Abstract
Purpose
To investigate the subjective effect of office-based blue laser therapy for inferior turbinate hypertrophy in patients with nasal obstruction.
Methods
Patients with nasal obstruction who underwent office-based blue laser for the inferior turbinate hypertrophy between October 2022 and December 2023 were included in the study. The two outcome measures used to gauge the improvement in nasal obstruction and success of surgery were the Nasal Obstruction Symptom Evaluation (NOSE) scale and the Visual Analogue Scale (VAS). Patient’s level of comfort during the procedure was also rated using a 10-point VAS scale.
Results
A total of 14 patients were included in this study. The mean age of the study group was 41.47 ± 18.52 and the F/M ratio was 4.67. All patients reported significant improvement in nasal breathing. The mean NOSE score decreased significantly from 13.07 ± 3.89 pre-operatively to 2.64 ± 2.43 post-operatively (p = 0.002). Similarly, the mean VAS score decreased from 7.43 ± 0.85 to 2.0 ± 1.57 (p = 0.002) following surgery. The procedure was well-tolerated by all participants and the mean total score ranged from 6 to 9 with an average of 7.59 ± 1.34.
Conclusion
Office-based blue laser therapy for inferior turbinate hypertrophy may be an effective treatment modality for nasal obstruction from the patient’s perspective. Although the procedures were tolerated well with no complications noted, these results should be cautiously interpreted until studies using objective measures are conducted.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Nasal obstruction is a common symptom affecting one third of the population [1]. It has a negative impact on quality of life, particularly in the presence of other symptoms such as nasal discharge and post-nasal drip. The most common cause of nasal obstruction is nasal septal deviation, followed by inferior turbinate hypertrophy [1, 2]. Other causes include anatomic variations of the nose and paranasal sinuses such as a septal spur and a large conchae bullosa, and/or infectious diseases such as sinusitis with or without polyposis.
Inferior turbinate hypertrophy (ITH) is a frequently identified cause of nasal obstruction on nasal endoscopy [2]. The most common etiology is allergic rhinitis, an IgE-mediated chronic inflammation of the epithelial lining of the nasal cavity that leads to mucosal hypertrophy [3]. Other causes of inflammation include non-allergic etiologies such as vasomotor rhinitis [3] and chronic hypertrophic rhinitis [1]. The first line of treatment of ITH is medical. It includes the use of antihistamines and topical corticosteroids with or without decongestants [4]. The estimated success rate of medical treatment ranges between 23.7% and 62% [5]. In patients who are refractory to medical therapy and with persistent nasal blockage, surgery becomes the treatment of choice [3, 4]. Various surgical procedures have been described in the literature most common of which are total and partial inferior turbinectomy. Although very effective in relieving nasal blockage, they are associated with a high risk of bleeding, crusting, pain, and prolonged recovery period [3, 4]. For that reason, total and partial inferior turbinectomy are being aborted by many surgeons and are being substituted by other types of surgeries that attempt to spare the mucosal lining. Many of these surgeries are performed in-office thus reducing the need for general anesthesia. These include radiofrequency ablation or coblation (RFA) which relies on heat to cause tissue fibrosis and shrinkage, electrocautery technique (diathermy electrode, among others) which uses an electrical current to destroy tissue, microdebrider-assisted inferior turbinoplasty (MAIT), and laser assisted turbinoplasty or turbinate reduction. There is ubiquity of reports in the literature on the use of diode lasers such as the Carbon Dioxide (CO2) laser and photoangiolytic lasers, such as the pulse dye laser (PDL) and potassium titanyl phosphate (KTP) laser with successful results. In 2018, Hess et al. introduced the application of blue laser in laryngology [6]. The blue laser is a new photoangiolytic laser, with a wavelength of 445 nm that is preferentially absorbed by oxyhemoglobin leading to selective photoangiolysis with minimal injury to the mucosal lining. It can be used in contact and non-contact modes allowing cutting and photothermolysis with excellent hemostasis. Its hybrid property has markedly expanded its use among otolaryngologists, particularly in office-based laryngeal surgery [6].
There are no studies in the literature on the use of the blue laser in-office for the treatment of ITH. Most of the reports are on office-based blue laser therapy for diseases of the larynx. The aim of this pilot study is to investigate the subjective effect of blue laser turbinate reduction on nasal breathing in a cohort of patients with nasal obstruction. Patient tolerance to the procedure was also analyzed.
Materials and methods
Participants and outcome measures
After obtaining approval from the Institutional Review Board (IRB ID: BIO 2022 − 0280), the medical records and video recordings of patients presenting to a tertiary referral center with nasal obstruction between October 2022 and December 2023, were reviewed. Patients with persistent nasal obstruction despite medical therapy (at least 3 months of intranasal steroid and oral antihistamines) and with evidence of inferior turbinate hypertrophy for which they underwent office-based blue laser therapy were included in the study. The presence of inferior turbinate hypertrophy was confirmed by endoscopic examination of the nasal cavity using a flexible nasopharyngoscope. Patients with history of infectious sinusitis and other sinonasal symptoms such as nasal discharge, post-nasal drip, facial pain, and headache were excluded.
Demographic data retrieved from the patients’ medical charts included age, gender, smoking, presence or absence of septal deviation, and history of prior nasal surgery. The two outcome measures used to gauge the success of surgery were the Nasal Obstruction Symptom Evaluation (NOSE) scale and the Visual Analogue Scale (VAS) for nasal obstruction. The NOSE is a 5-tem questionnaire that rates the symptoms of nasal obstruction from 0, indicating no problem, to 4, indicating a severe problem with a maximum total score of 20. The instrument is then scaled to a total score of 0 to 100 by multiplying the initial score by 5, with a higher score indicating a greater severity of nasal obstruction [7]. Patients also rated the degree of nasal obstruction using a 10-point Likert scale with a greater score reflecting a greater severity of nasal obstruction. Patient’s level of comfort during the procedure was also rated using a 10-point VAS scale with higher score indicating greater level of comfort.
Surgical technique for blue laser turbinate reduction
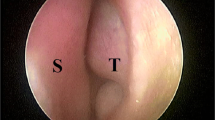
With the patient in a sitting position, nasal patties soaked with Lidocaine 2% were inserted into the nasal cavities and kept in place for 10 min. Following the successful application of topical anesthesia, a 400-micrometer blue laser glass fiber was introduced into the nasal cavity using a 3 mm metallic nasal suction and a Tuohy Borst adapter for fixation. A zero-degree telescope (HOPKINS straightforward telescope 0° from Karl Storz, 2020, Germany) was used for guidance. The blue laser was set at power 10 W, pulse duration 40 ms, and pulse pause 300 ms. The posterior aspect of the inferior turbinate was targeted first and then the anterior aspect until the tip of the turbinate is reached. The laser was used mostly in non-contact mode trying to spare the mucosal lining. Figure 1. In many instances, it was also used in near-contact and contact mode to ensure deeper penetration. Horizontal lines along the inferior and medial surfaces of the inferior turbinate were made simulating zebra lines. Figure 2. The surgery was completed when the medial and inferior surface of the inferior turbinate was blanched. The same procedure was repeated on the contralateral side. An average of 228 J were delivered to the left side and 191 J to the right side with a total mean of 419 Joules. Nasal patties soaked with decongestant (xylometazoline hydrochloride 0.1%) were inserted into the nasal cavities after surgery and kept for 5 min as a pre-emptive measure to ensure good hemostasis. The procedure was well tolerated by all patients.
Statistical analysis
Statistical analysis was conducted using IBM SPSS Statistics version 29. Non-parametric data underwent analysis via the Wilcoxon signed-rank test for intra-group comparison before and after intervention and the Mann-Whitney U test was used for inter-group comparison. Parametric data were analyzed using the paired samples t-test for intra-group comparison and independent sample t for inter-group comparison. Chi-square test was used for the comparison of proportions between categorical variables. For all the tests, a p-value of < 0.05 was considered as statistically significant.
Results
Demographic data
A total of 14 patients, 12 males and 2 females, were included in this investigation. The mean age of the study group was 41.47 ± 18.52 years. Almost half the patients were smokers, and 14.2% reported a prior history of nasal surgery. See Table 1.
The NOSE and VAS scores before and after blue laser therapy
All patients had a decrease in the NOSE score after surgery. The mean NOSE score of the study group decreased significantly from 13.07 ± 3.89 pre-operatively to 2.64 ± 2.43 post-operatively (p = 0.002). Similarly, all patients had a decrease in the VAS score for nasal obstruction after surgery, The mean VAS score of the study group decreased from 7.43 ± 0.85 pre-operatively to 2.0 ± 1.57 post-operatively (p = 0.002). See Table 2.
Level of comfort during the procedure
The procedure was well-tolerated by all patients. Using the VAS, the level of comfort ranged from 6 to 9 with an average of 7.59 ± 1.34.
Discussion
The blue laser is a new photoangiolytic laser that is taking place over the old generation of photoangiolytic lasers. Its high affinity to oxyhemoglobin allows selective photo-thermolysis of vascular structures. Moreover, its low energy setting and minimal scattering result in minimal injury and necrosis to surrounding tissues [6]. When applied to the inferior turbinate in non-contact mode, it leads to selective photocoagulation of the submucosal microvasculature with negligeable injury to the epithelial lining. This is best seen as blanching of the mucosal cover of the inferior turbinate during surgery. The results of this study indicate that office-based blue laser therapy for ITH is effective in treating nasal obstruction. All patients had subjective improvement in nasal breathing following treatment. There was a significant decrease in the mean NOSE score from 13.07 ± 3.89 to 2.64 ± 2.43, and a significant decrease in the mean VAS score from 7.43 ± 0.85 to 2.0 ± 1.57 post-operatively. Moreover, the procedure was tolerated well by all the patients.
Our findings are in agreement with many studies in the literature on the efficacy of laser-assisted turbinoplasty in patients with nasal obstruction using other types of lasers [8,9,10,11,12,13,14]. In 2014, in a study on the efficacy of CO2 laser therapy for ITH among other treatment modalities, Prokopakis et al. reported improvement in the VAS score for nasal obstruction by 3.99 [16]. In 2016, Vijayakumar et al. noted an overall subjective improvement in nasal obstruction following KTP laser therapy for ITH in 73.33% of their case study of 30 patients. The subjective improvement in nasal symptoms was associated with a significant reduction in patient self-reported Sino-Nasal Outcome Test score [14]. In 2020, Ravichandran et al. conducted a randomized controlled trial on 209 patients with ITH who were treated in-office using the KTP or CO2 laser and noted a significant improvement in the NOSE score at follow-up in 93% and 77% of the cases, respectively [15]. In 2021, Harju et al. evaluated the effect of diode laser therapy for ITH in comparison to radiofrequency ablation and MAIT and noted a significant decrease in the VAS score for severity of nasal obstruction by 4.2 [17]. In 2022, in a study on 53 patients treated with the CO2 laser, Hussain and Ahmad reported a significant reduction in the NOSE score from 64.9 ± 13.29 to 5.09 ± 4.28, and in the VAS score from 6.05 ± 2.1 to 1.18 ± 0.4 at 3 months postoperatively [11]. A recent systematic review by Zhang et al. looked into all inferior turbinate reduction techniques and demonstrated a statistically significant improvement in the VAS for nasal obstruction when using the laser-assisted turbinate reduction [3].
This is the first study that investigates the effectiveness of blue laser treatment of ITH in patients with nasal obstruction. In the era where KTP laser is phasing out and being substituted with the blue laser, the findings of this pilot study may be useful. Nevertheless, although this study showed that blue laser inferior turbinate therapy is effective in improving nasal obstruction, the results should be cautiously interpreted. There are limitations to the use of the blue laser in turbinate surgery, namely in regard to the depth of penetration which is limited to 1 mm at low power and 3–4 mm at high power when used in close contact [6]. Another limiting factor is the high scattering that varies with the angle of divergence of the laser which in turn varies with the distance from the glass fiber to target. These two limitations may be disadvantageous when trying to reach the deep erectile tissues of the inferior turbinates. Another constraint of blue laser turbinate therapy is the inability to spare entirely the mucosal epithelium as a result of thermogenesis and or direct contact of the glass fiber with the mucosa. Histological examination of the inferior turbinates is needed to establish the deep and superficial structural changes following therapy and probably its long-term effects.
This study has its limitations; One is its limited sample size and second is the lack of objective measure of nasal obstruction such as rhinometry. More prospective studies comparing the blue laser to other types of lasers or other inferior turbinate volume reduction techniques are needed to highlight the added value of the blue laser in the treatment of ITH.
Conclusion
Office-based blue laser therapy for inferior turbinate hypertrophy may be an effective treatment modality for nasal obstruction from the patient’s perspective. Although the procedures were tolerated well with no complications noted, these results should be cautiously interpreted until studies using objective measures will compare blue laser coagulation with established techniques such as mucosa-sparing sub-mucous turbinate reduction.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Karamatzanis I, Kosmidou P, Ntarladima V et al (2022) Inferior turbinate hypertrophy: a comparison of Surgical techniques. Cureus. https://doi.org/10.7759/cureus.32579
Clark DW, Del Signore AG, Raithatha R et al (2018) Nasal airway obstruction: prevalence and anatomic contributors. Ear Nose Throat J. https://doi.org/10.1177/014556131809700615
Zhang K, Pipaliya RM, Miglani A et al (2023) Systematic review of Surgical interventions for Inferior Turbinate Hypertrophy. Am J Rhinol Allergy. https://doi.org/10.1177/19458924221134555
Abdullah B, Singh S (2021) Surgical interventions for Inferior Turbinate Hypertrophy: a Comprehensive Review of Current techniques and technologies. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph18073441
Benninger M, Farrar JR, Blaiss M et al (2010) Evaluating approved medications to treat allergic rhinitis in the United States: an evidence-based review of efficacy for nasal symptoms by class. Ann Allergy Asthma Immunol. https://doi.org/10.1016/j.anai.2009.11.020
Hess MM, Fleischer S, Ernstberger M (2018) New 445 nm blue laser for laryngeal surgery combines photoangiolytic and cutting properties. Eur Arch Otorhinolaryngol. https://doi.org/10.1007/s00405-018-4974-8
Stewart MG, Witsell DL, Smith TL et al (2004) Development and validation of the nasal obstruction symptom evaluation (NOSE) scale. Otolaryngol Head Neck Surg. https://doi.org/10.1016/j.otohns.2003.09.016
Caffier PP, Frieler K, Scherer H et al (2008) Rhinitis medicamentosa: therapeutic effect of diode laser inferior turbinate reduction on nasal obstruction and decongestant abuse. Am J Rhinol. https://doi.org/10.2500/ajr.2008.22.3199
Cakli H, Cingi C, Güven E et al (2012) Diode laser treatment of hypertrophic inferior turbinates and evaluation of the results with acoustic rhinometry. Eur Arch Otorhinolaryngol. https://doi.org/10.1007/s00405-012-1963-1
Volk GF, Pantel M, Guntinas-Lichius O et al (2010) Prognostic value of anterior rhinomanometry in diode laser turbinoplasty. Arch Otolaryngol Head Neck Surg. https://doi.org/10.1001/archoto.2010.161
Hussain RT, Ahmad R (2022) Role of CO2 laser in the management of symptomatic hypertrophy of Inferior nasal turbinates. Indian J Otolaryngol Head Neck Surg. https://doi.org/10.1007/s12070-020-01876-z
Testa D, Motta G, Galli V et al (2006) Outcome assessment in patients with chronic obstructive rhinitis CO2 laser treated. Acta Otorhinolaryngol Ital
Supiyaphun P, Aramwatanapong P, Kerekhanjanarong V et al (2003) KTP laser inferior turbinoplasty: an alternative procedure to treat the nasal obstruction. Auris Nasus Larynx. https://doi.org/10.1016/s0385-8146(02)00104-9
Vijayakumar S, Divakaran S, Parida PK et al (2016) Potassium titanyl phosphate laser turbinate reduction in the management of allergic inferior turbinate hypertrophy: our experience. Allergy Rhinol (Providence). https://doi.org/10.2500/ar.2016.7.0151
Ravichandran SP, Ramasamy K, Parida PK et al (2020) Comparison of efficacy of potassium titanyl phosphate laser & diode laser in the management of inferior turbinate hypertrophy: a randomized controlled trial. Indian J Med Res. https://doi.org/10.4103/ijmr.IJMR_424_18
Prokopakis EP, Koudounarakis EI, Velegrakis GA (2014) Efficacy of inferior turbinoplasty with the use of CO(2) laser, radiofrequency, and electrocautery. Am J Rhinol Allergy. https://doi.org/10.2500/ajra.2014.28.4044
Harju T, Numminen J (2021) The effect of inferior turbinate surgery on nasal symptoms and inferior turbinate contractility. Am J Otolaryngol. https://doi.org/10.1016/j.amjoto.2020.102778
Acknowledgements
Not applicable.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by Jad Hosri, Yara Yammine, Patrick Abou Raji Feghali and Lana Ghzayel. The first draft of the manuscript was written by Abdul-Latif Hamdan, Jad Hosri, Yara Yammine and Nader Nawfal. Critical review and editing were done by Elie Alam and Maher Kasti. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Institutional Review Board of the American University of Beirut (IRB ID: BIO-2022-0280).
Competing interests
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hamdan, AL., Hosri, J., Yammine, Y. et al. Office-based blue laser therapy for inferior turbinate hypertrophy: a pilot study. Eur Arch Otorhinolaryngol 281, 5357–5361 (2024). https://doi.org/10.1007/s00405-024-08781-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-024-08781-z