05, using two-sample t test; two-tailed distribution) (Fig. 2b).
A. castellanii and/or HBMEC were incubated with P. aeruginosa and Corynebacterium for 1 h, after which gentamicin was added to kill the extracellular bacteria, following which amoebae and intracellular bacteria were enumerated as described in “Materials and methods.” a Represents ratio of bacteria per amoeba, while b represents the number of bacteria invading HBMEC (percent of the original inoculum). The results are the mean of three independent experiments performed in duplicate. Error bars represent standard error
Bacterial survival of A. castellanii encystment process
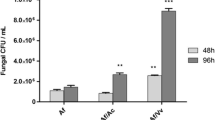
The viability of P. aeruginosa and Corynebacterium spp., inside A. castellanii during encystment and recovery from mature cysts, was determined by performing intracellular cyst survival assays. The SDS treatment affected cyst viability (no growth observed in PYG) through lysing the ostiole membrane and leading to the recovery of any intracellular bacteria. The results revealed that both P. aeruginosa and Corynebacterium spp. remained viable during encystment, albeit P. aeruginosa exhibited significantly higher levels of recovery from mature cysts (74.54 bacteria per amoebae ratio) compared with Corynebacterium spp. (2.69 bacteria per amoeba ratio) (P < 0.05, using two-sample t test; two-tailed distribution) (Fig. 3a).
a A. castellanii were incubated with each, P. aeruginosa and Corynebacterium for 1 h, followed by the addition of gentamicin to kill the extracellular bacteria. Finally, A. castellanii plus intracellular bacteria were inoculated onto non-nutrient agar plates for several days, followed by amoebae counting. The bacterial counts intracellular of cysts were calculated as described in “Materials and methods.” The results are the mean of three independent experiments performed in duplicate. Error bars represent standard error. b HBMEC were incubated with each, P. aeruginosa and Corynebacterium for 1 h, followed by the addition of gentamicin to kill the extracellular bacteria and plates that were incubated for 24 h, followed by counting of intracellular bacteria as described in “Materials and methods.” The results are presented as the mean ± standard error of three individual experiments performed in duplicate
For HBMEC, the results revealed that P. aeruginosa increased in number exponentially (Fig. 3b) and HBMEC monolayers were completely destroyed. In contrast, Corynebacterium spp. showed no damage to HBMEC as evident by intact monolayers and minimal bacterial recovery compared with P. aeruginosa (P < 0.05, using two-sample t test; two-tailed distribution) (Fig. 3b). This was further confirmed using cytotoxicity assays, which revealed that P. aeruginosa exhibited significantly higher HBMEC cytotoxicity compared with Corynebacterium spp. (P < 0.05) (Fig. 4).
HBMECs were incubated with each P. aeruginosa and Corynebacterium for 1 h, followed by gentamicin treatment as described in Fig. 2. Next, plates were incubated for 24 h at 37 °C in a 5 % CO2 incubator, followed by the determination of cytotoxic effect of bacteria on HBMEC. The LDH release from 1 % Triton X-100-treated HBMEC was considered 100 % cell death, and bacterial-mediated cell death is expressed as the relative change. The results are the mean of three independent experiments performed in duplicate. Error bars represent standard error
A. castellanii and P. aeruginosa exhibited growth when bacterial-ridden amoebae cysts were exposed to favourable conditions (nutrient-rich)
Following survival assays, the mature cysts containing intracellular bacteria were inoculated in different conditions: PYG growth medium, LB growth medium, PBS and dH2O. The results revealed that in all the nutrient conditions tested, A. castellanii trophozoites emerged and remained viable, when observed for up to 72 h, along with fewer numbers of P. aeruginosa, but Corynebacterium spp. were rarely observed (Table 1). For either PYG or LB, A. castellanii trophozoites emerged from bacterial-ridden cysts along with few P. aeruginosa were observed. However, when incubated with PBS or dH2O; A. castellanii remained in the cyst form (Table 1). Of note, at all nutrient conditions tested, P. aeruginosa were unable to lyse or overgrow A. castellanii and vice versa.
Bacterial conditioned medium did not affect A. castellanii growth
Assays were performed to determine the effect of bacterial conditioned medium on A. castellanii growth. Bacterial conditioned media (CM) was inoculated with A. castellanii trophozoites. Following this, the mixtures were transferred to PYG medium, and growth was observed visually under a phase-contrast microscope for 24 h. The findings revealed that the presence of CM did not affect A. castellanii growth as viable amoebae were observed at all-time points tested and at numbers approximately similar to PYG alone.
Discussion
Acanthamoeba acts as a host for a variety of microbes, including viruses, bacteria, protists and yeast/fungi (reviewed in Khan 2009; La Scola et al. 2001, 2003). For this reason, Acanthamoeba are receiving profuse attention from the scientific and medical world due to their ability to act as bacterial predators, as bacterial transmission vehicles or a Trojan horse, and notably as biological reservoirs. The ability of amoebae to host bacteria may enhance bacterial infectivity for mammalian cells, thus increasing their transmission to susceptible hosts, as well as enhancing the pathogenicity of the host amoebae; however, the underlying mechanisms remain incompletely understood (Khan 2009; La Scola et al. 2001, 2003; Molmeret et al. 2005; Greub and Raoult 2004). Also, Acanthamoeba shares remarkable similarities with macrophages in their phagocytic properties, and it is considered as an environmental phagocyte (Khan 2009). Here, we determined Corynebacterium spp. and P. aeruginosa interactions with non-phagocytic HBMEC and phagocytic A. castellanii.
It was interesting to note that both Corynebacterium spp. and P. aeruginosa associated and invaded/taken up by A. castellanii, but only P. aeruginosa showed higher association and/or invasion of HBMEC. These findings suggest that Corynebacterium spp. are weakly pathogenic and are likely taken up by amoeba but unable to invade HBMEC. This is consistent with our findings of cyst survival assays which revealed that Corynebacterium spp. exhibited reduced recovery from mature A. castellanii cysts compared with P. aeruginosa. Amoebae take up bacteria; however, it is not clear whether they are being used as food source. The fact that at least some bacteria are being recovered from cysts suggests that they are able to avoid complete killing by amoeba. Perhaps, this explains the difference between pathogenic and/or weak-pathogenic bacteria who avoid killing, while non-pathogenic bacteria are eaten up by amoeba (Siddiqui et al. 2013; Yousuf et al. 2013). This was confirmed by plating amoeba on non-nutrient agar plates without any food and left for 10 days. During this time, any remaining food bacteria will be eaten up and only the pathogenic ones would be able to remain viable. Overall, these findings suggest that A. castellanii cysts act as a reservoir for P. aeruginosa and may aid in their transmission to the susceptible hosts, while Corynebacterium spp. are weak-pathogenic. These findings corroborate with Ott et al. (2012) who showed that A. polyphaga use Corynebacterium spp. as food source. Notably, our findings showed that P. aeruginosa exhibited higher levels of recovery from mature cysts as compared to A. castellanii trophozoite post-invasion counts suggesting that P. aeruginosa are able to resist amoebal grazing and multiply within A. castellanii cysts. Based on these findings, it is tempting to speculate that Acanthamoeba and P. aeruginosa are involved in convoluted interactions and suggest their long co-evolutionary history combined with a series of adjustments (including lateral gene transfers) ensuring bacterial survival and that grazing resistance that may have influenced evolutionary gain of P. aeruginosa pathogenicity and this will be the subject of future studies. This is strengthened with the fact that Acanthamoeba and P. aeruginosa are often isolated as co-inhabitants from eyewash stations, drinking water system of hospitals, contact lens cases, biofilms, etc. (Paszko-Kolva et al. 1991; Michel et al. 1995; Greub and Raoult 2004; La Scola et al. 2003). The evolution of one species to house inside another species is a remarkable adaptation and consistent with the fundamental principle of natural selection to favour cooperation. Based on this property, Acanthamoeba has often been described as the training ground to learn to evade immune attack (Molmeret et al. 2005). In particular, the ability of bacteria to survive the encystment process may be a useful indicator for bacterial pathogenicity and may aid in the differentiation of pathogenic bacterial species. For example, our previous studies showed that neuropathogenic E. coli K1 showed higher recovery from mature cysts but not non-pathogenic K-12 (Jung et al. 2007). Likewise, P. aeruginosa (clinical isolate) exhibited higher recovery from mature cysts compared with Corynebacterium spp. (environmental isolate). However, this proposal can only be tested for bacterial genus that interact with Acanthamoeba.
One of the interesting findings observed in this study was the inability of P. aeruginosa to inhibit the growth of A. castellanii, even under favourable conditions. Similarly, P. aeruginosa conditioned medium had no negative effect on A. castellanii growth. This is in contrast to previous studies which showed that P. aeruginosa affected A. castellanii viability and inhibited growth in a type III secretion system-dependent manner and due to P. aeruginosa toxin L-2-amino-4-methoxy-trans-3-butenoic (Wang and Ahearn 1997; Abd et al. 2008; Lee et al. 2012). There are several explanations for these contrasting results, different strains of A. castellanii and P. aeruginosa used; the strain of A. castellanii used in the present study is a clinical isolate belonging to T4 genotype, isolated from a keratitis patient compared with the strain used in the study by Abd et al. (2008) that was derived from a yeast culture, while Lee et al. (2012) used a soil isolate of A. castellanii. Alternatively, assay conditions (24 h co-incubation in our assays versus 7 days co-incubation in previous studies) may explain these differences.
Overall, these results showed that bacteria that were highly pathogenic to HBMEC resisted amoebal grazing and survived encystment process with higher yield from mature cysts, compared with bacteria that were weakly pathogenic to HBMEC. Pathogenic bacteria tested have the potential to exploit amoebae cysts as biological vectors; however, the molecular mechanisms of bacterial localization within amoebae, evasion of phago-lysosome processes and inability of amoeba to expel bacteria during encystment remain unclear. Of note, recent studies showed the presence of a diffusible factor produced by amoebae, mediating survival and replication of B. cepacia and V. parahaemolyticus (Marolda et al. 1999; Laskowski-Arce and Orth 2008), which may explain our findings. Overall, Acanthamoeba acts as an environmental sanctuary for bacterial pathogens, and perhaps facilitating genetic exchanges affecting their virulence, and contributes to microbial survival in harsh environmental conditions along with aiding their transmission to susceptible hosts that is of immense concern for human and animal health. Interaction studies will help to identify the role of Acanthamoeba in the evolution of superbugs and in turn expedite discovery of novel therapeutic and/or preventative measures.
References
Abd H, Wretlind B, Saeed A, Idsund E, Hultenby K, Sandström G (2008) Pseudomonas aeruginosa utilises its type III secretion system to kill the free-living amoeba Acanthamoeba castellanii. J Eukaryot Microbiol 55(3):235–243
Alsam S, Kim KS, Stins M, Rivas AO, Sissons J, Khan NA (2003) Acanthamoeba interactions with human brain microvascular endothelial cells. Microb Pathogen 35:235–241
Collins MD, Hoyles L, Foster G, Falsen E (2004) Corynebacterium caspium sp. nov., from a Caspian seal (Phoca caspica). Int J Syst Evol Microbiol 54:925–928
Ferguson MW, Maxwell JA, Vincent TS, da Silva J, Olson JC (2001) Comparison of the exoS gene and protein expression in soil and clinical isolates of Pseudomonas aeruginosa. Infect Immun 69(4):2198–2210
Giamarellou H (2000) Therapeutic guidelines for Pseudomonas aeruginosa infections. Int J Antimicrob Agents 16:103–106
Greub G, Raoult D (2004) Microorganisms resistant to free-living amoebae. Clin Microbiol Rev 17(2):413–433
Jung S, Matin A, Kim KS, Khan NA (2007). The capsule plays an important role in Escherichia coli K1 interactions with Acanthamoeba. Int J Parasitol 37:417–423
Khan NA (2006) Acanthamoeba: biology and increasing importance in human health. FEMS Microbiol Rev 30(4):564–595
Khan NA (2009) Acanthamoeba: biology and pathogenesis. Caister Academic Press, Linton, Cambs, UK, 290pp. ISBN: 978-1-904455-43-1
La Scola B, Mezi L, Weiller PJ, Raoult D (2001) Isolation of Legionella anisa using an amoebic coculture procedure. J Clin Microbiol 39(1):365–366
La Scola B, Boyadjiev I, Greub G, Khamis A, Martin C, Raoult D (2003) Amoeba-resisting bacteria and ventilator-associated pneumonia. Emerg Infect Dis 9(7):815–821
Laskowski-Arce MA, Orth K (2008) Acanthamoeba castellanii promotes the survival of Vibrio parahaemolyticus. Appl Environ Microbiol 74:7183–7188
Lee X, Reimmann C, Greub G, Sufrin J, Croxatto A (2012) The Pseudomonas aeruginosa toxin L-2-amino-4-methoxy-trans-3-butenoic acid inhibits growth and induces encystment in Acanthamoeba castellanii. Microbes Infect 14(3):268–272
Lyczak JB, Cannon CL, Pier GB (2000) Establishment of Pseudomonas aeruginosa infection: lessons from a versatile opportunist. Microbes Infect 2:1051–1060
Marciano-Cabral F, Cabral G (2003) Acanthamoeba spp. as agents of disease in humans. Clin Microbiol Rev 16:273–307
Marolda CL, Hauröder B, John MA, Michel R, Valvano MA (1999) Intracellular survival and saprophytic growth of isolates from the Burkholderiacepacia complex in free-living amoebae. Microbiol 145:1509–1517
Michel R, Burghardt H, Bergmann H (1995) Acanthamoeba, naturally intracellularly infected with Pseudomonas aeruginosa, after their isolation from a microbiologically contaminated drinking water system in a hospital. Zentralbl Hyg Umweltmed 196(6):532–544
Molmeret M, Horn M, Wagner M, Santic M, Abu Kwaik Y (2005) Amoebae as training grounds for intracellular bacterial pathogens. Appl Environ Microbiol 71:20–28
Ott L, McKenzie A, Baltazar MT, Britting S, Bischof A, Burkovski A, Hoskisson PA (2012) Evaluation of invertebrate infection models for pathogenic Corynebacteria. FEMS Immunol Med Microbiol 65(3):413–421
Ovrutsky AR, Chan ED, Kartalija M, Bai X, Jackson M, Gibbs S, Falkinham JO 3rd, Iseman MD, Reynolds PR, McDonnell G, Thomas V (2013) Cooccurrence of free-living amoebae and nontuberculous Mycobacteria in hospital water networks, and preferential growth of Mycobacterium avium in Acanthamoeba lenticulata. Appl Environ Microbiol 79(10):3185–3192
Paszko-Kolva C, Yamamoto H, Shahamat M, Sawyer TK, Morris G, Colwell RR (1991) Isolation of amoebae and Pseudomonas and Legionella spp. from eyewash stations. Appl Environ Microbiol 57(1):163–167
Siddiqui R, Khan NA (2012) Biology and pathogenesis of Acanthamoeba. Parasit Vect 5:6
Siddiqui R, Sagheer M, Khan NA (2013) Prevalence of Acanthamoeba and superbugs in a clinical setting: coincidence or hyperparasitism. Parasitol Res 112:1349–1351
Sissons J, Kim KS, Stins M, Jayasekera S, Alsam S, Khan NA (2005) Acanthamoeba castellanii induces host cell death via a phosphatidylinositol 3-kinase-dependent mechanism. Infect Immun 73:2704–2708
Stins MF, Gilles F, Kim KS (1997) Selective expression of adhesion molecules on human brain microvascular endothelial cells. J Neuroimmunol 76:81–90
Visvesvara GS, Moura H, Schuster FL (2007) Pathogenic and opportunistic free-living amoebae: Acanthamoeba spp., Balamuthia mandrillaris, Naegleria fowleri, and Sappinia diploidea. FEMS Immunol Med Microbiol 50:1–26
Wang X, Ahearn DG (1997) Effect of bacteria on survival and growth of Acanthamoeba castellanii. Curr Microbiol 34:212–215
Yousuf FA, Siddiqui R, Khan NA (2013) Acanthamoeba castellanii is a potential environmental host for Enterobacter aerogenes and Aeromonas hydrophila. Parasit Vect 6:169
Acknowledgments
The authors are grateful for the kind support provided by The Aga Khan University, Pakistan.
Conflict of interest
None to declare.
Author information
Authors and Affiliations
Corresponding author
Additional information
Naveed Khan holds a BSc, MSc, PhD., Aga Khan University.
Rights and permissions
About this article
Cite this article
Siddiqui, R., Lakhundi, S. & Khan, N.A. Interactions of Pseudomonas aeruginosa and Corynebacterium spp. with non-phagocytic brain microvascular endothelial cells and phagocytic Acanthamoeba castellanii . Parasitol Res 114, 2349–2356 (2015). https://doi.org/10.1007/s00436-015-4432-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-015-4432-0