Abstract
Purpose
Bariatric surgery is widely known to improve pregnancy outcomes and to increase the risk of having small for gestational age neonates. However, the specific causes of neonatal growth restriction are still unclear. This study aimed to investigate the impacts of bariatric surgery on pregnancy and perinatal status at a single institution.
Methods
24 women delivered singleton births among the 193 reproductive-aged women who underwent bariatric surgery. We classified the surgery into three types: laparoscopic adjustable gastric banding (LAGB; n = 6), laparoscopic sleeve gastrectomy (LSG; n = 5), and malabsorptive surgery (MS; n = 13), and investigated the pregnancy complications and perinatal impacts.
Results
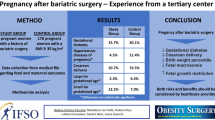
The median maternal weight gain after LAGB was 12.5 kg (LSG 6.9 kg, MS 9.0 kg). Gestational hypertension was observed in half of the women who underwent LAGB, but in none of those who underwent MS. No significant difference in neonatal birth weight was observed between the LAGB (median 3272 g) and LSG (median 3005 g) groups. The maternal impact after MS was a remarkable decrease in hemoglobin during prepregnancy (median 1.9 g/dl). About 69% of women developed gestational anemia after MS, and their neonatal birth weight was the lowest (median 2660 g). However, the birth weight of neonates delivered by mothers without anemia after undergoing MS was similar to that of those delivered by mothers after undergoing other types of bariatric surgery (median 3037 g).
Conclusions
Maternal anemia after MS may lead to low neonatal birth weight, which could be attributed to the large-scale reduction in maternal micronutrient levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obesity has been widely known as one of the major factors associated with infertility in reproductive-aged women [1]. Furthermore, maternal obesity is a risk factor for gestational diabetes, hypertension, or preeclampsia, increasing the risk of delivery complications, stillbirth, preterm birth, neonatal macrosomia, and some congenital malformations [2,3,4,5].
According to the published reports, bariatric surgery has been commonly used as a weight loss method associated with long-term metabolic remission [6]. Therefore, the American College of Obstetrics and Gynecology recommends losing weight prior to conception and acknowledges bariatric surgery as promising in prepregnancy obesity treatment [7]. However, some reports recently presented the risk of having small neonates, preterm birth, and maternal anemia after bariatric surgery [8, 9]. Furthermore, Swedish studies reported similar perinatal outcomes after bariatric surgery in a large population [10, 11]. Although the Swedish studies were clinically significant for bariatric surgeons and obstetricians, there was a bias in the type of surgical procedure, of which 98% were gastric bypasses [11]. However, there are several types of bariatric procedures performed worldwide [12], necessitating the need to evaluate the different maternal impacts and pregnancy outcomes of each procedure. This retrospective study aimed to investigate the pregnancy impacts and perinatal outcomes according to the surgical procedure at a single institution.
Materials and methods
This is a single-center retrospective case–control study investigating 24 women who gave singleton births among the 193 reproductive-aged women after undergoing four procedures [laparoscopic adjustable gastric banding (LAGB), laparoscopic sleeve gastrectomy (LSG), laparoscopic Roux-en-Y gastric bypass (LRYGB), and LSG with duodenojejunal bypass (LSG/DJB)] from October 2005 to October 2014. All singleton pregnancies during the postoperative period were reported, and questionnaire surveys regarding the physical data of mothers and neonates as well as complications in terms of the pregnancy and delivery among 33 singleton pregnancies were obtained from the mothers, who provided informed consent for this study.
For the evaluation of the pregnancy impacts depending on the surgical procedure, we extracted data from only 24 pregnancies, which was the first pregnancy in mothers among 33 singleton births, and divided the patients according to the type of surgery they underwent [LAGB; LSG; and malabsorptive surgery (MS), including LRYGB and LSG/DJB] and compared the difference in weight loss, remission of metabolic comorbidities in the postoperative period, complications of pregnancy and delivery, and neonatal birth weight.
In addition, we also investigated the maternal hemoglobin and serum iron levels for all types of surgery during prepregnancy as well as the relationship between the neonatal birth weight and maternal anemia.
Anemia definition
Anemia was defined using the age- and gender-specific World Health Organization criteria (hemoglobin < 12 g/dl in adult women and 11 g/dl during pregnancy).
Gestational diabetes mellitus definition
The women were diagnosed to have overt diabetes during pregnancy when their glycosylated hemoglobin is ≥ 6.5% [13].
Gestational hypertension definition
Gestational hypertension was defined as systolic blood pressure over 140 mmHg or diastolic blood pressure over 90 mmHg during pregnancy.
Patients and treatment
We recommended that all patients regularly take supplements (iron, zinc, vitamins, folate, calcium, etc.) after all types of surgery and strictly ordered the patients who underwent MS to continue taking supplementations indefinitely. We asked the reproductive-aged women to avoid pregnancy for 18 months and consult us with regard to the appropriate time for conceiving should they wish to get pregnant after surgery. When patients reported pregnancy after LAGB, they were asked to visit our center to completely loosen the tight banding to prevent dehydration and nutritional deficiencies, and no additional adjustment was performed during pregnancy unless the patients requested re-tightening.
Micronutrient supplementation
Based on the standard minimum daily requirement for Japanese women, our recommended supplementations included elementary iron (12 mg), folic acid (200–400 µg), and vitamin B12 (1000 µg). In case of nutritional deficiencies, we usually prescribe the appropriate supplementation for treatment.
Statistical analysis
Descriptive results regarding continuous variables were reported as the median and interquartile range (IQR) and were analyzed using the Kruskal–Wallis and Steel–Dwass tests. All tests were two-sided and a p value of < 0.05 indicated a statistically significant difference.
Results
The number of women who underwent LAGB was 6, LSG 5, and MS 13, with their characteristics being described in Table 1. The physical findings at the preoperative stage among the three groups were similar, except for age. The median % total weight loss (TWL) was, respectively, 7.8% (IQR 7.0–23.6) for LAGB, 30.0% (IQR 29.4–35.9) for LSG, and 36.0% (IQR 32.6–39.0) for MS, with significant differences in %TWL and postoperative body mass index (BMI) between LAGB and the other procedures.
Preoperative comorbidities and complete remission during prepregnancy are described in Table 2. Type 2 diabetes mellitus and hypertension were completely controlled during prepregnancy in women who underwent MS. However, hypertension was completely resolved in only approximately half of the women after LAGB and LSG.
Maternal weight changes and complications among 24 pregnancies are described in Table 3. The weight gain (median 12.5 kg, IQR 9.8–20.5) and maximum body weight (median 98 kg, IQR 91.5–106) during pregnancy in patients who underwent LAGB was significantly different compared with that in patients who underwent LSG (weight gain, median 6.9 kg; maximum body weight, median 68.9 kg) and MS (weight gain, median 9.0 kg; maximum body weight, median 73.5 kg). However, no difference was observed between the LSG and MS groups.
The most frequent pregnancy complication, especially after undergoing MS, was anemia (69%), and two patients were diagnosed with severe anemia during pregnancy (hemoglobin levels under 8.0 g/dl). Except for one patient who only had mild anemia, the patients had been continuously taking iron supplements including vitamins and minerals after surgery. Gestational diabetes mellitus was not observed in patients who underwent MS. However, two patients who underwent LSG, of whom none had type 2 diabetes mellitus during the preoperative period, had progressed to gestational diabetes mellitus, and one patient was treated for impaired glucose tolerance after delivery. HELLP (hemolysis, elevated liver enzymes, lowered platelets) syndrome was noted in only one patient who underwent LAGB but did not have hypertension during prepregnancy. Gestational hypertension was observed in half of the patients who underwent LAGB, of whom two were in complete remission without any treatment during prepregnancy.
The median neonatal birth weight was, respectively, 3272 g (IQR 3028–3539) in LAGB, 3005 g (IQR 2966–3174) in LSG, and 2664 g (IQR 2640–3024) in MS, and a significant difference in neonatal birth weight was noted only between LAGB and MS (Table 4). The rate of emergency cesarean section due to non-reassuring neonatal status was not so different among three types of surgery. There were no preterm births after any of the surgical procedures.
As described in Table 3, the most frequent pregnancy complication especially in patients who underwent MS was anemia (69%). Table 5 presents the analysis of serum iron and hemoglobin levels during the preoperative and prepregnancy period of all types of surgery. Although the hemoglobin and serum iron level immediately before surgery were similar among the three groups, a significant decrease in hemoglobin (median 1.9 g/dl) and low serum iron (median 38.5 mg/dl) were recognized in patients who underwent MS, and their median hemoglobin level during prepregnancy was the lowest among the three types of surgery. The differences in hemoglobin levels and neonatal birth weights in patients who underwent MS with or without maternal anemia are shown in Table 6. Hemoglobin (median 11.3 g/dl, IQR 10.9–12.0) and serum iron (median 33 mg/dl, IQR 29–39) levels in patients with anemia immediately before pregnancy were lower than those in patients without anemia. Moreover, although there was no significant difference in gestational period in patients with or without maternal anemia, the neonatal birth weight in patients with maternal anemia (median 2660 g, IQR 2640–2868) was relatively lower than that in patients without maternal anemia (median 3,037 g, IQR 2,914–3,082) and was suggested to be the lowest among all neonates.
Discussion
The important findings in our analysis indicate distinct maternal features depending on the surgical procedure performed.
In our study, the maternal weight and weight gain during pregnancy of patients who underwent LAGB were the highest among the three types of surgery. According to the 2009 guideline from the Institute of Medicine of National Academies, women whose BMI was over 30 kg/m2 were recommended to have a restriction of 5.0–9.1 kg from the baseline weight during pregnancy for neonatal birth weight control [14]. In Japan, a weight gain of 5–7 kg during pregnancy was also recommended by the Japan Society for the Study of Obesity and Japan Society of Obstetrics and Gynecology to prevent pregnancy and delivery complications in obese women. Although the evidence supporting these weight control guidelines remains insufficient, the maternal weight gain after LAGB was certainly beyond these ranges in our series. Does consistent band adjustment influence poor weight control during pregnancy? Should the band be completely loosened or not? Jeffrey et al. [15] state in the American Society for Metabolic and Bariatric Surgery (ASMBS) recommendations that patients who become pregnant should have band adjustment as necessary for appropriate weight gain to support neonatal growth. Carelli et al. showed that patients who had never had their band adjusted during pregnancy had an average weight gain of 10.6 kg, whereas patients whose band was fully deflated had an average weight gain of 14.1 kg. However, there were no differences between their study and the national statistics in terms of the rate of low or very low birth weight neonates (average 3268 g vs. 3298 g) [16]. Skull et al. [17] also reported that 49 pregnant patients who underwent LAGB and had their band adjusted had a significantly less weight gain compared with those who underwent non-LAGB surgery (3.7 kg vs. 15.6 kg), but their neonatal birth weight was not statistically different (3310 g vs. 3530 g). In our study, one of six patients had delivered with the band kept tight and her predelivery weight gain was only 1.7 kg. In another patient, the banding was completely loosened during early pregnancy and re-tightened by the 33rd week, but the banding was completely re-loosened and her maximum weight gain was 9 kg during predelivery. The bands in the other four patients were completely loosened by the 24th week of pregnancy, and their median weight gain was 18 kg (range 13–30 kg). According to these reports and our results, we suppose that completely loosening the banding certainly must have significantly influenced the excessive maternal weight gain, and thus, keeping the banding was necessary for appropriate maternal weight control. Heude et al. [18] previously reported that high BMI during prepregnancy and weight gain during pregnancy were strongly related to the risk of gestational hypertension. In our study, the mean weight gain in patients with gestational hypertension after LAGB was 14.7 kg (range 9–23 kg), and this must have been undesirable for patients with a BMI of > 30 kg/m2. Moreover, the mean prepregnancy BMI of patients diagnosed with gestational hypertension was 35.4 kg/m2, which was relatively higher than that of patients without gestational hypertension (31.2 kg/m2). Therefore, both high BMI and excessive weight gain during pregnancy must have influenced the gestational blood pressure, thereby necessitating modification of the banding, such as loosening only in symptomatic patients.
According to our study, we should recognize the importance of a decrease in hemoglobin, particularly among patients who undergo MS. The mechanisms of anemia are commonly known, which has been attributed to iron, vitamin B12, and folate deficiency in almost all patients undergoing bariatric surgery. Therefore, routine supplementation to prevent elemental deficiencies has been recommended in the guidelines of the American Association of Clinical Endocrinologists, The Obesity Society, and ASMBS. According to the guidelines, the total elemental iron supplemented should be 45–60 mg via multivitamins for patients who undergo bariatric surgery as compared with the recommended individual intake of 10–18 mg per day especially for adult women. However, there has been some controversy concerning the rate of anemia after LRYGB over the various reported follow-up periods; therefore, the frequency and related micronutrient deficiencies are highly variable [19]. The specific difficulty in recovering from anemia caused by iron deficiency after MS has been commonly acknowledged to be due to the lack of an acidic environment, reducing the absorptive surface of the duodenum and proximal jejunum. Vargas-Ruiz et al. [20] found that the rates of iron deficiency and vitamin B12 deficiency were 54.5% and 27.2%, respectively, at 3 years after surgery in patients who underwent LRYGB with routine supplementation consisting of 18 mg of iron, 6 mg of vitamin B12, and 400 μg of folic acid. On the other hand, Del Villar Mardrigal et al. [21] also reported that the anemia rate was only 4% in patients who underwent LRYGB, with iron deficiency alone at 2.4% and iron deficiency combined with low vitamin B12 at under 1% only in women who received supplementation exceeding the recommended amounts: elemental iron 98.35 mg/day, vitamin B12 1 mg/day, and folic acid 400 μg/day. However, the percentage of patients with iron deficiency who did not develop anemia was 11%. At our center, the iron supplementation dosage was obviously low compared to the guidelines and previously published reports. However, the cases of maternal anemia post-LSG and post-LAGB were few in our series. Therefore, we presume that the dosage used at our center was adequate for patients who underwent restrictive surgery, but insufficient for those who underwent MS, especially reproductive-aged women. Consequently, we should consider the specific recommendation of additional supplementation or medical prescription especially for reproductive-aged women after MS.
Maternal anemia is known as one of the main causes of low birth weight [22]. In our study, none of the mothers who underwent LAGB and LSG subsequently developed maternal anemia, and the birth weight of their neonates were appropriate for their gestational age. Therefore, we focused on the relationship between maternal anemia and neonatal birth weight in patients who underwent MS and investigated their hemoglobin levels in the prepregnancy stage and their neonatal birth weight. In our study, though the period of gestation at delivery were similar in mothers with or without maternal anemia, the neonatal birth weight in patients with anemia was extremely lower than that in those without anemia, but this difference was not statistically significant due to the small number of patients who underwent MS. Maternal anemia is generally caused by low hemoglobin levels in early pregnancy and the greater expansion of plasma volume compared with the increase in red cell volume in late pregnancy. Haider et al. [23] also showed in a meta-analysis that the neonates who were born from mothers with anemia in the first or second trimester have higher risks of low birth weight, and an improvement in prenatal mean hemoglobin significantly increased their neonatal birth weight. Based on these findings, we believe that MS lead to malabsorption of oral supplements leading to worsening of the maternal anemia and, subsequently, relatively lower fetal birth weights. Therefore, we can generate a hypothesis that the gestational anemia in patients who underwent MS is one of the causes of low birth weight. From these results, we believe that the statistical relationship between anemia as a side effect of MS and neonatal low birth weight should be evaluated in the future using a multivariate analysis in a large number of patients who underwent MS. The findings may contribute to the development of a solution to the problem of low birth weight after bariatric surgery.
As an unexpected result, two patients who underwent LSG developed gestational diabetes mellitus. Their weight gain during pregnancy were 6.9 kg and 7.2 kg, which is regarded as an appropriate weight gain during the pregnancy period, and they were never diagnosed with type 2 diabetes mellitus during the preoperative period. Therefore, the specific cause of gestational diabetes mellitus after LSG was unclear in our study.
With regard to the difference in the mode of delivery, especially in emergency cesarean section, there were no relations with either the maternal condition or the type of bariatric surgery. Furthermore, there were no elective cesarean sections due to maternal obesity, even in patients with a relatively high BMI who underwent LAGB. In previous reports, statistical relationships between a shorter gestation period or preterm birth and bariatric surgery were noted, but the causes remained unclear in this study. Therefore, a detailed large-scale investigation on the maternal conditions after bariatric surgery may lead to significant findings.
Strengths and limitations of the study
The main strength of our study was its novelty, focusing on the maternal impacts related to neonatal growth and delivery analyzed according to the types of surgery. Bariatric surgery is currently considered the most effective treatment for morbid obesity, and various procedures are performed worldwide. However, the main concepts underlying bariatric surgery are based on the restriction and malabsorption of caloric intake, and the awareness of maternal treatment according to the type of restrictive surgery or MS is important. On the other hand, the main limitation of this study was its small sample size. Therefore, we could only mention the possibility of relationships between maternal anemia after MS and neonatal low birth weight. Moreover, considering our preliminary outcomes, future large-scale research is required to explore the causes of gestational diabetes mellitus development in patients who underwent LSG.
Conclusion
Not all bariatric procedures might lead to lower fetal birth weight. In particular, the birth weights of neonates born from mothers who had undergone restrictive bariatric were not decreased. The patients who underwent MS tended to be anemic mainly due to iron deficiency caused by taking only the standard dosage of iron supplements recommended for adult women; consequently, this appears to decrease the neonatal birth weight. Therefore, the nutritional status of the pregnant patients should be closely monitored, and the proper collaboration between the bariatric team and obstetricians will result in the effective management of maternal and neonatal health. Moreover, the causes of small for gestational age neonates after bariatric surgery may be determined by investigating the maternal characteristics and complications according to the types of surgery with a large patient cohort.
References
Sharma R, Biedenharm KR, Fender JM et al (2013) Lifestyle factors and reproductive health: taking control of your fertility. Reprod Biol Endocrinol 11:66
Ovesen PG, Jensen DM, Damm P et al (2015) Maternal and neonatal outcomes in pregnancies complicated by gestational diabetes: a nation-wide study. J Matern Fetal Neonatal Med 28(14):1720–1724
Weiss JL, Malone FD, Emig D et al (2004) Obesity, obstetric complications and cesarean delivery rate-a population-based screening study. Am J Obstet Gynecol 190(4):1091–1097
Mcdonald SD, Han Z, Mulla S et al (2010) Overweight and obesity in mothers and risk of preterm birth and low birth weight in infants: systematic review and meta-analysis. BMJ 341:c3428
Blomberg MI, Källén B (2010) Maternal obesity and morbid obesity: the risk for birth defects in the offspring. Birth Defects Res A Clin Mol Teratol 88(1):35–40
Ribaric G, Buchwald JN, McGlennon TW (2014) Diabetes and weight in comparative studies of bariatric surgery vs conventional medical therapy: a systematic review and meta-analysis. Obes Surg 24:437–455
American College of Obstetricians and Gynecologists (2005) ACOG Committee Opinion 315: obesity in pregnancy. Obstet Gynecol 106:671–675
Chevrot A, Kayem G, Coupaye M et al (2016) Impact of bariatric surgery on fetal growth restriction: experience of a perinatal and bariatric surgery center. Am J Obstet Gynecol 214(5):655. e1-7
Galazis N, Docheva N, Simillis C et al (2014) Maternal and neonatal outcomes in women undergoing bariatric surgery: a systematic review and meta-analysis. Eur J Obstet Gynecol Reprod Biol 181:45–53
Roos N, Neovius M, Cnattinguis S et al (2013) Perinatal outcomes after bariatric surgery: nationwide population based matched cohort study. BMJ 347:f6460
Johansson K, Cnattinguis S, Näslund I et al (2015) Outcomes of pregnancy after bariatric surgery. N Engl J Med 372(9):814–824
Angrisani L, Santonicola A, lovino P, et al. Bariatric surgery and endoluminal procedures: IFSO worldwide survey. Obes Surg 2017;27(9): 2279–89.
International Association of Diabetes and Pregnancy Study Groups (2010) Recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care 33(3):676–682
Rsmussen KM, Yaktine AL (2009) Weight gain during pregnancy: reexamining the guidelines, report brief, institute of medicine (IOM) of national academies
Mechanick JI, Youdim A, Jones DB et al (2013) Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient-2013 update: cosponsored by American Association of Clinical Endocrinologists: The Obesity Society, and American Society for Metabolic and Bariatric Surgery. Obesity 21:S1–27
Carelli AM, Ren CJ, Youn HA et al (2011) Impact of laparoscopic adjustable gastric banding on pregnancy, maternal weight, and neonatal health. Obes Surg 21(10):1552–1558
Skull AJ, Slater GH, Duncombe JE et al (2004) Laparoscopic adjustable banding in pregnancy: safety, patient tolerance and effect on obesity-related pregnancy outcomes. Obes Surg 14(2):230–235
Heude B, Thiébaugeorges O, Goua V et al (2012) Pre-pregnancy body mass index and weight gain during pregnancy: relation with gestational diabetes and hypertension, and birth outcomes. Matern Child Health J 16(2):355–363
Cable CT, Colbert CY, Showalter T et al (2011) Prevalence of anemia after Roux-en-Y gastric bypass surgery: what is the right number? Surg Obes Relat Dis 7(2):134–139
Vargas-Ruiz AG, Hernández-Rivera G, Herrera MF (2008) Prevalence of iron, folate, and vitamin B12 deficiency anemia after laparoscopic Roux-en-Y gastric bypass. Obes Surg 18(3):288–293
Del Villar Madrigal E, Neme-Yunes Y, Clavellina-Gaytan D et al (2015) Anemia after Roux-en-Y gastric bypass: how feasible to eliminate the risk by proper supplementation? Obes Surg 25(1):80–84
Kaur M, Chauhan A, Manzar MD et al (2015) Maternal anaemia and neonatal outcome: a prospective study on urban pregnant women. J Clin Diagn Res 9(12):QC04–8
Haider BA, Olofin I, Wang M et al (2013) Anaemia, prenatal iron use, and risk of adverse pregnancy outcomes: systematic review and meta-analysis. BMJ 346:f3443
Author information
Authors and Affiliations
Contributions
AW and KK conceived of the presented idea. AW designed the study, and wrote the initial draft of the manuscript. EK and HH supported to analysis and interpretation of data, and assisted in the preparation of the manuscript. SY and KK supervised the findings of this work. All other authors have contributed to data collection and interpretation, and critically reviewed the manuscript. All authors approved the final version of the manuscript, and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
All other authors have no conflicts of interest to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Watanabe, A., Seki, Y., Haruta, H. et al. Maternal impacts and perinatal outcomes after three types of bariatric surgery at a single institution. Arch Gynecol Obstet 300, 145–152 (2019). https://doi.org/10.1007/s00404-019-05195-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05195-9