Abstract
Natural killer (NK) cells provide important host defense against herpesvirus infections and influence subsequent T cell control of replication and maintenance of latency. NK cells exhibit phases of expansion, contraction and memory formation in response to the natural mouse pathogen murine cytomegalovirus (MCMV). Innate and adaptive immune responses are tightly regulated in mammals to avoid excess tissue damage while preventing acute and chronic viral disease and assuring resistance to reinfection. Caspase (CASP)8 is an autoactivating aspartate-specific cysteine protease that initiates extrinsic apoptosis and prevents receptor interacting protein (RIP) kinase (RIPK)1–RIPK3-driven necroptosis. CASP8 also promotes death-independent signal transduction. All of these activities make contributions to inflammation. Here, we demonstrate that CASP8 restricts NK cell expansion during MCMV infection but does not influence NK memory. Casp8−/−Ripk3−/− mice mount higher NK response levels than Casp8+/−Ripk3−/− littermate controls or WT C57BL/6 J mice, indicating that RIPK3 deficiency alone does not contribute to NK response patterns. MCMV m157-responsive Ly49H+ NK cells support increased expansion of both Ly49H− NK cells and CD8 T cells in Casp8−/−Ripk3−/− mice. Surprisingly, hyperaccumulation of NK cells depends on the pronecrotic kinase RIPK1. Ripk1−/−Casp8−/−Ripk3−/− mice fail to show the enhanced expansion of lymphocytes observed in Casp8−/−Ripk3−/− mice even though development and homeostasis are preserved in uninfected Ripk1−/−Casp8−/−Ripk3−/− mice. Thus, CASP8 naturally regulates the magnitude of NK cell responses in response to infection where strong activation signals depend on another key regulator of death signaling, RIPK1. In addition, the strong NK cell response promotes survival of effector CD8 T cells during their expansion. Thus, hyperaccumulation of NK cells and crosstalk with T cells becomes amplified in the absence of extrinsic cell death machinery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
NK cells are innate lymphocytes that contribute to early control of virus infections. NK-dependent antiviral responses develop rapidly and exhibit robust cytotoxicity [1]. Activation depends on receptors that override inhibitory signals and trigger NK cell expansion, contraction, memory formation [2]. Murine cytomegalovirus (MCMV) has yielded invaluable insights into antiviral NK cell function due to the ability of virus-encoded MHC class I-like glycoprotein m157 to specifically engage host Ly49H, an activating receptor mediating robust proliferation and strong cytotoxic effector responses [3] that dictate early control over MCMV [4, 5]. Following peak expansion, most Ly49H+ NK cells contract to leave a memory-like population that persists [6] in a manner reminiscent of the adaptive T cell response. Human (H)CMV-infected individuals have higher persistent levels of CD94+NKG2C+ NK cells compared to seronegative individuals [7, 8], suggesting that NK cell memory also follows HCMV infection. Given that comparable patterns of memory have been observed in humans [9] and mice [6], MCMV-infected mice help to provide mechanistic insights into memory NK cell generation.
In addition to the Ly49H receptor, NK cell expansion depends on proinflammatory cytokines and costimulatory receptors. IL-12, IL-18, IL-33 and type I IFNs regulate NK cell proliferation, cytotoxic function and memory formation [10]. IL-12-triggered, STAT4-dependent signal transduction upregulates MyD88 and consequent expression of the IL-18 receptor to promote NK cell proliferation [11]. Type I IFN-induced transcription factors STAT1, STAT2, IRF8 and IRF9 all contribute to NK cell survival during expansion [12,13,14]. In addition, both IL-12 and type I IFN promote NK cell cytotoxic function and IFNγ production [15, 16]. Signaling through NKG2D augments m157-dependent Ly49H+ NK proliferation, although stimulation via NKG2D alone is not sufficient to trigger NK cell expansion [17]. All of these factors contribute to the levels, differentiation programs and longevity of NK cells, which is mediated by the balance of proliferation and death.
Lymphocyte turnover and cell death occur primarily via cell-intrinsic apoptosis, mediated by Bcl2 family member Bim acting upstream of Bax- and Bak-dependent mitochondrial outer membrane permealization (MOMP) and release of cytochrome c [18, 19]. Similar to its role in antiviral T cell contraction, Bim functions during Ly49H+ NK cell contraction and formation of a memory pool [20, 21]. Extrinsic cell death is activated by cell-surface TNF receptor superfamily death receptors (DRs, including Fas, as well as TNFR1 and TRAIL) that drive cytosolic events resulting in death-dependent (apoptotic, necroptotic) and death-independent signaling outcomes [22,23,24,25]. Fas death receptor-mediated signaling and Bid amplification of signals [19] contribute to T cell homeostatic turnover [25]. Fas also contributes to contraction following herpesvirus infection [26]. We have recently shown that CASP8-dependent extrinsic apoptosis is dispensable for NK or T cell contraction during MCMV or HSV1 infection of viable and immunocompetent Casp8−/−Ripk3−/− mice [27, 28], a topic that is elaborated in the accompanying review. Our data are consistent with the predominant role of the intrinsic pathway in the shutdown of acute NK cell responses following clearance of viral antigens.
CASP8 was initially believed to support lymphocyte activation due to defective NF-κB signaling via CD244 (or 2B4) and CD16 in mice with T cell-specific deficiency [29, 30], events likely to result from the vital role that CASP8 plays in suppressing RIPK3-mediated necroptosis [31]. Our recent study of Casp8−/−Ripk3−/− mice reveals that the Ly49H+ NK cell expansion peaks higher compared to either Casp8+/−Ripk3−/− or WT C57BL/6 J controls during the acute phase of MCMV infection [27], indicating that CASP8 restricts Ly49H+ NK cell expansion in a necroptosis-deficient background. However, the interpretation of these results is complicated by other environmental considerations, including viral antigen load as well as the abnormal B220+CD3+ T cell accumulation [27, 31] and enhanced DCs numbers that accompany MCMV infection in Casp8−/−Ripk3−/− mice [27].
In this study, we show that CASP8 restricts Ly49H+ NK cell accumulation as well as effector differentiation but is dispensable for memory NK cell development. While our previous study has shown that Ly49H+ NK cell hyperaccumulation in Casp8−/−Ripk3−/− mice requires m157 MCMV antigen, data from the current work show that enhancement requires active virus replication. Further, using a co-transfer system, it appears that CASP8 makes a cell-autonomous contribution to restricting NK cell expansion. Strikingly, RIPK1 elimination in Casp8−/−Ripk3−/− mice completely ablates NK cell responses, although Ripk1−/−Casp8−/−Ripk3−/− mice exhibit normal homeostatic NK cell development [32]. Finally, Casp8−/−Ripk3−/− NK cells support robust memory development that results in normal levels of CD11bloCD27+ and higher percentages of Ly6C+ and KLRG1hi subsets when compared with WT mice.
Materials and methods
Mice, viruses and experimental infection
Casp8−/−Ripk3−/− [31] and Casp8−/−Ripk3K51A/K51A [33] mice were > 97% C57BL/6 J. Casp8−/−Ripk3−/− and Casp8+/−Ripk3−/− littermates were generated by mating Casp8−/−Ripk3−/− and Casp8+/−Ripk3−/− mice. Ripk1−/−Casp8−/−Ripk3−/− mice were generated as described previously [32]. C57BL/6 J mice were obtained from The Jackson Laboratory, used for backcrossing and bred at Emory University Division of Animal Resources. K181-BAC-derived WT virus and K181-BAC-derived ∆m157, kindly provided by Wolfram Brune (Heinrich Pette Institute), were propagated in NIH3T3 fibroblasts. Mice were inoculated intraperitoneally with 1 × 106 PFU virus per mouse. The cell culture medium was purified and concentrated for virus stock preparation, which were stored in single-use aliquots at − 80 °C until use.
Plaque assay
Homogenized tissue in DMEM medium was overlaid on NIH3T3 cells plated in 6-well plates. On day 4 post infection, cells were fixed with methanol and stained with Giemsa for visualizing plaques that were counted with the aid of a dissecting microscope.
Antibodies
For flow cytometry, antibodies to CD16/CD32 (FcγRII/III; Clone 2.4G2), CD45 (Clone 30-F11), CD45.1 (Clone A20), CD45.2 (Clone 104), CD11b (Clone M1/70), NK1.1 (Clone PK136), B220 (Clone RA3-6B2), CD3ε (Clone 17A2), CD3ε (Clone 145-2C11), CD8 (Clone 53–6.7), KLRG1 (Clone 2F1), Ki67 (Clone SolA15) were from BD PharMingen; and CD3ε (Clone 17A2) were from BioLegend; and Ly49H (Clone 3D10) was from eBioscience. For Annexin V analysis, splenocytes harvested from mice were stained with Annexin V (BD Bioscience).
Flow cytometry
Spleens were harvested from euthanized mice, and were pressed through metal sieves for organ disruption. Cells were then incubated with red blood cell lysis buffer and then passed through a 100-mm strainer. In all experiments, 2 × 106 viable cells, as determined by trypan blue exclusion, were stained with antibodies specific for surface and intracellular proteins and were prepared for detection by flow cytometry (BD LSRII cytometer and FACSDiva Software; BD Biosciences). Data were analyzed with FlowJo (TreeStar), and graphed with Prism 7 (GraphPad).
Results
MCMV-infected mice deficient in CASP8 and RIPK3 show enhanced Ly49H+ NK cell accumulation compared to controls [27]. Thus, similar to the cell-autonomous impact on CD8 T cells [27, 28], CASP8 naturally restricts Ly49H+ NK cell expansion, once unleashed necroptosis has been eliminated from the host. To determine whether enhancement was Ly49H+ NK cell specific, the time course of Ly49H+ and Ly49H− NK cell expansion was determined. Splenocytes from Casp8−/−Ripk3−/−, Casp8+/−Ripk3−/− and WT mice were collected at various times following MCMV infection, and NK cell number and phenotype were assessed. Total NK cell numbers were comparable in all groups on days 1.5, 3 and 5 post MCMV infection (Fig. 1a), but expanded to peak levels at 7 dpi that were dramatically higher in Casp8−/−Ripk3−/− mice relative to controls. A similar pattern of contraction occurred in all mice from 9 to 14 dpi. The data suggest that CASP8 restricts NK cell numbers during the expansion phase but is dispensable for cell contraction, a pattern that has been observed with antiviral CD8 T cells in these mice [28]. Numbers of MCMV m157-driven Ly49H+ NK cells [3] increased to significantly higher levels by 7 dpi in Casp8−/−Ripk3−/− mice, as expected [27] (Fig. 1b); whereas, the numbers of Ly49H− NK cells remained generally comparable independent of genotype over the two-week observation period (Fig. 1c). Consistent with the cell count analysis, percentages of Ly49H+ NK cells were significantly higher in Casp8−/−Ripk3−/− mice at 7 dpi compared to WT and Casp8+/−Ripk3−/− controls, while levels were comparable at 1.5 dpi independent of genotype (Fig. 1d). To further investigate whether Casp8 regulates cells through a cell-autonomous or cell-extrinsic mechanism, equal numbers of CD45.1+ WT and CD45.2+ DKO NK cells were cotransferred into Ly49H-deficient mice. Expansion and contraction of Ly49H+ NK cells were measured in peripheral blood following MCMV infection. DKO cells exhibited increased expansion with a peak that was higher than WT controls (Fig. 2a). Following the peak NK cell response, Ly49H+ NK cells from both genotypes contracted between days 14 and 28 post infection. Consistent with the enhanced accumulation, DKO cells made up the majority of the total Ly49H+ population throughout the infection (Fig. 2b). These data show that Casp8 mediates an NK cell-autonomous restriction of expansion but is dispensable for contraction.
NK cell expansion, contraction, and differentiation during the acute phase of MCMV infection. 6–8-week-old C57BL/6 (WT), Casp8+/−Ripk3−/− (HET) and Casp8−/−Ripk3−/− (DKO) mice [31] were inoculated intraperitoneally (i.p.) with 1 × 106 PFU MCMV K181-BAC per mouse. Spleens were processed at 1.5, 3, 5, 7, 9 and 14 days post infection (dpi) and stained with antibodies specific for the indicated cell-surface markers. Splenic CD45+B220−CD3−NK1.1+ NK cells were gated to identify Ly49H+ and Ly49H− NK cells. Graphs comparing numbers of total (a), Ly49H+ (b), and Ly49H− (c) NK cells. Data are presented as mean numbers ± S.E.M. Representative flow plots comparing the frequencies of Ly49H+ subset out of total NK cells (d). Representative histograms showing the frequencies of Ly49H+ NK cells expressing KLRG1 (e). C57BL/6 mice were from The Jackson Laboratory and maintained at Emory University Division of Animal Resources, and experimental procedures were conducted in accordance with the National Institutes of Health and Emory University Institutional Animal Care and Use Committee guidelines; K181-BAC virus strain was propagated in NIH3T3 cells, purified and concentrated from clarified cell culture medium; flow cytometry and antibodies (Abs) have been described [28]. Data represent at least two independent experiments using n = 5 mice per group. Significant differences between DKO and WT (*) or HET (#) mice are indicated as **p < 0.01; *** or ###p < 0.001; **** or ####p < 0.0001
Cell-autonomous impact of CASP8 on NK cell expansion and contraction during the acute phase of MCMV infection. Equal numbers (106) of the purified TCRβ−NK1.1+ cells from naïve CD45.1+ WT mice and CD45.2+ DKO mice were mixed (1:1) and co-transferred into Ly49H-deficient recipients, followed with MCMV infection the next day. Graph showing the percentages ± S.E.M. of Ly49H+ cells in blood on days 0, 7, 14, and 28 post infection (a). Representative plots showing the ratios of WT and DKO Ly49H+ NK cells in blood of the recipients on the indicated days post infection (b). Data represent one experiment with n = 3 mice per group
Upon infection, all three genotypes upregulated KLRG1 on Ly49H+ NK cells, suggesting that maturation occurs independently of CASP8 or RIPK3 (Fig. 1e). However, a higher proportion of Casp8−/−Ripk3−/− Ly49H+ NK cells upregulated KLRG1 at 7 dpi, again reminiscent of responding CD8 T cells in these mice [28]. Taken together, CASP8 appears to restrict m157-specific Ly49H+ NK cell accumulation following MCMV infection without playing a role in contraction.
Expansion of NK cells during antiviral prophylaxis
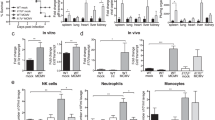
Next, we sought to investigate whether the NK cell response pattern depended on MCMV antigen levels. Differences between Casp8-deficient mice and controls do not result from differential viral replication levels or clearance [27, 28]. Infected mice were treated with cidofovir (CDV) to inhibit virus replication, conditions where T cell expansion patterns were preserved [28]. NK cell responses were investigated at 7 dpi where CDV effectively suppressed viral load to undetectable levels in these mice [28]. Compromised replication, which would be expected to reduce m157 levels markedly, did not impact total or Ly49H+ NK cell responses, but reversed the heightened numbers in Casp8−/−Ripk3−/− mice (Fig. 3a). Interestingly, numbers of Ly49H+ cells in CDV-treated Casp8−/−Ripk3−/− mice actually trended lower than in controls (Fig. 3b) which was reflected in reduced percentages as well (Fig. 3c). CDV-compromised virus levels reduced the levels of NK cell differentiation and percentages of KLRG1hi Ly49H+ NK cells, regardless of genotype (Fig. 3d). Nevertheless, independent of CDV treatment, Casp8−/−Ripk3−/− mice exhibited higher percentages of KLRG1hi Ly49H+ NK cells than control mice. These data show that the enhancement of Ly49H+ NK cell number in Casp8−/−Ripk3−/− mice requires active replication, although CASP8 suppresses NK cell differentiation independent of antigen load.
Patterns of NK cell responses during antigen level compromise. Mice were administered 5 mg/kg/day CDV i.p. in PBS, starting from 3 day prior to infection with MCMV as described in Fig. 2 and previously [28]. All groups were euthanized and splenocytes were analyzed at 7 dpi. Bar graphs comparing the numbers of total (a) and Ly49H+ (b) NK cells. Data are presented as mean ± S.E.M. Representative flow plots showing the percentages of Ly49H+ cells within the total NK population (c). Representative histograms showing the percentage of Ly49H+ NK cells expressing KLRG1 (d). Data represent two independent experiments with n = 4 mice per group
NK hyperaccumulation in different CASP8-deficient settings
To investigate whether Ly49H+ NK cell hyperaccumulation occurs with another necroptosis incompetent, CASP8-deficient strain, NK cells in Casp8−/−Ripk3K51A/K51A mice, where the kinase activity has been specifically disrupted [33], were compared to Casp8−/−Ripk3−/− as well as WT controls. The enhancement of NK cells was observed consistently in either CASP8-deficient setting due to the activation of Ly49H+ cells (Fig. 4). Finally, RIPK1 is a death domain-containing pro-necroptotic kinase involved in regulating apoptosis and pro-survival signaling transduction as a component of the ripoptosome [25]. To understand whether RIPK1 contributed to Ly49H+ NK cell responses, Ripk1−/−Casp8−/−Ripk3−/− mice were infected, and splenocytes were analyzed at 7 dpi. Interestingly, total and Ly49H+ NK cell responses were severely impaired in mice lacking RIPK1 at 7 dpi (Fig. 4), even though uninfected mice exhibit normal NK cell development [32] and homeostasis [27]. This does not appear to be an NK cell-intrinsic dysregulation because similar impairment occurs with CD8 T cells (data not shown), indicating that RIPK1 contributes to lymphocyte response properties in the absence of CASP8 function. Thus, CASP8 restricts NK cell accumulation during MCMV infection; however, RIPK1 supports hyperaccumulation when CASP8 and RIPK3 are absent.
Assessment of NK cell responses in another CASP8-deficienct strain and the contribution of RIPK1 to the response. WT, DKO, Casp8–/−Ripk3K51A/K51A (C8−/−R3K51A; [33]) and Ripk1−/−Casp8−/−Ripk3−/− (TKO, [32]) mice were infected with MCMV as described in Fig. 2. Bar graphs comparing the mean numbers ± S.E.M. of the splenic total (a), Ly49H+ (b), and Ly49H− (c) NK cells at 7 dpi. Representative flow plots showing the percentages of CD45+CD3−B220− cells expressing NK1.1 (d) or Ly49H (e). Combined data of n = 7 mice from two independent experiments are shown
Hyperaccumulation of NK cells requires m157–Ly49H interactions
In C57BL/6 mice, only NK cells express the Ly49H receptor and only Ly49H+ NK cells respond directly to the viral m157-encoded glycoprotein [4, 5]. Ly49H− NK cells are stimulated indirectly, although Ly49H+ NK cells are the drivers [3, 34] such that proliferation and cytotoxicity do not develop to a demonstrable level during infection with ∆m157 MCMV [10]. Infection with ∆m157 virus failed to drive hyperaccumulation (Fig. 5a) in Casp8−/−Ripk3−/− mice, which showed kinetics distinct from WT MCMV, but comparable to either Casp8+/−Ripk3−/− or WT mice. Thus, the increased accumulation is totally dependent on m157, consistent with data showing Ly49H+ NK cell hyperaccumulation in MCMV-infected Casp8−/−Ripk3−/− mice (See Fig. 1).
Impact of m157-driven NK cells on antiviral CD8 T cell responses in DKO mice. WT, HET and DKO mice were inoculated i.p. with 1 × 106 PFU/mouse of K181-BAC or ∆m157 virus and mean numbers ± S.E.M. of Ly49H+ NK cells were determined in spleens on days 1.5, 5, 7, and 14 pi (a). Expansion, contraction, and phenotype of splenic CD8 T cell response to infection, showing mean numbers ± S.E.M. of total CD8 T cells (b) as well as numbers (c) and percentages (d) of M45-specific cells on days 5, 7, and 14 post infection. Bar graphs comparing numbers ± S.E.M. of different effector subsets (e, left panel) and representative zebra plots showing KLRG1 and CD127 expression (e, right panel) following gating on M45-specific CD8 T cells at 7 dpi. Cell death analysis on day 7 post infection with K181-BAC or ∆m157 virus, comparing mean frequencies of FVS+ dead cells in spleens of WT and DKO mice (f), mean percentages of annexin V+ cells within CD8 T cell subset (g) when FVS+ dead cells were excluded from this analysis. Data are presented as mean ± S.E.M. and represent two independent experiments with n ≥ 4 mice per group
NK cell hyperaccumulation dictates survival of antiviral CD8 T cells
∆m157 MCMV has yielded invaluable insights into positive and negative impacts of NK cell function on CD8 T cell responses [35,36,37,38]. In addition to the striking impact on NK cell hyperaccumulation, both total (Fig. 5b) and M45-specific (Fig. 5c, d) CD8 T cell responses returned to control levels during ∆m157 MCMV infection of Casp8−/−Ripk3−/− mice. KLRG1hiCD127lo and KLRG1hiCD127hi effector subsets failed to hyperaccumulate (Fig. 5e). ∆m157 virus infection resulted in higher frequencies of fixable viability staining (FVS+) dead cells in spleens of Casp8−/−Ripk3−/− mice at 7 dpi compared to m157-expressing K181-BAC virus (Fig. 5f), suggesting that the Ly49H+ NK cell response supported Casp8−/−Ripk3−/− splenocyte survival. Casp8−/−Ripk3−/− mice exhibited higher frequencies of annexin V+Casp8−/−Ripk3−/− CD8 T cell subsets (Fig. 5g), suggesting that greater numbers of T cells underwent apoptosis in Casp8−/−Ripk3−/− mice when the Ly49H+ NK cell response was compromised. Overall, these experiments implicate the m157-driven Ly49H+ NK response in supporting Casp8−/−Ripk3−/− T cell survival as they hyperaccumulate following MCMV infection.
To determine whether NK cell-autonomous CASP8 and RIPK3 contributed to Casp8−/−Ripk3−/− CD8 T cell accumulation, CFSE-labeled total CD45.2+ WT or Casp8−/−Ripk3−/− splenocytes that contained 106 CD8 T cells were transferred into congenic CD45.1+ recipients, followed by infection with K181-BAC or ∆m157 virus 24 h later (Fig. 6a). The numbers of endogenous CD45.1+ Ly49H+ NK cells were comparable in all K181-BAC-infected recipients but were compromised during infection with ∆m157 virus (Fig. 6b). The numbers of responding Ly49H+ NK cells appeared to be generated independent of the donor cell genotype. Strikingly, hyperaccumulation of total and M45-specific Casp8−/−Ripk3−/− CD8 T cells was compromised in ∆m157 virus-infected mice (Fig. 6c), indicating that WT Ly49H+ NK cells sufficed to enhance Casp8−/−Ripk3−/− CD8 T cell accumulation. Cell proliferation assessment by CFSE dilution revealed that the m157-driven Ly49H+ NK cell response did not have an impact on Casp8−/−Ripk3−/− CD8 T cell proliferation (Fig. 6d), reinforcing the CD8 T cell-intrinsic underpinnings of hyperaccumulation [28]. Altogether, Ly49H+ NK cells have an impact independent of CASP8 and RIPK3 on Casp8−/−Ripk3−/− CD8 T cell proliferative potential following MCMV infection, by supporting the survival of Casp8−/−Ripk3−/− CD8 T cells.
Impact of WT m157-driven NK cells on antiviral DKO CD8 T cell responses. CFSE-labeled total splenocytes containing 1 × 106 NK cells from naive WT (CD45.2+) or DKO mice (CD45.2+) mice were transferred into CD45.1+ WT mice, followed with infection of 1 × 106 PFU/mouse K181-BAC or ∆m157 the next day followed by flow cytometric evaluation of splenocytes at 6 dpi (a). Numbers of endogenous CD45.1+ Ly49H+ NK cells in the recipients (b). Bar graphs comparing numbers of donor CD45.2+ total CD8 T cells, and numbers as well as percentages of CD45.2+ M45-specific cells (c). Bar graphs showing the percentages of CFSElo divided cells within the transferred donor CD45.2+ CD8 T cells in the recipients (d)
Cytokines, together with m157-driven Ly49H receptor signaling, contribute to memory NK cell formation after contraction [10]. Memory NK cells express high levels of markers related to differentiation and maturation [6]. We sought to investigate whether the heightened acute response of CASP8-deficient NK cells altered memory formation. NK cell numbers and memory cell differentiation markers were assessed in WT, Casp8−/−Ripk3−/− and Casp8−/−Ripk3K51A/K51A mice at 8 wpi. Both CASP8-deficient mutants exhibited lower numbers and percentages of Ly49H+ NK cells than WT controls (Fig. 7), despite hyperaccumulation during the acute phase of infection. Enhanced percentages of KLRG1hi Ly49H+ NK cells were observed in both CASP8-deficient settings when compared with controls. The proportion of Ly6C+ NK cells was comparable regardless of genotype, suggesting that robust memory NK cell development is independent of CASP8 or RIPK3 function. Consistent with this observation, over 90% of the cells had a mature NK cell phenotype of CD27loCD11bhi regardless of genotype. Thus, CASP8 is dispensable for memory NK cell formation, where Bim control of intrinsic apoptosis likely plays the central role [20]. The amplified Ly49H+ NK cell response and pattern of enhanced terminal differentiation do not lead to better viral control [27], again indicating that the quality of Casp8−/−Ripk3−/− NK cells may be compromised in some ways.
Phenotype of NK cells in long-term-infected CASP8-deficient mice. WT, DKO, C8−/−R3K51A mice were infected and splenocytes were analyzed at 60 dpi. Bar graphs comparing the numbers (a) and percentages (b) of Ly49H+ NK cells. Graphs comparing the percentages of KLRG1hi (c) and Ly6Chi (d) cells within the Ly49H+ NK population. Representative flow plots depicting CD27 versus CD11b expression on the NK cell subset (e). Data are presented as mean ± S.E.M. and represent one experiment with mice n = 5 in each group
Discussion
Recent studies have highlighted the adaptive immune features of NK cells in mice, humans, and nonhuman primates [2, 39]. Like the virus-specific CD8 T cell proliferation, signals through Ly49H receptor, cytokines and co-stimulatory molecules together drive efficient NK cell proliferation, differentiation and memory development. The extent to which cell death machinery contributes to NK cell responses has not been fully explored [21]. In the current study, we show that CASP8, a critical mediator of extrinsic death pathway [23], restricts NK cell expansion during the acute phase of MCMV infection but is dispensable for memory NK cell formation. These observations seem to parallel the cell-autonomous role of CASP8 in restraining CD8 T cell proliferation; however, additional studies will be needed to clarify this area, particularly given that regulation is independent of pro-necroptotic RIPK3 but dependent on RIPK1. In addition to driving hyperaccumulation of Ly49H+ NK cells in Casp8−/−Ripk3−/− mice, the resulting environment supports CASP8-deficient T cell survival during expansion, but does not appear to directly drive proliferation. Rather, NK and CD8 T cell-autonomous CASP8 play different, but interdependent roles once the consequences of RIPK3 necroptosis are removed from the host.
Elimination CASP8 together with RIPK3 enhances the magnitude of Ly49H+ NK cell responses, a result reminiscent of observations in Bim-deficient mice [20]. Where Bim-deficiency impairs memory NK cell development, Casp8−/−Ripk3−/− mice do not show defects in NK memory. The impact of Bim in T cell memory is likely to be due to the importance of intrinsic apoptosis, which is intact in the mice we have studied here. Bim alters terminal differentiated effector subsets as well as memory precursors accumulating during the acute phase of virus infection [40], whereas combined deficiency in CASP8 and RIPK3 only affects the terminal differentiated effector subsets without evident impact on the memory precursors [28]. In addition, differences may be attributable to a death-independent role of CASP8 in regulating cell differentiation. CASP8 is likely to crosstalk with Akt–mTOR pathway [41], which is important for NK cell activation [42, 43]. Thus, disruption of CASP8 may interfere with NK or other adaptive immune cell differentiation through the Akt–mTOR signaling axis, areas that are ripe for further investigation.
Studies of CASP8 in NK cells were initially performed in patients with a CASP8 catalytic mutation [29, 30] which exhibited a defect in NF-κB activation following CD16 or 2B4 ligation. Whether this result may be compared to results of T cell-specific disruption of CASP8 in mice remains to be resolved. Importantly, studies in T cell-specific CASP8-deficient mice certainly suffered from unleashed RIPK3-mediated necroptosis that was not recognized at the time but was resolved in 2011 [44,45,46]. The dual elimination of CASP8 together with RIPK3 removes risk of death and results in enhanced Ly49H+ NK cells response upon MCMV infection. Thus, as in T cells [28], CASP8 restricts NK cell proliferation once the risk of unleashed necroptosis is eliminated. Similar to TCR signal transduction, Ly49H receptor activation triggers the formation of the CARMA–MALT1–BCL10 complex that subsequently drives NF-κB activation [47]. Studies of T cell signal transduction have shown that this complex recruits FADD and CASP8 through the DD interactions between FADD and MALT1 [30, 47, 48]. Given the similarity between TCR- and Ly49H-dependent pathways, a complex may form directly in association with Ly49H, although this may also be influenced by Fas DR activation of CASP8 and contribute [49] to Ly49H signal transduction.
By comparing WT and Δm157 virus, we show that a robust Ly49H+ NK cell response supports survival of proliferating Casp8−/−Ripk3−/− CD8 T cells, mainly affecting the KLRG1hi subsets that contribute to a higher peak CD8 T cell response. Indeed, the normal peak of Casp8−/−Ripk3−/−CD8 T cell response following Δm157 virus infection is reminiscent of patterns observed with LCMV-infected mice once T cell-specific CASP8 deficiency was placed on a RIPK3-deficient background (Cd4CreCasp8flox/floxRipk3−/−) [46]. In our work, Ly49H+ NK cells promote Casp8−/−Ripk3−/− CD8 T cell survival by either reducing viral antigen levels in a critical site or by otherwise altering the environment. Curiously, the increased accumulation of Casp8−/−Ripk3−/− CD8 T cells following TCR stimulation in culture does not require help from other immune cells [28], including NK cells. NK cells may support Casp8−/−Ripk3−/− CD8 T cell survival by metering antigen–TCR interactions in vivo, such as by maintaining DC numbers and increasing the amount of viral antigen available for cross-presentation by DCs. Previous studies show that NK cell function influences DC levels during MCMV infection [35,36,37,38]. Casp8−/−Ripk3−/− CD8 T cell hyperaccumulation may result from the more sustained antigen stimulation that occurs in vivo but through some de facto quality of in vitro stimulation assays [35,36,37,38]. Sustained DC levels would be expected to drive terminal differentiated KLRG1hiCD127lo cell accumulation, which depend more on sustained TCR stimulation than their KLRG1lo counterparts [18]. Therefore, hyperaccumulation is an inherent feature of Casp8−/−Ripk3−/− T cells following TCR stimulation and is maintained via a NK cell-dependent survival mechanism during herpesvirus infection.
The function of Casp8 in NK cell regulation beyond suppressing necroptosis remains unknown, although this intensely studied protease has many uncharacterized substrates, oligomerization states and interaction partners [25]. We show that Casp8 restricts Ly49H+ NK cell expansion with no obvious impact on Ly49H− NK cell levels. Strikingly, NK cell responses are ablated once RIPK1 is eliminated along with Casp8 and RIPK3. Thus, Casp8 and RIPK1, likely via a FADD bridge in a ripoptosome-like complex, collaborate to influence NK cell responses following infection.
References
Lanier LL (2008) Up on the tightrope: natural killer cell activation and inhibition. Nat Immunol 9:495–502
Sun JC, Lanier LL (2011) NK cell development, homeostasis and function: parallels with CD8(+) T cells. Nat Rev Immunol 11:645–657
Smith HR, Heusel JW, Mehta IK, Kim S, Dorner BG, Naidenko OV, Iizuka K, Furukawa H, Beckman DL, Pingel JT, Scalzo AA, Fremont DH, Yokoyama WM (2002) Recognition of a virus-encoded ligand by a natural killer cell activation receptor. Proc Natl Acad Sci USA 99:8826–8831
Picarda G, Benedict CA (2018) Cytomegalovirus: shape-shifting the immune system. J Immunol 200:3881–3889
Vivier E, Raulet DH, Moretta A, Caligiuri MA, Zitvogel L, Lanier LL, Yokoyama WM, Ugolini S (2011) Innate or adaptive immunity? The example of natural killer cells. Science 331:44–49
Sun JC, Beilke JN, Lanier LL (2009) Adaptive immune features of natural killer cells. Nature 457:557–561
Guma M, Angulo A, Vilches C, Gomez-Lozano N, Malats N, Lopez-Botet M (2004) Imprint of human cytomegalovirus infection on the NK cell receptor repertoire. Blood 104:3664–3671
Guma M, Cabrera C, Erkizia I, Bofill M, Clotet B, Ruiz L, Lopez-Botet M (2006) Human cytomegalovirus infection is associated with increased proportions of NK cells that express the CD94/NKG2C receptor in aviremic HIV-1-positive patients. J Infect Dis 194:38–41
Lopez-Verges S, Milush JM, Schwartz BS, Pando MJ, Jarjoura J, York VA, Houchins JP, Miller S, Kang SM, Norris PJ, Nixon DF, Lanier LL (2011) Expansion of a unique CD57(+)NKG2Chi natural killer cell subset during acute human cytomegalovirus infection. Proc Natl Acad Sci USA 108:14725–14732
Lam VC, Lanier LL (2017) NK cells in host responses to viral infections. Curr Opin Immunol 44:43–51
Madera S, Sun JC (2015) Cutting edge: stage-specific requirement of IL-18 for antiviral NK cell expansion. J Immunol 194:1408–1412
Geary CD, Krishna C, Lau CM, Adams NM, Gearty SV, Pritykin Y, Thomsen AR, Leslie CS, Sun JC (2018) Non-redundant ISGF3 components promote NK cell survival in an auto-regulatory manner during viral infection. Cell Rep 24(1949–1957):e1946
Adams NM, Lau CM, Fan X, Rapp M, Geary CD, Weizman OE, Diaz-Salazar C, Sun JC (2018) Transcription factor IRF8 orchestrates the adaptive natural killer cell response. Immunity 48(1172–1182):e1176
Madera S, Rapp M, Firth MA, Beilke JN, Lanier LL, Sun JC (2016) Type I IFN promotes NK cell expansion during viral infection by protecting NK cells against fratricide. J Exp Med 213:225–233
Orange JS, Biron CA (1996) An absolute and restricted requirement for IL-12 in natural killer cell IFN-gamma production and antiviral defense. Studies of natural killer and T cell responses in contrasting viral infections. J Immunol 156:1138–1142
Nguyen KB, Salazar-Mather TP, Dalod MY, Van Deusen JB, Wei XQ, Liew FY, Caligiuri MA, Durbin JE, Biron CA (2002) Coordinated and distinct roles for IFN-alpha beta, IL-12, and IL-15 regulation of NK cell responses to viral infection. J Immunol 169:4279–4287
Nabekura T, Gotthardt D, Niizuma K, Trsan T, Jenus T, Jonjic S, Lanier LL (2017) Cutting Edge: NKG2D signaling enhances NK cell responses but alone is insufficient to drive expansion during mouse cytomegalovirus infection. J Immunol 199:1567–1571
Kurtulus S, Tripathi P, Hildeman DA (2012) Protecting and rescuing the effectors: roles of differentiation and survival in the control of memory T cell development. Front Immunol 3:404
Bouillet P, O’Reilly LA (2009) CD95, BIM and T cell homeostasis. Nat Rev Immunol 9:514–519
Min-Oo G, Bezman NA, Madera S, Sun JC, Lanier LL (2014) Proapoptotic Bim regulates antigen-specific NK cell contraction and the generation of the memory NK cell pool after cytomegalovirus infection. J Exp Med 211:1289–1296
Min-Oo G, Kamimura Y, Hendricks DW, Nabekura T, Lanier LL (2013) NK cells: walking three paths down memory lane. Trends Immunol 34:251–258
Mocarski ES, Guo H, Kaiser WJ (2015) Necroptosis: the Trojan horse in cell autonomous antiviral host defense. Virology 479–480:160–166
Mocarski ES, Kaiser WJ, Livingston-Rosanoff D, Upton JW, Daley-Bauer LP (2014) True grit: programmed necrosis in antiviral host defense, inflammation, and immunogenicity. J Immunol 192:2019–2026
Mocarski ES, Upton JW, Kaiser WJ (2012) Viral infection and the evolution of caspase 8-regulated apoptotic and necrotic death pathways. Nat Rev Immunol 12:79–88
Tummers B, Green DR (2017) Caspase-8: regulating life and death. Immunol Rev 277:76–89
Masson F, Kupresanin F, Mount A, Strasser A, Belz GT (2011) Bid and Bim collaborate during induction of T cell death in persistent infection. J Immunol 186:4059–4066
Feng Y, Livingston-Rosanoff D, Roback L, Sundararajan A, Speck SH, Mocarski ES, Daley-Bauer LP (2018) Remarkably robust antiviral immune response despite combined deficiency in caspase-8 and RIPK3. J Immunol 201:2244–2255
Feng Y, Daley-Bauer LP, Roback L, Guo H, Koehler HS, Potempa M, Lanier LL, Mocarski ES (2019) Caspase-8 restricts antiviral CD8 T cell hyperaccumulation. Proc Natl Acad Sci USA (In press)
Chun HJ, Zheng L, Ahmad M, Wang J, Speirs CK, Siegel RM, Dale JK, Puck J, Davis J, Hall CG, Skoda-Smith S, Atkinson TP, Straus SE, Lenardo MJ (2002) Pleiotropic defects in lymphocyte activation caused by caspase-8 mutations lead to human immunodeficiency. Nature 419:395–399
Su H, Bidere N, Zheng L, Cubre A, Sakai K, Dale J, Salmena L, Hakem R, Straus S, Lenardo M (2005) Requirement for caspase-8 in NF-kappaB activation by antigen receptor. Science 307:1465–1468
Kaiser WJ, Upton JW, Long AB, Livingston-Rosanoff D, Daley-Bauer LP, Hakem R, Caspary T, Mocarski ES (2011) RIP3 mediates the embryonic lethality of caspase-8-deficient mice. Nature 471:368–372
Kaiser WJ, Daley-Bauer LP, Thapa RJ, Mandal P, Berger SB, Huang C, Sundararajan A, Guo H, Roback L, Speck SH, Bertin J, Gough PJ, Balachandran S, Mocarski ES (2014) RIP1 suppresses innate immune necrotic as well as apoptotic cell death during mammalian parturition. Proc Natl Acad Sci USA 111:7753–7758
Mandal P, Berger SB, Pillay S, Moriwaki K, Huang C, Guo H, Lich JD, Finger J, Kasparcova V, Votta B, Ouellette M, King BW, Wisnoski D, Lakdawala AS, DeMartino MP, Casillas LN, Haile PA, Sehon CA, Marquis RW, Upton J, Daley-Bauer LP, Roback L, Ramia N, Dovey CM, Carette JE, Chan FK, Bertin J, Gough PJ, Mocarski ES, Kaiser WJ (2014) RIP3 induces apoptosis independent of pronecrotic kinase activity. Mol Cell 56:481–495
Dokun AO, Kim S, Smith HR, Kang HS, Chu DT, Yokoyama WM (2001) Specific and nonspecific NK cell activation during virus infection. Nat Immunol 2:951–956
Robbins SH, Bessou G, Cornillon A, Zucchini N, Rupp B, Ruzsics Z, Sacher T, Tomasello E, Vivier E, Koszinowski UH, Dalod M (2007) Natural killer cells promote early CD8 T cell responses against cytomegalovirus. PLoS Pathog 3:e123
Mitrovic M, Arapovic J, Jordan S, Fodil-Cornu N, Ebert S, Vidal SM, Krmpotic A, Reddehase MJ, Jonjic S (2012) The NK cell response to mouse cytomegalovirus infection affects the level and kinetics of the early CD8(+) T-cell response. J Virol 86:2165–2175
Andrews DM, Scalzo AA, Yokoyama WM, Smyth MJ, Degli-Esposti MA (2003) Functional interactions between dendritic cells and NK cells during viral infection. Nat Immunol 4:175–181
Andrews DM, Estcourt MJ, Andoniou CE, Wikstrom ME, Khong A, Voigt V, Fleming P, Tabarias H, Hill GR, van der Most RG, Scalzo AA, Smyth MJ, Degli-Esposti MA (2010) Innate immunity defines the capacity of antiviral T cells to limit persistent infection. J Exp Med 207:1333–1343
Lau CM, Sun JC (2018) The widening spectrum of immunological memory. Curr Opin Immunol 54:42–49
Kurtulus S, Sholl A, Toe J, Tripathi P, Raynor J, Li KP, Pellegrini M, Hildeman DA (2015) Bim controls IL-15 availability and limits engagement of multiple BH3-only proteins. Cell Death Differ 22:174–184
Arechiga AF, Bell BD, Leverrier S, Weist BM, Porter M, Wu Z, Kanno Y, Ramos SJ, Ong ST, Siegel R, Walsh CM (2007) A Fas-associated death domain protein/caspase-8-signaling axis promotes S-phase entry and maintains S6 kinase activity in T cells responding to IL-2. J Immunol 179:5291–5300
Marcais A, Marotel M, Degouve S, Koenig A, Fauteux-Daniel S, Drouillard A, Schlums H, Viel S, Besson L, Allatif O, Blery M, Vivier E, Bryceson Y, Thaunat O, Walzer T (2017) High mTOR activity is a hallmark of reactive natural killer cells and amplifies early signaling through activating receptors. Elife 6:e26423
Marcais A, Cherfils-Vicini J, Viant C, Degouve S, Viel S, Fenis A, Rabilloud J, Mayol K, Tavares A, Bienvenu J, Gangloff YG, Gilson E, Vivier E, Walzer T (2014) The metabolic checkpoint kinase mTOR is essential for IL-15 signaling during the development and activation of NK cells. Nat Immunol 15:749–757
Ch’en IL, Beisner DR, Degterev A, Lynch C, Yuan J, Hoffmann A, Hedrick SM (2008) Antigen-mediated T cell expansion regulated by parallel pathways of death. Proc Natl Acad Sci USA 105:17463–17468
Hedrick SM, Ch’en IL, Alves BN (2010) Intertwined pathways of programmed cell death in immunity. Immunol Rev 236:41–53
Ch’en IL, Tsau JS, Molkentin JD, Komatsu M, Hedrick SM (2011) Mechanisms of necroptosis in T cells. J Exp Med 208:633–641
Juilland M, Thome M (2018) Holding all the CARDs: how MALT1 controls CARMA/CARD-dependent signaling. Front Immunol 9:1927
Arechiga AF, Bell BD, Solomon JC, Chu IH, Dubois CL, Hall BE, George TC, Coder DM, Walsh CM (2005) Cutting edge: fADD is not required for antigen receptor-mediated NF-kappaB activation. J Immunol 175:7800–7804
Paulsen M, Janssen O (2011) Pro- and anti-apoptotic CD95 signaling in T cells. Cell Commun Signal 9:7
Acknowledgements
We thank Sam Speck (Emory University) and Rafi Ahmed (Emory University) for reagents and discussion and Wolfram Brune (Heinrich Pette Institute) for ∆m157 MCMV. This research was supported the National Institute of Health (NIH) Tetramer Core Facility for MHC class I tetramers and the Emory Vaccine Center Flow Core for materials and Public Health Service Grants R01 AI020211 and AI118853 (to E.S.M.) as well as AI068129 (to L.L.L.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no conflict of interest.
Ethical approval
Animal experiments were approved according to the United States Public Health Service National Institutes of Health and Emory University Institutional Animal Care and Use Committee guidelines.
Additional information
Edited by: Matthias J. Reddehase.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Special Issue on Immunological Imprinting during Chronic Viral Infection.
Rights and permissions
About this article
Cite this article
Feng, Y., Daley-Bauer, L.P., Roback, L. et al. Caspase-8 restricts natural killer cell accumulation during MCMV Infection. Med Microbiol Immunol 208, 543–554 (2019). https://doi.org/10.1007/s00430-019-00617-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00430-019-00617-6