Abstract
Introduction
Accumulating evidence shows that SQSTM1 plays a vital role in the pathogenesis of frontotemporal dementia (FTD) and amyotrophic lateral sclerosis (ALS), which represent a neurodegenerative disease continuum. Here, we report a novel SQSTM1 variant in a patient presenting with progressive nonfluent aphasia (PNFA) and progressive bulbar palsy (PBP). Relevant literature about FTD and FTD-ALS caused by SQSTM1 mutation was reviewed to better understand its clinical features.
Methods
We collected data from a 66-year-old male patient with a novel heterozygous variant (c.995C > G, p.S332X) in the SQSTM1 gene who was diagnosed with PNFA and PBP and performed a PubMed literature search using the advanced research criteria: [(“frontotemporal lobar degeneration”) OR (“frontotemporal dementia”) OR (“amyotrophic lateral sclerosis”) OR (“motor neuron disease”)] AND (“SQSTM1”). The clinical features of FTD and FTD-ALS related to SQSTM1 mutation were summarized based on previous cases and our new case.
Results
The initial symptom of the current patient was progressive verb finding difficulties and effortful speech output, which developed into dysarthria and dysphagia in subsequent months. The results, including tongue atrophy, fasciculations, neurogenic changes, and mild left dominant hypometabolism of 18F-fluorodeoxyglucose PET in the frontal cortex, suggest the possibility of PNFA and PBP. A novel likely pathogenic heterozygous variant (c.995C > G, p.S332X) in the SQSTM1 gene was identified. The literature search revealed a total of 33 FTD and FTD-ALS cases related to the SQSTM1 mutation with detailed clinical information. The mean age of onset (including our patient) was 63.5 ± 9.7 years. bvFTD was the most common clinical phenotype. The missense mutation in the SQSTM1 gene coding region and the UBA domain involvement are its main genetic characteristics.
Conclusion
Although rare, mutations in SQSTM1 can lead to various clinical subtypes of FTD and FTD-ALS, including the rare combination of PNFA and PBP. Exon missense mutation is the main type of mutation, which is common in the UBA domain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
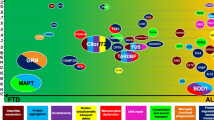
Frontotemporal dementia (FTD) is the second most common dementia subtype under 65 years and is characterized by selective frontal and temporal lobe atrophy [1]. FTD has two main clinical variant: the primary progressive aphasia variant—either semantic and nonfluent—and the behavioral variant [2]. In addition, an increasing number of studies suggest substantial overlap between FTD and motor neuron disease (MND) syndrome with respect to clinical and pathological features and genotype [3]. Now, they are thought to belong to the same clinicopathological spectrum of disorders [4]. Unlike AD, FTD has a stronger genetic background, and the most frequently mutated genes are chromosome 9 open reading frame 72 (C9orf 72), progranulin (GRN), and microtubule-associated protein tau (MAPT) [5]. The SQSTM1 gene is located at 5q35 and encodes protein P62 consisting of 440 amino acids that mediates various biological processes, including intracellular signaling, oxidative stress response, and apoptosis [6]. Mutations in the SQSTM1 gene were initially identified as a cause of Paget’s disease of bone (PDB) [7]. In recent years, it has been found in patients with FTD and FTD with amyotrophic lateral sclerosis (ALS) (FTD-ALS) [8,9,10]. As a relatively rare gene type of FTD, its clinical and genetic characteristics are not fully understood. Here, we report a patient clinically diagnosed with PNFA and progressive bulbar palsy (PBP), whose genetic tests suggest new variant in the SQSTM1 gene. Moreover, we reviewed the literature on FTD and FTD-ALS caused by SQSTM1 mutation and then summarized their clinical and genetic characteristics, hoping to improve the understanding of its clinical features.
Materials and methods
-
1.
Clinical data collection: the clinical history, physical examination, laboratory examination, imaging examination and cognitive evaluation of the patient were collected.
-
2.
Genetic procedures: DNA was prepared and amplified from peripheral blood according to standard procedures from the patient after informed consent was obtained for genetic studies. The quality of DNA was assessed by agarose gel electrophoresis and Qubit 3.0 (Thermo Fisher, USA). Libraries were prepared using the SureSelectXT Target Enrichment System Manual (Agilent, USA), and whole-exome sequencing was performed by HiSeq X Ten (Illumina, USA). Next-generation sequencing and bioinformatics analysis of the sequencing data, including MAPT, GRN, CHMP2B, C9orf 72, VCP, FUS, SQSTM1, SOD1, TARDBP, OPTN, APP, PSEN1 and PSEN2, were performed. A nonsense variant in the SQSTM1 gene was found and was subsequently Sanger sequenced (forward primer: 5′-AGCGTCTGCCCAGACTACGA-3′ and reverse primer: 5′-CAGGCACTTAGGCACCTCAG-3′). The pathogenicity of detected variant was predicted by Mutation Taster software (https://www.mutationtaster.org/).
-
3.
Literature review: a literature review was carried out from articles published in PubMed using the advanced research criteria: [(“frontotemporal lobar degeneration”) OR (“frontotemporal dementia”) OR (“amyotrophic lateral sclerosis”)] OR (“motor neuron disease”)] AND (“SQSTM1”) to search all previous FTD and FTD-ALS cases with SQSTM1 mutation. The cases with detailed medical histories were analyzed and summarized.
This study was approved by the Ethics Committee of Shengjing Hospital of China Medical University, and was conducted in accordance with the Declaration of Helsinki.
Results
Case report
A right-handed 66-year-old man with 9 years of education was referred to our hospital in March 2020 for assessment of a progressive language disorder that had started 1 year earlier, which were characterized by difficulty in speaking, finding words, poor expression, pause in the middle of long sentences, comprehension of the meaning of a single word and semantic memory are normal, while comprehension of grammatically complex sentences is impaired. The impairment of memory is not obvious. At the time of referral, the patient showed significant dysphagia and dysdipsia, and apraxia of speech, accompanied by stuttering, frequent speech and phoneme errors, and increasingly severe expressive agrammatism. His wife reported that he was more irritable due to his difficulties in communication and independent in all activities of daily living. Physical examination revealed clear consciousness, dysarthria, soft palate elevation weakness, reduced pharyngeal reflex, tongue atrophy and fasciculations, normal limb muscle strength and muscle volume, positive palm–chin reflex and pathological crying and laughing, and negative bilateral Babinski sign. Routine biochemistry, thyroid function, folic acid, vitamin B12, and blood HIV, treponema pallidus, tumor markers, and parathyroid antibody were normal. His MiniMental State Examination score was 26/30. The ADL score was 22 (20 items). The results of a standard language test for aphasia by the Aphasia Battery of Chinese (ABC) show that the information volume, word fluency and retelling ability of oral expression are significantly lower than healthy people (Fig. 1a). Brain MRI showed no significant abnormality (Fig. 1b). 18F-Fluorodeoxyglucose PET revealed mild left dominant hypometabolism in the frontal cortex (Fig. 1c). Determination of nerve conduction velocity no abnormality was found. Electromyography (EMG) showed fibrillation potentials and positive sharp waves, with longer duration and higher amplitude of MUAP in tongue muscles with normal findings on limbs, sternocleidomastoid muscle and lower thoracic paraspinal muscles. The patient’s parents are deceased, the only son currently has no neurological clinical symptoms, and other members’ information were not available.
Genetic analysis
The variant c.995 C > G, p.S332X of SQSTM1 was detected in the patient and validated by Sanger sequencing (Fig. 2a). This variant has not been reported elsewhere and has not been found in the human gene mutation database (HGMD), 1000 Genomes Project or ExAC database. Bioinformatics analysis indicated that the protein expression was truncated, while MutationTaster software predicted that it was harmful and located at a highly conserved position (Fig. 2b). According to the standard references of the American Society of Medical Genetics and Genomics (ACMG) [11], it was determined to be likely pathogenic.
Clinical and genetic features
A total of 51 patients with FTD and FTD-ALS caused by SQSTM1 mutation were searched [8,9,10, 12,13,14,15,16], of which 34 patients with relatively complete clinical and genetic data were collected and summarized (including our case) (Table 1). More than half of them (20/30) were male, and 60% of them had a family history of dementia (20/34). The mean age of onset was 63.5 ± 9.7 (41–79) years (male 64.2 ± 9.4 years, female 58.8 ± 9.1 years), and most of the patients were older than 60 years [< 50 years (4/34), 50–60 years (8/34), 60–70 years (10/34), and > 70 years (12/34)[, the duration of illness of 14 dead patients was 7.2 ± 4.8 (1–18) years, and among them, the combined ALS was 3.3 ± 0.5 (3–4) years; bvFTD (25/34) was the most common clinical phenotype and is partially associated with PDB (5/25), followed by PPA (5/34) and FTD-ALS (4/34). Gene detection results: except for 2 patients with compound mutations of C9orf 72, most were missense mutations (19/23) in the coding region of the SQSTM1 gene, and the mutation sites involved all domains of p62, UBA (7/25), TB (6/25), LIR (3/25), SMIR (4/25), PB1 (3/25), and KIR (2/25) (Table 2).
Discussion
In the past, frontotemporal dementia (FTD) and amyotrophic lateral sclerosis (ALS) were thought to be completely different concepts. However, with the rapid development of molecular pathology and neurogenetics, increasing evidence supports that the two diseases are a clinical continuum [4]. Our patients showed a restricted but remarkable deficit in verbal functioning, mild frontal lobe hypometabolism on 18F-fluorodeoxyglucose PET, and a positive electromyography (EMG) appearance on tongue muscle. These findings suggested progressive nonfluent aphasia (PNFA) and progressive bulbar palsy (PBP). Gene sequencing showed that the SQSTM1 variant (c.995 C > G, S332X) was found in the patient. To the best of our knowledge, the variant and clinical phenotype of our patient are reported for the first time, which expands the FTD-ALS gene and clinical phenotype spectrum.
Although the specific pathogenesis is still poorly understood, autophagy, which plays a critical role in the removal pathway of damaged and aggregated proteins and organelles, is implicated as a candidate pathogenic mechanism for neurodegeneration disorders such as FTD and ALS [17]. Mutations affecting the autophagy cargo receptors SQSTM1/p62 were initially identified as a cause of Paget’s disease of bone (PDB) [7]. Recently, mutations have been found in 0.9–3% of cases of FTD and ALS [8, 10, 18, 19]. Due to the low prevalence, previous studies were mostly individual case reports of families and sporadic cases. This paper hopes to increase the number of cases through the review of the previous literature to better summarize its clinical and genetic characteristics. A total of 34 patients with FTD and FTD-ALS caused by mutation in SQSTM1 were retrieved, including our patient. The results showed that only approximately 60% of patients had a family history, which is consistent with previous studies [15]. Although there are family history loss factors caused by some patients dying before the onset of the disease or the disease not being recognized, we suspect that the main reason is that the SQSTM1 gene itself may not be completely penetrant. According to a study of gene penetrance, it was found that microtubule-associated protein tau (MAPT) was almost fully penetrant, and chromosome 9 open reading frame 72 (C9orf 72) and progranulin (GRN) have obvious age-related penetrance [20, 21]. For example, Majounie E et al. showed that C9orf 72 expansions are 50% penetrant by 58 years and usually > 95% penetrant at 80 years [22]. In our study, the average age of onset of 63.5 ± 9.7 years was significantly later than that of the above three genotypes [23, 24], and only 35% of patients under 60 years showed obvious SQSTM1 age-related penetrance. Similar to previous studies [25], we also found that sex may play a role, as the onset age of male cases is later than that of female cases.
Relevant clinical phenotype studies have shown that bvFTD is the most common subtype [26], which is also confirmed by our research. FTD-ALS is a rare clinical phenotype, although it appears in our patients; however, it is far lower than the incidence of the C9orf 72 genotype [24]. In addition, 14% of the patients in our study had PDB. Since the two diseases are rarely screened at the same time in clinical practice, the real data may be underestimated. More interestingly, in most of these patients, PDB was diagnosed earlier than FTD, suggesting that more detailed bone disease screening may be used as a biomarker for early diagnosis of SQSTM1 genotype FTD, although more cases are needed to confirm it.
Due to the irreversibility of FTD and ALS disease itself, survival time has become the focus of attention. Our research shows that the average time of death of patients with the SQSTM1 genotype is 7.2 ± 4.8 years, which is shorter than that of GRN and MAPT [23] but longer than that of the C9orf 72 genotype, which may be related to the fact that C9orf 72 is more prone to the FTD-ALS phenotype [24]. Previous studies have shown that approximately half of patients with FTD-ALS have bulbar onset [27], and they are more likely to lead to fatal malnutrition and lung infections due to dysphagia and dysdipsia.
In recent years, numerous missense and truncating mutations of the SQSTM1 gene have been identified in patients with FTD and ALS [18], and except for a few introns or promoters [10], most mutations occur in the coding region of the gene. Our findings are consistent with those of previous studies. The functional characteristics of the p62 protein are reflected by its domain structure, such as the Phox and Bem1 domain (PB1), ZZ-type zinc finger domain (ZZ), tumor necrosis factor receptor-associated factor 6 binding domain (TB), light chain 3 interaction region (LIR), Keapl interacting region (KIR) and ubiquitin-association domain (UBA) [28]. The UBA domain is responsible for ubiquitin binding [29] and has been considered to be the most common mutation site in patients with PDB [30]. As our study shows, UBA is also the most common mutation domain in patients with FTD and has been identified as a susceptible factor [9]. In addition, we also found that in some patients with mutations in the SOD1 mutant interaction region (SMIR), previous studies have shown that they can combine with the mutant SOD1 gene to participate in the pathogenesis of ALS [31], but its specific mechanism in causing FTD needs further study.
In addition, there was a factor that limited the findings of the present study. It is difficult to prove that the heterozygous variant (c.995C > G, p.S332X) in the SQSTM1 gene is the pathogenic gene of FTD-ALS, due to insufficient genetic samples, lack of whole-exome sequencing and segregation information of family members, as well as a lack of cell experiments to confirm the effects of the S332X variant on the transcriptional activity and protein expression of the SQSTM1 gene.
Conclusion
In summary, we report a case of a patient with PNFA-PBP with SQSTM1 new site nonsense variant. On the one hand, it provides genetic evidence for FTD-ALS as a spectrum of diseases, and on the other hand, it expands the gene spectrum and clinical phenotype in the spectrum. By summing the previous cases, it was found that the FTD of SQSTM1 genotype has obvious age-related penetrance, and the clinical phenotype is mainly bvFTD. Although there are double gene and intron mutations, the main types are still a single gene exon mutation, and the mutation site involves more UBA domains.
References
Hogan DB, Jetté N, Fiest KM, Roberts JI, Pearson D, Smith EE, Roach P, Kirk A, Pringsheim T, Maxwell CJ (2016) The prevalence and incidence of frontotemporal dementia: a systematic review. Can J Neurol Sci 43:S96–S109
Rascovsky K, Hodges JR, Knopman DS et al (2011) Sensitivity of revised diagnostic criteria for the behavioural variant of frontotemporal dementia. Brain 134:2456–2477
Burrell JR, Kiernan MC, Vucic S, Hodges JR (2011) Motor neuron dysfunction in frontotemporal dementia. Brain 134:2582–2594
Devenney E, Vucic S, Hodges JR, Kiernan MC (2015) Motor neuron disease-frontotemporal dementia: a clinical continuum. Expert Rev Neurother 15:509–522
Sieben A, Van Langenhove T, Engelborghs S, Martin J, Boon P, Cras P, De Deyn PP, Santens P, Van Broeckhoven C, Cruts M (2012) The genetics and neuropathology of frontotemporal lobar degeneration. Acta Neuropathol 124:353–372
Rea SL, Walsh J, Layfield R, Ratajczak T, Xu J (2013) New insights into the role of sequestosome 1/p62 mutant proteins in the pathogenesis of paget’s disease of bone. Endocr Rev 34:501–524
Laurin N, Brown JP, Morissette J, Raymond V (2002) Recurrent mutation of the gene encoding sequestosome 1 (SQSTM1/p62) in Paget disease of bone. Am J Hum Genet 70:1582–1588
Le Ber I, Camuzat A, Guerreiro R, Bouya-Ahmed K, Bras J, Nicolas G, Gabelle A, Didic M, De Septenville A, Millecamps S, Lenglet T, Latouche M, Kabashi E, Campion D, Hannequin D, Hardy J, Brice A (2013) SQSTM1 mutations in french patients with frontotemporal dementia or frontotemporal dementia with amyotrophic lateral sclerosis. JAMA Neurol 70:1403–1410
Der Zee JV, Van Langenhove T, Kovacs GG et al (2014) Rare mutations in SQSTM1 modify susceptibility to frontotemporal lobar degeneration. Acta Neuropathol 128:397–410
Rubino E, Rainero I, Chio A, Rogaeva E, Galimberti D, Fenoglio P, Grinberg Y, Isaia G, Calvo A, Gentile S, Bruni AC, St George-Hyslop PH, Scarpini E, Gallone S, Pinessi L (2012) SQSTM1 mutations in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Neurology 79:1556–1562
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, Grody WW, Hegde M, Lyon E, Spector E, Voelkerding K, Rehm HL (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the association for molecular pathology. Genet Med 17:405–424
Sun L, Rong Z, Li W, Zheng H, Xiao S, Li X (2018) Identification of a novel hemizygous SQSTM1 nonsense mutation in atypical behavioral variant frontotemporal dementia. Front Aging Neurosci 10:26–26
Boutoleaubretonniere C, Camuzat A, Ber IL, Bouya-Ahmed K, Guerreiro R, Deruet AL, Evrard C, Bras J, Lamy E, Auffray-Calvier E, Pallardy A, Hardy J, Brice A, Derkinderen P, Vercelletto M (2018) A phenotype of atypical apraxia of speech in a family carrying SQSTM1 mutation. J Alzheimers Dis 43:625–630
Miller L, Rollinson S, Callister JB, Young K, Harris J, Gerhard A, Neary D, Richardson A, Snowden J, Mann DM, Pickering-Brown SM (2015) p62/SQSTM1 analysis in frontotemporal lobar degeneration. Neurobiol Aging 36:1603.e5-1603.e9
Blauwendraat C, Wilke C, Simón-Sánchez J, Jansen IE, Reifschneider A, Capell A, Haass C, Castillo-Lizardo M, Biskup S, Maetzler W, Rizzu P, Heutink P, Synofzik M (2018) The wide genetic landscape of clinical frontotemporal dementia: systematic combined sequencing of 121 consecutive subjects. Genet Med 20:240–249
Almeida MR, Letra L, Pires P, Santos A, Rebelo O, Guerreiro R, van der Zee J, Van Broeckhoven C, Santana I (2016) Characterization of an FTLD-PDB family with the coexistence of SQSTM1 mutation and hexanucleotide (G4C2) repeat expansion in C9orf72 gene. Neurobiol Aging 40:1–1
Sasaki S (2011) Autophagy in spinal cord motor neurons in sporadic amyotrophic lateral sclerosis. J Neuropathol Exp Neurol 70:349–359
Rea SL, Majcher V, Searle MS, Layfield R (2014) SQSTM1 mutations–bridging Paget disease of bone and ALS/FTLD. Exp Cell Res 325:27–37
Fecto F, Yan J, Vemula SP, Liu E, Yang Y, Chen W, Zheng JG, Shi Y, Siddique N, Arrat H, Donkervoort S, Ajroud-Driss S, Sufit RL, Heller SL, Deng HX, Siddique T (2011) SQSTM1 mutations in familial and sporadic amyotrophic lateral sclerosis. Arch Neurol 68:1440–1446
Gass J, Cannon A, Mackenzie IR et al (2006) Mutations in progranulin are a major cause of ubiquitin-positive frontotemporal lobar degeneration. Hum Mol Genet 15:2988–3001
Murphy NA, Arthur KC, Tienari PJ, Houlden H, Chiò A, Traynor BJ (2017) Age-related penetrance of the C9orf72 repeat expansion. Sci Rep 7:2116
Majounie E, Renton AE, Mok K et al (2012) Frequency of the C9orf72 hexanucleotide repeat expansion in patients with amyotrophic lateral sclerosis and frontotemporal dementia: a cross-sectional study. Lancet Neurol 11:323–330
Seelaar H, Kamphorst W, Rosso SM, Azmani A, Masdjedi R, de Koning I, Maat-Kievit JA, Anar B, Kaat LD, Breedveld GJ, Dooijes D, Rozemuller JM, Bronner IF, Rizzu P, van Swieten JC (2008) Distinct genetic forms of frontotemporal dementia. Neurology 71:1220–1226
DeJesus-Hernandez M, Mackenzie IR et al (2011) Expanded GGGGCC hexanucleotide repeat in noncoding region of C9ORF72 causes chromosome 9p-linked FTD and ALS. Neuron 72:245–256
Williams KL, Fifita JA, Vucic S, Durnall JC, Kiernan MC, Blair IP, Nicholson GA (2013) Pathophysiological insights into ALS with C9ORF72 expansions. J Neurol Neurosurg Psychiatry 84:931–935
Wood EM, Falcone D, Suh E, Irwin DJ, Chen-Plotkin AS, Lee EB, Xie SX, Van Deerlin VM, Grossman M (2013) Development andvalidation of pedigree classification criteria for frontotemporallobar degeneration. JAMA Neurol 70:1411–1417
Portet F, Cadilhac C, Touchon J, Camu W (2001) Cognitive impairment in motor neuron disease with bulbar onset. Amyotroph Lateral Scler Other Motor Neuron Disord 2:23–29
Lin X, Li S, Zhao Y, Ma X, Zhang K, He X, Wang Z (2013) Interaction domains of p62: a bridge between p62 and selective autophagy. DNA Cell Biol 32:220–227
Seibenhener ML, Babu JR, Geetha T, Wong HC, Krishna NR, Wooten MW (2004) Sequestosome 1/p62 is a polyubiquitin chain binding protein involved in ubiquitin proteasome degradation. Mol Cell Biol 24:8055–8068
Cavey JR, Ralston SH, Sheppard PW, Ciani B, Gallagher TR, Long JE, Searle MS, Layfield R (2006) Loss of ubiquitin binding is a unifying mechanism by which mutations of SQSTM1 cause Paget’s disease of bone. Calcif Tissue Int 78:271–277
Gal J, Ström AL, Kwinter DM, Kilty R, Zhang J, Shi P, Fu W, Wooten MW, Zhu H (2009) Sequestosome 1/p62 links familial ALS mutant SOD1 to LC3 via an ubiquitin-independent mechanism. J Neurochem 111:1062–1073
Acknowledgements
We thank the subjects and medical staff for their assistance with this study.
Funding
Data collection, analysis, and interpretation of the study were supported by grants from the Natural Science Foundation of Liaoning Province (Grant no. 2018225091).
Author information
Authors and Affiliations
Contributions
Conceptualization: WSL and DMZ; data collection, analysis and investigation: HG and XYD; writing (original draft preparation): WSL and DMZ; writing (review and editing): DMZ. All the authors approved the final version of the manuscript and agreed to be accountable for all the aspects of the work.
Corresponding author
Ethics declarations
Conflicts of interests
The authors declare that they have no competing interests.
Ethics approval
This study was approved by the Ethics Committee of Affiliated Shengjing Hospital of China Medical University. Patients and the patient’s next-of-kin provided written informed consent to participate. In addition, this was also approved by the ethics committee.
Informed consent
A copy of the written consent is available for review by the Editor of this journal.
Consent for publication
Written informed consent was obtained from the patients and the patient’s next-of-kin for publication of this research and any accompanying images.
Rights and permissions
About this article
Cite this article
Li, W., Gao, H., Dong, X. et al. SQSTM1 variant in disorders of the frontotemporal dementia–amyotrophic lateral sclerosis spectrum: identification of a novel heterozygous variant and a review of the literature. J Neurol 268, 1351–1357 (2021). https://doi.org/10.1007/s00415-020-10283-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-10283-x