Abstract
Heart rate variability (HRV) is an important biomarker for parasympathetic function and future health outcomes. The present study examined how the structure of regions in a neural network thought to maintain top–down control of parasympathetic function is associated with HRV during both rest and social stress. Participants were 127 young women (90 Black American), who completed a structural MRI scan and the Trier Social Stress Test (TSST), during which heart rate was recorded. Regression analyses were used to evaluate associations between cortical thickness in five regions of the Central Autonomic Network (CAN; anterior midcingulate cortex [aMCC], pregenual and subgenual anterior cingulate cortex [pgACC, sgACC], orbitofrontal cortex [OFC], and anterior insula) and high-frequency HRV during rest and stress. Results indicated that cortical thickness in CAN regions did not predict average HRV during rest or stress. Greater cortical thickness in the right pgACC was associated with greater peak HRV reactivity during the TSST, and survived correction for multiple comparisons, but not sensitivity analyses with outliers removed. The positive association between cortical thickness in the pgACC and peak HRV reactivity is consistent with the direction of previous findings from studies that examined tonic HRV in adolescents, but inconsistent with findings in adults, which suggests a possible neurodevelopmental shift in the relation between brain structure and autonomic function with age. Future research on age-related changes in brain structure and autonomic function would allow a more thorough understanding of how brain structure may contribute to parasympathetic function across neurodevelopment.
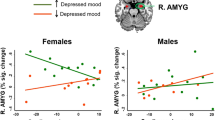
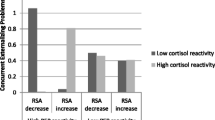
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The parasympathetic nervous system (PNS) plays an important role in stress reactivity and recovery, and long-term health outcomes. Higher parasympathetic activity, indexed by higher heart rate variability (HRV) at rest, has been positively associated with a more flexible and adaptive set of psychophysiological responses in preparation for dynamic environmental demands (Thayer and Sternberg 2006; Hollenstein et al. 2012; Hamilton and Alloy 2016; Rottenberg 2007). Conversely, lower parasympathetic activity (lower HRV at rest) prospectively predicts adverse health consequences, such as premature mortality and coronary heart disease (Thayer and Lane 2007; Hillebrand et al. 2013; Goldenberg et al. 2019), depression (Kemp et al. 2012; Jandackova et al. 2016), and other types of psychopathology, such as anxiety disorders and attention-deficit hyperactivity disorder (Chalmers et al. 2014, 2016; Kemp et al. 2014; Rash and Aguirre-Camacho 2012). Therefore, tonic HRV can be considered a biomarker of autonomic flexibility and future disease risk (Kemp et al. 2010; Beauchaine and Thayer 2015).
Associations between brain structure and parasympathetic function can help elucidate the neural characteristics of adaptive stress regulation, which could then identify individuals who are at a higher risk for adverse health outcomes. The Neurovisceral Integration Model (NIM), an initial theoretical framework first proposed by Thayer and Lane (2000), posits that parasympathetic activity and reactivity are governed by neural connections between the heart and a network of subcortical and cortical prefrontal regions which constitute the Central Autonomic Network (CAN). The reciprocally interconnected CAN structures output to the sinoatrial node via the stellate ganglia and vagus nerve, and ultimately produce a dynamic, vagally-dominated cardiac response in the presence of a stressor (Thayer and Lane 2009; Thayer et al. 2009; Barrett and Simmons 2015). Information relevant to automatic regulation flows bidirectionally from the CAN to peripheral organs, such as the heart, such that HRV can indicate the degree of integration between the central nervous system (CNS) and autonomic nervous system (ANS). The interplay of neural circuits in cardiac regulation inextricably influences the automatic generation and cognitive regulation of emotional states (Koenig 2020; Kupfer et al. 2012). Therefore, HRV can further indicate the functional integrity of neural networks implicated in emotion-cognition interactions (Park and Thayer 2014).
CAN structures, including the anterior midcingulate cortex (aMCC), pregenual and subgenual anterior cingulate cortex (pgACC and sgACC, respectively), orbitofrontal cortex (OFC), and anterior insular cortex, are not only critically implicated during autonomic regulation, but also serve as a neural hub for the top–down regulation of emotion (Beauchaine and Cicchetti 2019). For example, the aMCC is thought to be involved in the perception of threat and safety, emotional salience, as well as contextually relevant modulation of bodily arousal states (Winkelmann et al. 2016; Stevens et al. 2011; Critchley et al. 2003). The pgACC has numerous projections to critical structures involved in autonomic regulation and has been implicated in the emotional experience of pain and discomfort (Vogt 2005; Gianaros et al. 2007). The sgACC, primarily a visceral-motor division, can be considered an essential component in the regulation of affective and autonomic responses (Palomero-Gallagher et al. 2009; Lane et al. 2013; Drevets et al. 2008a, b). The OFC, strongly interconnected with the ACC, serves a critical role in emotional processing and inhibitory control (Wagner et al. 2008; Protopopescu et al. 2005). The anterior insular cortex has been implicated in the subjective awareness of emotions as well as the accompanying interoceptive response (Menon and Uddin 2010; Gogolla 2017).
Structural characteristics of regions within the CAN, including cortical thickness, volume, and myelination, may promote higher parasympathetic function and more adaptive stress response (Radley et al. 2015; Carnevali et al. 2018). In support of this hypothesis, structural MRI studies have indicated that thicker cortices in regions within the CAN—including bilateral rostral and caudal ACC, right middle frontal gyrus (MFG), bilateral OFC, pars triangularis, and bilateral insula—are associated with higher tonic HRV in healthy adults (Yoo et al. 2018; Winkelmann et al. 2016), as well as higher tonic HRV in veterans with post-traumatic stress disorder (PTSD; Woodward et al. 2008). Given the positive association between CAN cortical thickness and tonic HRV, thicker cortices may allow for a greater recruitment of neural resources during adaptive cardiac autonomic regulation. Furthermore, cortical thickness has been significantly associated with various forms of psychopathology, such as depression (Sacher et al. 2012; Bora et al. 2012; Drevets et al. 2008a), PTSD (Bromis et al. 2018; Woodward et al. 2006), anxiety disorders (Shang et al. 2014; Frick et al. 2013), and borderline personality disorder (Morandotti et al. 2013), as well as self-injurious behavior (Beauchaine et al. 2019).
In contrast to the positive association between tonic HRV and cortical thickness in adults, findings from studies of participants in mid-adolescence suggest that higher parasympathetic activity is associated with lower cortical thickness in the rostral and caudal ACC (mean age = 15.92; Koenig et al. 2018a), as well as the insula (mean age = 16.04; Koenig et al. 2018b). Adolescence through emerging adulthood is a critical period of neuromaturation (Foland-Ross et al. 2015), particularly in regions of the CAN (Koenig 2020; Tamnes et al. 2017; Shaw et al. 2008). Furthermore, the link between exposure to stressors and adverse mental health outcomes may be pronounced during adolescence and young adulthood, when major mental disorders rise in incidence (Paus et al. 2008; Kessler et al. 2001), especially among girls and women (Hankin et al. 2015). This dramatic increase in psychopathology may be due, in part, to increases in exposure to stressors that occur while the autonomic and neural systems that regulate stress response continue to develop (Davey et al. 2008; Forbes and Dahl 2010; Beauchaine et al. 2007). In a longitudinal study, girls and boys (8–12 years-old) who had increasing HRV across development later reported fewer difficulties with emotion regulation in adolescence (2–3 years later; Vasilev et al. 2009). In a different longitudinal study by Vijayakumar et al. (2014), girls in early adolescence (12 years-old) with increased cortical thinning in the dorsolateral prefrontal cortex and ventrolateral prefrontal cortex across a four-year period reported using more adaptive emotion regulation strategies by young adulthood (age 19). These two longitudinal studies provide converging evidence that emotion dysregulation, especially that seen in depression and other affective disorders, may result from a disrupted integration of the PNS and CNS. Furthermore, normative development of vagal activity across adolescence has important implications for the onset of psychopathology, and may compensate for abnormal cortical thinning in emotion regulation-oriented prefrontal structures (Koenig 2020). Age-related differences in the association between autonomic regulation and the integrity of certain characteristics of the brain’s architecture suggest that there may be a functional flip as the prefrontal cortex reaches maturity in adulthood. However, few studies have examined associations between CAN structures and HRV within narrowly-defined periods of neurodevelopment (i.e., 19–20 years-old) to constrain the influence of chronological age. A recent mega-analysis utilizing data from 20 research groups worldwide revealed a positive association between the left lateral OFC and HRV across the lifespan, but the study did not explicitly investigate the potential change in direction of association between cortical thickness and HRV from adolescence to adulthood (Koenig 2020). Therefore, replication of pre-existing findings at these developmental milestones as well as additional research to illuminate the nebulous gap between adolescence and adulthood is critically needed.
Existing research linking cortical thickness in the CAN to parasympathetic function has also focused heavily on tonic HRV rather than phasic HRV. Phasic HRV, an index of parasympathetic reactivity, can be construed as the acute autonomic self-regulatory response as the body shifts from resting state to one of relative arousal elicited by internal or external stressors (Beauchaine et al. 2007, 2001; El-Sheikh et al. 2011; Schwerdtfeger and Derakhshan 2010). The system copes with environmental demands through parasympathetically-directed vagal withdrawal, reflected by a decrease in HRV, which allows engagement of sympathetic processes, indicated by an increase in heart rate (Beauchaine 2001). Although phasic HRV has been shown to both predict (Dworkin 1993, 2000; Salomon 2005) and be predicted by tonic HRV (Park et al. 2014), phasic HRV may have distinct predictive utility for understanding the risk for adverse health outcomes. For example, blunted phasic HRV has been concurrently associated with increased anxiety and depressive symptoms (Shinba et al. 2008), as well as current depression (Ehrenthal et al. 2010). Therefore, parasympathetic regulation of heart rate during threat reactivity may be especially relevant in models that implicate brain structure and cardiovascular function as mechanisms of future disease risk (Thayer et al. 2010; Schiweck et al. 2019). Although tonic and phasic HRV are interrelated autonomic constructs (Park et al. 2014), each index has a distinct and important regulatory function: tonic HRV is a measure of self-regulatory capacity, whereas phasic HRV captures the body’s acute response to environmental stressors. Hence, future research should include both measures to provide a more nuanced characterization of adaptive parasympathetic regulation.
Based on the NIM (Thayer and Lane 2000), we sought to evaluate the association of cortical thickness and parasympathetic regulation during rest and acute social stress in a sample of young women. In the present study, participants underwent an MRI scan and completed the Trier Social Stress Test (TSST; Kirschbaum et al. 1993), which is thought to reliably induce acute parasympathetic engagement (Roos et al. 2017) and is contextually relevant for emerging young adults. If associations between cortical thickness and parasympathetic function in young adults replicate results in adult samples, individuals with greater cortical thickness in CAN regions (i.e., aMCC, subgenual ACC, pregenual ACC, OFC, anterior insula) should have higher tonic HRV and lower phasic HRV than those with thinner cortices. However, if associations between cortical thickness and parasympathetic function in young adults replicate results in adolescent samples, individuals who have lower cortical thickness in CAN regions should have higher tonic HRV and lower phasic HRV. Although chronological age is often studied as a marker of neurodevelopmental change, pubertal maturation similarly shows associations indicative of the maturation of brain structure (Herting and Sowell 2017; Chahal et al. 2018). Therefore, pubertal timing, which has frequently been neglected in similar research, was included to more fully characterize the association between brain structure and parasympathetic function. Depression symptom severity was also included in analyses to control for the aggravating influence on parasympathetic regulation (Koenig et al. 2016, 2018b) and cortical structure (Li et al. 2020; Suh et al. 2019). The present study is the first to examine the association between cortical thickness and parasympathetic regulation during periods of both rest and stress in an emerging young adult population of women.
Method
Participants
Participants were 127 young women recruited during the ninth wave of the Pittsburgh Girls Study—Emotions substudy (PGS-E; Keenan et al. 2008). The PGS-E is a study of precursors to depression that includes 232 girls from the longitudinal Pittsburgh Girls Study (PGS; Hipwell et al. 2002; Keenan et al. 2010). PGS participants were initially recruited by oversampling low-income neighborhoods to identify girls between 5 and 8 years of age (N = 2451). Participants in the PGS-E included the youngest cohort of girls from the PGS, who were initially recruited at 5 years of age. At the time of the MRI scan for the present substudy, participants had a mean age of 19.59 (SD = 0.49, range 19–20) and self-identified race as follows: Black American (70.9%), White American (22.0%), and multi-racial (5.5%).
Procedure
Participants completed a structural MRI scan at the Magnetic Resonance Research Center at the University of Pittsburgh Medical Center. They also completed the TSST and study questionnaires either on the day of the scan or during a separate visit, determined by participant’s availability. The TSST is a standardized protocol that reliably induces autonomic arousal and moderate psychosocial stress (Kirschbaum et al. 1993). The protocol included continuous measurement of electrocardiography (ECG) and respiration during a 30-min resting baseline, 5-min speech preparation period, 5-min speech task, 5-min mental arithmetic task, and a 30-min recovery period. The stressor task was operationalized to include the speech and arithmetic periods as a single 10-min block.
Measures
Heart rate variability (HRV)
During the TSST protocol, ECG was performed continuously at 1024 Hz using a Mindware Bionex 2-slot amplifier and Biolab acquisition software (Gahanna, OH). Beats were identified with an automatic scoring algorithm in Mindware HRV 3.1.4 and manually inspected for ectopic beats, arrhythmias, and signal artifacts. Ectopic beats and arrhythmias were corrected by interpolating preceding and successive beats (Fallen and Kamath 1995). Segments with arrhythmias or artifacts that obscured more than 50% of the epoch were omitted (Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology 1996). HRV was indexed by the high-frequency band (i.e., 0.15–0.40 Hz) across each of 75, one-minute segments. High-frequency heart rate variability (HF-HRV) is a frequency-domain based measure of cardiac vagal activity that is also highly correlated with the root mean square of successive differences (RMSSD; Laborde et al. 2017). As a time-domain measure, RMSSD is relatively independent of respiratory influences (Hill et al. 2009) and appropriate for derivation of HRV from brief recording intervals (Ellis et al. 2015). However, due to the focus on high-frequency bands, HF-HRV captures parasympathetic influences on HRV without including the noise of sympathetic influences seen in lower frequency bands, as measured by RMSSD (Berntson et al. 2005). As a result, tonic HRV was represented by the average HF-HRV across the 30-min baseline period. Phasic HRV was indexed by the difference between average and peak change in HF-HRV during the 10-min stressor period relative to the baseline period.
Image acquisition
High-resolution anatomical images were acquired using a T1-weighted, Magnetization Prepared Rapid Acquisition Gradient Echo (MPRAGE) sequence on a Siemens 3.0 T Tim Trio scanner (Siemens Medical Solutions, Erlangen, Germany) with the following parameters: TR = 2.3 s; TE = 2.98 ms; flip angle = 9°; 160 slices; FOV = 256 × 240 mm; acquisition voxel size = 1.0 × 1.0 × 1.2 mm. The anatomical scan was acquired as part of a larger scan battery. Acquisition time for the T1-weighted image was 9 min 14 s.
Image processing
MR images were processed with FreeSurfer 5.3 (http://surfer.nmr.mgh.harvard.edu/). We followed the standard FreeSurfer processing pipeline (i.e., recon-all) for cortical surface reconstruction. The automated processing pipeline consisted of motion correction, intensity normalization, skull stripping, transformation into Talairach space, tissue segmentation into white matter, gray matter and cerebrospinal fluid (CSF), tessellation of the gray/white matter boundary, topology correction, and surface deformation following intensity gradients to determine the gray/white and gray/CSF borders based on where the greatest shift in intensity defines the transition to the other tissue class. Details of the processing pipeline are described in prior publications (Fischl et al. 2002; Dale et al. 1999; Dale and Sereno 1993) and on the FreeSurfer website. Cortical thickness (CT) was calculated as the closest distance from the gray/white boundary to the gray/CSF boundary at each vertex on the tessellated surface (Fischl and Dale 2000). All scans were visually inspected and rated for scan quality (1 = excellent, 2 = some minor problems, 3 = major problems) to rule out gross artifacts before inclusion in the FreeSurfer processing pipeline. Only scans with a quality rating of 1 or 2 were included. In addition, all FreeSurfer output was visually inspected to identify any gross processing mistakes.
Subsequent analyses were limited to five ROIs, separated by hemisphere, that have been implicated in parasympathetic regulation of heart rate: aMCC, pgACC, sgACC, OFC, and anterior insula. Gray matter volume primarily scales with surface area across development, whereas cortical thickness is much less dependent on global brain size (Malone et al. 2015; Winkler et al. 2010). Therefore, cortical thickness was used for analyses to circumvent corrections for intracranial volume as well as to select a more stable measure of brain structure. ROIs were selected by matching MNI coordinates from recent literature that used the Desikan-Killiany atlas (Desikan et al. 2006) to the more recently parcellated Destrieux atlas (Destrieux et al. 2010). Based on peak coordinates reported in recent work, the aMCC was represented by the “middle-anterior part of the cingulate gyrus and sulcus” (Destrieux index #7; Koenig et al. 2018a; Winkelmann et al. 2016; Yoo et al. 2018), the sgACC was represented by the “subcallosal area” (Destrieux index #32; van Reekum et al. 2007), the pgACC was represented by “anterior part of the cingulate gyrus and sulcus” (Destrieux index #6; Thayer et al. 2012; Schiller et al. 2008), and the anterior insula was represented by “superior segment of the circular sulcus of the insula” (Destrieux index #49; Lane et al. 2009) in the Destrieux atlas. The Destrieux atlas has a more finely parcellated set of ROIs that constitute the OFC than the Desikan-Killiany atlas; therefore, we used peak coordinates from Wagner et al. (2008) and averaged the cortical thickness of the “orbital gyri” (Destrieux index #24) and “orbital sulci” (Destrieux index #64) to create a single ROI for analyses of OFC.
Pubertal Development Scale (PDS)
The PDS is an interview assessment of five participant-reported physical indicators of pubertal status that can be used to classify pubertal development into five levels: pre-pubertal, early pubertal, mid-pubertal, late pubertal, and post-pubertal. The PDS was administered during annual PGS assessments from 9–14 years of age. There is evidence to suggest that both age and puberty independently predict cortical maturation across adolescence (Goddings et al. 2014; Herting and Sowell 2017). To adjust for potential differences in trajectories of prefrontal cortex development from adolescence through early adulthood (Tamnes et al. 2017; Shaw et al. 2008; Chahal et al. 2018), the age at which participants first reached mid-puberty (Crockett stage 3; Petersen et al. 1988) was included as a covariate in analyses linking age 19 cortical thickness and HRV (Sisk and Zehr 2005).
Body mass index (BMI)
Height and weight were measured in participants at 19 years of age and used to calculate BMI. Several neuroimaging studies have found evidence that BMI is associated with localized abnormalities in gray matter (i.e., reduced volume or increased cortical thinning) in frontal regions during adolescence (Alosco et al. 2014) and adulthood (Raji et al. 2010; Marqués-Iturria et al. 2013), and also inversely associated with HRV at rest (Williams et al. 2017). Based on this converging evidence across neurodevelopment and the link to parasympathetic regulation, BMI was included as a covariate in analyses between parasympathetic function and brain structure to account for the likely unique influence of body mass.
Center for Epidemiological Studies Depression Scale (CES-D)
The CES-D is a 20-item self-report scale that measures the frequency of depressive symptoms over the past week. Each question is rated on a scale ranging from 0 (rarely or none of the time, < 1 day) to 3 (most or all of the time, 5–7 days). Scores 16 or above indicate a probable depressive disorder (Lewinsohn et al. 1997; Radloff 1977). The CES-D scale is considered a reliable and valid psychometric measure of depressive symptom severity (Cosco et al. 2017), and was found to have high internal consistency in the present study (α = 0.90).
Statistical analyses
Descriptive analyses
All analyses were conducted in RStudio version 1.1.383 for Mac OS X. Central tendency, distribution, and outliers were examined for all variables prior to hypothesis tests. Variables with skewed data (i.e., HF-HRV) were log transformed. Seven participants (5.5%) were excluded from analyses due to > 50% unusable/missing segments during the stressor period. Bivariate correlations were estimated for all predictor and outcome variables. Grand average graphs were created for HRV during the baseline, stressor, and recovery periods and examined to determine the most appropriate means of operationalizing stress reactivity. Multiple imputation was used to estimate values for partially incomplete questionnaire data on the CES-D using predictive mean matching (PMM) within the RStudio package ‘mice.’ Remaining missing data for BMI (24 participants), PDS (two participants), and CES-D scores (10 participants) were treated with case-wise deletion during analyses, resulting in a final sample of 80 for analyses.
Consistent with previous HRV studies, we first calculated average stress reactivity by subtracting the mean HRV during the stressor period from the mean tonic HRV during the baseline period (Hamilton and Alloy 2016). Since we observed a pattern of rapid decline and recovery in the grand average graph of HRV during the stressor period (see Fig. 1), we calculated a second measure of stress reactivity by subtracting the lowest segment of HRV during the stressor period from mean HRV during the baseline period for each participant. This method captures the magnitude of peak stress reactivity during the stressor task.
Grand average graph showing mean HF-HRV during the TSST (N = 127), with the stressor period highlighted. The four sections of the TSST were operationalized by time (minute), such that the baseline period contained segments 1–30, preparation period contained segments 31–35, stressor period contained segments 36–45, and recovery period contained segments 46–75. HF-HRV High-frequency heart rate variability. TSST Trier Social Stress Test
Primary analyses
Ten regression models were performed in RStudio to evaluate the magnitude and direction of the association between cortical thickness and the five CAN regions with HF-HRV during rest and stress. Cortical thickness in each ROI, separated by brain hemisphere, was entered as a predictor of mean HF-HRV during the 30-min baseline period (i.e., rest), and mean and peak HF-HRV during the stressor relative to mean HF-HRV during rest (i.e., stress reactivity). PDS, BMI, CES-D scores, and racial identity were included as covariates in the analyses. We employed a correction for multiple comparisons using false discovery rate (FDR) for our two primary hypotheses in which cortical thickness would be significantly associated with HRV during periods of rest and stress (Benjamini and Hochberg 1995). FDR applies a correction for the number of unique hypotheses tested and is considered an appropriate method for hypothesis testing that avoids overcorrection for the probability of false positives. Results are also presented without FDR correction in light of inconsistent findings between similar studies, as well as differences between studies in method of correcting for multiple comparisons and the inclusion of relevant covariates (Koenig et al. 2018a, b; Yoo et al. 2018; Winkelmann et al. 2016). Sensitivity analyses were conducted to measure the robustness of significant findings by detecting HRV and cortical thickness outliers, and determining the extent of their influence on the association between CAN regions and HRV. Outliers were identified as values exceeding two standard deviations from the mean. Analyses were also conducted using RMSSD and chronotropic state (CS)-adjusted RMSSD (i.e., controlling for heart period; de Geus et al. 2019; Monfredi et al. 2014) as time-domain measures of parasympathetic activity, so that we could thoroughly evaluate whether the metric for HRV varies as a function of the measure (i.e., RMSSD, CS-adjusted RMSSD, or HF-HRV).
Results
Descriptive statistics
Mean log-transformed HF-HRV was 6.22 (SD = 1.71) during the resting baseline and 6.05 (SD = 1.39) during the stressor period (see Fig. 1). The mean HF-HRV for log-transformed peak stress reactivity (difference between baseline and lowest point in HF-HRV during the stressor) was 1.39 (SD = 1.25).
The mean age for reaching mid-puberty was 9.77 (SD = 0.99). Pubertal timing did not predict cortical thickness or HRV during times of rest or stress. Mean BMI was 27.86 (SD = 6.76), indicating that participants were overweight on average. BMI independently predicted cortical thickness in the right hemisphere of the aMCC (R2 = .172, p = .008), pgACC (R2 = .075, p = .039), and anterior insula (R2 = .092, p = .007; Medic et al. 2016), but not tonic or phasic HRV. The overall mean CES-D score was 14.28 (SD = 9.09), and 34.19% of participants (N = 117) met the diagnostic cutoff for probable depression. CES-D scores did not predict cortical thickness, tonic HRV or stress reactivity, and did not account for substantial variance in regression analyses. Racial identity was significantly associated with cortical thickness in the left aMCC (R2 = .030, p = .042), as well as the left (R2 = .026, p = .035) and right insula (R2 = .105, p = .004). When controlling for PDS, BMI, and CES-D scores, racial identity did not significantly predict tonic HRV, average or peak stress reactivity, nor did the covariate explain a significant amount of variance in the regression models.
Regression of HF-HRV during rest and stress on cortical thickness in the CAN
Table 1 presents the results of regression analyses of HF-HRV on cortical thickness during rest and social stress. Cortical thickness in CAN regions was not linearly associated with tonic HRV or average phasic HRV.
The right pgACC was positively associated with peak stress reactivity such that greater cortical thickness in the right pgACC was associated with increased parasympathetic withdrawal during the stressor task, R2 = .119, uncorrected p = .005. The right pgACC was still significantly associated with peak HRV reactivity following FDR correction (p = .009), but not following sensitivity analyses in which ten outliers were removed (p = .20). Associations between peak HRV reactivity and cortical thickness in all other CAN regions were not significant.
There were not substantial differences in findings across tonic HRV, average stress reactivity, and peak stress reactivity when using RMSSD or CS-adjusted RMSSD in place of HF-HRV. Consistent with primary analyses, CS-adjusted RMSSD analyses revealed a significant association in the right pgACC during peak stress reactivity (R2 = .079, p = .039), which was no longer significant following FDR correction for multiple comparisons (p = .078). RMSSD analyses also replicated the significant association between peak stress reactivity and the right pgACC (R2 = .088, p = .027), but did not survive further FDR correction (p = .054).
Discussion
The present study evaluated the relation between cortical thickness in CAN regions and HRV during periods of rest and stress in young adult women. In contrast with recent literature in adults and adolescents of mixed gender (Woodward et al. 2008; Winkelmann et al. 2016; Yoo et al. 2018; Koenig et al. 2018a), we did not find a relation between tonic HRV and prefrontal cortical thickness in the aMCC, pgACC, sgACC, OFC, or anterior insula. However, we found a significant positive relationship between HRV reactivity during social stress and cortical thickness in the right pgACC. Individuals with relatively thicker right pgACC cortices tended to experience greater reactivity in parasympathetic function during the stressor task. Given that the significant association was established only in the models investigating peak stress reactivity and did not survive sensitivity analyses, this association should be interpreted with caution. However, previous studies (Yoo et al. 2018; Winkelmann et al. 2016; Koenig et al. 2018a, b) reported small to moderate effect sizes in analyses linking cortical thickness to tonic HRV (R2 = .049–.397), which is consistent with the small effect size (R2 = .119) in the present study for HF-HRV peak reactivity. Peak stress reactivity may be a more sensitive measure of parasympathetic regulation than average HRV during the stressor period given the relatively swift HRV recovery in this sample. However, associations with peak HRV reactivity may also be less reliable than associations with mean HRV response across multiple epochs.
Associations between pgACC and HRV are among the most replicated findings for studies that focus on parasympathetic regulation and brain structure (Koenig et al. 2018a; Yoo et al. 2018; Thayer et al. 2012). Furthermore, the observed unilateral association with the right pgACC, rather than left pgACC, is consistent with both the purported right-sided preference of neural structures in the autonomic innervation of the heart via the sinoatrial node (Lane et al. 2009; Chuang et al. 2004; Ahern et al. 2001), as well as similar papers investigating autonomic regulation (Winkelmann et al. 2016). Because the pgACC plays an essential role in the integration and regulation of affective information, disruptions to the structure’s normative maturation (e.g., altered cortical thinning) may have downstream effects on vagal activity during stressors. Increased activation of the pgACC during emotion conflict resolution has been closely tied to inhibition of amygdalar response (Etkin et al. 2011, 2006). As this top–down circuit becomes disinhibited, there may then be prolonged and exaggerated stress responses due to the subsequent parasympathetic withdrawal. Over time, this disproportionate reactivity may lead to adverse health outcomes.
Previous research by Koenig et al. (2018a, b) has twice supported a negative association between the cortical thickness of prefrontal regions and tonic HRV in adolescents, whereas findings from adult samples have repeatedly yielded a positive relation (Woodward et al. 2008; Winkelmann et al. 2016; Yoo et al. 2018). Given the negative association of cortical thickness with tonic HRV in adolescents (Koenig et al. 2018a, b), but not in adults (Winkelmann et al. 2016; Yoo et al. 2018), and the negative association of right pgACC cortical thickness and peak HRV reactivity in young adult women in this study, there may be a developmental shift in the relation between parasympathetic regulation and cortical thickness as the brain continues to mature. However, the flip in the relation between CAN structures and parasympathetic relationship may occur later in young adult men, due to known developmental differences in the trajectories of autonomic function and cortical thinning (Koenig 2020). Additional research on sex differences has suggested that girls and female adolescents may have a disproportionately high risk for developing psychopathology due to lower tonic HRV (Koenig et al. 2017). While girls and female adolescents are reported to have lower parasympathetic activity than boys, a meta-analysis by Koenig and Thayer (2016) revealed that women have comparatively greater vagal activity than men, suggesting a shift in this modulation process with maturation. Interestingly, the increase in vagal dominance from adolescence into adulthood for women may protect against various somatic health concerns, such as cardiovascular disease. Since the mean age of the present study’s sample is developmentally between adolescence and adulthood (Tamnes et al. 2017; Shaw et al. 2008), the cross-sectional findings serve to further delineate developmental trends in this relation in the CAN. Because cortical architecture is being shaped across adolescence and into early adulthood (Mills et al. 2012; Vijayakumar et al. 2016), research should similarly focus on the association between cortical thinning and parasympathetic regulation across these developmental periods. Results of the present study offer another component for understanding the broader developmental picture.
Based on the effect sizes in the present study and other research, the NIM may be an incomplete conceptualization of the neurobiological integration between the brain and heart. Previous literature has inconsistencies in the specific CAN regions that have been associated with tonic HRV (Koenig et al. 2018a, b; Yoo et al. 2018; Winkelmann et al. 2016). Additionally, there is a dearth of research investigating the relationship between brain structure and stress reactivity, especially among emerging young adults, so interpretations of the results from the present study may be limited. Furthermore, studies that have focused on cortical thickness typically do not integrate the potential influences of subcortical components (i.e., amygdala) on parasympathetic regulation (Thayer and Lane 2009). There also exists the possibility that anatomical parcellation of CAN structures is too broad, and thus not an adequately precise representation of regional differences. Although a neurodevelopmental shift in associations between brain structure and autonomic function between adolescence and adulthood is one potential explanation of the study results, an alternative interpretation is that the differences in results reflect publication bias for selective findings. In support of this interpretation, the mega-analysis by Koenig et al. (2020) found that the relationship between CAN regions and resting state parasympathetic function may have been overestimated due to type 1 errors. After correction for multiple comparisons, HRV was only associated cortical thickness in the left lateral OFC (BF = 5.22, p = .015; Koenig et al. 2020).
There are several merits to the present study, including the racial and socioeconomic diversity of the sample, the narrow age range of the sample, robust sample size, rigor in analyses, as well as the investigation of HRV during times of both rest and stress. The present study had a much larger sample size than comparable studies relating parasympathetic function to brain structure (N range = 20–90; Koenig et al. 2018a, b; Yoo et al. 2018; Winkelmann et al. 2016), which provides more confidence that the findings are representative of emerging young adults. As compared to similar research, analyses conducted in this study were characterized by a more conservative approach, where potential factors (i.e., BMI, pubertal timing, and depressive symptom severity) that alter cortical development in frontal regions were controlled. Although the study focused on HF-HRV as a metric for HRV due to inclusion in previous studies (Winkelman et al. 2016; Koenig et al. 2018b), effect sizes for RMSSD and CS-adjusted RMSSD were remarkably consistent (R2 = .079–.088) and further replicated the significant finding in the right pgACC during peak stress reactivity. The racial and socioeconomic diversity in the sample extends generalizability of the findings beyond previous samples, which are characterized by a predominantly white and higher socioeconomic status composition. Given that the study sample was entirely 19-year-old females, there is higher internal validity and experimental control when investigating the relationship between cortical thickness and autonomic reactivity. Because adolescent girls have a significantly disproportionate risk for developing many forms of psychopathology than boys (Ge et al. 2001), this study is a valuable addition to the growing literature investigating the neurophysiological biomarkers of adverse mental health outcomes. Consistent with Laborde et al. (2017) recommendations, we also examined both tonic and phasic HRV to provide a more comprehensive and rigorous narrative of the relations between autonomic regulation and neural structure than found in previous research.
An important limitation to consider while interpreting these results is the cross-sectional design. Consequently, causal claims regarding the relation between parasympathetic regulation and cortical thickness of the CAN cannot be drawn from this study. Longitudinal studies are essential to disentangle the effects of stressors from the within-individual variability in cortical thickness expected during typical neurodevelopment. Longitudinal designs can also aim to address the underlying neural mechanisms that accelerate or decelerate cortical thinning across adolescence. Additionally, the homogenous gender and age composition of the study does not allow for generalization to other populations. Future studies could address this concern of limited generalizability with a more balanced demographic distribution. This research could then more precisely evaluate the influence of developmental trajectories across genders, ages, and sociodemographic characteristics. These studies could also compare various measures of stress reactivity to tonic HRV to determine their relative utility in predicting health outcomes.
Extending previous literature, the current study found modest support for a neurodevelopmentally distinct understanding of the relation between autonomic regulation and cortical thickness in a region of the CAN. In this diverse sample of emerging young adult women, there was partial support for a positive association between cortical thickness in right pgACC and parasympathetic response to social stress, but this association was only present with peak HRV reactivity prior to correction for multiple comparisons and sensitivity analyses. Differences in results between previous studies of adolescents versus adults, combined with the limited support for associations between cortical thickness in CAN regions and HRV in previous literature hints that neuromaturation may alter the nature of the relation between brain structure and parasympathetic functioning across adolescence into adulthood. Future work should test the bidirectional relation between top–down control of autonomic function by the prefrontal cortex and bottom-up regulation of vagal activity by the heart to better predict who will develop adverse health outcomes. Furthermore, characterizing processes related to neural regulation of the heart during rest and acute stress reactivity may help identify mechanisms of disruption in stress response systems across development.
Data availability
Data used in the present study can be made available upon request to the primary contact author.
Code availability
Code used in the study can be requested by emailing the primary contact author.
References
Ahern GL, Sollers JJ, Lane RD, Labiner DM, Herring AM, Weinand ME, Thayer JF (2001) Heart rate and heart rate variability changes in the intracarotid sodium amobarbital test. Epilepsia 42(7):912–921
Alosco ML, Stanek KM, Galioto R, Korgaonkar MS, Grieve SM, Brickman AM, Gunstad J (2014) Body mass index and brain structure in healthy children and adolescents. Int J Neurosci 124(1):49–55
Barrett LF, Simmons WK (2015) Interoceptive predictions in the brain. Nat Rev Neurosci 16(7):419
Beauchaine T (2001) Vagal tone, development, and Gray’s motivational theory: toward an integrated model of autonomic nervous system functioning in psychopathology. Dev Psychopathol 13(2):183–214
Beauchaine TP, Cicchetti D (2019) Emotion dysregulation and emerging psychopathology: a transdiagnostic, transdisciplinary perspective. Dev Psychopathol 31(3):799–804
Beauchaine TP, Thayer JF (2015) Heart rate variability as a transdiagnostic biomarker of psychopathology. Int J Psychophysiol 98(2):338–350
Beauchaine TP, Katkin ES, Strassberg Z, Snarr J (2001) Disinhibitory psychopathology in male adolescents: discriminating conduct disorder from attention-deficit/hyperactivity disorder through concurrent assessment of multiple autonomic states. J Abnorm Psychol 110(4):610
Beauchaine TP, Gatzke-Kopp L, Mead HK (2007) Polyvagal theory and developmental psychopathology: emotion dysregulation and conduct problems from preschool to adolescence. Biol Psychol 74(2):174–184
Beauchaine TP, Sauder CL, Derbidge CM, Uyeji LL (2019) Self-injuring adolescent girls exhibit insular cortex volumetric abnormalities that are similar to those seen in adults with borderline personality disorder. Dev Psychopathol 31(4):1203–1212
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J Roy Stat Soc Ser B (Methodol) 57(1):289–300
Berntson GG, Lozano DL, Chen YJ (2005) Filter properties of root mean square successive difference (RMSSD) for heart rate. Psychophysiol 42(2):246–252
Bora E, Fornito A, Pantelis C, Yücel M (2012) Gray matter abnormalities in major depressive disorder: a meta-analysis of voxel based morphometry studies. J Affect Disord 138(1–2):9–18
Bromis K, Calem M, Reinders AA, Williams SC, Kempton MJ (2018) Meta-analysis of 89 structural MRI studies in posttraumatic stress disorder and comparison with major depressive disorder. Am J Psychiatry 175(10):989–998
Carnevali L, Koenig J, Sgoifo A, Ottaviani C (2018) Autonomic and brain morphological predictors of stress resilience. Front Neurosci 12:228
Chahal R, Vilgis V, Grimm KJ, Hipwell AE, Forbes EE, Keenan K, Guyer AE (2018) Girls’ pubertal development is associated with white matter microstructure in late adolescence. NeuroImage 181:659–669
Chalmers JA, Quintana DS, Abbott MJ, Kemp AH (2014) Anxiety disorders are associated with reduced heart rate variability: a meta-analysis. Front Psychiatry 5:80
Chalmers JA, Heathers JA, Abbott MJ, Kemp AH, Quintana DS (2016) Worry is associated with robust reductions in heart rate variability: a transdiagnostic study of anxiety psychopathology. BMC Psychol 4(1):32
Chuang KS, Wan-Cherng Liu NHL, Liu JC (2004) Sympathetic postganglionic and parasympathetic preganglionic neurons innervating the monkey heart. Chin J Physiol 47(2):95–99
Cosco TD, Prina M, Stubbs B, Wu YT (2017) Reliability and validity of the center for epidemiologic studies depression scale in a population-based cohort of middle-aged US adults. J Nurs Meas 25(3):476–485
Critchley HD, Mathias CJ, Josephs O, O’Doherty J, Zanini S, Dewar BK, Dolan RJ (2003) Human cingulate cortex and autonomic control: converging neuroimaging and clinical evidence. Brain 126(10):2139–2152
Dale AM, Sereno MI (1993) Improved localizadon of cortical activity by combining EEG and MEG with MRI cortical surface reconstruction: a linear approach. J Cogn Neurosci 5(2):162–176
Dale AM, Fischl B, Sereno MI (1999) Cortical surface-based analysis: I. Segmentation and surface reconstruction. Neuroimage 9(2):179–194
Davey CG, Yücel M, Allen NB (2008) The emergence of depression in adolescence: development of the prefrontal cortex and the representation of reward. Neurosci Biobehav Rev 32(1):1–19
de Geus EJ, Gianaros PJ, Brindle RC, Jennings JR, Berntson GG (2019) Should heart rate variability be “corrected” for heart rate? biological, quantitative, and interpretive considerations. Psychophysiology 56(2):e13287
Desikan RS, Ségonne F, Fischl B, Quinn BT, Dickerson BC, Blacker D, Albert MS (2006) An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. Neuroimage 31(3):968–980
Destrieux C, Fischl B, Dale A, Halgren E (2010) Automatic parcellation of human cortical gyri and sulci using standard anatomical nomenclature. Neuroimage 53(1):1–15
Drevets WC, Price JL, Furey ML (2008a) Brain structural and functional abnormalities in mood disorders: implications for neurocircuitry models of depression. Brain Struct Funct 213(1–2):93–118
Drevets WC, Savitz J, Trimble M (2008b) The subgenual anterior cingulate cortex in mood disorders. CNS Spectr 13(8):663
Dworkin BR (1993) Learning and physiological regulation. University of Chicago Press, Chicago
Dworkin BR (2000) Interoception. In: Cacioppo JT, Tassinary LG, Berntson GG (eds) Handbook of psychophysiology, 2nd edn. Cambridge University Press, Cambridge, pp 482–506
Ehrenthal JC, Herrmann-Lingen C, Fey M, Schauenburg H (2010) Altered cardiovascular adaptability in depressed patients without heart disease. World J Biol Psychiatry 11(3):586–593
Ellis RJ, Zhu B, Koenig J, Thayer JF, Wang Y (2015) A careful look at ECG sampling frequency and R-peak interpolation on short-term measures of heart rate variability. Physiol Meas 36(9):1827
El-Sheikh M, Hinnant JB, Erath S (2011) Developmental trajectories of delinquency symptoms in childhood: the role of marital conflict and autonomic nervous system activity. J Abnorm Psychol 120(1):16
Etkin A, Egner T, Peraza DM, Kandel ER, Hirsch J (2006) Resolving emotional conflict: a role for the rostral anterior cingulate cortex in modulating activity in the amygdala. Neuron 51(6):871–882
Etkin A, Egner T, Kalisch R (2011) Emotional processing in anterior cingulate and medial prefrontal cortex. Trends Cogn Sci 15(2):85–93
Fallen EL, Kamath MV (1995) Circadian rhythms of heart rate variability. Heart Rate Variability. Futura, New York, Armonk, pp 293–309
Fischl B, Dale AM (2000) Measuring the thickness of the human cerebral cortex from magnetic resonance images. Proc Natl Acad Sci 97(20):11050–11055
Fischl B, Salat DH, Busa E, Albert M, Dieterich M, Haselgrove C, Montillo A (2002) Whole brain segmentation: automated labeling of neuroanatomical structures in the human brain. Neuron 33(3):341–355
Foland-Ross LC, Sacchet MD, Prasad G, Gilbert B, Thompson PM, Gotlib IH (2015) Cortical thickness predicts the first onset of major depression in adolescence. Int J Dev Neurosci 46:125–131
Forbes EE, Dahl RE (2010) Pubertal development and behavior: hormonal activation of social and motivational tendencies. Brain Cogn 72(1):66–72
Frick A, Howner K, Fischer H, Eskildsen SF, Kristiansson M, Furmark T (2013) Cortical thickness alterations in social anxiety disorder. Neurosci Lett 536:52–55
Ge X, Conger RD, Elder GH Jr (2001) Pubertal transition, stressful life events, and the emergence of gender differences in adolescent depressive symptoms. Dev Psychol 37(3):404
Gianaros PJ, Horenstein JA, Cohen S, Matthews KA, Brown SM, Flory JD, Hariri AR (2007) Perigenual anterior cingulate morphology covaries with perceived social standing. Social Cogn Affect Neurosci 2(3):161–173
Goddings AL, Mills KL, Clasen LS, Giedd JN, Viner RM, Blakemore SJ (2014) The influence of puberty on subcortical brain development. Neuroimage 88:242–251
Gogolla N (2017) The insular cortex. Curr Biol 27(12):R580–R586
Goldenberg I, Goldkorn R, Shlomo N, Einhorn M, Levitan J, Kuperstein R, Johnson B (2019) Heart rate variability for risk assessment of myocardial ischemia in patients without known coronary artery disease: the HRV-DETECT (heart rate variability for the detection of myocardial ischemia) study. J Am Heart Assoc 8(24):e014540
Hamilton JL, Alloy LB (2016) Atypical reactivity of heart rate variability to stress and depression across development: systematic review of the literature and directions for future research. Clin Psychol Rev 50:67–79
Hankin BL, Young JF, Abela JR, Smolen A, Jenness JL, Gulley LD, Oppenheimer CW (2015) Depression from childhood into late adolescence: influence of gender, development, genetic susceptibility, and peer stress. J Abnorm Psychol 124(4):803
Herting MM, Sowell ER (2017) Puberty and structural brain development in humans. Front Neuroendocrinol 44:122–137
Hill LK, Siebenbrock A, Sollers JJ, Thayer JF (2009) Are all measures created equal? Heart rate variability and respiration. Biomed Sci Instrum 45:71–76
Hillebrand S, Gast KB, de Mutsert R, Swenne CA, Jukema JW, Middeldorp S, Dekkers OM (2013) Heart rate variability and first cardiovascular event in populations without known cardiovascular disease: meta-analysis and dose–response meta-regression. Europace 15(5):742–749
Hipwell AE, Loeber R, Stouthamer-Loeber M, Keenan K, White HR, Kroneman L (2002) Characteristics of girls with early onset disruptive and antisocial behaviour. Crim Behav Mental Health 12(1):99–118
Hollenstein T, McNeely A, Eastabrook J, Mackey A, Flynn J (2012) Sympathetic and parasympathetic responses to social stress across adolescence. Dev Psychobiol 54(2):207–214
Jandackova VK, Britton A, Malik M, Steptoe A (2016) Heart rate variability and depressive symptoms: a cross-lagged analysis over a 10-year period in the Whitehall II study. Psychol Med 46(10):2121–2131
Keenan K, Hipwell A, Feng X, Babinski D, Hinze A, Rischall M, Henneberger A (2008) Subthreshold symptoms of depression in preadolescent girls are stable and predictive of depressive disorders. J Am Acad Child Adolesc Psychiatry 47(12):1433–1442
Keenan K, Hipwell A, Chung T, Stepp S, Stouthamer-Loeber M, Loeber R, McTigue K (2010) The Pittsburgh girls study: overview and initial findings. J Clin Child Adolesc Psychol 39(4):506–521
Kemp AH, Quintana DS, Gray MA, Felmingham KL, Brown K, Gatt JM (2010) Impact of depression and antidepressant treatment on heart rate variability: a review and meta-analysis. Biol Psychiat 67(11):1067–1074
Kemp AH, Quintana DS, Felmingham KL, Matthews S, Jelinek HF (2012) Depression, comorbid anxiety disorders, and heart rate variability in physically healthy, unmedicated patients: implications for cardiovascular risk. PLoS ONE 7(2):e30777
Kemp AH, Brunoni AR, Santos IS, Nunes MA, Dantas EM, Carvalho de Figueiredo R, Thayer JF (2014) Effects of depression, anxiety, comorbidity, and antidepressants on resting-state heart rate and its variability: an ELSA-Brasil cohort baseline study. Am J Psychiatry 171(12):1328–1334
Kessler RC, Avenevoli S, Merikangas KR (2001) Mood disorders in children and adolescents: an epidemiologic perspective. Biol Psychiat 49(12):1002–1014
Kirschbaum C, Pirke KM, Hellhammer DH (1993) The ‘Trier Social Stress Test’–a tool for investigating psychobiological stress responses in a laboratory setting. Neuropsychobiology 28(1–2):76–81
Koenig J (2020) Neurovisceral regulatory circuits of affective resilience in youth: principal outline of a dynamic model of neurovisceral integration in development. Psychophysiology 57(5):e13568
Koenig J, Thayer JF (2016) Sex differences in healthy human heart rate variability: a meta-analysis. Neurosci Biobehav Rev 64:288–310
Koenig J, Kemp AH, Beauchaine TP, Thayer JF, Kaess M (2016) Depression and resting state heart rate variability in children and adolescents—a systematic review and meta-analysis. Clin Psychol Rev 46:136–150
Koenig J, Rash JA, Campbell TS, Thayer JF, Kaess M (2017) A meta-analysis on sex differences in resting-state vagal activity in children and adolescents. Front Physiol 8:582
Koenig J, Parzer P, Reichl C, Ando A, Thayer JF, Brunner R, Kaess M (2018a) Cortical thickness, resting state heart rate, and heart rate variability in female adolescents. Psychophysiology 55(5):e13043
Koenig J, Westlund Schreiner M, Klimes-Dougan B, Ubani B, Mueller B, Kaess M, Cullen KR (2018b) Brain structural thickness and resting state autonomic function in adolescents with major depression. Social Cognit Affect Neurosci 13(7):741–753
Koenig J, Abler B, Agartz I, Åkerstedt T, Andreassen OA, Anthony M, Quintana DS (2020) Cortical thickness and resting‐state cardiac function across the lifespan: a cross‐sectional pooled mega‐analysis. Psychophysiology. https://doi.org/10.1111/psyp.13688
Kupfer DJ, Frank E, Phillips ML (2012) Major depressive disorder: new clinical, neurobiological, and treatment perspectives. Lancet 379(9820):1045–1055
Laborde S, Mosley E, Thayer JF (2017) Heart rate variability and cardiac vagal tone in psychophysiological research–recommendations for experiment planning, data analysis, and data reporting. Front Psychol 8:213
Lane RD, McRae K, Reiman EM, Chen K, Ahern GL, Thayer JF (2009) Neural correlates of heart rate variability during emotion. Neuroimage 44(1):213–222
Lane RD, Weidenbacher H, Smith R, Fort C, Thayer JF, Allen JJ (2013) Subgenual anterior cingulate cortex activity covariation with cardiac vagal control is altered in depression. J Affect Disord 150(2):565–570
Lewinsohn PM, Seeley JR, Roberts RE, Allen NB (1997) Center for epidemiologic studies depression scale (CES-D) as a screening instrument for depression among community-residing older adults. Psychol Aging 12(2):277
Li Q, Zhao Y, Chen Z, Long J, Dai J, Huang X, Sweeney JA (2020) Meta-analysis of cortical thickness abnormalities in medication-free patients with major depressive disorder. Neuropsychopharmacology 45(4):703–712
Malone IB, Leung KK, Clegg S, Barnes J, Whitwell JL, Ashburner J, Ridgway GR (2015) Accurate automatic estimation of total intracranial volume: a nuisance variable with less nuisance. Neuroimage 104:366–372
Marqués-Iturria I, Pueyo R, Garolera M, Segura B, Junqué C, García-García I, Jurado MÁ (2013) Frontal cortical thinning and subcortical volume reductions in early adulthood obesity. Psychiatry Res Neuroimag 214(2):109–115
Medic N, Ziauddeen H, Ersche KD, Farooqi IS, Bullmore ET, Nathan PJ, Fletcher PC (2016) Increased body mass index is associated with specific regional alterations in brain structure. Int J Obes 40(7):1177–1182
Menon V, Uddin LQ (2010) Saliency, switching, attention and control: a network model of insula function. Brain Struct Funct 214(5–6):655–667
Mills KL, Lalonde F, Clasen LS, Giedd JN, Blakemore SJ (2012) Developmental changes in the structure of the social brain in late childhood and adolescence. Social Cogn Affect Neurosci 9(1):123–131
Monfredi O, Lyashkov AE, Johnsen A-B, Inada S, Schneider H, Wang R, Nirmalan M, Wisloff U, Maltsev VA, Lakatta EG, Zhang H, Boyett MR (2014) Biophysical characterization of the underappreciated and important relationship between heart rate variability and heart rate. Hypertension 64(6):1334–1343
Morandotti N, Dima D, Jogia J, Frangou S, Sala M, De Vidovich GZ, Barale F (2013) Childhood abuse is associated with structural impairment in the ventrolateral prefrontal cortex and aggressiveness in patients with borderline personality disorder. Psychiatry Res Neuroimag 213(1):18–23
Palomero-Gallagher N, Vogt BA, Schleicher A, Mayberg HS, Zilles K (2009) Receptor architecture of human cingulate cortex: evaluation of the four-region neurobiological model. Hum Brain Mapp 30(8):2336–2355
Park G, Vasey MW, Van Bavel JJ, Thayer JF (2014) When tonic cardiac vagal tone predicts changes in phasic vagal tone: the role of fear and perceptual load. Psychophysiology 51(5):419–426
Paus T, Keshavan M, Giedd JN (2008) Why do many psychiatric disorders emerge during adolescence? Nat Rev Neurosci 9(12):947–957
Petersen AC, Crockett L, Richards M, Boxer A (1988) A self-report measure of pubertal status: reliability, validity, and initial norms. J Youth Adolesc 17(2):117–133
Protopopescu X, Pan H, Altemus M, Tuescher O, Polanecsky M, McEwen B, Stern E (2005) Orbitofrontal cortex activity related to emotional processing changes across the menstrual cycle. Proc Natl Acad Sci 102(44):16060–16065
Radley J, Morilak D, Viau V, Campeau S (2015) Chronic stress and brain plasticity: mechanisms underlying adaptive and maladaptive changes and implications for stress-related CNS disorders. Neurosci Biobehav Rev 58:79–91
Radloff LS (1977) The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1(3):385–401
Raji CA, Ho AJ, Parikshak NN, Becker JT, Lopez OL, Kuller LH, Thompson PM (2010) Brain structure and obesity. Hum Brain Mapp 31(3):353–364
Rash JA, Aguirre-Camacho A (2012) Attention-deficit hyperactivity disorder and cardiac vagal control: a systematic review. ADHD Atten Def Hyperact Disord 4(4):167–177
Roos LE, Knight EL, Beauchamp KG, Berkman ET, Faraday K, Hyslop K, Fisher PA (2017) Acute stress impairs inhibitory control based on individual differences in parasympathetic nervous system activity. Biol Psychol 125:58–63
Rottenberg J (2007) Cardiac vagal control in depression: a critical analysis. Biol Psychol 74(2):200–211
Sacher J, Neumann J, Fünfstück T, Soliman A, Villringer A, Schroeter ML (2012) Mapping the depressed brain: a meta-analysis of structural and functional alterations in major depressive disorder. J Affect Disord 140(2):142–148
Salomon K (2005) Respiratory sinus arrhythmia during stress predicts resting respiratory sinus arrhythmia 3 years later in a pediatric sample. Health Psychol 24(1):68–76. https://doi.org/10.1037/0278-6133.24.1.68
Schiller D, Levy I, Niv Y, LeDoux JE, Phelps EA (2008) From fear to safety and back: reversal of fear in the human brain. J Neurosci 28(45):11517–11525
Schiweck C, Piette D, Berckmans D, Claes S, Vrieze E (2019) Heart rate and high frequency heart rate variability during stress as biomarker for clinical depression. A systematic review. Psychol Med 49(2):200–211
Schwerdtfeger A, Derakshan N (2010) The time line of threat processing and vagal withdrawal in response to a self-threatening stressor in cognitive avoidant copers: evidence for vigilance-avoidance theory. Psychophysiology 47(4):786–795
Shang J, Fu Y, Ren Z, Zhang T, Du M, Gong Q, Zhang W (2014) The common traits of the ACC and PFC in anxiety disorders in the DSM-5: meta-analysis of voxel-based morphometry studies. PLoS ONE 9(3):e93432
Shaw P, Kabani NJ, Lerch JP, Eckstrand K, Lenroot R, Gogtay N, Giedd JN (2008) Neurodevelopmental trajectories of the human cerebral cortex. J Neurosci 28(14):3586–3594
Shinba T, Kariya N, Matsui Y, Ozawa N, Matsuda Y, Yamamoto KI (2008) Decrease in heart rate variability response to task is related to anxiety and depressiveness in normal subjects. Psychiatry Clin Neurosci 62(5):603–609
Sisk CL, Zehr JL (2005) Pubertal hormones organize the adolescent brain and behavior. Front Neuroendocrinol 26(3–4):163–174
Stevens FL, Hurley RA, Taber KH (2011) Anterior cingulate cortex: unique role in cognition and emotion. J Neuropsychiatry Clin Neurosci 23(2):121–125
Suh JS, Schneider MA, Minuzzi L, MacQueen GM, Strother SC, Kennedy SH, Frey BN (2019) Cortical thickness in major depressive disorder: a systematic review and meta-analysis. Prog Neuropsychopharmacol Biol Psychiatry 88:287–302
Tamnes CK, Herting MM, Goddings AL, Meuwese R, Blakemore SJ, Dahl RE, Mills KL (2017) Development of the cerebral cortex across adolescence: a multisample study of interrelated longitudinal changes in cortical volume, surface area and thickness. J Neurosci 37:3302–3316
Task Force of the European Society of Cardiology (1996) The North American society of pacing and electrophysiology (1996) Heart rate variability: standards of measurement, physiological interpretation and clinical use. Circulation 93(5):1043–1065
Thayer JF, Lane RD (2000) A model of neurovisceral integration in emotion regulation and dysregulation. J Affect Disord 61(3):201–216
Thayer JF, Lane RD (2007) The role of vagal function in the risk for cardiovascular disease and mortality. Biol Psychol 74(2):224–242
Thayer JF, Lane RD (2009) Claude Bernard and the heart–brain connection: further elaboration of a model of neurovisceral integration. Neurosci Biobehav Rev 33(2):81–88
Thayer JF, Sternberg E (2006) Beyond heart rate variability: vagal regulation of allostatic systems. Ann NY Acad Sci 1088(1):361–372
Thayer JF, Hansen AL, Saus-Rose E, Johnsen BH (2009) Heart rate variability, prefrontal neural function, and cognitive performance: the neurovisceral integration perspective on self-regulation, adaptation, and health. Ann Behav Med 37(2):141–153
Thayer JF, Yamamoto SS, Brosschot JF (2010) The relationship of autonomic imbalance, heart rate variability and cardiovascular disease risk factors. Int J Cardiol 141(2):122–131
Thayer JF, Åhs F, Fredrikson M, Sollers JJ III, Wager TD (2012) A meta-analysis of heart rate variability and neuroimaging studies: implications for heart rate variability as a marker of stress and health. Neurosci Biobehav Rev 36(2):747–756
Van Reekum CM, Urry HL, Johnstone T, Thurow ME, Frye CJ, Jackson CA, Davidson RJ (2007) Individual differences in amygdala and ventromedial prefrontal cortex activity are associated with evaluation speed and psychological well-being. J Cogn Neurosci 19(2):237–248
Vasilev CA, Crowell SE, Beauchaine TP, Mead HK, Gatzke-Kopp LM (2009) Correspondence between physiological and self-report measures of emotion dysregulation: a longitudinal investigation of youth with and without psychopathology. J Child Psychol Psychiatry 50(11):1357–1364
Vijayakumar N, Whittle S, Yücel M, Dennison M, Simmons J, Allen NB (2014) Thinning of the lateral prefrontal cortex during adolescence predicts emotion regulation in females. Social Cogn Affect Neurosci 9(11):1845–1854
Vijayakumar N, Allen NB, Youssef G, Dennison M, Yücel M, Simmons JG, Whittle S (2016) Brain development during adolescence: a mixed-longitudinal investigation of cortical thickness, surface area, and volume. Hum Brain Mapp 37(6):2027–2038
Vogt BA (2005) Pain and emotion interactions in subregions of the cingulate gyrus. Nat Rev Neurosci 6(7):533
Wagner G, Koch K, Schachtzabel C, Reichenbach JR, Sauer H, Schlösser RG (2008) Enhanced rostral anterior cingulate cortex activation during cognitive control is related to orbitofrontal volume reduction in unipolar depression. J Psychiatry Neurosci JPN 33(3):199
Williams DP, Joseph N, Sones E, Chetluru S, Hillecke TK, Thayer JF, Koenig J (2017) Effects of body mass index on parasympathetic nervous system reactivity and recovery following orthostatic stress. J Nutrit Health Aging 21(10):1250–1253
Winkelmann T, Thayer JF, Pohlack S, Nees F, Grimm O, Flor H (2016) Structural brain correlates of heart rate variability in a healthy young adult population. Brain Struc Funct 222(2):1061–1068
Winkler AM, Kochunov P, Blangero J, Almasy L, Zilles K, Fox PT, Glahn DC (2010) Cortical thickness or grey matter volume? The importance of selecting the phenotype for imaging genetics studies. Neuroimage 53(3):1135–1146
Woodward SH, Kaloupek DG, Streeter CC, Martinez C, Schaer M, Eliez S (2006) Decreased anterior cingulate volume in combat-related PTSD. Biol Psychiat 59(7):582–587
Woodward SH, Kaloupek DG, Schaer M, Martinez C, Eliez S (2008) Right anterior cingulate cortical volume covaries with respiratory sinus arrhythmia magnitude in combat veterans. J Rehabil Res Dev 45(3):451
Yoo HJ, Thayer JF, Greening S, Lee TH, Ponzio A, Min J, Koenig J (2018) Brain structural concomitants of resting state heart rate variability in the young and old: evidence from two independent samples. Brain Struct Funct 223(2):727–737
Acknowledgements
We are grateful to all the families who took part in this study, and to the PGS team, which includes interviewers and their supervisors, data managers, student workers and volunteers. This research was specifically funded by R01-MH093605, R01-MH66167, R01-MH56630, R01-HD067185 and K01-MH103511.
Funding
This study was funded by R01-MH093605, R01-MH66167, R01-MH56630, R01-HD067185 and K01-MH103511.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no relevant financial or non-financial conflicts of interest among the authors to disclose.
Ethical approval
Approval was obtained from the University of Pittsburgh Institutional Review Board.
Consent to participate
Informed consent was obtained from the caregiver and verbal assent was obtained from the child prior to initial collection of data at intake.
Consent for publication
Participants consented to the submission of non-identifiable data for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fridman✉, A.J., Yang, X., Vilgis, V. et al. Brain structure and parasympathetic function during rest and stress in young adult women. Brain Struct Funct 226, 1195–1207 (2021). https://doi.org/10.1007/s00429-021-02234-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00429-021-02234-7