Abstract
Purpose
We determine the clinical characteristics, visual and anatomical outcomes, and factors associated with poor visual outcome and anatomical success in pediatric open-globe injuries (OGI).
Methods
The records of patients aged 17 years and younger who had undergone surgical intervention after OGI between January 2000 and June 2010 were reviewed retrospectively.
Results
In total, 182 patients were enrolled in the study (70.9 % males, 29.1 % females; mean age: 8.6 ± 4.5 years [range 1–17 years]). Injuries occurred mostly at home (45.1 %). Objects most often causing the ocular trauma were sharp objects (74.1 %). Over one-third of the eyes (39.7 %) had final visual acuities of 20/200 or better. Anatomical success was achieved in 76.9 % of eyes. Time between primary globe repair and secondary surgical intervention was 61.4 ± 144 days. Visual outcomes were poor in eyes with initial visual acuity less than for counting fingers, retinal detachment, proliferative vitreoretinopathy, and endophthalmitis. Anatomical success rates were low with retinal detachment.
Conclusion
Visual outcomes seem to be poor in more than half of the patients despite advanced microsurgical techniques.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ocular trauma is the leading cause of monocular vision loss in children [1, 2]. Although eye injuries occur suddenly and unexpectedly, previous studies have indicated that up to 90 % of eye injuries are preventable with education, adult supervision, and protective eyewear [3]. Despite advanced medical and surgical techniques and increased understanding of the mechanisms of trauma, amblyopia seems to be a challenging problem during rehabilitation after ocular trauma [4].
Ocular trauma may cause either open-globe injuries (OGI) or closed-globe injuries (CGI). CGI constitute a large proportion of mechanical globe injuries in childhood, but visual and anatomical outcomes seem to be poorer in OGI than CGI [5–9]. There have been limited and conflicting studies on the prognosis of OGI and factors affecting the prognosis [4–6, 10–16]. Therefore, there is still a need for detailed reports to increase our understanding of this potentially sight-threatening injury.
The aim of this study is to determine the clinical characteristics, visual and anatomical outcomes, and factors associated with poor visual and anatomical outcomes in OGI.
Materials and methods
We reviewed the records of the Gazi University Faculty of Medicine (Ankara, Turkey), Department of Ophthalmology, from the period January 2000 until June 2010 for consecutive patients aged 17 years and younger who needed surgical intervention after OGI.
Written informed consent was obtained from all of the patients or their relatives. Our study was reviewed and approved by the ethics committee of the Gazi University Faculty of Medicine.
Epidemiological characteristics such as age, gender, causative agent, and place were reviewed. We determined clinical characteristics (anterior and posterior segment findings), initial and final visual acuities (VAs), mean number of surgeries, follow-up time, and mean age at last follow-up from each patient’s records. Initial VA was defined as VA at presentation before the primary globe repair. Initial VAs of the referrals were accessed from the records of other clinics. VAs were measured using a Snellen chart. OGI was classified according to Birmingham Eye Trauma Terminology [10]. The time between the trauma and the primary repair of the globe could be determined only in eyes that were operated on at Gazi University. The time between the primary surgical repair and the secondary surgical intervention was identified in each patient. All patients who were under the age of 10, had strict amblyopia treatment with best-spectacle correction and occlusion therapy after surgical interventions.
Poor visual outcome was defined as a final VA less than 20/200, according to a previous study [4]. Anatomical success was defined as persisting retinal attachment and/or no phthisis bulbi at the last follow-up visit. We analyzed the factors associated with poor visual outcome and anatomical success.
We summarized the data using descriptive statistics (e.g., mean, standard deviation, frequency, percentage). We used Student’s t-test to determine and compare the means, and we used the chi-squared (χ 2) test for the categorical data. The clinical variables that were associated with visual outcome and anatomical success in the χ2 test were included in a regression model to better delineate the effects of the clinical variables on visual outcome and anatomical success. The Statistical Package for the Social Sciences (SPSS) software (version 16.0 for Windows, SPSS Inc., Chicago, Illinois, USA) was used for all of the analysis. A p value of less than 0.05 was considered to indicate statistical significance.
Results
We identified 182 eyes in 182 patients during the 10-year period. There were 129 males (70.9 %) and 53 females (29.1 %) (male:female ratio: 2.4:1). The mean age of the cohort was 8.6 ± 4.5 years (range; 1–17 years). The mean age at the last follow-up was 10.1 ± 4.3 years (range; 1–19 years).
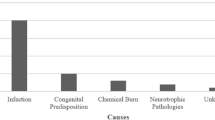
The place of injury was determined in 144 patients (79.1 %). Most of the injuries occurred at home (45.1 %) (Table 1). In 163 patients, the injury sources were identified: 135 sharp objects (74.1 %) [the most frequent sharp objects were knives in 26 injuries (14.3 %)], 20 projectiles (10.9 %), and 8 blunt objects (4.3 %) (Table 1).
Forty-three eyes with OGI (23.6 %) had undergone primary surgical repair at our clinic. Twenty-one out of 43 eyes underwent only primary surgical repair (20 eyes underwent primary surgical repair and one eye underwent primary surgical repair combined with lensectomy and intraocular lens implantation). Twenty-two out of 43 eyes needed further surgical management. The remaining 139 eyes underwent primary surgical repair at other clinics and were referred to our hospital for further surgical management.
All patients underwent primary surgical repair within 48 hours of initial trauma. One hundred and sixty-three patients (89.5 %) presented within 24 hours, 19 (10.5 %) patients between 24–48 hours of trauma. The mean time between the trauma and the primary surgical repair was 12.3 ± 5.5 hours (range; 5–35 hours) in 43 patients who were operated on at Gazi University. We could not determine the mean time between the trauma and the primary surgical repair in referrals due to lack of information for the exact primary surgical repair time in some patients.
One hundred and sixty-one eyes underwent secondary surgical interventions (surgeries for cataract, secondary lens implantation, vitreous hemorrhage, retinal detachment [RD], intraocular foreign body [IOFB] removal and endophthalmitis). The mean time between the primary repair of the globe and the secondary surgical interventions was 61.4 ± 144 days (range 2–1460 days). The mean follow-up time was 18.2 ± 17.8 months (range; 6–120 months).
Ocular findings and visual outcomes
One hundred and forty-three eyes (78.5 %) had penetrating injuries, 12 eyes (6.7 %) had ruptures, and 27 eyes (14.8 %) had IOFB. There were no perforating injuries.
The most common ocular findings were corneal lacerations or scars (58.7 %) and RD (51.6 %) (Table 2).
Initial VA was determined in 166 patients and final VA was determined in 174 patients at the last follow-up (Table 3). The initial VA was 20/200 or better in ten eyes (5.4 %). At the last follow-up visit, 69 eyes (37.9 %) had a final VA of 20/200 or better. Patients who had initial VAs counting fingers (CF) or greater had significantly better final VAs than patients who had initial VAs less than CF (63.4 % vs. 32 %) (Table 4).
The mean patient age was 9.9 ± 4.6 years in eyes that had final VAs of 20/200 or better and 8.3 ± 4.1 years in eyes that had final VAs less than 20/200; the difference was statistically significant (t-test, p = 0.013).
One hundred and thirty-four eyes (73.6 %) had posterior segment involvement, and 48 eyes (26.4 %) had isolated anterior segment injury. Final VA was less than 20/200 in 96 out of 130 eyes (73.8 %) with posterior segment involvement and in nine out of 44 eyes (20.5 %) with isolated anterior segment injury (p < 0.001). All patients who needed secondary vitreoretinal interventions were operated on within two weeks of the primary repair of the globe or admission to our hospital. The mean number of vitreoretinal surgeries in eyes with posterior segment injury was 1.52 ± 0.68 (range: 1–3). Five eyes underwent primary globe repair in our clinic but they were concluded to be inoperable for the secondary reconstructive surgery.
Vitreous hemorrhage was detected in 56 eyes. There was accompanying RD in 36 eyes and proliferative vitreoretinopathy (PVR) in 15 eyes. Final VA was 20/200 or better in 17 eyes (30.4 %).
RD was seen in 94 eyes (51.6 %). Eighty eyes (85 %) had rhegmatogen RD and 14 eyes (15 %) had combined rhegmatogen and tractional RD. Macula was involved in all patients. RD was detected immediately after primary surgical repair in 22 eyes (23.4 %) and during the control examinations in the remaining 72 eyes (76.4 %). In 31 eyes (32.9 %), there was total RD. Retinal incarceration was detected in 13 eyes (13.8 %) and retinal dialysis in 11 eyes (11.7 %). PVR was detected in 52 eyes (55.3 %). The mean number of surgeries in eyes with RD was 1.69 ± 0.72 (range; 1–3). The mean number of surgeries in eyes with PVR was 1.78 ± 0.75 (range; 1–3). In 18 eyes (19.6 %), the final VA was 20/200 or better. In 56 eyes (59.6 %), anatomical success was achieved. In 28 out of 56 eyes (50 %), anatomical success was achieved with one surgery.
The following types of IOFB were identified; nine metallic foreign bodies, four gunshots , four pieces of stone, three nails, two pieces of fireworks, two pieces of wire, one air-gun shot, and one piece of glass. Two eyes underwent primary repair at our clinic, and 25 eyes underwent primary repair at other clinics and were sent for IOFB removal. The mean time for IOFB removal was 21.3 ± 14.7 days (range; 1–60 days). Of the eyes with IOFB, endophthalmitis was seen in four eyes (14.8 %). All of these eyes had been injured with a metallic foreign body. In 14 eyes (53.8 %), the final VA was 20/200 or better.
Endophthalmitis was seen in 22 patients (12.1 %). Four eyes had undergone primary surgical repair at Gazi University. Three out of four eyes had undergone primary surgical repair more than 24 hours after the trauma. In these four eyes, mean time between the trauma and the primary surgical repair was 27.7 ± 5.9 hours (range; 22–35 hours). Of the referrals, 13 out of 18 eyes underwent primary surgical repair more than 24 hours, and five out of 18 eyes within 24 hours after the trauma. The mean time between the trauma and the primary surgical repair could not be determined due to lack of information about the exact primary repair time in some patients. In three eyes, intravitreal tap and vancomycin (1 mg/ml)-ceftazidime (2.25 mg/ml) injections were performed. In 19 eyes vitrectomy combined with intravitreal vancomycin-ceftazidime was performed for the reasons of IOFB removal, RD, and vitritis. The cultures were positive in four eyes; two were staphylococcus aureus, and two were staphylococcus epidermidis. RD was detected in 11 eyes (50 %); in three eyes, endophthalmitis was present, in eight eyes RD developed after endophthalmitis treatment. In three eyes (15 %), the final VA was 20/200 or greater at the final follow-up.
Factors associated with functional and anatomical success
Posterior segment involvement, glob rupture, an initial VA less than CF, RD, PVR and endophthalmitis were associated with poor visual outcome (Tables 4 and 5). RD and glob rupture were also associated with anatomical failure (Tables 6 and 7). Furthermore, phthisis bulbi was more frequent in ruptures (3/12 eyes; 25 %) than penetrating injuries (8/145 eyes; 5.3 %), and the difference was statistically significant (p = 0.04).
Discussion
In this retrospective study, we summarized the clinical characteristics of pediatric OGI in our clinic. We found that OGIs were mostly seen in males (male:female ratio: 2.4:1), as reported by other studies [11, 12, 17]. In the literature, OGI occurs in up to 60 % of cases at home; 32–79 % of injuries caused by sharp objects [4, 5, 18–20]. Our findings are consistent with literature results that most of the injuries occurred at home (45.1 %) and were caused by sharp objects (71 %). A lack of safety, preventative measures, and adult supervision are thought to be the main reasons for the high incidence of OGI at home and injuries due to sharp objects.
A young age and low initial VA were shown to be poor prognostic factors in OGI [4, 12–14]. Younger patients are more susceptible to amblyopia and are expected to have a worse visual outcome. We compared the mean age between the patients with final VA better or worse than 20/200 with the t-test (univariate analysis). The patients with worse final VA were significantly younger than patients with better final VA. Furthermore, children with an initial VA less than CF had significantly worse final VA than children with better initial VA.
Wound localization did not significantly affect functional success, although scleral injuries (i.e., more posterior lacerations) were associated with poorer visual outcomes, as suggested by previous studies [6, 15, 16, 21]. Injuries involving the posterior segment had a significantly worse final VA, as in the reports of Bunting et al. and Tok et al. [22, 23].
Other factors associated with poor visual outcome were globe rupture, RD, PVR, and endophthalmitis. Factors associated with anatomical failure were globe rupture and RD.
Globe ruptures had poor anatomical and visual outcomes in our study, consistent with the results of Farr et al. [11] that 41 % of OGI caused by blunt trauma had a final VA less than 5/200. Furthermore, the number of phthisis bulbi was significantly higher for ruptured globes.
Trauma is the most frequent cause of RD in childhood [24]. In the present study, despite the high anatomical success due to improved surgical techniques, the visual outcome was low, similar to previous studies [21, 24, 25]. Delayed diagnosis is a significant feature of RD. Only 23.4 % eyes had immediate diagnosis, in the remaining patients RD was detected in the control examinations. In other words, we do not definitely know how many patients had diagnoses of RD and were promptly referred for surgical management . An RD diagnosis after OGI in a pediatric population is difficult due to their lack of awareness of visual deterioration owing to young age, corneal scar, lens opacification, and vitreous hemorrhage. Delays in surgical intervention, which can be connected with high preoperative PVR rates in our study, may be associated with delayed diagnoses. Furthermore, half of the eyes had two or more surgeries in anatomically successful cases. Additionally, macular attachment before surgery has been associated with a good visual outcome by some previous reports [24, 26]. However in our study, all patients had macula off RD. Therefore, delays in surgical intervention, anatomical failures after surgical intervention and macula off status before surgery can cause irreversible damage to the macula and amblyopia that are thought to be the main reasons for the low functional successes in the treatment of traumatic RD [4, 24, 26].
PVR is seen in up to 64 % of traumatic pediatric RD cases and is the most frequent cause of anatomical failure after surgical intervention [26]. In our study, however, anatomical success was not associated with PVR, visual outcomes were significantly lower in eyes with PVR.
In this study, the majority of the IOFBs were metallic, similar to the literature [27, 28]. Some authors have advised that IOFB be removed within 24 hours due to the high risk of endophthalmitis and the risk of PVR [29, 30]. However, in a recent study, there was no correlation with the time of IOFB removal and functional success [31]. In this same study, endophthalmitis did not develop with oral and topical antibiotic use. In our investigation, the mean time for IOFB removal seems to be long (21 days). Most of the IOFB cases were referrals and the prolonged removal time may be due to a failure to diagnose IOFB or the delay in referring patients. Despite the mean long removal time, the rate of endophthalmitis (14.8 %) is considered to be acceptable. We consider that IOFB removal can be delayed for a while unless acute intoxication or endophthalmitis is present.
The reported frequency of endophthalmitis after OGI varies from 6.8 % to 54.2 % [6, 31, 32]. In our study, endophthalmitis was detected in 22 patients (12.1 %). As reported in previous studies, the final VA was worse in eyes with endophthalmitis in this study. The cultures were positive in four vitreus specimens and all of them were staphylococcus species. Delayed repair was associated with the development of endophthalmitis [33]. We also found that, 16 out of 22 eyes had undergone primary surgical repair more than 24 hours after trauma, which reveals the importance of immediate repair of OGI (as shown by the literature). RD is seen in up to 57 % of eyes with endophthalmitis [34]. In our study, 11 eyes (50 %) with endophthalmitis had RD, and in eight of them RD developed after endophthalmitis treatment (late RD). This result highlights the importance of following these eyes for RD development even after endophthalmitis treatment.
In conclusion, more than half of the eyes seem to be legally blind despite advanced microsurgical techniques combined with strict amblyopia treatment after OGI that were shown to be 90 % preventable. The high PVR rates in eyes with RD and the prolonged time for IOFB removal may be the result of delays at first surgical intervention after the primary repair of the globe. These high rates can be attributed to the inadequate compliance of patients in terms of follow-up examinations, delays in referring or admission to our hospital. The relatives or parents should be strictly warned and clinicians should take care to have timely examinations and surgical interventions, which is important for removing amblyogenic factors such as cataracts, vitreous hemorrhage, and RD.
All authors certify that they have no affliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speaker’s bureaus; membership employment, consultancies, stock ownership, or other equity interest; and expert testimony or patient-licensing arrangements), or non-financial interest (such as personal or professional relationships, affliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
References
May DR, Kuhn FP, Morris RE et al (2000) The epidemiology of serious eye injuries from the United States Eye Injury Registry. Graefes Arch Clin Exp Ophthalmol 238:153–157
Sternberg P, deJuan E, Michels R (1984) Penetrating ocular injuries in young patients. Initial injuries and visual results. Retina 4:5–8
Coody D, Banks JM, Yetman RJ, Musgrove K (1997) Eye trauma in children: epidemiology, management, and prevention. J Pediatr Health Care 11:182–188
Jandeck C, Kellner U, Bornfeld N et al (2000) Open globe injuries in children. Graefes Arch Clin Exp Ophthalmol 238:420–426
Serrano JC, Chalela P, Arias JD (2003) Epidemiology of childhood ocular trauma in a northeastern Colombian region. Arch Ophthalmol 121:1439–1445
Lee CH, Su WY, Lee L, Yang ML (2008) Pediatric ocular trauma in Taiwan. Chang Gung Med J 31:59–65
Strahlman E, Elman M, Daub E et al (1990) Causes of pediatric eye injuries. A population based study. Arch Ophthalmol 108:603–606
Karaman K, Znaor L, Lakos V, Olujic I (2009) Epidemiology of pediatrice eye injury in Split-Dalmatia County. Ophthalmic Res 42:199–204
Liu ML, Chang YS, Tseng SH et al (2010) Major pediatric ocular trauma in Taiwan. J Pediatr Ophthalmol Strabismus 47:88–95
Kuhn F, Morris R, Witherspoon D et al (1996) A standard classification of ocular trauma. Graefes Arch Clin Exp Ophthalmol 234:399–403
Farr AK, Hairston RJ, Humayun MU et al (2001) Open globe injuries in children: a retrospective analysis. J Pediatr Ophthalmol Strabismus 38:72–77
Baxter RJ, Hodgkins PR, Calder I, Morrell AJ, Vardy S, Elkington AR (1994) Visual outcome of childhood anterior perforating eye injuries: prognostic indicators. Eye 8:349–352
Gupta A, Rahman I, Leatherbarrow B (2009) Open globe injuries in children: factors predictive of a poor final visual acuity. Eye 23:621–625
Rostomianm K, Thach AB, Isfahani A, Pakkar A, Pakkar A, Borchert M (1998) Open globe injuries in children. J AAPOS 2:234–238
De Juan E, Sternberg P, Michels RG (1983) Penetrating ocular injuries: types of injuries and visual results. Ophthalmology 90:1318–1322
Lesniak SP, Bauza A, Son JH et al (2012) Twelve-year review of pediatric traumatic open globe injuries in an urban U.S. population. J Pediatr Ophthalmol Strabismus 49:73–79
Rudd JC, Jaeger EA, Freitag SK, Jeffers JB (1994) Traumatically ruptured globes in children. J Pediatr Ophthalmol Strabismus 31:307–311
Hill JR, Crawford BD, Lee H, Tawansy KA (2006) Evaluation of open globe injuries of children in the last 12 years. Retina 26:65–68
MacEwen CJ, Baines PS, Desai P (1999) Eye injuries in children: the current picture. Br J Ophthalmol 83:933–936
Soylu M, Demircan N, Yalaz M, Isiguzel (1998) Etiology of pediatric perforating eye injuries in southern Turkey. Ophthalmic Epidemiol 5:7–12
Moisseiev J, Vidne O, Treister G (1998) Vitrectomy and silicone oil injection in pediatric patients. Retina 18:221–227
Bunting H, Stephens D, Mireskandar K (2013) Prediction of visual outcomes after open globe injury in children: a 17-year Canadian experience. J AAPOS 17:43–48
Tok O, Tok L, Ozkaya D, Eraslan E, Ornek F, Bardak Y (2011) Epidemiological characteristics and visual outcome after open globe injuries in children. J AAPOS 15(6):556–561
Sarrazin L, Averbukh E, Halpert M, Hemo I, Rumelt S (2004) Traumatic pediatric retinal detachment: a comparison between open and closed globe injuries. Am J Ophthalmol 137:1042–1049
Sheard RM, Mireskandari K, Ezra E, Sullivan PM (2007) Vitreoretinal surgery after childhood ocular trauma. Eye 21:793–798
Wang NK, Chen YP, Yeung L et al (2007) Traumatic pediatric retinal detachment following open globe injury. Ophthalmologica 221:255–263
Greven CM, Engelbrecht NE, Slusher MM, Nagy SS (2000) Intraocular foreign bodies: management, prognostic factors, and visual outcomes. Ophthalmology 107:608–617
Williams DF, Mieler WF, Abrams GW et al (1988) Results and prognostic factors in penetrating ocular injuries with retained intraocular foreign bodies. Ophthalmology 95:911–916
Jonas JB, Budde WM (1999) Early versus late removal of intraocular foreign bodies. Retina 19:193–197
Jonas JB, Knorr HL, Budde WM (2000) Prognostic factors in ocular injuries caused by intraocular or retrobulbar foreign bodies. Ophthalmology 107:823–828
Colyer MH, Weber ED, Weichel ED et al (2007) Delayed intraocular foreign body removal without endophthalmitis during Operations Iraqi Freedom and Enduring Freedom. Ophthalmology 114:1439–1447
Essex RW, Yi Q, Charles PG et al (2004) Post-traumatic endophthalmitis. Ophthalmology 111:2015–2022
Narang S, Gupta V, Simalandhi P et al (2004) Paediatric open globe injuries: visual outcome and risk factors for endophthalmitis. Indian J Ophthalmol 52:29–34
Thordsen JE, Harris L, Hubbard GB (2008) Pediatric endophthalmitis. A 10-year consecutive series. Retina 28:3–7
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sul, S., Gurelik, G., Korkmaz, S. et al. Pediatric open-globe injuries: clinical characteristics and factors associated with poor visual and anatomical success. Graefes Arch Clin Exp Ophthalmol 254, 1405–1410 (2016). https://doi.org/10.1007/s00417-015-3087-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-3087-y