Abstract
Despite being relatively rare, pediatric traumatic spinal cord injury (TSCI) is a debilitating event with high morbidity and long-term damage and dependency. This study aims to provide insight on the epidemiological characteristics of pediatric TSCI worldwide. The studies were included if they provided data for the pediatric population with the diagnosis of TSCI. Information sources included PubMed, Embase, Web of Science, and Scopus. All databases were searched from 1990 to April 2023. The quality of included studies was evaluated by Joanna Briggs Institute Critical Appraisal Tools. The results of the meta-analysis were presented as forest plots. PROSPERO Registration code: CRD42020189757. We identified 87 studies from 18 developed and 11 developing countries. Of the 87 studies evaluated, 52 studies were considered medium quality, 27 studies were considered high quality, and 8 studies were considered low quality. In developed countries, the proportion of TSCIs occurring in patients aged 0–15 years was 3% (95% CI: 2.2%; 3.9%), while in developing countries, it was 4.5% (95% CI: 2.8%; 6.4%). In developed countries, the pooled incidence of pediatric TSCI was 4.3/millions of children aged 0–15/year (95% CI: 3.1; 6.0/millions children aged 0–15/year) and boys comprised 67% (95% CI: 63%; 70%) of cases. The most prevalent level of injury was cervical (50% [95% CI: 41%; 58%]). The frequency of SCI Without Obvious Radiological Abnormality (SCIWORA) was 35% (95% CI: 18%; 54%) among children 0–17 years. The most common etiology in developed countries was transport injuries (50% [95% CI: 42%; 57%]), while in developing countries falls were the leading cause (31% [95% CI: 20%; 42%]). The most important limitation of our study was the heterogeneity of studies in reporting age subgroups that hindered us from age-specific analyses.
Conclusion: Our study provided accurate estimates for the epidemiology of pediatric TSCI. We observed a higher proportion of pediatric TSCI cases in developing countries compared to developed countries. Furthermore, we identified distinct epidemiological characteristics of pediatric TSCI when compared to adult cases and variations between developing and developed countries. Recognizing these unique features allows for the implementation of cost-effective preventive strategies aimed at reducing the incidence and burden of TSCI in children.
What is Known: • Pediatric Traumatic Spinal Cord Injury (TSCI) can have profound physical and social consequences for affected children, their families, and society as a whole. • Epidemiological insights are vital for they provide the data and understanding needed to the identification of vulnerable populations, aiding in the development of targeted prevention strategies and effective resource allocation. | |
What is New: • The estimated incidence of pediatric TSCI in developed countries is 4.3 cases per million children aged 0-15. The proportion of pediatric TSCI cases in relation to all-age TSCI cases is 3% in developed countries and 4.5% in developing countries. • The etiology of TSCI in pediatric cases differs between developing and developed countries. In developed countries, transport injuries are the most prevalent cause of pediatric TSCI, while falls are the least common cause. Conversely, in developing countries, falls are the leading cause of pediatric TSCI. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The age distribution of traumatic spinal cord injury (TSCI) exhibits a bimodal pattern with two distinct peaks [1]. The first peak is observed among young adults, typically between the ages of 15 and 29. This group is particularly prone to traumatic injuries caused by motor vehicle accidents, sports-related incidents, and falls. The second peak occurs among older adults, generally over the age of 65, primarily due to the increased risk of falls associated with aging [1, 2]
Pediatric TSCI can devastate the health and social well-being of affected children, their families, and society.Although neurological recovery in children with TSCI is thought to be better than in adults [3], the prognosis for most children is bleak, with complete SCI leaving patients functions requiring full assistance to perform their physiologic functions [4]. Furthermore, diagnosing TSCI in children is more challenging because a significant percentage of these patients present with SCI without obvious radiological abnormalities (SCIWORA) on X-ray or CT scans [5]. Therefore the use of MRI is necessary to accurately diagnose these cases.
In general, the causes of pediatric TSCI worldwide are transport-related injuries, sports/leisure activities, assault, and falls [4]. These causes are frequently avoidable, albeit occasionally inevitable. To ensure adequate preventive measures, physicians and potential children and families at risk must have a thorough understanding of the epidemiology of pediatric TSCI. However, data on pediatric TSCI is scant and fragmented. Furthermore, when compared to adults the heterogeneity of data and the lack of a clear global definition of pediatric TSCI incidence necessitate extensive epidemiologic research [6, 7]. Evidence-based knowledge about pediatric TSCI epidemiology is useful for preventing traumatic events and assisting physicians in tailoring treatment and rehabilitative programs to the needs of individuals based on their prognostic status. Furthermore, epidemiologic knowledge is important to determining the global distribution of pediatric TSCI. This can assist various health administrators and organizations in providing equitable infrastructure and financial aid.
Given the limited attention to pediatrics compared to adults in existing studies, the objective of this study was to offer comprehensive insights into pediatric TSCI epidemiology, uncovering differences in incidence, etiology, and injury severity between developed and developing countries. Additionally, the study acknowledged and tackled the inconsistency in defining "pediatrics," thereby enhancing the clarity surrounding this crucial facet of pediatric healthcare.
Material and methods
This systematic review and meta-analysis were carried out following the guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [8]. Furthermore, the study was pre-registered with a predefined review protocol in PROSPERO (registration number CRD42020189757).
Eligibility criteria
The inclusion criteria are presented in Table 1. The studies were included if they provided data for the pediatric population (≤ 21 years) with the diagnosis of TSCI.
Search strategy
A librarian (MG) performed the search in PubMed, Embase, Web of Science, and Scopus all from 1900 to April 2023. The search syntax was performed by combining the MeSH terms and keywords of related articles and expert opinions. The detailed search syntax is presented in Table 2. The strategy for other databases is given in Supplementary files. The last search was carried out on 15th April 2023.
Selection process
After elimination of duplicate records, two reviewers (SFM and MADO) screened the titles and abstracts independently. In case of disagreement, a third reviewer (SBJ) was consulted to reach a consensus. The full texts of all potentially eligible abstracts were retrieved and assessed based on inclusion criteria by the same two reviewers independently. The reference lists of all included studies and reviews were screened to identify any additional relevant papers.
Data collection process
Three reviewers (SBJ, SFM, and MRF) independently extracted data from included full texts in accordance with the International Spinal Cord Injury Core and Basic Data Sets for children and youth with SCI [9, 10]. Any discrepancy was resolved by consulting a fourth reviewer (AG). A specialized Excel spreadsheet tailored to the study's objectives was used as the data collection tool. Discrepancies arising from data extraction were identified through a comparison of results, and agreement was reached through consensus.
Information on participant characteristics (sample size, age, sex, etiology, level of injury, completeness of injury, Frankel grade or American Spinal Injury Association (ASIA) impairment Scale (AIS), descriptive characteristics (publication time, country, period of observation), methodological details (study design, the extent of study (national, subnational) were extracted. Additional information for data extraction can be found in Supplementary files.
Critical appraisal
The assessment of the studies' quality was conducted using the Joanna Briggs Institute critical appraisal tool designed for evaluating observational studies [11]. Further details regarding critical appraisal can be found in Supplementary files.
Meta-analysis
For meta-analysis we separately analyzed developing and developed countries because it is known that there are significant differences in epidemiology of TSCI between developing and developed countries [12, 13]. We used the definition of the developing countries from the International Monetary Fund (IMF) 2021 update [14]. Only studies that were published after 1990 and had extractable data regarding age category of 0–15 years were included in meta-analysis. We considered pediatrics cut-off age of 0–15 years to be consistent with recent guidelines [7]. Based on data availability of studies we decided that the studies for 0–14 or 0–15 age groups were not sufficient for a distinct meta-analysis; however, we were able to perform meta-analysis after combining these two age groups. The details of data synthesis have been described in Supplementary files.
Results
Study selection
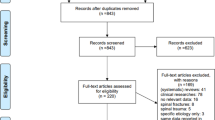
The PRISMA flow diagram displays the recognized studies at each stage (Fig. 1). The search resulted in the identification of 7828 records following the removal of duplications. After title screening, 681 abstracts were investigated, of which 87 full texts were included.
Methodological quality
The quality of 87 studies was evaluated. The quality score of studies ranged between 3 to 9 and only nine studies got the maximum score. Overall, 52 studies (60%) had medium quality, 27 studies (31%) had high quality and 8 studies (9%) had low quality. The details of individual study scores can be found in Supplementary files.
Review findings
Prevalence or incidence rate of TSCI in the pediatric population was reported in 42 studies [15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56] (Supplementary Table 1). The descriptive information of pediatric TSCI patients, level of injury and severity of TSCI were reported in 50 studies [15, 16, 20, 22, 23, 26, 31, 34, 36, 38,39,40,41,42, 48, 49, 52, 55, 57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88] (Supplementary Table 2). The etiology of pediatric SCI was reported in 41 studies [15, 16, 20, 22, 23, 26, 31, 34, 36, 39,40,41,42, 52, 57,58,59,60,61, 63,64,65,66,67, 69, 71,72,73,74,75,76,77,78,79,80, 82, 84,85,86,87,88] (Supplementary Table 3). Thirty-seven studies contained data for all-age TSCI (0–99 years) [17, 20,21,22,23,24,25,26,27, 30, 32, 37, 53, 54, 60, 71, 79, 81, 86, 87, 89, 59, 90,91,92,93,94,95,96,97,98,99,100,101,102,103,104]. These studies were used to estimate the proportion of pediatric TSCI (0–15 years) to all-age TSCI.
The incidence, gender, and severity of pediatric TSCI (0–15 years)
Twenty-one studies contained sufficient TSCI incidence data (number of cases and population at risk) for age category of 0–15 and were eligible for meta-analysis. The estimation of incidence in developed countries with meta-analysis among 18 studies was 4.3 cases per millions of children aged 0–15 (95% CI: 3.1; 6.0) Fig. 2). Only three studies reported TSCI incidence in developing countries including Tanzania and China where the incidence varied between 1.5 to 11.7 cases per millions of children aged 0–15 [37, 53, 54]
Taking into account gender distribution, a total of thirteen studies focusing on developed countries were incorporated into the meta-analysis. The analysis yielded an estimated male cases proportion of 67% (95% CI: 63%; 70%) within the pooled sample of 6,300 individuals from these developed countries (as presented in Appendix Fig. 1A). Only four studies reported gender proportion of 0–15 age group in developing countries. In these studies, male proportion ranged between 59% and 79% [64, 79, 82, 86].
Totally, eleven studies provided data about the completeness/incompleteness of TSCIs in age group 0–15, of which ten were related to developed countries and were included in the meta-analysis. The frequency of complete injury in the pooled sample of 6,396 individuals was 44% (95% CI: 28%; 59%, Fig. 3A) while the frequency of incomplete injury was 56% (95% CI: 40%; 72%, Fig. 3B). The frequency of complete injury among children aged 0–15 in developing countries was reported in Pakistan [64], India [82] and China [88] as 80%, 50% and 31%, respectively.
Regarding tetraplegia versus paraplegia we considered six studies related to developed countries that reported the severity of injury. The proportion of complete tetraplegia and incomplete tetraplegia in the pooled sample of 222 individuals in six included studies was 15% (95% CI: 8.1%; 23%, Appendix Fig. 1B) and 27% (95% CI: 14%; 43%, Appendix Fig. 1C), respectively. The complete paraplegia and incomplete paraplegia proportion in the pooled sample of 222 individuals in 6 included studies was 28% (95% CI: 11%; 55%, Appendix Fig. 1D) and 24% (95% CI: 16%; 32%, Appendix Fig. 1E), respectively. The frequency of paraplegia and tetraplegia among the 0–15 age group in developing countries were reported in Pakistan, and were 86% and 14%, respectively [64].
Etiologies of TSCIs
In the meta-analysis encompassing 16 studies focused on developed countries, the leading etiology of TSCIs was transport injuries, constituting the highest relative frequency. Specifically, the relative frequency of transport injuries within the pooled sample of 7,368 individuals was 50% (95% CI: 42%; 57%, as demonstrated in Fig. 4A). Notably, among five studies from developing countries, the relative frequency of transport injuries in the pooled sample of 401 individuals was 24% (95% CI: 13%; 37%, as indicated in Fig. 4A*).
Meta-analysis of the etiology of pediatric TSCIs. A Transport injuries in developed countries A* Transport injuries in developing countries. B Falls in developed countries B* Falls in developing countries. C Sports-leisure activity in developed countries C*Sports-leisure activity in developing countries. D Assault in developed countries D* Assault in developing countries
Regarding falls, a meta-analysis of 16 studies pertaining to developed countries revealed a frequency of 10% (95% CI: 7.1%; 15%) within the pooled sample of 7,368 individuals (as shown in Fig. 4B). In contrast, within the context of developing countries, the relative frequency of falls among five studies comprising 401 individuals was notably higher at 31% (95% CI: 20%; 42%, as illustrated in Fig. 4B*).
The analysis of TSCI etiologies related to sports, involving twelve studies associated with developed countries, unveiled a frequency of 16% (95% CI: 12%; 21%) within the pooled sample of 7,293 individuals (depicted in Fig. 4C). Among studies from developing countries, involving 401 individuals across five studies, the relative frequency of sports-related injuries was 14% (95% CI: 1.7%; 34%, as presented in Fig. 4C*).
Regarding assaults as an etiology, among 10 studies covering developed countries and a pooled sample of 7,240 individuals, the frequency of assault-related TSCIs was 11% (95% CI: 7.1%; 17%, shown in Fig. 4D). Notably, within two studies from Brazil and Pakistan, assault emerged as the primary cause of TSCIs. Among four studies from developing countries encompassing 359 individuals, the relative frequency of assault-related injuries was 18% (95% CI: 5.1%; 37%, as seen in Fig. 4D*).
Furthermore, the frequency of other/unrecognized etiologies within the pooled sample of 7,293 individuals from 13 studies in developed countries was 14% (95% CI: 8.5%; 21%, as presented in Appendix Fig. 1H). In the context of developing countries, this relative frequency was notably lower at 5.6% (95% CI: 0.7%; 13%, as depicted in Appendix Fig. 1H*).
Level of TSCIs
In the meta-analysis focused on injury level, our consideration was limited to studies that categorized injuries into three distinct groups: cervical, thoracic, or lumbosacral. Within the pooled dataset of 2,897 individuals from six studies centered on developed countries, the frequency of cervical-level injuries was found to be 50% (95% CI: 41%; 58%, as shown in Appendix Fig. 1I). Moreover, thoracic-level injuries constituted 35% (95% CI: 23%; 47%, as presented in Appendix Fig. 1J), while lumbosacral-level injuries accounted for 13% (95% CI: 6.9%; 20%, as illustrated in Appendix Fig. 1K). Regarding developing countries only three studies had level specific data. In India [82] cervical level was injured in 50% of children 0–15 years. However thoracic level was more prevalent than cervical level in studies from Pakistan [62] and China [88].
TSCI proportion in pediatrics
For meta-analysis, 21 studies provided data about the proportion of pediatric TSCI (0–15 years) to all-age (0–99 years) TSCI in developed countries, while there were 16 studies related to developing countries. The frequency of TSCI related to pediatrics in the pooled sample of 130,945 individuals in developed countries was 3% (95% CI: 2.2%; 3.9%, Fig. 5A) while in developing countries in the pooled sample of 86,669 was 4.5% (95% CI: 2.8%; 6.4%, Fig. 5B).
SCIWORA (0–17 years)
Based on data availability we calculated the frequency of SCIWORA in 0–17 years. In a pooled sample of 11,299 individuals from 7 included studies related to developed countries the frequency of SCIWORA was 35% (95% CI: 19%; 54%, Appendix Fig. 1L). There were no studies of SCIWORA in this age group in developing countries.
Sensitivity analysis
The results of sensitivity analysis are provided in supplementary files.
Discussion
In this comprehensive epidemiological study, we sought to bridge the difference among reports on the incidence of pediatric TSCI using a meta-analytical approach. Importantly, this epidemiological data can support and lead clinical and policy efforts to improve TSCI in children among marginalized groups. New et al. reviewed pediatric TSCI in 25 countries and found that pediatric TSCI incidence varied from 3.3–13.2 case per million population in different regions [7]. According to our meta-analysis, the estimated incidence of pediatric TSCI among developed countries was 4.3 cases per million children aged 0–15 (95% CI: 3.1–6.0 cases per million children aged 0–15).
Regarding the trend of TSCI over time we found an upward trend in two studies in Norway, and a constant or decreasing trend in seven studies form Australia, Netherlands, Spain and the U.S (Supplementary Table 1). The increasing trend in incidence of pediatric TSCI observed in Norway can be explained by a decrease in the rate of prehospital mortality, and higher number of transport-related injuries and more sports/leisure activities in pediatric population [20, 21]. It is also important to analyze the reasons behind the decreasing pattern of TSCI incidence. In the United States, Saunders et al. observed a significant decrease in incidence of pediatrics TSCI from 1998–2012 only in Whites. They also showed higher incidence of assault-related injuries in non-Whites in comparison to Whites (29% vs 5%) during the study period. Therefore, they suggested that future preventive measures should be focused on assault-related injuries in non-White pediatric population [39]. Two studies also observed a decreasing trend in incidence of pediatric TSCI in Spain, but they related this decrease to the decline in the frequency of transport-related injuries as a result of improvement in road-safety, and implementation of awareness raising campaigns [16, 22]. Lystad et al. observed that over a period of 10 years, the hospitalization rates for spinal cord and nerve injuries declined by 2.8% per year in Australia. However, contrasting trends were observed for spinal fractures and spinal sprains/strains, with rates increasing by 1.1% and 4.7% respectively. The authors also observed an increase in female hospitalization especially as a result of equestrian injuries [55].
The reported proportion of pediatric TSCI to all-age TSCI varies among individual studies and literature reviews. However, the rate of pediatric TSCI in most data are heterogeneous and mixed [6, 71, 105, 106]. The pooled proportion of pediatric TSCI in this study was 3% and 4.5% in developed and developing countries, respectively. These results suggest that the proportion of pediatric TSCI injuries is higher in developing countries compared to developed countries. This finding aligns with the findings of Ding et al. study which similarly highlighted that children from families with lower socioeconomic status face an increased risk of encountering SCI [107].
We observed a male predominance for pediatric TSCI. However, seemingly there is an increase in the trend of female spine injuries due to the recent increase in female sport activities since the latter part of the twentieth century [55].
De Vivo and Vogel found complete injury to be highest in children aged from 0 to 5, while incomplete injury was more common in ages between 13 and 15 years [66]. However, we found that most children are more susceptible to incomplete injury (56%) than complete injury (44%). The higher incidence of incomplete injury compared with complete injury can be attributed to the lower number of traffic accidents and improved initial care and treatment modalities in developed countries [22]. In our meta-analysis the frequency of complete paraplegia > incomplete tetraplegia > incomplete paraplegia > complete tetraplegia was observed in developed countries. Some publications discovered significant correlation between tetraplegia and incomplete injury, and paraplegia and complete injury [34, 60, 66, 78]. However, the exact explanation for this correlation is yet to be elucidated.
SCIWORA may be explained by the difference in elasticity between the spinal column and the spinal cord [100]. Notably, children below 8 years are at risk of SCIWORA and consequently complete or severe partial cord lesions [68, 70, 76, 105, 108, 109]. We estimated the frequency of SCIWORA to be 35% in developed countries. It indicates that a significant proportion of individuals in the studied population experienced spinal cord injuries without accompanying radiographic abnormalities. The best diagnostic technique for SCIWORA is MRI, which allows for the evaluation of extradural spaces as well as the integrity of the spinal ligaments [110].
Craniocervical junction and atlanto-axis (C1-C2) injuries are more common in children below 8 or pre-teens[3, 66, 111]. However, C4-C5 injuries are observed most in teens and adults[3]. The large head-to-torso ratio and the horizontally aligned vertebra in younger children account for the higher proportion of cervical injuries [4, 111, 112]. Interestingly, the craniocervical junction and atlanto-axis joint become more secure and less prone to injuries, as the child grows. [111]. By 8 to 10 years of age, the spine is thought to acquire a more adult position, with cervical fractures in children in this age group having a comparable spectrum to adult fractures [103]. While certain studies have suggested that the percentage of cervical injuries could range between 60% and 80% [105, 113], we found a relatively lower frequency of 50% for cervical injuries, with subsequent rates of 35% for thoracic injuries and 13% for lumbosacral injuries. Variations in the definitions used for categorizing and classifying injuries, as well as regional disparities in injury patterns, can contribute to differences in reported percentages.
The etiology of TSCI in pediatrics tends to differ from developing and developed countries. In our meta-analysis, we found that the most prevalent cause of pediatric TSCI in developed countries was transport injuries and falls were the least common while in developing countries falls were the leading etiology. This could be due to factors such as inadequate infrastructure, unsafe living conditions, or lack of safety measures in homes and public spaces. Falls from heights, such as from trees or buildings, may be more common in these settings. In addition assault related injuries were prevalent in developing countries such as Brazil [63] and Pakistan [64]. This suggests that intentional acts of violence, including physical abuse or assaults, contribute significantly to the occurrence of TSCI in pediatric populations in these regions. Sports-related injuries were found to be common causes of pediatric TSCI in both developing and developed countries. These injuries often occur in older children who engage in sports activities. Participation in contact sports or high-risk activities without proper safety precautions can lead to spinal cord injuries. Giving careful consideration to sports-related injuries is of utmost importance in the context of children. This significance stems from the fact that children have a relatively higher head-to-body ratio and their paraspinal muscle support hasn't fully matured [114]. As a result, they are more vulnerable to cervical injuries, which could potentially lead to paralysis and respiratory complications, ultimately carrying the risk of fatal outcomes [115].
Understanding the variation in etiology of pediatric TSCI in different countries is crucial for developing targeted prevention strategies, improving infrastructure and safety measures, and providing appropriate medical care. Our findings highlights the need for context-specific approaches to prevent and manage pediatric TSCI based on the prevalent causes in each country or region.
Limitations
The most important limitation of our study was the fact that the outcome reporting of studies was highly heterogeneous. Various age cut-offs were used as definition of pediatric population, furthermore different age sub-groups were used which precluded us from performing a sub-group meta-analysis of age-specific level, severity and etiology of injury. Additionally, there were only few studies from developing countries, which hindered us from performing a meta-analysis of incidence rate, gender proportion, injury completeness, severity, and level of TSCI in these countries. Overall, we could find data only for 29 countries, most of which were developed countries, which can reduce the generalizability of data. Most of the included studies were medium or low quality which can increase the risk of bias in the published articles.
Conclusion
This systematic review, to our knowledge, is the first to use a meta-analytic approach to describe the epidemiology of pediatric TSCI. According to our meta-analysis, the proportion of pediatric TSCI to all age TSCI was higher in developing countries than in developed countries. Developed countries have an estimated incidence of 4.3 cases per million children aged 0–15. Regarding the level of TSCI, cervical injuries were more than thoracic and lumbosacral injuries in developed countries. The most common etiology of TSCI were transport-related injuries in developed countries and falls in developing countries. The distinct epidemiological features identified in TSCIs have the potential to guide the development of targeted and cost-effective preventive strategies, aimed at reducing the incidence and overall impact of TSCIs in the pediatric population.
Implications for future studies
In order to improve the quality of studies and to ensure the comparability of data, we encourage global spine fracture and SCI registry and future registry-based studies to use a standardized form of data reporting. The International Spinal Cord Injury Core data set provides useful recommendations in this regard [9, 10].
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Van den Berg M et al (2010) Incidence of spinal cord injury worldwide: a systematic review. Neuroepidemiology 34(3):184–192
Jabbour P et al (2008) Traumatic spine injuries in the geriatric population. Neurosurg Focus 25(5):E16
Parent S et al (2011) Spinal cord injury in the pediatric population: a systematic review of the literature. J Neurotrauma 28(8):1515–1524
Vogel L, Anderson C (2003) Spinal cord injuries in children and adolescents: a review. J Spinal Cord Med 26(3):193–203
Szwedowski D, Walecki J (2014) Spinal Cord Injury without Radiographic Abnormality (SCIWORA) - Clinical and Radiological Aspects. Pol J Radiol 79:461–464
Augutis M, Abel R, Levi R (2006) Pediatric spinal cord injury in a subset of European countries. Spinal Cord 44(2):106–112
New PW et al (2019) Global mapping for the epidemiology of paediatric spinal cord damage: Towards a living data repository. Spinal Cord 57(3):183–197
Page MJ et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Biering-Sørensen F et al (2017) International Spinal Cord Injury Core Data Set (version 2.0)-including standardization of reporting. Spinal Cord 55(8):759–764
Carroll A et al (2017) Relevance of the international spinal cord injury basic data sets to youth: an Inter-Professional review with recommendations. Spinal Cord 55(9):875–881
Munn Z et al (2020) Methodological quality of case series studies: an introduction to the JBI critical appraisal tool. JBI Evid Synth 18(10):2127–2133
Golestani A et al (2022) Epidemiology of Traumatic Spinal Cord Injury in Developing Countries from 2009 to 2020: A Systematic Review and Meta-Analysis. Neuroepidemiology 56(4):219–239
Rahimi-Movaghar V et al (2013) Epidemiology of traumatic spinal cord injury in developing countries: a systematic review. Neuroepidemiology 41(2):65–85
Fund IM (2021) World Economic Outlook Database. Cited 31 May 2021. Available from: https://www.imf.org/external/pubs/ft/weo/data/changes.htm
Augutis M, Levi R (2003) Pediatric spinal cord injury in Sweden: incidence, etiology and outcome. Spinal Cord 41(6):328–336
Canosa-Hermida E et al (2019) Epidemiology of traumatic spinal cord injury in childhood and adolescence in Galicia, Spain: report of the last 26-years. J Spinal Cord Med. 42(4):423–429. https://doi.org/10.1080/10790268.2017.1389836. (Epub 2017 Oct 23. PMID: 29058557; PMCID: PMC6776227)
Ferro S et al (2017) Incidence of traumatic spinal cord injury in Italy during 2013–2014: A population-based study. Spinal Cord 55(12):1103–1107
Fine PR et al (1979) Spinal cord injury: an epidemiologic perspective. Paraplegia 17(2):237–250
Griffin MR et al (1985) Traumatic spinal cord injury in Olmsted County, Minnesota, 1935–1981. Am J Epidemiol 121(6):884–895
Hagen EM, Eide GE, Elgen I (2011) Traumatic spinal cord injury among children and adolescents; a cohort study in western Norway. Spinal Cord 49(9):981–985
Halvorsen A et al (2019) Epidemiology of traumatic spinal cord injury in Norway in 2012–2016: a registry-based cross-sectional study. Spinal Cord 57(4):331–338
Montoto-Marqués A et al (2017) Epidemiology of traumatic spinal cord injury in Galicia, Spain: trends over a 20-year period. Spinal Cord 55(6):588–594
Moorin R, Miller TR, Hendrie D (2014) Population-based incidence and 5-year survival for hospital-admitted traumatic brain and spinal cord injury, Western Australia, 2003–2008. J Neurol 261(9):1726–1734
Noonan VK et al (2012) Incidence and prevalence of spinal cord injury in Canada: a national perspective. Neuroepidemiology 38(4):219–226
Pickett GE et al (2006) Epidemiology of traumatic spinal cord injury in Canada. Spine (Phila Pa 1976) 31(7):799–805
Price C et al (1994) Epidemiology of traumatic spinal cord injury and acute hospitalization and rehabilitation charges for spinal cord injuries in Oklahoma, 1988–1990. Am J Epidemiol 139(1):37–47
Surkin J et al (2000) Spinal cord injury in Mississippi. Findings and evaluation, 1992–1994. Spine (Phila Pa 1976) 25(6):716–21
Buechner JS, Speare MC, Fontes J (2000) Hospitalizations for spinal cord injuries, 1994–1998. Med Health R I 83(3):92–93
Dixon GS, Danesh JN, Caradoc-Davies TH (1993) Epidemiology of spinal cord injury in New Zealand. Neuroepidemiology 12(2):88–95
Martins F et al (1998) Spinal cord injuries–epidemiology in Portugal’s central region. Spinal Cord 36(8):574–578
Galvin J, Scheinberg A, New PW (2013) A retrospective case series of pediatric spinal cord injury and disease in Victoria, Australia. Spine (Phila Pa 1976) 38(14):E878–82
New PW et al (2015) Estimating the incidence and prevalence of traumatic spinal cord injury in Australia. Arch Phys Med Rehabil 96(1):76–83
Piatt J, Imperato N (2018) Epidemiology of spinal injury in childhood and adolescence in the United States: 1997–2012. J Neurosurg Pediatr 21(5):441–448
Smith E, Finn S, Fitzpatrick P (2017) Epidemiology of Pediatric Traumatic and Acquired Nontraumatic Spinal Cord Injury in Ireland. Top Spinal Cord Inj Rehabil 23(3):279–284
McCaughey EJ et al (2016) Changing demographics of spinal cord injury over a 20-year period: a longitudinal population-based study in Scotland. Spinal Cord 54(4):270–276
Kewalramani LS, Kraus JF, Sterling HM (1980) Original article acute spinal-cord lesions in a pediatric population: Epidemiological and clinical features. Paraplegia 18(3):206–219
Moshi H et al (2017) Traumatic spinal cord injury in the north-east Tanzania - describing incidence, etiology and clinical outcomes retrospectively. Glob Health Action 10(1):1355604
Puisto V et al (2010) Incidence of spinal and spinal cord injuries and their surgical treatment in children and adolescents: a population-based study. Spine (Phila Pa 1976) 35(1):104–7
Saunders LL et al (2015) Epidemiology of Pediatric Traumatic Spinal Cord Injury in a Population-Based Cohort, 1998–2012. Top Spinal Cord Inj Rehabil 21(4):325–332
Chien LC et al (2012) Age, Sex, and Socio-Economic Status Affect the Incidence of Pediatric Spinal Cord Injury: An Eleven-Year National Cohort Study. Plos One 7(6)
Selvarajah S et al (2014) The epidemiology of childhood and adolescent traumatic spinal cord injury in the United States: 2007–2010. J Neurotrauma 31(18):1548–1560
Vitale MG et al (2006) Epidemiology of pediatric spinal cord injury in the United States: Years 1997 and 2000. J Pediatr Orthop 26(6):745–749
Sabre L et al (2012) High incidence of traumatic spinal cord injury in Estonia. Spinal Cord 50(10):755–759
Karamehmetoglu SS et al (1995) Traumatic spinal cord injuries in Istanbul, Turkey. An epidemiological study. Paraplegia 33(8):469–471
Karacan I et al (2000) Traumatic spinal cord injuries in Turkey: a nation-wide epidemiological study. Spinal Cord 38(11):697–701
Karamehmetoğlu SS et al (1997) Traumatic spinal cord injuries in southeast Turkey: an epidemiological study. Spinal Cord 35(8):531–533
Bracken MB, Freeman DH Jr, Hellenbrand K (1981) Incidence of acute traumatic hospitalized spinal cord injury in the United States, 1970–1977. Am J Epidemiol 113(6):615–622
Mendoza-Lattes S et al (2015) Pediatric Spine Trauma in the United States-Analysis of the HCUP Kid’S Inpatient Database (KID) 1997–2009. Iowa Orthop J 35:135–139
Piatt JH Jr (2015) Pediatric spinal injury in the US: epidemiology and disparities. J Neurosurg Pediatr 16(4):463–471
van Asbeck FW, Post MW, Pangalila RF (2000) An epidemiological description of spinal cord injuries in The Netherlands in 1994. Spinal Cord 38(7):420–424
Nijendijk JH, Post MW, van Asbeck FW (2014) Epidemiology of traumatic spinal cord injuries in The Netherlands in 2010. Spinal Cord 52(4):258–263
Crispo JAG et al (2022) Pediatric Traumatic Spinal Cord Injury in the United States: A National Inpatient Analysis. Topics in spinal cord injury rehabilitation 28(1):1–12
Hao D et al (2021) Trends of epidemiological characteristics of traumatic spinal cord injury in China, 2009–2018. Eur Spine J 30(10):3115–3127
Jiang B et al (2022) Prevalence, incidence, and external causes of traumatic spinal cord injury in China: a nationally representative cross-sectional survey. Front Neurol 20(12):784647. https://doi.org/10.3389/fneur.2021.784647. (PMID: 35126291; PMCID: PMC8811043)
Lystad RP et al (2020) Trends of traumatic spinal injury-related hospitalizations in Australian children over a 10-year period: a nationwide population-based cohort study. Spine J 20(6):896–904
Barbiellini Amidei C et al (2022) Epidemiology of traumatic spinal cord injury: a large population-based study. Spinal Cord 60(9):812–819
Al-Habib A et al (2014) Causes and patterns of spine trauma in children and adolescents in Saudi Arabia: Implications for injury prevention. Ann Saudi Med 34(1):31–37
Andrews LG, Jung SK (1979) Spinal cord injuries in children in British Columbia. Paraplegia 17(4):442–451
Apple DF Jr et al (1995) Spinal cord injury in youth. Clin Pediatr (Phila) 34(2):90–95
Beck B et al (2019) Traumatic spinal cord injury in Victoria, 2007–2016. Med J Aust 210(8):360–366
Burke DC (1974) Traumatic spinal paralysis in children. Paraplegia 11(4):268–276
Carreon LY, Glassman SD, Campbell MJ (2004) Pediatric spine fractures: a review of 137 hospital admissions. J Spinal Disord Tech 17(6):477–482
Costacurta MLG et al (2010) Epidemiological profile of a pediatric population with acquired spinal cord injury from AACD: Sao Paulo/Brazil. Spinal Cord 48(2):118–121
Darain H et al (2018) Epidemiology, Clinical Features and Consequences of Spinal Cord Injury in Children. J Coll Physicians Surg Pak 28(7):532–535
de Amoreira Gepp R, Nadal LG (2012) Spinal cord trauma in children under 10 years of age: clinical characteristics and prevention. Childs Nerv Syst 28(11):1919–24
DeVivo MJ, Vogel LC (2004) Epidemiology of spinal cord injury in children and adolescents. J Spinal Cord Med 27(Suppl 1):S4-10
Erhan B et al (2005) Pediatric Spine and Spinal Cord Injury in Istanbul: A Retrospective Analysis of 106 Patients. Neurosurg Q 15(1):21–24
Hadley MN et al (1988) Pediatric spinal trauma: review of 122 cases of spinal cord and vertebral column injuries. J Neurosurg 68(1):18–24
Haffner DL, Hoffer MM, Wiedbusch R (1993) Etiology of children's spinal injuries at Rancho Los Amigos. Spine (Phila Pa 1976) 18(6):679–84
Hamilton MG, Mylks ST (1992) Pediatric spinal injury: review of 174 hospital admissions. J Neurosurg 77(5):700–704
Jackson AB et al (2004) A demographic profile of new traumatic spinal cord injuries: change and stability over 30 years. Arch Phys Med Rehabil 85(11):1740–1748
Kim C et al (2016) Traumatic spinal injuries in children at a single level 1 pediatric trauma centre: report of a 23-year experience. Can J Surg 59(3):205–212
Lee JH et al (2009) Characteristics of pediatric-onset spinal cord injury: Original Article. Pediatr Int 51(2):254–257
Nadarajah V et al (2018) What are the trends and demographics in sports-related pediatric spinal cord injuries? Phys Sportsmed 46(1):8–13
Pickett W et al (2003) Traumatic spinal cord injury in Ontario, Canada. J Trauma 55(6):1070–1076
Ruge JR et al (1988) Pediatric spinal injury: the very young. J Neurosurg 68(1):25–30
Scher AT (1976) Trauma of the spinal cord in children. S Afr Med J 50(51):2023–2025
Schottler J, Vogel LC, Sturm P (2012) Spinal cord injuries in young children: a review of children injured at 5 years of age and younger. Dev Med Child Neurol 54(12):1138–1143
Taşoğlu Ö et al (2018) Demographic and clinical characteristics of persons with spinal cord injury in Turkey: One-year experience of a primary referral rehabilitation center. J Spinal Cord Med 41(2):157–164
Wang MY et al (2004) High rates of neurological improvement following severe traumatic pediatric spinal cord injury. Spine (Phila Pa 1976) 29(13):1493–7; discussion E266
Yang NP et al (2008) The incidence and characterisation of hospitalised acute spinal trauma in Taiwan–a population-based study. Injury 39(4):443–450
Bansal ML et al (2020) Spinal Injury in Indian Children: Review of 204 Cases. Global Spine Journal 10(8):1034–1039
Compagnon R et al (2020) Epidemiology of spinal fractures in children: Cross-sectional study. Orthop Traumatol Surg Res 106(7):1245–1249
Katar S et al (2020) Pediatric Spinal Traumas. Pediatr Neurosurg 55(2):86–91
Kim W et al (2022) Characteristics of Pediatric Spinal Cord Injury in South Korea: A Single-Centered Study. Ann Rehabil Med 46(5):248–255
Liu H et al (2021) The changing demographics of traumatic spinal cord injury in Beijing, China: a single-centre report of 2448 cases over 7 years. Spinal Cord 59(3):298–305
Liu J et al (2022) Epidemiological features of traumatic spinal cord injury in Beijing, China. J Spinal Cord Med 45(2):214–220
Zou Z et al (2023) Pediatric spinal cord injury with radiographic abnormality: the Beijing experience. Spine J 23(3):403–411
AboAbat AM (1999) Spinal cord injury in Saudi Arabia: Characteristics, bone mineral density, and functional electrical stimulation for upright mobility. University of Salford, Salford
Chang F-S et al (2018) Epidemiological study of Spinal Cord Injury individuals from halfway houses in Shanghai, China. J Spinal Cord Med 41(4):450–458
Chen HY et al (1997) A nationwide epidemiological study of spinal cord injuries in Taiwan from July 1992 to June 1996. Neurol Res 19(6):617–622
Chen Y, He Y, DeVivo MJ (2016) Changing Demographics and Injury Profile of New Traumatic Spinal Cord Injuries in the United States, 1972–2014. Arch Phys Med Rehabil 97(10):1610–1619
Derakhshanrad N et al (2016) Epidemiological study of traumatic spinal cord injuries: experience from a specialized spine center in Iran. Spinal Cord 54(10):901–907
Gur A et al (2005) Characteristics of traumatic spinal cord injuries in south-eastern Anatolia, Turkey: a comparative approach to 10 years’ experience. Int J Rehabil Res 28(1):57–62
Kuptniratsaikul V (2003) Epidemiology of spinal cord injuries: a study in the Spinal Unit, Siriraj Hospital, Thailand, 1997–2000. J Med Assoc Thai 86(12):1116–1121
Löfvenmark I et al (2015) Traumatic spinal cord injury in Botswana: Characteristics, aetiology and mortality. Spinal Cord 53(2):150–154
Ning GZ et al (2016) Epidemiological features of traumatic spinal cord injury in Chongqing, China. J Spinal Cord Med 39(4):455–460
Nwankwo OE, Uche EO (2013) Epidemiological and treatment profiles of spinal cord injury in southeast Nigeria. Spinal Cord 51(6):448–452
Oliver M et al (2012) The changing epidemiology of spinal trauma: A 13-year review from a Level i trauma centre. Injury 43(8):1296–1300
Pagliacci MC et al (2003) An Italian survey of traumatic spinal cord injury. The Gruppo Italiano Studio Epidemiologico Mielolesioni study. Arch Phys Med Rehabil 84(9):1266–75
Thurman DJ et al (1994) Surveillance of spinal cord injuries in Utah, USA. Paraplegia 32(10):665–669
Tugcu I et al (2011) Epidemiologic data of the patients with spinal cord injury: seven years’ experience of a single center. Ulus Travma Acil Cerrahi Derg 17(6):533–538
Wang HF et al (2013) Epidemiological features of traumatic spinal cord injury in Anhui Province, China. Spinal Cord 51(1):20–22
Johansson E et al (2021) Epidemiology of traumatic spinal cord injury in Finland. Spinal Cord 59(7):761–768
Cirak B et al (2004) Spinal injuries in children. J Pediatr Surg 39(4):607–612
Rush JK et al (2013) Associated injuries in children and adolescents with spinal trauma. J Pediatr Orthop 33(4):393–397
Ding W et al (2022) Spinal Cord Injury: The Global Incidence, Prevalence, and Disability From the Global Burden of Disease Study 2019. Spine (Phila Pa 1976) 47(21):1532–1540
Pang D, Wilberger JE (1982) Spinal cord injury without radiographic abnormalities in children. J Neurosurg 57(1):114–129
Turgut M et al (1996) Spinal injuries in the pediatric age group: A review of 82 cases of spinal cord and vertebral column injuries. Eur Spine J 5(3):148–152
Lustrin ES et al (2003) Pediatric cervical spine: normal anatomy, variants, and trauma. Radiographics 23(3):539–560
Martin B, Dykes E, Lecky FE (2004) Patterns and risks in spinal trauma. Arch Dis Child 89(9):860–865
Huisman TA et al (2015) Pediatric spinal trauma. J Neuroimaging 25(3):337–353
Yadav A et al (2022) Pediatric Cervical Spine Injuries. Asian J Neurosurg 17(4):557–562
Alas H et al (2021) Sports-related cervical spine fracture and spinal cord injury: a review of nationwide pediatric trends. Spine 46(1):22–28
Copley PC et al (2019) Management of cervical spine trauma in children. Eur J Trauma Emerg Surg 45:777–789
Acknowledgements
We would like to express our gratitude to Dr. Rasoul Masoomi for his valuable assistance in updating our search.
Funding
This work was funded by Tehran University of Medical Sciences, [grant number is 99-2-93-49831].
Author information
Authors and Affiliations
Contributions
VRM and SMG conceived the presented idea and supervised the project. ZG provided critical feedback and edited the draft. MRF, SFM, MADO and SBJ contributed to data collection. HM, SBK and SBJ contributed to quality appraisal. AG and PS analyzed the data and SBJ wrote the draft. SBJ and AG contributed to data interpretation. MG performed the search. All authors discussed the results and contributed to finalizing the manuscript.
Corresponding authors
Ethics declarations
Ethical approval
The Ethics Committee of Tehran University of Medical Sciences approved the study, and the reference number is IR.TUMS.SINAHOSPITAL.REC.1400.001.
Conflict of interests
The authors announce that there is no competing of interests.
Additional information
Communicated by Gregorio Milani
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jazayeri, S.B., Kankam, S.B., Golestani, A. et al. A systematic review and meta-analysis of the global epidemiology of pediatric traumatic spinal cord injuries. Eur J Pediatr 182, 5245–5257 (2023). https://doi.org/10.1007/s00431-023-05185-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-023-05185-9