Abstract
Purpose
Sexuality and the desire for children are closely linked, and infertility can increase the risk of sexual dysfunction (SD). Among heterosexual infertile couples undergoing assisted reproductive technology (ART) cycles, those referred for donor sperm cycles constitute a specific subgroup, potentially different than those undergoing ART with partner’s sperm, as giving up on biological parenthood can be difficult to overcome. However, the impact of donor sperm ART on infertile couples’ sexuality has been hardly explored in the literature. This study aimed to describe the sexual function in couples undergoing ART with donor sperm.
Methods
This monocentric prospective observational study was conducted in heterosexual couples undergoing ART cycle with sperm donor, using the FSFI and the IIEF15 questionnaires. Seventy-nine couples were solicited to participate in the study.
Results
In our sample, 39.3% (n = 24) of women had sexual dysfunction (SD). Among men, 26.5% (n = 13) had erectile dysfunction (ED). No statistically significant difference was found between both groups (with or without SD) in men and women in univariate analysis. Therefore, multivariate analysis was not performed and no specific predictor of SD could be identified.
Conclusion
Although this should be confirmed in a larger number of participants, our study demonstrates that a significant proportion of infertile patients undergoing ART with donor semen suffer from SD. No significant predictor could, however, be identified. Further research should focus on the evaluation of psychological interventions to treat or improve these disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
"A significant proportion of infertile patients undergoing ART with donor semen suffer from Sexual Dysfunction, but no significant predictor could however be identified in this study". |
Introduction
An increasing number of couples face infertility. Although many of them will achieve childbearing, the diagnosis of infertility, as well as subsequent infertility care, are very likely to affect their quality of life [1]. Infertility can indeed lead to a feeling of physical and/or psychological aggression due to the diagnosis, the therapies, but also the repeated failures [1], which can trigger feelings of injustice or anger. Infertility and its treatments may also lead to changes in self-esteem and are associated with anxiety and sadness [2]. Low self-esteem has been shown to increase stress levels during treatment [3].
“Healthy sexuality is essential for psychological well-being and quality of life” according to the World Health Organization [4]. As sexuality and the desire for children may be linked, infertility can lead to dissociating sexuality from sexual desire and pleasure [5] with an increased risk of sexual dysfunction (SD) diagnosed when the disturbances in sexual functioning described by the patient cause marked subjective suffering. A significant impact on sexual life was reported with 21% of patients reporting an absence of sexual intercourse for several weeks or even months [6]. It has been reported that as much as 32% of women and 23% of men show signs of depression with sexual desire disorders resulting from the discovery of infertility and its management [7]. Men often associate fertility with virility [8]. The prevalence of erectile dysfunction (ED) appears to be higher in men with infertility [7]. After diagnosis of impaired semen parameters, 11% of erectile or orgasmic problems were reported [9], and male sexual satisfaction scores were lower compared to men in couples with female factor infertility [10]. The prevalence of SD in women in infertile couples also appears to be higher than in the general population [7]. Women whose male partner suffers from severe infertility seem to have a decrease in satisfaction during sexual intercourse [11]. The announcement of azoospermia can be a devastating experience and men with infertility will feel stigmatized because they are perceived as being deficient in a specific component of their masculinity [12].
Surprisingly, the impact on the sexuality of couples resorting to donor conception has been hardly explored in the literature. In a small cohort of 16 couples, men reported a period of impotence and a decrease in the number of sexual encounters following the diagnosis, and women experienced anger for a short period of time, but without any decrease in the frequency of sexual encounters [13]. In contrast, Reder et al. [14] reported a higher frequency of sexual desire disorders in couples enrolled in autologous ART compared to those in intrauterine insemination with donor sperm (IUI-D). Among the numerous scientific questionnaires available in the literature to assess human sexuality, the Female Sexual Function Index (FSFI) and the International Index of Erectile Function (IIEF) appear to be the most relevant ones.
This preliminary study aimed to describe sexual function in couples undergoing ART with donor sperm and to determine which demographic characteristics or medical covariates were associated with SD.
Patients and methods
This monocentric prospective observational study was conducted in heterosexual couples undergoing ART cycle with sperm donation, either in vitro fertilization (IVF) or intra-uterine insemination (IUI) in our University-based ART center between October 2019 and October 2021. Of note, inclusions were suspended for several months due to the closure of the center in the context of the COVID-19 epidemic. All couples with women aged between 18 and 43 years who referred for donor sperm-assisted reproduction were solicited. Oral informed consent was obtained from all individual participants included in the study. Exclusion criteria were pre-existing sexual disorders unrelated to diagnosis or medical management or oral opposition by the patients when the study is offered to them. The study was approved by the local ethics committee GNEDS (Groupe Nantais d’Ethique dans le Domaine de la Santé).
Male and female demographic characteristics were first recorded. Of note, primary–secondary infertility refers to couples with a history of early pregnancy loss without live birth. An anonymous questionnaire was distributed to all eligible couples via the Sphinx software. It included the FSFI questionnaire for women and the IIEF15 questionnaire for men. We chose the Female Sexual Function Index (FSFI) and the International Index of Erectile Function (IIEF) because these questionnaires are often used in studies of sexuality and ART. In addition, they are short, adapted to our study, and easily interpretable. Both questionnaires are scientifically validated. The questionnaires are validated in French. [15,16,17,18,19].
The FSFI consists of 19 questions investigating 6 areas of female sexual function over the past 4 weeks: desire, lubrication, arousal, orgasm, satisfaction, and pain. Scores range from 0 or 1 to 5 for each question. Each domain is given its own coefficient. The scores for each area are then added together to give a total score between 2 and 36. SD is defined by a score below 26.55 with a specificity of 0.73 and a sensitivity of 0.88 [17]. The IIEF-15 explores male sexual function over the past 4 weeks through 15 questions with 5 or 6 answer choices and grouped into 5 domains: erectile function, orgasm, desire, satisfaction during sex, and overall satisfaction. There is a score per dimension but no overall score, unlike FSFI. The IIEF-15 scores increase with the improvement in the patient's sexuality components. Questions 1–5 and question 15 assess erectile function. According to Cappelleri et al. [19], an Erectile Function (EF) score ≤ 25 out of 30 for these six questions defines erectile dysfunction (ED) with good sensitivity and specificity (Se 0.97 and Sp 0.88). ED severity was then classified into five categories: no ED, mild, mild to moderate, moderate, and severe.
All analyses were performed using Excel version 2019 and/or BiostaTGV online. We first performed a descriptive analysis of the data. Qualitative variables (smoking status, infertility type and etiology, ART protocol, frequency of sexual intercourse) were described by counts and percentages. Quantitative variables were described with means and standard deviation (age, BMI, FFSI score, and IIEF15 domains). To search for independent predictive factors of SD, we divided the male and female populations into two groups (with or without SD) and performed univariate comparative analyses by Fischer's exact test, followed by multivariate analysis when appropriate. A p value < 0.05 was considered statistically significant.
Results
Characteristics of the population
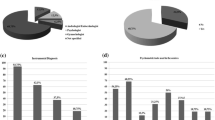
Seventy-nine couples were initially solicited to participate in the study. Sixty-one female questionnaires were finally collected, representing a participation rate of 77.2%, and fifty male questionnaires representing a participation rate of 63.3%. The characteristics of the population are presented in Table 1. Among the respondents, the majority of women reported having sex 1–3 times per month, while men reported having sex 1–2 times per week.
FSFI and IIEF scores
In our sample, 39.3% (n = 24) of women had SD, defined as a FSFI score < 26.55. The average score was 27.5 ± 5.6. Among men, 26.5% (n = 13) had ED according to the IIEF15 erectile function domain analysis. One participant did not answer three out of fifteen questions, so his total IIEF-15 score was not usable; the statistics are calculated on a total of forty-nine men. The average for each domain of FSFI and IIEF-15 scores analyzed is presented in Table 2.
Comparison of populations with and without sexual dysfunction
The comparison of general characteristics between the groups “with SD” and “without SD” is presented in Table 3. No statistically significant difference was found between both groups in men and women in univariate analysis. Therefore, multivariate analysis was not performed and no specific predictor of SD could be identified.
Discussion
In this original study, we found a significant prevalence of ED (26.5%) and female SD (39.3%) among heterosexual couples undergoing ART cycles with sperm donation. Specifically, our study is the first to analyze the prevalence of ED in the context of sperm donation management.
Several studies evaluated sexology among infertile couples. The prevalence of SD detected by the FSFI questionnaire has been reported to range between 26 and 40% among women with infertility [20, 21]. The prevalence of ED observed in the literature ranges between 15 and 22% of men with infertility [7] and was 35% in azoospermic men [22]. A meta-analysis [23] reported a high prevalence of SD (43–90% in women and 48–58% in men). Many reasons are suggested to explain the observed association between SD and infertility: scheduled sexual intercourses, fear of involuntary childlessness, diagnosis of the infertility etiology.
Infertility could also be associated with premature ejaculation and occasional psychological anejaculation for 90% of men at some point in the management of infertility [7]. The prevalence of ED and premature ejaculation has been reported to be positively correlated with the severity of semen abnormalities in men with infertility [24]. According to the European Society of Sexual Medicine (ESSM), ED has been reported in 9–62% of male partners of infertile couples, with severe impairment observed in only 1–3% of ED cases [25]. Moreover, worse semen parameters have been associated with greater ED severity, and low sexual desire has been reported by one third of men of infertile couples [25]. However, in our study, the prevalence of SD was not significantly higher in the “azoospermia” group than in the “another cause” group.
Some studies found that fertile women had a higher FSFI score than women with infertility, the most common disorders being related to desire and lubrication [26]. In a study using the FSFI questionnaire [27], the proportion of females with SD was higher in the infertile versus control group (47% versus 30%, p value: < 0.001). Total orgasm, satisfaction, and pain scores were significantly lower in infertile versus control group [27]. The impact of the primary or secondary character seems contradictory with studies which find that the impact on sexuality was more severe when it came to primary infertility [28] and other studies which find a higher prevalence of SD in secondary women with infertility [29] with a decreased sexual desire, orgasm, and satisfaction compared with primary women with infertility.
Approximately a third of the survey respondents were not fully satisfied with their sexuality. This is in agreement with the literature [30]. We also observed that the frequency of sexual intercourse seemed lower in that population of infertile couples than that of the general population, which has been reported in France to 8.7 per month for both sexes or 1.5 per week on average [31].
Regarding the impact of ART treatment on sexual function, we found no significant difference between newly diagnosed couples awaiting treatment onset but not yet started, and those who already started ART cycles with sperm donation. Studies assessing the impact of the timing of treatment are discordant, probably due to small numbers and the heterogeneity scores used. According to Marci et al. [30], ED were more common in men with a recent diagnosis of infertility compared to the on-treatment group. Similarly, women in the newly diagnosed infertility group had poorer sexual function than those already included in the ART program. In contrast, Bayar et al. [32] reported a significant increase of SD in couples 3 months into treatment compared to the beginning of treatment. This needs further exploration in large-scale and long-term studies. In our study, we did not find a significant association between the duration of infertility and SD. According to a case–control study [33], a duration of infertility of 3 to 6 years was associated with a significant increase in marital conflict. In a recent study, as the number of years of infertility increased, the total score of FSFI was not significantly different but, using the multivariable logistic regression model, when the infertility duration was greater than 8 years, there was a significant increase in the incidence of female SD [34].
Sexuality disorders associated with infertility have, therefore, been widely studied. However, only one study focusing on oocyte recipient population explored sexual function and reported 47% of women with a FSFI score < 26.55 [35]. One study finds that, men using donor sperm expect more positive effects from parenthood on relationships and feelings of fulfillment, and report fewer negative effects of infertility on sexuality, compared with men using their own sperm, but a lower self-image and more guilt [36]. To our knowledge, no study explored sexual function of patients undergoing ART with sperm donation. However, the use of gamete donation seems to lead to a different impact on sexual function as compared to autologous ART (with partner’s sperm) [37]. Indeed, couples enrolled in autologous IUI and IVF had more sexual disorders than couples receiving sperm donation. They were more likely to admit to seeking pregnancy rather than sexual pleasure. In our study, many couples using sperm donation after failed intra-marital techniques had SD. It can be assumed that they already had a long history of infertility treatments before resorting to sperm donation. Moreover, some people wait for a long period of 9–12 months from registration to their first attempt.
We acknowledge that our study has some limitations. First of all, its monocentric design calls for caution when generalizing, and advocates for confirmation in other settings. The second limitation lies within the use of only one questionnaire per gender. Although the FSFI and the IIEF-15 appear to be the most relevant ones to help evaluating the prevalence of SD, especially using the IIEF-15, the psychological factors causing SD might be underestimated with these tools. Therefore, additional evaluation of mood and self-perception as well as anxiety and depressive symptoms should be considered for future studies. The fact that the study was completely anonymized made it impossible to relate the responses of the man and the woman from the same couple, preventing from performing dyadic analyses. In addition, the number of participants in this study was relatively low, and the numbers were actually insufficient to allow multivariate analysis and to have sufficient statistical power to identify predictive risk factors for SD. For instance, a larger number of participants would enable to evaluate the effect of age, of the type or duration of infertility, and the effect of the protocol (IUI-D versus IVF-D). It is unclear whether COVID-19 pandemic may have impacted results after March 2020 [38]. However, this is the first study to analyze SD in a population using sperm donation. Moreover, the participation rate was high, and therefore representative of our population and the scores used are scientifically validated [15,16,17,18,19]. Finally, the majority of couples underwent IUI-D, and too few couples underwent IVF-D to allow separate analysis.
Although this study was not designed to explain the psychological mechanisms involved in infertility-induced SD (as stated above), some hypotheses can be raised. Literature largely found that intimacy and sexuality appear impaired by intrusiveness of treatments. The discovery of infertility first causes a narcissistic wound in couples who have a desire for a child. The shift from a pleasant and spontaneous sexuality to a scheduled and procreative one contributes to SD. SD in infertile couples might be underdiagnosed and not enough taken into consideration, as doctors do not dare to discuss sexuality during consultations, either out of modesty or for fear of increasing suffering of patients by asking intrusive questions [14]. Additionally, the use of sperm donation triggers a psychological upheaval in patients, as giving up on biological parenthood can be a painful ordeal to overcome. Patients should be encouraged to express their feelings and share about the sexual problems they might encounter. In this context, a better collaboration between doctors and sexologists would help couples maintaining a better quality of sexual life and hopefully ultimately improve the quality of care and ART outcomes [39]. A couple-centered program for the integrated management of psychological and SD should be considered in the context of ART programs [40]. Doctors might be encouraged to propose self-questionnaires, such as the FertQol, designed to assess the quality of life of infertile patients during treatment with questions on sexuality. Further research should focus on the evaluation of psychological interventions (sex therapy, focus groups, etc.) to treat or improve these disorders.
Data availability
The data that support this paper are available from the corresponding author, upon reasonable request.
References
Rossin B (2019) How infertility can be a source of aggression. Sexologies. https://doi.org/10.1016/j.sexol.2018.12.001
Fisher JR, Hammarberg K (2012) Psychological and social aspects of infertility in men: an overview of the evidence and implications for psychologically informed clinical care and future research. Asian J Androl. https://doi.org/10.1038/aja.2011.72
Schneider MG, Forthofer MS (2005) Associations of Psychosocial Factors with the Stress of Infertility Treatment. Health Soc Work. https://doi.org/10.1093/hsw/30.3.183
Definition of sexual health. World Health Organization. http://www.euro.who.int/fr/health-topics/Life-stages/sexual-and-reproductive-health/news/news/2011/06/sexual-health-throughout-life/definition. Accessed 28 July 2022
Pirard C, (2010). Desire for children, sexual desire: when infertility and sexuality collide. Louvain med
Courbiere B, Lacan A, Grynberg M, Grelat A, Rio V, Arbo E et al (2020) Psychosocial and professional burden of Medically Assisted Reproduction (MAR): results from a French survey. Laganà AS, éditeur. PLOS One. https://doi.org/10.1371/journal.pone.0238945
Huyghe E, Bonal M, Daudin M, Droupy S (2013) Sexual dysfunctions and infertility. Prog Urol. https://doi.org/10.1016/j.purol.2013.02.004
Gannon K, Glover L, Abel P (2004) Masculinity, infertility, stigma and media reports. Soc Sci Med. https://doi.org/10.1016/j.socscimed.2004.01.015
Saleh RA, Ranga GM, Raina R, Nelson DR, Agarwal A (2003) Sexual dysfunction in men undergoing infertility evaluation: a cohort observational study. Fertil Steril. https://doi.org/10.1016/S0015-0282(02)04921-X
Smith JF, Walsh TJ, Shindel AW, Turek PJ, Wing H, Pasch L et al (2009) Sexual, marital, and social impact of a man’s perceived infertility diagnosis. J Sex Med. https://doi.org/10.1111/j.1743-6109.2009.01383.x
Lee T-Y, Sun G-H, Chao S-C (2001) The effect of an infertility diagnosis on the distress, marital and sexual satisfaction between husbands and wives in Taiwan. Hum Reprod. https://doi.org/10.1093/humrep/16.8.1762
Bechoua S, Hamamah S, Scalici E (2016) Male infertility: an obstacle to sexuality? Andrology. https://doi.org/10.1111/andr.12160
Berger DM (1980) Couple’s reactions to male infertility and donor insemination. Am J Psychiatry. https://doi.org/10.1176/ajp.137.9.1047
Reder F, Fernandez A, Ohl J (2009) Does sexuality still have a place for couples treated with assisted reproductive techniques? J Gynecol Obstet Reprod Biol. https://doi.org/10.1016/j.jgyn.2009.05.002
Rosen C, Brown J, Heiman S, Leiblum C, Meston R, Shabsigh D, Ferguson R, D’Agostino R (2011) The female sexual function index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther. https://doi.org/10.1080/009262300278597
Wylomanski S, Bouquin R, Philippe H-J, Poulin Y, Hanf M, Dréno B et al (2014) Psychometric properties of the French Female Sexual Function Index (FSFI). Qual Life Res. https://doi.org/10.1007/s11136-014-0652-5
Meston CM, Freihart BK, Handy AB, Kilimnik CD, Rosen RC (2020) Scoring and interpretation of the FSFI: what can be learned from 20 years of use? J Sex Med. https://doi.org/10.1016/j.jsxm.2019.10.007
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology. https://doi.org/10.1016/s0090-4295(97)00238-0
Cappelleri JC, Rosen RC, Smith MD, Mishra A, Osterloh IH (1999) Diagnostic evaluation of the erectile function domain of the International Index of Erectile Function. Urology. https://doi.org/10.1016/s0090-4295(99)00099-0
Millheiser LS, Helmer AE, Quintero RB, Westphal LM, Milki AA, Lathi RB (2010) Is infertility a risk factor for female sexual dysfunction? A case-control study. Fertil Steril. https://doi.org/10.1016/j.fertnstert.2010.01.037
Nelson CJ, Shindel AW, Naughton CK, Ohebshalom M, Mulhall JP (2008) Prevalence and predictors of sexual problems, relationship stress, and depression in female partners of infertile couples. J Sex Med. https://doi.org/10.1111/j.1743-6109.2008.00880.x
Yıkılmaz TN, Öztürk E, Hamidi N, Selvi İ, Başar H, Peşkircioğlu L (2020) Evaluation of sexual dysfunction prevalence in infertile men with non-obstructive azoospermia. Arch Ital Urol Androl. https://doi.org/10.4081/aiua.2019.4.241
Starc A, Trampuš M, Pavan Jukić D, Rotim C, Jukić T, Polona MA (2019) Infertility and sexual dysfunctions a systematic literature review. Acta Clin Croat. https://doi.org/10.20471/acc.2019.58.03.15
Lotti F, Corona G, Castellini G, Maseroli E, Fino MG, Cozzolino M et al (2016) Semen quality impairment is associated with sexual dysfunction according to its severity. Hum Reprod. https://doi.org/10.1093/humrep/dew246
Capogrosso P, Jensen CFS, Rastrelli G, Torremade J, Russo GI, Raheem AA et al (2021) Male sexual dysfunctions in the infertile couple-recommendations from the European society of sexual medicine (ESSM). Sex Med. https://doi.org/10.1016/j.esxm.2021.100377
Okobi OE (2021) A systemic review on the association between infertility and sexual dysfunction among women utilizing female sexual function index as a measuring tool. Cureus. https://doi.org/10.7759/cureus.16006
Gabr AA, Omran EF, Abdallah AA, Kotb MM, Farid EZ, Dieb AS et al (2017) Prevalence of sexual dysfunction in infertile versus fertile couples. Eur J Obstet Gynecol Reprod Biol. https://doi.org/10.1016/j.ejogrb.2017.08.025
Winkelman WD, Katz PP, Smith JF, Rowen TS (2016) The sexual impact of infertility among women seeking fertility care. Sex Med. https://doi.org/10.1016/j.esxm.2016.04.001
Keskin U, Coksuer H, Gungor S, Ercan CM, Karasahin KE, Baser I (2011) Differences in prevalence of sexual dysfunction between primary and secondary infertile women. Fertil Steril. https://doi.org/10.1016/j.fertnstert.2011.08.007
Marci R, Graziano A, Piva I, Lo Monte G, Soave I, Giugliano E et al (2012) Procreative sex in infertile couples: the decay of pleasure? Health Qual Life Outcomes. https://doi.org/10.1186/1477-7525-10-140
INED. (2007) First results of the CSF survey “Contexte de la sexualité en France”
Bayar U, Basaran M, Atasoy N, Kokturk F, Arikan II, Barut A et al (2014) Sexual dysfunction in infertile couples: evaluation and treatment of infertility. J Pak Med Assoc 64(2):138–145
Drosdzol A, Skrzypulec V (2009) Evaluation of marital and sexual interactions of Polish infertile couples. J Sex Med. https://doi.org/10.1111/j.1743-6109.2009.01355.x
Dong M, Xu X, Li Y, Wang Y, Jin Z, Tan J (2021) Impact of infertility duration on female sexual health. Reprod Biol Endocrinol. https://doi.org/10.1186/s12958-021-00837-7
Carter J, Applegarth L, Josephs L, Grill E, Baser RE, Rosenwaks Z (2011) A cross-sectional cohort study of infertile women awaiting oocyte donation: the emotional, sexual, and quality-of-life impact. Fertil Steril. https://doi.org/10.1016/j.fertnstert.2010.10.004
Indekeu A, D’Hooghe T, De Sutter P, Demyttenaere K, Vanderschueren D, Vanderschot B et al (2012) Parenthood motives, well-being and disclosure among men from couples ready to start treatment with intrauterine insemination using their own sperm or donor sperm. Hum Reprod. https://doi.org/10.1093/humrep/der366
Ohl J, Reder F, Fernandez A, Bettahar-Lebugle K, Rongières C, Nisand I (2009) Impact of infertility and assisted reproductive techniques on sexuality. Gynecol Obstet Fertil. https://doi.org/10.1016/j.gyobfe.2008.08.012
Nobre P, Rosa PJ, Vasconcelos P, Tavares I, Carvalho J, Quinta-Gomes A et al (2022) Sexual health and the pandemic crisis: testing the role of psychological vulnerability/protective factors on sexual functioning and sexual distress during a critical life period in Portugal. Arch Sex Behav. https://doi.org/10.1007/s10508-021-02209-z
Collier F (2010) When a couple wants a baby: what are the consequences on their sexuality? Sexologies. https://doi.org/10.1016/j.sexol.2010.03.002
Luca G, Parrettini S, Sansone A, Calafiore R, Jannini EA (2021) The Inferto-Sex Syndrome (ISS): sexual dysfunction in fertility care setting and assisted reproduction. J Endocrinol Invest. https://doi.org/10.1007/s40618-021-01581-w
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
JLG: study design, data collection, manuscript drafting. AR: study design, manuscript revision. SM: study design, manuscript revision. SD: study design, data collection. PB: study design, manuscript revision. TF: study design, data analysis, manuscript revision, study supervision, final validation of manuscript. TL: study design, data analysis, manuscript revision, study supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Le Goff, J., Reignier, A., Mirallie, S. et al. Sexual function in heterosexual couples undergoing assisted reproductive technology (ART) cycles with donor sperm. Arch Gynecol Obstet 307, 625–632 (2023). https://doi.org/10.1007/s00404-022-06877-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06877-7