Abstract
Purpose
Uterine cancer risk is high in breast cancer survivors. Although breast cancer and uterine cancer share some common epidemiological risk factors, association of metabolic syndrome with incident uterine cancer in breast cancer survivors is under-studied. We evaluated the association of metabolic syndrome conditions with second primary uterine cancer in breast cancer survivors.
Methods
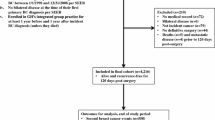
In this retrospective cohort study, 37,303 breast cancer patients diagnosed between 2008 and 2020 at Kaiser Permanente Southern California, an integrated healthcare system, were included. Data on cancer-related variables, sociodemographic, and clinical variables were extracted from KPSC’s Surveillance, Epidemiology, and End Results (SEER)-affiliated cancer registry and electronic health records, as appropriate. Patients were followed from breast cancer diagnosis until 12/31/2021 for incident uterine cancer. Proportional hazards regression was used to report association [HR (95% CI)] between metabolic conditions and uterine cancer.
Results
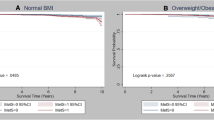
More than half (53.1%) of the breast cancer survivors had 1–2 metabolic conditions; 19.4% had 3 + , while 27. 5% had no metabolic conditions. Median time to follow-up was 5.33 years and 185 (0.5%) patients developed second primary uterine cancer. Obesity was associated with an elevated uterine cancer risk in the adjusted model [HR (95% CI) 1.64 (1.20–2.25)]. Having 1–2 metabolic conditions (versus none) was not associated with increased uterine cancer risk [adjusted HR (95% CI) 1.24 (0.85–1.82)]; however, there was an increased uterine cancer risk with 3 + metabolic conditions [adjusted HR (95% CI) 1.82 (1.16–2.87)].
Conclusion
Although not statistically significant, we found a trend demonstrating greater uterine cancer risk by increasing numbers of metabolic syndrome conditions in breast cancer survivors.

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Arteaga DP, DeKraker C, Ennis M, Dewey N, Goebel EA, Welch S, Pimentel I, Ippolito JE, Lohmann AE (2023) Body composition and endometrial cancer outcomes. J Natl Cancer Inst Monogr 2023(61):49–55. https://doi.org/10.1093/jncimonographs/lgad012
Arthur RS, Kabat GC, Kim MY, Wild RA, Shadyab AH, Wactawski-Wende J, Ho GYF, Reeves KW, Kuller LH, Luo J, Beebe-Dimmer J, Simon MS, Strickler H, Wassertheil-Smoller S, Rohan TE (2019) Metabolic syndrome and risk of endometrial cancer in postmenopausal women: a prospective study. Cancer Causes Control 30(4):355–363. https://doi.org/10.1007/s10552-019-01139-5
Bergman L, Beelen ML, Gallee MP, Hollema H, Benraadt J, van Leeuwen FE (2000) Risk and prognosis of endometrial cancer after tamoxifen for breast cancer Comprehensive Cancer. Centres’ ALERT Group. Assessment of Liver and Endometrial cancer Risk following Tamoxifen. Lancet 356(9233):881–887. https://doi.org/10.1016/s0140-6736(00)02677-5
Chlebowski RT, Schottinger JE, Shi J, Chung J, Haque R (2015) Aromatase inhibitors, tamoxifen, and endometrial cancer in breast cancer survivors. Cancer 121(13):2147–2155. https://doi.org/10.1002/cncr.29332
Corso G, Veronesi P, Santomauro GI, Maisonneuve P, Morigi C, Peruzzotti G, Intra M, Sacchini V, Galimberti V (2018) Multiple primary non-breast tumors in breast cancer survivors. J Cancer Res Clin Oncol 144(5):979–986. https://doi.org/10.1007/s00432-018-2621-9
Cust AE, Kaaks R, Friedenreich C, Bonnet F, Laville M, Tjonneland A, Olsen A, Overvad K, Jakobsen MU, Chajes V, Clavel-Chapelon F, Boutron-Ruault MC, Linseisen J, Lukanova A, Boeing H, Pischon T, Trichopoulou A, Christina B, Trichopoulos D, Riboli E (2007) Metabolic syndrome, plasma lipid, lipoprotein and glucose levels, and endometrial cancer risk in the European Prospective Investigation into Cancer and Nutrition (EPIC). Endocr Relat Cancer 14(3):755–767. https://doi.org/10.1677/ERC-07-0132
Deng Z, Jones MR, Wang MC, Visvanathan K (2022) Mortality after second malignancy in breast cancer survivors compared to a first primary cancer: a nationwide longitudinal cohort study. NPJ Breast Cancer 8(1):82. https://doi.org/10.1038/s41523-022-00447-5
Esposito K, Chiodini P, Capuano A, Bellastella G, Maiorino MI, Rafaniello C, Giugliano D (2013) Metabolic syndrome and postmenopausal breast cancer: systematic review and meta-analysis. Menopause 20(12):1301–1309. https://doi.org/10.1097/GME.0b013e31828ce95d
Esposito K, Chiodini P, Colao A, Lenzi A, Giugliano D (2012) Metabolic syndrome and risk of cancer: a systematic review and meta-analysis. Diabetes Care 35(11):2402–2411. https://doi.org/10.2337/dc12-0336
Huang PL (2009) A comprehensive definition for metabolic syndrome. Dis Model Mech 2(5–6):231–237. https://doi.org/10.1242/dmm.001180
Kitson SJ, Lindsay J, Sivalingam VN, Rutter MK, Crosbie EJ (2018) High prevalence of metabolic syndrome in women newly diagnosed with endometrial cancer. Gynecol Oncol Rep 26:109–110. https://doi.org/10.1016/j.gore.2018.08.006
Lee DY, Lee TS (2020) Associations between metabolic syndrome and gynecologic cancer. Obstet Gynecol Sci 63(3):215–224. https://doi.org/10.5468/ogs.2020.63.3.215
Liu J, Jiang W, Mao K, An Y, Su F, Kim BY, Liu Q, Jacobs LK (2015) Elevated risks of subsequent endometrial cancer development among breast cancer survivors with different hormone receptor status: a SEER analysis. Breast Cancer Res Treat 150(2):439–445. https://doi.org/10.1007/s10549-015-3315-5
Morice P, Leary A, Creutzberg C, Abu-Rustum N, Darai E (2016) Endometrial cancer. Lancet 387(10023):1094–1108. https://doi.org/10.1016/S0140-6736(15)00130-0
Reeves, G. K., Pirie, K., Beral, V., Green, J., Spencer, E., Bull, D., & Million Women Study, C (2007) Cancer incidence and mortality in relation to body mass index in the Million******* Women Study: cohort study. BMJ 335(7630):1134. https://doi.org/10.1136/bmj.39367.495995.AE
Sung H, Freedman RA, Siegel RL, Hyun N, DeSantis CE, Ruddy KJ, Jemal A (2021) Risks of subsequent primary cancers among breast cancer survivors according to hormone receptor status. Cancer 127(18):3310–3324. https://doi.org/10.1002/cncr.33602
Trabert B, Wentzensen N, Felix AS, Yang HP, Sherman ME, Brinton LA (2015) Metabolic syndrome and risk of endometrial cancer in the United States: a study in the SEER-medicare linked database. Cancer Epidemiol Biomarkers Prev 24(1):261–267. https://doi.org/10.1158/1055-9965.EPI-14-0923
Wijayabahu AT, Egan KM, Yaghjyan L (2020) Uterine cancer in breast cancer survivors: a systematic review. Breast Cancer Res Treat 180(1):1–19. https://doi.org/10.1007/s10549-019-05516-1
Yang X, Wang J (2019) The role of metabolic syndrome in endometrial cancer: a review. Front Oncol 9:744. https://doi.org/10.3389/fonc.2019.00744
Acknowledgements
The authors thank all patients included in the study.
Funding
This study was supported by National Institutes of Health (NIH)/National Heart, Lung, and Blood Institute (NHLBI) grant number R01HL154319 (Drs. Haque and Potosky).
Author information
Authors and Affiliations
Contributions
Amrita Mukherjee, Lie Hong Chen, and Reina Haque contributed to the study conception and design. Material preparation and data collection were performed by Lie Hong Chen and Zheng Gu. Formal analysis was done by Amrita Mukherjee. The first draft of the manuscript was written by Amrita Mukherjee. All the authors revised the first draft and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
This study was supported by NIH/NHLBI grant number R01HL154319 (Drs. Haque and Potosky). The contents do not represent the view of the NIH/NHLBI. The authors declare no other financial interests/personal relationships which may be considered as potential competing interests.
Ethics approval
The study was approved by the KPSC Institutional Review Board (IRB).
Consent to participate
Due to use of data collected as part of routine care, requirement of verbal or written informed consent was waived by the IRB.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mukherjee, A., Gu, Z., Chen, L.H. et al. Association of metabolic syndrome conditions with risk of second primary uterine cancer in breast cancer survivors. J Cancer Res Clin Oncol 149, 17749–17755 (2023). https://doi.org/10.1007/s00432-023-05489-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05489-1