Abstract
Purpose
The objective of the study is to evaluate the possible association between history of subfertility, fertility treatments, BRCA mutations and the risk of ovarian cancer.
Methods
This Israeli National Case–Control study included 1269 consecutive ovarian cancer cases and 2111 individually matched healthy controls. All participants were interviewed and molecular analysis of BRCA mutations were performed to 896 cases. The main outcome measure was reported history of subfertility and exposure to fertility treatments.
Results
The rate of reported subfertility was 15.1% and 14.3% in ovarian cancer cases and controls, respectively. However, subfertility was more prevalent in cases with borderline ovarian cancer (but not for invasive ovarian cancer cases) than controls. Multivariate conditional logistic regression revealed that the risk of borderline ovarian cancer was elevated in both women treated for subfertility and those that were not treated for subfertility, (OR = 1.74; 95% CI 0.9–3.36 and OR = 1.79; 95% CI 0.98–3.26, respectively). In non-carriers of BRCA1/2 mutations, fertility treatments were associated with a decreased risk of invasive ovarian cancer while a significant increased risk of borderline ovarian cancer was observed (OR = 2.92, 95%CI 1.67–5.10).
Conclusions
Reported subfertility and exposure to fertility treatments were associated with borderline but not with invasive ovarian tumors. This association was more prominent in women who are non-carriers of a BRCA mutation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ovarian cancer represents the sixth most common female cancer in western countries and is the most fatal gynecological malignancy, with 5-year survival rate of approximately 40% [1]. The use of fertility drugs and in vitro fertilization (IVF) is rising worldwide. In Israel, fertility drugs were introduced in 1964 and IVF treatments started in 1982 and are offered free of charge to all women up to the age of 45 for first and second child. For example, the number of IVF cycles that were performed in Israel in 2012 was over 39,000, which is an 80% increase as compared to 2000 [2]. In light of the increasing exposure to fertility treatments (both fertility drugs and IVF), probable sequelae should be investigated.
A number of identifiable factors have been associated with an increased risk of ovarian cancer, including: environmental factors [3], hormonal factors [4], and genetic factors [5]. In particular, the presence of BRCA1 and BRCA2 gene mutations were associated with increased risk for ovarian cancer [6].
A series of articles published by Whittemore et al [7] and Harris et al. [8] in 1992, led to renewed interest in the potential carcinogenic effects of infertility and ovulation inducing drugs. A 2.8 fold increase was observed [7] in the risk for invasive ovarian cancer, in women who were exposed to fertility drugs as compared to those who were not. However, case–control studies failed to repeat this finding for invasive ovarian cancer [9,10,11]. Several cohort studies addressed the same possible association; however, none were able to present an increased risk for invasive ovarian cancer in association with exposure to ovulation inducing drugs [12,13,14,15,16,17,18,19,20].
The incidence of borderline tumors of the ovary, was found to be elevated in women treated for infertility in several studies published thus far. Shushan et al. [9], in a case–control study, reported an excess risk in the subgroup of women with borderline tumors who had used any fertility drugs (OR = 3.52; 95% CI 1.23–10.09). A Pooled analysis of individual level data from population based case control studies, performed by Ness et al [11], on infertility and fertility drug use, also reported an excess risk of borderline tumors of the ovary in association to infertility and ovulation inducing drug exposure.
Kashyap et al. [21] critically evaluated seven case control and three cohort studies that were published between 1987 and 2000. In this meta-analysis, the results indicated that fertility drugs usage did not increase the risk for ovarian cancer both invasive and borderline. Similar findings were also evident in the recently published meta-analysis by Zhao et al [22].
The notion that BRCA may play a role in the relationship between infertility and Ovarian Cancer has recently been described [23,24,25,26]. Considering the frequency of BRCA mutations in Caucasian Ashkenazi population which is over 2% [27] and the high frequency of BRCA mutation in ovarian cancer patients in Israel [28, 29], the implication that BRCA has a possible role in the interaction between infertility and ovarian cancer, warrants further investigation.
The aim of this study was to evaluate the effect of reported history of subfertility and fertility treatments on the development of invasive and borderline ovarian cancer, while adjusting for other established risk factors.
Due to the role of BRCA mutations in ovarian aging and possibly subfertility, BRCA mutation status in association to subfertility among ovarian cancer cases (invasive and borderline), was also analyzed.
Methods
Study population
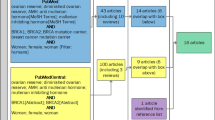
All Jewish women with pathologically confirmed cancer of the ovary (code 183.0 of the International Classification of Diseases, 9th Revision, Clinical Modification), or primary peritoneal carcinoma, possibly of ovarian origin (code 158), diagnosed in Israel between March 1, 1994, and June 30, 1999, were identified. To ensure that no patients with newly diagnosed cancer were overlooked, all the departments of gynecology in the country, were monitored continually throughout the study, and pathology and oncology departments were checked monthly. During the 5-year study period, 1226 Jewish women were diagnosed with invasive epithelial ovarian cancer (histological subtypes were as follow; serous (n = 567, 44.4%); endometrioid (n = 187, 14.7%), mucinous (n = 65, 5.1%); adenocarcinoma (n = 122, 9.6%); other epithelial (n = 67, 18.4%); clear cell carcinoma (n = 31, 2.4%)). Additional 263 women were diagnosed with borderline histological findings, indicating that the lesion had a low malignant potential. Of these 1489 women, 1269 (85.2%) were interviewed. For each patient, two control women who were matched for age (± 2 years), area of birth, and place and length of residence in Israel (according to defined categories) were selected from the Central Population Registry resulting in 3103 controls; 2111(68%) were contacted and interviewed. All living subjects gave written informed consent. The study protocol, was approved by the Institutional Review Board of Israel and the National Institutes of Health (NIH) review board in the United States of America.
Study instruments
The cases, were interviewed during hospitalization; usually 4 to 6 days after gynecologic surgery and the controls were interviewed at their homes using the same questionnaire. The accuracy and thoroughness of each of the interviewers, were periodically checked, to help ensure that the method of data collections was standardized.
The questionnaire included the following information: demographic and socioeconomic characteristics; smoking habits; family history of cancer; reproductive history including; subfertility; length of use of oral and other contraceptives; age at menarche, age at menopause, length of menstrual cycles, menstrual irregularities, number of pregnancies and births; age at first birth, use of hormone replacement therapy; gynecologic morbidity and procedures. Women were categorized as "infertile", if they answered positively to the question whether they "ever tried to conceive for more than a year". Women classified as "infertile" were further asked whether they received fertility drugs and \ or underwent IVF. In addition, other morbidities; weight at age 18 years, "most of adult life", and "recently" (before illness for cases and 1 year before interview for controls); and height at end of growth, were also reported.
BRCA mutation status
The original study [29] that was conducted between 1994 and 1999, aimed to examine environmental and genetic factors (using family history of cancer) for ovarian cancer. In 1996, when genetic test for BRCA1/2 mutation became available, a genetic component was added to the study, and blood samples were collected for cases recruited from 1996 onwards. These blood samples were analyzed for the founder mutations as follows:
Biological samples (either peripheral blood or paraffin-embedded tissue sections) were available for cases of ovarian cancer only. These samples were tested for BRCA1 (185delAG and 5382insC) and BRCA2 (6174delT) mutations, using genetic laboratory techniques that have been described previously [28]. Briefly, a multiplex polymerase chain reaction, was designed to amplify the exons containing the three mutations with the use of fluorescence-labeled primers in a single reaction. Since each mutation is a small insertion or deletion, it can be detected as a length polymorphism with the use of a genetic analyser (model 310, Applied Biosystems) and Genescan software (Applied Biosystems). These genetic tests, were carried out by the Laboratory of Population Genetics at the National Cancer Institute, Bethesda, MD, USA.
Statistical analysis
Univariable and multivariable conditional logistic regression models, were used to estimate the effect of subfertility with or without fertility treatments, on the risk of ovarian cancer in general and by tumor invasiveness (invasive and borderline tumors). Adjustments for well known risk / protective factors were employed. The controlling variables were: family history of breast / ovarian cancer, oral contraceptive use (women that reported the use of oral contraceptives for a period of less than 6 months were considered as no oral contraceptive use), parity, number of pregnancies, age at first birth, education, BMI and family status. Odds ratios (OR) and 95% confidence intervals (CI) associated with subfertility were estimated. In addition, the association between reported subfertility, fertility treatments and BRCA 1/2 mutations status, were assessed for cases of ovarian cancer only, by tumor invasiveness. In order to evaluate the effect of subfertility and fertility treatments on the risk of ovarian cancer according to BRCA mutation status, a multinomial unconditional logistic regression with all controls as the reference category and adjustment for the above covariates, was applied for the total group as well as by stratification according to tumor invasiveness.
All statistical analyses were performed using the SAS software version 9.1 (SAS institute, Inc, Cary, NC, USA).
Results
No differences were found between the cases and control groups in most of the socio-demographic characteristics (Table 1); 61.2% of the cases had up to 12 years of education, however, significantly more controls than cases had higher education of ≥ 16 years (19.3% vs 15.7%, p = 0.009). There were significant differences in family status between cases and controls (p < 0.001); more controls than cases were married (71.1% vs. 60.4% respectively), while more cases were single (7.7% versus 3.4% among controls).
Established risk factors for ovarian cancer; family history, obstetric characteristics and obesity were also analyzed. Our results indicate that family history of ovarian and/or breast cancer was significantly more prevalent in cases than controls (12.5% vs. 7.7%; OR = 1.67, 95% CI 1.31–2.12).
Use of Oral contraceptives was more common among controls (19.4% in controls vs. 15.7% in cases, P = 0.007). Oral contraceptive use, had a significant protective effect (OR = 0.73, 95% CI 0.58–0.91) for ovarian cancer development.
More cases than controls were never pregnant (10.0% vs. 4.5%). Ever being pregnant, had a protective effect compared with never being pregnant (OR = 0.33, 95% CI 0.24–0.45). Each additional pregnancy significantly reduced the risk for ovarian cancer by 6% (95% CI 0.92–0.97). More cases than controls never gave birth (13.0% vs. 6.6%) and each additional birth significantly reduced the risk for ovarian cancer by 12% (95% CI 0.84–0.92).
The majority of cases and controls were < 30 years old at first birth. Both categories of age (< 30 and ≥ 30 years) at first birth, exhibit a significant protective effect compared to nulliparity (OR = 0.42, 95% CI 0.32–0.54 and OR = 0.37. 95% CI 0.26–0.52, respectively).
BMI of ≥ 30 at most adult life as compared to < 30, was significantly associated with increased risk for ovarian cancer (OR = 1.37, 95% CI 1.10–1.70). Similar associations were also observed, when the cases were stratified by tumor invasiveness to invasive ovarian cancer cases and borderline ovarian cancer cases (supplemental Table 1).
Subfertility was more prevalent in cases than in controls (15.1% versus 14.3%), although not significantly for total ovarian cancer cases. However, this association was significant and more prominent in the borderline ovarian cancer cases (OR = 1.68, 95% CI 1.09–2.60).
Fertility treatments (Table 2) were reported by 7.6% of all cases and 6.3% of the controls; in patients with borderline tumors, the difference was more prominent (13.7% versus 8.0%). In borderline ovarian cancer cases, but not in invasive ovarian cancer cases, an indication for increased risk associated with subfertility treatments was observed (OR = 1.69, 95% CI 0.97–2.95 and OR = 1.03, 95% CI 0.73–1.45, respectively).
There were no women that reported exposure to fertility treatments without reporting subfertility, and 7.5% of the women, reported subfertility without receiving any fertility treatments. In addition, IVF treatments were reported by 33 participants (19 cases and 14 controls). The mean number of IVF cycles was 4.0 with no statistical differences between cases and controls.
Table 3 presents multivariable models for the risk for ovarian cancer, associated with subfertility and adjusted for other known risk factors for ovarian cancer. While the risk associated with subfertility and fertility treatments completely diminished for invasive ovarian cancer cases, the risk associated with borderline ovarian cancer, remained elevated for both treated and untreated infertile women (Adjusted OR = 1.79, 95% CI 0.98–3.26 and Adjusted OR = 1.74, 95% CI 0.90–3.36, respectively). A negative association between education and invasive ovarian cancer, but not borderline ovarian cancer, was observed. Oral contraceptive use showed a protective effect for both invasive and borderline ovarian cancer development (although only significant in borderline cases). Positive 1st degree family history of breast and\ or ovarian cancer, was found to be a risk factor for both (only significant for invasive ovarian cancer cases).
Molecular analysis for founder mutations in BRCA1/2, was completed successfully in 896 of the 1269 women with epithelial ovarian cancer (779 cases with invasive cancer and 117 with borderline ovarian cancer (Table 4). Of these, 234 women (26.1%) were positive for BRCA mutations (29.4% and 4.3% among women with invasive and borderline ovarian cancer, respectively). 176 women were carriers of BRCA1 mutation and 78 were carriers of BRCA2 mutation.
In women who reported subfertility, 21.0% were positive for BRCA mutations as compared to 27.0% among those who did not report subfertility (p = 0.14). The risk for subfertility was lower among cases that tested positive for either any BRCA mutation or BRCA1 or BRCA2 controlling for age (OR = 0.71, 95% CI 0.46–1.10, p = 0.13, OR = 0.96, 95% CI 0.60–1.51, p = 0.8 and OR = 0.45, 95% CI 0.19–1.06, p = 0.07; respectively) (not shown). The higher frequency of BRCA mutation carriers in subfertile women, was evident in women who developed invasive ovarian cancer, but not in those who were diagnosed with borderline tumors (27.2% versus 2.9%); 18.6% versus 0 for untreated subfertility in invasive versus borderline and 38.6% versus 4.8% for treated subfertility. Ovarian cancer cases that reported subfertility without fertility treatments had significantly less BRCA mutations (15.1% versus 27.1%; p = 0.03). This difference, is mainly attributed to the invasive ovarian cancer group.
Table 5 presents the effect of subfertility and fertility treatments on the risk of ovarian cancer by mutation status. Women carriers of a BRCA1/2 mutation and ovarian cancer patients' non-carriers of BRCA1/2 mutations, were compared with the entire control group. Although fertility treatments were associated with a decreased risk, in women diagnosed with invasive ovarian cancer non-carriers of a BRCA1/2 mutation (OR = 0.69, 95% CI 0.43–1.10); a significant increase in risk was observed among non-carriers with borderline cancer (OR = 2.92, 95% CI 1.67–5.10).
Discussion
Infertility and nulliparity are known risk factors for epithelial ovarian cancer [4]. The present study supports these findings, as cases with ovarian cancer were more likely to have no pregnancies or births, to have their first birth over the age of 30 and to report more infertility than healthy controls. Other known risk factors for ovarian cancer such as family history of breast and/or ovarian cancer were also confirmed in this study. The differentiation between the effect of infertility per se and the possible effect of fertility treatments on ovarian cancer development is not trivial.
The possible link between exposure to fertility treatments and ovarian cancer development has biological credibility and is aligned with the "incessant ovulation" [30] and "gonadotropin" hypotheses [31]. The association between infertility, fertility treatments and invasive ovarian cancer development, was investigated in numerous case–control [8,9,10,11] and cohort studies [12,13,14,15,16,17,18,19,20, 32,33,34,35,36]. Most case–control studies observed excess risk in infertile women that did not receive hormonal treatments. With the exception of one case–control study [7], all other studies, failed to demonstrate a significant excess risk of invasive ovarian cancer following fertility treatments.
In addition, numerous cohort studies have compared ovarian cancer rates in infertile women with those of the general population. Although cohort sizes were sufficient, most studies failed to present a significant association between exposure to infertility and fertility treatments and invasive ovarian cancer development. Nevertheless, Tworoger et al. [36] observed a significant excess risk for ovarian cancer development in women with female factor infertility. The potential limitations of most of these cohort studies are the small number of ovarian cancer cases, as well as lack of information regarding significant confounding factors. Some of the cohort studies [21] included an internal comparison between infertile women who were treated with fertility treatments and those who were not, with similar results. Recent publications failed to observe an increased risk for invasive ovarian cancer [21, 32, 33].
In the present study, approximately 30% of women with invasive ovarian cancer were found to be BRCA positive. However, infertile women as compared to fertile, were less likely to be BRCA positive (although not significantly). In a cohort study that followed over 2500 Israeli infertile women, 12 women developed invasive ovarian cancer, none of which was positive for BRCA mutations [26]. Recently, Perri et al [23] investigated whether BRCA mutation carriers who undergo fertility treatment are at increased risk of developing invasive ovarian cancer and found that fertility treatments were not associated with invasive ovarian cancer risk. Similar findings were also observed by Grownwald et al [25]. In light of information regarding the possible association of BRCA1 mutations with occult primary ovarian insufficiency [24]. a recent review [37], assessed the role of BRCA mutations and ovarian aging. BRCA and especially BRCA1 function in DNA repair is decreasing with age in the human oocytes. Therefore, women with BRCA 1 mutations might have lower ovarian reserves and experience earlier menopause, leading to infertility. Moreover, Ponce at al [38] measured the levels of anti-Mullerian hormone (as a proxy for infertility) in BRCA carriers. Women that were positive for BRCA 2 had lower levels of anti-Mullerian hormone and higher probability of infertility (although not statistically significant) as compared to BRCA1 carriers and BRCA mutation-negative women.
Due to the controversy regarding the role of BRCA mutation and ovarian function, larger studies regarding the association between types of infertility, BRCA and subsequent development of ovarian cancer, should be conducted.
In our study, while the association between subfertility and invasive ovarian cancer was not observed, cases with borderline tumors reported significantly more subfertility (adjusted OR = 1.76, 95% CI 1.10–2.82). The risk for borderline tumors of the ovary in infertile women was found to be significantly increased in both case control [8, 9, 11] and cohort studies [13, 33,34,35, 39], with magnitude ranging from 1.76 to 4.00, for various fertility treatments.
Borderline tumors of the ovary present a unique entity of ovarian malignancy with less family history, less detection of BRCA mutations, higher incidence of estrogen receptors, younger age at diagnosis and significantly higher 5 years survival rates [40,41,42], as compared to invasive ovarian cancer. Therefore, the different role of subfertility in borderline tumors may also support the distinct etiology of these tumors. Since borderline tumors of the ovary may be diagnosed due to surveillance, especially in women exposed to fertility treatments (which requires repeated ultrasonographic examinations), the association between subfertility and borderline tumors may represent surveillance bias.
Being a BRCA carrier was not significantly associated with borderline tumor development and women with borderline tumors had much lower rates of BRCA positive tests (4.3%). However, women with subfertility that were treated, were tested positive for BRCA, at higher rate than women with no reported subfertility, although this finding was not significant.
One of the strengths of our study is that in Israel, infertility treatments, are covered by the national health insurance law, for first and second child to every woman under the age of 45 years. As a result, our study population was non-selective. Nevertheless, Israel's relatively small population, limited the number ovarian cancer cases and especially borderline tumors that could be investigated. Due to the case–control design of the present study, information regarding subfertility and fertility treatments (including type and dose) was obtained, only by self-reporting from the women and therefore, may be incomplete and/or subjected to recall bias. However, women reported both subfertility problems and use of fertility treatments, therefore representing better validity of the information. Unfortunately, specific data regarding doses of IVF treatments was not available. In addition, the present study that investigated a representative unselected population, attempted to evaluate the role of BRCA mutation status, in association to subfertility and fertility treatments and ovarian cancer, a topic that only very limited number of studies addressed. Moreover, the present study investigated subfertility in women that were already diagnosed with either invasive ovarian cancer or borderline ovarian tumors, with association to their BRCA mutation status, while other publications reported the association of subfertility and BRCA mutation, regardless of ovarian cancer morbidity.
Conclusions
Results regarding the possible association of subfertility, fertility treatments and invasive ovarian cancer, as observed in the present study, show no increased risk and therefore, support previous reassuring publications.
Different risk factors, were found to be associated with invasive ovarian cancer and borderline tumors. In light of the possible association between subfertility and borderline ovarian tumors, but not invasive ovarian cancers, which has also been reported by others, further consideration needs to be given to the distinction between these two types of tumors in terms of hormonal exposures, both intrinsic (types of infertility) and extrinsic (types and dose of fertility treatments). Further studies targeted to borderline tumors of the ovary, are needed to support this finding.
Availability of data and materials
The dataset generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Sopik V, Iqbal J, Rosen B, Narod SA (2015) Why have ovarian cancer mortality rates declined? Part II. Case-fatality. Gynecol Oncol. https://doi.org/10.1016/j.ygyno.2015.06.016 (Published online)
Health in Israel 2010 (2010) http://www.health.gov.il/PublicationsFiles/Health_Status_in_Israel2010.pdf. Accessed 1 Oct 2021
Parazzini F, Franceschi S, La Vecchia C, Fasoli M (1991) The epidemiology of ovarian cancer. Gynecol Oncol 43(1):9–23
McGowan L, Norris HJ, Hartge P, Hoover R, Lesher L (1988) Risk factors in ovarian cancer. Eur J Gynaecol Oncol 9(3):195–199
Lynch HT, Casey MJ, Shaw TG, Lynch JF (1998) Hereditary factors in gynecologic cancer. Oncologist 3(5):319–338
Easton DF, Bishop DT, Ford D, Crockford GP (1993) Genetic linkage analysis in familial breast and ovarian cancer: results from 214 families. The Breast Cancer Linkage Consortium. Am J Hum Genet 52(4):678–701
Whittemore AS, Harris R, Itnyre J (1992) Characteristics relating to ovarian cancer risk: collaborative analysis of 12 US case-control studies. II. Invasive epithelial ovarian cancers in white women. Collaborative Ovarian Cancer Group. Am J Epidemiol 136(10):1184–1203
Harris R, Whittemore AS, Itnyre J (1992) Characteristics relating to ovarian cancer risk: collaborative analysis of 12 US case-control studies. III. Epithelial tumors of low malignant potential in white women. Collaborative Ovarian Cancer Group. Am J Epidemiol 136(10):1204–1211
Shushan A, Paltiel O, Iscovich J, Elchalal U, Peretz T, Schenker JG (1996) Human menopausal gonadotropin and the risk of epithelial ovarian cancer. Fertil Steril 65(1):13–18
Parazzini F, Pelucchi C, Negri E et al (2001) Use of fertility drugs and risk of ovarian cancer. Hum Reprod 16(7):1372–1375
Ness RB, Cramer DW, Goodman MT et al (2002) Infertility, fertility drugs, and ovarian cancer: a pooled analysis of case-control studies. Am J Epidemiol 155(3):217–224. https://doi.org/10.1093/aje/155.3.217
Modan B, Ron E, Lerner-Geva L et al (1998) Cancer incidence in a cohort of infertile women. Am J Epidemiol 147(11):1038–1042
Rossing MA, Daling JR, Weiss NS, Moore DE, Self SG (1994) Ovarian tumors in a cohort of infertile women. N Engl J Med 331(12):771–776. https://doi.org/10.1056/NEJM199409223311204
Venn A, Watson L, Lumley J, Giles G, King C, Healy D (1995) Breast and ovarian cancer incidence after infertility and in vitro fertilisation. Lancet 346(8981):995–1000
Venn A, Watson L, Bruinsma F, Giles G, Healy D (1999) Risk of cancer after use of fertility drugs with in-vitro fertilisation. Lancet 354(9190):1586–1590. https://doi.org/10.1016/S0140-6736(99)05203-4
Potashnik G, Lerner-Geva L, Genkin L, Chetrit A, Lunenfeld E, Porath A (1999) Fertility drugs and the risk of breast and ovarian cancers: results of a long-term follow-up study. Fertil Steril 71(5):853–859. https://doi.org/10.1016/S0015-0282(99)00085-0
Doyle P, Maconochie N, Beral V, Swerdlow AJ, Tan SL (2002) Cancer incidence following treatment for infertility at a clinic in the UK. Hum Reprod 17(8):2209–2213
Dor J, Lerner-Geva L, Rabinovici J et al (2002) Cancer incidence in a cohort of infertile women who underwent in vitro fertilization. Fertil Steril 77(2):324–327. https://doi.org/10.1016/S0015-0282(01)02986-7
Lerner-Geva L, Geva E, Lessing JB, Chetrit A, Modan B, Amit A (2003) The possible association between in vitro fertilization treatments and cancer development. Int J Gynecol Cancer 13(1):23–27
Brinton LA, Lamb EJ, Moghissi KS et al (2004) Ovarian cancer risk associated with varying causes of infertility. Fertil Steril 82(2):405–414. https://doi.org/10.1016/j.fertnstert.2004.02.109
Kashyap S, Moher D, Fung MF, Rosenwaks Z (2004) Assisted reproductive technology and the incidence of ovarian cancer: a meta-analysis. Obstet Gynecol 103(4):785–794. https://doi.org/10.1097/01.AOG.0000119226.39514.1d
Zhao J, Li Y, Zhang Q, Wang Y (2015) RETRACTED: Does ovarian stimulation for IVF increase gynaecological cancer risk? A systematic review and meta-analysis. Reprod Biomed Online 31(1):20–29. https://doi.org/10.1016/j.rbmo.2015.03.008
Perri T, Lifshitz D, Sadetzki S et al (2015) Fertility treatments and invasive epithelial ovarian cancer risk in Jewish Israeli BRCA1 or BRCA2 mutation carriers. Fertil Steril 103(5):1305–1312. https://doi.org/10.1016/j.fertnstert.2015.02.011
Oktay K, Kim JY, Barad D, Babayev SN (2010) Association of BRCA1 mutations with occult primary ovarian insufficiency: a possible explanation for the link between infertility and breast/ovarian cancer risks. J Clin Oncol 28(2):240–244. https://doi.org/10.1200/JCO.2009.24.2057
Gronwald J, Glass K, Rosen B et al (2016) Treatment of infertility does not increase the risk of ovarian cancer among women with a BRCA1 or BRCA2 mutation. Fertil Steril 105(3):781–785. https://doi.org/10.1016/j.fertnstert.2015.11.034
Menczer J, Lerner-Geva L, Sade-Bruchim RB, Friedman E (1999) Lack of the predominant BRCA1 and BRCA2 mutations in Jewish ovarian carcinoma patients who previously underwent ovulation induction. Eur J Gynaecol Oncol 20(5–6):371–372
Struewing JP, Hartge P, Wacholder S et al (1997) The risk of cancer associated with specific mutations of BRCA1 and BRCA2 among Ashkenazi Jews. N Engl J Med 336(20):1401–1408. https://doi.org/10.1056/NEJM199705153362001
Modan B, Gak E, Sade-Bruchim RB et al (1996) High frequency of BRCA1 185delAG mutation in ovarian cancer in Israel. National Israel Study of Ovarian Cancer. JAMA 276(22):1823–1825
Modan B, Hartge P, Hirsh-Yechezkel G et al (2001) Parity, oral contraceptives, and the risk of ovarian cancer among carriers and noncarriers of a BRCA1 or BRCA2 mutation. N Engl J Med 345(4):235–240. https://doi.org/10.1056/NEJM200107263450401
Fathalla MF (1971) Incessant ovulation—a factor in ovarian neoplasia? Lancet 2(7716):163. https://doi.org/10.1016/S0140-6736(71)92335-X
Casagrande JT, Louie EW, Pike MC, Roy S, Ross RK, Henderson BE (1979) “Incessant ovulation” and ovarian cancer. Lancet 2(8135):170–173. https://doi.org/10.1016/S0140-6736(79)91435-1
Calderon-Margalit R, Friedlander Y, Yanetz R et al (2009) Cancer Risk After Exposure to Treatments for Ovulation Induction. Am J Epidemiol 169(3):365–375. https://doi.org/10.1093/aje/kwn318
Sanner K, Conner P, Bergfeldt K et al (2009) Ovarian epithelial neoplasia after hormonal infertility treatment: long-term follow-up of a historical cohort in Sweden. Fertil Steril 91(4):1152–1158. https://doi.org/10.1016/j.fertnstert.2008.01.073
van Leeuwen FE, Klip H, Mooij TM et al (2011) Risk of borderline and invasive ovarian tumours after ovarian stimulation for in vitro fertilization in a large Dutch cohort. Hum Reprod 26(12):3456–3465. https://doi.org/10.1093/humrep/der322
Yli-Kuha A-N, Gissler M, Klemetti R, Luoto R, Hemminki E (2012) Cancer morbidity in a cohort of 9175 Finnish women treated for infertility. Hum Reprod 27(4):1149–1155. https://doi.org/10.1093/humrep/des031
Tworoger SS, Fairfield KM, Colditz GA, Rosner BA, Hankinson SE (2007) Association of oral contraceptive use, other contraceptive methods, and infertility with ovarian cancer risk. Am J Epidemiol 166(8):894–901
Turan V, Oktay K (2020) BRCA-related ATM-mediated DNA double-strand break repair and ovarian aging. Hum Reprod Update 26(1):43–57. https://doi.org/10.1093/humupd/dmz043
Ponce J, Fernandez-Gonzalez S, Calvo I et al (2020) Assessment of ovarian reserve and reproductive outcomes in BRCA1 or BRCA2 mutation carriers. Int J Gynecol Cancer 30(1):83–88. https://doi.org/10.1136/ijgc-2019-000626
Bjornholt SM, Kjaer SK, Nielsen TS, Jensen A (2015) Risk for borderline ovarian tumours after exposure to fertility drugs: results of a population-based cohort study. Hum Reprod 30(1):222–231. https://doi.org/10.1093/humrep/deu297
Hirsh-Yechezkel G, Chetrit A, Lubin F et al (2003) Population attributes affecting the prevalence of BRCA mutation carriers in epithelial ovarian cancer cases in Israel. Gynecol Oncol 89(3):494–498. https://doi.org/10.1016/S0090-8258(03)00152-5
Gotlieb WH, Chetrit A, Menczer J, Hirsh-Yechezkel G, Lubin F, Friedman E, Modan B, Ben-Baruch G (2005) Demographic and genetic characteristics of patients with borderline ovarian tumors as compared to early stage invasive ovarian cancer. Gynecol Oncol 97(3):780–783. https://doi.org/10.1016/j.ygyno.2005.02.022
Ben David Y, Chetrit A, Hirsh-Yechezkel G, Friedman E, Beck BD, Beller U, Ben-Baruch G, Fishman A, Levavi H, Lubin F, Menczer J, Piura B, Struewing JP, Modan B (2002) Effect of BRCA mutations on the length of survival in epithelial ovarian tumors. J Clin Oncol 20(2):463–466. https://doi.org/10.1200/JCO.2002.20.2.463
Funding
Funded in part by Grant CA 61126-03 from the National Cancer Institute, National Institutes of Helath, Bethesda, MD, USA and NCI R01CA061126-03 (PI Prof. Modan).
Author information
Authors and Affiliations
Consortia
Contributions
LLG was responsible for conception and design of the study, interpetation of data, writing draft of manuscript and review the final draft. AC was responsible for conception and design of the study, conducted the statistical analysis, interpetation of data and review the final draft. AF was responsible for interpetation of data and review the final draft. FL was responsible for conception and design of the study and review the final draft. SS responsible for conception and design of the study, interpetation of data and review the final draft.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no competing interests.
Ethical approval
The study was approved by Sheba Medical Center Institutional Review Board #1298 date:30 October 2014.
Consent for publication
Since not individual details are part of the manuscript the consent is not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Nationall Israeli Study of Ovarian Cancer
The members of the National Israeli Study of Ovarian Cancer are:Shmuel Anderman, MD; Marco Altaras, MD; Shaul Anteby, MD; Jack Atad, MD; Amiram Avni, MD; Amiran Bar-Am, MD; Dan Beck, MD; Uzi Beller, MD; Gilad Ben-Baruch, MD; Yehuda Ben-David, MD; Haim Biran, MD; Moshe Ben Ami, MD; Angela Chetrit, MSc; Shulamit Cohan, MD; Ram Dgani MD; Yehudit Fishler, CTR; Ami Fishman, MD; Eitan Friedman, MD; Ofer Gemer, MD; Ruth Gershoni, MD; Walter Gottlieb, MD; Reuvit Halperin, MD; Galit Hirsh-Yechezkel, PhD; David Idelman, MD; Rafael Katan, MD; Yuri Kopilovic, MD; Efrat Lahad, MD; Liat Lerner Geva, MD; Hanoch Levavi, MD; Albert Levit, MD; Tally Levy, MD; Beatriz Lifschiz-Mercer, MD; Flora Lubin, MSc, RD; Zohar Liviatan, MD; Jacob Markovich, MD (deceased); Joseph Menzcer, MD; Baruch Modan, MD (Chairman, deceased); Hedva Nitzan, RN, MPH; Moshe Oettinger, MD; Tamar Peretz, MD; Benjamin Piura, MD; Shulamit Rizel, MD; Siegal Sadetzki, MD; Adi Shani, MD; David Schneider, MD; Michael Shtark, MD; Mariana Shteiner, MD; Zion Tal, MD; Chaim Yaffe, MD; Ilana Yanai, MD; Shifra Zohar, MD; and Ahuva Zoltan, RN, BA.
Rights and permissions
About this article
Cite this article
Lerner-Geva, L., Chetrit, A., Farhi, A. et al. Subfertility, use of fertility treatments and BRCA mutation status and the risk of ovarian cancer. Arch Gynecol Obstet 306, 209–217 (2022). https://doi.org/10.1007/s00404-021-06355-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06355-6