Abstract
Purpose
We studied the diagnostic value of cytokines, including vascular endothelial growth factor (VEGF), transforming growth factor-β (TGF-β), and interleukin-8 (IL-8), and the ratio of lactate dehydrogenase (LDH) to adenosine deaminase (ADA) in pleural fluid.
Methods
Prospective analysis of 44 inpatients or outpatients with pleural fluid, from December 2016 to March 2017 was conducted.
Results
We enrolled patients with malignant pleural effusion (MPE, N = 15), empyema (N = 11), parapneumonic effusion (PPE, N = 7), chronic renal failure (CRF)/chronic heart failure (CHF) (N = 7), and tuberculous pleural effusion (TBPE, N = 4). The pleural fluid values of IL-8 and VEGF were significantly higher in empyema patients than in CRF/CHF or PPE patients. In all patients, the pleural fluid VEGF and IL-8 values were significantly positively correlated (r = 0.405, p = 0.006; r = 0.474, p = 0.047, respectively). TGF-β was elevated in patients with empyema, PPE, TBPE, and MPE. The pleural LDH-to-ADA ratio in patients with MPE or empyema/PPE was significantly higher than in patients with CRF/CHF or TBPE. LDH and ADA levels correlated significantly only in patients with MPE (r = 0.648, p = 0.009) and empyema/PPE (r = 0.978, p < 0.001).
Conclusions
VEGF and IL-8 production in the pleural cavity appear to accelerate the progression of PPE to empyema, by enhancing vascular permeability associated with inflammation. Sequential sampling would be needed to confirm this. The pleural LDH/ADA ratio may be a useful diagnostic tool for discriminating between various pleural effusion etiologies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The most common etiologies for unilateral pleural effusion are parapneumonic effusion (PPE) or empyema, tuberculous pleural effusion (TBPE), and malignant pleural effusion (MPE). We previously reported a simple method for discriminating empyema from parapneumonic effusion, based on distinguishing between split and hemi-split signs, and calculating the total amount of pleural fluid using thoracic computed tomography (CT) [1]. In general practice, however, physicians cannot always use thoracic CT for the evaluation of pleural effusion. Furthermore, although several mechanisms underlying the accumulation of pleural effusion have been proposed, including the formation of endothelial fenestrations, loss of junctional integrity, and formation of transcellular gaps [2]; the precise mechanism has not yet been fully determined.
We hypothesized that vascular permeability mediated by cytokines in the pleural fluid, such as vascular endothelial growth factor (VEGF), transforming growth factor-β (TGF-β), and interleukin-8, can affect the total amount of pleural effusion. In this study, we prospectively examined the correlation between the total amount of pleural fluid (semi-quantitatively assessed from chest X-rays), and the levels of the aforementioned cytokines, in various diseases. We also developed a novel method for analyzing pleural fluid, based on measuring the ratio of pleural lactate dehydrogenase (LDH) to adenosine deaminase (ADA).
Materials and Methods
After obtaining informed consent, we prospectively enrolled adult patients, in outpatient or inpatient settings, who showed pleural effusion during the period from December 2016 to March 2017. All patients were enrolled either at the time of their first visit to the Kyorin University Hospital (a 1100-bed tertiary care center in Tokyo), with pleural fluid already evident, or after developing pleural effusion during hospitalization. This study was approved by the ethics committee of Kyorin University on December 1, 2016 (approval number H28-061).
Definition of the Diseases of the Enrolled Patients
The definition of empyema was based on Light’s criteria (including only classes 6 and 7) [3] and category 3 or 4 of the American College of Chest Physicians consensus (ACCP) [4]. Patients in classes 1–5 according to Light’s criteria, or category 1 or 2 according to ACCP criteria, were diagnosed with parapneumonic effusion. Tuberculous pleural effusion was defined when the ADA level was higher than 40 U/L, together with regression or resolution of the pleural effusion after initiation of antituberculosis therapy, or microbiological confirmation, including polymerase chain reaction confirmation, of Mycobacterium tuberculosis in the fluid. Malignant pleural effusion was defined when the fluid was cytologically positive for malignant cells. Congestive heart failure and/or chronic renal failure were based on a clinical diagnosis.
To evaluate the total amount of pleural effusion semi-quantitatively, a chest X-ray was divided at three levels: (1) bronchial bifurcation, (2) upper level of the diaphragm, and (3) midway between those levels (Fig. 1). The degree of fluid accumulation was defined as mild, moderate, or severe, according to whether the fluid observed in the chest X-ray rose higher than level 1, 2, or 3, respectively (Fig. 1). Patients who showed vertically oriented pleural effusion with pleural adhesion were excluded, because of difficulty in measuring the amount of fluid in such cases. Interobserver correlation scores among the three reviewers were as follows: T.S and T. W, κ = 0.813; M.T and T.W, κ = 0.772; and T.S and M.T, κ = 0.888, suggesting good to excellent reproducibility.
Definition of the degree of pleural fluid accumulation on chest X-ray. Each chest X-ray was divided at three levels: (1) the bronchial bifurcation, (2) the upper level of the diaphragm, and (3) midway between 1) and 2). The degree of fluid accumulation was defined as mild, moderate, and severe depending on whether the chest X-ray showed fluid rising above the respective levels
Statistical Analysis
Numerical data were evaluated for normal distribution and equal variance using the Kolmogorov–Smirnov test and Levene’s median test, respectively. Categorical data are presented as percentages of the total or as whole numbers, as appropriate. Statistical comparisons of non-parametric data were performed using the Mann–Whitney test. Comparisons of categorical data were made using Pearson’s Chi-square test. All tests were two-sided. Values of p < 0.05 were considered statistically significant. The data were analyzed using SPSS version 19.0 for Windows.
Results
Clinical Characteristics of Patients with Pleural Effusion
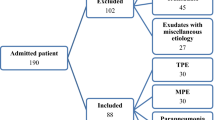
During the study period, we enrolled 44 patients with pleural effusion, comprising, in order of frequency malignant pleural effusion (MPE) (N = 15), empyema (N = 11), parapneumonic effusion (PPE) (N = 7), chronic renal failure (CRF)/chronic heart failure (CHF) (N = 7), and tuberculous pleural effusion (TBPE) (N = 4) (Table 1). The mean age of subjects in the CRF/CHF group (median: 85 years, range 80–90 years) was significantly higher than the ages of the MPE (median: 72 years, range 65–79 years, p = 0.002), PPE (median: 68 years, range 60–83 years, p = 0.026), and TBPE (median: 61 years, range 45–83, p = 0.003) groups; however, the male-to-female ratio and the frequency of underlying disease were comparable in each group, with the exception of lung cancer, for which every subject showed MPE.
Semi-quantitative Analysis of Total Amount of Pleural Fluid
Total Amount of Pleural Effusion on Chest X-ray
The total amount of pleural effusion was evaluated for each patient based on the chest X-ray classification defined in the Methods section (Fig. 1; Table 2). The proportion of patients with mild effusion was significantly higher in the CRF/CHF group (n = 6, 85.7%) than in the empyema (n = 2, 18.2%, p = 0.02) or MPE (n = 4, 26.7%, p = 0.02) groups. The PPE group (n = 5, 71.4%) also contained a higher frequency of patients with mild effusion than did the empyema group (n = 2, 18.2%, p = 0.049). Conversely, the proportion of patients with moderate effusion was significantly lower in the CRF/CHF group (n = 0, 0%) than in the MPE (n = 8, 53.5%, p = 0.002), TBPE (n = 3, 75%, p = 0.024), and empyema (n = 6, 54.5%, p = 0.038) groups. The proportion of subjects with severe effusion was comparable in all groups.
Proportion of Patients with Moderate and/or Severe Pleural Effusion on Chest X-ray
The proportion of patients with moderate or severe pleural effusion on chest X-ray was significantly higher in both the MPE (n = 11, 73.3%) and empyema (n = 9, 81.8%) groups than in the CRF/CHF group (n = 1, 14.3%) (Fig. 2). However, the proportion of moderate or severe pleural effusion was comparable in the MPE, TBPE, and empyema groups.
Proportion of patients with moderate to severe pleural effusion on the chest X-ray due to various diseases. CHF/CRF chronic heart failure/chronic renal failure, MPE malignant pleural effusion, TBPE tuberculous pleural effusion, PPE parapneumonic effusion. Black color means the patients with moderate or severe pleural effusion
Comparison of the Pleural LDH-to-ADA Ratio in Various Diseases
Pleural fluid analysis showed that the levels of LDH and ADA were significantly positively correlated only in the MPE (r = 0.648, p = 0.009) and empyema/PPE (r = 0.978, p < 0.001) groups, but not in the CRF/CHF (r = 0.332, p = 0.467) and TBPE (r = − 0.892, p = 0.108) groups (Table 3). Interestingly, the empyema/PPE group showed a higher coefficient of correlation than any other group. Furthermore, the pleural LDH-to-ADA ratio was significantly higher in the empyema/PPE group (median: 35.4, range 14.7–152) than in any other group, followed in order by the MPE (median: 28.8, range 8.7–144.8), CRF/CHF (median: 13.1, range 14.1–24.3), and TBPE (median: 6.4, range 4.6–41.0) groups (Table 3).
Detection of IL-8, VEGF, and TGF-β in Pleural Fluid
The level of interleukin-8 in the pleural fluid of the empyema group (median: 5940 pg/mL, range 263–135,000 pg/mL) was significantly higher than that in the CRF/CHF (median: 43.3 pg/mL, range 34.7–6060 pg/mL, p = 0.002) or PPE (median: 184 pg/mL, range 4.3–16,300 pg/mL, p = 0.008) (Fig. 3a) groups. For vascular endothelial growth factor (VEGF), the level was significantly higher in the empyema group (median: 5180 pg/mL, range 338–17,300 pg/mL) than in the CRF/CHF (median: 155 pg/mL, range 68–2660 pg/mL, p = 0.014) or PPE (median: 1450, range 171–4530 pg/mL, p = 0.044) groups, but was comparable to that of the MPE group (median: 1550 pg/mL, range 69–21,500 pg/mL). Similarly, the MPE group had a significantly higher level of VEGF than the CRF/CHF group (p = 0.001) (Fig. 3b). For transforming growth factor-β (TGF-β), the TBPE and empyema groups both had significantly higher levels (TBPE, median: 10.2 ng/mL, range 9.0–11.7, p = 0.027; empyema, median: 54.6 ng/mL, range 0.72–28.3 ng/mL, p = 0.032) than the MPE group (median: 3.8 ng/mL, range 1.8–17.6 ng/mL).
Interestingly, pleural IL-8 and VEGF both in all enrolled patients and in patients with empyema/PPE only were moderately but significantly correlated (Fig. 4a, r = 0.405, p = 0.006; Fig. 4b, r = 0.474, p = 0.047, respectively), but the correlations in all enrolled patients were not significant for pleural IL-8/TGF-β (r = 0.17, p = 0.27) or VEGF/TGF-β (r = 0.277, p = 0.068). The IL-8 levels and neutrophil level (%) in the pleural fluid also demonstrated a moderately positive correlation (r = 0.406, p = 0.009, data not shown).
Discussion
Abundant cytokines in pleural fluid have been considered to be associated with infectious disease or malignant disease [5, 6]. Among them, VEGF and TGF-β levels were thought to be correlated with vascular permeability. In particular, VEGF is a potent mediator of endothelial permeability and is regulated by TGF-β [5, 7].
First, the present study showed that both TGF-β and VEGF levels can be elevated in empyema, PPE, and MPE, and revealed a positive correlation between pleural VEGF and IL-8 levels in both all the enrolled patients and in only those with empyema/PPE (Fig. 4). Furthermore, it has not been described previously that the differences between empyema and PPE are related to significant elevation of both IL-8 and VEGF in the pleural effusion; this accelerates inflammatory processes and increases vascular permeability, resulting in greater fluid accumulation in the pleural cavity. Cheng et al. reported high levels of TGF-β in malignant mesothelioma, TBPE, and sepsis [8], but previous studies have not shown the differences between empyema and PPE in terms of cytokine levels in the pleural effusion. Our observations suggest that VEGF/IL-8 elevation, along with an increase in TGF-β, could play a part in the progression of PPE to empyema.
Second, we were able to use chest X-rays to evaluate differences in the total amount of pleural effusion semi-quantitatively, yielding results that are compatible with general expectations (Fig. 2).
Third, we demonstrated the clinical value of the pleural LDH/ADA ratio in the differential diagnosis of pleural effusion, which has not been described previously. Among the four clinical entities examined, only the MPE and empyema/PPE conditions produced significant positive correlations between pleural LDH and ADA levels (Table 3); these correlations were not seen in patients with CRF/CHF and TBPE. The former two entities showed comparable values of the pleural LDH/ADA ratio, but it is possible that differences could emerge if a larger number of cases were analyzed, especially if this analysis could be combined with the use of carcinoembryonic antigen levels in the pleural fluid, as previous reported [9].
This study has limitations, in that the total number of patients enrolled in each group was relatively small, particularly in the case of TBPE, and only three types of cytokines were examined, which is not enough to capture the whole picture of pathogenesis relating to vascular permeability.
It is, however, noteworthy that VEGF and IL-8 levels in the pleural fluid were positively correlated, which would accelerate the progression of PPE to empyema, and that the pleural LDH/ADA ratio proved to be moderately or strongly correlated only in patients with MPE or empyema/PPE. Accumulation of more cases might lead to the simple differential diagnosis for pleural effusion.
Conclusions
VEGF and IL-8 production in the pleural cavity appear to accelerate the progression of PPE to empyema, and the pleural LDH/ADA ratio may be a valuable diagnostic tool for discriminating the possible etiologies of pleural effusion.
References
Tsujimoto N, Saraya T, Light RW, Tsukahara Y, Koide T, Kurai D, Ishii H, Kimura H, Goto H, Takizawa H (2015) A simple method for differentiating complicated parapneumonic effusion/empyema from parapneumonic effusion using the split pleura sign and the amount of pleural effusion on thoracic CT. PLoS ONE 10:e0130141
Bradshaw M, Mansfield A, Peikert T (2013) The role of vascular endothelial growth factor in the pathogenesis, diagnosis and treatment of malignant pleural effusion. Curr Oncol Rep 15:207–216
Light RW (2002) Clinical practice. Pleural effusion. N Engl J Med 346:1971–1977
Colice GL, Curtis A, Deslauriers J, Heffner J, Light R, Littenberg B, Sahn S, Weinstein RA, Yusen RD (2000) Medical and surgical treatment of parapneumonic effusions: an evidence-based guideline. Chest 118:1158–1171
Antony VB (2003) Immunological mechanisms in pleural disease. Eur Respir J 21:539–544
Hassan T, Al-Alawi M, Chotirmall SH, McElvaney NG (2012) Pleural fluid analysis: standstill or a work in progress?. Pulm Med 2012:716235
Fiorelli A, Vicidomini G, Di Domenico M, Napolitano F, Messina G, Morgillo F, Ciardiello F, Santini M (2011) Vascular endothelial growth factor in pleural fluid for differential diagnosis of benign and malignant origin and its clinical applications. Interact Cardiovasc Thorac Surg 12:420–424
Cheng D, Lee YC, Rogers JT, Perkett EA, Moyers JP, Rodriguez RM, Light RW (2000) Vascular endothelial growth factor level correlates with transforming growth factor-beta isoform levels in pleural effusions. Chest 118:1747–1753
Koide T, Saraya T, Yokoyama T, Kurai D, Ishii H, Takizawa H (2015) Prognostic value of carcinoembryonic antigen in pleural effusion in patients with primary lung adenocarcinoma. Am J Respir Crit Care Med 191:A5102
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Saraya, T., Ohkuma, K., Watanabe, T. et al. Diagnostic Value of Vascular Endothelial Growth Factor, Transforming Growth Factor-β, Interleukin-8, and the Ratio of Lactate Dehydrogenase to Adenosine Deaminase in Pleural Effusion. Lung 196, 249–254 (2018). https://doi.org/10.1007/s00408-018-0090-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-018-0090-1