Abstract
Background
Delivering stereotactic ablative radiotherapy (SABR) in patients with multiple oligometastases represents a challenge for clinical and technical reasons. We aimed to evaluate the outcome of patients affected by multiple oligometastases treated with SABR and the impact of tumor volume on survival.
Materials and methods
We included all the patients treated with single course SABR for 3 to 5 extracranial oligometastases. All patients were treated with the volumetric modulated arc therapy (VMAT) technique with ablative intent. End-points of the analysis were overall survival (OS), progression free survival (PFS), local control (LC) and toxicity.
Results
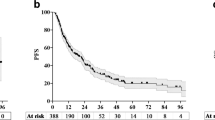
136 patients were treated from 2012 to 2020 on 451 oligometastases. Most common primary tumor was colorectal cancer (44.1%) followed by lung cancer (11.8%). A total of 3, 4 and 5 lesions were simultaneously treated in 102 (75.0%), 26 (19.1%), and 8 (5.9%) patients, respectively. Median total tumor volume (TTV) was 19.1 cc (range 0.6–245.1). With a median follow-up of 25.0 months, OS at 1 and 3 years was 88.4% and 50.2%, respectively. Increasing TTV was independent predictive factor of worse OS (HR 2.37, 95% CI 1.18–4.78, p = 0.014) and PFS (HR 1.63, 95% CI 1.05–2.54; p = 0.028). Median OS was 80.6 months if tumor volume was ≤ 10 cc (1 and 3 years OS rate 93.6% and 77.5%, respectively), and 31.1 months if TTV was higher than 10 cc (1 and 3 years OS rate 86.7% and 42.3%, respectively). Rates of LC at 1 and 3 years were 89.3% and 76.5%. In terms of toxicity, no grade 3 or higher toxicity was reported both in the acute and late settings.
Conclusion
We demonstrated the impact of tumor volume on survival and disease control of patients affected by multiple oligometastases treated with single course SABR.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, CF, upon reasonable request.
References
Ashram S, Bahig H, Barry A, Blanchette D, Celinksi A, Chung P et al (2022) Planning trade-offs for SABR in patients with 4 to 10 metastases: a substudy of the SABR-COMET-10 randomized trial. Int J Radiat Oncol Biol Phys 114:1011–1015. https://doi.org/10.1016/j.ijrobp.2022.05.035
Baschnagel AM, Meyer KD, Chen PY, Krauss DJ, Olson RE, Pieper DR et al (2013) Tumor volume as a predictor of survival and local control in patients with brain metastases treated with Gamma Knife surgery. J Neurosurg 119:1139–1144. https://doi.org/10.3171/2013.7.JNS13431
Chalkidou A, Macmillan T, Grzeda MT, Peacock J, Summers J, Eddy S et al (2021) Stereotactic ablative body radiotherapy in patients with oligometastatic cancers: a prospective, registry-based, single-arm, observational, evaluation study. Lancet Oncol 22:98–106. https://doi.org/10.1016/S1470-2045(20)30537-4
Chmura S, Winter KA, Robinson C, Pisansky TM, Borges V, Al-Hallaq H et al (2021) Evaluation of safety of stereotactic body radiotherapy for the treatment of patients with multiple metastases. JAMA Oncol 7:845. https://doi.org/10.1001/jamaoncol.2021.0687
Decaestecker K, De Meerleer G, Lambert B, Delrue L, Fonteyne V, Claeys T et al (2014) Repeated stereotactic body radiotherapy for oligometastatic prostate cancer recurrence. Radiat Oncol 9:135. https://doi.org/10.1186/1748-717X-9-135
Franzese C, Comito T, Toska E, Tozzi A, Clerici E, De Rose F et al (2018) Predictive factors for survival of oligometastatic colorectal cancer treated with stereotactic body radiation therapy. Radiother Oncol. https://doi.org/10.1016/j.radonc.2018.10.024
Gomez DR, Blumenschein GR, Lee JJ, Hernandez M, Ye R, Camidge DR et al (2016) Local consolidative therapy versus maintenance therapy or observation for patients with oligometastatic non-small-cell lung cancer without progression after first-line systemic therapy: a multicentre, randomised, controlled, phase 2 study. Lancet Oncol 17:1672–1682. https://doi.org/10.1016/S1470-2045(16)30532-0
Gomez DR, Tang C, Zhang J, Blumenschein GR, Hernandez M, Jack Lee J et al (2019) Local consolidative therapy vs. maintenance therapy or observation for patients with oligometastatic non–small-cell lung cancer: long-term results of a multi-institutional, phase II, randomized study. J Clin Oncol 37:1558–1565. https://doi.org/10.1200/JCO.19.00201
Guckenberger M, Lievens Y, Bouma AB, Collette L, Dekker A, DeSouza NM et al (2020) Characterisation and classification of oligometastatic disease: a European society for radiotherapy and oncology and European organisation for research and treatment of cancer consensus recommendation. Lancet Oncol 21:e18-28. https://doi.org/10.1016/S1470-2045(19)30718-1
Hellman S, Weichselbaum RR (1995) Oligometastases. J Clin Oncol 13:8–10. https://doi.org/10.1200/jco.1995.13.1.8
Hirshman BR, Wilson BR, Ali MA, Schupper AJ, Proudfoot JA, Goetsch SJ et al (2018) Cumulative intracranial tumor volume augments the prognostic value of diagnosis-specific graded prognostic assessment model for survival in patients with melanoma cerebral metastases. Neurosurgery 83:237–244. https://doi.org/10.1093/neuros/nyx380
Iyengar P, Wardak Z, Gerber DE, Tumati V, Ahn C, Hughes RS et al (2018) Consolidative radiotherapy for limited metastatic non-small-cell lung cancer: a phase 2 randomized clinical trial. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2017.3501
Kim J, Chang JS, Sung W, Kim JS, Kim TH, Choi SH et al (2022) A comparison of 2 disease burden assessment methods (3D volume versus the number of lesions) for prognostication of survival in metastatic melanoma: implications for the characterization of oligometastatic disease. Int J Radiat Oncol Biol Phys 114:883–891. https://doi.org/10.1016/j.ijrobp.2022.08.040
Lewis SL, Porceddu S, Nakamura N, Palma DA, Lo SS, Hoskin P et al (2017) Definitive stereotactic body radiotherapy (SBRT) for extracranial oligometastases. Am J Clin Oncol 40:418–422. https://doi.org/10.1097/COC.0000000000000169
Lievens Y, Guckenberger M, Gomez D, Hoyer M, Iyengar P, Kindts I et al (2020) Defining oligometastatic disease from a radiation oncology perspective: an ESTRO-ASTRO consensus document. Radiother Oncol 148:157–166. https://doi.org/10.1016/j.radonc.2020.04.003
Meyer E, Pasquier D, Bernadou G, Calais G, Maroun P, Bossi A et al (2018) Stereotactic radiation therapy in the strategy of treatment of metastatic renal cell carcinoma: a study of the Getug group. Eur J Cancer 98:38–47. https://doi.org/10.1016/j.ejca.2018.04.008
Muldermans JL, Romak LB, Kwon ED, Park SS, Olivier KR (2016) Stereotactic body radiation therapy for oligometastatic prostate cancer. Int J Radiat Oncol Biol Phys 95:696–702. https://doi.org/10.1016/j.ijrobp.2016.01.032
Ost P, Reynders D, Decaestecker K, Fonteyne V, Lumen N, De Bruycker A et al (2017) Surveillance or metastasis-directed therapy for oligometastatic prostate cancer recurrence: a prospective, randomized, multicenter phase II trial. J Clin Oncol. https://doi.org/10.1200/JCO.2017.75.4853
Ouyang W, Yu J, Nuerjiang S, Li Z, Wang D, Wang X et al (2019) Stereotactic body radiotherapy improves the survival of patients with oligometastatic non-small cell lung cancer. Cancer Med 8:4605–4614. https://doi.org/10.1002/cam4.2366
Palma DA, Olson R, Harrow S, Correa RJM, Schneiders F, Haasbeek CJA et al (2019) Stereotactic ablative radiotherapy for the comprehensive treatment of 4–10 oligometastatic tumors (SABR-COMET-10): study protocol for a randomized phase III trial. BMC Cancer 19:816. https://doi.org/10.1186/s12885-019-5977-6
Palma DA, Olson R, Harrow S, Gaede S, Louie AV, Haasbeek C et al (2020) Stereotactic ablative radiotherapy for the comprehensive treatment of oligometastatic cancers: long-term results of the SABR-COMET phase II randomized trial. J Clin Oncol. https://doi.org/10.1200/JCO.20.00818
Park C, Papiez LZS et al (2008) Universal survival curve and single fraction equivalent dose: useful tools in understanding potency of ablative radiotherapy: in regard to Parks et al. (Int J Radiat Oncol Biol Phys 2008;70:847–852). Int J Radiat Oncol Biol Phys 70:847–852. https://doi.org/10.1016/j.ijrobp.2008.08.032
Phillips R, Shi WY, Deek M, Radwan N, Lim SJ, Antonarakis ES et al (2020) Outcomes of observation vs stereotactic ablative radiation for oligometastatic prostate cancer: the ORIOLE phase 2 randomized clinical trial. JAMA Oncol 6:650–659. https://doi.org/10.1001/jamaoncol.2020.0147
Ruers T, van Coevorden F, Punt CJA, Pierie J-PEN, Borel-Rinkes I, Ledermann JA et al (2017) Local treatment of unresectable colorectal liver metastases: results of a randomized phase II trial. JNCI. https://doi.org/10.1093/jnci/djx015
Yamamoto M, Serizawa T, Shuto T, Akabane A, Higuchi Y, Kawagishi J et al (2014) Stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901): a multi-institutional prospective observational study. Lancet Oncol 15:387–395. https://doi.org/10.1016/S1470-2045(14)70061-0
Yamamoto T, Niibe Y, Aoki M, Shintani T, Yamada K, Kobayashi M et al (2020) Analyses of the local control of pulmonary oligometastases after stereotactic body radiotherapy and the impact of local control on survival. BMC Cancer 20:997. https://doi.org/10.1186/s12885-020-07514-9
Funding
No fundings were used for the present study.
Author information
Authors and Affiliations
Contributions
CF: conceptualization, roles/writing—original draft; VV: data curation; DF: data curation; TC: supervision; PN: supervision; EC: data curation; MAT: data curation; MM: data curation; LC: data curation; BM: data curation; CG: supervision; PM: formal analysis; ST: formal analysis; MS: writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Franzese, C., Vernier, V., Franceschini, D. et al. Total tumor volume as a predictor of survival in patients with multiple oligometastases treated with stereotactic ablative radiotherapy (SABR). J Cancer Res Clin Oncol 149, 10495–10503 (2023). https://doi.org/10.1007/s00432-023-04964-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-04964-z