Abstract
Lichen sclerosus (LS) is a severe, chronic, dermatosis characterised by inflammatory, sclerotic, pruritic lesions that causes significant morbidity in patients of all genders and ages. In boys, the lesions typically affect the foreskin and glans (termed balanitis xerotica obliterans (BXO)), leading to phimosis and potentially meatal stenosis. The incidence of the disease is not well reported but the average age of affected boys is 8 years (range 1–16). Diagnosis can often be made clinically, although histological study remains important to rule out important differential diagnoses. Complications include genital scarring, urinary and sexual dysfunction as well as the development of carcinomas in adult life. Circumcision has been regarded as definitive management of BXO in boys, but this may be supplemented with medical therapies such as topical steroids, immune modulators, intralesional triamcinolone and ozonated olive oil. Supportive measures including emollients, avoidance of irritants, surveillance of complications and recurrence as well as education and counselling remain important.
Conclusion: BXO remains an important cause of phimosis in boys. The frequency of this condition appears unclear but seems likely to be less than 1% of males. Treatment generally involves circumcision, with some evidence that topical steroids or immunomodulators may decrease the incidence of recurrent meatal stenosis.
What is Known: • Surgical circumcision is considered the definitive management of BXO • Many aspects of BXO are still in contention or require further study including the epidemiology and aetiology. | |
What is New: • There is increasing awareness of non-surgical modalities that may be used in adjunct to surgery including topical corticosteroids, immune modulators, intralesional triamcinolone and ozonated olive oil • Awareness of meatal stenosis-related BXO has led to the development of surgical techniques such as preputioplasty as well as buccal mucosal inlay grafts |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lichen sclerosus (LS) is a chronic, inflammatory dermatosis characterised by white, sclerotic plaques that can occur in both genders across all age groups [19, 39]. In males, LS that affects the penis is used interchangeably with the term balanitis xerotica obliterans (BXO) and the lesion typically affects the prepuce and glans penis leading to phimosis, meatal stenosis, painful erections and difficulties with intercourse in adults [4, 15]. LS was first described in 1887 and cases affecting children have been reported since 1934 [10, 19]. In this article, the literature on the epidemiology, clinical presentation, management and complications of BXO has been reviewed.
Methodology
A search of the literature was conducted of online databases including Medline. Search terms included “lichen sclerosus”, “balanitis xerotica obliterans”, “phimosis”, “pediatrics”, “children” and “males” with application of the appropriate Boolean operators. Forty-two articles were included in this review, with their bibliographies hand-searched for an additional 12 articles. Only papers written in English were included. Articles that discussed the aetiology, pathology, presentation and management of lichen sclerosus exclusively in girls were excluded.
Epidemiology
BXO has been reported to affected 0.3/1000 boys per year (0.5% affected before their 15th birthday) in the UK, between 0.1 and 0.4% in Germany and 0.06% among boys aged less than 10 in Texas, USA [3, 34, 48]. Prevalence is also a statistic difficult to determine. In Denmark, of 181 boys circumcised in 2014, 36 of 49 suspected cases of BXO were confirmed histologically, equivalent to a population rate of 0.37% [51]. The diagnosis appears infrequently made by general practitioners and paediatricians, indicating that the incidence of BXO may be higher than previously thought [22, 41]. This appears supported by a retrospective analysis of 346 foreskin samples by Jayakumar et al., which found an incidence 3.01/1000 boys under the age of 15 [30].
Ethnically, Black American and Hispanic patients have been reported to have twice the risk of developing BXO: although this may be confounded by lower circumcision rates in this population which may impact on both the risk of development of BXO and its progression [13, 25, 34]. Those with a Fitzpatrick phototype 1–2 also appear to have a higher risk of developing BXO (odds ratio (OR) = 0.232; 95% confidence interval = 0.124–0.435) [55]. These seemingly contradictory risk factors would be better clarified with a large-scale epidemiological study of boys with BXO.
The average of age of affected boys is 6.8–9 years old (range 1–16), with a peak incidence at 7 years of age [27, 28, 30, 33, 35, 52]. In the paediatric population, LS affects more females than males, although this generalisation has been challenged in some studies and affected girls might be more likely to present to a paediatrician or paediatric dermatologist than a paediatric surgeon [3, 38].
Several studies have looked at the incidence of BXO in patients presenting with phimosis. Kuehhas et al. reported an incidence of BXO in 17.4% of 76 boys with phimosis (mean age 3.7, range 1–10) [35]. In a prospective study, Mattioli et al. found that 44% of 100 patients with phimosis (mean age 7, range 1–13) had BXO [38]. A study with a larger cohort by Kiss et al. found that 40% of 1178 patients with phimosis (mean age 8.7, range 2–16) had BXO [33].
Aetiology and pathology
Folaranmi et al. attributes the development of BXO lesions to altered fibroblast activity in the dermis leading to fibrosis and atrophy [20]. Celis et al. postulated the involvement of lymphocytes in causing chronic inflammation of the foreskin [8]. The exact cause and aetiology of BXO remain unknown.
BXO seems likely to have a genetic component: in women, there has been an established association with autoimmune diseases (including autoimmune thyroiditis, alopecia areata and vitiligo) but the evidence for such an association in males appears weaker [11, 13, 19, 31]. Other potential associations with BXO include being overweight or obesity, hypertension, hypothyroidism, family history of BXO as well as higher levels of education [21, 57]. In boys, there has been an established link between atopic dermatitis and the development of BXO [4, 31]. With regards to other penile pathology, up to 15% of boys with hypospadias may also develop BXO [38]. Mechanical retraction of the foreskin (defined as retraction at least 5 times per month in the year preceding circumcision) was reported to increase the risk of developing BXO (OR = 5.344; 95%CI = 2.860–9.99) in a retrospective study of 297 children undergoing circumcision, although the age range and range of these boys were not stated [55].
In the past, the development of BXO was thought to be associated with infectious agents (including human papilloma virus, Epstein-Barr virus, acid-fast bacilli and spirochetes) but their role in disease development remains unproven [8, 9, 13, 19].
Under microscopic examination, histopathological changes in BXO are mostly confined to the inner mucosal surface and the mucocutaneous junction: the outer preputial area appears relatively spared [50]. The key histological characteristic in BXO is the presence of a subepidermal layer with homogenised collagen and oedema (Fig. 1). Other features include atrophy, dermoepidermal clefts and dermal bands of lymphocytes [18]. The fibrosis witnessed in BXO in boys is associated with increased levels of bone morphogenetic protein 2 (and its corresponding receptor); matrix metalloproteinases 1 and 9; tissue inhibitor of metalloproteinases 1; cytokine chemokine ligands 5 (RANTES, regulated on activation, normal T cell expressed and secreted) and interleukin 4; transforming growth factor-β2 (and its corresponding receptor); transglutaminase 2 and interferon-gamma [44, 46]. Decreased levels of transglutaminase 1, transglutaminase 3 and E-cadherin have been found in the foreskins of boys with BXO [46].
Symptoms
The signs and symptoms of BXO are summarised in Table 1. The clinical presentation of BXO can also be remembered using the 6 S mnemonic (Table 2) [40]. The key differential diagnoses for BXO include physiological phimosis, infective balanitis, lichen planus, atopic or contact dermatitis, psoriasis, erythroplasia of Queyrat (carcinoma in situ of the glans) and leukoplakia [9, 31, 34]. The average duration of symptoms appears to be about 6.5 months (range 2–48 months) [45].
Prognosis and complications
The natural course of BXO is one of the chronically progressive or relapsing episodes: spontaneous remissions appear rare [19]. Scarring of the genitals, ulceration of the glans, contraction of the frenulum and phimosis have been described [9]. This scarring and sclerosis can also lead to painful erections, urinary retention and retrograde damage to the ureters and bladder [9]. The obstructive urinary complications of BXO are rare but cause high morbidity if present. Singh et al. report on the urinary complications of 237 patients with BXO (age range from 7 to 79, mean age 37) and found that 22.5% had obstructed flow, 23.4% had acute urinary retention and 21.5% had chronic retention or overflow incontinence. They did not delineate between the rates of these complications in adults and children [49]. A literature review by Christman et al. found 7 documented cases of boys (mean age 12, range 11–13) with urinary complications of BXO, 5 had complete urinary obstruction, 1 had complete urinary obstruction with renal failure and 1 developed secondary enuresis with obstructive urinary symptoms [12].
While circumcision is considered an important element of surgical treatment for this condition, 20% of boys with confirmed BXO on histological examination receiving circumcision will require subsequent surgery for meatal stenosis [28]. This contrasts with 6% of boys who received circumcision for other penile pathology (e.g. recurrent bacterial balanitis, paraphimosis) (p < 0.05). As the prognosis is significantly different between BXO and other pathologies, this is important evidence for histological analysis of all surgically removed foreskins [28].
A rare complication of male genital BXO is the development of epithelial carcinomas in adult life [9, 19]. A recent review by Charlton et al. estimates that the rate of malignant transformation is between 3 and 8%, which is similar to the rate in vulvar LS, although the data on risk of this development in those males that acquired BXO in childhood appears limited [9]. In retrospective review of BXO biopsies from two studies, Fistarol et al. found a variety of malignancies, including squamous cell carcinoma (5.4–7%), erythroplasia of Queyrat (0.8–1%) and verrucous carcinoma (1–1.5%) [2, 19, 43]. In Barbagli et al., the mean age of diagnosis of premalignant or malignant lesions in these studies was 52 (the mean time from diagnosis of BXO to presentation of cancer was 12 years) [2]. In Nasca et al., all re-examined biopsies were from adults (average age of BXO diagnosis was 51 and the lag time to development of cancer was 17) [43].
Diagnosis and management
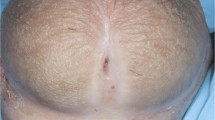
BXO may be diagnosed clinically but histological confirmation is important to rule out differential diagnoses (Table 3). Conversely, BXO may be diagnosed on histopathology in cases previously not suspected on the basis of clinical examination [7, 9, 19, 30, 35]. Typically, the boy will present with a scarred narrowing of the foreskin which has a pearly white, oedematous appearance around the opening of the foreskin with more proximal erythema. If the glans remains visible, there may also be evidence of pallor and similar thickening of the glans surface (Fig. 2). Failure to diagnose BXO can lead to further progression of the disease and recurrent unsuccessful management of meatal stenosis [6, 22].
Medical management
Whilst the most common treatment of BXO involving the foreskin is considered to be circumcision, medical treatment has been studied by several authors [20, 23, 28, 54]. Several studies have suggested medical treatment as a safe alternative to circumcision, but acknowledge that this remains controversial [20, 42]. The aims of medical treatment of BXO are to reduce scarring and atrophy and provide symptom relief, as well as prevent the occurrence of malignancy [54]. The medical treatment options include topical corticosteroids, topical immune modulators and other agents.
Topical corticosteroids
Topical corticosteroids have anti-inflammatory properties and may reverse the histologic changes in BXO [54]. It is the first-line medical treatment along with immune modulators [54]. Additionally, it is recommended to reduce voiding discomfort [27].
A double-blinded, placebo-controlled randomised study by Kiss et al. looked at 0.05% mometasone furoate ointment versus placebo in 40 boys with scarring phimosis and found that the topical steroid was effective and statistically significant (p < 0.0004) in improving symptoms [11, 32]. The authors concluded that steroids were effective in patients with mild to moderate BXO and either ineffective or slowed progression in severe disease; however, confirmation of BXO was conducted only at the end of treatment in those having a circumcision, and therefore, it is impossible to ascertain if BXO was treated in all patients.
Ghysel et al. conducted a large study of 0.05% betamethasone cream and skin stretching in 462 prepubertal boys with phimosis with follow-up at a median 22 months [23]. In the BXO subgroup (12/462), the boys were initially diagnosed clinically and confirmed to have BXO with microscopic examination if requiring circumcision: 67% of boys in the BXO subgroup (9/12) responded to treatment with 0.05% betamethasone cream and stretching after 6-week treatment [23]. The low numbers of boys with BXO treated with the steroid cream as well as the lack of a control group were limitations.
In a study of 56 boys with BXO, Vincent et al. suggested that topical corticosteroid creams were shown to be effective in patients with mild BXO; however, a variety of topical steroids (including 2.5% hydrocortisone cream and betamethasone cream of an unknown concentration) were used, making it difficult to draw solid conclusions from any one of them [56]. Additionally, these patients also did not have BXO confirmed before initiating treatment [56].
A review of 89 patients with BXO treated with topical corticosteroids across six studies (two of which were discussed in previous paragraphs) found that circumcision was avoided in 34.8% of cases [20]. However, severity of disease was not analysed comprehensively or evenly across those studies and a variety of topical steroids were used; this comparison makes it difficult to suggest which steroid was more effective. Reflecting generally across the studies, the small sample size (n = 89) and a median follow-up of only 4 months (range 6 weeks to 5 years) prevented evaluation of long-term recurrence, the development of later complications and eventual circumcision rates [20].
The use of steroids as an adjunct to surgical management has been suggested but efficacy remains unclear. In a study by of 7893 boys having surgery for BXO, Green et al. found that intralesional steroids (dose and formulation unspecified) during primary preputioplasty were associated with a reduction in requirement for subsequent circumcision (13.9% vs. 30.3%, p < 0.001), although the risk of further surgical intervention was high, with 22% requiring a circumcision for recurrent disease within a mean of 2 years following preputioplasy [24]. This result is in contrast to the findings of Pradhan et al., who showed that most of their procedures following circumcision (72.2%) occurred in patients who were treated post-operatively with topical corticosteroid creams [45]. Both studies were retrospective and did not detail the type and formulation of the steroid creams used.
The adverse effects of topical corticosteroids include skin atrophy, striae, telangiectasias, infection and suppression of the hypothalamic-pituitary axis [26]. Systemic side effects are very unlikely to occur with a short course (2–8 weeks) application of topical corticosteroids twice daily [16]. The timeline of the development of local adverse effects from applying topical steroids to the genital region is unclear [29]. The application of topical steroids to the mucosal surfaces (glans penis) is generally safe, as mucosal skin is resistant to atrophy [54].
Topical immune modulators
Topical medications such as tacrolimus or pimecrolimus have anti-inflammatory and immune-modulatory effects that can be used in the management of BXO [54]. The mechanism of action involves the inhibition of interferon-γ and interleukins 2, 4 and 10 which leads to suppression of T cell activity. Pimecrolimus 1% cream was found to be as effective as clobetasol propionate 0.05% ointment once a day in relieving symptoms: coupled with the advantage of not causing skin atrophy, these medications are second-line medical therapy for BXO [11, 54]. In Australia, topical tacrolimus remains comparatively expensive and relatively hard to access; Pimecrolimus is part of the Australian Pharmaceutical Benefits Scheme but requires an authority script and is only indicated for use under this scheme on the patient’s face or eyelid.
The adverse effects of these immune modulators include burning and stinging upon initial treatment [54]. Tacrolimus 0.1% ointment was found to be safe in a pilot study of 20 boys with BXO; none of the patients reported any burning and 4 boys (20%) reported itching that self-resolved [17]. In the United States, topical tacrolimus and pimecrolimus are labelled with a warning of potential risk of malignancy with use of these medications; this is a theoretical adverse effect based upon the oral formulation of these medications and is unlikely to occur in their topical use [36, 37].
Other medical treatments
Oral retinoids and topical hormonal medications have been described in the treatment of adult BXO, but are generally not recommended in children due to the side effect profile [13, 54].
Systemic retinoids such as etretinate, isotretinoin and acitretin are believed to work by ultimately inhibiting interleukin 6, interferon-γ and migration inhibitory factor-related protein 8, thereby reducing inflammation and cell proliferation. Their side effects include teratogenicity and thus are not approved for use in children [54].
Additionally, intralesional triamcinolone (10 mg/mL, 1–3 mL) injected at the end of preputioplasty has been proposed as an alternate treatment of BXO in a retrospective case study by Wilkinson et al. [58]. In their study, 81% of 104 patients undergoing preputioplasty and triamcinolone injection had fully retractable foreskin and no macroscopic signs of BXO at follow-up (median 14 months) [58].
Ozonated olive oil with vitamin E acetate (OZOILE® cream) was observed to reduce the upregulation of inflammatory cytokines (tumour necrosis factor-α, interleukin-1β and interferon-γ) and increase regenerative factors (hypoxia inducible factor 1-α, vascular endothelial growth factor and E-cadherin) compared to untreated controls in a study involving 30 children with BXO (mean age 9.9, range 5–15) [14].
Surgical management
Among paediatric surgeons and urologists, the definitive management of BXO in children remains circumcision [8, 9, 20, 28, 35]. In 92–100% of patients, surgical management is curative or is at least disease stabilising [12]. Patients with meatal stenosis may also require a urethroplasty or meatoplasty [9]. In the state of Victoria, Australia, the Royal Children’s Hospital Melbourne guidelines indicate that cases of pathologic phimosis (including BXO) refractory to topical corticosteroids should be referred to a paediatric surgeon for circumcision [53].
There are also drawbacks to circumcision as treatment for BXO: haemorrhage in patients receiving circumcision for BXO was higher than patients undergoing circumcision for other reasons (2.3% vs 0.3%, respectively, p < 0.0003, relative risk 6.08) [52]. It is also possible that circumcision alone does cause complete resolution of BXO. Between 20 and 47% of patients receiving circumcision for BXO require a subsequent operation for meatal pathology [27, 28]. A case study Sandler et al. described a 1-month course of twice daily hydrocortisone cream as effective in treating meatal stenosis following circumcision for BXO prior to meatal dilatation under anaesthesia [47]. Bochove-Overgaauw et al. also describe using post-operative topical corticosteroids [7].
Surgical treatment of severe meatal stenosis associated with BXO has been explored in several studies. In the experience of Green et al., the authors showed that preputioplasty was also a safe, initial option [24]. In their study, none (0%) of the 326 patients undergoing preputioplasty had any post-operative bleeding compared to 7567 boys undergoing circumcision (61, 0.8%) [24]. However, the patients undergoing preputioplasty had a higher rate of subsequent surgical procedures compared to those with complete circumcision (27.9% vs. 7.9%, p < 0.001) [24]. Buccal mucosal inlay grafts were reported to successfully treat meatal stenosis in five patients following circumcision (median age 13, range 10–17) with BXO [1]. None of those patients reported recurrence of BXO and all had improvement in urine flow [1].
Supportive management
The use of emollients, minimisation of contact with irritants (such as alkaline soaps or stale urine), treatment of infections and long-term surveillance for recurrence or development of epithelial neoplasia are recommended measures [19]. Any pruritus symptoms should be treated with antihistamines, such as diphenhydramine or hydroxyzine [5, 54]. Additionally, it is important that parents and patients be counselled and educated about the disease, its treatment and complications; intense pruritus and pain can be distressing in children and the potential development of erectile dysfunction as boys mature should also be addressed [31, 54].
Ongoing clinical review is poorly documented in the literature but is highly important; in one study, up to 47% of patients required further intervention (meatotomy or dilatation) at 11 months post-circumcision, and without follow-up, they may not have received the necessary treatment [27]. In the same study, the authors suggested that boys receiving circumcision be followed up at 3 months and discharged if voiding and appearance are normal. Patients with a scarred meatal lumen or requiring further meatoplasties should be followed up for at least 2 years [27].
Future research
Few topical corticosteroids have been studied as part of a randomised controlled study in the medical management of BXO. Apart from mometasone furoate and clobetasol propionate, it is unclear if other corticosteroids are effective for BXO and more studies could broaden the range of treatments offered for BXO [8].
There is no agreed system to classify the severity of BXO; this has made it difficult for many studies to categorise their patients into subgroups that would allow for comparison of treatment between different disease burdens [38]. In several prospective studies, a 4-grade system has been used to classify the severity of phimosis (Table 4) [28, 46]. Such a system could be further evaluated and may be correlated with the best treatment for the patient.
Conclusions
BXO is an uncommon but potentially severe disease that can cause significant morbidity in children. The general prognosis is positive in boys with prompt diagnosis and treatment, although ongoing disease and meatal stenosis remain important complications. The paucity of randomised controlled trials for the management of BXO indicates the need for further research.
Abbreviations
- BXO:
-
Balanitis xerotica obliterans
- CI:
-
Confidence interval
- LS:
-
Lichen sclerosus
- OR:
-
Odds ratio
- OZOILE® cream:
-
Ozonated olive oil with vitamin E acetate
- RANTES:
-
Regulated on activation, normal T cell expressed and secreted
References
Ashraf J, Turner A, Subramaniam R (2018) Single-stage urethroplasty with buccal mucosal inlay graft for stricture caused by balanitis xerotica obliterans in boys: Outcomes in the medium term. J Pediatr Urol 14:66.e61–66.e65
Barbagli G, Palminteri E, Mirri F, Guazzoni G, Turini D, Lazzeri M (2006) Penile Carcinoma in Patients With Genital Lichen Sclerosus: A Multicenter Survey. J Urol 175:1359–1363
Becker K (2011) Lichen sclerosus in boys. Dtsch Arztebl Int 108:53–58
Becker K, Meissner V, Farwick W, Bauer R, Gaiser MR (2013) Lichen sclerosus and atopy in boys: coincidence or correlation? Br J Dermatol 168:362–366
Bercaw-Pratt JL, Boardman LA, Simms-Cendan JS (2014) Clinical recommendation: pediatric lichen sclerosus. J Pediatr Adolesc Gynecol 27:111–116
Beuke M, Riechardt S, Fisch M (2007) Complications after Surgery of the External Genitalia in Children with Lichen Sclerosus (BXO). J Pediatr Urol 3:S36
Bochove-Overgaauw DM, Gelders W, De Vylder AM (2009) Routine biopsies in pediatric circumcision: (non) sense? J Pediatr Urol 5:178–180
Celis S, Reed F, Murphy F, Adams S, Gillick J, Abdelhafeez AH, Lopez P-J (2014) Balanitis xerotica obliterans in children and adolescents: a literature review and clinical series. J Pediatr Urol 10:34–39
Charlton OA, Smith SD (2018) Balanitis xerotica obliterans: a review of diagnosis and management. Int J Dermatol 58:777–781
Chernosky ME, Derbes VJ, Burks JW (1957) Lichen sclerosus et atrophicus in children. Arch Dermatol 75:647–652
Chi C-C, Kirtschig G, Baldo M, Lewis F, Wang S-H, Wojnarowska F (2012) Systematic review and meta-analysis of randomized controlled trials on topical interventions for genital lichen sclerosus. J Am Acad Dermatol 67:305–312
Christman MS, Chen J, Holmes N (2009) Obstructive complications of lichen sclerosus. J Pediatr Urol 5:165–169
Clouston D, Hall A, Lawrentschuk N (2011) Penile lichen sclerosus (balanitis xerotica obliterans). BJU Int 108:14–19
Curro M, Russo T, Ferlazzo N, Caccamo D, Antonuccio P, Arena S, Parisi S, Perrone P, Ientile R, Romeo C, Impellizzeri P (2018) Anti-Inflammatory and Tissue Regenerative Effects of Topical Treatment with Ozonated Olive Oil/Vitamin E Acetate in Balanitis Xerotica Obliterans. Molecules 23:645
Depasquale I, Park AJ, Bracka A (2000) The treatment of balanitis xerotica obliterans. BJU Int 86:459–465
Drake T, Rustom J, Davies M (2013) Phimosis in childhood. BMJ 346:f3678
Ebert AK, Rosch WH, Vogt T (2008) Safety and tolerability of adjuvant topical tacrolimus treatment in boys with lichen sclerosus: a prospective phase 2 study. Eur Urol 54:932–937
Fischer G (1995) Lichen sclerosus in childhood. Australas J Dermatol 36:166–167
Fistarol S, Itin P (2013) Diagnosis and Treatment of Lichen Sclerosus. Am J Clin Dermatol 14:27–47
Folaranmi SE, Corbett HJ, Losty PD (2017) Does application of topical steorids for lichen sclerosus (balanitis xerotica obliterans) affect the rate of circumcision? A systematic review. J Pediatr Surg 53:2225–2227
Fuchs ME, Beecroft N, Dajusta DG, McLeod DJ (2017) The Association Between BXO and Obesity in Boys Undergoing Circumcision. Global Pediatr Health 4:2333794x17742749
Gargollo PC, Kozakewich HP, Bauer SB, Borer JG, Peters CA, Retik AB, Diamond DA (2005) Balanitis xerotica obliterans in boys. J Urol 174:1409–1412
Ghysel C, Vander Eeckt K, Bogaert GA (2009) Long-Term Efficiency of Skin Stretching and a Topical Corticoid Cream Application for Unretractable Foreskin and Phimosis in Prepubertal Boys. Urol Int 82:81–88
Green PA, Bethell GS, Wilkinson DJ, Kenny SE, Corbett HJ (2019) Surgical management of genitourinary lichen sclerosus et atrophicus in boys in England: A 10-year review of practices and outcomes. J Pediatr Urol 15:45.e41–45.e45
Hartley A, Ramanathan C, Siddiqui H (2011) The surgical treatment of Balanitis Xerotica Obliterans. Indian J Plast Surg 44:91–97
Hengge UR, Ruzicka T, Schwartz RA, Cork MJ (2006) Adverse effects of topical glucocorticosteroids. J Am Acad Dermatol 54:1–15
Holbrook C, Tsang T (2011) Management of boys with abnormal appearance of meatus at circumcision for balanitis xerotica obliterans. Ann R Coll Surg Engl 93:482–484
Homer L, Buchanan KJ, Nasr B, Losty PD, Corbett HJ (2014) Meatal stenosis in boys following circumcision for lichen sclerosus (balanitis xerotica obliterans). J Urol 192:1784–1788
Howard M, Hall A (2018) Treatment of penile lichen sclerosus with topical corticosteroids for over 25 years' duration: A case report. SAGE Open Med Case Rep 6:2050313X18795047-12050313X18795047
Jayakumar S, Antao B, Bevington O, Furness P, Ninan GK (2012) Balanitis xerotica obliterans in children and its incidence under the age of 5 years. J Pediatr Urol 8:272–275
Kirtschig G (2016) Lichen sclerosus - Presentation, diagnosis and management. Dtsch Arztebl Int 113:337–343
Kiss A, Csontai A, Pirót L, Nyirády P, Merksz M, Király L (2001) The response of balanitis xerotica obliterans to local steroid application compared with placebo in children. J Urol 165:219–220
Kiss A, Király L, Kutasy B, Merksz M (2005) High Incidence of Balanitis Xerotica Obliterans in Boys with Phimosis: Prospective 10-Year Study. Pediatr Dermatol 22:305–308
Kizer SW, Prarie FT, Morey FA (2003) Balanitis Xerotica Obliterans: Epidemiologic Distribution in an Equal Access Health Care System. South Med J 96:9–11
Kuehhas FE, Miernik A, Weibl P, Schoenthaler M, Sevcenco S, Schauer I, Tosev G, Oezsoy M, Lassmann J (2013) Incidence of Balanitis Xerotica Obliterans in Boys Younger than 10 Years Presenting with Phimosis. Urol Int 90:439–442
Legendre L, Barnetche T, Mazereeuw-Hautier J, Meyer N, Murrell D, Paul C (2015) Risk of lymphoma in patients with atopic dermatitis and the role of topical treatment: A systematic review and meta-analysis. J Am Acad Dermatol 72:992–1002
Margolis DJ, Abuabara K, Hoffstad OJ, Wan J, Raimondo D, Bilker WB (2015) Association Between Malignancy and Topical Use of Pimecrolimus. JAMA Dermatol 151:594–599
Mattioli G, Repetto P, Carlini C, Granata C, Gambini C, Jasonni V (2002) Lichen sclerosus et atrophicus in children with phimosis and hypospadias. Pediatr Surg Int 18:273–275
McLelland J (2004) Lichen sclerosus in children. J Obstet Gynaecol 24:733–735
Meuli M, Briner J, Hanimann B, Sacher P (1994) Lichen sclerosus et atrophicus causing phimosis in boys: a prospective study with 5-year followup after complete circumcision. J Urol 152:987–989
Mohammed A, Shegil IS, Christou D, Khan A, Barua JM (2012) Paediatric balanitis xerotica obliterans: an 8-year experience. Arch Ital Urol Androl 84:12–16
Moreno G, Corbalán J, Peñaloza B, Pantoja T (2014) Topical corticosteroids for treating phimosis in boys. Cochrane Database Syst Rev 2:CD008973
Nasca MR, Innocenzi D, Micali G (1999) Penile cancer among patients with genital lichen sclerosus. J Am Acad Derm 41(6):911–914
Pilatz A, Altinkilic B, Schormann E, Maegel L, Izykowski N, Becker J, Weidner W, Kreipe H, Jonigk D (2013) Congenital phimosis in patients with and without lichen sclerosus: distinct expression patterns of tissue remodeling associated genes. J Urol 189:268–274
Pradhan A, Patel R, Said AJ, Upadhyaya M (2019) 10 Years’ Experience in Balanitis Xerotica Obliterans: A Single-Institution Study. Eur J Pediatr Surg 29:302–306
Russo T, Curro M, Barbera A, Caccamo D, Antonuccio P, Arena S, Montalto AS, Parisi S, Marseglia L, Gitto E, Ientile R, Impellizzeri P, Romeo C (2016) Expression of Transglutaminase in Foreskin of Children with Balanitis Xerotica Obliterans. Int J Mol Sci 17:1551
Sandler G, Patrick E, Cass D (2008) Long standing balanitis xerotica obliterans resulting in renal impairment in a child. Pediatr Surg Int 24:961–964
Shankar R (1999) The incidence of phimosis in boys. BJU Int 84:101–102
Singh J, Priyadarshi V, Goel H, Vijay M, Pal D, Chakraborty S, Kundu A (2015) Penile lichen sclerosus: An urologist's nightmare! - A single center experience. Urol Ann 7:303–308
Singh L, Sengar M, Goyal S, Mansi M, Khurana N, Mohta A (2018) Childhood Phimosis Secondary to Lichen Sclerosus: Is There a Spatial Pattern of Histopathological Changes? Am J Dermatopathol 40:824–828
Sneppen I, Thorup J (2016) Foreskin Morbidity in Uncircumcised Males. Pediatrics 137:e20154340
Somov P, Chan B, Wilde C, Corbett H (2017) Bleeding after circumcision is more likely in children with lichen sclerosus (balanitis xerotica obliterans). J Pediatr Urol 13:208.e1–208.e4
The Royal Children’s Hospital Melbourne (2018) The penis and foreskin. https://www.rch.org.au/clinicalguide/guideline_index/The_penis_and_foreskin/. Accessed 28/5/2019
Tong LX, Sun GS, Teng JMC (2015) Pediatric Lichen Sclerosus: A Review of the Epidemiology and Treatment Options. Pediatr Dermatol 32:593–599
Villa M, Dragonetti E, Grande M, Bove P, Sansalone S, Rulli F, Tambucci R, Tucci G, Baldi A (2012) Skin phototype and local trauma in the onset of balanitis xerotica obliterans (BXO) in circumcised patients. In Vivo 26:143–146
Vincent MV, MacKinnon E (2005) The response of clinical balanitis xerotica obliterans to the application of topical steroid-based creams. J Pediatr Surg 40:709–712
Virgili A, Borghi A, Cazzaniga S, Di Landro A, Naldi L, Minghetti S, Verrone A, Stroppiana E, Caproni M, Nasca MR, D’Antuono A, Papini M, Di Lernia V, Corazza M (2017) New insights into potential risk factors and associations in genital lichen sclerosus: Data from a multicentre Italian study on 729 consecutive cases. J Eur Acad Dermatol Venereol 31:699–704
Wilkinson DJ, Lansdale N, Everitt LH, Marven SS, Walker J, Shawis RN, Roberts JP, Mackinnon AE, Godbole PP (2012) Foreskin preputioplasty and intralesional triamcinolone: a valid alternative to circumcision for balanitis xerotica obliterans. J Pediatr Surg 47:756–759
Acknowledgements
The authors would like to thank Dr Jack Garland from the Department of Anatomical Pathology at Liverpool Hospital, NSW, Australia, for his assistance with the histological slide.
Author information
Authors and Affiliations
Contributions
Alexander T M Nguyen - Literature search, Drafting of manuscript, Final approval of manuscript.
Andrew J A Holland - Concept for article, Literature search, Critical revision of article, Final approval of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Communicated by Piet Leroy
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nguyen, A.T.M., Holland, A.J.A. Balanitis xerotica obliterans: an update for clinicians. Eur J Pediatr 179, 9–16 (2020). https://doi.org/10.1007/s00431-019-03516-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-019-03516-3