Abstract
Background
Tobacco use is the leading preventable cause of cancer and premature death, smoking has a clear causal relationship with a variety of cancers. However, the relationship between exposure to secondhand smoke (SHS) and other cancers besides lung cancer is not clear. In this study, we intend to investigate the cancers mortality risks especially other cancers besides lung cancer associated with exposure to SHS.
Methods
The National Health and Nutrition Examination Survey is a longitudinal population-based, nationally representative health survey and mortality rates linked to the National Death Index (NDI) database. In this study, the participants completed a questionnaire assessing sociodemographic data, anthropometry, and lifestyle information, including smoking and alcohol consumption, meanwhile, all the participants were screened for serum cotinine. First, Spearman correlation analysis was performed to confirm the correlation between serum cotinine level and exposure status. And then, exposure to SHS was divided into two groups: low exposure group (serum cotinine level between 0.015 and 10) and high exposure group (serum cotinine level ≥ 10), Cox proportional hazards regression modeling was used to evaluate the association between exposure to SHS and eight different types of smoke-related cancer.
Results
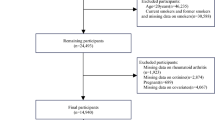
In this study, we evaluated a cohort of 25,794 US residents older than 19 years from 2005 to 2016 and were followed for mortality through the February 2019. We conducted Spearman correlation analysis to confirm the correlation between serum cotinine level and exposure status (including smoking and exposure to SHS), it demonstrated the correlation coefficient between serum cotinine level and exposure to smoke was 0.976, p < 0.00001. By Cox proportional hazards regression modeling, high exposure group were found to be positively associated with all neoplasms with a total Hazard Ratio (HR) of 1.748 (95% Confidence Interval (CI), 1.415–2.159), had higher all-cause mortality risks than non-exposure to tobacco smoke. Regarding the specific types, we found the following associations: cancer of the lung (HR, 1.484; 95% CI, 1.191–1.849), stomach (HR, 1.491; 95% CI, 1.199–1.854), bladder (HR, 1.487; 95% CI, 1.198,1.846), esophageal (HR, 1.487; 95% CI 1.194–1.852), kidney (HR, 1.497; 95% CI, 1.201–1.865), pancreatic (HR, 1.479; 95% CI 1.189–1.841), leukemia (HR, 1.479; 95% CI 1.190–1.839), cervical (HR, 1.490; 95% CI 1.198–1.853). However, low exposure group were non-existent statistically significant with a Hazard Ratio (HR) of 1.062 (95% Confidence Interval (CI), 0.953–1.183).
Conclusions
The research demonstrated that serum cotinine has a significant correlation with smoke exposure status, which confirmed serum cotinine can be used as an indicator to reflect human smoke exposure. What’s more, our results confirmed high exposure of SHS (serum cotinine level ≥ 10) has a significant effect on lung, stomach, bladder, esophagus, kidney, pancreatic, leukemia, cervical cancer.


Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- SHS:
-
Secondhand smoke
- HR:
-
Hazard ratio
- NDI:
-
National Death Index
- NHANES:
-
National Health and Nutrition Examination Survey
- STROBE:
-
Strengthening the Reporting of Observational Studies in Epidemiology
References
Altshuler B (1989) Quantitative models for lung cancer induced by cigarette smoke. Environ Health Perspect 81:107–122. https://doi.org/10.1289/ehp.8981107
Asfar T, Dietz NA, Arheart KL, Tannenbaum SL, McClure LA, Fleming LE, Lee DJ (2016) Smoking behavior among adult childhood cancer survivors: what are we missing? J Cancer Surviv 10(1):131–141. https://doi.org/10.1007/s11764-015-0459-6
Benowitz NL (1996) Cotinine as a biomarker of environmental tobacco smoke exposure. Epidemiol Rev 18(2):188–204. https://doi.org/10.1093/oxfordjournals.epirev.a017925
Benowitz NL, Jacob P 3rd (1994) Metabolism of nicotine to cotinine studied by a dual stable isotope method. Clin Pharmacol Ther 56(5):483–493. https://doi.org/10.1038/clpt.1994.169
Benowitz NL, Jacob P 3rd, Fong I, Gupta S (1994) Nicotine metabolic profile in man: comparison of cigarette smoking and transdermal nicotine. J Pharmacol Exp Ther 268(1):296–303
Chen TC, Clark J, Riddles MK, Mohadjer LK, Fakhouri T (2020) National health and nutrition examination survey, 2015–2018: sample design and estimation procedures. Vital and health statistics. Series 2. Data Eva Methods Res 184:1–35
Doll R, Hill AB (1954) The mortality of doctors in relation to their smoking habits; a preliminary report. BMJ 1(4877):1451–1455. https://doi.org/10.1136/bmj.1.4877.1451
Doll R, Hill AB (1956) Lung cancer and other causes of death in relation to smoking; a second report on the mortality of British doctors. BMJ 2(5001):1071–1081. https://doi.org/10.1136/bmj.2.5001.1071
Gaffney M, Altshuler B (1988) Examination of the role of cigarette smoke in lung carcinogenesis using multistage models. J Natl Cancer Inst 80(12):925–931. https://doi.org/10.1093/jnci/80.12.925
Gram IT, Wiik AB, Lund E, Licaj I, Braaten T (2022) Never-smokers and the fraction of breast cancer attributable to second-hand smoke from parents during childhood: the Norwegian Women and Cancer Study 1991–2018. Int J Epidemiol 50(6):1927–1935. https://doi.org/10.1093/ije/dyab153
Hammond SK, Leaderer BP (1987) A diffusion monitor to measure exposure to passive smoking. Environ Sci Technol 21(5):494–497. https://doi.org/10.1021/es00159a012
Hecht SS, Carmella SG, Murphy SE, Akerkar S, Brunnemann KD, Hoffmann D (1993) A tobacco-specific lung carcinogen in the urine of men exposed to cigarette smoke. N Engl J Med 329(21):1543–1546. https://doi.org/10.1056/NEJM199311183292105
Hukkanen J, Jacob P 3rd, Benowitz NL (2005) Metabolism and disposition kinetics of nicotine. Pharmacol Rev 57(1):79–115. https://doi.org/10.1124/pr.57.1.3
IARC Working Group on the Evaluation of Carcinogenic Risks to Humans (2004) Tobacco smoke and involuntary smoking. IARC Monogr Eval Carcinog Risks Hum 83:1–1438
Jaakkola MS, Jaakkola JJ (1997) Assessment of exposure to environmental tobacco smoke. Eur Respir J 10(10):2384–2397. https://doi.org/10.1183/09031936.97.10102384
Kim S (2016) Overview of cotinine cutoff values for smoking status classification. Int J Environ Res Public Health 13(12):1236
Kim AS, Ko HJ, Kwon JH, Lee JM (2018) Exposure to secondhand smoke and risk of cancer in never smokers: a meta-analysis of epidemiologic studies. Int J Environ Res Public Health 15(9):1981. https://doi.org/10.3390/ijerph15091981
Lee CK, Brown BG, Reed EA, Coggins CR, Doolittle DJ, Hayes AW (1993) Ninety-day inhalation study in rats, using aged and diluted sidestream smoke from a reference cigarette: DNA adducts and alveolar macrophage cytogenetics. Fundam Appl Toxicol 20(4):393–401. https://doi.org/10.1006/faat.1993.1051
Levy RV, Brathwaite KE, Sarathy H, Reidy K, Kaskel FJ, Melamed ML (2021) Analysis of active and passive tobacco exposures and blood pressure in US children and adolescents. JAMA Netw Open 4(2):e2037936. https://doi.org/10.1001/jamanetworkopen.2020.37936
Maclure M, Katz RB, Bryant MS, Skipper PL, Tannenbaum SR (1989) Elevated blood levels of carcinogens in passive smokers. Am J Public Health 79(10):1381–1384. https://doi.org/10.2105/ajph.79.10.1381
Mohtashamipur E, Mohtashamipur A, Germann PG, Ernst H, Norpoth K, Mohr U (1990) Comparative carcinogenicity of cigarette mainstream and sidestream smoke condensates on the mouse skin. J Cancer Res Clin Oncol 116(6):604–608. https://doi.org/10.1007/BF01637081
Nelson E (2001) The miseries of passive smoking. Hum Exp Toxicol 20(2):61–83. https://doi.org/10.1191/096032701670538508
Office on Smoking and Health (US) (2006) The health consequences of involuntary exposure to tobacco smoke: a report of the surgeon general, Centers for Disease Control and Prevention (US).
Rattan P, Penrice DD, Ahn JC, Ferrer A, Patnaik M, Shah VH, Kamath PS, Mangaonkar AA, Simonetto DA (2022) Inverse Association of telomere length with liver disease and mortality in the US population. Hepatol Commun 6(2):399–410. https://doi.org/10.1002/hep4.1803
Rowland C, Eiser C, Rowe R, Danson S (2012) The effect of smoking on health-related quality of life in lung cancer patients: a systematic review. BMJ Support Palliat Care 2(4):312–318. https://doi.org/10.1136/bmjspcare-2011-000186
Sandra L., Strokoff et al. (2010). Compilation of patient protection and affordable care act. Available at https://www.healthcare.gov/glossary/affordable-care-act/
Shikata S, Takemura Y (2017) Secondhand smoke exposure and risk of lung cancer in Japan: a systematic review and meta-analysis of epidemiologic studies. Jpn J Clin Oncol 47(3):282. https://doi.org/10.1093/jjco/hyw173
Sung H, Ferlay J, Siegel RL et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
US Centers for Disease Control and Prevention (2021) Environmental health: laboratory procedure manual, Revised September 10, 2008. Accessed January 20, 2021.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, Initiative STROBE (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. PLoS Med 4(10):e296. https://doi.org/10.1371/journal.pmed.0040296
Wen Q, Wang X, Lv J, Guo Y, Pei P, Yang L, Chen Y, Du H, Burgess S, Hacker A, Liu F, Chen J, Yu C, Chen Z, Li L, China Kadoorie Biobank Collaborative Group (2022) Association between involuntary smoking and risk of cervical cancer in Chinese female never smokers: a prospective cohort study. Environ Res 212:113371. https://doi.org/10.1016/j.envres.2022.113371
World Health Organization (2007) Protection from exposure to second-hand tobacco smoke: policy recommendations. World Health Organization, Geneva
Zhang YB, Chen C, Pan XF, Guo J, Li Y, Franco OH, Liu G, Pan A (2021) Associations of healthy lifestyle and socioeconomic status with mortality and incident cardiovascular disease: two prospective cohort studies. BMJ (clin Res Ed) 373:n604. https://doi.org/10.1136/bmj.n604
Funding
This work is supported by the National Natural Science Foundation (82074187) and Clinical Research Fund of Wu Jieping Medical Foundation (320.6750.17233).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Dr ZL had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Concept and design were put forward by Pro JL Material preparation, data collection and analysis were performed by ZZ, ZL and XZ. JC, LW and ZL prepared Figs. 1, 2 and Tables 1, 2. The first draft of the manuscript was written by Zhongmian Zhang, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
This work has not been published or accepted for publication, nor is it under consideration at another journal. Moreover, one would like to declare on behalf of the authors that there are no ethical nor other conflicts of interests and that all authors have seen and approved the manuscript.
Ethical standards
Every participant in the NHANES provided written informed consent, and the survey data collection was approved by the NCHS Research Ethics Review Board. The data used for these analyses were completely deidentified and released as public-use data, and therefore, deemed exempt from review by institutional review board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, Z., Li, Z., Zhang, X. et al. Association between secondhand smoke and cancers in adults in the US population. J Cancer Res Clin Oncol 149, 3447–3455 (2023). https://doi.org/10.1007/s00432-022-04266-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04266-w