Abstract
Purpose
Oropharyngeal and tongue exercises (myofunctional therapy) have been shown to improve obstructive sleep apnea. However, to our knowledge, a systematic review has not been performed for snoring. The study objective is to perform a systematic review, with a meta-analysis, dedicated to snoring outcomes after myofunctional therapy.
Methods
PubMed/MEDLINE and three other databases were searched through November 25, 2017. Two authors independently searched the literature. Eligibility (1) patients: children or adults with snoring, (2) intervention: oropharyngeal and/or tongue exercises, (3) comparison: pre and post-treatment data for snoring, (4) outcomes: snoring frequency and snoring intensity, (5) study design: publications of all study designs.
Results
A total of 483 articles were screened, 56 were downloaded in their full text form, and nine studies reported outcomes related to snoring. There were a total of 211 patients (all adults) in these studies. The snoring intensity was reduced by 51% in 80 patients from pre-therapy to post-therapy visual analog scale values of 8.2 ± 2.1 (95% CI 7.7, 8.7) to 4.0 ± 3.7 (95% CI 3.2, 4.8). Berlin questionnaire snoring intensity reduced by 36% in 34 patients from 2.5 ± 1.0 (95% CI 2.2, 2.8) to 1.6 ± 0.8 (95% CI 1.3, 1.9). Finally, time spent snoring during sleep was reduced by 31% in 60 patients from 26.3 ± 18.7% (95% CI 21.6, 31.0) to 18.1 ± 20.5% (95% CI 12.9, 23.3) of total sleep time.
Conclusions
This systematic review demonstrated that myofunctional therapy has reduced snoring in adults based on both subjective questionnaires and objective sleep studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There have been several treatments developed over the years to treat snoring and obstructive sleep apnea (OSA) [1,2,3,4]. Of the current techniques to treat snoring and OSA, many of them are invasive and involve either performing surgery or wearing a device during sleep [5,6,7]. A technique that can serve either as a primary treatment or as an adjunct treatment to treat primary snoring that does not require either surgery or wearing a device would be beneficial. Tongue exercises and oropharyngeal exercises (myofunctional therapy) have improved OSA in children and adults [8]. In a previous meta-analysis evaluating myofunctional therapy, apnea-hypopnea index was reduced by 50% in adults and 62% in children [8]. The sub-analysis, evaluating patients with sleep study snoring, demonstrated a significant reduction from 14.05 ± 4.89% to 3.87 ± 4.12% of total sleep time, p value < 0.001 [8].
Since the publication of the meta-analysis for OSA, there have been several studies evaluating oropharyngeal exercises and tongue exercises and their outcomes for snoring; however, to our knowledge, there has been no systematic review or meta-analysis evaluating the effect on snoring. To provide the most up-to-date information, a systematic review would be required. Therefore, the objective of this study was to perform a systematic review for snoring, specifically using the PICOS acronym, as follows: (1) Patients (P) adults or children who snore; (2) Intervention (I) oropharyngeal exercises and/or tongue exercises; (3) Comparison (C) data pre and post-exercises; (4) Outcomes (O) snoring frequency, snoring index, percentage of night spent snoring, visual analog scale (VAS), and Likert scales; (5) Study design (S) any study type or design. After obtaining the studies, the pre- and post-oropharyngeal exercises and tongue exercises snoring data were analyzed.
Methods
The preferred reporting items for systematic reviews and meta-analysis (PRISMA) statement were reviewed and used as a guide during this study [9].
Protocol
Our Institutional Department of Clinical Investigation was contacted, and a protocol was submitted and was approved. For this type of study, formal consent is not required.
Eligibility criteria
The inclusion criteria for this review: (1) studies with adult or pediatric patients who were treated with oropharyngeal exercises and tongue exercises as the sole intervention and (2) the publication provided both pre- and post-oropharyngeal exercises and tongue exercises quantitative outcomes for snoring. Exclusion criteria: studies with additional treatments performed, studies using devices, and studies without data for myofunctional therapy alone.
Information sources
We searched PubMed/MEDLINE, Google Scholar, The Cochrane Library and Cumulative Index to Nursing and Allied Health (CINAHL).
Search
Authors M. C. and M. W. N searched through May 8, 2017 initially, and provided additional updating through November 25, 2017. An example of a search strategy is the one used for PubMed/MEDLINE: [(Snoring OR Sleep) AND (“tongue exercise” OR “tongue exercises” OR “orofacial” OR “myotherapy” OR “speech therapy” OR “oropharyngeal exercises” OR “myofascial reeducation” OR “myofunctional therapy” OR “upper airway exercises” OR (“Myofunctional Therapy“[MeSH]))]. For the remaining databases, we applied very similar keywords and terms, just tailored to the specific databases.
Authors extracted the snoring data from the studies meeting the predefined selection criteria. If a study did not provide the information necessary to include it in the review, then the study authors were emailed at least twice in an attempt to obtain the data.
Risk of bias and heterogeneity
If there are sufficient summary measures provided, then an analysis for bias and heterogeneity would be performed using REVMAN.
Summary measures
Study measures collected include the means, standard deviations (SD), medians, and other summary measures provided by the individual studies.
Results
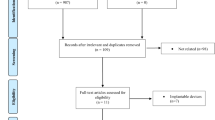
A total of 483 articles were screened, 56 were downloaded in their entirety, and nine studies [10,11,12,13,14,15,16,17,18] with 211 patients met the inclusion criteria, see Supplementary Fig. 1. The studies provided data for snoring frequency, snoring intensity, snoring severity, and bedpartner visual analog scale scores, see Table 1. The studies that used Berlin questionnaire and values for snoring frequency were rated as follows: 0 = never, 1 = 1–2 times a month, 2 = 1–2 times a week, 3 = 3–4 times a week, and 4 = every day [19]. Values for snoring intensity were 0 = no snoring, 1 = similar to breathing, 2 = as loud as talking, 3 = louder than talking, and 4 = very loud, and can be heard in adjacent rooms [19].
For the 211 patients who performed myofunctional therapy, the mean snoring frequency and snoring intensity were reduced, see Table 2. In 80 patients, the snoring intensity reduced by 51%, from pre-therapy to post-therapy using the VAS values [from 8.2 ± 2.1 (95% CI 7.7, 8.7) to 4.0 ± 3.7 (95% CI 3.2, 4.8)]. A sub-analysis was performed for VAS using random effects modeling, which demonstrated a mean difference of − 3.67 [95% CI − 4.44, − 2.90], overall effect Z = 9.34, p value < 0.00001, Q statistic p value = 0.64, and I 2 = 0% (Fig. 1). The VAS standardized mean difference was − 1.46 (95% CI − 1.81, − 1.11), overall effect Z = 8.15, p value < 0.00001, Q statistic p value = 0.54, and I 2 = 0% (Fig. 1).
In studies that used the Berlin questionnaire, snoring intensity reduced in 34 patients from 2.5 ± 1.0 (95% CI 2.16, 2.84) to 1.6 ± 0.8 (95% CI 1.33, 1.87). A sub-analysis was performed for Berlin scores for snoring using random effects modeling, which demonstrated a mean difference of − 0.95 (95% CI − 1.46, − 0.44], overall effect Z = 3.67, p value = 0.0002, Q statistic p value = 0.22, and I 2 = 33% (Fig. 2). The Berlin scores for snoring using standardized mean difference were − 1.17 (95% CI − 2.70, 0.35), overall effect Z = 1.51 p value = 0.13, Q statistic p value = 0.005, and I 2 = 88% (Fig. 2).
Time spent snoring during sleep was reduced by 31.2% in 60 patients from 26.3 ± 18.7% (95% CI 21.6, 31.0) to 18.1 ± 20.5% (95% CI 12.9, 23.3) of total sleep time. A sub-analysis was performed for percentage of time spent snoring with random effects modeling, demonstrating a mean difference of − 10.01 percent of the night (95% CI − 12.24, − 7.78), overall effect Z = 8.79, p value < 0.0001, Q statistic p value = 0.45, and I 2 = 0% (Fig. 3). The percentage of time spent snoring’s standardized mean difference was − 1.26 (95% CI − 3.14, 0.63) (large effect using Cohen’s guidelines), overall effect Z = 1.31 p value = 0.19, Q statistic p value < 0.00001, and I 2 = 95%.
Overall, the exercises described were generally performed for 3 months and consisted of four main locations, the soft palate, the tongue, facial exercises, pharyngeal exercises, jaw exercises, and stomatognathic exercises [10,11,12,13,14,15,16,17,18]. Soft palate exercises generally consisted of saying vowels, which recruits the palatoglossus, palatopharyngeus, tensor veli palatini, levator veli palatini, and the uvula [12]. Tongue exercises generally consisted of moving the tongue in different directions with or without sticking the tongue out, pressing against bony and soft tissue structures within the oral cavity, sucking the tongue against the palate, and other tongue movements with or without resistance [10,11,12,13,14,15,16,17,18]. Facial exercises generally involve recruitment of the buccinator muscles by placing a finger into the oral cavity and pressing in an outward direction and puckering, closing or moving the lips [10,11,12,13,14,15,16,17,18]. Jaw exercises involve opening/closing/exercising the jaw. Pharyngeal exercises can involve swallowing exercises. Finally, stomatognathic functional exercises can involve sucking through a narrow straw, inflating balloons and swallowing and chewing exercises.
Individual studies
Diaferia et al. [12] evaluated 100 patients who were randomized into various treatments and 27 were placed into the myofunctional therapy treatment arm. The myofunctional therapy consisted of tongue, soft palate, stomatognathic function, and facial exercises [12]. The patients performed the exercises three times daily, for 20 min sessions, a total of 3 months [12]. The snoring frequency using the visual analog scale was 8.5 ± 2.3 and 4.9 ± 3.2 (42% reduction) before and after myofunctional therapy [12]. The snoring intensity reduced from 7.7 ± 2.3 to 4.3 ± 2.8 before and after treatment, corresponding to a 44% reduction) [12].
Mohamed et al. [18] treated 30 patients with OSA by having them perform oropharyngeal exercises (soft palate, tongue, facial muscles, and stomatognathic function exercises) [18]. Exercises were performed for at least 10 min, three to five times a day for 3 months. The patients were divided into two groups (Group 1 with moderate OSA and Group 2 with severe OSA) [18]. Snoring index in patients with moderate OSA reduced by 24%, and the percent time spent snoring during the sleep study decreased by 37%. However, in patients with severe OSA, the snoring index only reduced by 10%, and the percent time spent snoring during the sleep study only reduced by 9%.
Verma et al. [17] evaluated 20 patients who were treated with myofunctional therapy. The exercises were performed five times daily, for 3 months [17]. The exercises performed included tongue exercises, jaw exercises, lip exercises, and soft palate exercises [17]. The researchers used the Berlin scoring for snoring. The snoring intensity was reduced from 2.8 ± 0.5 before myofunctional therapy down to 1.7 ± 0.6 after myofunctional therapy (a 39% reduction) [17].
Ieto et al. [14] treated nineteen patients with myofunctional therapy to include tongue exercises, palate exercises, facial exercises, and chewing/swallowing exercises. The patients performed the myofunctional therapy exercises for approximately 8 min daily for 3 months [14]. The researchers used the Berlin scoring. The median values for snoring frequency were reported and were 4 (3–4) before myofunctional therapy and 2 (1.5–3) after myofunctional therapy [14]. The snoring intensity reduced from 4 (2.5–4) before treatment, down to 1 (1–2) after treatment [14].
Kayamori and Filho [15] had 14 patients who underwent myofunctional therapy and had data that could be analyzed. The exercises were performed three times a day for 3 months [15]. Exercises included tongue exercises, soft palate exercises, facial exercises, and chewing/swallowing exercises [15]. The researchers used the Berlin scoring. The authors found that the snoring frequency did not change significantly 2.7 ± 1.4 to 2.6 ± 1.3 (4% reduction); however, the snoring intensity did decrease from 2.0 ± 1.4 to 1.5 ± 1.0 (25% reduction) [15].
Nemati et al. [16] reported treating 53 patients with primary snoring with myofunctional therapy for 30 min sessions, 5 days a week for 3 months. Patients performed soft palate exercises, tongue exercises, and facial exercises [16]. The researchers used the Lim and Curry snoring scale score (SSS) [20], frequency of snoring (every night, most nights, some nights, and seldom/never), the duration of snoring (all night long, most hours of the night, or some hours of the night), and the visual analog scale (0–10) [16]. The snoring severity scale demonstrated a reduction in snoring from 7.0 ± 1.7 to 3.1 ± 2.7 (56% reduction) [16]. The frequency of snoring based on the percentage of patients who snored every night or most nights was reduced from 91 to 36% [16]. The visual analog scale demonstrated an improvement in snoring from 8.5 ± 1.9 to 4.7 ± 2.9 (45% reduction) [16].
Baz et al. [10] evaluated 30 patients based on symptoms and a sleep study. The patients performed exercises for at least 10 min, 3–5 times daily for 3 months [10]. The myofunctional therapy included tongue exercises, the soft palate exercises, and pharyngeal exercises. Before myofunctional therapy, 100% of patients snored and afterwards 53% snored [10]. The sleep study demonstrated a reduction in the total time spent snoring from 14.1 ± 4.9% down to 3.9 ± 4.1%, which is a 72% reduction [10].
Guimaraes et al. [13] reported outcomes for 16 patients who were treated with myofunctional therapy for 3 months. Exercises performed included the tongue exercises, soft palate exercises, facial exercises, and stomatognathic function exercises [13]. The snoring frequency and intensity were obtained using the Berlin questionnaire. The median values for snoring frequency reduced from 4 (4–4) down to 3 (1.5–3.5) [13]. The median values for snoring intensity reduced from 3 (3–4) down to 1 (1–2), a 67% reduction [13].
Berreto et al. [11] had two patients who performed myofunctional therapy for 16 weeks. Exercises included tongue exercises, facial exercises, soft palate exercises, pharyngeal exercises, jaw exercises, and stomatognathic function exercises. Snoring was grades 0–4, where 0 = no snoring, 1 = heavy breathing, 2 = light snoring, 3 = snoring that disturbs the bedpartner, and 4 = snoring that disturbs the family [11]. The snore score decreased from 3 to 2 for both patients, corresponding to a 33% reduction [11].
Discussion
There are three main findings from this systematic review. First, the systematic review has demonstrated an improvement in snoring by approximately 50% after myofunctional therapy. An improvement is seen in all the study measures (Berlin questionnaires, VAS, and snoring during the sleep study). The studies have all been in adult patients thus far, and to our knowledge, a pediatric study has not reported outcomes for snoring. Interestingly, the 50% improvement in snoring seen in adults is consistent with the improvement seen in OSA (also 50%) in the meta-analysis performed for myofunctional therapy and OSA [8]. In addition, there was objective improvement in snoring based on polysomnography, with a 31% improvement in the percentage of time spent snoring.
Second, pediatric studies are lacking. Although there are no pediatric studies evaluating snoring, there was a significant improvement in pediatric OSA after myofunctional therapy in the previous meta-analysis [8]. Therefore, it is likely that the improvement in snoring would have also been noted in children; however, we cannot generalize, since there were no studies identified. Anecdotally, a few of the authors’ (MC, CG, and SZ) pediatric patients undergoing myofunctional therapy as adjunct or primary treatment for snoring or OSA have been noted to have significant decreases in the snoring intensity and frequency. Interestingly, there is debate regarding snoring in pediatric patients: younger children have a greater chance of sleeping closer to their parents, while older pre- and peri-pubertal children usually sleep farther away from where parents sleep; therefore, the parents are more likely to hear younger children. This snoring phenomenon is even more true for pubertal and post-pubertal teenagers: therefore, there is a clear change in the possibility of perception of snoring during childhood and this has been pointed out in different pediatrics studies. In adults, there is a bias on reporting given that snoring complaints are bedpartner driven; therefore, adults who sleep alone generally do not have people complain unless they share a room for some reason. This bedpartner phenomenon presents a risk of bias concerning snoring outcomes, but despite this potential bias, the studies were consistent in their findings of decreased snoring noted after myofunctional therapy.
Third, although there are improvements in snoring, the mechanism of action as to why myofunctional therapy improves snoring are not completely understood. Given that the lips, facial muscles, tongue, soft palate, oral cavity, and pharynx are exercised by the techniques used in the studies in this manuscript, we hypothesize that the training improves both tone and positioning. An analogy could be seen in people who have never lifted weights and want to start weight training; initially, they will not be able to lift as much weight, but after lifting for 3 months, they will have improved strength and tone. It is possible, therefore, that the myofunctional therapy can help improve the tone and strength of the oral cavity, tongue, soft palate, and pharynx analogous to the improvement in strength and tone that is seen with weight training. Friberg et al. demonstrated that heavy snorers have a neuropathy of the soft palate when compared to control patients and there is even more neuropathy in patients with OSA [21]. Engelke et al. explored orofacial training and hypothesized that it promotes a closed oral rest position which can help to keep the tongue in contact with the palate and lead to an intraoral negative pressure which may help stabilize the pharynx into a more open position (and may also reduce the neuromuscular activity necessary to maintain the open airway) [22].
Limitations
As with all systematic reviews, we are limited to the currently published studies. It is possible that authors who have not seen a difference in snoring outcomes for their patients did not submit their findings, or if they did submit their findings, then maybe their study was not accepted secondary to publication bias against negative studies.
Conclusions
This systematic review demonstrated that myofunctional therapy has reduced snoring in adults based on both subjective questionnaires and objective sleep studies. No pediatric studies were identified. Additional research is recommended based on these initial encouraging results.
References
Abdullatif J, Certal V, Zaghi S, Song SA, Chang ET, Gillespie MB, Camacho M (2016) Maxillary expansion and maxillomandibular expansion for adult OSA: a systematic review and meta-analysis. J Cranio-Maxillo-Fac Surg 44(5):574–578. https://doi.org/10.1016/j.jcms.2016.02.001
Camacho M, Certal V, Capasso R (2013) Comprehensive review of surgeries for obstructive sleep apnea syndrome. Braz J Otorhinolaryngol 79(6):780–788. https://doi.org/10.5935/1808-8694.20130139
Camacho M, Li D, Kawai M, Zaghi S, Teixeira J, Senchak AJ, Brietzke SE, Frasier S, Certal V (2016) Tonsillectomy for adult obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope. https://doi.org/10.1002/lary.25931
Riaz M, Certal V, Nigam G, Abdullatif J, Zaghi S, Kushida CA, Camacho M (2015) Nasal expiratory positive airway pressure devices (provent) for OSA: a systematic review and meta-analysis. Sleep Disord 2015:734798. https://doi.org/10.1155/2015/734798
Certal V, Nishino N, Camacho M, Capasso R (2013) Reviewing the systematic reviews in OSA surgery. Otolaryngol Head Neck Surg. 149 (6):817–829. https://doi.org/10.1177/0194599813509959
Certal VF, Zaghi S, Riaz M, Vieira AS, Pinheiro CT, Kushida C, Capasso R, Camacho M (2015) Hypoglossal nerve stimulation in the treatment of obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope 125(5):1254–1264. https://doi.org/10.1002/lary.25032
Kumar AR, Guilleminault C, Certal V, Li D, Capasso R, Camacho M (2014) Nasopharyngeal airway stenting devices for obstructive sleep apnoea: a systematic review and meta-analysis. J Laryngol Otol:1–9. https://doi.org/10.1017/s0022215114003119
Camacho M, Certal V, Abdullatif J, Zaghi S, Ruoff CM, Capasso R, Kushida CA (2015) Myofunctional therapy to treat obstructive sleep apnea: a systematic review and meta-analysis. Sleep 38(5):669–675. https://doi.org/10.5665/sleep.4652
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Baz H, Elshafey M, Elmorsy S, Abu-Samra M (2012) The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea. PAN Arab J Rhinol 2(1):17–22
Berreto e Silva Pitta D, Farias Pessoa A, Sampaio AL, Nonato Rodrigues R, Guiot Tavares M, Tavares P (2007) Oral myofunctional therapy applied on two cases of severe obstructive sleep apnea. Intl Arch Otorhinolaryngol 11(3):350–354
Diaferia G, Santos-Silva R, Truksinas E, Haddad FL, Santos R, Bommarito S, Gregorio LC, Tufik S, Bittencourt L (2016) Myofunctional therapy improves adherence to continuous positive airway pressure treatment. Sleep Breath (Schlaf & Atmung). https://doi.org/10.1007/s11325-016-1429-6
Guimaraes KC, Drager LF, Genta PR, Marcondes BF, Lorenzi-Filho G (2009) Effects of oropharyngeal exercises on patients with moderate obstructive sleep apnea syndrome. Am J Respir Crit Care Med 179(10):962–966. https://doi.org/10.1164/rccm.200806-981OC
Ieto V, Kayamori F, Montes MI, Hirata RP, Gregorio MG, Alencar AM, Drager LF, Genta PR, Lorenzi-Filho G (2015) Effects of oropharyngeal exercises on snoring: a randomized trial. Chest 148(3):683–691. https://doi.org/10.1378/chest.14-2953
Kayamori F (2015) The effects of myofunctional and orofascial therapy in patients with primary snoring and obstructive sleep apnea and anatomy and airway function. Doctoral thesis, Faculdade de Medicina, pp 1–116
Nemati S, Gerami H, Soltanipour S, Saberi A, Moghadam SK, Setva F (2015) The effects of oropharyngeal-lingual exercises in patients with primary snoring. Eur Arch Oto-Rhino-Laryngol 272 (4):1027–1031. https://doi.org/10.1007/s00405-014-3382-y
Verma RK, Johnson JJ, Goyal M, Banumathy N, Goswami U, Panda NK (2016) Oropharyngeal exercises in the treatment of obstructive sleep apnoea: our experience. Sleep Breath (Schlaf Atmung) 20(4):1193–1201. https://doi.org/10.1007/s11325-016-1332-1
Mohamed AS, Sharshar RS, Elkolaly RM, Serageldin SM (2016) Upper airway muscle exercises outcome in patients with obstructive sleep apnea syndrome. Egypt J Chest Dis Tuberc. https://doi.org/10.1016/j.ejcdt.2016.08.014 (Epub ahead of print)
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP (1999) Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491
Lim PV, Curry AR (1999) A new method for evaluating and reporting the severity of snoring. J Laryngol Otol 113(4):336–340
Friberg D (1999) Heavy snorer’s disease: a progressive local neuropathy. Acta oto-laryngologica 119(8):925–933
Engelke W, Engelhardt W, Mendoza-Gartner M, Decco O, Barrirero J, Knosel M (2010) Functional treatment of snoring based on the tongue-repositioning manoeuvre. Eur J Orthod 32(5):490–495. https://doi.org/10.1093/ejo/cjp135
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria, educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required. There is no additional need for informed consent as no identifying information is included in this article.
Additional information
The views expressed in this abstract/manuscript are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Camacho, M., Guilleminault, C., Wei, J.M. et al. Oropharyngeal and tongue exercises (myofunctional therapy) for snoring: a systematic review and meta-analysis. Eur Arch Otorhinolaryngol 275, 849–855 (2018). https://doi.org/10.1007/s00405-017-4848-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-017-4848-5