Abstract
Rationale
Activity levels in patients with pulmonary arterial hypertension (PAH) have correlated with surrogate markers of disease severity. It is not known whether physical activity measures are useful in monitoring patients with PAH.
Objectives
This pilot study aimed to evaluate whether change in physical activity measured by an accelerometer correlates with changes in six-minute walk distance (6MWD), echocardiographic parameters, NT-proBNP, or health-related quality-of-life measures (HRQOL).
Methods
The study design was a prospective, observational study in subjects with prevalent PAH. Subjects wore a wrist-worn accelerometer (Fitbit Charge HR®) between two outpatient visits. Daily step count and activity levels were recorded, and the change over time was correlated with changes in 6MWD, echocardiographic parameters, HRQOL, and NT-proBNP.
Measurements and Main Results
30 subjects were enrolled, of which 20 patients had adequate accelerometer data to be analyzed over the study duration. The mean duration of follow-up was 136.4 ( ± 47.3) days. The change in daily step count correlated with a change in 6MWD (r 0.43, p 0.05). Changes in duration spent in moderately active (r 0.52, p 0.02), lightly active (r 0.48, p 0.05), and sedentary activity levels (r − 0.54, p 0.02) correlated with a change in HRQOL. Changes in activity levels did not correlate with echocardiographic measures or NT-pro BNP.
Conclusions
Changes in daily step count and time spent at fairly active, lightly active, and sedentary activity levels correlate with changes in 6MWD, and HRQOL in subjects with PAH suggesting that accelerometry may be a useful monitoring tool.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The six-minute walk test (6MWT) is a measure of sub-maximal exercise capacity and is an accepted surrogate endpoint in pulmonary arterial hypertension(PAH) as it correlates with survival, functional class, hemodynamics, echocardiographic parameters, biomarkers and health-related quality of life (HRQOL) [1, 2].
Activity monitors, have been used to measure an individual’s activity using step-counts [3, 4]. Accelerometers are a valid, and reliable measure of activity in patients with chronic lung diseases [3, 5, 6]. The validity, reliability, widespread availability, ease of use, high compliance, and economic viability of accelerometers provide us with a unique opportunity to measure activity of PAH patients as they go about their daily lives.
Patients with PAH are less physically active than healthy controls [7,8,9]. Physical activity levels have correlated with markers of severity. Ulrich S et al. measured activity for 2 weeks using an ActiGraph in patients with PAH and chronic thromboembolic pulmonary hypertension (CTEPH) [10]. After a four-year follow-up, patients with > 15 h of activity had a greater transplant-free survival compared to patients with < 15 h per day of activity. Okumus et al. found that steps per day (SPD) in patients with PAH correlated with HRQOL measures, WHO functional class (WHO FC), and six-minute walk distance (6MWD) [4].
The Fitbit Charge HR™ is a commercially available device, which contains a tri-axial accelerometer. It is worn around the wrist and continuously measures activity and heart rate. Activity levels are calculated, using proprietary algorithms, and displayed as steps taken and level of intensity.
While physical activity is known to correlate with 6MWD, it is unknown whether change in physical activity correlates with changes in markers of PAH severity. We studied physical activity changes in individual patients and their correlation with changing disease severity. We hypothesized that a change in physical activity over time, detected by the Fitbit Charge HR®, correlates with a change in 6MWD. This pilot, prospective, observational study was conducted in patients with prevalent WSPH group one PAH being followed at the Cleveland Clinic.
Methods
The study was approved by the IRB at the Cleveland Clinic (IRB number 15–1392).
Subject Selection and Duration
Subjects with hemodynamically confirmed WSPH group one PAH, who could ambulate were enrolled. A convenience sample of 30 subjects was selected since a sample size of 30 would produce an approximate normal sampling distribution for the sample mean [11]. Patients were monitored prospectively between two subsequent clinical visits, which were at least 3 months apart. Society guidelines recommend performing a 6MWT every 3–6 months in stable patients, and change in exercise capacity over this duration has been noted in several clinical trials [12]. We thus anticipated a change in physical activity over a similar duration.
Endpoints
-
Primary endpoint—Correlation of change in SPD with changes in 6MWD between two consecutive outpatient visits.
-
Exploratory endpoints—Correlation of changes in measures of physical activity (SPD, level of activity) with changes in “traditional” PAH parameters (WHO FC, Nt-proBNP, echocardiographic indices, and HRQOL)
Study Visits
Study visits occurred during two routine consecutive outpatient appointments. During both visits, patients received ‘routine care’, which included WHO FC stratification, 6MWT, blood work, and echocardiogram if clinically indicated. Echocardiograms were analyzed following American Society of Echocardiography guidelines [13, 14]. Subjects completed the EuroQol-5D questionnaire and visual analog scale, which is an instrument to measure generic HRQOL. During the first visit, a Fitbit Charge HR™ was set up and given to the patient. A similar protocol was followed during the follow-up visit.
Monitoring Physical Activity
We used the Fitbit Charge HR™ to measure physical activity due to its widespread availably, ease of use, and acceptability with users. An anonymized online profile for each subject was created, and the Fitbit Charge HR™ was set up. They were instructed to wear it on the non-dominant wrist, for ‘as long as possible’, except during exposure to water. Data collected included step count, and time spent in various activity levels. The level of activity was determined by Fitbit® using proprietary algorithms. Compliant days were defined as any day in which the patient had a measured step count. Days without recorded activity were censured from the analysis.
Analysis
We correlated physical activity measured by the accelerometer over the first two weeks, with baseline “traditional” PAH parameters [15]. We analyzed the subgroup of subjects who had data available for > 75% of the study duration with respect to change over time (per protocol analysis). We measured change over time by measuring the slope of graph of activity measures over the duration of the study. This was assessed for correlation with a change in PAH parameters between the two visits.
Statistical Analysis
Clinical parameters were summarized as sample mean with standard deviation or median with interquartile range for continuous variables, as frequency (proportion) for categorical variables. Pearson correlation coefficient was used for measuring the strength and relationship between baseline measures with activity level, and between changes in physical activity and changes in “traditional” PAH parameters. Analysis of Variance (ANOVA) was used for functional class comparison. Scatter plots with fitted line and parameter estimates were generated to show the correlation between the average step count and 6MWD. The level of statistical significance was set at p < 0.05 (two tailed). All analyses were performed using SAS 9.4 for Linux (SAS, Cary, North Carolina).
Results
Patient Characteristics and Follow-Up (Fig. 1)
Thirty subjects were enrolled in the study; two patients withdrew consent after enrollment. All were on medical management, and most were on combination therapy (Table 1). Twenty subjects had available accelerometer data for > 75% of study duration, and five subjects did not have any accelerometer data. The mean duration of follow-up was 136.4 ( ± 46.3) days. There was no difference in baseline characteristics of patients who completed the study and those who did not
.
Baseline Measures and Physical Activity (Table S1, Fig. S1)
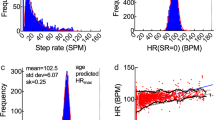
PAH parameters recorded during the screening visit were correlated with physical activity during the first two weeks. A significant correlation between the mean SPD, and 6MWD (r 0.55; p 0.04) was noted. Subjects in WHO FC one and two had a higher mean SPD (6571.1 vs. 4560.5 steps; p 0.007) and 6MWD (453.16 vs 333.52 meters; p 0.0003) compared to subjects who were in WHO FC three and four. No correlation between SPD, and invasive hemodynamic measures, NT-proBNP levels, echocardiographic indices was seen. The 6MWD also did not correlate with invasive hemodynamic parameters, NT-proBNP or echocardiographic indices.
Changes in Physical Activity Clinical Parameters Over Time (Table 2, Fig. S2)
Twenty subjects completed follow-up with accelerometer data available for more than 75% of the study duration. Data from this subgroup of subjects was analyzed (per protocol analysis) We plotted each patient’s physical activity measures, over the follow-up duration, as the representation of change over time. The slope of this plot was correlated with a change in 6MWD between the two visits. A change in SPD correlated with a change in 6MWD (r 0.43; p 0.05).
HRQOL (Table 3)
Changes in daily time spent in “moderate” and “light” activities correlated with changes in the EurQol-5D index and EuroQol VAS. A change in time spent in “sedentary activity” had an inverse correlation with changes in the EuroQol-5D index and EuroQol VAS. However, SPD, and 6MWD did not have a statistically significant correlation with EuroQol index or EuroQol VAS score.
Echocardiographic Indices and Serum Biomarkers
85% (17/20) of patients had baseline and follow-up echocardiography done, and 50% (10/20) patients had baseline and follow-up NT-proBNP levels measured. Changes in physical activity measures did not correlate with changes in echocardiographic parameters or NT-proBNP levels.
Hospital Admissions (Fig. 2)
Two subjects required hospital admission for worsening PAH. Subject one had a decline in weekly mean SPD from a peak of 13,000 SPD to 2000 SPD in the week preceding her hospital admission (84.6% drop). The mean SPD for subject twenty decreased from 3000 to 1500 SPD in the week preceding his hospital admission (50% drop). The decline in both cases was gradual over a period of four weeks preceding the hospital admission.
Daily step count in two patients admitted to the hospital for worsening pulmonary hypertension. Number of weeks from study enrollment plotted in X axis, mean daily step count (a), mean light activity duration (b), sedentary activity duration (c) plotted on y axis. Blue line—patient 1, red line—patient 20. Arrow marks the week of hospitalization on X axis
Compliance (Fig. S3)
Compliant days were defined as any day with a recorded step count. Sixty-eight percent of the subjects were compliant for > 75% of the duration of the study, while twenty one percent were compliant for < 25% of the study duration. In the subgroup of subjects who wore and synced the accelerometer for at least one day, the mean compliance was 87%, with 83% being compliant for > 75% of the study duration.
Ease of Use (Table S2)
Most subjects in the study found the wrist-worn accelerometer to be an acceptable measure of activity, technically easy to use and charge, and would be willing to use it outside of a research study.
Discussion
Physical activity is any activity produced by skeletal muscles that produce movement, and exercise capacity is defined as the maximum amount of physical exertion a person can sustain [16]. Measurement of submaximal exercise capacity with a 6MWT has been an important surrogate for outcomes in PAH, but has several limitations including cost, resource intensiveness, and a ceiling effect in patients with mild impairment [17, 18]. Although physical activity can be affected by cardiopulmonary status, muscular strength, and motivation, the ability to measure longitudinal physical activity adds another weapon in our arsenal to monitor patients objectively over time. In this pilot study, we looked at the accelerometer measured physical activity as a surrogate tool for monitoring subjects with PAH.
We found a significant correlation between SPD measured during the first two weeks of the study with baseline 6MWD. Not surprisingly, subjects with a higher WHO FC were significantly less active than subjects with a lower WHO FC. These findings conform to prior studies, which demonstrated that physical activity correlates with submaximal exercise capacity and WHO FC. Mainguy et al. found a strong correlation between 6MWD and SPD in patients with idiopathic and scleroderma associated PAH [19].
We found an inverse correlation between subject’s body mass index and physical activity levels as well as 6MWD. This is similar to findings from the REVEAL registry in which obesity was associated with lower 6MWD [20]. In our subjects, both the 6MWD and physical activity measures did not correlate with invasive hemodynamic measurements, echocardiographic measures of RV function, and NTproBNP levels. These findings should be interpreted with caution. The hemodynamic measurements in our patients were not contemporaneous with time of enrollment in the study, and echocardiography was performed only if clinically indicated. All these factors, together with our small sample size, may explain this finding. In contrast to our findings, Ulrich et al. reported that subjects in the group with the lowest PA pressures had increased activity duration [10].
A change in SPD correlated with a change in 6MWD over the duration of this study. This finding is significant since it provides a method to continuously monitor patients for clinical change over a prolonged duration of time, potentially via telemedicine. Given the high degree of uncertainty surrounding the utility of patient-generated health data and its use, this study highlights a potential, clinically relevant use [21].
HRQOL is often considered the most meaningful disease measure from a patient perspective and in patients with PAH, improvement in HRQOL with treatment have been observed [22]. Studies have demonstrated that an improvement in 6MWD of 31–33 m has shown clinically meaningful improvement in HRQOL [23]. In our patients, a change in 6MWD did not correlate with a change in HRQOL measures; rather changes in physical activity levels over time correlated with change in HRQOL. SPD and activity levels measure two different aspects of physical activity in an individual. SPD is a measure of the sum of all physical activity; activity levels define the intensity of activity that was involved [24]. The reason for the discrepancy between SPD and activity levels and correlation with outcomes is unclear. We speculate that the ability to spend time in higher intensity activities may have a greater impact on quality of life than the total daily activity or submaximal exercise capacity, thus being a more sensitive marker of change. Our patients spent minimal time being “very active”, thus no significant change or correlation with severity was seen. The 6MWD has the limitation of a “ceiling effect” in detecting change in patients with mild/moderate disease [18, 18]. Our patients had well-preserved 6MWD and were mostly clinically stable during the duration of the study thus limiting the utility of 6MWD in our study population. Physical activity measures do not seem to have this limitation, which may be of interest when monitoring patients with early or mild disease. These findings will need to be confirmed in larger trials to further characterize this relationship and identify a clinically meaningful change in activity levels.
Zijlstra et al., measured activity in children with PAH over one week, and found it to be a good predictor of outcomes such as PAH-related hospitalizations [8]. The decrease in physical activity levels in the two hospitalized patients prior to admission give us a unique insight into physical activity decline weeks prior to clinical worsening. Both patients had a gradual and significant decline weeks before presenting to the hospital. Thus, a drop in physical activity may be a potential biomarker for clinical worsening in between clinic visits, allowing for early intervention. However, due to our small sample size, we were not able to identify factors that predict a decline in walk distance or hospital admissions.
Patient compliance and acceptance to using a wrist worn accelerometer was better than previously described for other home monitoring devices such as peak flow measurement [25, 26]. Fourteen percent of our patients never used the accelerometer at all, which is similar to studies in patients with other pulmonary conditions [3]. In patients who used the device for at least one day, the compliance was excellent at 87%. This study was conducted in the “real-world” scenario, with no additional support by the study team. When considering long-term monitoring, these would be important characteristics favoring the use of a wrist-worn accelerometer.
There are several limitations to our study. Our cohort included patients with prevalent, stable PAH, who in most cases remained clinically stable during the study duration. Several of our patients had comorbidities that could have impacted physical activity. However, since such comorbidities in PAH are common, this seems to be representative of the larger population living with PAH [20]. A short follow-up duration and the lack of significant change during the follow-up period may have limited the ability to detect correlation with change. A small sample size of 30 patients, of which only two-thirds completed the study is certainly a limitation to the widespread applicability of the results. However, the results of this pilot study provide important data for future study design using physical activity as a longitudinal monitoring tool. The use of an accelerometer may have impacted the daily physical activity of patients, especially in the first few weeks of use, although the effect lasting over the entire study duration is unlikely. The exploratory outcome measures of echocardiographic indices and serum biomarkers were only obtained based on clinical need as deemed by the treating physician, thus limiting the statistical power to detect changes. We used a commercially available accelerometer due to its widespread availability and acceptability among patients, while acknowledging the disadvantages of proprietary algorithms which are unavailable for scrutiny and have not been clinically validated. To use physical activity monitoring in clinical practice, several issues will need to be considered: utility in patients with very limited activity, device selection, interoperability with electronic health records, and optimal measure of activity.
Studies to date have measured physical activity over a short duration of time in PAH patients, showing significant correlation with severity of disease. To our knowledge, this is the first study exploring the role of monitoring physical activity over a long duration and demonstrating that changing physical activity correlates with the changes in markers of PAH severity and HRQOL in individual patients.
SPD and time spent at various activity levels are the best measures of physical activity, and a combination of these two measures provide the best overall picture of activity and change in PAH severity over time. Larger, multicenter studies are needed to further explore accelerometry use as a monitoring tool, perhaps as an exploratory endpoint in future clinical trials. Despite several limitations and unknowns, activity measurement has great potential for longitudinal monitoring in PAH.
Abbreviations
- 6MWD:
-
Six-minute walk distance
- 6MWT:
-
Six-minute walk test
- BMI:
-
Body mass index
- CTEPH:
-
Chronic thromboembolic disease
- ERA:
-
Endothelin receptor antagonist
- HRQOL:
-
Health-related quality of life
- PA:
-
Pulmonary artery
- PAH:
-
Pulmonary arterial hypertension
- PCWP:
-
Pulmonary capillary wedge pressure
- PDE-5:
-
Phosphodiesterase type 5
- PVR:
-
Pulmonary vascular resistance
- RA:
-
Right atrium
- RHC:
-
Right heart catheterization
- RV:
-
Right ventricle
- SPD:
-
Steps per day
- TAPSE:
-
Tricuspid annular plane systolic excursion
- VAS:
-
Visual analog scale
- WHO FC:
-
World health organization functional class
- WSPH:
-
World Symposium on pulmonary hypertension
References
Miyamoto S, Nagaya N, Satoh T, Kyotani S, Sakamaki F, Fujita M, Nakanishi N, Miyatake K (2012) Clinical correlates and prognostic significance of six-minute walk test in patients with primary pulmonary hypertension. Am J Respir Crit Care Med. https://doi.org/10.1164/ajrccm.161.2.9906015#.V03ik_nhDIU
Taichman DB, Shin J, Hud L, Archer-Chicko C, Kaplan S, Sager JS, Gallop R, Christie J, Hansen-Flaschen J, Palevsky H (2005) Health-related quality of life in patients with pulmonary arterial hypertension. Respir. Res. 6:92. https://doi.org/10.1186/1465-9921-6-92
F. Pitta, T. Troosters, V.S. Probst, M. a Spruit, M. Decramer, R. Gosselink, Quantifying physical activity in daily life with questionnaires and motion sensors in COPD. Eur Respir J Off J Eur Soc Clin Respir Physiol 27:1040–1055. https://doi.org/10.1183/09031936.06.00064105
Okumus G, Aslan GK, Arseven O, Ongen G, Issever H, Kıyan E, Mauritz G-J, Rizopoulos D, Groepenhoff H, Tiede H, Felix J, Eilers P, Bosboom J, Postmus PE, Westerhof N, Vonk-Noordegraaf A, Pugh ME, Buchowski MS, Robbins IM, Newman JH, Hemnes AR (2012) Physical activity limitation as measured by accelerometry in pulmonary arterial hypertension. Am. J. Cardiol. 142:1391–1398. https://doi.org/10.1378/chest.12-0150
Dhillon SS, Sima CA, Kirkham AR, Syed N, Camp PG (2015) Physical Activity Measurement Accuracy in Individuals With Chronic Lung Disease: A Systematic Review With Meta-Analysis of Method Comparison Studies. Arch. Phys. Med. Rehabil. 96:2079–2088. https://doi.org/10.1016/j.apmr.2015.05.015
Chen M-D, Kuo C-C, Pellegrini CA, Hsu M-J (2016) Accuracy of wristband activity monitors during ambulation and activities. Med Sci Sports Exerc. https://doi.org/10.1249/MSS.0000000000000984
Pugh ME, Buchowski MS, Robbins IM, Newman JH, Hemnes AR (2012) Physical activity limitation as measured by accelerometry in pulmonary arterial hypertension. Chest 142:1391–1398. https://doi.org/10.1378/chest.12-0150
Zijlstra WMH, Ploegstra M-J, Vissia-Kazemier T, Roofthooft MTR, du Sarvaas GM, Bartelds B, Rackowitz A, van den Heuvel F, Hillege HL, Plasqui G, Berger RMF (2017) Physical activity in pediatric pulmonary arterial hypertension measured by accelerometry. A candidate clinical endpoint. Am J Respir Crit Care Med 196:220–227. https://doi.org/10.1164/rccm.201608-1576OC.
González-Saiz L, Santos-Lozano A, Fiuza-Luces C, Sanz-Ayán P, Quezada-Loaiza CA, Ruiz-Casado A, Alejo LB, Flox-Camacho A, Morán M, Lucia A, Escribano-Subías P (2018) Physical activity levels are low in patients with pulmonary hypertension. Ann. Transl. Med. 6:205–205. https://doi.org/10.21037/atm.2018.05.37
Ulrich S, Fischler M, Speich R, Bloch KE (2013) Wrist actigraphy predicts outcome in patients with pulmonary hypertension. Respiration. 86:45–51. https://doi.org/10.1159/000342351
Hogg RV, Tanis EA, Zimmerman DL (2014) Probability and statistical inference, 9th edn. Pearson
Galie N, Hoeper MM, Humbert M, Torbicki A, Vachiery J-L, Barbera JA, Beghetti M, Corris P, Gaine S, Gibbs JS, Gomez-Sanchez MA, Jondeau G, Klepetko W, Opitz C, Peacock A, Rubin L, Zellweger M, Simonneau G, Rubin L, Zellweger M, Simonneau G (2009) Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur. Respir. J. 34:1219–1263. https://doi.org/10.1183/09031936.00139009
Rudski LG, Lai WW, Afilalo J, Hua L, Handschumacher MD, Chandrasekaran K, Solomon SD, Louie EK, Schiller NB (2010) Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. J Am Soc Echocardiogr 23(2010):685–713; quiz 786–8. https://doi.org/10.1016/j.echo.2010.05.010
R.M. Lang, L.P. Badano, V. Mor-Avi, J. Afilalo, A. Armstrong, L. Ernande, F.A. Flachskampf, E. Foster, S.A. Goldstein, T. Kuznetsova, P. Lancellotti, D. Muraru, M.H. Picard, E.R. Rietzschel, L. Rudski, K.T. Spencer, W. Tsang, J.-U. Voigt, Recommendations for Cardiac Chamber Quantification by Echocardiography in Adults: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging, Eur. Hear. J. – Cardiovasc. Imaging. 16 (2015) 233–271. https://doi.org/10.1093/ehjci/jev014
Van Hout B, Janssen MF, Feng YS, Kohlmann T, Busschbach J, Golicki D, Lloyd A, Scalone L, Kind P, Pickard AS (2012) Interim scoring for the EQ-5D-5L: Mapping the EQ-5D-5L to EQ-5D-3L value sets. Value Heal. 15:708–715. https://doi.org/10.1016/j.jval.2012.02.008
Physical Activity and Your Heart | National Heart, Lung, and Blood Institute (NHLBI) (n.d.). https://www.nhlbi.nih.gov/health-topics/physical-activity-and-your-heart. Accessed July 4, 2018.
Frost AE, Langleben D, Oudiz R, Hill N, Horn E, McLaughlin V, Robbins IM, Shapiro S, Tapson VF, Zwicke D, DeMarco T, Schilz R, Rubenfire M, Barst RJ (2005) The 6-min walk test (6MW) as an efficacy endpoint in pulmonary arterial hypertension clinical trials: Demonstration of a ceiling effect. Vascul. Pharmacol. 43:36–39. https://doi.org/10.1016/j.vph.2005.03.003
Gaine S, Simonneau G (2013) The need to move from 6-minute walk distance to outcome trials in pulmonary arterial hypertension. Eur. Respir. Rev. 22:487–494. https://doi.org/10.1183/09059180.00006213
V. Mainguy, S. Provencher, F. Maltais, S. Malenfant, D. Saey (2011) Assessment of daily life physical activities in pulmonary arterial hypertension, PLoS ONE. https://doi.org/10.1371/journal.pone.0027993
Poms AD, Turner M, Farber HW, Meltzer LA, McGoon MD (2013) Comorbid conditions and outcomes in patients with pulmonary arterial hypertension: A reveal registry analysis. Chest 144:169–176. https://doi.org/10.1378/chest.11-3241
Chung AE, Basch EM (2015) Potential and challenges of patient-generated health data for high-quality cancer care. J. Oncol. Pract. 11:195–197. https://doi.org/10.1200/JOP.2015.003715
Rival G, Lacasse Y, Martin S, Bonnet S, Provencher S (2014) Effect of pulmonary arterial hypertension-specific therapies on health-related quality of life: a systematic review. Chest 146:686–708. https://doi.org/10.1378/chest.13-2634
Mathai SC, Puhan MA, Lam D, Wise RA (2012) The minimal important difference in the 6-minute walk test for patients with pulmonary arterial hypertension. Am. J. Respir. Crit. Care Med. 186:428–433. https://doi.org/10.1164/rccm.201203-0480OC
Sehgal S, Small B, Highland KB (2019) Activity monitors in pulmonary disease. Respir Med. https://doi.org/10.1016/j.rmed.2019.03.019.
Côté J, Cartier A, Malo JL, Rouleau M, Boulet LP (1998) Compliance with peak expiratory flow monitoring in home management of asthma. Chest 113(1998):968–972. https://www.ncbi.nlm.nih.gov/pubmed/9554633. Accessed April 12, 2018.
Verschelden P, Cartier A, L’Archevêque J, Trudeau C, Malo JL (2018) Compliance with and accuracy of daily self-assessment of peak expiratory flows (PEF) in asthmatic subjects over a three month period., Eur. Respir. J. 9 (1996) 880–5. https://www.ncbi.nlm.nih.gov/pubmed/8793446. Accessed April 12, 2018.
Funding
This study was funded by United Therapeutics.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest:
Sameep Sehgal—United Therapeutics: Research Funding. Kristin B Highland—Actelion Pharmaceuticals: research funding, speaker's bureau; Bayer Healthcare: Research funding, Speaker's bureau; Boehringer Ingelheim: Consulting, Steering Committee, Research Funding, Speaker's Bureau; Eiger Pharmaceuticals: Research funding; Genetech: Research funding; Gilead Sciences: Speaker's Bureau; Reata Pharmaceuticals: Research funding; United Therapeutics: Research Funding.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Sehgal, S., Chowdhury, A., Rabih, F. et al. Counting Steps: A New Way to Monitor Patients with Pulmonary Arterial Hypertension. Lung 197, 501–508 (2019). https://doi.org/10.1007/s00408-019-00239-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-019-00239-y